Abstract
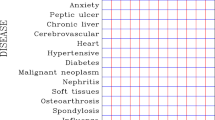
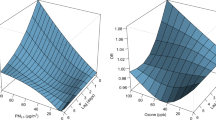
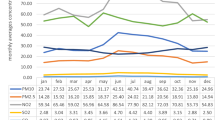
Existing studies of the association between air pollution, aeroallergens and emergency department (ED) visits have generally examined the effects of a few pollutants or aeroallergens on individual conditions such as asthma or chronic obstructive pulmonary disease. In this study, we considered a wide variety of respiratory and cardiac conditions and an extensive set of pollutants and aeroallergens, and utilized prospectively collected information on possible effect modifiers which would not normally be available from purely administrative data. The association between air pollution, aeroallergens and cardiorespiratory ED visits (n=19,821) was examined for the period 1992 to 1996 using generalized additive models. ED visit, air pollution and aeroallergen time series were prefiltered using LOESS smoothers to minimize temporal confounding, and a parsimonious model was constructed to control for confounding by weather and day of week. Multipollutant and multi-aeroallergen models were constructed using stepwise procedures and sensitivity analyses were conducted by season, diagnosis, and selected individual characteristics or effect modifiers. In single-pollutant models, positive effects of all pollutants but NO2 and COH were observed on asthma visits, and positive effects on all respiratory diagnosis groups were observed for O3, SO2, PM10, PM2.5, and SO42−. Among cardiac conditions, only dysrhythmia visits were positively associated with all measures of particulate matter. In the final year-round multipollutant models, a 20.9% increase in cardiac ED visits was attributed to the combination of O3 (16.0%, 95% CI 2.8–30.9) and SO2 (4.9%, 95%CI 1.7–8.2) at the mean concentration of each pollutant. In the final multipollutant model for respiratory visits, O3 accounted for 3.9% of visits (95% CI 0.8–7.2), and SO2 for 3.7% (95% CI 1.5–6.0), whereas a weak, negative association was observed with NO2. In multi-aeroallergen models of warm season asthma ED visits, Ascomycetes, Alternaria and small round fungal spores accounted for 4.5% (95% CI 1.8–7.4), 4.7% (95% CI 1.0–8.6) and 3.0% (95% CI 0.8–5.1), respectively, of visits at their mean concentrations, and these effects were not sensitive to adjustment for air pollution effects. In conclusion, we observed a significant influence of the air pollution mix on cardiac and respiratory ED visits. Although in single-pollutant models, positive associations were noted between ED visits and some measures of particulate matter, in multipollutant models, pollutant gases, particularly ozone, exhibited more consistent effects. Aeroallergens were also significantly associated with warm season asthma ED visits.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
STIEB, D., BEVERIDGE, R., BROOK, J. et al. Air pollution, aeroallergens and cardiorespiratory emergency department visits in Saint John, Canada. J Expo Sci Environ Epidemiol 10, 461–477 (2000). https://doi.org/10.1038/sj.jea.7500112
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jea.7500112
Keywords
This article is cited by
-
Synergistic health effects of air pollution, temperature, and pollen exposure: a systematic review of epidemiological evidence
Environmental Health (2020)
-
Systematic review and meta-analysis of case-crossover and time-series studies of short term outdoor nitrogen dioxide exposure and ischemic heart disease morbidity
Environmental Health (2020)
-
Airborne Cladosporium and Alternaria spore concentrations through 26 years in Copenhagen, Denmark
Aerobiologia (2020)
-
Short-acting β2-agonists (SABA) bronchodilator sales and outdoor mould in central France
Clinical and Translational Allergy (2019)
-
Short-term effect of PM2.5 on pediatric asthma incidence in Shanghai, China
Environmental Science and Pollution Research (2019)