Abstract
Fibroblast growth factors (FGF) regulate bone growth, but their expression in human cartilage is unclear. Here, we determined the expression of entire FGF family in human fetal growth plate cartilage. Using reverse transcriptase PCR, the transcripts for FGF1, 2, 5, 8–14, 16–19, and 21 were found. However, only FGF1, 2, 17, and 19 were detectable at the protein level. By immunohistochemistry, FGF17 and 19 were uniformly expressed within the growth plate. In contrast, FGF1 was found only in proliferating and hypertrophic chondrocytes whereas FGF2 localized predominantly to the resting and proliferating cartilage. In addition, only the 18 kD isoform of FGF2 was found in resting chondrocytes while proliferating chondrocytes also synthesized 22 kD and 24 kD FGF2, similar to in vitro cultivated chondrocytes. In cell growth experiments, FGF1, 2, and 17 but not FGF19 inhibited the proliferation of FGFR3-expressing rat chondrosarcoma chondrocytes (RCS) with relative potency FGF2 ≫ FGF1 = FGF17. We conclude that FGF1, 2, 17, and 19 are the predominant FGF ligands present in developing human cartilage that are, with the exception of FGF19, experimentally capable of inhibiting chondrocyte proliferation.
Similar content being viewed by others
Main
The human FGF family consists of 22 proteins that signal via FGFR1–5. Several forms of human dwarfism are caused by activating mutations in FGFR3, demonstrating the important role of FGF signaling in endochondral bone growth. Mutations in the extracellular domain, transmembrane domain, or kinase domain of FGFR3 result in short stature syndromes, with graded severity ranging from the mildest disorder, hypochondroplasia, to lethal TD (1).
In vitro studies utilizing mutated FGFR3 expressed in model cell lines show that mutations activate FGFR3 in a constitutive, ligand-independent fashion (2,3). However, receptor activity may be affected by the existing FGF background. For instance, phosphorylation of FGFR3 was increased by ligand binding in cells harboring achondroplasia (G380R) or TD (K650E) mutations (4–6). When expressed at physiologic levels, FGFR3-G380R required, like its wild-type counterpart, ligand for activation (7). Similarly, in vitro cultivated human TD chondrocytes as well as chondrocytes isolated from Fgfr3-K644M mice had an identical time course of Fgfr3 activation compared with wild-type chondrocytes and showed no receptor activation in the absence of ligand (8,9).
Despite the importance of the FGF ligand for activation of both wild-type and mutated FGFR3, our knowledge about FGF expression in cartilage remains poor, leaving the nature of FGF involved in activation of FGFR3 unclear. The aim of this study was to identify the physiologic FGF ligands for FGFR3 in human fetal cartilage.
MATERIALS AND METHODS
Chondrocyte isolation and culture.
Human material was obtained through the International Skeletal Dysplasia Registry at Cedars-Sinai Medical Center, Los Angeles, CA. Cartilage was dissected from the ends of long bones of 20–28 wk gestation fetuses and cleared of the soft tissues. In TD cases, the diagnosis was based on the radiographic appearance, histologic studies of cartilage sections, and FGFR3 mutational analysis (10). Chondrocytes were isolated by 24 h treatment with 0.1% bacterial collagenase (Invitrogen, Carlsbad, CA) and grown in monolayer in Dulbecco's modified Eagle's medium (DMEM, MediaTech, Herndon, VA) supplemented with 10% fetal bovine serum (Atlanta Biologicals, Norcross, GA) and antibiotics. Alginate suspension cultures were prepared as described (11) at a density of 2 ×106 cells/mL and the cells were cultivated in Opti-MEM (Invitrogen) supplemented with 10% FBS, 1 mM L-ascorbic acid, and antibiotics. Putative redifferentiation was assessed by detection of anchorage-independent cell growth.
For cell growth experiments, RCS chondrocytes (12) were seeded in 24-well plates, treated with FGF1, 2, 17, and 19 (R&D Systems, Minneapolis, MN) with or without heparin (Invitrogen; 1 μg/mL) for 72 h and counted. For Erk MAP activation, cultivated human control chondrocytes were serum-starved for 24 h, treated with FGF1, 2, 17, and 19 (20 ng/mL) with or without heparin for 30 min, and analyzed for Erk activation by WB.
