Abstract
No validated biological markers (or biomarkers) currently exist for appropriately selecting patients with cancer for antiangiogenic therapy. Nor are there biomarkers identifying escape pathways that should be targeted after tumors develop resistance to a given antiangiogenic agent. A number of potential systemic, circulating, tissue and imaging biomarkers have emerged from recently completed phase I–III studies. Some of these are measured at baseline (for example VEGF polymorphisms), others are measured during treatment (such as hypertension, MRI-measured Ktrans, circulating angiogenic molecules or collagen IV), and all are mechanistically based. Some of these biomarkers might be pharmacodynamic (for example, increase in circulating VEGF, placental growth factor) while others have potential for predicting clinical benefit or identifying the escape pathways (for example, stromal-cell-derived factor 1α, interleukin-6). Most biomarkers are disease and/or agent specific and all of them need to be validated prospectively. We discuss the current challenges in establishing biomarkers of antiangiogenic therapy, define systemic, circulating, tissue and imaging biomarkers and their advantages and disadvantages, and comment on the future opportunities for validating biomarkers of antiangiogenic therapy.
Key Points
-
There are no validated biomarkers for selecting patients who will respond to antiangiogenic therapy; however, a number of systemic, circulating, tissue and imaging biomarkers are emerging and need to be prospectively validated
-
Antiangiogenic therapy can prune tumor vessels and 'normalize' the remaining vasculature, which decreases vessel diameter, vascular basement membrane thickness, vascular permeability, interstitial fluid pressure and increases pericyte coverage
-
A 'vascular normalization index' is associated with increased overall survival in patients with recurrent glioblastoma treated with cediranib, a pan-VEGFR tyrosine kinase inhibitor
-
Baseline levels of VEGF in tumors or the circulation seem to correlate with the outcome for some disease-agent combinations (bevacizumab with chemotherapy in metastatic breast cancer) but not others (metastatic colorectal cancer)
-
The most prevalent toxic effect of antiangiogenic therapy is hypertension, which when severe might be associated with certain genotypes but also with a better outcome in patients with metastatic breast cancer
-
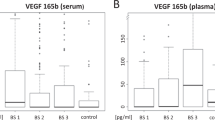
VEGF and placental growth factor levels increase after anti-angiogenic treatment, but other biomarkers are associated with poor outcome, which suggests that these pathways have a role in resistance to anti-VEGF therapies
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on SpringerLink
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Carmeliet, P. & Jain, R. K. Angiogenesis in cancer and other diseases. Nature 407, 249–257 (2000).
Jain, R. K. Molecular regulation of vessel maturation. Nat. Med. 9, 685–693 (2003).
Folkman, J. Tumor angiogenesis: therapeutic implications. N. Engl. J. Med. 285, 1182–1186 (1971).
Hurwitz, H. et al. Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N. Engl. J. Med. 350, 2335–2342 (2004).
Miller, K. et al. Paclitaxel plus bevacizumab versus paclitaxel alone for metastatic breast cancer. N. Engl. J. Med. 357, 2666–2676 (2007).
Rini, B. I. et al. Bevacizumab plus interferon alfa compared with interferon alfa monotherapy in patients with metastatic renal cell carcinoma: CALGB 90206. J. Clin. Oncol. 26, 5422–5328 (2008).
Sandler, A. et al. Paclitaxel-carboplatin alone or with bevacizumab for non-small-cell lung cancer. N. Engl. J. Med. 355, 2542–2550 (2006).
Escudier, B. et al. Sorafenib in advanced clear-cell renal-cell carcinoma. N. Engl. J. Med. 356, 125–134 (2007).
Motzer, R. J. et al. Sunitinib versus interferon alfa in metastatic renal-cell carcinoma. N. Engl. J. Med. 356, 115–124 (2007).
Llovet, J. M. et al. Sorafenib in advanced hepatocellular carcinoma. N. Engl. J. Med. 359, 378–390 (2008).
Giantonio, B. J. et al. Bevacizumab in combination with oxaliplatin, fluorouracil, and leucovorin (FOLFOX4) for previously treated metastatic colorectal cancer: results from the Eastern Cooperative Oncology Group Study E3200. J. Clin. Oncol. 25, 1539–1544 (2007).
Demetri, G. D. et al. Efficacy and safety of sunitinib in patients with advanced gastrointestinal stromal tumour after failure of imatinib: a randomised controlled trial. Lancet 368, 1329–1338 (2006).
Hughes, B. (2007). Novel risk-sharing scheme puts the spotlight on biomarkers. Nat. Rev. Drug Discov. 6, 945.
