Abstract
Several lines of evidence have indicated that the prevalence of depression in diabetic subjects is higher than that in the general population, however, little information is available on the effects of antidepressants in diabetes. In the present study, the antidepressant-like effect mediated by the activation of 5-HT1A receptors was examined using the tail suspension test in streptozotocin-induced diabetic mice. Long-lasting increases in 5-HT turnover rates were observed in the diabetic mouse midbrain and frontal cortex, but not in the hippocampus. Duration of immobility was significantly longer in diabetic than in nondiabetic mice in the tail suspension test. The 5-HT1A receptor agonist (±)-8-hydroxy-2-(di-n-propylamino) tetralin (8-OH-DPAT) (3–30 μg/kg, i.p.) reduced the duration of immobility in nondiabetic mice, and this effect was completely antagonized by pretreatment with N-[2-[4-(2-methoxyphenil)-1-piperazinyl]ethyl]-N-2-pyridinylcyclohexanecarboxamide (WAY-100635) (30 μg/kg, s.c.), a selective 5-HT1A receptor antagonist. In contrast, 8-OH-DPAT (3 μg/kg–3 mg/kg, i.p.) was ineffective in diabetic mice. The selective 5-HT reuptake inhibitor fluoxetine (3–56 mg/kg, i.p.) reduced the duration of immobility in both nondiabetic and diabetic mice. However, fluoxetine was less effective in diabetic mice than in nondiabetic mice. WAY-100635 (30 μg/kg, s.c.) reversed the suppression of the duration of immobility by fluoxetine (30 mg/kg, i.p.) in nondiabetic mice. On the other hand, the anti-immobility effect of fluoxetine (56 mg/kg, i.p.) was not antagonized by WAY-100635 (30 μg/kg, s.c.) in diabetic mice. The selective 5-HT2 receptor antagonist 6-methyl-1-(1-methylethyl)-ergoline-8β-carboxylic acid 2-hydroxy-1-methylpropyl ester (LY53,857) (30 μg/kg, s.c.) reversed the anti-immobility effect of fluoxetine in both nondiabetic and diabetic mice. Spontaneous locomotor activity in diabetic mice was not different from that in nondiabetic mice. 8-OH-DPAT (30 μg/kg, i.p.), but not fluoxetine, increased the spontaneous locomotor activity in both nondiabetic and diabetic mice. The number of 5-HT1A receptors in the mouse frontal cortex was unaffected by diabetes. Plasma corticosterone levels in diabetic mice were significantly higher than that in nondiabetic mice. These results suggest that the antidepressant-like effect mediated by 5-HT1A receptors may be attenuated by diabetes.
Similar content being viewed by others
INTRODUCTION
The pathogenesis of depression is closely related to the monoaminergic system, and particularly involves serotonergic mechanisms (Maes and Meltzer, 1995). Selective inhibitors of serotonin (5-HT) uptake, such as fluoxetine and sertraline, have been shown to be as effective in the treatment of depression as established antidepressant drugs in double-blind clinical trials (Chouinard, 1985; Feighner and Cohn, 1985; Reimherr et al, 1988). In addition, buspirone and gepirone, 5-HT1A receptor agonists, have therapeutic value as antidepressant drugs (Goldberg and Finnerty, 1979; Schweizer et al, 1986; Amsterdam et al, 1987).
Several animal models, such as forced swimming test and learned helplessness test, have been developed to evaluate putative antidepressants (Porsolt et al, 1978; Willner, 1990). Among these, the tail suspension test proposed by Steru et al (1985), (1987) is a convenient model in which many antidepressants reduce duration of immobility, indicating that this is an index of antidepressant activity (Teste et al, 1993). Selective 5-HT reuptake inhibitors (SSRIs) and 5-HT1A receptor agonists show antidepressant-like effects in these models (Wieland and Lucki, 1990; Teste et al, 1993).
It has been reported that changes in the 5-HT systems occur in some areas of diabetic human and animal brain. In the post-mortem study, 5-HT concentration was increased in the hypothalamus of diabetic subjects (Lackovic et al, 1990). In addition, a recent positron emission tomography (PET) study, significantly greater 5-HT1A receptor binding was detected in mesial temporal cortex in type 2 diabetic subjects (Price et al, 2002). Streptozotocin-induced hyperglycemic state has been used as an animal model for diabetes mellitus (Tarui et al, 1987; McCall, 1992). Streptozotocin selectively destroys pancreatic islet beta-cells and causes hypoinsulinemia, leading to hyperglycemia (Arison et al, 1967; Hohenegger and Rudas, 1971). Streptozotocin itself does not enter the brain (Bhuyan et al, 1974). It has been reported that streptozotocin-induced diabetic rats showed changed concentration of 5-HT and its major metabolite 5-hydroxyindoleacetic acid (5-HIAA) in the brain (Bitar et al, 1985; Lackovic et al, 1990; Bellush et al, 1991; Ohtani et al, 1997; Sandrini et al, 1997). In addition, receptor binding studies suggested that streptozotocin-induced diabetes increased or unaffected the 5-HT1A receptor number in rat brain (Sandrini et al, 1997; Sumiyoshi et al, 1997). These changes may contribute greater vulnerability to psychiatric disorders, such as depression, in the diabetic patients. In fact, it is well established that the prevalence of depression in diabetic patients is higher than that in the general population, and this higher prevalence is unrelated to the type of diabetes (insulin-dependent or noninsulin-dependent diabetes mellitus) (Anderson et al, 2001). Several antidepressants, such as SSRIs and tricyclic antidepressants, were effective in the treatment of depression in diabetic patients (Lustman et al, 1997, 2000b). However, tricyclic antidepressants, but not SSRIs, produced to worsen glycemic control whereas depression improvement (Lustman et al, 1997). Therefore, SSRIs were useful agents to reduce the severity of depression in diabetic patients. We previously reported that the efficacy of some antidepressants, such as fluoxetine, fluvoxamine, and desipramine, were decreased by diabetes in the mouse tail suspension test (Kamei et al, 2003). In addition, it has also been reported that 5-HT1A receptor agonist-induced head-weaving behavior was attenuated by diabetes in mice (Fujii et al, 1991). These reports led us to speculate that the efficacy of antidepressants might be attenuated by diabetes.
