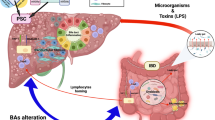
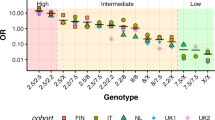
Abstract
CCR5 plays a key role in the distribution of CD45RO+ T cells and contributes to generation of a T helper 1 immune response. CCR5-Δ32 is a 32-bp deletion associated with significant reduction in cell surface expression of the receptor. We investigated the role of CCR5-Δ32 on susceptibility to ulcerative colitis (UC), Crohn's disease (CD) and primary sclerosing cholangitis (PSC). Genotype and allelic association analyses were performed in 162 patients with UC, 131 with CD, 71 with PSC and 419 matched controls. There was a significant difference in CCR5 genotype (OR 2.27, P=0.003) between patients with sclerosing cholangitis and controls. Similarly, CCR5-Δ32 allele frequency was significantly higher in sclerosing cholangitis (17.6%) compared to controls (9.9%, OR 2.47, P=0.007) and inflammatory bowel disease patients without sclerosing cholangitis (11.3%, OR 1.9, P=0.027). There were no significant differences in CCR5 genotype or allele frequency between those with either UC or CD and controls. Genotypes with the CCR5-Δ32 variant were increased in patients with severe liver disease defined by portal hypertension and/or transplantation (45%) compared to those with mild liver disease (21%, OR 3.17, P=0.03). The CCR5-Δ32 mutation may influence disease susceptibility and severity in patients with PSC.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 digital issues and online access to articles
$119.00 per year
only $19.83 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Montgomery SM, Morris DL, Thompson NP, Subhani J, Pounder RE, Wakefield AJ . Prevalence of inflammatory bowel disease in British 26 year olds: national longitudinal birth cohort. Br Med J 1998; 316: 1058–1059.
Podolsky DK . Inflammatory bowel disease (1). N Engl J Med 1991; 325: 928–937.
Shanahan F . Crohn's disease. Lancet 2002; 359: 62–69.
Thoree VC, Golby SJ, Boursier L et al. Related IgA1 and IgG-producing cells in blood and diseased mucosa in ulcerative colitis. Gut 2002; 51: 44–50.
Chapman RW . Aetiology and natural history of primary sclerosing cholangitis: a decade of progress? Gut 1991; 32: 1433–1435.
Broome U, Olsson R, Loof L et al. Natural history and prognostic factors in 305 Swedish patients with primary sclerosing cholangitis. Gut 1990; 31: 961–963.
Snook J . Are the inflammatory bowel diseases autoimmune disorders? Gut 1990; 31: 961–963.
Radford-Smith GL . Ulcerative colitis—an immunological disease? Bailliers Clin Gastroenterol 1997; 11: 35–52.
Hugot JP, Chamaillard M, Zouali H et al. Association of NOD2 leucine-rich repeat variants with susceptibility to Crohn's disease. Nature 2001; 411: 599–603.
Ogura Y, Bonen DK, Inohara N et al. A frameshift mutation in NOD2 associated with susceptibility to Crohn's disease. Nature 2001; 411: 603–606.
Satsangi J, Welsh KI, Bunce M et al. Contribution of genes of the major histocompatibility complex to susceptibility and disease phenotype in inflammatory bowel disease. Lancet 1996; 347: 1212–1217.
Mitchell SA, Grove J, Spurkland A et al. Association of the tumour necrosis factor alpha –308 but not the interleukin 10–627 promoter polymorphism with genetic susceptibility to primary sclerosing cholangitis. Gut 2001; 49: 288–294.
Satsangi J, Chapman RW, Haldar N et al. A functional polymorphism of the stromelysin gene (MMP-3) influences susceptibility to primary sclerosing cholangitis. Gastroenterology 2001; 121: 124–130.
Mackay CR . Chemokines: immunology's high impact factors. Nat Immunol 2001; 2: 95–101.
Gerard C, Rollins BJ . Chemokines and disease. Nat Immunol 2001; 2: 108–115.
Dwinell MB, Eckmann L, Leopard JD, Varki NM, Kagnoff MF . Chemokine receptor expression by human intestinal epithelial cells. Gastroenterology 1999; 2: 359–367.
Agace WW, Roberts I, Wu L, Greinede C, Ebert EC, Parker CM . Human intestinal lamina propria and intraepithelial lymphocytes express receptors specific for chemokines induced by inflammation. Eur J Immunol 2000; 30: 819–826.
Shields PL, Morland CM, Salmon M, Qin S, Hubscher SG, Adams DH . Chemokine and chemokine receptor interactions provide a mechanism for selective T cell recruitment to specific liver compartments within hepatitis C-infected liver. J Immunol 1999; 163: 6236–6243.
Venkatesan S, Petrovic A, Van Ryk DI, Locati M, Weissman D, Murphy PM . Reduced cell surface expression of CCR5 in CCR5Delta 32 heterozygotes is mediated by gene dosage, rather than by receptor sequestration. J Biol Chem 2001; 277: 2287–2301.
