Abstract
Objective:
To investigate the effect of postnatal age at patent ductus arteriosus (PDA) ligation on postoperative need for cardiotropic support.
Study Design:
A significant proportion of premature infants with a hemodynamically significant ductus arteriosus (HSDA) require surgical intervention. The relationship of postnatal maturation to postoperative cardiorespiratory stability is poorly understood. All preterm neonates who underwent PDA ligation between October 2002 and September 2004 were identified and divided according to postnatal age at ductal ligation, into early (⩽4 weeks, n=29) and late (>4 weeks, n=36) groups. Neonatal birth demographics and morbidities, characteristics of the HSDA and reason for ligation were reviewed. Indices of cardiorespiratory stability (for example heart rate, mean arterial pressure) were recorded before and 1, 4, 8, 12 and 24 h following ligation. Details of perioperative cardiovascular interventions (for example crystalloid boluses, cardiotropic agents) were recorded.
Result:
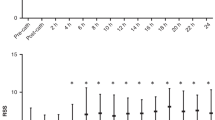
There were no differences in baseline neonatal demographics between the groups although a greater number of babies requiring early ligation had contraindication to indomethacin as the main reason for ligation. Early PDA ligation was associated with increased postoperative cardiotrope requirement (27.6 vs 5.6%, P=0.02) and decreased systolic blood pressure 8 h after intervention (P<0.05). Although increased oxygenation index was observed in both groups during the first 12 h it was only sustained to 24 h in the early group (P<0.05). Age at ligation remained a significant risk factor for postoperative cardiotrope requirement on multiple logistic regression analysis.
Conclusion:
Surgical ligation of the ductus arteriosus in preterm infants less than 28 days old is associated with oxygenation difficulties, decreased systolic arterial pressure and an increased need for cardiotropic support in the initial 24 postoperative hours. These data suggest the need to prospectively characterize perioperative cardiovascular physiology and identify predictive factors of clinical deterioration.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Dollberg S, Lusky A, Reichman B . Patent ductus arteriosus, indomethacin and necrotizing enterocolitis in very low birth weight infants: a population-based study. J Pediatr Gastroenterol Nutr 2005; 40 (2): 184–188.
Ellison RC, Peckham GJ, Lang P, Talner NS, Lerer TJ, Lin L et al. Evaluation of the preterm infant for patent ductus arteriosus. Pediatrics 1983; 71 (3): 364–372.
Teixeira LS, McNamara PJ . Enhanced intensive care for the neonatal ductus arteriosus. Acta Paediatr 2006; 95 (4): 394–403.
Trus T, Winthrop AL, Pipe S, Shah J, Langer JC, Lau GY . Optimal management of patent ductus arteriosus in the neonate weighing less than 800 g. J Pediatr Surg 1993; 28 (9): 1137–1139.
Moin F, Kennedy KA, Moya FR . Risk factors predicting vasopressor use after patent ductus arteriosus ligation. Am J Perinatol 2003; 20 (6): 313–320.
Noori S, Friedlich P, Seri I, Wong P . Changes in myocardial function and hemodynamics after ligation of the ductus arteriosus in preterm infants. J Pediatr 2007; 150 (6): 597–602.
Rowland DG, Gutgesell HP . Noninvasive assessment of myocardial contractility, preload, and afterload in healthy newborn infants. Am J Cardiol 1995; 75 (12): 818–821.
McNamara PJ, Sehgal A . Towards rational management of the patent ductus arteriosus: the need for disease staging. Arch Dis Child Fetal Neonatal Ed 2007; 92 (6): F424–F427.
Stevens B, Johnston C, Petryshen P, Taddio A . Premature infant pain profile: development and initial validation. Clin J Pain 1996; 12 (1): 13–22.
Bell MJ, Ternberg JL, Feigin RD, Keating JP, Marshall R, Barton L et al. Neonatal necrotizing enterocolitis. Therapeutic decisions based upon clinical staging. Ann Surg 1978; 187 (1): 1–7.
Papile LA, Burstein J, Burstein R, Koffler H . Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1500 gm. J Pediatr 1978; 92 (4): 529–534.
Bose CL, Laughon MM . Patent ductus arteriosus: lack of evidence for common treatments. Arch Dis Child Fetal Neonatal Ed 2007; 92 (6): F498–F502.
Laughon MM, Simmons MA, Bose CL . Patency of the ductus arteriosus in the premature infant: is it pathologic? Should it be treated? Curr Opin Pediatr 2004; 16 (2): 146–151.
