Abstract
Because peripheral blood mononuclear cells play an important role in the perpetuation of the autoimmune process in rheumatoid arthritis (RA) and because the maintenance of these cells might be caused by the dysregulation of apoptosis, we investigated the apoptosis susceptibility of peripheral blood mononuclear cells from patients with RA. Freshly separated peripheral blood lymphocytes were stained for apoptosis markers (CD95, Bax, Bcl-2, TNF receptor) and for an activation marker (CD45-RO), and the apoptosis frequency of cells bearing these markers were assessed by the terminal-deoxynucleotidyl transferase-mediated dUTP digoxigenin nick end labeling method and nuclear condensation analysis with laser scanning cytometry. Also, the ability of CD4+ and CD8+ T-cell populations to undergo apoptosis was investigated with 24-hour culture in medium alone or with different apoptosis inducers (anti-CD3, anti-CD95, anti-TNF receptor). Laser scanning cytometry analysis was used to enumerate the phenotype and apoptosis ratios of both freshly isolated and cultured lymphocytes. Quantitative ELISA was performed to detect plasma levels of TNF-α and soluble Fas ligand. Furthermore, we studied the relationship between marked apoptotic defects in patients with RA and the severity of clinical disease. CD4+ T-cell counts in patients with RA were elevated compared with controls. A decreased rate of anti-CD95–mediated apoptosis was found within the CD4+ and CD8+ lymphocytic subpopulations. In patients with RA, decreased Bax expression and decreased apoptosis rate within the Bax-positive cells were found, whereas Bcl-2 expression was elevated. The CD45-RO expression was higher, whereas the apoptosis within CD45-RO+ cells were decreased in RA. Evaluation of plasma soluble Fas ligand revealed significantly decreased levels in patients compared with controls. The reduced susceptibility to CD95-mediated apoptosis may contribute to the expansion of an activated CD4+ lymphocyte subpopulation and thus to the maintenance of peripheral autoreactive T-cell clones in RA. We also revealed a relationship between in vitro demonstrated lymphocyte apoptosis defects and clinical disease activity.
Similar content being viewed by others
Main
Rheumatoid arthritis (RA) is a chronic, systemic autoimmune disease that affects primarily the joints and results in their progressive destruction. The destruction of articular cartilage and bone is the unique and most prominent feature of this disease, characterized by synovial hyperplasia, chronic inflammation, and autoimmune processes (Pap et al, 2002).
In RA, the synovial membrane undergoes considerable changes that are highly variable and characterized by infiltration of mononuclear cells such as T cells, B cells, and macrophages. Lymphocytic infiltration is mainly perivascular with T-cell predominance (Ziff M, 1989). Although the most prominent immunopathologic events take place in situ in the joints and within the synovial membrane, immune abnormalities are not limited to the activation and clonal expansion of synovium-infiltrating lymphocytes but also involve the majority of circulating T cells (Wagner et al, 1998).
In human RA peripheral blood cells, the percentage of total apoptosis induced with CD28 mAb/PMA has previously been found similar to that in normal donor peripheral blood mononuclear cells (PBMCs); this phenomenon has been explained by activated T-cell migration to the peripheral joints from peripheral vessels (Emlen et al, 1994; Lorenz et al, 1997). Because PBMCs play an important role in the pathogenesis of various systemic autoimmune diseases, such as systemic lupus erythematosus (Bijl et al, 2001; Funauchi et al, 2001; Papo et al, 1998), Sjögren’s syndrome (Zeher et al, 1999), and systemic sclerosis, (Stummvoll et al, 2000), we further investigated this phenomenon in RA.
Our aim was to determine, in RA, the apoptotic capability of PBMCs exposed to various apoptosis inducers, the presence of pro- and antiapoptotic markers, and apoptosis rates within PBMCs positive for these markers. We further classified peripheral blood lymphocytes into CD4+ and CD8+ T-cell subpopulations and investigated the apoptotic capability of these cells by inducing apoptosis with various cell death inducers [eg, anti-CD3, anti-CD95, anti-TNF receptor (anti-TNF-R)]. In addition, we quantified the expression of Bax, Bcl-2, CD95, TNF-R, and CD45-RO on freshly isolated lymphocytes and determined the rate of apoptosis in lymphocytes positive for these markers. Laser scanning cytometry (LSC), a “slide-based form” of flow cytometry, was used in the evaluation of these samples, with the advantage that marked cells (apoptotic cells determined by the scattergram data) could be rescanned, visualized, and analyzed. We used the combined information of flow cytometry, image analysis, and automated fluorescence microscopy for the evaluation and distinction of apoptotic and nonapoptotic cells with LSC. With this triple analysis, we could confidently distinguish between apoptotic and nonapoptotic cells. Finally, TNF-α and soluble Fas ligand (sFas-L) levels were evaluated using quantitative ELISA to measure the concentration of the most common natural apoptosis-inducers in the plasma of patients with RA and controls. A relationship between the investigated lymphocyte apoptotic defects and the clinical disease activity of patients with RA was demonstrated.
