Abstract
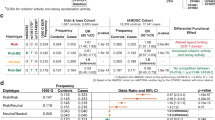
Complement factor H (CFH) is a key regulator of the alternative pathway of complement and its mutations have been associated with membranoproliferative glomerulonephritis type II, atypical hemolytic uremic syndrome and age-related macular degeneration (AMD), suggesting that alternative pathway dysregulation is a common pathogenetic feature of these ocular and renal conditions. In this study we tested the hypothesis that common CFH variants have a global role in renal function in the Australian population-based Blue Mountains Eye Study (BMES). We replicated the association of I62V with estimated glomerular filtration rate (GFR; P=0.017) and creatinine clearance (CRCL; P=0.015). The minor allele of I62V (G) was deleterious: adding one copy of the G allele decreased GFR/CRCL by ∼0.98 ml min−1 per 1.73 m2 (95% confidence interval (CI): 0.97, 0.99). We also replicated the association of Y402H with AMD and provided an unbiased estimate of population attributable risk (PAR). The minor allele of Y402H (C) was deleterious: the odds ratio estimate of CC genotype compared to TT was 1.87 (95% CI: 1.44, 2.45). The PAR of the C allele was estimated as 0.22 (95% CI: 0.15, 0.28). In summary, in the BMES population we confirmed the association between I62V and renal function, as measured by the estimated GFR, plus the association of Y402H with both early- and late-stage AMD.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 digital issues and online access to articles
$119.00 per year
only $19.83 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Alexander JJ, Quigg RJ . The simple design of complement factor H: looks can be deceiving. Mol Immunol 2007; 44: 123–132.
Rodriguez de Cordoba S, Esparza-Gordillo J, Goicoechea de Jorge E, Lopez-Trascasa M, Sanchez-Corral P . The human complement factor H: functional roles, genetic variations and disease associations. Mol Immunol 2004; 41: 355–367.
Zipfel PF, Heinen S, Jozsi M, Skerka C . Complement and diseases: defective alternative pathway control results in kidney and eye diseases. Mol Immunol 2006; 43: 97–106.
Colville D, Guymer R, Sinclair RA, Savige J . Visual impairment caused by retinal abnormalities in mesangiocapillary (membranoproliferative) glomerulonephritis type II (‘dense deposit disease’). Am J Kidney Dis 2003; 42: E2–E5.
Duvall-Young J, MacDonald MK, McKechnie NM . Fundus changes in (type II) mesangiocapillary glomerulonephritis simulating drusen: a histopathological report. Br J Ophthalmol 1989; 73: 297–302.
Duvall-Young J, Short CD, Raines MF, Gokal R, Lawler W . Fundus changes in mesangiocapillary glomerulonephritis type II: clinical and fluorescein angiographic findings. Br J Ophthalmol 1989; 73: 900–906.
Mullins RF, Aptsiauri N, Hageman GS . Structure and composition of drusen associated with glomerulonephritis: implications for the role of complement activation in drusen biogenesis. Eye 2001; 15: 390–395.
Mullins RF, Russell SR, Anderson DH, Hageman GS . Drusen associated with aging and age-related macular degeneration contain proteins common to extracellular deposits associated with atherosclerosis, elastosis, amyloidosis, and dense deposit disease. FASEB J 2000; 14: 835–846.
Abrera-Abeleda MA, Nishimura C, Smith JL, Sethi S, McRae JL, Murphy BF et al. Variations in the complement regulatory genes factor H (CFH) and factor H related 5 (CFHR5) are associated with membranoproliferative glomerulonephritis type II (dense deposit disease). J Med Genet 2006; 43: 582–589.
Hageman GS, Anderson DH, Johnson LV, Hancox LS, Taiber AJ, Hardisty LI et al. A common haplotype in the complement regulatory gene factor H (HF1/CFH) predisposes individuals to age-related macular degeneration. Proc Natl Acad Sci USA 2005; 102: 7227–7232.
Pickering MC, de Jorge EG, Martinez-Barricarte R, Recalde S, Garcia-Layana A, Rose KL et al. Spontaneous hemolytic uremic syndrome triggered by complement factor H lacking surface recognition domains. J Exp Med 2007; 204: 1249–1256.
