Abstract
We have previously shown that acetaldehyde, a constituent of tobacco smoke, increases nicotine self-administration in adolescent, but not adult, rats. The aim of this study was to determine whether acetaldehyde influences other behavioral, endocrine, or neuronal responses to nicotine at either age. Juvenile (postnatal day (P) 27) and adult (P90) male Sprague–Dawley rats were treated with saline, acetaldehyde (16 μg/kg/injection × 2, i.v.), nicotine (30 μg/kg/injection × 2, i.v.) or a combination of acetaldehyde and nicotine. Locomotion and center time were evaluated for 30 min in a novel open field, before measurement of plasma corticosterone levels and brain c-fos mRNA. Nicotine increased locomotor activity in juveniles but decreased it in adults; in contrast, center time was increased at both ages. Acetaldehyde potentiated nicotine's locomotor effects, but not center time. Nicotine induced c-fos expression in the bed nucleus of the stria terminalis, the central nucleus of the amygdala (CeA), nucleus accumbens, and the superior colliculus (SC) at both ages, whereas it activated the hypothalamic paraventricular nucleus (PVN) and consequent corticosterone secretion only in adults. Acetaldehyde potentiated nicotine-induced c-fos in CeA and SC, and activation of PVN c-fos expression/plasma corticosterone release; however, this drug interaction was only observed in behaviorally tested animals, not those that were minimally stressed. Thus, acetaldehyde may modulate the interaction of nicotine and stress. Although pharmacokinetic studies showed that acetaldehyde did not change nicotine levels in either brain or serum, nicotine penetration into the brain was slower in juveniles as compared to adults.
Similar content being viewed by others
INTRODUCTION
Adolescence is a critical period of vulnerability for the onset of smoking (Kandel and Logan, 1984). Approximately 80% of smokers initiate tobacco use before age 18 (US Department of Health and Human Services, 1994). As compared to their adult counterparts, juveniles more readily develop symptoms of tobacco dependence (Kandel and Chen, 2000) and those who begin smoking in early adolescence are more likely to experience difficulty in quitting than those who start at later ages (Breslau and Peterson, 1996; Chen and Millar, 1998). Although extensive efforts have been made to prevent acquisition of smoking, more than 4000 adolescents in the United States start smoking each day, of whom one-third will die prematurely from smoking-related diseases (Centers for Disease Control and Prevention, 2003). It is therefore important to understand the factors that lead to smoking so as to develop more effective smoking prevention and cessation therapies.
Animal models, with fewer ethical constraints and greater control of experimental variables, have provided valuable information about adolescent drug addiction. Adolescence, when risk-taking and novelty seeking behaviors emerge, has been defined in rodents as the fifth and sixth postnatal weeks (Spear, 2000). Animal studies have shown that nicotine, the major psychoactive component of tobacco, has distinct effects on adolescents. Adolescent rats are more sensitive to nicotine-induced conditioned place preference (Vastola et al, 2002; Belluzzi et al, 2004), and self-administer more nicotine than adults (Adriani et al, 2002; Levin et al, 2003; Chen et al, 2006). Whereas these findings indicate that juveniles are more sensitive to the rewarding effects of nicotine, they are also less sensitive to its aversive effects (Wilmouth and Spear, 2004; O’Dell et al, 2006; Shram et al, 2006). This shift in the balance of rewarding and aversive effects of nicotine may make adolescents more vulnerable to nicotine addiction.
Although nicotine is believed to be the major psychoactive substance in tobacco, nicotine replacement therapy is not highly effective as a treatment for tobacco addiction, particularly in adolescents (Moolchan et al, 2005). Given that there are thousands of components in tobacco smoke, some of which also have pharmacological effects (US Surgeon General's Report, 1989), tobacco research should also take these components into account. Acetaldehyde, which has been studied extensively as a metabolite of ethanol (Quertemont et al, 2005), is also present in tobacco smoke in a concentration half that of nicotine (Hoffmann and Hoffmann, 2001). We have previously shown a synergistic interaction of nicotine and acetaldehyde in self-administration in juveniles, which was not observed in adults (Belluzzi et al, 2005). However, the underlying mechanisms are not yet clear. Although acetaldehyde has been reported to induce behavioral effects, including reward, these are usually only observed following peripheral administration of high doses of drug or following central administration (Quertemont et al, 2005). Given the localization of the metabolic enzyme, aldehyde dehydrogenase, at capillary endothelial junctions, there has been considerable controversy as to whether acetaldehyde can cross the blood brain barrier (BBB).
The present study was designed to determine whether acetaldehyde influences other behavioral effects of nicotine in adolescents and/or adults, and to evaluate the mechanisms underlying acetaldehyde enhancement of nicotine-induced responding. As it is difficult to examine mechanisms using the self-administration paradigm in which animals control intravenous drug intake, we have evaluated the effects of experimenter administration of nicotine, with and without acetaldehyde, given by the intravenous route. In order to determine possible mechanisms underlying acetaldehyde-induced changes in behavior, we have examined potential peripheral and central targets of drug action; peripheral plasma corticosterone levels and central neuronal activation were measured in parallel in the same groups of animals. We have also conducted pharmacokinetic analyses to determine whether acetaldehyde influences the penetration of nicotine into the brain.
MATERIALS AND METHODS
Animals
Male Sprague–Dawley rats were maintained in a temperature (21°C) and humidity (50%) controlled room on a 12-h light–dark cycle (lights on 0700–1900 hours) with unlimited access to food and water. All experiments were carried out in accordance with the Institutional Animal Care and Use Committee at the University of California, Irvine, and were consistent with Federal guidelines. To minimize prenatal stress effects on the offspring, young animals were delivered with dams at P16 and habituated in the vivarium for 5 days before weaning at P21. Four animals per litter were assigned to each experimental group and treated with different drugs. Adults, aged P80, were delivered a minimum of 1 week before use. All animals were group housed until implantation of intravenous catheters.
Surgical Implantation of Intravenous Catheters
Catheter construction and implantation was as described previously (Belluzzi et al, 2005). Animals were anesthetized with Equithesin (2.5 ml/kg juveniles, 3 ml/kg adults, i.p.) and a chronic catheter was surgically implanted into the right external jugular vein. The catheter was passed subcutaneously from the animals’ back to the jugular vein where the tubing was inserted. The cannula assembly was mounted on the animal's back and was sealed to prevent clogging and to keep a closed system. The wounds were closed with wound clips, antiseptic ointment was applied to the wounds, and Baytril (0.1 ml/150 g, i.m.) was injected to prevent infection. The animals were kept in a warm cage for postsurgical observation until they recovered from anesthesia.
