Abstract
Our studies examined the hypothesis that the distribution of cerebral injury after a focal ischemic insult in the immature rat pup is associated with the regional distribution of nitric oxide synthase (NOS) activity and that differences in the vulnerability to ischemia between pup and adult might be related to differences in cofactor availability. We measured NOS activity in well-defined regions prone to become either core or penumbra in controls and at different times (end of occlusion, 0.5 h, and 24 h reperfusion) after middle cerebral artery occlusion (MCAO) from the right and left hemispheres in a 14- to 18-day-old rat pup filament model. Three groups of corresponding isoflurane sham controls were also included. “Core” NOS activity for combined right and left hemispheres ranged from 113% to 217% more than “penumbral” regions in control and sham groups. In the three MCAO groups, marked decreases in ischemic core and penumbral NOS activity were seen; however, core NOS remained higher than penumbral regions bilaterally. The effects of cofactor addition (10 μM tetrahydrobiopterin, 3 μM flavin adenine dinucleotide, and 3 μM flavin mononucleotide) on NOS activity were similar in “core” and “penumbral” regions in control and sham groups. However, after 24 h MCAO, cofactor addition preferentially increased NOS activity in the ischemic hemisphere. Cofactor addition in the pup also had a greater effect on enhancing NOS activity in all regions compared with the adult. Greater NOS activity in core regions in the rat pup, as in the adult, could in part, explain the increased vulnerability of that region to ischemia. NOS activity also can be influenced by the availability of cofactors and this effect may be greater in the immature animal.
Similar content being viewed by others
Main
Increasingly, the importance of NO during global and focal ischemic injury in the neonatal (1, 2) and immature (3) animal is being recognized. Similarly, developmental differences in NOS activity also are present (4). In whole brain homogenates, we have shown that NOS activity is 46% higher in the adult rat compared with 14- to 18-day-old pups and that differences in the Km for arginine (27% more in pups) and maximum enzyme velocity for NOS (96% more in adults) are present (5).
Regional differences in cerebral NOS activity also have been demonstrated (6, 7). Our recent studies in an adult rat model of MCAO followed by 24 h reperfusion have shown consistently greater amounts of NOS activity in core compared with penumbral regions in control, sham, and ischemic groups (8). Interpretation of these data suggested that greater NOS activity in core regions could, in part, explain the increased vulnerability of that region to ischemia and that these differences could contribute to maturation of the infarct over time.
The current study determined whether differences in core and penumbral NOS activity are present in the 14- to 18-day-old rat pup. If so, these findings would support the general hypothesis that regional differences in NOS activity may account to some degree for the regional differences in ischemic vulnerability in the immature nervous system.
Developmental differences in NOS activity could be related to differences in either enzyme or cofactor concentration. As our previous studies have shown that cofactor addition increased NOS activity, we repeated the NOS assays in separate homogenate samples for core and penumbral regions from both hemispheres after adding BH4, FAD, and FMN in concentrations shown to generate maximum activity (5, 8). If cofactor addition in the pup restored NOS activity, then alterations in cofactor concentration might be important in the regulation of NOS activity in the immature animal as it appears to be in the adult. Comparing the results of cofactor addition in pups to data from our recent adult rat studies, allowed us to determine that cofactor addition in pups had a greater effect on increasing NOS activity. These findings suggest that NOS cofactor concentration may be decreased in the rat pup and that this could be an additional factor that contributes to the greater resistance to ischemia observed in the immature animal.
METHODS
NOS activity was determined in 14- to 18-day-old SHR pups using a modified version of the method reported by Bredt and Snyder (8, 9) in core and penumbral regions in four separate series of experiments. These studies had received prior approval by the Institutional Review Board of Loma Linda University Medical Center and Children's Hospital. In the first group (n= 9), animals were anesthetized, immediately decapitated, and NOS activity measured from right and left hemisphere brain regions that corresponded to the core (lateral striatum and overlying cortex) and penumbra (adjacent ventrolateral cortex) as described in detail below. The three other groups consisted of SHRs undergoing 4 h of MCAO and either no reperfusion (R0), 0.5 h reperfusion (R0.5), or 24 h reperfusion (R24). Additional sham controls were done for the total time period of MCAO and reperfusion for these three groups (S4.0, S4.5, S24) and NOS activity was measured in designated core and penumbral regions to control for anesthetic effects on NOS activity (10).
Establishment of reversible focal cerebral ischemia.
Male SHR pups (30–35 g;n= 51) were anesthetized with 1.2% isoflurane (Forane, Ohmeda Caribe, Inc., Guayoma, Puerto Rico) and a 60/40% air/oxygen mixture by mask and allowed to breathe spontaneously. As previously reported in this model, 4 h of MCAO in the pup produces an infarct (measured at 24 h using the stain TTC) that is similar in magnitude to the adult SHR after 1.5 h MCAO (11). Body temperature was maintained at 37°C throughout the experimental procedure and the rat pups were maintained during the 24-h period of reperfusion in a temperature controlled environment at 95–100°F. The temperatures were rechecked at 24 h and were similar in both control and experimental groups.
Focal ischemia was accomplished using a filament model of temporary unilateral proximal occlusion of the middle cerebral artery as previously reported by our laboratory (3, 11) that was based on the earlier studies of Tamura et al. (12). Although we have not determined whether reperfusion occurs after filament removal in our model by measuring cerebral blood flow, previous studies in adult MCAO models (13–15) as well as our own previous observations of needing at least a 4-h time period to produce an infarct (11) suggest that reperfusion likely occurs after filament removal in the 14- to 18-day-old pup.
SHR pups were placed in the supine position on the platform of a Zeiss stereoscopic microscope (model OMP1) and the left common carotid artery exposed. The left external carotid artery was isolated and ligated. A tie was loosely placed around the internal carotid artery to control backflow and a vascular clamp was placed on the common carotid artery 1 cm proximal to the bifurcation. A small incision was made in the external carotid artery close to the ligature and a no. 6–0 (0.07 mm) nylon filament passed proximally into the internal carotid artery to transiently occlude the middle cerebral artery. The filament was then sutured in place, the clamp on the common carotid artery removed, and the skin closed with 3–0 silk. The duration of this procedure was 20 min. The pups were allowed to recover from anesthesia, returned to their litters, and maintained in a normoxic environment for 4 h. After this period of normoxic MCAO, the pups were reanesthetized, the filament carefully removed, the external corotid artery ligated, and the wound closed.