Reverse transcriptase PCR.
Poly-dT-primed cDNA was synthesized from 3 μg of total chondrocyte RNA using the Omniscript RT Kit (QIAGEN, Valencia, CA). Table 1 shows the PCR primers used. All primers were designed to prevent amplification of genomic DNA and verified by PCR containing genomic DNA as a template. PCR reactions were initially carried out using TaqDNA polymerase (Applied Biosystems, Foster City, CA). When no product was detected, the Expand high-fidelity PCR system or GC-rich PCR system (Roche Diagnostics, Indianapolis, IN) were used for greater sensitivity or to avoid false-negative results due to the high GC content of the template. The identity of PCR products was confirmed by direct sequencing using the BigDye Terminator Cycle Sequencing kit (Applied Biosystems).
WB and immunohistochemistry.
Cells were lysed in ice-cold lysis buffer (50 mM Tris-HCl, pH 8.0; 150 mM NaCl; 1% NP-40; 0.5% deoxycholate; 0.1% SDS) supplemented with proteinase inhibitors (1 mM phenylmethylsulfonyl fluoride, 0.2 μM aprotinin, 1 μg/mL leupeptin). Cartilage protein was extracted after homogenization of tissue in liquid nitrogen followed by lysis. Lysates (30 μg) were resolved by SDS-PAGE, transferred onto a PVDF membrane, and visualized by luminescence (Amersham Pharmacia Biotech, Inc., Piscataway, NJ). The following antibodies were used: FGF1 (Sigma Chemical Co., St. Louis, MO); FGF2 (Upstate Biotechnology, Lake Placid, NY); FGF5, 9–16, 19, 21 and actin (Santa Cruz Biotechnology, Santa Cruz, CA); FGF8, 17, and 18 (R&D Systems); collagen type II (Chemicon, Temecula, CA); collagen type III (Oncogene; San Diego, CA); and Erk1/2, P-Erk1/2T183/Y185 (Cell Signaling, Beverly, MA). Recombinant FGF1, 2, and 17–19 were from R&D Systems. For detection of FGF2 and FGF18 in the growth plate, 15-μm-thick frozen sections of femora were soaked with PBS supplemented with proteinase inhibitors. Tissue-specific samples were collected using inoculation needle under an inverted microscope.
For immunohistochemistry, paraformaldehyde-fixed, 15 μm thick frozen sections of femora were quenched with 3% hydrogen peroxide in methanol, digested in 2 mg/mL hyaluronidase (Sigma Chemical Co.), and incubated with primary antibody overnight in 4°C. Staining was developed by adding 0.6 mg/mL of DAB (Sigma Chemical Co.) in 0.05 M Tris-HCl pH 7.6 and 0.03% hydrogen peroxide. Antibodies used for detection of FGF1 and 2 were the same as those used for WB. The specificity of staining was confirmed by lack of staining when the primary antibody was omitted. Goldner's trichrome staining was performed as described (13). For immunocytochemistry, chondrocytes cultivated on glass slides were processed as described above. Human fibroblast-specific antibody (CBL-271, Chemicon) was used to evaluate fibroblast contamination of isolated chondrocytes. Only cultures containing <1% of positive cells were used.
RESULTS
RNA samples isolated from femoral growth plate cartilage of 20–28 wk gestation fetuses were examined for expression of human FGF family (FGF1–23) by conventional, nonquantitative reverse transcriptase (RT)-PCR. Using this technique, FGF1, 2, 5, 8–14, 16–19, and 21 were detected whereas the transcripts for FGF3, 4, 6, 7, 20, 22, and 23 were not found (Fig. 1A). Next, WB was used to examine FGF presence in cartilage at the protein level. The sensitivity of FGF1, 2, 5, 8–10, and 16–18 WB was evaluated by determining the lowest amount of recombinant FGF visualized by the corresponding antibody (14). With the exception of FGF9 and FGF16, all antibodies recognized their targets at low picogram levels. The detection limit of the FGF19 antibody, evaluated here, was 5 pg of FGF19 (not shown).