Drug Treatment
All of the following experiments were conducted on animals aged P27 and P90, which were the starting ages for our previous self-administration study (Belluzzi et al, 2005). Nicotine doses and concentrations are expressed as weight of the base. To mimic the first two injections of the self-administration, animals were injected with drugs twice at an interval of 1 min.
For initial experiments, handling and housing conditions were similar to that used in the previous self-administration studies (Belluzzi et al, 2005). Animals were single housed after intravenous catheter implantation. For 3 days before the experiment, the catheters were flushed with 0.2 ml of a heparinized saline solution (600 or 300 U of heparin in 30 ml saline for adult and young animals, respectively) to prevent clogging. Propofol (10 mg/ml), a fast-acting, short-lived intravenous anesthetic, was administered (0.1 ml for adults and 0.05 ml for juveniles) to test catheter patency 1 day before the experiment. Only rats that were immediately anesthetized by propofol and recovered from anesthesia within 10 min were used. On the experimental day, rats were habituated to the lab for 30 min. The experiments were carried out, and samples collected, from 0800 to 1100 hours when plasma corticosterone concentration is at its lowest level (Critchlow et al, 1963). Animals were given two intravenous injections, spaced 1 min apart, of saline, acetaldehyde (16 μg/kg/100 μl), nicotine (30 μg/kg/100 μl), or a combination of acetaldehyde and nicotine (NicAc). These doses of drugs are what were used in our previous self-administration experiments (Belluzzi et al, 2005), and the inter-injection time interval was equivalent to the timeout period for reinforced responding. Animals were placed into locomotion boxes immediately after drug administration and monitored for 30 min, after which they were removed and immediately sacrificed by decapitation. Brains were extracted and frozen in 2-methylbutane at −20°C for 30 s, then stored at −70°C until use. Trunk blood (2 ml) was collected in tubes to which 1.48 mg/ml of ethylenediaminetetracetic acid was added. Blood samples were centrifuged at 2200 r.p.m. in 4°C for 30 min. Aliquots of plasma supernatant were stored at −20°C before analysis of corticosterone concentration.
The above behavioral testing condition is significantly different from our standard paradigm for c-fos experiments, in which housing and handling stress are minimized (Park et al, 2006). To examine whether experimental condition influenced drug effects on neuronal and hormonal activation, we repeated these analyses in other groups of animals under minimal stress conditions. These animals were group housed after catheter implantation, and handled daily for 3 days before catheters were flushed with heparinized saline solution as described above. Each animal was also habituated for 5 min daily in a single cage with home cage bedding. Propofol tests were carried out as described above. On the experimental day, animals were habituated to the test environment for 120 min before drug injection. After drug administration, animals were placed into the cages to which they had been habituated without further behavioral testing. Blood and brain samples were collected 30 min after drug injection as described above.
Behavioral Test: Locomotion and Center Time
Behaviorally tested animals were placed into the middle of a well-illuminated locomotion box immediately after drug injection. Locomotor activity was measured for 30 min in an open-field activity system measuring 43.2 × 43.2 × 30.5 cm (MED Associates Inc., St Albans, VT). Horizontal movement was monitored by 16 evenly spaced infrared beams located along two adjacent sides of the chamber. The time spent in the center area was monitored simultaneously.
In Situ Hybridization
Coronal sections were cryostat cut at a thickness of 20 μm at −20°C. Sections were mounted onto poly L-lysine-coated glass slides and fixed with 4% paraformaldehyde in 0.1 M phosphate-buffered saline (PBS) for 1 h at room temperature. Tissue sections were washed in 0.1 M PBS for 3 × 5 min, dried and stored in airtight boxes at −20°C until use.
Tissue sections were processed for in situ hybridization according to the method of Winzer-Serhan et al (1999). [35S]-labeled riboprobes were transcribed in antisense and sense directions from a pGEM-3Z plasmid containing a 680 bp fragment of c-fos cDNA between T7 and SP6 promoter sites (kindly provided by Dr Stanley Watson, University of Michigan). Sections were pretreated with proteinase K (0.05 μg/ml), acetylated, dehydrated through graded ethanols (50, 75, 95, and 100%) and air-dried, then incubated for 18 h at 60°C with hybridization solution containing 35[S]-labeled sense or antisense riboprobes (1 × 107 c.p.m./ml). After hybridization, sections were treated with RNase A and washed at high stringency. Tissue sections were dehydrated and exposed to Kodak Biomax film with 14C standards of known radioactivity (Winzer-Serhan et al, 1999).
Autoradiographic images were quantified using a computer-based image analysis system (MCID, Image Research Inc., St Catharines, ON, Canada). Corresponding sections were chosen from different ages. Brain areas on autoradiograms were identified with reference to adjacent brain sections processed for fast cresyl violet stain (Paxinos and Watson, 1986). Brain areas chosen for analysis included those that have been previously reported to be activated by nicotine in adolescent or adult forebrain (Leslie et al, 2004; Schochet et al, 2005; Park et al, 2006). These included cingulate, motor, somatosensory, and retrosplenial cortices, paraventricular nucleus of the hypothalamus (PVN), central nucleus of the amygdale (CeA), superior colliculus (SC), bed nucleus of the stria terminalis (BNST), and nucleus accumbens (NAc) shell. Sections were also qualitatively analyzed by visual inspection, and one region, the paraventricular nucleus of the thalamus (PVTh), which appeared to exhibit systematic differences in c-fos levels across groups, was selected for further quantitative analysis. Optical densities in discrete brain regions were measured and the corresponding values of radioactivity were determined by interpolation from a standard curve, generated from 14C standards of known radioactivity (Broide et al, 1995). In each brain region, mRNA expression was quantified by subtracting corresponding regional measures of sense hybridization. Averages were attained from readings of the right and left hemispheres for each brain region.
Plasma Corticosterone Radioimmunoassay
Plasma samples were thawed on ice and plasma corticosterone concentrations were determined in duplicate samples using a commercial RIA kit (ICN, Costa Mesa, CA) as instructed. Briefly, diluted plasma was incubated with rabbit anti-corticosterone serum in the presence of synthetic 125I-corticosterone at room temperature for 2 h. The complex was precipitated by centrifugation at 2200 r.p.m. for 15 min after adding goat anti-rabbit gamma globulin. The radioactivity in the precipitate was determined by gamma scintillation counter. A standard curve was generated with a series of known corticosterone samples using commercial software (Prism, GraphPad Software, San Diego, California, USA) and the plasma hormonal concentrations in the unknown samples were interpolated from the curve.