Sinha, G. Expensive cancer drugs with modest benefit ignite debate over solutions. J. Natl. Cancer Inst. 100, 1347–1349 (2008).
Karapetis, C. S. et al. K-ras mutations and benefit from cetuximab in advanced colorectal cancer. N. Engl. J. Med. 359, 1757–1765 (2008).
Oldenhuis, C. N., Oosting, S. F., Gietema, J. A. & de Vries, E. G. Prognostic versus predictive value of biomarkers in oncology. Eur. J. Cancer 44, 946–953 (2008).
McShane, L. M. et al. Reporting recommendations for tumor marker prognostic studies (REMARK). Nat. Clin. Pract. Oncol. 2, 416–422 (2005).
Batchelor, T. T. et al. AZD2171, a pan-VEGF receptor tyrosine kinase inhibitor, normalizes tumor vasculature and alleviates edema in glioblastoma patients. Cancer Cell 11, 83–95 (2007).
Ebos, J. M., Lee, C. R., Christensen, J. G., Mutsaers, A. J. & Kerbel, R. S. Multiple circulating proangiogenic factors induced by sunitinib malate are tumor-independent and correlate with antitumor efficacy. Proc. Natl Acad. Sci. USA 104, 17069–17074 (2007).
Kamoun, W. S. et al. Edema control by cediranib, a vascular endothelial growth factor receptor-targeted kinase inhibitor, prolongs survival despite persistent brain tumor growth in mice. J. Clin. Oncol. doi:10.1200/JCO.2008.19.9356 (2009).
Norden-Zfoni, A. et al. Blood-based biomarkers of SU11248 activity and clinical outcome in patients with metastatic imatinib-resistant gastrointestinal stromal tumor. Clin. Cancer Res. 13, 2643–2650 (2007).
Willett, C. G. et al. Efficacy, safety and biomarkers of neoadjuvant bevacizumab, radiation therapy and 5-Fluorouracil in rectal cancer: a multidisciplinary phase II study. J. Clin. Oncol. doi:10.1200/JCO.2008.21.1771 (2009).
Zhu, A. X. et al. Efficacy, safety and potential biomarkers of sunitinib monotherapy in advanced hepatocellular carcinoma: A phase II study. J. Clin. Oncol. doi: 10.1200/jco.2008.20.9908
Crabb, S. J. et al. Tumor cavitation: impact on objective response evaluation in trials of angiogenesis inhibitors in non-small-cell lung cancer. J. Clin. Oncol. 27, 404–410 (2009).
Hudis, C. A. Trastuzumab—mechanism of action and use in clinical practice. N. Engl. J. Med. 357, 39–51 (2007).
Cameron, D. A. & Stein, S. Drug Insight: intracellular inhibitors of HER2--clinical development of lapatinib in breast cancer. Nat. Clin. Pract. Oncol. 5, 512–520 (2008).
Carmeliet, P. Angiogenesis in life, disease and medicine. Nature 438, 932–936 (2005).
Jain, R. K., Duda, D. G., Clark, J. W. & Loeffler, J. S. Lessons from phase III clinical trials on anti-VEGF therapy for cancer. Nat. Clin. Pract. Oncol. 3, 24–40 (2006).
Jain, R. K. Normalization of tumor vasculature: an emerging concept in antiangiogenic therapy. Science 307, 58–62 (2005).
Winkler, F. et al. Kinetics of vascular normalization by VEGFR2 blockade governs brain tumor response to radiation: role of oxygenation, angiopoietin-1, and matrix metalloproteinases. Cancer Cell 6, 553–563 (2004).
Willett, C. G. et al. Direct evidence that the VEGF-specific antibody bevacizumab has antivascular effects in human rectal cancer. Nat. Med. 10, 145–147 (2004).
Willett, C. G. et al. Surrogate markers for antiangiogenic therapy and dose-limiting toxicities for bevacizumab with radiation and chemotherapy: continued experience of a phase I trial in rectal cancer patients. J. Clin. Oncol. 23, 8136–8139 (2005).
Kerbel, R. S. Tumor angiogenesis. N. Engl. J. Med. 358, 2039–2049 (2008).
Rini, B. I. et al. Association of diastolic blood pressure (dBP) ≥90 mmHg with overall survival (OS) in patients treated with axitinib (AG-013736) [Abstract]. ASCO Meeting Abstracts 26, 3543 (2008).