Depending on the experimental protocol, the rats were killed as follows: (1) anesthetized and immediately decapitated, (2) after 4 h MCAO—R0; (3) after 4 h MCAO and 0.5 h reperfusion—R0.5; and (4) after 4 h MCAO, filament removal and 24 h recovery—R24. In the three sham groups (S4.0, S4.5, and S24) that corresponded to the three occlusion/reperfusion experimental groups, all procedures and time periods were identical except for lack of filament insertion into the external carotid artery.
Brain sectioning for measurement of NOS activity and TTCstaining.
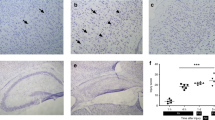
In each animal, the brain was sectioned into three slices beginning 2 mm from the anterior tip of the frontal lobe (Fig. 1) (8). Section 2 (4-mm thick) was used for measurement of NOS activity and sections 1 and 3 (3-mm thick) for estimating the area of mitochondrial ischemic injury.
Depiction of the 4-mm coronal section (section 2) from which core and penumbral tissues were taken for NOS assays. Percent area of ischemic injury for section 2 was indirectly estimated by using the TTC area of pallor that reflected ischemic injury determined from the posterior surface of section 1 (3 mm) and the anterior surface of section 3 (3 mm) (fromRef. 8).
Regions from the left hemisphere of section two that corresponded to the ischemic core and penumbra were dissected. We initially identified the midline between the two hemispheres and then made a longitudinal cut (from top to bottom) approximately 2 mm from the midline through each hemisphere. This was done to avoid mesial hemispheric structures, which are supplied primarily by the anterior cerebral artery. We then made a transverse diagonal cut at approximately the “2 o'clock” position, to separate the core (i.e. striatum and overlying cortex) from the penumbra (adjacent cortex). Designation of these core and penumbral regions was based on pharmacological and histopathological studies by other investigators that defined the core to include subcortical structures, primarily the lateral caudoputamen and overlying cortex, whereas the adjacent ventrolateral cortex was designated as penumbra (8, 13–16).
We also dissected similar regions from the contralateral nonischemic right hemisphere that corresponded to the core and penumbral regions of the ischemic left hemisphere. Throughout this study these nonischemic regions are referred to as “core” and “penumbra” to indicate that they are taken from homologous but nonischemic tissue. In addition, the terms “core” and “penumbra” are also used to describe those regions in all control and sham groups, again to differentiate them from the three ischemia groups in which the left hemisphere underwent focal ischemia.
Because of the smaller brain volume in the rat pup compared with the adult SHR, tissue volume per individual rat pup was too small to reliably determine NOS values. Accordingly, the “sandwich” technique was modified. Pooled core and penumbral NOS determinations were made by combining these respective regions (separately for the ischemic and nonischemic hemispheres) from two littermates who underwent MCAO on the same day. Infarct volumes (see below) were separately measured in each animal and the results averaged and reported for the combined NOS activity sample. For example, mean values reported for NOS activity and infarct volume in the control group (n= 8) were based on data collected from 16 rat pups.
We used the histochemical stain TTC to verify that an ischemic insult had occurred and only used those animals with definite evidence of ischemia for measurement of NOS activity (8). Because, we used a “sandwich” technique, in which TTC staining was performed on the two outer sections with the middle section taken for NOS assay, immersion rather than the perfusion of the brain slices was used. The immersion technique may have underestimated the area of ischemia in the R0 and R0.5 groups but probably accurately measured the area of ischemia in the R24 group. Thus, for the two early MCAO groups (R0 and R0.5) we included those animals who had at least a 20% area of pallor as earlier studies have shown that with the immersion TTC technique, an approximate 10 to 20% area of pallor after 1 to 2 h MCAO can be identified (17, 18).
Two brain sections from each animal (sections one and three) were immersed in TTC solution for 10 min and then stored in 15 mL of 10% buffered formalin. The two sections were photographed with color slide film (Ektachrome, Tungsten 160 ASA) and analyzed using a Drexel/DUMAS image processing system. The infarct area of the posterior surface of section 1 and the anterior area of section 3 were averaged to obtain an estimate of the percent area of ischemic injury that corresponded to section two. The effect of edema on these measurements was corrected by using the method of Swanson et al. (19).
Measurement of core and penumbra NOS activity.
Regions predesignated as core and penumbra from the left hemisphere and nonischemic “core” and “penumbra” from the right hemisphere were assayed in duplicate for NOS activity determined as the conversion of 14C-L-arginine (Du Pont, Boston, MA) to 14C-citrulline, modified from the method of Bredt and Snyder (5, 8, 9).
Specimens from each region from two littermates were combined and homogenized in 50 mM HEPES with 1 mM EDTA at pH 7.4, then centrifuged at 1500 ×g for 10 min at 4°C. The supernates were analyzed for protein content using the BCA Protein Assay Reagent (Pierce, Rockford, IL) with bovine serum albumin as a standard and then frozen at −80°C for subsequent measurement of NOS activity. The ratio of tissue wet weight to homogenization buffer volume was routinely adjusted for each preparation to yield an average protein concentration of \F150 μg in each 25-μL aliquot of supernatant.
Each assay sample contained 25 μL of supernatant from a cerebral homogenate, 25 μL (45 pmol) of 14C-L-arginine and 100 μL of reaction buffer (50 mM HEPES, 1 mM EDTA, 1 mM CaCl2, and 1 mM β-NADPH at pH 7.4). After a 10-min incubation at 37°C the reaction was terminated by addition of 2.0 mL of an ice-cold stop solution containing 20 mM HEPES and 2 mM EDTA at pH 5.5. The combined volume was then applied to Poly-Prep chromatography columns preloaded with 1.0 mL AG 50W-X8 Resin (NaOH form; Bio-Rad, Richmond, CA) and rinsed with 2.0 mL distilled water. The eluted volume, containing 14C-citrulline, was measured by liquid scintillation counting. A separate standard curve was run with each assay to correct for interassay variations in quench and counting efficiency. Samples and standards were run in duplicate and NOS activity was calculated as pmol/mg protein/min.
Effect of cofactors on core and penumbral NOS activity.
We repeated the NOS assays for all regions after adding cofactors to separate homogenate samples (5). In the current series only 10 μM BH4, 3 μM FAD, and 3 μM FMN were added as our previous studies showed a relatively small effect of CaM on NOS activity. For each cofactor assay, the sample contained 25 μL of supernatant from a cerebral homogenate, 25 μL (45 pmol) of 14C-L-arginine, 100 μL of reaction buffer (50 mM HEPES, 1 mM EDTA, 1 mM CaCl2, 1 mM β-NADPH, 10 μM BH4, 3 μM FAD, and 3 μM FMN at pH 7.4). To minimize the contributions of interassay variability to our measurements, these determinations were run in parallel along with assays done without cofactor addition using samples from the same animals.