Nicotine Pharmacokinetic Analysis
Nicotine levels in the brain and serum were analyzed in another group of animals aged P27 and P90 under behavioral test conditions. Brains and trunk blood were collected 1, 5, 10, or 30 min after injection of nicotine or NicAc in the same doses as were used in the behavioral experiment (n=5–12 per group). Brains were stored at −20°C until nicotine assay. Brain and blood samples were processed as described by Pentel et al (2000). Blood samples were allowed to sit on ice for 10 min before centrifugation at 2200 r.p.m. in 4°C for 30 min. Aliquots of plasma supernatant were stored at −20°C before use.
Nicotine concentrations in serum and brain were measured by gas chromatography with nitrogen-phosphorous detection (Jacob et al, 1981). Nicotine levels in the brains were normalized according to brain weight and expressed as ng/g brain tissue.
Statistics
Locomotor activity and center time was analyzed using a three-way ANOVA for Age × Drug × Time, with repeated measures on Time. Plasma corticosterone levels were independently analyzed using a two-way ANOVA for Age × Drug. C-fos mRNA was analyzed using a three-way ANOVA for Age × Drug × Brain area, with repeated measures on Brain area. Nicotine levels in brain and serum, and brain:serum ratios for each animal, were analyzed using three-way ANOVA for Age × Drug × Time. Significant main effects were further evaluated with one-way ANOVAs and Bonferroni-or Dunnett's-corrected post hoc comparison tests.
RESULTS
Acetaldehyde Enhances Nicotine's Locomotor Effects in Both Adolescent and Adult Rats
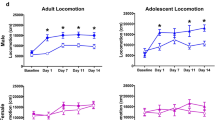
As shown in Figure 1, nicotine significantly increased locomotion at P27 as compared to saline-treated controls (p<0.01), whereas it decreased locomotion in adults (p<0.01). This drug effect was observed only during the first 5 min of monitoring in the novel locomotor apparatus. Although acetaldehyde alone had no significant effect, it potentiated nicotine's effects at both ages. Acetaldehyde significantly increased the duration of action of nicotine from 5 to 10 min at each age, and further potentiated the initial inhibitory locomotor effects of nicotine in adults (p<0.05).
Time course of ambulatory count in novel environment during 30 min after drug injection. P27 (a) and adult (b) animals were treated with saline (open circles and dotted lines), acetaldehyde (filled circles and dotted lines) (16 μg/kg/injection × 2, i.v.), nicotine (open circles and solid lines) (30 μg/kg/injection × 2, i.v.), or NicAc (filled circles and solid lines). There is a significant age effect (F1,74=29.840, p<0.0001) and an interaction of age by drug (F3,74=6.621, p=0.001). *p<0.05, **p<0.01, significantly different from saline control. +p<0.05, +++p<0.001, significantly different from nicotine alone. n=7–13 per group.
Acetaldehyde does not Influence Nicotine's Anxiolytic Effects at Either Age
Time spent in the center area of the locomotor apparatus was evaluated during locomotor monitoring (Figure 2). As there were no age differences (F1,73=0.000, p=0.990), data from adults and juveniles were combined. Consistent with an anxiolytic effect (Prut and Belzung, 2003), nicotine significantly increased center time during the first 5 min. There was also a trend of increased center time at this time point after NicAc treatment, although it did not reach significance (Figure 2a). Nicotine significantly increased total center time as compared to saline-treated controls (p<0.05). Acetaldehyde had no effect on center time, alone or in combination with nicotine (Figure 2b).
Time spent in the center of novel locomotion chambers during the 30 min after drug injection. As there is significant drug effect (F3,73=5.306, p<0.01) but not age effect (F1,73=0.000, p=0.990), data from both ages are combined. Time course (a) and total center time (b) were evaluated in animals treated with saline (open circles and dotted lines; open bars), acetaldehyde (filled circles and dotted lines; horizontal bars) (16 μg/kg/injection × 2, i.v.), nicotine (open circles and solid lines; vertical bars) (30 μg/kg/injection × 2, i.v.), or NicAc (filled circles and solid lines; filled bars). *p<0.05 significantly different from saline treatment. n=14–26 per group.
Acetaldehyde Enhances Nicotine Activation of the Hypothalamo-Pituitary-Adrenal Axis in Behaviorally Tested Adults
Following the measurement of locomotor activity and center time, blood and brain samples were collected. Hypothalamo-Pituitary-Adrenal (HPA) axis activation was evaluated by examining c-fos mRNA expression in the PVN (Figure 3a) and plasma corticosterone levels (Figure 3b). In adults, nicotine significantly increased c-fos mRNA expression in the PVN (p<0.01) and significantly induced corticosterone release (p<0.01), as compared to saline-treated controls. In contrast, nicotine had no effects at P27. Acetaldehyde alone had no direct effect at either age. However, acetaldehyde potentiated nicotine-induced c-fos mRNA expression in adult PVN (p<0.01) and increased nicotine-induced corticosterone release in adults (p<0.01). In contrast, NicAc had no effects on HPA activity at P27.
HPA axis activation in behaviorally tested animals. C-fos mRNA expression in the PVN (a) and plasma corticosterone levels (b) were evaluated in P27 and adult rats treated with saline (open bars), acetaldehyde (horizontal bars) (16 μg/kg/injection × 2, i.v.), nicotine (vertical bars) (30 μg/kg/injection × 2, i.v.), or NicAc (filled bars). There is significant drug effect (F3,24=15.47, p<0.001), age effect (F1,24=9.890, p<0.01), and interaction of age by drug (F3,24=7.373, p<0.01) in the PVN c-fos mRNA expression. In parallel, there is also a significant drug effect (F3,53=17.91, p<0.001), age effect (F1,53=23.64, p<0.001), and an interaction of age by drug (F3,53=19.46, p<0.001) in plasma corticosterone levels. **p<0.01 significantly different from saline. ++p<0.01 significantly different from nicotine alone. n=4–5 for each c-fos group and n=6–8 for each corticosterone group.