Shojaei, F. et al. Tumor refractoriness to anti-VEGF treatment is mediated by CD11b+Gr1+ myeloid cells. Nat. Biotechnol. 25, 911–920 (2007).
Hamzah, J. et al. Vascular normalization in Rgs5-deficient tumours promotes immune destruction. Nature 453, 410–414 (2008).
Batchelor, T. T. et al. A multidisciplinary phase II study of AZD2171 (cediranib), an oral pan-VEGF receptor tyrosine kinase inhibitor, in patients with recurrent glioblastoma [Abstract]. AACR Meeting Abstracts LB-247 (2008).
Schneider, B. P. et al. Association of vascular endothelial growth factor and vascular endothelial growth factor receptor-2 genetic polymorphisms with outcome in a trial of paclitaxel compared with paclitaxel plus bevacizumab in advanced breast cancer: ECOG 2100. J. Clin. Oncol. 26, 4672–4678 (2008).
Burstein, H. J. et al. VEGF as a marker for outcome among advanced breast cancer patients receiving anti-VEGF therapy with bevacizumab and vinorelbine chemotherapy. Clin. Cancer Res. 14, 7871–7877 (2008).
Jubb, A. M. et al. Impact of vascular endothelial growth factor-A expression, thrombospondin-2 expression, and microvessel density on the treatment effect of bevacizumab in metastatic colorectal cancer. J. Clin. Oncol. 24, 217–227 (2006).
Dowlati, A., Gray, R., Sandler, A. B., Schiller, J. H. & Johnson, D. H. Cell adhesion molecules, vascular endothelial growth factor, and basic fibroblast growth factor in patients with non-small cell lung cancer treated with chemotherapy with or without bevacizumab—an Eastern Cooperative Oncology Group Study. Clin. Cancer Res. 14, 1407–1412 (2008).
Jain, R. K. Lessons from multidisciplinary translational trials on anti-angiogenic therapy of cancer. Nat. Rev. Cancer 8, 309–316 (2008).
Ferrara, N., Hillan, K. J., Gerber, H. P. & Novotny, W. Discovery and development of bevacizumab, an anti-VEGF antibody for treating cancer. Nat. Rev. Drug Discov. 3, 391–400 (2004).
Dvorak, H. F. Vascular permeability factor/vascular endothelial growth factor: a critical cytokine in tumor angiogenesis and a potential target for diagnosis and therapy. J. Clin. Oncol. 20, 4368–4380 (2002).
Sorensen, A. G., Batchelor, T. T., Wen, P. Y., Zhang, W. T. & Jain, R. K. Response criteria for glioma. Nat. Clin. Pract. Oncol. 5, 634–644 (2008).
Heymach, J. V. et al. Baseline VEGF as a potential predictive biomarker of vandetanib clinical benefit in patients with advanced NSCLC [Abstract]. ASCO Meeting Abstracts 26, 8009 (2008).
Tannir, N. M. et al. A randomized phase II trial of sorafenib versus sorafenib plus low-dose interferon-alfa: Clinical results and biomarker analysis [Abstract]. ASCO Meeting Abstracts 26, 5093 (2008).
Rini, B. I. et al. Antitumor activity and biomarker analysis of sunitinib in patients with bevacizumab-refractory metastatic renal cell carcinoma. J. Clin. Oncol. 26, 3743–3748 (2008).
Deprimo, S. E. et al. Circulating protein biomarkers of pharmacodynamic activity of sunitinib in patients with metastatic renal cell carcinoma: modulation of VEGF and VEGF-related proteins. J. Transl. Med. 5, 32 (2007).
Drevs, J. et al. Phase I clinical study of AZD2171, an oral vascular endothelial growth factor signaling inhibitor, in patients with advanced solid tumors. J. Clin. Oncol. 25, 3045–3054 (2007).
Mita, M. M. et al. A phase II, pharmacokinetic, and biologic study of semaxanib and thalidomide in patients with metastatic melanoma. Cancer Chemother. Pharmacol. 59, 165–174 (2007).
Motzer, R. J. et al. Activity of SU11248, a multitargeted inhibitor of vascular endothelial growth factor receptor and platelet-derived growth factor receptor, in patients with metastatic renal cell carcinoma. J. Clin. Oncol. 24, 16–24 (2006).
Saltz, L. B. et al. Phase II trial of sunitinib in patients with metastatic colorectal cancer after failure of standard therapy. J. Clin. Oncol. 25, 4793–4799 (2007).
Fischer, C. et al. Anti-PlGF inhibits growth of VEGF(R)-inhibitor-resistant tumors without affecting healthy vessels. Cell 131, 463–475 (2007).