Results
Evaluation of CD4+ and CD8+ T-Cell Counts and Quantification of Apoptosis Rates Within these Subsets Exposed to Various Apoptosis Inducers
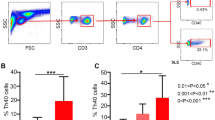
First, we compared the difference in the CD4+ and CD8+ T-cell counts from PBMCs between patients with RA and controls. Significantly higher levels of CD4+ lymphocytes were found in patients with RA compared with controls (RA: mean 41.13± 0.78 vs control: mean 37.7± 0.57, p = 0.0016) (Fig. 1A), whereas no significant difference was observed for CD8+ T cells between patients and controls (RA: mean 22.53± 0.51 vs control: mean 21.74± 0.55, p = 0.301) (Fig. 1B).
Comparison of CD4+ and CD8+ T-cell subsets between patients with rheumatoid arthritis (RA) (n = 15) and controls (n = 15). Bars show the mean and sem. A, CD4+ percentage of peripheral blood mononuclear cells (PBMCs). *Significantly different from control values by t test (p < 0.05). B, Percentage of CD8+ lymphocytes within PBMCs.
Furthermore, we analyzed the impact of different apoptosis inducers on triggering apoptosis within CD4+ and CD8+ T-lymphocyte subpopulations. We found that the rate of spontaneous apoptosis did not differ between patients and controls in the CD4+ population (RA: mean 5.06± 0.32 vs control: mean 5.66± 0.41, p = 0.254) and that the various apoptosis inducers had similar intensity of apoptosis induction in controls (Fig. 2A). However, when patients and controls were compared, a significantly lower apoptosis rate in patients with RA induced by anti-CD95 was found (RA: mean 7.45± 0.49 vs control: mean 9.99± 0.65, p = 0.0043), whereas for other apoptosis inducers we did not find a difference between patients and controls (α-CD3–induced apoptosis—RA: mean 9.41± 0.64 vs control: mean 10.05± 0.61, p = 0.47; α-TNF–induced apoptosis—RA: mean 9.39± 0.42 vs control: mean 9.79± 0.70, p = 0.63) (Fig. 2A).
Stimulation by various apoptosis inducers of PBMCs. CD4+ (A) and CD8+ (B) subsets from patients with RA and healthy controls. In the scattergram, each symbol indicates an individual patient/control; horizontal lines indicate mean values. *Significantly different from control values by t test (p < 0.05).
Similar to what was found for CD4+ lymphocytes, the spontaneous apoptosis frequencies within the CD8+ population were similar between patients and controls (RA: mean 4.98± 0.37 vs control: mean 5.26± 0.35, p = 0.59) (Fig. 2B). A significantly lower apoptosis rate was found among patients compared with controls, when induced by anti-CD95 (RA: mean 6.3± 0.36 vs control: mean 8.07± 0.32, p = 0.0012), whereas we did not find a significant difference (α-CD3–induced apoptosis—RA: mean 8.61± 0.52 vs control: mean 9.23± 0.53, p = 0.41; α-TNF–induced apoptosis—RA: mean 7.87± 0.56 vs control: mean 8.48± 0.44, p = 0.39) when comparing the effect of other apoptosis inducers (Fig. 2B).
Generally, in both the CD4+ and CD8+ subpopulations, anti-CD3 Ab was the most effective apoptosis inducer either in controls or in patients with RA. A tendency of lower apoptosis capability was observed among PBMCs from patients with RA.
Quantification of Apoptosis Markers, the Activation Marker CD45-RO, and Assessment of Apoptosis Ratio of PBMCs Positive for These Molecules
We next analyzed the presence of various markers involved in the apoptotic pathway, expressed by peripheral blood lymphocytes from freshly separated cells. By using LSC we could quantify these markers and define the frequency of apoptosis within positive cells.
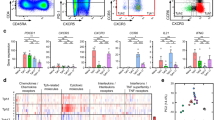
Figure 3A demonstrates the rate of expression of the proapoptotic molecule Bax between controls and patients. In patients with RA, the presence of Bax expression was significantly lower than in controls (RA: mean 76.77± 2.38 vs control: mean 87.19± 2.92, p = 0.01); the apoptosis rate within the Bax-positive cells was also lower in controls (RA: mean 4.74± 0.57 vs control: mean 7.57± 0.61, p = 0.0012) (Fig. 3B). We further quantified the antiapoptotic Bcl-2 expression levels and found a significantly higher expression in patients compared with controls (RA: mean 84.89± 3.17 vs control: mean 73.25± 3.55, p = 0.02) (Fig. 3C). The apoptosis rate within the Bcl-2–positive cells was lower among patients with RA than controls, but this did not reach a significant level (RA: mean 4.38± 0.77 vs control: mean 6.38± 0.75, p = 0.073) (Fig. 3D).
Comparison of expression levels of various markers and the apoptosis frequencies within cells positive to the indicated marker between patients with RA (n = 15) and controls (n = 15). Bars show the mean and sem. A, Percentage of Bax-positive cells within PBMCs. B, Apoptosis rate within Bax-positive PBMCs. C, Percentage of Bcl-2–positive cells within PBMCs. D, Apoptosis rate within Bcl-2–positive PBMCs. E, Percentage of CD45-RO–positive cells within PBMCs. F, Apoptosis rate within CD45-RO–positive PBMCs. G, Percentage of FAS (CD95)-positive cells within PBMCs. H, Apoptosis rate within FAS (CD95)-positive PBMCs. I, Percentage of TNF receptor (TNF-R)–positive cells within PBMCs. J, Apoptosis rate within TNF-R–positive PBMCs. *Significantly different from control values by t test (p < 0.05).