Acetaldehyde Enhances Nicotine-Induced c-fos mRNA Expression in Forebrain Regions of Behaviorally Tested Animals
C-fos mRNA expression was also evaluated in other brain areas of behaviorally tested animals. There were no drug effects on cingulate, motor, somatosensory, or retrosplenial cortex (F3,27=1.839, p=0.164). In contrast, we found drug effects in the CeA, SC, BNST, and NAc shell (Figure 4). As there were no age differences (F1,27=1.086, p=0.307) in c-fos expression in these regions, measurements from both ages were combined. Nicotine significantly increased c-fos mRNA expression in the CeA (p<0.01), SC (p<0.01), BNST (p<0.01), and NAc shell (p<0.01), as compared to saline-treated controls. Acetaldehyde alone did not induce c-fos mRNA expression in any of these brain regions. However, acetaldehyde potentiated the effects of nicotine on c-fos mRNA expression in CeA (p<0.05) and SC (p<0.001), but not in BNST or NAc shell.
C-fos mRNA expression in brains of behaviorally tested animals. c-fos mRNA expression was evaluated in the CeA (a), the SC (b), BNST (c), and NAc shell (d) in animals treated with saline (open bars), acetaldehyde (horizontal bars) (16 μg/kg/injection × 2, i.v.), nicotine (vertical bars) (30 μg/kg/injection × 2, i.v.), and NicAc (filled bars). There is a significant drug effect (F3,27=65.182, p<0.0001) but not age effect (F1,27=1.086, p=0.307), so data from both ages are combined. **p<0.01 significantly different from saline. +p<0.05, +++p<0.001 significantly different from nicotine alone. n=8–10 per group.
Acetaldehyde does not Enhance Nicotine-Induced Activation of the HPA Axis in Minimally Stressed Adult Animals
To examine whether experimental conditions influence drug effects, we evaluated HPA activity in another group of animals, which were group housed, well-handled and habituated to the test environment. They were also returned to the habituated cages after drug injection instead of being placed in novel locomotion chambers. C-fos mRNA expression in the PVN (Figure 5a) and plasma corticosterone levels (Figure 5b) were evaluated.
HPA axis activation in minimally stressed animals. C-fos mRNA expression in the PVN (a) and plasma corticosterone levels (b) were evaluated in P27 and adult rats treated with saline (open bars), acetaldehyde (horizontal bars) (16 μg/kg/injection × 2, i.v.), nicotine (vertical bars) (30 μg/kg/injection × 2, i.v.), or NicAc (filled bars). There is a significant drug effect (F3,27=28.63, p<0.001), age effect (F1,27=18.57, p<0.001), and interaction of age by drug ((F3,27=18.90, p<0.001) in the PVN c-fos mRNA expression. In parallel, there is also a significant drug effect (F3,26=38.31, p<0.001), age effect ((F1,26=76.67, p<0.001), and interaction of age by drug (F3,26=30.47, p<0.001) in plasma corticosterone levels. **p<0.01 significantly different from saline. n=4–5 per group.
In this minimally stressed group, corticosterone levels in saline-treated juveniles were significantly lower than that in behaviorally tested animals (p<0.05). A similar trend of decreased basal corticosterone levels was observed in minimally stressed adults as compared to behaviorally tested adults, although it did not reach significance. Nicotine significantly increased c-fos mRNA expression in the PVN (p<0.01) and corticosterone release (p<0.01) in minimally stressed adults as compared to saline-treated controls, whereas it had no effects at P27. Nicotine-induced corticosterone secretion in minimally stressed adults was significantly higher than in the behaviorally tested group (p<0.05). Acetaldehyde alone had no direct effect on PVN c-fos mRNA levels or on plasma corticosterone at either age. Furthermore, in contrast to behaviorally tested adults, acetaldehyde did not enhance the action of nicotine on HPA activity of minimally stressed adults.
Acetaldehyde does not Enhance Nicotine-Induced c-fos mRNA Expression in Forebrain Regions of Minimally Stressed Animals
In minimally stressed animals, c-fos mRNA expression was evaluated in the same brain areas in which there were significant drug effects under behavioral test conditions (Figure 6). Measurements from the two ages were combined, as there were no age differences (F1,26=0.985, p=0.330). Similar to behaviorally tested animals, nicotine significantly induced c-fos mRNA expression in the CeA (p<0.01), BNST (p<0.01), SC (p<0.01), and NAc shell (p<0.01), as compared to saline-treated controls. Acetaldehyde had no effect by itself and, in contrast to behaviorally tested animals, did not potentiate the effects of nicotine in any of these brain regions.
C-fos mRNA expression in the brains of minimally stressed animals. C-fos mRNA expression was evaluated in the CeA (a), SC (b), BNST (c), and NAc shell (d) in animals treated with saline (open bars), acetaldehyde (horizontal bars) (16 μg/kg/injection × 2, i.v.), nicotine (vertical bars) (30 μg/kg/injection × 2, i.v.), or NicAc (filled bars). There is a significant drug effect (F3,26=115.545, p<0.0001) but no age effect (F1,26=0.985, p=0.330), so data from both ages are combined. **p<0.01 significantly different from saline. n=8–10 per group.
Both Acetaldehyde and Nicotine Stimulate the Thalamic Paraventricular Nucleus in Juveniles
There was only one brain region examined, the PVTh, in which c-fos mRNA expression was increased by acetaldehyde alone (Figure 7). This dorsal thalamic region, which is minimally protected by the BBB (Ueno et al, 2000), was equally activated by acetaldehyde, nicotine and the combination of the two. These drug effects were restricted to juveniles, and were observed in both behaviorally tested and minimally stressed animals.
C-fos mRNA expression in the PVTh in both behaviorally tested animals (a) and minimally stressed animals (b) in P27 and adult rats. Animals were treated with saline (open bars), acetaldehyde (horizontal bars) (16 μg/kg/injection × 2, i.v.), nicotine (vertical bars) (30 μg/kg/injection × 2, i.v.), or NicAc (filled bars). There are significant effects of age (F1,50=4.2915, p=0.0435), drug (F3,50=5.8476, p=0.0017), experimental condition (F1,50=7.8765, p=0.0071), and a significant interaction of age by drug (F3,50=5.3873, p=0.0027). *p<0.05 significantly different from saline. n=4–5 per group.
Age but not Drug Effects on Nicotine Levels in the Brain and Serum
Acetaldehyde did not alter nicotine concentration in the brain (F1,101=0.896, p=0.346), serum (F1,101=0.212, p=0.646), or the ratio of nicotine levels in the brain vs serum (F1,101=0.291, p=0.591). Therefore, data from nicotine and NicAc were combined (Figure 8). Nicotine levels in the brain and serum decreased over time in both juveniles and adults. There were no significant age differences in serum nicotine levels (F1,109=3.555, p>0.05) (Figure 8a). In contrast, brain nicotine levels were significantly different in juveniles and adults (F1,109=50.22, p<0.001). Post hoc analysis showed that brain nicotine levels during the first 5 min after drug injection were significantly higher in adults as compared to juveniles (1 min, p<0.001; 5 min, p<0.05) (Figure 8b). The brain: serum nicotine concentration ratio in the first minute was also significantly higher in adults as compared to juveniles (p<0.05) (Figure 8c).