Verheul, H. M. et al. Platelets take up the monoclonal antibody bevacizumab. Clin. Cancer Res. 13, 5341–5347 (2007).
Ebos, J. M. et al. Accelerated metastasis after short-term treatment with a potent inhibitor of tumor angiogenesis. Cancer Cell 15, 232–239 (2009).
Phase III C-08 study of Avastin in early-stage colon cancer does not meet primary endpoint [online], http://www.roche.com/media_releases/med-cor-009-04-22.htm (2009).
Horowitz, N. S. et al. A multidisciplinary phase II study of bevacizumab combined with oxaliplatin, gemcitabine in women with recurrent mullerian carcinoma [Abstract]. AACR Annual Abstracts 4484 (2008).
Ince, W. L. et al. Association of k-ras, b-raf, and p53 status with the treatment effect of bevacizumab. J. Natl Cancer Inst. 97, 981–989 (2005).
Wilson, P. M. et al. Use of intratumoral mRNA expression of genes involved in angiogenesis and HIF1 pathway to predict outcome to VEGFR tyrosine kinase inhibitor in patients enrolled in CONFIRM1 and CONFIRM2 [Abstract]. ASCO Meeting Abstracts 26, 4002 (2008).
Kohne, C. et al. Final results of CONFIRM 2: A multinational, randomized, double-blind, phase III study in 2nd line patients with metastatic colorectal cancer receiving FOLFOX4 and PTK787/ZK 222584 (PTK/ZK) or placebo [Abstract]. ASCO Meeting Abstracts 25, 4033 (2007).
Schultheis, A. M. et al. Polymorphisms and clinical outcome in recurrent ovarian cancer treated with cyclophosphamide and bevacizumab. Clin. Cancer Res. 14, 7554–7563 (2008).
Loges, S., Mazzone, M., Hohensinner, P. & Carmeliet, P. Silencing or fueling metastasis with VEGF inhibitors: antiangiogenesis revisited. Cancer Cell 15, 167–170 (2009).
Paez-Ribes, M. et al. Antiangiogenic therapy elicits malignant progression of tumors to increased local invasion and distant metastasis. Cancer Cell 15, 220–231 (2009).
Duda, D. G. et al. A comparative study of circulating endothelial cells (CECs) and circulating progenitor cells (CPCs) kinetics in four multidisciplinary phase 2 studies of antiangiogenic agents [Abstract]. ASCO Meeting Abstracts 26, 3544 (2008).
Patterson, D. M., Padhani, A. R. & Collins, D. J. Technology insight: water diffusion MRI—a potential new biomarker of response to cancer therapy. Nat. Clin. Pract. Oncol. 5, 220–233 (2008).
Hamstra, D. A. et al. Functional diffusion map as an early imaging biomarker for high-grade glioma: correlation with conventional radiologic response and overall survival. J. Clin. Oncol. 26, 3387–3394 (2008).
Sorensen, A. G. Magnetic resonance as a cancer imaging biomarker. J. Clin. Oncol. 24, 3274–3281 (2006).
Sorensen, A. G. et al. A “vascular normalization index” as potential mechanistic biomarker to predict survival after a single dose of cediranib in recurrent glioblastoma patients: Insights from a phase II study. Cancer Res. (in press).
Chen, W. et al. Predicting treatment response of malignant gliomas to bevacizumab and irinotecan by imaging proliferation with [18F] fluorothymidine positron emission tomography: a pilot study. J. Clin. Oncol. 25, 4714–4721 (2007).
Tofts, P. S. et al. Estimating kinetic parameters from dynamic contrast-enhanced T(1)-weighted MRI of a diffusable tracer: standardized quantities and symbols. J. Magn. Reson. Imaging 10, 223–232 (1999).
Motzer, R. J. et al. Prognostic nomogram for sunitinib in patients with metastatic renal cell carcinoma. Cancer 113, 1552–1558 (2008).
Sandler, A. B. et al. Retrospective evaluation of the clinical and radiographic risk factors associated with severe pulmonary hemorrhage in first-line advanced, unresectable non-small-cell lung cancer treated with carboplatin and paclitaxel plus bevacizumab. J. Clin. Oncol. 27, 1405–1412 (2009).
Casanovas, O., Hicklin, D. J., Bergers, G. & Hanahan, D. Drug resistance by evasion of antiangiogenic targeting of VEGF signaling in late-stage pancreatic islet tumors. Cancer Cell 8, 299–309 (2005).