Saunders RE, Abarrategui-Garrido C, Fremeaux-Bacchi V, Goicoechea de Jorge E, Goodship TH, Lopez Trascasa M et al. The interactive factor H-atypical hemolytic uremic syndrome mutation database and website: update and integration of membrane cofactor protein and factor I mutations with structural models. Hum Mutat 2007; 28: 222–234.
Saunders RE, Goodship TH, Zipfel PF, Perkins SJ . An interactive web database of factor H-associated hemolytic uremic syndrome mutations: insights into the structural consequences of disease-associated mutations. Hum Mutat 2006; 27: 21–30.
Ferreira VP, Herbert AP, Hocking HG, Barlow PN, Pangburn MK . Critical role of the C-terminal domains of factor H in regulating complement activation at cell surfaces. J Immunol 2006; 177: 6308–6316.
Giannakis E, Jokiranta TS, Male DA, Ranganathan S, Ormsby RJ, Fischetti VA et al. A common site within factor H SCR 7 responsible for binding heparin, C-reactive protein and streptococcal M protein. Eur J Immunol 2003; 33: 962–969.
Herbert AP, Uhrin D, Lyon M, Pangburn MK, Barlow PN . Disease-associated sequence variations congregate in a polyanion recognition patch on human factor H revealed in three-dimensional structure. J Biol Chem 2006; 281: 16512–16520.
Perkins SJ, Goodship TH . Molecular modelling of the C-terminal domains of factor H of human complement: a correlation between haemolytic uraemic syndrome and a predicted heparin binding site. J Mol Biol 2002; 316: 217–224.
Edwards AO, Ritter III R, Abel KJ, Manning A, Panhuysen C, Farrer LA . Complement factor H polymorphism and age-related macular degeneration. Science 2005; 308: 421–424.
Haines JL, Hauser MA, Schmidt S, Scott WK, Olson LM, Gallins P et al. Complement factor H variant increases the risk of age-related macular degeneration. Science 2005; 308: 419–421.
Klein RJ, Zeiss C, Chew EY, Tsai JY, Sackler RS, Haynes C et al. Complement factor H polymorphism in age-related macular degeneration. Science 2005; 308: 385–389.
Neary JJ, Conlon PJ, Croke D, Dorman A, Keogan M, Zhang FY et al. Linkage of a gene causing familial membranoproliferative glomerulonephritis type III to chromosome 1. J Am Soc Nephrol 2002; 13: 2052–2057.
Tsukaguchi H, Yager H, Dawborn J, Jost L, Cohlmia J, Abreu PF et al. A locus for adolescent and adult onset familial focal segmental glomerulosclerosis on chromosome 1q25–31. J Am Soc Nephrol 2000; 11: 1674–1680.
Fuchshuber A, Jean G, Gribouval O, Gubler MC, Broyer M, Beckmann JS et al. Mapping a gene (SRN1) to chromosome 1q25–q31 in idiopathic nephrotic syndrome confirms a distinct entity of autosomal recessive nephrosis. Hum Mol Genet 1995; 4: 2155–2158.
Vollmer M, Jung M, Ruschendorf F, Ruf R, Wienker T, Reis A et al. The gene for human fibronectin glomerulopathy maps to 1q32, in the region of the regulation of complement activation gene cluster. Am J Hum Genet 1998; 63: 1724–1731.
Alexander JJ, Wang Y, Chang A, Jacob A, Minto AW, Karmegam M et al. Mouse podocyte complement factor H: the functional analog to human complement receptor 1. J Am Soc Nephrol 2007; 18: 1157–1166.
Hogasen K, Jansen JH, Mollnes TE, Hovdenes J, Harboe M . Hereditary porcine membranoproliferative glomerulonephritis type II is caused by factor H deficiency. J Clin Invest 1995; 95: 1054–1061.
Pickering MC, Cook HT, Warren J, Bygrave AE, Moss J, Walport MJ et al. Uncontrolled C3 activation causes membranoproliferative glomerulonephritis in mice deficient in complement factor H. Nat Genet 2002; 31: 424–428.
Liew G, Mitchell P, Wong TY, Iyengar SK, Wang JJ . CKD increases the risk of age-related macular degeneration. J Am Soc Nephrol 2008; 23 [e-pub ahead of print].
Fox CS, Yang Q, Cupples LA, Guo CY, Larson MG, Leip EP et al. Genomewide linkage analysis to serum creatinine, GFR, and creatinine clearance in a community-based population: the Framingham Heart Study. J Am Soc Nephrol 2004; 15: 2457–2461.