Nicotine levels in the brain (a), serum (b), and brain to serum nicotine concentration ratio(c) in P27 (white bars) and adult (black bars) rats after injection of nicotine (30 μg/kg/injection × 2, i.v.) or NicAc. There were no drug effects on nicotine concentrations in the brain (F1,101=0.896, p=0.346), serum (F1,101=0.212, p=0.646), or the brain:serum nicotine concentration ratio(F1,101=0.291, p=0.591). Therefore, data from nicotine and NicAc were combined. There were significant time differences (F3,109=10.45, p<0.001) but no age differences (F1,109=3.555, p>0.05) nor any interaction of age by time (F3,10=0.3188, p>0.05) in serum nicotine levels. In contrast, there were significant effects of age (F1,109=50.22, p<0.001), time (F3,109=111.1, p<0.001), and interaction of age by time(F3,109=6.324, p<0.001) in brain nicotine levels. There were significant time differences (F3,109=6.489, p<0.001) and interaction of age by time (F3,109=3.443, p<0.05) in brain:serum nicotine concentration ratio. ***p<0.001, *p<0.05 significantly different from P27 (n=5–12 per group).
DISCUSSION
Early adolescence is a period of increased vulnerability for initiation of cigarette smoking as compared with later ages (Kandel and Chen, 2000). However, the underlying mechanisms are not well understood. Although nicotine is believed to be the major psychoactive component in tobacco, nicotine's rewarding and locomotor stimulant effects in animal studies are weaker than that of other psychostimulants (Manzardo et al, 2002; Villegier et al, 2006). Given that nicotine is not the only psychoactive ingredient in tobacco, other tobacco constituents may also contribute to smoking behaviors. We have previously shown a synergistic interaction of nicotine and acetaldehyde in self-administration, which was observed only in juveniles but not in adults (Belluzzi et al, 2005). In the present studies, we have further evaluated the interaction of nicotine and acetaldehyde, and have examined underlying mechanisms. As it is difficult to assess mechanisms using the self-administration paradigm in which the animal controls drug administration, we have modeled the first two self-injections with experimenter controlled intravenous injections. Thus, we have examined initial response to the drugs.
We have evaluated acetaldehyde's effects on endocrine, neuronal and other behavioral responses to nicotine, as well as nicotine levels in the brain and serum. To examine whether nicotine-acetaldehyde interactions are age-specific, we have studied both juveniles and adults at the same ages used for our previous self-administration studies (Belluzzi et al, 2005). The behaviorally tested animals were examined under the same housing and handling conditions as that used for self-administration. To evaluate the influence of the environment on endocrine and neuronal responses to drugs, these measurements were repeated in another group of animals, which were subjected to minimal housing and handling stress. The intravenous drug administration paradigm which we have used more closely models the pharmacokinetics of smoking than other routes of administration. The amount of nicotine injected into each animal is comparable to that inhaled in 2–4 cigarettes (Benowitz et al, 1990). The ratio of nicotine to acetaldehyde is also consistent with the relative concentrations found in cigarette smoke (Hoffmann and Hoffmann, 2001).
Behavioral Studies
Consistent with other findings in our laboratory (Cao et al, in preparation), there was an age-dependent transition from ambulatory stimulant effects of nicotine in early adolescence to depressant effects in adulthood, which was only observed during the first 5 min of testing. These age differences are also consistent with findings of other studies in which different routes of drug administration were used (Belluzzi et al, 2004). Given that these groups of animals were not habituated to the experimental apparatus before the behavioral test, the short-term effect of nicotine on locomotor activity may reflect an interaction of novel environment and drug effects. When in a habituated environment, it has been shown that adult rats do not show a depressant locomotor response to nicotine (O’Neill et al, 1991). Acetaldehyde potentiated the locomotor effects of nicotine at both ages and consequently increased the observed age differences. Acetaldehyde not only increased but also prolonged nicotine's depressant effects in adults. In contrast, acetaldehyde only prolonged but did not increase nicotine's stimulant effects in juveniles, which may reflect a ceiling effect of nicotine on locomotor activity in the first 5 min.
Time spent in the center area of the novel locomotor apparatus, which is inversely correlated with anxiety (Prut and Belzung, 2003), was evaluated simultaneously with locomotor behavior. Although nicotine has been reported to have both anxiolytic and anxiogenic effects, there are inconsistencies in the literature, which may reflect differences in anxiety models and experimental conditions (Picciotto et al, 2002, review). The present study has shown that nicotine increased center time, which indicates anxiolytic effects, in both juveniles and adults. In contrast to the effects on locomotion, acetaldehyde did not alter the anxiolytic effect of nicotine. Thus, acetaldehyde potentiated some nicotine-induced behaviors but not others, even when they were measured simultaneously. This may reflect distinct neuronal circuitry underlying the two behaviors.
Mechanisms
Although acetaldehyde has been studied extensively in alcohol research, it is controversial as to whether acetaldehyde can cross the BBB and directly affect the central nervous system (Quertemont et al, 2005). To overcome the aldehyde dehydrogenase in the BBB (Zimatkin, 1991), blood acetaldehyde has to be present at high concentrations (>100 μM) (Tabakoff et al, 1976). Consequently, acetaldehyde, at the present dose, may not cross the BBB, at least in adults. However, it is still not clear whether this is also true in juveniles because of the lack of acetaldehyde pharmacokinetics studies at earlier ages. In order to evaluate mechanisms underlying acetaldehyde potentiation of nicotine effects, we have studied both brain and periphery.