Neuropathological studies.
In a separate group of rat pups (n= 6) who underwent MCAO, we examined the serial neuropathological changes in the contralateral nonischemic hemisphere, ischemic core-penumbral interface, ischemic core, and ischemic penumbra. Two pups from each of the three ischemia/reperfusion time periods (R0, R0.5, R24) underwent MCAO and reperfusion and at the end of that time period were killed, the brains removed, and placed in 10% formulin solution. Representative sections were taken through the middle of section two (as described previously), stained with hematoxylin and eosin, and reviewed by a neuropathologist. Because low power photomicrographs do not show maturation of the infarct over the 24-h time period, higher power (20x) was used to examine microscopic rather than gross anatomical changes. For all three time periods, we selected the same region of the brain section for the contralateral nonischemic hemisphere, ischemic core, and ischemic penumbra (see Figs. 3-5) to evaluate the pathological changes that occurred over time. As the core/penumbral interface shifts position over time, we selected the area where we could detect this interface microscopically and designated this in the respective TTC sections.
After 4 h MCAO (R0 group). The center panel depicts a representative TTC-stained brain section with the area of pallor in the left hemisphere corresponding to the area of ischemic injury. The mean area of injury averages 39 ± 1% for this group. Corresponding neuropathology (hematoxylin and eosin, all at magnification of 20x) taken from the four labeled regions of this section in a separate series of pups show (A) contralateral nonischemic hemisphere; (B) core/penumbral interface; (C) ischemic core; and (D) ischemic penumbra. Neurons in the contralateral nonischemic hemisphere appear normal whereas the majority of neurons in the ischemic core are shrunken and pyknotic with spongiform edema present in the surrounding tissue. In the ischemic penumbra, the majority of neurons are intact; some show neuronal shrinkage and the neuropil appears intact. A well demarcated core/penumbral interface is present (B) with the core seen on the left and the penumbra on the right.
After 4 h MCAO/24 h reperfusion (R24 group). The layout in this group is also similar to that described in Figure 3 with the mean percent area of ischemic injury averaging 47 ± 2%. Marked neuronal loss and edema formation are seen in the ischemic core (C) compared with the penumbra (D) at this time or to the core at earlier time points (Figs. 3C and 4C). Similarly, the penumbra shows greater neuronal loss than earlier penumbral specimens (Figs. 3D and 4D). The core/penumbral interface has again shifted position. Demarcation is less distinct but still detectable between the core and penumbra at 24 h (B). The penumbra (left) has a greater number of intact neurons and those that appeared injured are less shrunken and irregular than those in the core (left). In the contralateral hemisphere (A), some neuronal loss is now identifiable.
Data analysis.
NOS activity for all four experimental groups as well as the additional three sham groups were compared. Because of the skewed distribution of the NOS activity values, the data were log transformed, which resulted in a normal distribution. The resulting transformed data were than subjected to a two-way analysis of variance with region and duration of reperfusion as factors. In a separate analysis, we also examined the effect of cofactors on NOS activity for all regions and groups. To normalize for intrinsic differences in maximal NOS activity, cofactor effects were calculated as ratios of NOS activity observed in the absence of cofactors relative to that observed after cofactor addition. These data were also log transformed and resulted in a normal distribution. The transformed ratios were then subjected to a two-way analysis of variance with region and duration of reperfusion as factors. Unless otherwise indicated, data are expressed as the mean ± SEM and statistical significance was assumed at p< 0.05.
RESULTS
“Core” and “Penumbral” NOS Activity in Control and Sham Groups
NOS activity was consistently greater in “core” than “penumbral” regions in the control and all sham groups. Combined right plus left hemisphere “core” NOS activity in these four groups were increased compared to “penumbra” as follows: control (113%); S4.0 (77%); S4.5 (185%); and S24 (217%) (p< .0001) (Fig. 2; top). There were no significant differences in NOS activity between the left (434 ± 5 pmol/mg protein/min) and right hemisphere (451 ± 8) in these four groups p= 0.80).
Core and penumbral NOS activity in control (n= 8), S4.0 (n= 6), S4.5 (n= 6), and S24 (n= 5) groups. Regions designated as “core” and “penumbra” were based on studies as described in the text that correspond with the area of injury after an ischemic insult but in the control and sham groups, no ischemia or reperfusion was performed. S4.0 SHRs were anesthetized for 4.0 h and then killed; S4.5 SHRs were anesthetized for 4.5 h and then killed and S24 anesthetized for 4.0 h, recovered for 24 h and then killed. In all groups hemisphere “core” NOS activity was greater than the corresponding NOS activity determined from the “penumbra” (*p< 0.05). Hemispheric differences for “core” or “penumbral” NOS activity were not observed. Addition of cofactors increased NOS activity in all regions (p< 0.05). “Core” (dashed lines) and “penumbra” (solid lines) depict regional NOS activity in the right hemisphere (large symbols) and the left hemisphere (small symbols).
Effects of Isoflurane on NOS Activity in Control and Sham Groups
Compared with controls, “core” and “penumbral” NOS activity was little affected by administration of 1.2% isoflurane for 4 h (S4.0) or 4.5 h (S4.5). However, “core” and “penumbral” NOS activity was significantly increased in the group in which isoflurane was administered for 4.5 h and the animals maintained for 24 h (S24) compared with the control and other two sham groups (p< 0.01). For example, NOS activity in the S24 group was higher in each brain region compared with the S4.0 group as follows: left “core” (84%), left “penumbra” (64%), right “core” (315%), and right “penumbra” (161%).
Percent Area of Ischemic Injury and Neuropathology
Figures 3-5 demonstrate the serial changes observed in the three ischemic groups (R0, R0.5, R24) as depicted with TTC staining (center panel of each figure) as well as the hematoxylin and eosin photomicrographs (20x) showing the contralateral nonischemic hemisphere (A, upper left); ischemic core/penumbral interface (B, lower left); ischemic core (C, upper right); and ischemic penumbra (D, lower right). The percent area of ischemic injury measured 39 ± 1% after 4.0 h occlusion (R0 group;n= 9) and remained about the same after 0.5 h reperfusion (36 ± 1% (R0.5 group;n= 7). By 24 h, the area of injury extended to adjacent regions as shown and measured 47 ± 2% (R24 group).