In the present study, we examined the effects of the 5-HT1A receptor agonist (±)-8-hydroxy-2-(di-n-propylamino) tetralin (8-OH-DPAT) and fluoxetine on the duration of immobility in the tail suspension test in diabetic mice.
MATERIALS AND METHODS
Animals
Male ICR mice (Tokyo Laboratory Animals Science Co., Ltd, Tokyo), 4 weeks of age and weighing approximately 20 g at the beginning of the experiments, were used. They were housed 10 per cage and had free access to food and water. The animal room was maintained at 24±1°C and 55±5% humidity with a 12-h light–dark cycle (light on at 0800, light off at 2000). Animals were rendered diabetic by an injection of streptozotocin (200 mg/kg, i.v.) dissolved in 0.1 N citrate buffer at pH 4.5. Age-matched control mice were injected with the vehicle alone. Blood glucose levels were determined using a glucose analyzer (ANTSENSE II, Sankyo Co., Ltd, Tokyo, Japan). In the behavioral test, 6-week-old mice (ie 14 days after the induction of diabetes) with hyperglycemia (blood glucose levels >400 mg/dl) were defined as diabetic. All behavioral observations were performed between 1100 and 1500 each day. The animals were used only once. This study was carried out in accordance with the Guide for the Care and Use of Laboratory Animals as adopted by the Committee on the Care and Use of Laboratory Animals of Hoshi University, which is accredited by the Ministry of Education, Science, Sports, and Culture.
Pilot Study
The temporal effects of diabetes on body weight, blood glucose levels, and 5-HT turnover rates were determined. Body weight and blood glucose level were measured 0, 2, 4, 7, 14, 28, and 56 days after the injection of streptozotocin (diabetic group) or vehicle (nondiabetic group). Diabetic and nondiabetic mice at 7, 14, 28, and 56 days after induction were killed by decapitation and the brain, which was used to determine 5-HT turnover rates, was quickly removed.
5-HT Concentration
The concentration of 5-HT and 5-HIAA were determined by high-performance liquid chromatography (HPLC). The brain was dissected into the midbrain, frontal cortex, and hippocampus on an ice-cold glass plate. Dissected brain tissues were stored at −80°C until homogenized. The tissues were homogenized in solution containing 300 μl of 0.2 M perchloric acid with 100 μM EDTA (2Na) and 100 μl of 1 mg/l isoproterenol as an internal standard (total volume of 400 μl). To remove the proteins completely, the homogenates were placed in ice-cold water for 30 min. The homogenates were then centrifuged at 20 000 g for 15 min at 0–4°C, and the supernatants were removed to other tubes. Then, the solution was maintained at pH 3.0 using 1 M sodium acetate, and stored at −80°C until assayed. Solution samples of 20 μl were analyzed by HPLC (EP-300, Eicom, Co., Kyoto, Japan) with electrochemical detection. The electrochemical detector (EC-300, Eicom Co.) included a graphite electrode (WE-3G, Eicom Co.), which was used at a voltage setting of 0.7 V vs a Ag/AgCl reference electrode. The mobile phase consisted of sodium acetate (0.1 M)/citric acid (0.1 M) buffer, pH 3.5, containing 15% (v/v) methanol, sodium 1-octanesulfonate, and EDTA (2Na). The flow rate was set to 0.5 ml/min with a column temperature of 25°C. 5-HT turnover rates were calculated as 5-HIAA/5-HT ratio.
Drugs
The drugs used in this study were streptozotocin (Sigma Chemical Co., St Louis, MO), (±)-8-hydroxy-2-(di-n-propylamino)tetralin hydrbromide (8-OH-DPAT) (Sigma Chemical Co.), N-[2-[4-(2-methoxyphenil)-1-piperazinyl]ethyl]-N-2-pyridinylcyclohexanecarboxamide (WAY-100635) (Sigma Chemical Co.), 6-methyl-1-(1-methylethyl)-ergoline-8β-carboxylic acid 2-hydroxy-1-methylpropyl ester (LY53,857) (Sigma Chemical Co.), and fluoxetine hydrochloride (Tocris Cookson, Ltd, UK). 8-OH-DPAT, WAY-100635, and LY53,857 were dissolved in saline and administered in a volume of 0.1 ml/10 g of body weight. Fluoxetine was dissolved in saline and administered in a volume of 0.19 ml/10 g of body weight because the solubility of fluoxetine in saline was limited to 10 mM (about 35 mg/kg at a volume of 0.1 ml/10 g).