Nicotine pharmacokinetics
One hypothesis that was tested was that acetaldehyde alters nicotine pharmacokinetics and accumulation in the brain. No effect of acetaldehyde on nicotine levels in brain or serum was observed. However, there were significant age differences in initial nicotine penetration into the brain, which was faster in adults than juveniles. Although this effect is transient, it may contribute to age differences in behavioral responses to nicotine. It has been reported that brain nicotine levels largely correlate with nicotine's locomotor effects (Hatchell and Collins, 1980; Pentel et al, 2000). Furthermore, the rate of nicotine delivery significantly influences drug-induced plasticity in neuronal and behavioral response (Samaha et al, 2005). However, there are several reasons why it is unlikely that pharmacokinetic differences alone can explain age differences in nicotine effect: (1) the acute locomotor effect of nicotine on adult rats was not found to be influenced by the rate of drug administration (Samaha et al, 2005); (2) the contrasting locomotor effects of nicotine in juveniles and adults are still observed when drugs are administered by subcutaneous injection, which would be expected to yield slower rates of delivery to the brain (Belluzzi et al, 2004); (3) acetaldehyde does not influence nicotine pharmacokinetics but does potentiate the drug-induced locomotor effects at each age.
Neuronal mechanisms
We have examined expression of the immediate early gene, c-fos, to evaluate central neuronal responses to drug administration. Whereas previous studies, in which nicotine was given by the subcutaneous route, have shown age differences in cortical c-fos mRNA expression (Leslie et al, 2004; Schochet et al, 2005), we did not detect significant increases in cortical c-fos mRNA levels at either age when nicotine was administered intravenously in behaviorally tested animals. Other areas, which have been reported to be activated by subcutaneous nicotine injection in adolescents and/or adults (Park et al, 2006), including CeA, BNST, NAc, and SC, showed increased c-fos expression following intravenous drug administration with no significant effect of age. Acetaldehyde potentiated the effect of nicotine in two of these regions, SC and CeA, which are involved in defensive behaviors (Brandao et al, 1999). In contrast, this did not occur in NAc and BNST, which are more involved in the regulation of appetitive behaviors and neuroendocrine output (Swanson, 2000). These findings suggest that acetaldehyde potentiation is specific to some neuronal circuitry. Interestingly, this effect of acetaldehyde was only observed in behaviorally tested but not in minimally stressed animals. This is consistent with previous findings, which show that environment can modulate psychostimulant-induced c-fos expression (Badiani and Robinson, 2004). The environmental dependence of the observed drug interaction suggests that this effect of acetaldehyde may be associated with stress-induced plasticity.
In two brain regions, PVTh and PVN, nicotine-induced c-fos mRNA expression was age dependent. In the PVTh of both minimally stressed and behaviorally tested juveniles, both nicotine and acetaldehyde induced c-fos expression in a non-additive manner. PVTh, which is not protected by the BBB (Ueno et al, 2000), was the only region in which acetaldehyde alone was observed to alter gene expression. Thus, acetaldehyde may induce some central effects by actions on brain areas, which are unprotected by the BBB and are directly accessible to the peripheral circulation. In contrast to the PVTh, nicotine activated c-fos expression in the PVN of juveniles but not adults. Although we previously reported nicotine activation of adolescent PVN (Park et al, 2006), this was in older animals by a different route of drug administration. As discussed below, differential drug activation of the PVN and PVTh may underlie observed age differences in corticosterone secretion.
HPA axis
There is substantial evidence of reciprocal interactions between nicotine and the HPA system (Caggiula et al, 1998; Matta et al, 1998). Nicotine stimulates HPA activity, and the resulting corticosteroid secretion strongly influences nicotine's physiological and behavioral effects. We have shown that intravenously administered nicotine induces increased plasma corticosterone secretion only in adults. This finding is not dependent on ambient stress levels, as the same age difference was observed in minimally stressed animals in which basal corticosterone levels were reduced. Although we have studied only one time point following drug administration in this experiment, we have recently shown nicotine to have no effects on adolescent corticosterone secretion at time intervals from 15 to 60 min after drug injection (Cao et al, in preparation). This decreased HPA response to nicotine in juveniles is unlikely due to a ceiling effect, as nicotine at very high doses increases ACTH release to a similar degree in juveniles and adults (Matta et al, 1987). Furthermore, corticosterone release in response to other stressors reaches adult levels by adolescence (Goldman et al, 1973; Vazquez and Akil, 1993; Choi and Kellogg, 1996).
In parallel to corticosterone secretion, nicotine significantly induced c-fos mRNA expression in adult PVN, but not in juveniles, which indicates that age differences in HPA response to nicotine likely have a central mechanism. Nicotine stimulates the HPA axis in adults by activating brainstem noradrenergic/adrenergic cell bodies with resulting release of norepinephrine within the PVN (Matta et al, 1987, 1990, 1998). The continuing development of this neuronal circuitry in adolescence may be involved in the observed age differences in HPA response to nicotine. This is consistent with the suggestion that the adrenergic projections to the PVN continue to mature in adolescence (Choi and Kellogg, 1996). Alternatively, age differences in nicotine induced c-fos mRNA expression in the PVTh may also contribute to HPA response to nicotine. As PVTh has inhibitory effects on HPA activity (Herman et al, 2003; Jaferi and Bhatnagar, 2006), nicotine activation of this brain area in juveniles may result in decreased HPA response to nicotine at this age.
Acetaldehyde potentiated nicotine activation of PVN c-fos expression and corticosterone secretion in adults, but not in juveniles. Furthermore, this effect of acetaldehyde on HPA activity was only observed in the behaviorally tested animals. As nicotine-induced corticosterone secretion was lower in behaviorally tested animals than in those that were minimally stressed, our findings tend to support those of a recent study, which reported that HPA response to nicotine is decreased by previous stress (Gadek-Michalska and Bugajski, 2005). Our data also suggest that acetaldehyde may reverse this habituation of the HPA axis to stress. PVTh, the only brain area showing acetaldehyde-induced c-fos mRNA expression in the present study, plays an important role in the habituation of the HPA axis to stress (Bhatnagar et al, 2002; Jaferi and Bhatnagar, 2006). Although acetaldehyde-induced c-fos mRNA expression in the PVTh was only observed in juveniles, the present study did show this nucleus to be a target of acetaldehyde. Given that c-fos has limitations as a marker of neuronal activation (Hoffman and Lyon, 2002), future studies may make use of other markers to evaluate acetaldehyde's effects on this brain area.
Conclusions
In conclusion, we have shown that juveniles have unique behavioral and endocrine responses to acute administration of nicotine as compared with adults. Acetaldehyde influences many but not all of these responses to nicotine. Interactions of nicotine and acetaldehyde were observed not only in juveniles, but also in adults. Although age differences exist in the rate of nicotine penetration into the brain, this was not influenced by acetaldehyde. Rather, the effects of acetaldehyde are complex and are dependent on the environment. These findings add to a growing literature that emphasizes the critical role of environmental factors in influencing the actions of nicotine and other psychostimulant drugs (Caggiula et al, 1998; Badiani and Robinson, 2004; Park et al, in press). Although the mechanisms underlying the interaction of nicotine and acetaldehyde are still not clearly understood, our data suggest that acetaldehyde may influence habituation to stress, possibly via effects on the PVTh, which is not protected by the BBB. As we have studied only initial response to drug, further studies will be required to evaluate interactions between these tobacco constituents after chronic exposure.