FGF expression in cartilage and cultivated chondrocytes. (A) RT-PCR analysis of the expression of human FGF family in control and TD whole growth plate cartilage. GAPDH serves as a control for template quantity. (B, C, D) FGF detected by WB in resting cartilage(B) and in vitro cultivated chondrocytes grown in monolayer (C) or alginate suspension (D). For each FGF, three control and five TD cartilage samples or cell lines are shown. The type of TD as well as the FGFR3 mutation are indicated. Note that C and D show only results different from resting cartilage, i.e. the presence of FGF1 as well as HMW FGF2 (22 and 24 kD) in cultured chondrocytes. rFGF, recombinant FGF.(E) FGF2 isoform expression during isolation and subsequent in vitro cultivation of chondrocytes. Cells were isolated from resting cartilage of control 26 wk gestation fetus, plated, and cultivated for the indicated times. FGF2 was determined by WB. Actin serves as loading control. The molecular weights of FGF2 isoforms are indicated.
In the resting cartilage lysates, only FGF2, 17, and 19 were detected by WB (Fig. 1B). With exception of FGF17 and 19, we next performed the same analysis with protein samples isolated from in vitro cultivated chondrocytes grown either in monolayer or in alginate suspension. The results were identical to the resting cartilage with two differences: In vitro cultivated chondrocytes contained weakly detectable FGF1, and there was a significant difference in FGF2 isoform expression pattern (Fig. 1, C and D). Specifically, only 18 kD FGF2 was detected in resting cartilage whereas cultivated chondrocytes synthesized, in addition, at least two HMW (15) variants of FGF2 (22 and 24 kD). Chondrocytes, isolated by 24 h of collagenase treatment, showed abundant HMW FGF2 signal by 3 d after plating (Fig. 1E).
The distribution of FGF1, 2, 17, and 19 within the growth plate was determined by immunohistochemistry. FGF1 antibody stained the proliferative and hypertrophic zones of the growth plate but not the resting zone (Fig. 2B). In contrast, FGF2 antibody stained both the resting and proliferative zones, with more signal intensity in the latter (Fig. 2C). Antibodies specific to FGF17 and 19 stained the entire growth plate, i.e. resting, proliferating, and hypertrophic chondrocytes (Fig. 3).
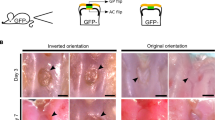
Distribution of FGF1 and 2 in the growth plate. (A) Histologic appearance of resting (r), proliferative (p), and hypertrophic (h) zone of the femoral growth plate of a control 25 wk gestation fetus. Sections were stained with Goldner's trichrome. cj, chondro-osseous junction. Immunohistochemical localization of (B) FGF1 and (C) FGF2 in the femoral growth plate of control 25 and 28 wk gestation fetuses, respectively. Note the significant FGF2 matrix staining in the proliferative zone. Bar = 100 μm.
The production of HMW FGF2 by in vitro proliferating chondrocytes prompted us to test whether this phenomenon occurs also in vivo or simply represents an artifact of tissue culture. By immunohistochemistry, it is impossible to distinguish among the different FGF2 variants. We therefore used frozen femoral sections to harvest, by microdissection, the cartilage samples corresponding specifically to the resting, proliferative, and hypertrophic zones of the growth plate, and subjected such samples to FGF2 WB. Figure 4 shows that in vivo proliferating chondrocytes synthesize at least three molecular variants of FGF2 (18, 22, 24 kD), whereas only 18 kD FGF2 was detected in resting cartilage. Very little FGF2 was found in the hypertrophic chondrocytes.
FGF2 isoform distribution in the growth plate. Ten micrograms of protein extracted from different zones of femoral growth plate as well as from surrounding bone and perichondrium of a control 25 wk gestation fetus was subjected to FGF2 and 18 WB. Type II and type III collagen detection serves to confirm the origin of the samples, whereas actin serves as a loading control. The isoform molecular weight is indicated for FGF2 and the position of closest protein marker bands is indicated for FGF18 and collagens. rFGF, recombinant FGF2 or 18.