Tail Suspension Test
The tail suspension apparatus consisted of a white translucent plastic box (30 × 30 × 30 cm) with a hook in the middle of the ceiling from which to suspend the mouse. Mice were suspended by the tail using adhesive Scotch tape affixed to the hook, which was connected to a strain gauge (TAIL SUSPENSION AMP, Neuroscience Inc., Tokyo, Japan) that picked up all movements of the mouse and transmitted them to a central processing unit that calculated the total duration of immobility and the strength of movements during the 10 min of the test. Each mouse was suspended individually. The movements of the mice were measured for 10 min and digitized and processed by Super Scope II (GWI; Somerville, MA, USA). The threshold level was set so as to exclude respiration movement. The duration of immobility was defined as the total amount of time that the animal showed no movement. 8-OH-DPAT and fluoxetine were injected i.p. 30 min before the measurement of duration of immobility. WAY-100635 and LY53,857 were injected s.c. 30 min before treatment with 8-OH-DPAT and fluoxetine.
Locomotor Activity
Spontaneous locomotor activity of mice was measured by a digital counter with an infrared sensor (NS-AS01, Neuroscience Inc., Tokyo, Japan). A mouse was placed in a transparent plastic cage (27 × 17 × 13 cm), a transparent plastic ceiling was installed, and an infrared sensor was placed at the center of the ceiling. Mice were placed in the measurement cage for a habituation period of 60 min, and then each drug was injected. Total activity counts were automatically recorded for 10 min. 8-OH-DPAT and fluoxetine were injected i.p. 30 min before the measurement of locomotor activity.
Measurement of [3H]WAY-100635 Binding
Diabetic and nondiabetic mice 14 days after the injection of streptozotocin or the vehicle were killed by decapitation. The brain was dissected into the frontal cortex on an ice-cold glass plate. Dissected brain tissues were stored at −80°C until homogenized. The 5-HT1A receptor binding was assayed as described by Khawaja et al (1995) with a minor modification. In brief, the frontal cortex was homogenized in 50 volumes (w/v) of 50 mM Tris-HCl buffer (pH 7.4) using a Polytron homogenizer (setting of 5, 30 s; Kinematica, Lucerne, Switzerland). The homogenates were centrifuged twice at 27 000 g for 20 min at 4°C. The membrane pellets were resuspended in Tris-HCl buffer and incubated at 37°C for 20 min, before a final centrifugation step (27 000 g × 20 min at 4°C). The final pellets were stored at −80°C until assayed. The membrane preparation (150 μg of protein per tube) was suspended in the same buffer and incubated with 0.1−5 nM [3H]WAY-100635 (77.0 Ci/mmol; Amersham, Buckinghamshire, UK) in the absence (for measuring total binding) or the presence (for measuring nonspecific binding) of unlabeled 1 μM 5-HT (Sigma Chemical Co.). The reaction mixture (total volume, 500 μl) was incubated at 37°C for 60 min. Following incubation, membrane-bound radioligand was separated from free radioligand by rapid vacuum filtration over presoaked (0.5% polyethylenimine) Whatman GF/B glass microfiber filter (Whatman, Maidstone, UK) and washed through with three 5 ml volumes of ice-cold 50 mM Tris-HCl (pH 7.4). Filter-bound radioactivity was transferred to scintillation vials containing 4 ml of Aquasol-2 scintillation cocktail and counted by liquid scintillation counter. Specific binding was calculated as the difference between total and nonspecific binding. Protein content was determined by the Bio-Rad method (Bio-Rad Laboratories Ltd, Hemel Hempstead, Hertfordshire, UK) using bovine γ-globulin as the standard. Assays of [3H]WAY-100635 binding were performed in duplicate.
Plasma Corticosterone Determination
Mice were killed by decapitation, and then trunk blood was collected in heparinized tubes. Blood was centrifuged at 10 000 g for 15 min, and plasma was removed and stored at −80°C until analysis. Blood was collected between 1100 and 1115. Plasma corticosterone concentrations were determined using commercially available EIA kit (DSL, Inc., USA) following the manufacturer's directions.
Statistics
The data were expressed as means with SEM. Significant differences were determined by two-way analysis of variance (ANOVA) for factorial comparisons and the Bonferroni test for multiple comparisons. Student's t-test or Aspin–Welch's t-test was used to evaluate differences between two groups. P-values less than 0.05 were considered significant.
RESULTS
Effects of Diabetes on Body Weight Gain and Blood Glucose Levels in Mice
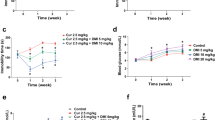
Body weight gain and blood glucose levels in both diabetic and nondiabetic mice are shown in Figure 1. The mean body weights on the first day in nondiabetic and diabetic group were 19.6±0.16 and 19.2±0.15, respectively (not significant). Two-way ANOVA revealed that diabetes significantly reduced body weight (F(1, 108)=294.237, P<0.0001) and increased blood glucose levels (F(1, 126)=1904.11, P<0.0001).