These findings have indicated that adolescence is a unique period in response to psychostimulants. This study also demonstrates that other constituents in tobacco and tobacco smoke may also contribute to the effects of nicotine and may, consequently, affect smoking behaviors. It is more meaningful to study not only ‘nicotine addiction’ but also ‘tobacco addiction’ by including other tobacco components. Clarification of the roles of tobacco components other than nicotine should aid in developing more effective smoking cessation therapies.
References
Adriani W, Macri S, Pacifici R, Laviola G (2002). Peculiar vulnerability to nicotine oral self-administration in mice during early adolescence. Neuropsychopharmacology 27: 212–224.
Badiani A, Robinson TE (2004). Drug-induced neurobehavioral plasticity: the role of environmental context. Behav Pharmacol 15: 327–339.
Belluzzi JD, Lee AG, Oliff HS, Leslie FM (2004). Age-dependent effects of nicotine on locomotor activity and conditioned place preference in rats. Psychopharmacology (Berlin) 174: 389–395.
Belluzzi JD, Wang R, Leslie FM (2005). Acetaldehyde enhances acquisition of nicotine self-administration in adolescent rats. Neuropsychopharmacology 30: 705–712.
Benowitz NL, Porchet H, Jacob III P (1990). Pharmacokinetics, metabolism, and pharmacodynamics of nicotine. In: Wonnacott SRM, Stolerman IP (eds). Nicotine Pharmacology: Molecular, Celllular, and Behavioral Aspects. Oxford University Press: Oxford. pp 112–151.
Bhatnagar S, Huber R, Nowak N, Trotter P (2002). Lesions of the posterior paraventricular thalamus block habituation of hypothalamic-pituitary-adrenal responses to repeated restraint. J Neuroendocrinol 14: 403–410.
Brandao ML, Anseloni VZ, Pandossio JE, De Araujo JE, Castilho VM (1999). Neurochemical mechanisms of the defensive behavior in the dorsal midbrain. Neurosci Biobehav Rev 23: 863–875.
Breslau N, Peterson EL (1996). Smoking cessation in young adults: age at initiation of cigarette smoking and other suspected influences. Am J Public Health 86: 214–220.
Broide RS, O’Connor LT, Smith MA, Smith JA, Leslie FM (1995). Developmental expression of alpha 7 neuronal nicotinic receptor messenger RNA in rat sensory cortex and thalamus. Neuroscience 67: 83–94.
Caggiula AR, Donny EC, Epstein LH, Sved AF, Knopf S, Rose C et al (1998). The role of corticosteroids in nicotine's physiological and behavioral effects. Psychoneuroendocrinology 23: 143–159.
Cao J. Age and sex differences in behavioral and endocrine responses to nicotine (in preparation).
Centers for Disease Control and Prevention (CDC) (2003). Tobacco use among middle and high school students—United States, 2002. MMWR Morb Mortal Wkly Rep 52: 1096–1098.
Chen H, Matta SG, Sharp BM (2006). Acquisition of nicotine self-administration in adolescent rats given prolonged access to the drug. Neuropsychopharmacology, print copy in press (originally published online June 14, 2006, at http://www.nature.com/npp/journal/vaop/ncurrent/abs/1301135a.html).
Chen J, Millar WJ (1998). Age of smoking initiation: implications for quitting. Health Rep 9: 39–46 (English); 39–48 (French).
Choi S, Kellogg CK (1996). Adolescent development influences functional responsiveness of noradrenergic projections to the hypothalamus in male rats. Brain Res Dev Brain Res 94: 144–151.
Critchlow V, Liebelt RA, Bar-Sela M, Mountcastle W, Lipscomb HS (1963). Sex difference in resting pituitary-adrenal function in the rat. Am J Physiol 205: 807–815.
Gadek-Michalska A, Bugajski J (2005). Nitric oxide mediates the interleukin-1beta- and nicotine-induced hypothalamic-pituitary-adrenocortical response during social stress. J Physiol Pharmacol 56: 491–503.
Goldman L, Winget C, Hollingshead GW, Levine S (1973). Postweaning development of negative feedback in the pituitary-adrenal system of the rat. Neuroendocrinology 12: 199–211.
Hatchell PC, Collins AC (1980). The influence of genotype and sex on behavioral sensitivity to nicotine in mice. Psychopharmacology (Berlin) 71: 45–49.
Herman JP, Figueiredo H, Mueller NK, Ulrich-Lai Y, Ostrander MM, Choi DC et al (2003). Central mechanisms of stress integration: hierarchical circuitry controlling hypothalamo-pituitary-adrenocortical responsiveness. Front Neuroendocrinol 24: 151–180.
Hoffman GE, Lyon D (2002). Anatomical markers of activity in neuroendocrine systems: are we all ‘fos-ed out’? J Neuroendocrinol 14: 259–268.
Hoffmann D, Hoffmann I (2001). The changing cigarette: chemical studies and bioassays. In: Shopland DR (ed). Risks Associated with Smoking Cigarettes with Low Machine-Measured Yields of Tar and Nicotine. National Cancer Institute Smoking and Tobacco Control Monograph 13: Washington, DC.
Jacob III P, Wilson M, Benowitz NL (1981). Improved gas chromatographic method for the determination of nicotine and cotinine in biologic fluids. J Chromatogr 222: 61–70.
Jaferi A, Bhatnagar S (2006). Corticosterone can act at the posterior paraventricular thalamus to inhibit hypothalamic-pituitary-adrenal activity in animals that habituate to repeated stress. Endocrinology 147: 4917–4930.
Kandel DB, Chen K (2000). Extent of smoking and nicotine dependence in the United States: 1991–1993. Nicotine Tob Res 2: 263–274.
Kandel DB, Logan JA (1984). Patterns of drug use from adolescence to young adulthood: I. Periods of risk for initiation, continued use, and discontinuation. Am J Public Health 74: 660–666.
Leslie FM, Loughlin SE, Wang R, Perez L, Lotfipour S, Belluzzi JD (2004). Adolescent development of forebrain stimulant responsiveness: insights from animal studies. Ann NY Acad Sci 1021: 148–159.