Hunt SC, Coon H, Hasstedt SJ, Cawthon RM, Camp NJ, Wu LL et al. Linkage of serum creatinine and glomerular filtration rate to chromosome 2 in Utah pedigrees. Am J Hypertens 2004; 17: 511–515.
Thompson CL, Klein BE, Klein R, Xu Z, Caprioli J, Joshi T et al. Complement factor H and hemicentin-1 in age-related macular degeneration and renal phenotypes. Hum Mol Genet 2007; 16: 2135–2148.
International HapMap Consortium. A haplotype map of the human genome. Nature 2005; 437: 1299–1320.
Fisher RA . Combining independent tests of significance. Am Statist 1948; 2: 30.
Cockcroft DW, Gault MH . Prediction of creatinine clearance from serum creatinine. Nephron 1976; 16: 31–41.
Levey AS, Bosch JP, Lewis JB, Greene T, Rogers N, Roth D . A more accurate method to estimate glomerular filtration rate from serum creatinine: a new prediction equation. Modification of Diet in Renal Disease Study Group. Ann Intern Med 1999; 130: 461–470.
Lin J, Knight EL, Hogan ML, Singh AK . A comparison of prediction equations for estimating glomerular filtration rate in adults without kidney disease. J Am Soc Nephrol 2003; 14: 2573–2580.
Poggio ED, Wang X, Greene T, Van Lente F, Hall PM . Performance of the modification of diet in renal disease and Cockcroft–Gault equations in the estimation of GFR in health and in chronic kidney disease. J Am Soc Nephrol 2005; 16: 459–466.
Caprioli J, Castelletti F, Bucchioni S, Bettinaglio P, Bresin E, Pianetti G et al. Complement factor H mutations and gene polymorphisms in haemolytic uraemic syndrome: the C-257T, the A2089G and the G2881T polymorphisms are strongly associated with the disease. Hum Mol Genet 2003; 12: 3385–3395.
Neumann HP, Salzmann M, Bohnert-Iwan B, Mannuelian T, Skerka C, Lenk D et al. Haemolytic uraemic syndrome and mutations of the factor H gene: a registry-based study of German speaking countries. J Med Genet 2003; 40: 676–681.
Baird PN, Islam FM, Richardson AJ, Cain M, Hunt N, Guymer R . Analysis of the Y402H variant of the complement factor H gene in age-related macular degeneration. Invest Ophthalmol Vis Sci 2006; 47: 4194–4198.
Despriet DD, Klaver CC, Witteman JC, Bergen AA, Kardys I, de Maat MP et al. Complement factor H polymorphism, complement activators, and risk of age-related macular degeneration. JAMA 2006; 296: 301–309.
Fisher SA, Rivera A, Fritsche LG, Babadjanova G, Petrov S, Weber BH . Assessment of the contribution of CFH and chromosome 10q26 AMD susceptibility loci in a Russian population isolate. Br J Ophthalmol 2007; 91: 576–578.
Magnusson KP, Duan S, Sigurdsson H, Petursson H, Yang Z, Zhao Y et al. CFH Y402H confers similar risk of soft drusen and both forms of advanced AMD. PLoS Med 2006; 3: e5.
Conley YP, Jakobsdottir J, Mah T, Weeks DE, Klein R, Kuller L et al. CFH, ELOVL4, PLEKHA1 and LOC387715 genes and susceptibility to age-related maculopathy: AREDS and CHS cohorts and meta-analyses. Hum Mol Genet 2006; 15: 3206–3218.
Schaumberg DA, Christen WG, Kozlowski P, Miller DT, Ridker PM, Zee RY . A prospective assessment of the Y402H variant in complement factor H, genetic variants in C-reactive protein, and risk of age-related macular degeneration. Invest Ophthalmol Vis Sci 2006; 47: 2336–2340.
Levin ML . The occurrence of lung cancer in man. Acta Unio Int Contra Cancrum 1953; 9: 531–541.
Rockhill B, Newman B, Weinberg C . Use and misuse of population attributable fractions. Am J Public Health 1998; 88: 15–19.
Chamberlain M, Baird P, Dirani M, Guymer R . Unraveling a complex genetic disease: age-related macular degeneration. Surv Ophthalmol 2006; 51: 576–586.