To quantify the rate of activated T cells, we stained for the activation marker CD45-RO (Fig. 3E). A higher number of activated T cells was found in patients compared with controls (RA: mean 54.07± 2.43 vs control: mean 42.55± 1.807, p = 0.0007), whereas the CD45-RO apoptosis level was highly significantly lower in patients (RA: mean 2.97 ± 0.23 vs control: mean 6.707± 0.61, p < 0.0001), indicating a longer survival of activated, CD45-RO+ T cells in RA (Fig. 3F). The next apoptosis marker analyzed and compared was CD95. Although in the patients group, the expression of CD95 was lower then in controls, it did not reach a significant level (RA: mean 47.18± 3.69 vs control: mean 54.47± 2.59, p = 0.12) (Fig. 3G). Further investigations showed that the rate of apoptosis within the CD95+ subset was significantly lower in patients with RA compared with controls (RA: mean 5.17± 0.78 vs control: mean 8.29± 0.55, p = 0.0027) (Fig. 3H). Neither TNF-R expression (RA: mean 46.23± 1.46 vs control: mean 46.53± 2.16, p = 0.909) (Fig. 3I), nor the apoptosis rate within TNF-R–expressing cells (RA: mean 6.42± 0.65 vs control: mean 6.033± 0.77, p = 0.703) differed significantly between patients and controls (Fig. 3J).
Plasma Levels of TNF-α and sFas-L
To measure the level of major apoptosis inducers in plasma of patients with RA and controls, we performed quantitative ELISA analysis for TNF-α and sFas-L. Concerning plasma TNF-α levels, no significant difference between patients and controls was detected (RA: mean 1024 ± 448.3 pg/ml vs control: mean 616.3 ± 322.7 pg/ml, p = 0.46) (Fig. 4A). Furthermore, soluble Fas-L levels between patients with RA and controls were analyzed, and a significantly lower level of plasma sFas-L in patients with RA was found (RA: mean 188.8 ± 16.28 pg/ml vs control: mean 252.1 ± 22.91 pg/ml, p = 0.032) (Fig. 4B).
Correlation Between the Activation Marker, CD45-RO Expression/CD45-RO+ Apoptosis, and the Clinical Disease Activity
First we compared the CD45-RO (activation marker) expression levels between patients with high activation score (DAS28+) and patients with low activation score (DAS28−). The results confirmed that in DAS28+ patients the level of CD45-RO was significantly higher then in the DAS28− RA patients (p = 0.048) (Fig. 5A).
Comparison of the expression levels of the activation marker CD45-RO and the apoptosis rate within CD45-RO+ cells between DAS28+ (n = 9) and DAS28− (n = 3) patients with RA and controls (n = 15). Bars show the mean and sem. A, Percentage of CD45-RO–positive cells within PBMCs. B, Apoptosis rate within CD45-RO–positive PBMCs. *Significantly different from control values by t test (p < 0.05).
We made further investigations and evaluated the level of apoptosis within the CD45-RO+ cells in the DAS28+ and DAS28− RA patient groups. Our results verified the hypothesis that among the activated cells, the percentage of apoptosis was significantly lower in DAS28+ patients (p = 0.011), suggesting that there is a prolonged survival of the CD45-RO+ cells in patients with clinically more severe/active disease (Fig. 5B).
Discussion
Peripheral blood T cells play an important role in the maintenance of autoreactive cell clones in RA and provide new supplies to the synovium and joint infiltrations (Cope, 2002; Hale and Haynes, 2001). Therefore, we investigated the survival of this cell population derived from peripheral blood of patients with RA.
Our findings suggest that RA PBMCs are characterized by a decrease in CD95 expression and lower apoptosis rate within the CD95-expressing lymphocytes. A decrease of sFas-L levels in serum of patients with RA indicates the diminished presence of natural apoptosis-inducing ligands, possibly resulting in the survival of CD4+ lymphocytes. In other studies on synovial fluid or synovial tissue in RA, it was shown that lymphocytes expressed CD95 and could be induced to undergo apoptosis by CD95 cross-linking (Cantwell et al, 1997). Furthermore, little or no expression of Fas-L by RA synovial lymphocytes has been detected, which could explain the ineffective clearance of activated cells in the RA joints (Cantwell et al, 1997). Other studies imply that synovial fluid lymphocytes from patients with RA express Fas-L, and cleaved sFas-L accumulates in the synovial fluid of inflamed joints (Hashimoto et al, 1998). The different killing activity of membrane-bound Fas-L and sFas-L against synovial cells may regulate Fas-mediated apoptosis in synovial cells (Hashimoto et al, 1998). Our results revealed that in RA, the impaired expression of TNF-R or the TNF-α–mediated apoptosis does not seem to contribute considerably in the peripheral blood lymphocyte apoptosis processes.