Levin ED, Rezvani AH, Montoya D, Rose JE, Swartzwelder HS (2003). Adolescent-onset nicotine self-administration modeled in female rats. Psychopharmacology (Berlin) 169: 141–149.
Manzardo AM, Stein L, Belluzzi JD (2002). Rats prefer cocaine over nicotine in a two-lever self-administration choice test. Brain Res 924: 10–19.
Matta SG, Beyer HS, McAllen KM, Sharp BM (1987). Nicotine elevates rat plasma ACTH by a central mechanism. J Pharmacol Exp Ther 243: 217–226.
Matta SG, Fu Y, Valentine JD, Sharp BM (1998). Response of the hypothalamo-pituitary-adrenal axis to nicotine. Psychoneuroendocrinology 23: 103–113.
Matta SG, McAllen KM, Sharp BM (1990). Role of the fourth cerebroventricle in mediating rat plasma ACTH responses to intravenous nicotine. J Pharmacol Exp Ther 252: 623–630.
Moolchan ET, Robinson ML, Ernst M, Cadet JL, Pickworth WB, Heishman SJ et al (2005). Safety and efficacy of the nicotine patch and gum for the treatment of adolescent tobacco addiction. Pediatrics 115: e407–e414.
O’Dell LE, Bruijnzeel AW, Smith RT, Parsons LH, Merves ML, Goldberger BA et al (2006). Diminished nicotine withdrawal in adolescent rats: implications for vulnerability to addiction. Psychopharmacology (Berlin) 186: 612–619.
O’Neill MF, Dourish CT, Iversen SD (1991). Evidence for an involvement of D1 and D2 dopamine receptors in mediating nicotine-induced hyperactivity in rats. Psychopharmacology (Berlin) 104: 343–350.
Park MK, Belluzzi JD, Han SH, Cao J, Leslie FM. Age, sex and early environment contribute to individual differences in nicotine/acetaldehyde-induced behavioral and endocrine responses in rats. Pharmacol Biochem Behav (in press).
Park MK, Loughlin SE, Leslie FM (2006). Gestational nicotine-induced changes in adolescent neuronal activity. Brain Res 1094: 119–126.
Paxinos G, Watson C (1986). The Rat Brain in Stereotaxic Coordinates, 2nd edn. Academic Press Inc.: San Diego.
Pentel PR, Malin DH, Ennifar S, Hieda Y, Keyler DE, Lake JR et al (2000). A nicotine conjugate vaccine reduces nicotine distribution to brain and attenuates its behavioral and cardiovascular effects in rats. Pharmacol Biochem Behav 65: 191–198.
Picciotto MR, Brunzell DH, Caldarone BJ (2002). Effect of nicotine and nicotinic receptors on anxiety and depression. Neuroreport 13: 1097–1106.
Prut L, Belzung C (2003). The open field as a paradigm to measure the effects of drugs on anxiety-like behaviors: a review. Eur J Pharmacol 463: 3–33.
Quertemont E, Tambour S, Tirelli E (2005). The role of acetaldehyde in the neurobehavioral effects of ethanol: a comprehensive review of animal studies. Prog Neurobiol 75: 247–274.
Samaha AN, Yau WY, Yang P, Robinson TE (2005). Rapid delivery of nicotine promotes behavioral sensitization and alters its neurobiological impact. Biol Psychiatry 57: 351–360.
Schochet TL, Kelley AE, Landry CF (2005). Differential expression of arc mRNA and other plasticity-related genes induced by nicotine in adolescent rat forebrain. Neuroscience 135: 285–297.
Shram MJ, Funk D, Li Z, Le AD (2006). Periadolescent and adult rats respond differently in tests measuring the rewarding and aversive effects of nicotine. Psychopharmacology (Berlin) 186: 201–208.
Spear LP (2000). The adolescent brain and age-related behavioral manifestations. Neurosci Biobehav Rev 24: 417–463.
Swanson LW (2000). Cerebral hemisphere regulation of motivated behavior. Brain Res 886: 113–164.
Tabakoff B, Anderson RA, Ritzmann RF (1976). Brain acetaldehyde after ethanol administration. Biochem Pharmacol 25: 1305–1309.
Ueno M, Akiguchi I, Hosokawa M, Kotani H, Kanenishi K, Sakamoto H (2000). Blood–brain barrier permeability in the periventricular areas of the normal mouse brain. Acta Neuropathol (Berlin) 99: 385–392.
US Department of Health and Human Services (1994). Preventing tobacco use among young people: a report of the Surgeon General.
US Surgeon General's Report (1989). Reducing the Health Consequences of Smoking. pp 79–92.
Vastola BJ, Douglas LA, Varlinskaya EI, Spear LP (2002). Nicotine-induced conditioned place preference in adolescent and adult rats. Physiol Behav 77: 107–114.
Vazquez DM, Akil H (1993). Pituitary-adrenal response to ether vapor in the weanling animal: characterization of the inhibitory effect of glucocorticoids on adrenocorticotropin secretion. Pediatr Res 34: 646–653.
Villegier AS, Salomon L, Granon S, Changeux JP, Belluzzi JD, Leslie FM et al (2006). Monoamine oxidase inhibitors allow locomotor and rewarding responses to nicotine. Neuropsychopharmacology 31: 1704–1713.
Wilmouth CE, Spear LP (2004). Adolescent and adult rats’ aversion to flavors previously paired with nicotine. Ann NY Acad Sci 1021: 462–464.
Winzer-Serhan UH, Broide RS, Chen Y, Leslie FM (1999). Highly sensitive radioactive in situ hybridization using full length hydrolyzed riboprobes to detect alpha 2 adrenoceptor subtype mRNAs in adult and developing rat brain. Brain Res Brain Res Protoc 3: 229–241.
Zimatkin SM (1991). Histochemical study of aldehyde dehydrogenase in the rat CNS. J Neurochem 56: 1–11.
Acknowledgements
We thank Yiling Chen, MD, and Ruihua Wang, MD for their assistance. This study is supported by DA 19138 and DA 21267.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cao, J., Belluzzi, J., Loughlin, S. et al. Acetaldehyde, a Major Constituent of Tobacco Smoke, Enhances Behavioral, Endocrine, and Neuronal Responses to Nicotine in Adolescent and Adult Rats. Neuropsychopharmacol 32, 2025–2035 (2007). https://doi.org/10.1038/sj.npp.1301327
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.npp.1301327