Taken together, our results demonstrate that FGF1, 2, 17, and 19 are the predominant FGF ligands expressed in human growth plate cartilage and thus may serve as cognate ligands for FGFR3. We therefore tested the response of human primary chondrocytes to the FGF1, 2, 17, and 19 stimulation. As a reporter, we used the FGF-mediated activation of Erk MAP kinase, which represents a prominent target of FGFR signaling in cells. The results show that treatment with FGF1, 2, and 17 but not FGF19 elicited potent Erk activation (Fig. 5A). Next, we compared the ability of FGF1, 2, 17 and 19 to inhibit the growth of FGFR3-expressing RCS chondrocytes. Figure 5B shows that FGF1, 2, and 17 but not FGF19 inhibit the proliferation of RCS chondrocytes with a relative potency FGF2 ≫ FGF1 = FGF17.
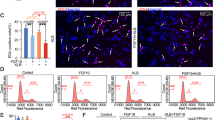
Effects of FGF treatment on chondrocytes. (A) Human primary chondrocytes were serum-starved for 24 h, treated for 30 min with FGF with or without heparin, and analyzed for Erk phosphorylation by WB. The levels of total Erk serve as a loading control. Note that FGF1, 2, and 17 but not FGF19 elicited significant Erk phosphorylation. (B) RCS chondrocytes were treated with FGF with or without heparin, cultivated for 72 h, and counted. Data represent the average from four wells with the indicated SD. Note that FGF1, 2, and 17 but not FGF19 inhibited RCS proliferation. Also note that both FGF1 and FGF17 required heparin to inhibit growth at low concentrations, whereas FGF2 inhibited growth alone.
DISCUSSION
Activating mutations in the FGFR3 tyrosine kinase account for a spectrum of human dwarfisms, highlighting the essential role of FGF signaling in regulation of long-bone growth. Although both wild-type and mutated FGFR3 appear to depend on FGF ligand for their activation (7), FGF expression in human cartilage remains, with the exception of FGF2 (16), unknown. In this study, we characterized the expression of the entire FGF family (FGF1-23) in human fetal cartilage.
By RT-PCR, we detected transcripts for FGF1, 2, 5, 8–14, 16–19, and 21 in the cartilage (Fig. 1A). This surprisingly broad array of expressed FGF may reflect the fetal stage of the tissue, with many genes being expressed in negligible amounts. Alternatively, given the sensitivity of the PCR method, the FGF signals may originate from minute amounts of contaminating soft tissue or blood vessel RNA. Western blot analysis revealed that only FGF1, 2, 17, and 19 are present in the growth plate or cultivated chondrocytes at the protein level (Fig. 1, B–D). The antibodies used for FGF detection showed comparable sensitivities (14), thus allowing us to conclude that FGF1, 2, 17, and 19 are the predominant FGF expressed in human fetal cartilage.
Recent data demonstrated that Fgf18 plays an important role in murine endochondral bone growth. Fgf18–/– mice had expanded zones of proliferating and hypertrophic chondrocytes and increased chondrocyte proliferation and differentiation (17). In general, this phenotype was similar to that observed in mice lacking functional Fgfr3 (18), implying that Fgf18 acts as a physiologic ligand for Fgfr3 in mice. Here, we did not detected FGF18 by WB in cartilage samples isolated from either resting cartilage, whole growth plate cartilage, or chondrocyte cell lines (data not shown). Since Fgf18 is expressed predominantly in perichondrium in mice (17), we probed protein samples isolated from human fetal perichondrium for FGF18. Again, no specific signal was found (Fig. 4). This absence of WB signal may be due to the slightly lower sensitivity of the FGF18 antibody when compared with FGF2 antibody (14). Alternatively, FGF18 may be significantly expressed in earlier gestational age than the 20–28 wk analyzed here.