Elevated levels of Bcl-2 protein, residing on the cytoplasmic side of the mitochondrial outer membrane and endoplasmic reticulum, can protect a wide variety of cells from apoptosis (Adams and Cory, 1998; Kusenda, 1998). Within lymphocytes from patients with RA, increased Bcl-2 expression and a lower level of apoptosis were found when patients were compared with controls, although this did not reach statistical significance.
Overexpression of Bax accelerates apoptotic death induced by cytokine deprivation, and Bax also counters the death receptor activity of Bcl-2 (Oltvai et al, 1993). Data obtained from the analysis of Bax-positive cells revealed a markedly lower expression of this protein in RA PBMCs, and the apoptosis rate within these cells was significantly decreased in the patient group. These results indicate that in RA PBMCs, an antiapoptotic process occurs that is characterized by Bcl-2 overexpression and Bax underexpression, possibly resulting in an increased survival rate of these cells. A similar antiapoptotic process of lymphocytes has recently been presented in Sjögren’s syndrome salivary gland infiltrations, underlying the importance of the dysregulation of Bax and Bcl-2 expression of lymphocytes, resulting in an inappropriate apoptosis of systemic autoimmune diseases (Ohlsson et al, 2002).
Furthermore, PBMCs in RA are highly activated, which is supported by a marked increase in CD45-RO+ cell counts compared with controls. Our findings suggest that the presence of this population is maintained by a decreased apoptosis of these cells in RA. The survival of these activated cells in the periphery may lead to their subsequent recruitment to the site of joint inflammation with a higher probability. Our results are concordant with recent findings suggesting that the CD45-RO population predominates in the peripheral blood and even more in the synovial fluid of patients with RA (Mamoune et al, 2000). The majority of patients with arthritis manifest increased expression of multiple TCR V gene families in the synovial tissue–derived CD4+CD45-RO+ T-cell population when compared with the peripheral blood–derived CD4+CD45-RO+ subset, probably because of a specific interaction with particular MHC-peptide complexes expressed at the site of inflammation (Struyk et al, 1994). In juvenile idiopathic arthritis, the difference between CD45-RO+ T cells from synovial fluid and from peripheral blood suggests that specific activation events have occurred in synovial T cells (Wedderburn et al, 2000). Highly activated T helper 1 cells within the chronically inflamed joints may reflect specific recruitment events that contribute to the polarization of these cells (Wedderburn et al, 2000). These findings suggest that activated T cells from the periphery can be recruited to the site of inflammation by specific chemokines (Szekanecz et al, 1998) and that they may undergo further activation and modification processes in situ. These events may be derived by a predominantly proinflammatory cytokine milieu.
To correlate the investigated lymphocyte apoptosis defects and the clinical disease activity of patients with RA, we classified RA patients into two disease severity groups on the basis of DAS28 (DAS28+ and DAS28−). Furthermore, we evaluated the CD45-RO+ cell percentages and the level of apoptosis within these lymphocyte populations in the DAS28+ and DAS28− RA patients. Our results showed that in the background of clinically more active RA, an increase of CD45-RO+ lymphocytes with a significantly decreased capability of apoptosis can be detected. The increased number of activated lymphocytes with a pathologically prolonged lifespan in patients with active disease might be—at least partly—responsible for the clinical activity/severity of the disease.
Clinical data strongly support the role of T cells in the inflammatory process of RA (Pap et al, 2002). Some of the earliest changes seen in RA synovium are endothelial swelling and transformation of blood vessels to those with high endothelial cells (high endothelial venules or HEVs) (Vollertsen and Conn, 1990), which provides a means for leukocytes to access the synovium. Lymphocytes exit the blood through HEVs to form perivascular infiltrates consisting of large numbers of CD4+ T cells and smaller numbers of CD8+ T cells and B cells (Hale and Haynes, 2001); this process is highly derived by chemotactic cytokines (Szekanecz et al, 1998). Also, analysis of RA synovial fluid revealed the predominance of activated CD4+ T cells (Nordstrom, 1989). The hierarchy of T-cell dysfunction from peripheral blood to inflamed joint suggests that these defects are acquired through prolonged exposure to proinflammatory cytokines, and it is proposed that T-cell survival and effector responses are driven by antigen-independent, cytokine-dependent mechanisms (Cope, 2002). Our findings assume that the antiapoptotic process in RA PBMCs prolongs the existence of these cells and that this subsequently increases the probability of migration through HEVs to the site of autoimmune inflammation.
Because activated autoreactive T cells are assumed to play a considerable role in the pathogenesis of RA, specific therapeutic protocols have been developed that target these cells (Choy et al, 1998; Schulze-Koops and Lipsky, 2000). The eradication of autoreactive T cells by high-dose therapy, and stem cell transplantation and the resultant alterations in the immunologic network, thymic reeducation, and peripheral tolerance provide treatment mechanisms for autoimmune and inflammatory diseases (Talmadge et al, 2001). In RA, the outcome of autologous stem cell transplantation is a significant decrease in the CD4/CD8 ratio caused by a loss of CD4+ cells and a depression in T-cell function (Talmadge et al, 2001). Also, new apoptosis-related targets for the treatment of RA are invented, resulting in the depletion of autoreactive T cells (Pope, 2002).