Dewan A, Liu M, Hartman S, Zhang SS, Liu DT, Zhao C et al. HTRA1 promoter polymorphism in wet age-related macular degeneration. Science 2006; 314: 989–992.
Gold B, Merriam JE, Zernant J, Hancox LS, Taiber AJ, Gehrs K et al. Variation in factor B (BF) and complement component 2 (C2) genes is associated with age-related macular degeneration. Nat Genet 2006; 38: 458–462.
Hughes AE, Orr N, Esfandiary H, Diaz-Torres M, Goodship T, Chakravarthy U . A common CFH haplotype, with deletion of CFHR1 and CFHR3, is associated with lower risk of age-related macular degeneration. Nat Genet 2006; 38: 1173–1177.
Li M, Atmaca-Sonmez P, Othman M, Branham KE, Khanna R, Wade MS et al. CFH haplotypes without the Y402H coding variant show strong association with susceptibility to age-related macular degeneration. Nat Genet 2006; 38: 1049–1054.
Maller J, George S, Purcell S, Fagerness J, Altshuler D, Daly MJ et al. Common variation in three genes, including a noncoding variant in CFH, strongly influences risk of age-related macular degeneration. Nat Genet 2006; 38: 1055–1059.
Maller JB, Fagerness JA, Reynolds RC, Neale BM, Daly MJ, Seddon JM . Variation in complement factor 3 is associated with risk of age-related macular degeneration. Nat Genet 2007; 39: 1200–1201.
Yang Z, Camp NJ, Sun H, Tong Z, Gibbs D, Cameron DJ et al. A variant of the HTRA1 gene increases susceptibility to age-related macular degeneration. Science 2006; 314: 992–993.
Mitchell P, Smith W, Attebo K, Wang JJ . Prevalence of age-related maculopathy in Australia. The Blue Mountains Eye Study. Ophthalmology 1995; 102: 1450–1460.
Levey AS, Coresh J, Balk E, Kausz AT, Levin A, Steffes MW et al. National Kidney Foundation practice guidelines for chronic kidney disease: evaluation, classification, and stratification. Ann Intern Med 2003; 139: 137–147.
Klein R, Davis MD, Magli YL, Segal P, Klein BE, Hubbard L . The Wisconsin age-related maculopathy grading system. Ophthalmology 1991; 98: 1128–1134.
Bird AC, Bressler NM, Bressler SB, Chisholm IH, Coscas G, Davis MD et al. An international classification and grading system for age-related maculopathy and age-related macular degeneration. The International ARM Epidemiological Study Group. Surv Ophthalmol 1995; 39: 367–374.
Liang KY, Zeger SL . Longitudinal data analysis for discrete and continuous outcomes. Biometrics 1986; 42: 121–130.
McPeek MS, Wu X, Ober C . Best linear unbiased allele-frequency estimation in complex pedigrees. Biometrics 2004; 60: 359–367.
SAS Institute. SAS Guide for Personal Computers: Version 9.1.3. SAS Institute: Cary, NC, 2006.
Barrett JC, Fry B, Maller J, Daly MJ . Haploview: analysis and visualization of LD and haplotype maps. Bioinformatics 2005; 21: 263–265.
Browning SR, Briley JD, Briley LP, Chandra G, Charnecki JH, Ehm MG et al. Case–control single-marker and haplotypic association analysis of pedigree data. Genet Epidemiol 2005; 28: 110–122.
Schaid DJ, Rowland CM, Tines DE, Jacobson RM, Poland GA . Score tests for association between traits and haplotypes when linkage phase is ambiguous. Am J Hum Genet 2002; 70: 425–434.
Acknowledgements
We thank the two anonymous reviewers for their insightful comments that led to great improvements in this article. This study was supported, in part, by US Public Health Service research grants GM28356, from the National Institute of General Medical Sciences, grant EY015810 from the National Eye Institute, and grants 974159 and 211069 from NHMRC.
Author information
Authors and Affiliations
Corresponding author
Additional information
Statement of competing financial interests
The authors have no competing conflicts of interests, financial or otherwise, to declare.
Rights and permissions
About this article
Cite this article
Xing, C., Sivakumaran, T., Wang, J. et al. Complement factor H polymorphisms, renal phenotypes and age-related macular degeneration: the Blue Mountains Eye Study. Genes Immun 9, 231–239 (2008). https://doi.org/10.1038/gene.2008.10
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/gene.2008.10