Abstract
Objective:
To document meal frequency and its relationship to body mass index (BMI) in a longitudinal sample of black and white girls from ages 9–19 years.
Design:
Ten-year longitudinal observational study.
Subjects:
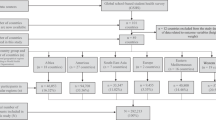
At baseline, 1209 Black girls (539 age nine years, 670 age 10 years) and 1,166 White girls (616 age nine years, 550 age 10 years) were enrolled in the National Heart, Lung and Blood Institute Growth and Health Study (NGHS).
Measurements:
Three-day food diaries, measured height and weight and self-reported physical activity and television viewing were obtained at annual in-person visits.
Results:
Over the course of the study, the percentage of girls eating 3+ meals on all 3 days was reduced by over half (15 vs 6%). Participants who ate 3+ meals on more days had lower BMI-for-age z-scores. Black girls, but not white girls, who ate 3+ meals on more days were less likely to meet criteria for overweight.
Conclusion:
Meal frequency was related to BMI and should be considered when developing guidelines to prevent childhood overweight.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Centers for Disease Control and Prevention Prevalence of overweight among children and adolescents: United States, 1999–2000. http://www.cdc.gov/nchs/products/pubs/pubd/hestats/overwght99.htm. 2002.
Ebbeling CB, Pawlak DB, Ludwig DS . Childhood obesity: public health crisis, common sense cure. Lancet 2002; 360: 473–482.
Flodmark CE, Marcus C, Britton M . Interventions to prevent obesity in children and adolescents: a systematic literature review. Int J Obes 2006; 30: 579–589.
Fabry P, Hejl Z, Fodor J, Braun T, Zvolankova K . The frequency of meals: its relation to overweight, hypercholesterolaemia, and decreased glucose-tolerance. Lancet 1964; 18: 614–615.
Edelstein SL, Barrett-Connor EL, Wingard DL, Cohn BA . Increased meal frequency associated with decreased cholesterol concentrations; Rancho Bernardo CA, 1984–1987. Am J Clin Nutr 1992; 55: 664–669.
Kant AK, Schatzkin A, Graubard BI, Ballard-Barbash R . Frequency of eating occasions and weight change in the NHANES I Epidemiologic Follow-Up Study. Int J Obes Relat Metab Disord 1995; 19: 468–474.
Metzner HL, Lamphiear DE, Wheeler NC, Larkin FA . The relationship between frequency of eating and adiposity in adult men and women in the Tecumseh Community Health Study. Am J Clin Nutr 1977; 30: 712–715.
Bellisle F, McDevitt R, Prentice AM . Meal frequency and energy balance. Br J Nutr 1997; 77 (Suppl 1): S57–S70.
Jenkins DJ, Khan A, Jenkins AL, Illingworth R, Pappu AS, Wolever TM et al. Effect of nibbling versus gorging on cardiovascular risk factors: serum uric acid and blood lipids. Metabolism 1995; 44: 549–555.
Jenkins DJ, Wolever TM, Vuksan V, Brighenti F, Cunnane SC, Rao AV et al. Nibbling versus gorging: metabolic advantages of increased meal frequency. N Engl J Med 1989; 321: 929–934.
Croll JK, Neumark-Sztainer D, Story M, Wall M, Perry C, Harnack L . Adolescents involved in weight-related and power team sports have better eating patterns and nutrient intakes than non-sport-involved adolescents. J Am Diet Assoc 2006; 106: 709–717.
Wyatt HR, Grunwald GK, Mosca CL, Klem ML, Wing RR, Hill JO . Long-term weight loss and breakfast in subjects in the National Weight Control Registry. Obes Res 2002; 10: 78–82.
Kerver JM, Yang EJ, Obayashi S, Bianchi L, Song WO . Meal and snack patterns are associated with dietary intake of energy and nutrients in US adults. J Am Diet Assoc 2006; 106: 46–53.
Nicklas TA, Yang SJ, Baranowski T, Zakeri I, Berenson G . Eating patterns and obesity in children: The Bogalusa Heart Study. Am J Prev Med 2003; 25: 9–16.
Nicklas TA, Morales M, Linares A, Yang S, Baranowski T, De Moor C et al. Children's meal patterns have changed over a 21-year period: the Bogalusa Heart Study. J Am Diet Assoc 2004; 104: 753–761.
Toschke AM, Kuchenhoff H, Koletzko B, von Kries R . Meal frequency and childhood obesity. Obes Res 2005; 13: 1932–1938.
Thompson OM, Ballew C, Resnicow K, Gillespie C, Must A, Bandini LG et al. Dietary patterns as a predictor of change in BMI z-score among girls. Int J Obes (London) 2006; 30: 176–182.
Nicklas TA, Baranowski T, Cullen KW, Berenson G . Eating patterns, dietary quality and obesity. J Am Coll Nutr 2001; 20: 599–608.
Siega-Riz AM . Three squares or mostly snacks--what do teens really eat? A sociodemographic study of meal patterns. J Adolesc Health 1998; 22: 29–36.
The National Heart, Lung, and Blood Institute Growth and Health Study Research Group. Obesity and cardiovascular disease risk factors in black and white girls: the NHLBI Growth and Health Study. Am J Public Health 1992; 82: 1613–1620.
Crawford PB, Obarzanek E, Morrison J, Sabry ZI . Comparative advantage of 3-day food records to 24-hour recall or 5-day food frequency validated by observation of 9- and 10-year-old girls. J Am Diet Assoc 1994; 94: 626–630.