Similarly to various systemic autoimmune diseases, in which altered apoptosis capability of PBMCs is characteristic and may contribute to the maintenance of the autoimmune processes (Bijl et al, 2001; Funauchi et al, 2001; Papo et al, 1998; Stummvoll et al, 2000; Zeher et al, 1999), our findings revealed the presence of activated peripheral blood T lymphocytes with impaired apoptosis, resulting in long-lived T cells peripherally in RA. This may contribute to the recruitment of these cells to the site of tissue damage and the perpetuation of the autoimmune inflammatory process. On the basis of these findings, we suggest that the depletion of autoreactive T-cell clones with apoptosis-related targets for treatment might be beneficial in RA.
Materials and Methods
Patients and Controls
Patients were recruited from the inpatient and outpatient clinic at the Department of Rheumatology, Haukeland University Hospital, Bergen, Norway. Subjects (n = 15; 11 women and 4 men) with RA (mean age 57.6 years, range 34–72; mean duration of disease 12.47 years, range 1–30) and age- and sex-matched healthy controls (n = 15) were involved in this study. Patients fulfilled the American Rheumatism Association classification criteria for RA (Arnett et al, 1988). The patients with RA were part of an infliximab trial study; samples were taken before obtaining the first infusion, as approved by the Ethics Committee of the University of Bergen.
Patients had been taking methotrexate in stable doses during the last months before inclusion in the study. If patients used nonsteroidal anti-inflammatory drugs or oral steroids, the doses were stable during the last month before inclusion. No other disease-modifying anti-rheumatic drugs were used during the last month before inclusion. Maximum dose for oral steroids was 7.5 mg of prednisolone. Informed consent was obtained from each patient before they were included in the study.
Primary Antibodies and Fluorochrome-Conjugated Secondary Antibodies
The following antibodies were used with the individually indicated specifications: mouse anti-human CD4 (IgG1; clone QS4120, Calbiochem-Novabiochem Corporation, San Diego, California); mouse anti-human CD8 (IgG1; clone SK1, Becton Dickinson, San Jose, California); mouse anti-human CD120a/TNF-R (IgG1; clone MR 1-2, Monosan, Uden, The Netherlands); mouse anti-human T cell CD45-RO (IgG2a; clone UCHL1, DAKO A/S, Glostrup, Denmark); mouse anti-human CD95/FAS (IgM; clone CH-11, Immunotech, Marseille, France); mouse anti-human CD3 (IgG1; clone SK7, Becton Dickinson); mouse anti-human Bcl-2 (IgG1; clone 124, DAKO A/S); and rabbit anti-human Bax (IgG; sc-526, Santa Cruz Biotechnology, Santa Cruz, California); FITC-conjugated goat anti-mouse (IgG/whole molecule; Sigma Corporation); and FITC-conjugated swine anti-rabbit (IgG/whole molecule; DAKO A/S).
Separation of PBMCs
Peripheral blood was diluted 1:1 in PBS before centrifugation over Lymphoprep (Axis-Shield PoC A/S, Oslo, Norway). Mononuclear cells were harvested from the interface of the Lymphoprep and the plasma and washed in PBS. For further analysis, plasma was collected and stored at −20° C. Cells were then cytospinned, fixed (direct staining for apoptosis markers), or cultured in complete RPMI-1640 medium for 1 day (apoptosis induction and CD4 or CD8 staining).
Cell Culture
Isolated mononuclear cells were cultured at 5 × 105 cells/ml in RPMI-1640 medium supplemented with 10% FCS, 2 mm glutamine, 20 mm HEPES, and 100 U/ml penicillin-streptomycin on 24-well plates for 24 hours at 37° C in an atmosphere containing 5% CO2. Cells were left in medium alone or treated with 100 μg/ml anti-CD3 antibody, 100 μg/ml anti-TNF antibody, or 1 mg/ml anti-CD95 antibody.
Immunofluorescent Labeling
Cells were harvested and cytospinned (Shandon Elliot Cytospin; Thermo Shandon Inc., Pittsburgh, Pennsylvania) at 580 rpm for 5 minutes on gelatin-coated glass slides. After stepwise fixation in methanol at −20° C for 1 hour and 4% paraformaldehyde at room temperature for 15 minutes, noncultured cells were then incubated for 60 minutes with any of the following antibodies diluted in 1% BSA/PBS: mouse anti-human CD120a/TNF-R (diluted 1:10); mouse anti-human T cell CD45-RO (diluted 1:100); mouse anti-human CD95 (diluted 1:25); mouse anti-human Bcl-2 (diluted 1:40); or rabbit anti-human Bax (diluted 1:200). Cultured cells were stained with either mouse anti-human CD4 (diluted 1:200) or mouse anti-human CD8 (diluted 1:20).
Fluorochrome-conjugated secondary reagents were then applied for 1 hour: FITC-conjugated goat anti-mouse (diluted 1:50) for CD4, CD8, CD120a/TNF-R, T cell CD45-RO, and CD95 for Bcl-2 staining or FITC-conjugated swine anti-rabbit (diluted 1:30) for Bax staining.
The staining procedures were performed at room temperature, and the sections were washed with PBS for 10 minutes after each incubation. Incubations with isotype- and concentration- matched immunoglobulins diluted in the respective blocking solutions (omitting the primary antibodies) were performed as negative controls: mouse IgG for CD4, CD8, CD120a/TNF-R, T cell CD45-RO for Bcl-2 staining, rabbit IgG for Bax staining, and mouse IgM for CD95 staining.