Effects of Diabetes on 5-HT Turnover Rates in Mice
In the midbrain, 5-HT turnover rates (5-HIAA/5-HT ratio) were significantly increased at 14, 28, and 56 days after the induction of diabetes (Table 1A). In addition, 5-HIAA concentration was significantly increased at 14 and 28 days after the induction of diabetes (Table 1A). 5-HT concentration was not significant deference between nondiabetic and diabetic mouse midbrain (Table 1A). In the frontal cortex, the diabetic mice showed significant increases in 5-HT turnover rates at 14, 28, and 56 days after injection and significant decreases in 5-HT turnover rates at 7 days after injection (Table 1B). 5-HIAA concentration in the frontal cortex was significantly increased at 14, 28, and 56 days after the induction of diabetes (Table 1B). Furthermore, 5-HT concentration was significantly increased at 28 days after the induction of diabetes in mouse frontal cortex (Table 1B). In the hippocampus, 5-HT turnover rates were markedly increased 14 days after the induction of diabetes (Table 1C). 5-HIAA concentration in the hippocampus was significantly increased at 14 and 28 days after the induction of diabetes (Table 1C). In addition, 5-HT concentration was significantly increased at 7 days after the induction of diabetes in mouse hippocampus (Table 1C). It is well known that 5-HT neuronal activities are altered by diabetes (Bitar et al, 1985; Lackovic et al, 1990; Bellush et al, 1991; Ohtani et al, 1997; Sandrini et al, 1997). We previously proposed that 14 days after the injection of streptozotocin (200 mg/kg, i.v.), mice exhibited diabetic neuropathy (Kamei et al, 1991). Therefore, in the subsequent behavioral test, mice 14 days after the induction of diabetes, with hyperglycemia, were considered diabetic.
Effects of 8-OH-DPAT on the Duration of Immobility in the Tail Suspension Test in Nondiabetic and Diabetic Mice
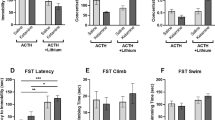
The duration of immobility in diabetic mice was longer than that in nondiabetic mice in the tail suspension test (Figure 2a). 8-OH-DPAT (3–30 μg/kg, i.p.), a 5-HT1A receptor agonist, significantly and dose-dependently reduced the duration of immobility in nondiabetic mice (Figure 2a). However, 8-OH-DPAT (3–30 μg/kg, i.p.) did not affect the duration of immobility in diabetic mice (Figure 2a). The 8-OH-DPAT (30 μg/kg, i.p.)-induced reduction in the duration of immobility in nondiabetic mice was completely antagonized by pretreatment with WAY-100635 (30 μg/kg, s.c.), a 5-HT1A receptor selective antagonist (Figure 2b). In diabetic mice, 8-OH-DPAT was also ineffective at high doses of 0.1–3 mg/kg (Figure 2c).
(a) Effects of 8-OH-DPAT (3–30 μg/kg, i.p.) on the duration of immobility in the tail suspension test in nondiabetic and diabetic mice. (b) Effect of WAY-100635 (30 μg/kg, s.c.) on 8-OH-DPAT-induced reduction in the duration of immobility in nondiabetic mice. (c) Effect of 8-OH-DPAT (0.1–3 mg/kg, i.p.) on the duration of immobility in diabetic mice. 8-OH-DPAT was injected i.p. 30 min before the test. WAY-100635 was injected s.c. 30 min before treatment with 8-OH-DPAT. Each column represents the mean±SEM of 8–10 mice. *P<0.05 statistically significant difference between saline-treated nondiabetic mice and saline-treated diabetic mice (Student's t-test). #P<0.05 vs respective saline-treated group (Bonferroni test). $P<0.05 vs 8-OH-DPAT alone-treated group (Bonferroni test).
Effects of Fluoxetine on the Duration of Immobility in Nondiabetic and Diabetic Mice
Fluoxetine (3–56 mg/kg, i.p.) dose-dependently and significantly decreased the duration of immobility in both nondiabetic and diabetic mice (Figure 3). The reduction in the duration of immobility in nondiabetic mice was statistically significant at doses of 30 and 56 mg/kg. However, the effect of fluoxetine in diabetic mice was less than that in nondiabetic mice, since the reduction in the duration of immobility in diabetic mice was significant at a dose of 56 mg/kg.
Effect of fluoxetine on the duration of immobility in nondiabetic and diabetic mice. Fluoxetine was injected i.p. 30 min before the test. Each square represents the mean±SEM of 8–10 mice. *P<0.05 statistically significant difference between saline-treated nondiabetic mice and saline-treated diabetic mice (Student's t-test). #P<0.05 vs respective saline-treated group (Bonferroni test).
Effects of WAY-100635 and LY53,857 on Fluoxetine-Induced Reduction in the Duration of Immobility in Nondiabetic and Diabetic Mice
In nondiabetic mice, the reduction in the duration of immobility by fluoxetine (30 mg/kg, i.p.) was significantly antagonized by pretreatment with WAY-100635 (30 μg/kg, s.c.) (Figure 4). In contrast, WAY-100635 (30 μg/kg, s.c.) did not antagonize the suppression of the duration of immobility by fluoxetine (56 mg/kg, i.p.) in diabetic mice (Figure 4). Pretreatment with LY53,857 (30 μg/kg, s.c.), a 5-HT2 receptor selective antagonist, significantly reversed the decrease in the duration of immobility by fluoxetine in both nondiabetic and diabetic mice (Figure 4). Duration of immobility was not significantly affected by WAY-100635 (30 μg/kg, s.c.) and LY53,857 (30 μg/kg, s.c.) given alone in both nondiabetic and diabetic mice (data not shown).
Effects of WAY-100635 and LY53,857 on the fluoxetine-induced reduction of the duration of immobility in nondiabetic and diabetic mice. Fluoxetine was injected i.p. 30 min before the test. WAY-100635 (WAY: 30 μg/kg, s.c.) and LY53,857 (LY: 30 μg/kg, s.c.) were injected 30 min before the injection of fluoxetine. Each column represents the mean±SEM of 8–10 mice. *P<0.05 statistically significant difference between saline-treated nondiabetic mice and saline-treated diabetic mice (Student's t-test). #P<0.05 vs respective saline-treated group (Bonferroni test). $P<0.05 vs respective fluoxetine-treated group (Bonferroni test).