We found a major difference in the FGF2 expression pattern between the resting cartilage, which produced only 18 kD FGF2, and proliferating chondrocytes, which produced two additional variants of FGF2—the 22 and 24 kD HMW FGF2 (Fig. 4). Unlike 18 kD FGF2 that is released from cells and acts by binding and activating the FGFR, the HMW FGF2 localizes predominantly to the nucleus and has an intracrine, FGFR-independent mode of action (15). Data from various cellular systems demonstrate that HMW FGF2 stimulates cell survival and proliferation in conditions when extracellular mitogenic signals are limited (19–22). We hypothesize that HMW FGF2 plays a similar role in chondrocytes, which proliferate in poorly vascularized growth plate where blood-borne growth factor and nutrient supply is restricted. Notably, the microscopic appearance of the growth plate of transgenic mice over-expressing human FGF2 (23) seems to support our view. In such animals, the growth plate appears short and flattened with marked expansion of the proliferative zone, suggesting intracrine action of HMW FGF2.
Given the fact that transgenic mice represent an important model for studying human FGFR3-related skeletal dysplasias, mouse to human comparison of the FGF/FGFR expression patterns in the growth plate is of interest (Table 2). Although there is, to our knowledge, no study evaluating FGF1 expression in the murine growth plate, FGF1 expression in the rat is similar to human (24) (Fig. 2B). FGF2 as well as FGFR3 localization in the murine growth plate is also similar to human (7,16,18,25,26) (Fig. 2C). In contrast, FGFR1 localizes to the hypertrophic zone in mice (18,27) but is predominantly expressed in the resting and proliferative zones in human (16,28).
We also compared FGF expression between control and TD cartilage. Although the immunohistochemistry results could not be fully compared due to marked disturbances of growth plate architecture in TD (data not shown), there was no significant difference in FGF expression among the control and TD cartilage (Fig. 1). It is therefore unlikely that signaling of mutated FGFR3 affects FGF expression in cartilage by either induction or repression of specific FGF.
We demonstrate that FGF1, 2, 17, and 19 are the predominant FGF ligands expressed in human growth plate cartilage. All FGF are experimentally able to bind FGFR3 (29,30) and thus may serve as cognate ligands for FGFR3. We challenged this hypothesis by testing the ability of FGF1, 2, 17, and 19 to 1) activate the FGFR3 signaling in chondrocytes, and 2) inhibit chondrocyte growth, the principal FGF-regulated phenotype in cartilage (5). Figure 5 shows that treatment with FGF1, 2, and 17 but not FGF19 induced both phenotypes.
Taken together, we identified FGF that are predominantly expressed in human growth plate cartilage and thus may serve as the autocrine physiologic ligands for FGFR3. The regulation of FGFR3 activation in cartilage appears, however, to be complex. This is clearly demonstrated in mice, where removal of cartilaginous (autocrine) Fgf1 and/or Fgf2 produces no skeletal phenotype (31), in contrast to removal of perichondrial (paracrine) Fgf18, which results in skeletal overgrowth from apparent lack of FGFR3 activation (17). Although our study represents the first step toward identifying the physiologic ligand(s) of FGFR3 in human cartilage, additional experimental evidence is needed to determine contribution of specific FGF autocrine and paracrine signals to FGFR3 activation in vivo.