A clear core/penumbral interface (B) can be seen in all three ischemic groups and as shown in the corresponding TTC sections the interface is located in different brain regions over time. Examination of the ischemic core (C) shows neuronal shrinkage and necrosis with some edema formation at the end of occlusion (Fig. 3) which worsens over time and by 24 h very few neurons can be identified. In contrast, the ischemic penumbra (D), shows some neuronal injury at R0 but by R0.5 this has become significant and similar to the changes noted in the ischemic core 0.5 h earlier. By 24 h, the area of the ischemic penumbra shows increased neuronal necrosis and edema but still is somewhat less affected than the core at that time point. The nonischemic contralateral hemisphere (A) remains intact at R0 and R0.5 h but in the R24 group shows evidence of some neuronal loss and shrinkage.
Comparison of Core Versus Penumbral NOS
Ischemic (left) and nonischemic (right) core NOS activity remained higher than corresponding penumbral regions as shown in Figure 6 (top;p< 0.05). These differences, expressed as the per cent that core NOS activity was greater than penumbra [100 × (core-penumbra)/penumbra)], averaged 66, 10, −21% in the ischemic hemisphere and 76, 77, 76% in the nonischemic hemisphere at the end of occlusion (R0;n= 9), 0.5 h reperfusion (R0.5;n= 7), and at 24 h (R24;n= 10) respectively. As shown in Figure 6 (top), even though the overall trend was for NOS activity to decrease in the ischemic hemisphere and to increase in the nonischemic hemisphere, the relation between core and penumbral NOS activity remained relatively constant except in the ischemic hemisphere at 24 h. NOS activity at this time was at the lowest limits of detection and no significant absolute difference between core (42 ± 2 pmol/mg protein/min) and penumbra (51 ± 2) was present. This was due to the fact that the rat pup has lower NOS activity than the adult and that in the model used in the current series of experiments, the infarct volume at 24 h was large (47%) and minimized core-penumbral differences.
Core and penumbral NOS activity in control (n= 8), R0 (n= 9), R0.5 (n= 7), and R24 (n= 10) groups. Both ischemic (left) and nonischemic (right) penumbral NOS activity were lower than corresponding core regions in the control and R0 and R0.5 groups (*p< 0.05). NOS activity was lower in the ischemic core (left) compared with the nonischemic “core” (right) in all three MCAO groups (p< 0.05). NOS activity in the ischemic core decreased by the end of occlusion and remained low as did ischemic penumbral NOS activity. A dramatic increase in NOS activity was seen in the nonischemic right “core” but not in the right “penumbra.” Core (dashed lines) and penumbra (solid lines) depict regional NOS activity in the right hemisphere (large symbols) and the left hemisphere (small symbols).
Ischemic (Left) Versus Nonischemic (Right) Hemisphere
Core and penumbral NOS activity was consistently lower in the ischemic hemisphere compared with the nonischemic hemisphere at all times (Fig. 6, top, p< 0.05). In core regions, NOS activity was 91, 85, and 97% lower in the ischemic compared with the nonischemic hemisphere in the R0, R0.5, and R24 groups. Similar differences in penumbral NOS activity for the same groups were also observed, i.e. 87, 82, and 44% lower in the ischemic versus nonischemic hemisphere.
Effects of Cofactor Addition on NOS Activity
Controls.
Addition of cofactors to separate homogenate samples from the control group increased NOS activity in all brain regions (Fig. 2, bottom). The per cent increase in NOS activity between the “without” cofactors and “with” cofactors groups were as follows: L-“core” (1,422%), L-“Pen” (1,945%), R-“core” (2,138%), R-“Pen” (1,995%) (p< 0.0001). For all regions combined this averaged 1,853%. There were no significant differences in the percent increase in NOS activity between “core” and “penumbra” or between ipsilateral and contralateral homologous regions. NOS activity after cofactor addition remained significantly higher in “core” compared with “penumbral” regions in both hemispheres (p< 0.05).
Isoflurane sham groups.
Addition of cofactors increased NOS activity in all regions in all sham groups (p< 0.05;Fig. 2, bottom). Addition of cofactors also had no effect on the right-left differences in any sham group. Cofactor addition also appeared to have a smaller effect on total NOS activity in sham-treated animals than controls. For all brain regions combined, the percent increases in NOS activity in the three sham groups was 1,089% (S4.0), 834% (S4.5), and 929% (S24) compared with the overall increase seen in the control group of 1,853% (p< 0.01). Even with the addition of cofactors, NOS activity remained significantly higher in “core” compared with “penumbral” regions in both hemispheres (p< 0.01). Combined “core” NOS activity in the S4.0, S4.5, and S24 groups was 77, 217, and 185% higher than the corresponding combined “penumbral” NOS activity (p< 0.01).
Ischemic groups.
In all groups and at all time points (Fig. 6, bottom), addition of cofactors increased NOS activity significantly (p< 0.05). For the four brain regions combined, the increase in NOS activity in the three MCAO groups averaged 877% (R0), 1,977% (R0.5), and 2,291% (R24). The effect of cofactor addition in these groups was similar when compared with the overall increase seen in the control group (1,853%) (p< 0.05). However, as shown at the top of Figure 7, the fractional activation of NOS supported by endogenous levels of cofactors did not vary significantly with region or side after zero or 0.5 h of reperfusion, but did vary significantly after 24 h of reperfusion. In particular, after 24 h of reperfusion fractional activation of NOS was not significantly different from control values in the noninfarcted right side, but was dramatically depressed in both the core and penumbral regions of the infarcted left side. These findings indicate that differences in cofactor availability probably do not contribute to differences in total NOS activity at the end of occlusion or early during reperfusion, but may be particularly important in infarcted regions after 24 h reperfusion.
Effects of cofactors on NOS activity. Data are presented as the log transformation of the ratios of NOS activity observed in the absence of cofactors relative to that observed after cofactor addition. The top panel shows the ratio data by region for the control and ischemia groups in the pups and reflects the fractional activation of NOS supported by endogenous levels of cofactors. No significant differences were observed when comparing the core versus penumbral regions or left vs right hemisphere. The bottom panel (control and MCAO groups in the adults) shows no differences at the end of occlusion (R0) or early during reperfusion (R0.5). However, after 24 h reperfusion, fractional activations of NOS were dramatically depressed in both the core and penumbral regions of the infarcted left side compared with similar regions from the right hemisphere in both the pups and the adults (*).