Effects of Fluoxetine and 8-OH-DPAT on Spontaneous Locomotor Activity in Nondiabetic and Diabetic Mice
It is possible that drugs increasing locomotor activity reduce the duration of immobility in tail suspension test. Therefore, we determined the effects of fluoxetine and 8-OH-DPAT on spontaneous locomotor activity in nondiabetic and diabetic mice. Fluoxetine, at a dose that was effective in the tail suspension test, produced a slight but not significant reduction in spontaneous locomotor activity for 10 min in nondiabetic and diabetic mice (Figure 5). On the other hand, 8-OH-DPAT (30 μg/kg, i.p.) significantly increased spontaneous locomotor activity in both nondiabetic and diabetic mice (Figure 5).
Effects of fluoxetine and 8-OH-DPAT on spontaneous locomotor activity in nondiabetic and diabetic mice. Locomotor activity was measured for 10 min. Fluoxetine and 8-OH-DPAT were injected i.p. 30 min before the test. Each column represents the mean±SEM of 8–10 mice. *P<0.05 vs respective saline-treated group (Bonferroni test).
Effect of Diabetes on the Number of 5-HT1A Receptors in the Mouse Frontal Cortex
The Bmax of [3H]WAY-100635 binding in the frontal cortex was not affected by diabetes in mice (Table 2). In addition, there was no significant difference in the Kd value of [3H]WAY-100635 binding in the frontal cortex between nondiabetic and diabetic mice (Table 2).
Effects of Diabetes on Plasma Corticosterone Levels in Mice
Plasma corticosterone levels were significantly greater in diabetic mice than in nondiabetic mice (Table 3).
Temporal Effect of Diabetes on Duration of Immobility in the Tail Suspension Test in Mice
Duration of immobility in the tail suspension test in mice 28 and 56 days after the treatment with streptozotocin (200 mg/kg, i.v.) was shown in Figure 6. Duration of immobility was significantly longer in both streptozotocin-treated groups than in respective vehicle-treated groups.
DISCUSSION
It has been recognized that patients with either type 1 or type 2 diabetes have a higher prevalence of major depression and depressive symptoms than the general population (Anderson et al, 2001). Psychological troubles, including depression, are likely to adversely affect glycemic control, and may be regarded as risk factors for the development of diabetes-related complications (Lustman et al, 2000a; de Groot et al, 2001).
It is well known that 5-HT systems in brain play a major role in the pathogenesis and treatment of depression (Maes and Meltzer, 1995). The dorsal and median raphe nuclei (DRN and MRN, respectively) of the midbrain are the main source of serotonergic innervation. The frontal cortex mainly receives a 5-HT projection from the DRN, and the hippocampus predominantly receives MRN innervation (McQuade and Sharp, 1997). Therefore, we examined the effect of diabetes on serotonergic neuronal activity, and its regional distribution. In the present study, 5-HT turnover rates were altered by diabetes in mouse brain, depending on the duration of the diabetic condition. In particular, long-term increases in 5-HT turnover rates were observed in the diabetic mouse midbrain and frontal cortex, but not in the hippocampus. Therefore, it is possible that the activity of 5-HT neurons may be affected by diabetes, region-specifically, and projection areas from the DRN may be vulnerable by diabetes. In contrast to the present observations, 5-HT turnover rates have been reported to be decreased in diabetic rat brain (Bitar et al, 1985; Bellush et al, 1991). This discrepancy may be due to the differences between species and the duration of the diabetic condition. Further studies are required to elucidate the moderating and causal factors related to the effect of diabetes on 5-HT systems. In the present behavioral study, diabetic mice showed a prolonged duration of immobility in the tail suspension test. Similarly, the duration of immobility in diabetic mice has also been reported to be greater than that in nondiabetic mice in the forced swimming test (Hilakivi-Clarke et al, 1990) and the tail-suspension test (Kamei et al, 2003). In addition, diabetic mice at 28 and 56 days after the induction of diabetes also showed prolonged duration of immobility in the tail suspension test in the present results. Thus, the long-lasting behavioral changes in diabetic mice are likely to be related to, at least in part, the changes in 5-HT systems, such as 5-HT neuronal activities and 5-HT receptor responses, caused by diabetes.
5-HT1A receptor agonists, such as buspirone and gepirone, have been shown to possess antidepressive properties in the clinical and animal studies (Goldberg and Finnerty, 1979; Schweizer et al, 1986; Amsterdam et al, 1987; Wieland and Lucki, 1990). Since head-weaving behavior induced by 5-HT1A receptor agonists was attenuated in diabetic mice (Fujii et al, 1991), we speculated that the effects of antidepressants mediated by 5-HT1A receptor would be altered in diabetes. In the present results, 8-OH-DPAT decreased the duration of immobility in nondiabetic mice in the tail suspension test. On the other hand, 8-OH-DPAT did not affect the duration of immobility in diabetic mice, despite the high doses used. However, spontaneous locomotor activity was increased by treatment with 8-OH-DPAT in both nondiabetic and diabetic mice. It has been reported that the activation of postsynaptic 5-HT1A receptor produced an antidepressant-like effect and hyperlocomotion (Tricklebank et al, 1985; Mayorga et al, 2001). These observations suggest that anti-immobility effect-mediated 5-HT1A receptor was specifically attenuated by diabetes in the tail suspension test. However, we cannot exclude another possibility because 8-OH-DPAT also has an agonistic property for 5-HT7 receptors, not only 5-HT1A receptors (Ruat et al, 1993). 5-HT7 receptors are widely distributed in thalamic, limbic, and cortical regions, which suggest a role for these receptors in affective behaviors (To et al, 1995; Gustafson et al, 1996). Further studies are needed to elucidate this problem.