Schakel GH, Sievert YA, Buzzard IM . Sources of data for developing and maintaining a nutrient database. J Am Diet Assoc 1988; 88: 1268–1271.
Ross CE, Mirowsky J . Refining the association between education and health: the effects of quantity, credential, and selectivity. Demography 1999; 36: 445–460.
Ku LC, Shapiro LR, Crawford PB, Hunenemann RL . Body composition and physical activity in 8-year-old children. Am J Clin Nutr 1981; 34: 2770–2775.
Kimm SY, Glynn NW, Kriska AM, Barton BA, Kronsberg SS, Daniels SR et al. Longitudinal changes in physical activity in a biracial cohort during adolescence. Med Sci Sports Exerc 2000; 32: 1445–1454.
Verbeke G, Molenberghs G . Linear mixed models for longitudinal data. Springer-Verlag: New York, 2000.
Beunckens C, Molenberghs G, Kenward MG . Direct likelihood analysis versus simple forms of imputation for missing data in randomized clinical trials. Clin Trials 2005; 2: 379–386.
Louis-Sylvestre J, Lluch A, Neat F, Blundell JE . Highlighting the positive impact of increasing feeding frequency on metabolism and weight management. Forum Nutr 2003; 56: 126–128.
Affenito SG, Thompson DR, Barton BA, Franko DL, Daniels SR, Obarzanek E et al. Breakfast consumption by African-American and White adolescent girls correlates positively with calcium and fiber intake and negatively with body mass index. J Am Diet Assoc 2005; 105: 938–945.
Pastore DR, Fisher M, Stanford FB . Abnormalities in weight status, eating attitudes, and eating behavior among urban high school students: correlations with self esteem. J Adol Health 1996; 18: 312–319.
Rampersaud GC, Pereira MA, Girard BL, Adams J, Metzl JD . Breakfast habits, nutritional status, body weight, and academic performance in children and adolescents. J Am Diet Assoc 2005; 105: 743–760.
Sjoberg A, Hallberg L, Hoglund D, Hulthen L . Meal pattern, food choice, nutrient intake and lifestyle factors in The Goteborg Adolescence Study. Eur J Clin Nutr 2003; 57: 1569–1578.
Centers for Disease Control and Prevention. Prevalence of Overweight Among Children and Adolescents: United States 1999–2002. Retrieved from http://www.cdc.gov/nchs/products/pubs/pubd/hestats/overwght99.htm on October 29, 2004.
Cullen KW, Baranowski T, Klesges LM, Watson K, Sherwood NE, Story M et al. Anthropometric, parental, and psychosocial correlates of dietary intakes of African-American girls. Obes Res 2004; 12 (Suppl): 20S–31S.
Roberts D, Foehr V, Rideout V . Kids and media at the new millennium. Kaiser Family Foundation: Menlo Park CA, 1999.
Barakat H, Davis J, Lang D, Mustafa SJ, McConnaughey MM . Differences in the expression of the adenosine A1 receptor in adipose tissue of obese black and white women. J Clin Endocrinol Metab 2006; 91: 1882–1886.
Patel DA, Srinivasan SR, Zu JH, Li S, Chen W, Berenson GS . Distribution and metabolic syndrome correlates of plasma C-reactive protein in biracial (black-white) younger adults: the Bogalusa Heart Study. Metabolism 2006; 55: 699–705.
Lytle LA, Seifert S, Greenstein J, McGovern P . How do children's eating patterns and food choices change over time? Results from a cohort study. Am J Health Promot 2000; 14: 222–228.
Acknowledgements
Supported by a grant from the National Heart, Lung and Blood Institute (NHLBI) (HL/DK71122) and by contracts HC55023-26 and Cooperative Agreements U01-HL-48941-44. Participating NGHS Centers included Children's Medical Center, Cincinnati, OH (Stephen R Daniels, MD, Principal Investigator, John A Morrison, PhD, Co-Investigator); Westat, Inc., Rockville, Maryland (George B Schreiber, ScD, Principal Investigator, Ruth Striegel-Moore, PhD, Co-Investigator) and University of California, Berkeley, California (Zak I Sabry, PhD, Principal Investigator, Patricia B Crawford, Dr PH, RD, Co-Investigator); Maryland Medical Research Institute, Baltimore, Maryland (Bruce A Barton, PhD, Principal Investigator) served as the data coordinating center. Program Office: NHLBI (Eva Obarzanek, PhD, RD, Project Officer 1992-present, Gerald H Payne, MD, Project Officer 1985–1991).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Franko, D., Striegel-Moore, R., Thompson, D. et al. The relationship between meal frequency and body mass index in black and white adolescent girls: more is less. Int J Obes 32, 23–29 (2008). https://doi.org/10.1038/sj.ijo.0803654
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ijo.0803654
Keywords
This article is cited by
-
Joint association of meal frequency and diet quality with metabolic syndrome in Iranian adults
BMC Nutrition (2022)
-
Body mass index and associated factors among refugees living in North Rhine-Westphalia, Germany: a cross-sectional study
BMC Nutrition (2021)
-
Decreased eating frequency linked to increased visceral adipose tissue, body fat, and BMI in Hispanic college freshmen
BMC Nutrition (2018)
-
Comparison of meal patterns across five European countries using standardized 24-h recall (GloboDiet) data from the EFCOVAL project
European Journal of Nutrition (2018)
-
Age and time trends in eating frequency and duration of nightly fasting of German children and adolescents
European Journal of Nutrition (2017)