Relf, M. et al. Expression of the angiogenic factors vascular endothelial cell growth factor, acidic and basic fibroblast growth factor, tumor growth factor beta-1, platelet-derived endothelial cell growth factor, placenta growth factor, and pleiotrophin in human primary breast cancer and its relation to angiogenesis. Cancer Res. 57, 963–969 (1997).
Yoshiji, H., Harris, S. R. & Thorgeirsson, U. P. Vascular endothelial growth factor is essential for initial but not continued in vivo growth of human breast carcinoma cells. Cancer Res. 57, 3924–3928 (1997).
Liu, G. et al. Dynamic contrast-enhanced magnetic resonance imaging as a pharmacodynamic measure of response after acute dosing of AG-013736, an oral angiogenesis inhibitor, in patients with advanced solid tumors: results from a phase I study. J. Clin. Oncol. 23, 5464–5473 (2005).
Thomas, A. L. et al. Phase I study of the safety, tolerability, pharmacokinetics, and pharmacodynamics of PTK787/ZK 222584 administered twice daily in patients with advanced cancer. J. Clin. Oncol. 23, 4162–4171 (2005).
Zhu, A. X. et al. Early antiangiogenic activity of bevacizumab evaluated by computed tomography perfusion scan in patients with advanced hepatocellular carcinoma. Oncologist 13, 120–125 (2008).
Yao, J. C. et al. Targeting vascular endothelial growth factor in advanced carcinoid tumor: a random assignment phase II study of depot octreotide with bevacizumab and pegylated interferon alpha-2b. J. Clin. Oncol. 26, 1316–1323 (2008).
de Bazelaire, C. et al. Magnetic resonance imaging-measured blood flow change after antiangiogenic therapy with PTK787/ZK 222584 correlates with clinical outcome in metastatic renal cell carcinoma. Clin. Cancer Res. 14, 5548–5554 (2008).
Acknowledgements
The authors thank the members of the Steele Lab, especially M. Ancukiewicz, Y. Boucher, E. di Tomaso, and L. Xu and M. Buyse, H. Chen, A. Grothey, C. Hudis, R. Horvitz, and A. Marshall for their helpful comments on this manuscript. The authors' work is supported by grants from the National Cancer institute P01-CA80124, P41-rr14075, R01-CA115767, R01-CA85140, R01CA126642, R21-CA99237, R21-CA117079, R01-CA129371, R01CA57683, K24-CA125440, Federal share/NCI Proton Beam Program income, M01-RR-01066, Harvard Clinical and Translational Science Center (CTSC) grant; the National Foundation for Cancer research; the Richard and Nancy Simches Endowment for Brain Tumor Research; the Montesi Family Fund; and MIND institute.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
R. K. Jain declares he is a Consultant for AstraZenenca, Dyax, Millenium and SynDevRx. He is on the Speakers' Bureau for Pfizer and Roche, and receives grant/research support from AstraZenenca and Dyax. He is a stockholder for SynDevRx. C. G. Willett is on the Speakers' Bureau for Genentech. A. X. Zhu declares he is a consultant for Bayer and Genentech. T. T. Batchelor declares he is a consultant for Exelixis, EMD-Serono, Genentech and ImClone Systems. He receives grant/research support from AstraZeneca and Millenium, and is on the Speakers Bureau for Schering–Plough. A. G. Sorensen declares he is a consultant for AstraZeneca, Genentech and Millenium and also receives grant/research support from AstraZeneca, Genentech, Exelixis, Millenium, Novartis and Schering–Plough. The others authors declare no competing interests.
Supplementary information
Rights and permissions
About this article
Cite this article
Jain, R., Duda, D., Willett, C. et al. Biomarkers of response and resistance to antiangiogenic therapy. Nat Rev Clin Oncol 6, 327–338 (2009). https://doi.org/10.1038/nrclinonc.2009.63
Issue Date:
DOI: https://doi.org/10.1038/nrclinonc.2009.63
This article is cited by
-
Angiogenic signaling pathways and anti-angiogenic therapy for cancer
Signal Transduction and Targeted Therapy (2023)
-
Cancer combination therapies by angiogenesis inhibitors; a comprehensive review
Cell Communication and Signaling (2022)
-
Senescence and cancer — role and therapeutic opportunities
Nature Reviews Clinical Oncology (2022)
-
Bridging the macro to micro resolution gap with angiographic optical coherence tomography and dynamic contrast enhanced MRI
Scientific Reports (2022)
-
Drug susceptibility testing of circulating lung cancer cells for personalized treatment
Medical Oncology (2022)