Lustman et al (2000b) reported that fluoxetine improved symptoms of depression in diabetic patients. Our present data support this clinical observation because fluoxetine significantly suppressed the duration of immobility in both nondiabetic and diabetic mice. However, a higher dose of fluoxetine was required to reduce the duration of immobility in diabetic mice. Interestingly, WAY-100635 antagonized the effect of fluoxetine in nondiabetic, but not diabetic, mice. These results suggest that the antidepressive effects of serotonergic antidepressants, such as SSRIs and 5-HT1A receptor agonists, may be attenuated by diabetes as a result of the dysfunction of 5-HT1A receptors. In this study, LY53,857 reversed the anti-immobility effect of fluoxetine in both nondiabetic and diabetic mice. Since 5-HT2C receptor agonists possess antidepressant-like activity (Cryan and Lucki, 2000), our present data suggest that the antidepressant effect of SSRIs in diabetes may be due, at least in part, to the activation of 5-HT2C receptor.
Several possibilities should be considered regarding the hyposensitivity of 5-HT1A receptors in diabetic mice. First, the response of 5-HT1A receptors may be downregulated by increased 5-HT turnover in diabetic mice. However, present result and previous report suggest that the number of 5-HT1A receptors was unaffected by diabetes in the frontal cortex and hippocampus (Sumiyoshi et al, 1997). Thus, it is possible that 5-HT1A receptor-coupled G protein activities and intracellular signaling pathway may be disturbed in diabetes. Second, the changes in endocrine systems caused by diabetes may affect the function of 5-HT1A receptors. Type 1 and type 2 diabetes cause hyperactivation of the hypothalamic–pituitary–adrenal (HPA) axis in humans (Cameron et al, 1984; Roy et al, 1990, 1993) and animals (Scribner et al, 1991; Takao et al, 2000). In consistent with these previous reports, diabetic mice showed the increases in plasma corticosterone levels in our present result. Long-term corticosterone treatment induced dysfunction of 5-HT1A receptors to 8-OH-DPAT in behavioral and electrophysiological studies (Haleem, 1992; Czyrak et al, 2002). Therefore, it is possible that the dysfunction of 5-HT1A receptors may be due to the chronic high corticosterone levels in diabetic mice. Finally, the rate of penetration into the brain and the metabolic rate of fluoxetine and 8-OH-DPAT may be affected by diabetes. These possibilities suggest that the efficacy of antidepressants mediated by the activation of 5-HT1A receptor may be decreased by diabetes. Further studies are necessary before these issues can be resolved unequivocally.
It has been reported that SSRIs and tricyclic antidepressants improved depression in diabetic patients (Goodnick et al, 1997; Lustman et al, 1997, 2000b). However, tricyclic antidepressants produced to worsen glycemic control whereas depression improvement (Lustman et al, 1997). In contrast, fluoxetine improved both glycemic control and depressive state in diabetic patients (Lustman et al, 2000b). Therefore, SSRIs are useful agents to reduce the severity of depression in diabetic patients. We previously reported that the antidepressant-like effect of fluoxetine and fluvoxamine, SSRIs, and desipramine, a selective norepinephrine reuptake inhibitor, were less in diabetic than in nondiabetic mice in the tail suspension test (Kamei et al, 2003). In addition, the present results suggest that attenuated efficacy of fluoxetine in diabetic mice may be due to reduced response of 5-HT1A receptors, which have anti-immobility effect and therapeutic properties as antidepressant drugs (Goldberg and Finnerty, 1979; Schweizer et al, 1986; Amsterdam et al, 1987). Therefore, our present results suggest a possibility that efficacy of antidepressants mediated by 5-HT1A receptors may be attenuated in depressive patients with diabetes.
In conclusion, our present results suggest that antidepressant-like effects mediated by 5-HT1A receptor may be attenuated by diabetes.
References
Amsterdam JD, Berwish N, Potter L, Rickels K (1987). Open trial of gepirone in the treatment of major depressive disorder. Curr Ther Res 41: 185–193.
Anderson RJ, Freedland KE, Clouse RE, Lustman PJ (2001). The prevalence of comorbid depression in adults with diabetes. A meta-analysis. Diabetes Care 24: 1069–1078.
Arison RN, Ciaccio EI, Glitzer MS, Cassaro JA, Pruss MP (1967). Light and electron microscopy of lesions in rats rendered diabetic with streptozotocin. Diabetes 16: 51–56.
Bellush LL, Reid SG, North D (1991). The functional significance of biochemical alterations in streptozotocin-induced diabetes. Physiol Behav 50: 973–981.
Bhuyan BK, Kuentzel SL, Gray LG, Fraser TJ, Wallach D, Neil GL (1974). Tissue distribution of streptozotocin (NSC-85998). Cancer Chemother Rep 58: 157–165.
Bitar MS, Koulu M, Rapoport SI, Linnoila M (1985). Diabetes-induced alterations in brain monoamine metabolism in rats. J Pharmacol Exp Ther 236: 432–437.