Cassady G, Crouse DT, Kirklin JW, Strange MJ, Joiner CH, Godoy G et al. A randomized, controlled trial of very early prophylactic ligation of the ductus arteriosus in babies who weighed 1000 g or less at birth. N Engl J Med 1989; 320 (23): 1511–1516.
Jaillard S, Larrue B, Rakza T, Magnenant E, Warembourg H, Storme L . Consequences of delayed surgical closure of patent ductus arteriosus in very premature infants. Ann Thorac Surg 2006; 81 (1): 231–234.
Chorne N, Leonard C, Piecuch R, Clyman RI . Patent ductus arteriosus and its treatment as risk factors for neonatal and neurodevelopmental morbidity. Pediatrics 2007; 119 (6): 1165–1174.
Kabra NS, Schmidt B, Roberts RS, Doyle LW, Papile L, Fanaroff A . Neurosensory impairment after surgical closure of patent ductus arteriosus in extremely low birth weight infants: results from the trial of indomethacin prophylaxis in preterms. J Pediatr 2007; 150 (3): 229–234.
Little DC, Pratt TC, Blalock SE, Krauss DR, Cooney DR, Custer MD . Patent ductus arteriosus in micropreemies and full-term infants: the relative merits of surgical ligation versus indomethacin treatment. J Pediatr Surg 2003; 38 (3): 492–496.
Zbar RI, Chen AH, Behrendt DM, Bell EF, Smith RJ . Incidence of vocal fold paralysis in infants undergoing ligation of patent ductus arteriosus. Ann Thorac Surg 1996; 61 (3): 814–816.
Taylor AF, Morrow WR, Lally KP, Kinsella JP, Gerstmann DR, deLemos RA . Left ventricular dysfunction following ligation of the ductus arteriosus in the preterm baboon. J Surg Res 1990; 48 (6): 590–596.
Takahashi Y, Harada K, Ishida A, Tamura M, Tanaka T, Takada G . Changes in left ventricular volume and systolic function before and after the closure of ductus arteriosus in full-term infants. Early Hum Dev 1996; 44 (1): 77–85.
Ratner I, Perelmuter B, Toews W, Whitfield J . Association of low systolic and diastolic blood pressure with significant patent ductus arteriosus in the very low birth weight infant. Crit Care Med 1985; 13 (6): 497–500.
Crepaz R, Pitscheider W, Radetti G, Gentili L . Age-related variation in left ventricular myocardial contractile state expressed by the stress velocity relation. Pediatr Cardiol 1998; 19 (6): 463–467.
Anderson PA . The heart and development. Semin Perinatol 1996; 20 (6): 482–509.
Meier SD, Eble BK, Stapleton GE, Morales DL, Chang AC, Andropoulos DB . Mesenteric oxyhemoglobin desaturation improves with patent ductus arteriosus ligation. J Perinatol 2006; 26 (9): 562–564.
Zaramella P, Freato F, Quaresima V, Ferrari M, Bartocci M, Rubino M et al. Surgical closure of patent ductus arteriosus reduces the cerebral tissue oxygenation index in preterm infants: a near-infrared spectroscopy and Doppler study. Pediatr Int 2006; 48 (3): 305–312.
Szymankiewicz M, Hodgman JE, Siassi B, Gadzinowski J . Mechanics of breathing after surgical ligation of patent ductus arteriosus in newborns with respiratory distress syndrome. Biol Neonate 2004; 85 (1): 32–36.
McCurnin DC, Yoder BA, Coalson J, Grubb P, Kerecman J, Kupferschmid J et al. Effect of ductus ligation on cardiopulmonary function in premature baboons. Am J Respir Crit Care Med 2005; 172 (12): 1569–1574.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Teixeira, L., Shivananda, S., Stephens, D. et al. Postoperative cardiorespiratory instability following ligation of the preterm ductus arteriosus is related to early need for intervention. J Perinatol 28, 803–810 (2008). https://doi.org/10.1038/jp.2008.101
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2008.101
Keywords
This article is cited by
-
Biventricular function in preterm infants with patent ductus arteriosus ligation: A three-dimensional echocardiographic study
Pediatric Research (2024)
-
Left ventricular function before and after percutaneous patent ductus arteriosus closure in preterm infants
Pediatric Research (2023)
-
Response categorization and outcomes in extremely premature infants born at 22–26 weeks gestation that received inhaled nitric oxide for hypoxic respiratory failure
Journal of Perinatology (2023)
-
Safety and Short-Term Outcomes for Infants < 2.5 kg Undergoing PDA Device Closure: A C3PO Registry Study
Pediatric Cardiology (2023)
-
Phenotyping respiratory decompensation following definitive closure of the patent ductus arteriosus in preterm infants
Journal of Perinatology (2022)