Blanpain C, Lee B, Tackoen M et al. Multiple nonfunctional alleles of CCR5 are frequent in various human populations. Blood 2000; 96: 1638–1645.
Stephens JC, Reich DE, Goldstein DB et al. Dating the origin of the CCR5-Delta32 AIDS-resistance allele by the coalescence of haplotypes. Am J Hum Genet 1998; 62: 1507–1515.
Dean M, Carrington M, Winkler C et al. Genetic restriction of HIV-1 infection and progression to AIDS by a deletion allele of the CKR5 structural gene. Science 1996; 273: 1856–1862.
Huang Y, Paxton WA, Wolinsky SM et al. The role of a mutant CCR5 allele in HIV-1 transmission and disease progression. Nat Med 1996; 3: 252–253.
Zimmerman PA, Buckler-White A, Alkhatib G et al. Inherited resistance to HIV-1 conferred by an inactivating mutation in CC chemokine receptor 5: studies in populations with contrasting clinical phenotypes, defined racial background, and quantified risk. Mol Med 1997; 3: 23–36.
Marmor M, Sheppard HW, Donnell D et al. Homozygous and heterozygous CCR5-Delta32 genotypes are associated with resistance to HIV infection. J Acquir Immune Defic Syndr 2001; 27: 472–481.
Gomez-Reino JJ, Pablos JL, Carreira PE et al. Association of rheumatoid arthritis with a functional chemokine receptor, CCR5. Arthritis Rheum 1999; 42: 989–992.
Barcellos LF, Schito AM, Rimmler J et al. CC-chemokine receptor 5 polymorphism and age of onset in familial multiple sclerosis. Immunogenetics 2000; 51: 281–288.
Sellebjerg F, Madsen HO, Jensen CV, Jensen J, Garred P . CCR5 delta32, matrix metalloproteinase-9 and disease activity in multiple sclerosis. J Neuroimmunol 2000; 102: 98–106.
Rector A, Vermeire S, Thoelen I et al. Analysis of the CC chemokine receptor 5 (CCR5) delta-32 polymorphism in inflammatory bowel disease. Hum Genet 2001; 180: 190–193.
Craggs A, Welfare M, Donaldson PT, Mansfield JC . The CC chemokine receptor 5 delta32 mutation is not associated with inflammatory bowel disease (IBD) in NE England. Genes Immun 2001; 2: 114–116.
Martin K, Heinzlmann M, Borchers R, Mack M, Loeschke K, Folwaczny C . Delta 32 mutation of the chemokine-receptor 5 gene in inflammatory bowel disease. Clin Immunol 2001; 98: 18–22.
Herfarth H, Pollok-Kopp B, Goke M, Press A, Oppermann M . Polymorphism of CC chemokine receptors CCR2 and CCR5 in Crohn's disease. Immunol Lett 2001; 77: 113–117.
Hampe J, Lynch NJ, Daniels S et al. Fine mapping of the chromosome 3p susceptibility locus in inflammatory bowel disease. Gut 2001; 48: 191–197.
Paavola P, Helio T, Kiuru M et al. Genetic analysis in Finnish families with inflammatory bowel disease supports linkage to chromosome 3p21. Eur J Hum Genet 2001; 9: 328–334.
Donaldson PT, Agarwal K, Saarinen S et al. Investigation of CCR5-Δ32 deletion and Fas/Apo-1 (CD95) single nucleotide polymorphisms in primary sclerosing cholangitis (PSC). Hepatology 2000; 32: 174A.
Satsangi J, Simmons J, Marshall S et al. CCR5-Δ32 polymorphism in inflammatory bowel disease: further association with ulcerative colitis and with primary sclerosing cholangitis. Gastroenterology 2000; 118: A337.
Fausa O, Schrumpf E, Elgjo K . Relationship of inflammatory bowel disease and primary sclerosing cholangitis. Semin Liver Dis 1991; 11: 31–39.
Boberg KM, Schrumpf E, Fausa O et al. Hepatobiliary disease in ulcerative colitis. An analysis of 18 patients with hepatobiliary lesions classified as small-duct primary sclerosing cholangitis. Scand J Gastroenterol 1994; 29: 744–752.
Sandborn WJ, Loftus Jr EV, Ahlquist DA . Association of primary sclerosing cholangitis and colorectal cancer in patients with ulcerative colitis: is it true and does it matter? Gastroenterology 1998; 115: 236–237.
Loetscher P, Uguccioni M, Bordoli L et al. CCR5 is characteristic of Th1 lymphocytes. Nature 1998; 391: 344–345.
Qin S, Rottman JB, Myers P et al. The chemokine receptors CXCR3 and CCR5 mark subsets of T cells associated with certain inflammatory reactions. J Clin Invest 1998; 101: 746–754.