DISCUSSION
Our recent investigations in an adult rat model of focal cerebral ischemia have concentrated on differences in NOS activity in regions destined to become the ischemic core and penumbra (8). In these studies we found that core NOS activity in controls, different sham groups, and at the end of occlusion and during reperfusion remained consistently higher than in the penumbra. Our study extends these observations to the rat pup and also demonstrates that there are regional core/penumbral developmental differences in NOS activity as well as regional effects of cofactor addition.
Although the principal reason for core necrotic injury relates to the severity and duration of reduced cerebral blood flow, these data suggest that higher core NOS activity might be an additional critical factor early during reperfusion that could account for the preferential vulnerability of core compared with penumbral regions. Also, the data suggest that ischemic core NOS activity might contribute to infarct maturation over time.
In pups, as in adults, “core” activity was consistently higher than penumbra in control and all sham groups (Fig. 2) as well as immediately at the end of ischemia (Figs. 6 and 8). As in the adult, higher pup NOS activity in the core could contribute to the preferential vulnerability of this region to ischemic injury and to maturation of the infarct over time. Data supporting this possibility has recently been published in a 7-day-old rat model of focal cerebral ischemia (unilateral carotid occlusion and 8% oxygen) (20). Histochemical studies using a polyclonal anti-nNOS antibody showed an increase in the number of nNOS neurons in the ipsilateral hemisphere that was most prominent in the ischemic core (i.e. dorsolateral striatum) by 3 h after the onset of hypoxia. Similarly, other studies in the neonatal rat that have used either selective (7-nitroindazole) or nonselective (NG-nitro-L-arginine methyl ester) inhibitors of NOS activity have shown reduction in infarct volumes primarily by rescue of penumbral tissues that presumably have lower NOS activity (3, 21). Additional supportive evidence for the importance of core/penumbral differences in the neonate comes from studies in neonatal mice lacking neuronal nitric oxide synthase due to targeted disruption of the nNOS gene (2). The nNOS-deficient mice appear less vulnerable to focal cerebral ischemic injury particularly in penumbral cortical regions as well as in the hippocampus. Thus, multiple sources of evidence suggest that core/penumbral differences are in some way associated with the regional vulnerability to ischemia.
Comparison of absolute NOS activity in pups and adults in control and R0, R0.5, and R24 groups. In controls, NOS activity in pups is lower than in adults in core and penumbral regions (*p< 0.05). This difference becomes more marked in the ischemic hemisphere at the end of occlusion and 0.5 h into reperfusion. By 24 h, NOS activity is markedly decreased in pups and adults.
Developmental differences in NOS activity.
Embryonic and postnatal changes in NOS and NADPH-diaphorase staining have previously been demonstrated (22–24). In rat cerebrum, measurement of particulate NOS activity (that primarily reflects endothelial NOS) has been shown to increase in the first postnatal week and then decrease to almost undetectable levels by adulthood (4). In contrast, cytosolic NOS (primarily neuronal) increases to some degree in the cerebrum and by about 8-fold in the cerebellum over the same time frame. In our previous studies, we found that NOS activity from whole brain homogenates was 46% higher in the adult rat compared with the 14- to 18-day-old pup and as stated previously, differences in the Km for arginine and Vmax for NOS were present (5).
These developmental changes in NOS activity raised the question as to whether there might be developmental differences in core and penumbral regions and whether such differences could account for the resistance to ischemic injury characteristic of the immature animal. Figure 8 summarizes data from the current pup study and our recently reported adult data by comparing core and penumbral NOS activity from both hemispheres in controls, R0, R0.5, and R24 groups. In controls, pup NOS activity is significantly lower in “core” and “penumbral” regions compared with adults in both hemispheres. At the end of MCAO, NOS activity remains unchanged in the adult ischemic core and penumbra whereas pup values decreased substantially. After 0.5 h of reperfusion, a moderate reduction in ischemic core and penumbral activity has occurred in the adult and pup values remain low. By 24 h, core and penumbral NOS activity is equally reduced and minimal in both pups and adults. Of interest is the greater degree of up-regulation of NOS activity in the nonischemic (right) “core” seen in the pup compared with the adult. For example, NOS activity in the nonischemic “core” compared with the ischemic core in the pup was consistently higher (979% at R0; 587% at R0.5; and 2824% at R24) than that observed in the adult (33% at R0; 83% at R0.5; and 1932% at R24).
Although the data from the control groups clearly show that “core” and “penumbral” activity is lower in pups (and might account for less NO neurotoxicity in the pup), interpretation of the data from the ischemic groups must be done with caution because of the differences in infarct maturation. Our original studies showed that 4.0 h MCAO produced an infarct at 24 h in the 14- to 18-day-old rat pup that was similar in volume to 1.5 h MCAO in the adult (11). As can be seen by the data included in Figure 8, infarct volumes at 24 h are similar but at the end of MCAO, the area of TTC pallor is greater in the pup (39%) compared with the adult (24%). However, these volume differences reflect greater and earlier recruitment of penumbral tissues in the pup. Comparison of core NOS activity (in contrast to penumbral activity) at these early stages is however legitimate, as the volume of tissue, methods of tissue dissection and preparation, and normalization of NOS activity determinations to tissue protein concentration, allow such comparison.
The much lower NOS activity observed in the ischemic core in the pup could be explained in several ways: (1) earlier loss of NOS neurons; (2) greater down-regulation of NOS; or (3) lower substrate or cofactor availability. The first two possibilities seem unlikely as several recent studies involving focal (20, 21) and global ischemia in the rat pup (25) have shown increased nNOS immunohistochemical staining within hours after the onset of ischemia; other studies have demonstrated up-regulation of eNOS (26). Similarly, the ability to restore much of the depressed NOS activity by the addition of cofactors also argues against these possibilities. As will be discussed in the next section, differences in cofactor availability in the pup compared with the adult may be a contributing factor.
Developmental effects of cofactor addition on NOS activity.
In our previous studies using whole brain homogenates, we found that cofactor effects were not significantly different between pup and adult, except for BH4, which increased absolute NOS activity more in adults than in pups (5). Our study allowed regional core and penumbral comparisons between pup and adult groups (Fig. 7). To normalize for differences in NOS concentration, we used the NOS activities observed in the absence of added cofactors and compared them to the NOS activities present with saturating levels of cofactors (without/with ratio). This approach eliminated differences between samples due to differences in NOS concentration, and expressed fractional activation as a function of endogenous cofactor concentrations. Lower values of the log (% without/with) indicate that a greater percentage of endogenous NOS activity is dependent on cofactor addition. As can be seen in Figure 7, these values in the pup control and ischemia groups are lower compared with the adult in core and penumbral regions (p< 0.05) and suggest that in the control groups and during ischemia a greater proportion of NOS activity in the pup is cofactor dependent. At 24 h after ischemia, our original observations described in the adult that the ischemic core and penumbra were more dependent on cofactors than the nonischemic hemisphere also appeared to hold true for the pup but no developmental effect was evident.