Detection of Apoptotic Cells with Terminal-Deoxynucleotidyl Transferase-Mediated dUTP Digoxigenin Nick End Labeling (TUNEL) Labeling
After incubation with the secondary antibody, sections were washed in PBS and equilibrated at 37° C for 2 × 5 minutes in terminal-deoxynucleotidyl transferase (TdT) buffer (0.5 m cacodylate, pH 6.8, 1 mm CoCl2, 0.5 mm dithiothreitol, 0.05% BSA, and 0.15 m NaCl). Incubation with TdT buffer containing 0.1 U/L TdT (Boehringer Mannheim, Mannheim, Germany) and 8 nmol/ml digoxigenin-conjugated dUTP (Boehringer Mannheim) was then performed in a humidified chamber for 1 hour at 37° C. Negative controls were incubated with reaction buffer alone, omitting either TdT or DIG-dUTP from the solution. The reaction was stopped by washing in PBS. TUNEL-positive cells were labeled with sheep anti-digoxigenin-rhodamine Fab fragments (Roche Diagnostics, Oslo, Norway), diluted 1:200 in 2% BSA/PBS for 30 minutes at room temperature.
Counterstaining with DNA Marker To-Pro3
Cells were finally incubated with To-Pro3 (diluted 1:1000; Molecular Probes Europe BV, Leiden, The Netherlands) for 15 minutes, then washed and mounted with aqueous Slow Fade antifade medium (Molecular Probes Europe BV).
LSC
Quantitative analysis of the multiple immunofluorescence stainings was performed by LSC (CompuCyte Corporation, Cambridge, Massachusetts) in a blinded fashion (see Table 1 for instrument setup). This technique is similar to flow cytometry but with the distinction that analysis is performed on cells fixed to a microscope slide rather than in a solution. This way it is possible to relocate cells and directly correlate objective physical and immunofluorescence measurements with light microscopic cytologic morphology on a cell-by-cell basis. This is useful when distinguishing between apoptotic and nonapoptotic cells.
A minimum of 3000 cells were selected for each specimen by contouring on nuclear fluorescence (To-Pro3) with a minimum threshold value. Fluorescence intensities for all fluorochromes were measured inside a contouring line 2 pixels outside this threshold contour. In the WinCyte (CompuCyte Corporation) software, each cell could be displayed in scattergrams and histograms with integral, area, or maximum pixel on the x or y axis (Fig. 6). Integral is the total measured fluorescence for a given cell, area is the cell area defined as pixel2, and maximum pixel is the brightest pixel value in a cell. The cell area and maximum pixel of To-Pro3 were displayed in a scattergram, and the cells used in the rest of the analysis were gated from this scattergram. By relocating cells and observing their morphology with epifluorescence or by rescanning, it was possible to exclude multiple selected cells and to distinguish between apoptotic and nonapoptotic cells. Cells were defined and colored as rhodamine (TUNEL)-positive cells and FITC-positive cells in a TUNEL integral histogram (Fig. 6A) and an FITC integral histogram (Fig. 6B), respectively. The percentages of cells that were FITC positive, TUNEL positive, and double positive were measured by dividing a scattergram with FITC Integral on the y axis and TUNEL integral on the x axis into four quadrants (Fig. 6C). Apoptotic cells have a small nucleus with condensed DNA, which stains brightly with To-Pro3, and this could be correlated with their TUNEL integral staining (Fig. 6D). Simultaneous application of TUNEL integral and ToPro-3 maximum pixel values provides a reliable method for the evaluation of apoptotic cells. Color images were created from regions of interest by rescanning with CompuColor (Fig. 7, A to D).
The apoptotic capability and phenotype of peripheral blood T lymphocytes measured by laser scanning cytometry (LSC). Cells were selected by contouring on nuclear DNA To-Pro3 staining, and apoptotic cells were identified by positive TdT-mediated dUTP digoxigenin nick end labeling (TUNEL) staining and high To-Pro3 MaxPixel values. FITC was conjugated with various antibodies for immunophenotyping (CD45-RO in these graphs). Logarithmic scale is used on all scattergrams and on the y axis of histograms. A total of 3000 cells were analyzed for each specimen. A, Cells that stained for TUNEL were selected and colored red. B, Cells that stained for FITC were selected and colored blue. C, Region 1: Nonapoptotic cells with positive FITC staining (blue). Region 2: Apoptotic cells with positive FITC staining; double positive (green). Region 4: Apoptotic cells with no FITC staining (red). Region 3: Cells with no staining. The percentage of the cell population in each quadrant is indicated. D, Validation of apoptotic cells. TUNEL positive cells (red color) have high ToPro Max Pixel values caused by DNA condensation and shrinkage of the nuclei in the apoptotic cells.
LSC images were created by rescanning and using CompuColor to assign a different color to each individual fluorochrome. TUNEL is blue, FITC is green, and To-Pro3 is red. A, Image created using only the long red sensor (To-Pro3). Apoptotic cells can be identified by their small, dense nuclei with condensed DNA, which stains brightly with To-Pro3 (arrows). B, TUNEL-positive cell (arrow). C, FITC-positive cell (arrow). D, Double-positive FITC+TUNEL− cell (arrow).