Cameron OG, Kronfol Z, Greden JF, Carroll BJ (1984). Hypothalamic–pituitary–adrenocortical activity in patients with diabetes mellitus. Arch Gen Psychiatry 41: 1090–1095.
Chouinard G (1985). A double-blind controlled clinical trial of fluoxetine and amitriptyline in the treatment of outpatients with major depressive disorder. J Clin Psychiatry 46: 32–37.
Cryan JF, Lucki I (2000). Antidepressant-like behavioral effects mediated by 5-hydroxytryptamine2C receptors. J Pharmacol Exp Ther 295: 1120–1126.
Czyrak A, Mackowiak M, Chocyk A, Fijal K, Tokarski K, Bijak M et al (2002). Prolonged corticosterone treatment alters the responsiveness of 5-HT1A receptors to 8-OH-DPAT in rat CA1 hippocampal neurons. Naunyn Schmiedeberg's Arch Pharmacol 366: 357–367.
de Groot M, Anderson RJ, Freedland KE, Clouse RE, Lustman PJ (2001). Association of depression and diabetes complications: a meta-analysis. Psychosom Med 63: 619–630.
Feighner JP, Cohn JB (1985). Double-blind comparative trials of fluoxetine and doxepin in geriatric patients with major depressive disorder. J Clin Psychiatry 46: 20–25.
Fujii E, Nomoto T, Muraki T (1991). Effects of two 5-hydroxytryptamine agonists on head-weaving behaviour in streptozotocin-diabetic mice. Diabetologia 34: 537–541.
Goldberg HL, Finnerty RJ (1979). The comparative efficacy of buspirone and diazepam in the treatment of anxiety. Am J Psychiatry 136: 1184–1187.
Goodnick PJ, Kumar A, Henry JH, Buki VM, Goldberg RB (1997). Sertraline in coexisting major depression and diabetes mellitus. Psychopharmacol Bull 33: 261–264.
Gustafson EL, Durkin MM, Bard JA, Zgombick J, Branchek TA (1996). A receptor autoradiographic and in situ hybridization analysis of the distribution of the 5-ht7 receptor in rat brain. Br J Pharmacol 117: 657–666.
Haleem DJ (1992). Repeated corticosterone treatment attenuates behavioural and neuroendocrine responses to 8-hydroxy-2-(di-n-propylamino) tetralin in rats. Life Sci 51: L225–L230.
Hilakivi-Clarke LA, Wozniak KM, Durcan MJ, Linnoila M (1990). Behavior of streptozotocin-diabetic mice in tests of exploration, locomotion, anxiety, depression and aggression. Physiol Behav 48: 429–433.
Hohenegger M, Rudas B (1971). Kidney function in experimental diabetic ketosis. Diabetologia 7: 334–338.
Kamei J, Miyata S, Morita K, Saitoh A, Takeda H (2003). Effects of selective serotoninreuptake inhibitors on the immobility time in tail suspension test in streptozotocin-induced diabetic mice. Pharmacol Biochem Behav 75: 247–254.
Kamei J, Ohhashi Y, Aoki T, Kasuya Y (1991). Streptozotocin-induced diabetes in mice reduces the nociceptive threshold, as recognized after application of noxious mechanical stimuli but not of thermal stimuli. Pharmacol Biochem Behav 39: 541–544.
Khawaja X, Evans N, Reilly Y, Ennis C, Minchin MC (1995). Characterisation of the binding of [3H]WAY-100635, a novel 5-hydroxytryptamine1A receptor antagonist, to rat brain. J Neurochem 64: 2716–2726.
Lackovic Z, Salkovic M, Kuci Z, Relja M (1990). Effect of long-lasting diabetes mellitus on rat and human brain monoamines. J Neurochem 54: 143–147.
Lustman PJ, Anderson RJ, Freedland KE, de Groot M, Carney RM (2000a). Depression and poor glycemic control: a meta-analytic review of the literature. Diabetes Care 23: 434–442.
Lustman PJ, Freedland KE, Griffith LS, Clouse RE (2000b). Fluoxetine for depression in diabetes: a randomized double-blind placebo-controlled trial. Diabetes Care 23: 618–623.
Lustman PJ, Griffith LS, Clouse RE, Freedland KE, Eisen SA, Rubin EH et al (1997). Effects of nortriptyline on depression and glycemic control in diabetes: results of a double-blind, placebo-controlled trial. Psychosom Med 59: 241–250.
Maes M, Meltzer H (1995). The serotonin hypothesis of major depression. In: B loom F, Kupfer D (eds) . Psychopharmacology the Fourth Generation of Progress. Raven Press: New York. pp 933–944.
Mayorga AJ, Dalvi A, Page ME, Zimov-Levinson S, Hen R, Lucki I (2001). Antidepressant-like behavioral effects in 5-hydroxytryptamine1A and 5-hydroxytryptamine1B receptor mutant mice. J Pharmacol Exp Ther 298: 1101–1107.
McCall AL (1992). The impact of diabetes on the CNS. Diabetes 41: 557–570.
McQuade T, Sharp T (1997). Functional mapping of dorsal and median raphe 5-hydroxytryptamine pathways in forebrain of the rat using microdialysis. J Neurochem 69: 791–796.
Ohtani N, Ohta M, Sugano T (1997). Microdialysis study of modification of hypothalamic neurotransmitters in streptozotocin-diabetic rats. J Neurochem 69: 1622–1628.