The 14- to 18-d-old rat pup model.
Our studies used the 14- to 18-d-old rat pup filament model as we have been unable to obtain reproducible strokes in the 7- to 10-day-old pup. Our model more closely resembles that of the immature or juvenile animal than a true neonatal model. Although it is well recognized that the Rice-Vannucci model (unilateral carotid occlusion with 8% hypoxia for 1.5 h) in the 7-day-old rat is not a true model of either focal or global cerebral ischemia, it has been used by most investigators studying neonatal asphyxia because it can be performed with good reproducibility (27).
Questions, however, remain concerning various aspects of brain development in either the 7- to 10- or 14- to 18-day-old rat pup and to what degree either model reflects brain development and function in the human neonate at term. For example, in a recent review of the model, Vannucci and Vannucci (28) indicated that the 7-day postnatal rat was chosen for study because at this stage of development the animal's brain is histologically similar to that of a 32- to 34-wk gestation human fetus or newborn infant. This broad range raises questions about the validity of the 7th postnatal day time frame as just reflecting the immediate neonatal period. Other investigators examining four parameters of postnatal rat brain development (synapse formation, glutamic acid decarboxylase activity, choline acetyltransferase activity, and electrocortical function) came to the conclusion that 10 to 12 days was developmentally closer to that of the human newborn (29). A more recent review examining 15 separate variables of brain maturation came to the conclusion that the 7- to 14-day-old rat brain corresponded to that of the human brain at term (30). These variables included growth/proliferation, persistence of a periventricular germinal matrix, neurochemical and metabolic data, the EEG pattern, synapse formation, and patency of the blood brain barrier.
These studies point out the limitations of our own 14- to 18-day-old model as well as the 7-day-old Rice-Vannucci model as it is unlikely that different variables are developmentally and regionally synchronized. One approach to resolving this dilemma is to use a model in which the specific questions being investigated have parallel developmental profiles between the animal model and human. Because our study is concerned with NOS activity, at least two issues must be considered. The first relates to glutamate and its relation to NOS activation and the second to the developmental profile of NOS activity. In the rat, it has been shown that ischemic injury parallels sensitivity to N-methyl-D-aspartate glutamate activation that peaks on the sixth postnatal day (31, 32). In part, this is due to the greater proportion of the N-methyl-D-aspartate glutamate receptor subtype compared with other subtypes. On this basis, it is believed that the 7-day-old rat pup serves as a good model of excitotoxic human perinatal injury (32). However, recent studies in human infants from 25 wk gestation to term found no differences in N-methyl-D-aspartate glutamate receptor density in motor or temporal cortex with development (33). In addition, although term frontal and occipital regions had greater receptor densities than preterm infants, receptor densities at term were similar to adults. As related to our experimental paradigm, these studies suggest that the 14- to 18-day-old model should reasonably reflect the processes associated with glutamate activation as seen in the human neonate.
The second concern relates to the development of nNOS activity. In the rat, several studies have shown that NOS activity develops around embryonic d 10 and continues to increase (23, 34). In humans, an adult-like pattern is achieved between 24 and 32 wk (35, 36). During embryonic life there also appears to be an additional temporary increase in NOS activity that is believed to reflect the role of NOS in relation to maturational processes including cell migration, axon growth, and cell death (37, 38). Others have shown continued growth of NOS neurons after postnatal differentiation with these neurons reaching their typical morphology in the second (39) or third week (40) depending on the region studied (41). Overall, postnatal development of NADPH-d neurons that are believed primarily to be NOS containing neurons appear to be regionally specific and follow the general pattern of cortical development (42, 43). Although few studies have been published, similar patterns of development have been reported in the human fetus and infant. In the human, NOS activity has been demonstrated during gestation in the basal ganglia (13 wk), subcortical white matter (18 wk), cortex (26 wk), and caudate nucleus and putamen (33–36 wk) (44). In many of these regions NOS activity had achieved an adult-like pattern by 24 to 32 wk (35, 36).
Thus, it is of interest to note that comparison of our previous reports of NOS inhibition in the 14- to 18-day-old pup with focal ischemia to studies in the the 7-day-old pup in which NO synthesis was also inhibited, found similar degrees of infarction and of infarct volume reduction (3, 45). Taken together, these observations suggest the possibility that NOS data from the 14- to 18-day-old rat pup is clearly indicative of an immature response and may also fall within the domain of the neonatal period.
Core/penumbral neuropathology.
Our studies also provide pathologic confirmation of infarct maturation as observed in the TTC-stained sections. As shown in Figures 3-5, there is progressive neuronal necrosis and edema formation in the ischemic core. Similar changes are noted in the penumbra but they are milder and delayed in their appearance compared with the changes present in core regions. Similarly, a well-defined core/penumbral interface can be seen at the end of occlusion and at 0.5 and 24 h reperfusion. The location of this interface changes over time and becomes less distinct as more of the tissue shows irreversible ischemic necrosis (e.g. at 24 h). Correlation of the histopathological evolution of injury with colocalization of changes in NOS immunoreactivity as detected by immunohistochemical staining would be of interest.
CONCLUSIONS
Core/penumbral differences in NOS activity were present in the rat pup as in the adult and suggest an additional explanation for the vulnerability of the core to ischemic and reperfusion injury. Lower core and penumbral NOS activity in the pup might also explain why the immature rat is more resistant to ischemic injury. In part, this may be related to the fact that the immature rat is more dependent on cofactors that appear to be less available than in the adult. This possibility is supported by recent observations in the hph-1 mouse, which displays GTP cyclohydolase deficiency necessary for BH4 synthesis (46). In these mice BH4 levels are reduced and brain intracellular NOS concentrations are unaffected; however, NO synthesis is significantly reduced.