Andres PG, Beck PL, Mizoguchi A et al. Mice with a selective deletion of the CC chemokine receptors 5 and 2 are protected from dextran sodium sulfate-mediated colitis: lack of CC chemokine receptor 5 expression results in an NK1.1+lymphocyte-associated Th2 type immune response in the intestine. J Immunol 2000; 164: 6303–6312.
Saarinen S, Olerup O, Broome U . Increased frequencies of autoimmune diseases in patients with with primary sclerosing cholangitis. Am J Gastroenterol 2000; 95: 3195–3199.
Chapman RW, Cottone M, Selby WS, Shepherd HA, Sherlock S, Jewell DP . Serum autoantibodies, ulcerative colitis and primary sclerosing cholangitis. Gut 1986; 27: 86–91.
Schrumpf E, Gjone E . Hepatobiliary disease in ulcerative colitis. Scand J Gastroenterol 1982; 17: 961–964.
Chapman RW, Varghese Z, Gaul R, Patel G, Kokinon N, Sherlock S . Association of primary sclerosing cholangitis with HLA-B8. Gut 1983; 24: 38–41.
Zhou Y, Kurihara T, Ryseck RP et al. Impaired macrophage function and enhanced T cell-dependent immune response in mice lacking CCR5, the mouse homologue of the major HIV-1 coreceptor. J Immunol 1998; 160: 4018–4025.
Afford SC, Fisher NC, Neil DA et al. Distinct patterns of chemokine expression are associated with leukocyte recruitment in alcoholic hepatitis and alcoholic cirrhosis. J Pathol 1998; 186: 82–89.
Goddard S, Williams A, Morland C et al. Differential expression of chemokines and chemokine receptors shapes the inflammatory response in rejecting human liver transplants. Transplantation 2001; 72: 1957–1967.
Bjornsson E, Boberg KM, Cullen S et al. Patients with small duct primary sclerosing cholangitis have a favourable long term prognosis. Gut 2002; 51: 731–735.
Boberg KM, Spurkland A, Rocca G et al. The HLA-DR3, DQ2 heterozygous genotype is associated with an accelerated progression of primary sclerosing cholangitis. Scand J Gastroenterol 2001; 36: 886–890.
Hellier S, Frodsham AJ, Hennig BJ et al. Association of genetic variants of the chemokine receptor CCR5 and its ligands, RANTES and MCP-2, with outcome of HCV infection. Hepatology 2003; 38: 1468–1476.
Promrat K, McDermott DH, Gonzalez CM et al. Association of chemokine system polymorphisms with clinical outcomes and treatment responses of chronic hepatitis C. Gastroenterology 2003; 124: 352–360.
Wasmuth HE, Werth A, Mueller T et al. CC chemokine receptor 5 Delta32 polymorphism in two independent cohorts of hepatitis C virus infected patients without hemophilia. J Mol Med 2004; 82: 64–69.
Moench C, Uhrig A, Lohse AW, Otto G . CC chemokine receptor 5 Delta32 polymorphism—a risk factor for ischaemic-type biliary lesions following orthotopic liver transplantation. Liver Transplant 2004; 10: 434–439.
Lennard-Jones JE . Classification of inflammatory bowel disease. Scand J Gastroenterol Suppl 1989; 170: 2–6.
Miller SA, Dykes DD, Polesky HF . A simple salting out procedure for extracting DNA from human nucleated cells. Nucleic Acids Res 1988; 16: 1215.
Levi S, Urbano-Ispizua A, Gill R et al. Multiple K-ras codon 12 mutations in cholangiocarcinomas demonstrated with a sensitive polymerase chain reaction technique. Cancer Res 1991; 51: 3497–3502.
Raport CJ, Gosling J, Schweickart VL, Gray PW, Charo IF . Molecular cloning and functional characterization of a novel human CC chemokine receptor (CCR5) for RANTES, MIP-1beta, and MIP-1alpha. J Biol Chem 1996; 271: 17161–17166.
Acknowledgements
Dr Eri was funded by a research grant from the Queensland Cancer Fund (2000–2002). The Brisbane IBD Research Group's database is supported by an educational grant from Pfizer Australia.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Eri, R., Jonsson, J., Pandeya, N. et al. CCR5-Δ32 mutation is strongly associated with primary sclerosing cholangitis. Genes Immun 5, 444–450 (2004). https://doi.org/10.1038/sj.gene.6364113
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.gene.6364113
Keywords
This article is cited by
-
A genome-wide CRISPR screen identifies a restricted set of HIV host dependency factors
Nature Genetics (2017)
-
The immunobiology of primary sclerosing cholangitis
Seminars in Immunopathology (2009)
-
Sclerosing Cholangitis Epidemiology and Etiology
Journal of Gastrointestinal Surgery (2008)
-
Variants of CCR5, which are permissive for HIV-1 infection, show distinct functional responses to CCL3, CCL4 and CCL5
Genes & Immunity (2005)