ELISA Assay for Detection of TNF-α and Fas-L in Plasma
To quantify plasma TNF-α levels, we used a DuoSet ELISA Development Kit (R&D Systems Inc., Minneapolis, Minnesota), with samples diluted 1:4. Plasma sFas-L levels were determined by a soluble Fas-L ELISA Kit (Diaclone Research, Besancon, France), with samples diluted. The assays were performed following the manufacturer’s instructions. Optical density of each well was determined immediately, using an Emax Precision microplate reader (Molecular Devices Corporation, Sunnyvale, California) set to 450 nm for the evaluation of TNF-α and to 450 and 620 nm for the evaluation of sFas-L.
Assessment of Disease Activity Score and the Evaluation of CD45-RO+ Cells/Apoptosis of CD45-RO+ Cells in Different DAS28 Groups
To evaluate the severity/activity of RA we used the Disease Activity Score (DAS28) assessment procedure (Prevoo et al, 1995).
Three patients of 15 lacked one or more of the variables needed to compute the DAS28 (erythrocyte sedimentation rate, swollen joints, tender joints, patient’s global assessment). The DAS28 can therefore not be computed for these patients. DAS28 was considered positive if the value was less than 5.1. After the evaluation of DAS28, nine patients had positive scores (DAS28+) and three had negative scores (DAS28−). In these two disease groups, we further assessed and compared the percentage of CD45-RO+ cells (activated lymphocytes) and the apoptosis levels within these cells.
Statistical Analysis
Statistical differences in measured values were analyzed using a two-tailed Student’s t test. p values less than 0.05 were considered statistically significant.
References
Adams JM and Cory S (1998). The Bcl-2 protein family: Arbiters of cell survival. Science 281: 1322–1326.
Arnett FC, Edworthy SM, Bloch DA, McShane DJ, Fries JF, Cooper NS, Healey LA, Kaplan SR, Liang MH, Luthra HS, Medsger TA, Mitchell DM, Neustadt DH, Pinals RS, Schaller JG, Sharp JT, Wilder RL, and Hunder GG (1988). The American Rheumatism Association 1987 revised criteria for the classification of rheumatoid arthritis. Arthritis Rheum 31: 315–324.
Bijl M, Horst G, Limburg PC, and Kallenberg CG (2001). Fas expression on peripheral blood lymphocytes in systemic lupus erythematosus (SLE): Relation to lymphocyte activation and disease activity. Lupus 10: 866–872.
Cantwell MJ, Hua T, Zvaifler NJ, and Kipps TJ (1997). Deficient Fas ligand expression by synovial lymphocytes from patients with rheumatoid arthritis. Arthritis Rheum 40: 1644–1652.
Choy EH, Kingsley GH, and Panayi GS (1998). Monoclonal antibody therapy in rheumatoid arthritis. Br J Rheumatol 37: 484–490.
Cope AP (2002). Studies of T-cell activation in chronic inflammation. Arthritis Res 4 (Suppl 3): S197–S211.
Emlen W, Niebur J, and Kadera R (1994). Accelerated in vitro apoptosis of lymphocytes from patients with systemic lupus erythematosus. J Immunol 152: 3685–3692.
Funauchi M, Sugiyama M, SukYoo B, Ikoma S, Ohno M, Kinoshita K, and Kanamaru A (2001). A possible role of apoptosis for regulating autoreactive responses in systemic lupus erythematosus. Lupus 10: 284–288.
Hale LP and Haynes BF (2001). Pathology of rheumatoid arthritis and associated disorders, 14th ed. In: Koopman WJ, editor. Arthritis and allied conditions: A textbook of rheumatology. Philadelphia: Lippincott Williams & Wilkins, 1103–1127.
Hashimoto H, Tanaka M, Suda T, Tomita T, Hayashida K, Takeuchi E, Kaneko M, Takano H, Nagata S, and Ochi T (1998). Soluble Fas ligand in the joints of patients with rheumatoid arthritis and osteoarthritis. Arthritis Rheum 41: 657–662.
Kusenda J (1998). Bcl-2 family proteins and leukemia: Minireview. Neoplasma 45: 117–122.
Lorenz HM, Grunke M, Hieronymus T, Herrmann M, Kuhnel A, Manger B, and Kalden JR (1997). in vitro apoptosis and expression of apoptosis-related molecules in lymphocytes from patients with systemic lupus erythematosus and other autoimmune diseases. Arthritis Rheum 40: 306–317.
Mamoune A, Durand V, Le Goff P, Pennec YL, Youinou P, and Le Corre R (2000). Abnormal distribution of CD45 isoforms expressed by CD4+ and CD8+ T cells in rheumatoid arthritis. Histol Histopathol 15: 587–591.
Nordstrom DC (1989). DNA synthesis in CD4- and CD8-positive cells in synovial fluid of patients with reactive and rheumatoid arthritis. Rheumatol Int 8: 269–272.
Ohlsson M, Szodoray P, Loro LL, Johannessen AC, and Jonsson R (2002). CD40, CD154, Bax and Bcl-2 expression in Sjögren’s syndrome salivary glands: A putative anti-apoptotic role during its effector phases. Scand J Immunol 56: 561–571.