After 4 h MCAO/0.5 h reperfusion (R0.5 group). The layout in this group is similar to that described in Figure 3 with the mean percent area of ischemic injury averaging 36 ± 1%. Increased neuronal shrinkage and loss is present in the ischemic core (C) compared with Figure 3C. The penumbra (D) at this time shows increasing neuronal shrinkage and loss distinctly worse than the penumbra shown in Figure 3D. The penumbra at this time appears similar to the ischemic core shown in Figure 3C. A core/penumbral interface (B) can still be demonstrated although it is in a different location than that shown earlier reflecting infarct maturation. The cells on the core side of this interface appear quite pyknotic and reduced in number compared with the penumbra. The contralateral nonischemic hemisphere (A) remains relatively normal although some neurons appear shrunken.
Abbreviations
- BH4:
-
tetrahydrobiopterin
- CaM:
-
calmodulin
- FAD:
-
flavin adenine dinucleotide
- FMN:
-
flavin mononucleotide
- MCAO:
-
middle cerebral artery occlusion
- NO:
-
nitric oxide
- NOS:
-
NO synthase
- SHR:
-
spontaneously hypertensive rat
- TTC:
-
2, 3, 5-triphenyltetrazolium chloride
References
Dorrepaal CA, Shadid M, Steendijk P, Van der Velde ET, Van de Bor M, Baan J, Van Bel F 1997 Effect of post-hypoxic-ischemic inhibition of nitric oxide synthesis on cerebral blood flow, metabolism and electrocortical brain activity in newborn lambs. Biol Neonate 72: 216–226.
Ferriero DM, Holtzman DM, Black SM, Sheldon RA 1996 Neonatal mice lacking neuronal nitric oxide synthase are less vulnerable to hypoxic-ischemic injury. Neurobiol Dis 3: 64–71.
Ashwal S, Cole DJ, Osborne TN, Osborne S, Pearce WJ 1995 L-NAME reduces infarct volume in a filament model of transient middle cerebral artery occlusion in the rat pup. Pediatr Res 38: 652–656.
Matsumoto T, Pollock JS, Nakane M, Förstermann U 1993 Developmental changes of cytosolic and particulate nitric oxide synthase in rat brain. Dev Brain Res 73: 199–203.
Pearce WJ, Tone B, Ashwal S 1997 Maturation alters cerebral NOS kinetics in the spontaneously hypertensive rat. Am J Physiol 42: R1–R7
Kuppusamy P, Ohnishi ST, Numagami Y, Ohnishi T, Zweier JL 1995 Three-dimensional imaging of nitric oxide production in the rat brain subjected to ischemia-hypoxia. J Cereb Blood Flow Metab 15: 904–913.
Salter M, Duffy C, Garthwaite J, Strubos PJLM 1995 Substantial regional and hemispheric differences in brain nitric oxide synthase (NOS) inhibition following intracerebroventricular administration of Nω-nitro-L-arginine (L-NA) and its methyl ester (L-NAME). Neuropharmacology 34: 639–649.
Ashwal S, Tone B, Tian HR, Cole DJ, Pearce WJ 1998 Core and penumbral nitric oxide synthase activity during cerebral ischemia and reperfusion. Stroke 29: 1037–1047.
Bredt DS, Snyder SH 1990 Isolation of nitric oxide synthetase, a calmodulin-requiring enzyme. Proc Natl Acad Sci USA 87: 682–685.
Tobin JR, Martin LD, Breslow MJ, Traystman RJ 1994 Selective anesthetic inhibition of brain nitric oxide synthase. Anesthesiology 81: 1264–1269.
Ashwal S, Cole DJ, Osborne S, Osborne TN, Pearce WJ 1995 A new model of neonatal stroke: Reversible middle cerebral artery occlusion in the rat pup. Pediatr Neurol 12: 191–196.
Tamura A, Graham DI, McCulloch J, Teasdale GM 1981 Focal cerebral ischaemia in the rat: 1. J Cereb Blood Flow Metab 1: 53–60.
Memezawa H, Minamisawa H, Smith ML, Siesjö BK 1992 Ischemic penumbra in a model of reversible middle cerebral artery occlusion in the rat. Exp Brain Res 89: 67–78.
Takagi K, Ginsberg MD, Globus MYT, Dietrich D, Martinez, Kraydieh S, Busto R 1993 Changes in amino acid neurotransmitters and cerebral blood flow in the ischemic penumbra region following middle cerebral artery occlusion in the rat: : correlation with histopathology. J Cereb Blood Flow Metab 13: 575–585.
Müller TB, Haraldseth O, Unsgård G 1994 Characterization of the microcirculation during ischemia and reperfusion in the penumbra of a rat model of temporary middle cerebral artery occlusion: : a laser doppler flowmetry study. Int J Microcirc 14: 289–295.
Zhang F, Iadecola C 1994 Reduction of focal cerebral ischemic damage by delayed treatment with nitric oxide donors. J Cereb Blood Flow Metab 14: 574–580.
Hatfield RH, Mendelow AD, Perry RH, Alvarez LM, Modha P 1991 Triphenyltetrazolium chloride (TTC) as a marker for ischaemic changes in rat brain following permanent middle cerebral artery occlusion. Neuropath Appl Neurobiol 17: 61–67.
Bartus RT, Dean RI, Cavanaugh K, Eveleth D, Carriero DL, Lynch G 1995 Time-related neuronal changes following middle cerebral artery occlusion: : implications for therapeutic intervention and the role of calpain. J Cereb Blood Flow Metab 15: 969–979.
Swanson RA, Morton MT, Tsao-Wu G, Savalos RA, Davidson C, Sharp FR 1990 A semiautomated method for measuring brain infarct volume. J Cereb Blood Flow Metab 10: 290–293.
Higuchi Y, Hattori H, Hattori R, Furusho K 1996 Increased neurons containing neuronal nitric oxide synthase in the brain of a hypoxic-ischemic neonatal rat model. Brain Dev 18: 369–375.
Higuchi Y, Hattori H, Kume T, Tsuji M, Akaike A, Furusho K 1998 Increase in nitric oxide in the hypoxic-ischemic neonatal rat brain and suppression by 7-nitroindazole and aminoguanidine. Eur J Pharmacol 342: 47–49.
Bredt DS, Snyder SH 1994 Transient nitric oxide synthase neurons in embryonic cerebral cortical plate, sensory ganglia, and olfactory epithelium. Neuron 13: 301–313.
Yan XX, Garey LJ, Jen LS 1994 Development of NADPH-diaphorase activity in the rat neocortex. Dev Brain Res 79: 29–38.
Samama B, Chateau D, Boehm N 1995 Expression of NADPH-diaphorase in the rat forebrain during development. Neurosci Lett 184: 204–207.