Porsolt RD, Anton G, Blavet N, Jalfre M (1978). Behavioral despair in rats: a new model sensitive to antidepressant treatments. Eur J Pharmacol 47: 379–391.
Price JC, Kelley DE, Ryan CM, Meltzer CC, Drevets WC, Mathis CA et al (2002). Evidence of increased serotonin-1A receptor binding in type 2 diabetes: a positron emission tomography study. Brain Res 927: 97–103.
Reimherr FW, Byerley WF, Ward MF, Lebegue BJ, Wender PH (1988). Sertraline, a selective inhibitor of serotonin uptake, for the treatment of outpatients with major depressive disorder. Psychopharmacol Bull 24: 200–205.
Roy M, Collier B, Roy A (1990). Hypothalamic–pituitary–adrenal axis dysregulation among diabetic outpatients. Psychiatry Res 31: 31–37.
Roy M, Roy A, Gallucci WT, Collier B, Young K, Kamilaris TC et al (1993). The ovine corticotrophin-releasing hormone-stimulation test in type I diabetic patients and controls: suggestion of mild chronic hypercortisolism. Metabolism 42: 696–700.
Ruat M, Traiffort E, Leurs R, Tardivel-Lacombe J, Diaz J, Arrang JM et al (1993). Molecular cloning, characterization, and localization of a high-affinity serotonin receptor (5-HT7) activating cAMP formation. Proc Natl Acad Sci USA 90: 8547–8551.
Sandrini M, Vitale G, Vergoni AV, Ottani A, Bertolini A (1997). Streptozotocin-induced diabetes provokes changes in serotonin concentration and on 5-HT1A and 5-HT2 receptors in the rat brain. Life Sci 60: 1393–1397.
Schweizer EE, Amsterdam J, Rickels K, Kaplan M, Droba M (1986). Open trial of buspirone in the treatment of major depressive disorder. Psychopharmacol Bull 22: 183–185.
Scribner KA, Walker CD, Cascio CS, Dallman MF (1991). Chronic streptozotocin diabetes in rats facilitates the acute stress response without altering pituitary or adrenal responsiveness to secretagogues. Endocrinology 129: 99–108.
Steru L, Chermat R, Thierry B, Mico JA, Lenegre A, Steru M et al (1987). The automated tail suspension test: a computerized device which differentiates psychotropic drugs. Prog Neuro-Psychopharmacol Biol Psychiatry 11: 659–671.
Steru L, Chermat R, Thierry B, Simon P (1985). The tail suspension test: a new method for screening antidepressants in mice. Psychopharmacology 85: 367–370.
Sumiyoshi T, Ichikawa J, Meltzer H (1997). The effect of streptozotocin-induced diabetes on dopamine2, serotonin1A and serotonin2A receptors in the rat brain. Neuropsychopharmacology 16: 183–190.
Takao T, Tojo C, Nishioka T, Hashimoto K (2000). Increased adrenocorticotropin responses to acute stress in Otsuka Long–Evans Tokushima Fatty (type 2 diabetic) rats. Brain Res 852: 110–115.
Tarui S, Yamada K, Hanafusa T (1987). Animal models utilized in the research of diabetes mellitus—with special reference in insulitis-associated diabetes. Prog Clin Biol Res 229: 211–223.
Teste JF, Pelsy-Johann I, Decelle T, Boulu RG (1993). Anti-immobility activity of different antidepressant drugs using the tail suspension test in normal or reserpinized mice. Fundam Clin Pharmacol 7: 219–226.
To ZP, Bonhaus DW, Eglen RM, Jakeman LB (1995). Characterization and distribution of putative 5-ht7 receptors in guinea-pig brain. Br J Pharmacol 115: 107–116.
Tricklebank MD, Forler C, Fozard JR (1985). The involvement of subtypes of the 5-HT1 receptor and of catecholaminergic systems in the behavioural response to 8-hydroxy-2-(di-n-propylamino) tetralin in the rat. Eur J Pharmacol 106: 271–282.
Wieland S, Lucki I (1990). Antidepressant-like activity of 5-HT1A agonists measured with the forced swim test. Psychopharmacology 101: 497–504.
Willner P (1990). Animal models of depression: an overview. Pharmacol Ther 45: 425–455.
Acknowledgements
We thank Ms M Atsumi and Ms M Namba for their excellent technical assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Miyata, S., Hirano, S. & Kamei, J. Diabetes Attenuates the Antidepressant-Like Effect Mediated by the Activation of 5-HT1A Receptor in the Mouse Tail Suspension Test. Neuropsychopharmacol 29, 461–469 (2004). https://doi.org/10.1038/sj.npp.1300354
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.npp.1300354
Keywords
This article is cited by
-
Anxiolytic and Antidepressant Actions of 3-Hydroxypyridine and Succinic Acid Derivatives in Alloxan Diabetes
Neuroscience and Behavioral Physiology (2016)
-
Modeling of Diabetes Mellitus-Related Depression
Neurophysiology (2014)
-
The antidepressant-like action of mGlu5 receptor antagonist, MTEP, in the tail suspension test in mice is serotonin dependent
Psychopharmacology (2014)
-
Brain Insulin Dysregulation: Implication for Neurological and Neuropsychiatric Disorders
Molecular Neurobiology (2013)
-
Streptozotocin-induced insulin deficiency leads to development of behavioral deficits in rats
Acta Neurologica Belgica (2013)