Abbreviations
- Erk MAP:
-
extracellular-signal regulated MAP kinase
- FGF:
-
fibroblast growth factor
- FGFR:
-
fibroblast growth factor receptor
- HMW:
-
high molecular weight
- RCS:
-
rat chondrosarcoma chondrocytes
- TD:
-
thanatophoric dysplasia
- WB:
-
Western blotting
References
Passos-Bueno MR, Wilcox WR, Jabs EW, Sertie AL, Alonso LG, Kitoh H 1999 Clinical spectrum of fibroblast growth factor receptor mutations. Hum Mutat 14: 115–125
Webster MK, Donoghue DJ 1997 FGFR activation in skeletal disorders: too much of a good thing. Trends Genet 13: 178–182
Su WC, Kitagawa M, Xue N, Xie B, Garofalo S, Cho J, Deng C, Horton WA, Fu XY 1997 Activation of Stat1 by mutant fibroblast growth-factor receptor in thanatophoric dysplasia type II dwarfism. Nature 386: 288–292
Raffioni S, Zhu YZ, Bradshaw RA, Thompson LM 1998 Effect of transmembrane and kinase domain mutations on fibroblast growth factor receptor 3 chimera signaling in PC12 cells. A model for the control of receptor tyrosine kinase activation. J Biol Chem 273: 35250–35259
Sahni M, Ambrosetti DC, Mansukhani A, Gertner R, Levy D, Basilico C 1999 FGF signalling inhibits chondrocyte proliferation and regulates bone development through the STAT-1 pathway. Genes Dev 13: 1361–1366
Chen L, Adar R, Yang X, Monsonego EO, Li C, Hauschka PV, Yayon A, Deng C 1999 Gly369Cys mutation in mouse FGFR3 causes achondroplasia by affecting both chondrogenesis and osteogenesis. J Clin Invest 104: 1517–1525
Monsonego-Ornan E, Adar R, Feferman T, Segev O, Yayon A 2000 The transmembrane mutation G380R in fibroblast growth factor receptor 3 uncouples ligand-mediated receptor activation from down-regulation. Mol Cell Biol 20: 516–522
Iwata T, Li CL, Deng CX, Francomano CA 2001 Highly activated FGFR3 with K644M mutation causes prolonged survival in severe dwarf mice. Hum Mol Genet 10: 1255–1264
Legeai-Mallet L, Benoist-Lasselin C, Delezoide AL, Munnich A, Bonaventure J 1998 Fibroblast growth factor receptor 3 mutations promote apoptosis but do not alter chondrocyte proliferation in thanatophoric dysplasia. J Biol Chem 273: 13007–13014
Wilcox WR, Tavormina PL, Krakow D, Kitoh H, Lachman RS, Wasmuth JJ, Thompson LM, Rimoin DL 1998 Molecular, radiologic, and histopathologic correlations in thanatophoric dysplasia. Am J Med Genet 78: 274–281
Guo JF, Jourdian GW, MacCallum DK 1989 Culture and growth characteristics of chondrocytes encapsulated in alginate beads. Connect Tissue Res 19: 277–297
Mukhopadhyay K, Lefebvre V, Zhou G, Garofalo S, Kimura JH, de Crombrugghe B 1995 Use of a new rat chondrosarcoma cell line to delineate a 119-base pair chondrocyte-specific enhancer element and to define active promoter segments in the mouse pro-alpha 1(II) collagen gene. J Biol Chem 270: 27711–27719
Gruber HE 1992 Adaptations of Goldner's Masson trichrome stain for the study of undecalcified plastic embedded bone. Biotech Histochem 67: 30–34
Krejci P, Mekikian PB, Wilcox WR 2006 The fibroblast growth factors in multiple myeloma. Leukemia 20: 1165–1168
Bugler B, Amalric F, Prats H 1991 Alternative initiation of translation determines cytoplasmic or nuclear localization of basic fibroblast growth factor. Mol Cell Biol 11: 573–577
Gonzalez AM, Hill DJ, Logan A, Maher PA, Baird A 1996 Distribution of fibroblast growth factor (FGF)-2 and FGF receptor-1 messenger RNA expression and protein presence in the mid-trimester human fetus. Pediatr Res 39: 375–385
Liu Z, Xu J, Colvin JS, Ornitz DM 2002 Coordination of chondrogenesis and osteogenesis by fibroblast growth factor 18. Genes Dev 16: 859–869
Deng C, Wynshaw-Boris A, Zhou F, Kuo A, Leder P 1996 Fibroblast growth factor receptor 3 is a negative regulator of bone growth. Cell 84: 911–921
Estival A, Louvel D, Couders B, Prats H, Hollande E, Vaysse N, Clemente F 1993 Morphological and biological modifications induced in a rat pancreatic acinar cancer cell line (AR4-2J) by unscheduled expression of basic fibroblast growth factors. Cancer Res 53: 1182–1187