Johnston MV 1997 Hypoxic and ischemic disorders of infants and children. Brain Dev 19: 235–239.
Beasley TC, Bari F, Thore C, Thrikawala N, Louis T, Busija D 1998 Cerebral ischemia/reperfusion increases endothelial nitric oxide synthase levels by an indomethacin-sensitive mechanism. J Cereb Blood Flow Metab 18: 88–96.
Roohey T, Raju TN, Moustogiannis AN 1997 Animal models for the study of perinatal hypoxic-ischemic encephalopathy: : a critical analysis. Early Hum Dev 47: 115–146.
Vannucci RC, Vannucci SJ 1997 A model of perinatal hypoxic-ischemic brain damage. Ann N Y Acad Sci 835: 234–249.
Romijn HJ, Hofman MA, Gramsbergen A 1991 At what age is the developing cerebral cortex of the rat comparable to that of the full-term newborn human baby?. Early Hum Dev 26: 61–67.
Hagberg H, Bona E, Gilland E, Puka-Sundvall M 1997 Hypoxia-ischaemia model in the 7-day-old rat: possibilities and shortcomings. Acta Paediatr Suppl 422: 85–88.
Ikonomidou C, Mosinger JL, Salles KS, Labruyere J, Olney JW 1989 Sensitivity of the developing rat brain to hypobaric/ischemic damage parallels sensitivity to N-methyl-aspartate neurotoxicity. J Neurosci 9: 2809–2818.
McDonald JW, Johnston MV 1990 Physiological and pathophysiological roles of excitatory amino acids during central nervous system development. Brain Res Rev 15: 41–70.
Andersen DL, Tannenberg AE, Burke CJ, Dodd PR 1998 Regional development of glutamate-N-methyl-D-aspartate receptor sites in asphyxiated newborn infants. J Child Neurol 13: 149–157.
Keilhoff G, Seidel B, Noack H, Tischmeyer W, Stanek D, Wolf G 1996 Patterns of nitric oxide synthase at the messenger RNA and protein levels during early rat brain development. Neuroscience 75: 1193–1201.
Yan XX, Garey LJ, Jen LS 1996 Prenatal development of NADPH-diaphorase-reactive neurons in human frontal cortex. Cereb Cortex 6: 737–745.
Gonzalez-Hernandez T, Gonzalez-Gonzalez B, Mantolan-Sarmiento B, Mendez-Medina R, Ferres-Torres R, Meyer G 1994 Transient NADPH-diaphorase activity in motor nuclei of the foetal human brain stem. Neuroreport 5: 758–760.
Bredt DS, Snyder SH 1994 Transient nitric oxide synthase neurons in embryonic cerebral cortical plate, sensory ganglia, and olfactory epithelium. Neuron 13: 301–313.
Santacana M, Uttenthal LO, Bentura ML, Fernandez AP, Serrano J, Martinez de Velasco J, Alonso D, Martinez-Murillo R, Rodrigo J 1998 Expression of neuronal nitric oxide synthase during embryonic development of the rat cerebral cortex. Brain Res Dev Brain Res 111: 205–222.
Luth HJ, Hedlich A, Hilbig H, Winkelmann E, Mayer B 1995 Postnatal development of NADPH-diaphorase/nitric oxide synthase positive nerve cells in the visual cortex of the rat. J Hirnforsch 36: 313–328.
Tenorio F, Giraldi-Guimaraes A, Mendez-Otero R 1995 Developmental changes of nitric oxide synthase in the rat superior colliculus. J Neurosci Res 42: 633–637.
Black SM, Bedolli MA, Martinez S, Bristow JD, Ferriero DM, Soifer SJ 1995 Expression of neuronal nitric oxide synthase corresponds to regions of selective vulnerability to hypoxia-ischaemia in the developing rat brain. Neurobiol Dis 2: 145–155.
van Eden CG, Steinbusch HW, Rinkens A, de Vente J 1996 Developmental pattern of NADPH-diaphorase activity and nitric oxide-stimulated cGMP immunoreactivity in the frontal rat cortex and its role in functional recovery from aspiration lesions. J Chem Neuroanat 10: 279–286.
Tomic D, Zobundzija M, Meaugorac M 1994 Postnatal development of nicotinamide adenine dinucleotide phosphate diaphorase (NADPH-d) positive neurons in rat prefrontal cortex. Neurosci Lett 170: 217–220.
Ohyu J, Takashima S 1998 Developmental characteristics of neuronal nitric oxide synthase (nNOS) immunoreactive neurons in fetal to adolescent human brains. Brain Res Dev Brain Res 110: 193–202.
Hamada Y, Hayakawa T, Hattori H, Mikawa H 1994 Inhibitors of nitric oxide synthesis reduces hypoxic-ischemic brain damage in the neonatal rat. Pediatr Res 35: 10–14.
Brand MP, Heales SJ, Land JM, Clark JB 1995 Tetrahydrobiopterin deficiency and brain nitric oxide synthase in the hph1 mouse. J Inherit Metab Dis 18: 33–39.
Author information
Authors and Affiliations
Additional information
Supported by the Pediatric Research Fund from the Department of Pediatrics, Loma Linda University School of Medicine and by the Department of Anesthesiology.
Rights and permissions
About this article
Cite this article
Ashwal, S., Tone, B., Tian, H. et al. Core and Penumbral Nitric Oxide Synthase Activity during Cerebral Ischemia and Reperfusion in the Rat Pup. Pediatr Res 46, 390 (1999). https://doi.org/10.1203/00006450-199910000-00006
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199910000-00006
This article is cited by
-
Enhanced autophagy interacting proteins negatively correlated with the activation of apoptosis-related caspase family proteins after focal ischemic stroke of young rats
BMC Neuroscience (2022)
-
Neuronal chemokine-like-factor 1 (CKLF1) up-regulation promotes M1 polarization of microglia in rat brain after stroke
Acta Pharmacologica Sinica (2022)
-
Morin Attenuated Cerebral Ischemia/Reperfusion Injury Through Promoting Angiogenesis Mediated by Angiopoietin-1-Tie-2 Axis and Wnt/β-Catenin Pathway
Neurotoxicity Research (2022)
-
Neferine Protects Against Brain Damage in Permanent Cerebral Ischemic Rat Associated with Autophagy Suppression and AMPK/mTOR Regulation
Molecular Neurobiology (2021)
-
Effects of Paired Associative Stimulation on Metabolites in Ischemia Stroke Rats Model as Studied by Nuclear Magnetic Resonance Spectrum
Neurochemical Research (2021)