Abstract
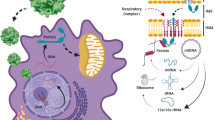
Defects of the mitochondrial genome cause a wide variety of clinical disorders. Except for rare cases where surgery or transplant is indicated, there is no effective treatment for patients. Genetic-based therapies are consequently being considered. On account of the difficulties associated with mitochondrial (mt) transfection, alternative approaches whereby mitochondrial genes can be engineered and introduced into the nucleus (allotopic expression) are being attempted with some success, at least in cultured cells. Defects in the activities of multi-subunit complexes of the oxidative phosphorylation apparatus have been circumvented by the targeted expression of simple single subunit enzymes from other species (xenotopic expression). Although far from the clinic, these approaches show promise. Similarly, nuclear transfection with genes encoding restriction endonucleases or sequence-specific zinc finger-binding proteins destined for mitochondria has also proved successful in targeting mtDNA-borne pathogenic mutations. This is particularly important, as mutated mtDNA is often found in cells that also contain normal copies of the genome, a situation termed heteroplasmy. Shifting the levels of heteroplasmy towards the normal mtDNA has become the goal of a variety of invasive and non-invasive methods, which are also highlighted in this review.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
McFarland R, Taylor RW, Turnbull DM . Mitochondrial disease—its impact, aetiology, and pathology. Curr Top Dev Biol 2007; 77: 113–155.
Nagley P, Farrell LB, Gearing DP, Nero D, Meltzer S, Devenish RJ . Assembly of functional proton-translocating ATPase complex in yeast mitochondria with cytoplasmically synthesized subunit 8, a polypeptide normally encoded within the organelle. Proc Natl Acad Sci USA 1988; 85: 2091–2095.
Bokori-Brown M, Holt IJ . Expression of algal nuclear ATP synthase subunit 6 in human cells results in protein targeting to mitochondria but no assembly into ATP synthase. Rejuvenation Res 2006; 9: 455–469.
Kaltimbacher V, Bonnet C, Lecoeuvre G, Forster V, Sahel JA, Corral-Debrinski M . mRNA localization to the mitochondrial surface allows the efficient translocation inside the organelle of a nuclear recoded ATP6 protein. RNA 2006; 12: 1408–1417.
Bonnet C, Kaltimbacher V, Ellouze S, Augustin S, Benit P, Forster V et al. Allotopic mRNA localization to the mitochondrial surface rescues respiratory chain defects in fibroblasts harboring mitochondrial DNA mutations affecting complex I or V subunits. Rejuvenation Res 2007; 10: 127–144.
Hakkaart GA, Dassa EP, Jacobs HT, Rustin P . Allotopic expression of a mitochondrial alternative oxidase confers cyanide resistance to human cell respiration. EMBO Rep 2006; 7: 341–345.
Seo BB, Nakamaru-Ogiso E, Flotte TR, Matsuno-Yagi A, Yagi T . In vivo complementation of complex I by the yeast Ndi1 enzyme. Possible application for treatment of Parkinson disease. J Biol Chem 2006; 281: 14250–14255.
Marella M, Seo BB, Nakamaru-Ogiso E, Greenamyre JT, Matsuno-Yagi A, Yagi T . Protection by the NDI1 gene against neurodegeneration in a rotenone rat model of Parkinson's disease. PLoS ONE 2008; 3: e1433.
Tarassov I, Kamenski P, Kolesnikova O, Karicheva O, Martin RP, Krasheninnikov IA et al. Import of nuclear DNA-encoded RNAs into mitochondria and mitochondrial translation. Cell Cycle 2007; 6: 2473–2477.
Mukherjee S, Basu S, Home P, Dhar G, Adhya S . Necessary and sufficient factors for the import of transfer RNA into the kinetoplast mitochondrion. EMBO Rep 2007; 8: 589–595.
Mahata B, Mukherjee S, Mishra S, Bandyopadhyay A, Adhya S . Functional delivery of a cytosolic tRNA into mutant mitochondria of human cells. Science 2006; 314: 471–474.
Mukherjee S, Mahata B, Mahato B, Adhya S . Targeted mRNA degradation by complex-mediated delivery of antisense RNAs to intracellular human mitochondria. Hum Mol Genet 2008; 17: 1292–1298.
Koulintchenko M, Temperley RJ, Mason PA, Dietrich A, Lightowlers RN . Natural competence of mammalian mitochondria allows the molecular investigation of mitochondrial gene expression. Hum Mol Genet 2006; 15: 143–154.
Katrangi E, D'Souza G, Boddapati SV, Kulawiec M, Singh KK, Bigger B et al. Xenogenic transfer of isolated murine mitochondria into human rho(0) cells can improve respiratory function. Rejuvenation Res 2007; 10: 561–570.
Yamada Y, Akita H, Kamiya H, Kogure K, Yamamoto T, Shinohara Y et al. MITO-Porter: a liposome-based carrier system for delivery of macromolecules into mitochondria via membrane fusion. Biochim Biophys Acta 2008; 1778: 423–432.
Taivassalo T, Gardner JL, Taylor RW, Schaefer AM, Newman J, Barron MJ et al. Endurance training and detraining in mitochondrial myopathies due to single large-scale mtDNA deletions. Brain 2006; 129 (Part 12): 3391–3401.
Taivassalo T, Gardner JL, Taylor RW, Schaefer AM, Haller RG, Turnbull DM . Resistance exercise training in mitochondrial myopathy due to single, large-scale mtDNA deletions: implications for therapy. Neuromuscul Disord 2007; 17: 829.
Bacman SR, Williams SL, Hernandez D, Moraes CT . Modulating mtDNA heteroplasmy by mitochondria-targeted restriction endonucleases in a ‘differential multiple cleavage-site’ model. Gene Ther 2007; 14: 1309–1318.
Minczuk M, Papworth MA, Kolasinska P, Murphy MP, Klug A . Sequence-specific modification of mitochondrial DNA using a chimeric zinc finger methylase. Proc Natl Acad Sci USA 2006; 103: 19689–19694.
Brown DT, Herbert M, Lamb VK, Chinnery PF, Taylor RW, Lightowlers RN et al. Transmission of mitochondrial DNA disorders: possibilities for the future. Lancet 2006; 368: 87–89.
Sato A, Kono T, Nakada K, Ishikawa K, Inoue S, Yonekawa H et al. Gene therapy for progeny of mito-mice carrying pathogenic mtDNA by nuclear transplantation. Proc Natl Acad Sci USA 2005; 102: 16765–16770.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kyriakouli, D., Boesch, P., Taylor, R. et al. Progress and prospects: gene therapy for mitochondrial DNA disease. Gene Ther 15, 1017–1023 (2008). https://doi.org/10.1038/gt.2008.91
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/gt.2008.91
Keywords
This article is cited by
-
Manipulation of mtDNA heteroplasmy in all striated muscles of newborn mice by AAV9-mediated delivery of a mitochondria-targeted restriction endonuclease
Gene Therapy (2012)
-
Dual Function MITO-Porter, a Nano Carrier Integrating Both Efficient Cytoplasmic Delivery and Mitochondrial Macromolecule Delivery
Molecular Therapy (2011)
-
DNA Delivery to Mitochondria: Sequence Specificity and Energy Enhancement
Pharmaceutical Research (2011)
-
Mitochondrial medicine: to a new era of gene therapy for mitochondrial DNA mutations
Journal of Inherited Metabolic Disease (2011)
-
Trial and Error: How the Unclonable Human Mitochondrial Genome was Cloned in Yeast
Pharmaceutical Research (2011)