Delrieu I, Arnaud E, Ferjoux G, Bayard F, Faye JC 1998 Overexpression of the FGF-2 24-kDa isoform up-regulates IL-6 transcription in NIH-3T3 cells. FEBS Lett 436: 17–22
Arese M, Chen Y, Florkiewicz RZ, Gualandris A, Shen B, Rifkin DB 1999 Nuclear activities of basic fibroblast growth factor: potentiation of low-serum growth mediated by natural or chimeric nuclear localization signals. Mol Biol Cell 10: 1429–1444
Gualandris A, Arese M, Shen B, Rifkin DB 1999 Modulation of cell growth and transformation by doxycycline-regulated FGF-2 expression in NIH-3T3 cells. J Cell Physiol 181: 273–284
Coffin JD, Florkiewicz RZ, Neumann J, Mort-Hopkins T, Dorn GW 2nd, Lightfoot P, German R, Howles PN, Kier A, O'Toole BA 1995 Abnormal bone growth and selective translational regulation in basic fibroblast growth factor (FGF-2) transgenic mice. Mol Biol Cell 6: 1861–1873
Jingushi S, Scully SP, Joyce ME, Sugioka Y, Bolander ME 1995 Transforming growth factor-beta 1 and fibroblast growth factors in rat growth plate. J Orthop Res 13: 761–768
Peters K, Ornitz D, Werner S, Williams L 1993 Unique expression pattern of the FGF receptor 3 gene during mouse organogenesis. Dev Biol 155: 423–430
Wezeman FH, Bollnow MR 1997 Immunohistochemical localization of fibroblast growth factor-2 in normal and brachyomorphic mouse tibial growth plate and articular cartilage. Histochem J 29: 505–514
Peters KG, Werner S, Chen G, Williams LT 1992 Two FGF receptor genes are differentially expressed in epithelial and mesenchymal tissues during limb formation and organogenesis in the mouse. Development 114: 233–243
Delezoide AL, Benoist-Lasselin C, Legeai-Mallet L, Le Merrer M, Munnich A, Vekemans M, Bonaventure J 1998 Spatio-temporal expression of FGFR 1, 2 and 3 genes during human embryo-fetal ossification. Mech Dev 77: 19–30
Ornitz DM, Xu J, Colvin JS, McEwen DG, MacArthur CA, Coulier F, Gao G, Goldfarb M 1996 Receptor specificity of the fibroblast growth factor family. J Biol Chem 271: 15292–15297
Zhang X, Ibrahimi OA, Olsen SK, Umemori H, Mohammadi M, Ornitz DM 2006 Receptor specificity of the fibroblast growth factor family. The complete mammalian FGF family. J Biol Chem 281: 15694–15700
Miller DL, Ortega S, Bashayan O, Basch R, Basilico C 2000 Compensation by fibroblast growth factor 1 (FGF1) does not account for the mild phenotypic defects observed in FGF2 null mice. Mol Cell Biol 20: 2260–2268
Acknowledgements
The authors thank Miranda Von Dornum for assistance with primer design and Kathy Bui for technical assistance.
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was supported by Yang Sheng Tang USA Company, National Institutes of Health (NIH) grants 5P01-HD22657, GCRC CAP M01-RR00425, NIH UCLA Child Health Research Center P30-HD34610, and the Human Growth Foundation.
Rights and permissions
About this article
Cite this article
Krejci, P., Krakow, D., Mekikian, P. et al. Fibroblast Growth Factors 1, 2, 17, and 19 Are the Predominant FGF Ligands Expressed in Human Fetal Growth Plate Cartilage. Pediatr Res 61, 267–272 (2007). https://doi.org/10.1203/pdr.0b013e318030d157
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/pdr.0b013e318030d157
This article is cited by
-
FGF19 increases mitochondrial biogenesis and fusion in chondrocytes via the AMPKα-p38/MAPK pathway
Cell Communication and Signaling (2023)
-
FGF19 induces the cell cycle arrest at G2-phase in chondrocytes
Cell Death Discovery (2023)
-
Differential gene expression of human chondrocytes cultured under short-term altered gravity conditions during parabolic flight maneuvers
Cell Communication and Signaling (2015)
-
Instability restricts signaling of multiple fibroblast growth factors
Cellular and Molecular Life Sciences (2015)
-
FGF17, a gene involved in cerebellar development, is downregulated in a patient with Dandy–Walker malformation carrying a de novo 8p deletion
neurogenetics (2011)