Oltvai ZN, Milliman CL, and Korsmeyer SJ (1993). Bcl-2 heterodimerizes in vivo with a conserved homolog, Bax, that accelerates programmed cell death. Cell 74: 609–619.
Pap T, Gay RE, and Gay S (2002). Rheumatoid arthritis, 2nd ed. In: Theofilopoulos AN and Bona CA, editors. The molecular pathology of autoimmune diseases. New York: Taylor & Francis, 376–401.
Papo T, Parizot C, Ortova M, Piette JC, Frances C, Debre P, Godeau P, and Gorochov G (1998). Apoptosis and expression of soluble Fas mRNA in systemic lupus erythematosus. Lupus 7: 455–461.
Pope RM (2002). Apoptosis as a therapeutic tool in rheumatoid arthritis. Nat Rev Immunol 2: 527–535.
Prevoo ML, van ’t Hof MA, Kuper HH, van Leeuwen MA, van de Putte LB, and van Riel PL (1995). Modified disease activity scores that include twenty-eight-joint counts: Development and validation in a prospective longitudinal study of patients with rheumatoid arthritis. Arthritis Rheum 38: 44–48.
Schulze-Koops H and Lipsky PE (2000). Anti-CD4 monoclonal antibody therapy in human autoimmune diseases. Curr Dir Autoimmun 2: 24–49.
Struyk L, Hawes GE, Dolhain RJ, van Scherpenzeel A, Godthelp B, Breedveld FC, and van den Elsen PJ (1994). Evidence for selective in vivo expansion of synovial tissue-infiltrating CD4+ CD45-RO+ T lymphocytes on the basis of CDR3 diversity. Int Immunol 6: 897–907.
Stummvoll GH, Aringer M, Smolen JS, Koller M, Kiener HP, Steiner CW, Bohle B, Knobler R, and Graninger WB (2000). Derangement of apoptosis related lymphocyte homeostasis in systemic sclerosis. Rheumatology 39: 1341–1350.
Szekanecz Z, Strieter RM, Kunkel SL, and Koch AE (1998). Chemokines in rheumatoid arthritis. Springer Semin Immunopathol 20: 115–132.
Talmadge JE, Singh R, Ageitos A, and Buyukberber S (2001). Potential for cytokine and product manipulation to improve the results of autologous stem cell transplantation for rheumatoid arthritis. J Rheumatol Suppl 64: 32–38.
Vollertsen RS and Conn DL (1990). Vasculitis associated with rheumatoid arthritis. Rheum Dis Clin North Am 16: 445–461.
Wagner UG, Koetz K, Wey CM, and Goronzy JJ (1998). Perturbation of the T cell repertoire in rheumatoid arthritis. Proc Natl Acad Sci USA 95: 14447–14452.
Wedderburn LR, Robinson N, Patel A, Varsani H, and Woo P (2000). Selective recruitment of polarized T cells expressing CCR5 and CXCR3 to the inflamed joints of children with juvenile idiopathic arthritis. Arthritis Rheum 43: 765–774.
Zeher M, Szodoray P, Gyimesi E, and Szondy Z (1999). Correlation of increased susceptibility to apoptosis of CD4+ T cells with lymphocyte activation and activity of disease in patients with primary Sjögren’s syndrome. Arthritis Rheum 42: 1673–1681.
Ziff M (1989). Pathways of mononuclear cell infiltration in rheumatoid synovitis. Rheumatol Int 9: 97–103.
Acknowledgements
We thank Turid Tynning for excellent help with the ELISA analysis, Dr. Maria Ohlsson for technical advices for LSC, and the medical and rheumatology laboratory staff at the Department of Rheumatology, Haukeland University Hospital, for helping in the collection of patients’ materials. We also thank Dr. Anne G. Kvalvik at the Haugesund Rheumatism Hospital, Haugesund, Norway, for protocol development of the main infliximab study, from which the patients of the present study were recruited.
This work was supported by The Broegelmann Foundation, The University of Bergen, Bergen, Norway.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Szodoray, P., Jellestad, S., Nakken, B. et al. Programmed Cell Death in Rheumatoid Arthritis Peripheral Blood T-Cell Subpopulations Determined by Laser Scanning Cytometry. Lab Invest 83, 1839–1848 (2003). https://doi.org/10.1097/01.LAB.0000101703.80133.99
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1097/01.LAB.0000101703.80133.99
Keywords
This article is cited by
-
Decreased serum cell-free DNA levels in rheumatoid arthritis
Autoimmunity Highlights (2015)
-
Initiation but no execution - modulation of peripheral blood lymphocyte apoptosis in rheumatoid arthritis - a potential role for heat shock protein 70
Journal of Inflammation (2011)
-
Rosmarinic Acid Induces Apoptosis of Activated T Cells from Rheumatoid Arthritis Patients via Mitochondrial Pathway
Journal of Clinical Immunology (2007)
-
Elevated levels of soluble Fas (APO-1, CD95), soluble Fas ligand, and matrix metalloproteinase-3 in sera from patients with active untreated adult onset Still’s disease
Clinical Rheumatology (2007)