Abstract
Acute myeloid leukemia (AML) is the most common acute leukemia in adults, with an incidence of over 20 000 cases per year in the United States alone. Large chromosomal translocations as well as mutations in the genes involved in hematopoietic proliferation and differentiation result in the accumulation of poorly differentiated myeloid cells. AML is a highly heterogeneous disease; although cases can be stratified into favorable, intermediate and adverse-risk groups based on their cytogenetic profile, prognosis within these categories varies widely. The identification of recurrent genetic mutations, such as FLT3-ITD, NMP1 and CEBPA, has helped refine individual prognosis and guide management. Despite advances in supportive care, the backbone of therapy remains a combination of cytarabine- and anthracycline-based regimens with allogeneic stem cell transplantation for eligible candidates. Elderly patients are often unable to tolerate such regimens, and carry a particularly poor prognosis. Here, we review the major recent advances in the treatment of AML.
Similar content being viewed by others
Introduction
Acute myeloid leukemia (AML) is the most common acute leukemia in adults, accounting for ~80 percent of cases in this group.1 Within the United States, the incidence of AML ranges from three to five cases per 100 000 population. In 2015 alone, an estimated 20 830 new cases were diagnosed, and over 10 000 patients died from this disease.2 The incidence of AML increases with age, from ~1.3 per 100 000 population in patients less than 65 years old, to 12.2 cases per 100 000 population in those over 65 years. Although advances in the treatment of AML have led to significant improvements in outcomes for younger patients, prognosis in the elderly who account for the majority of new cases remains poor.3 Even with current treatments, as much as 70% of patients 65 years or older will die of their disease within 1 year of diagnosis.4
Pathophysiology
AML can arise in patients with an underlying hematological disorder, or as a consequence of prior therapy (for example, exposure to topoisomerases II, alkylating agents or radiation).5 However in majority of cases, it appears as a de novo malignancy in previously healthy individuals. Regardless of its etiology, the pathogenesis of AML involves the abnormal proliferation and differentiation of a clonal population of myeloid stem cells. Well-characterized chromosomal translocations, such as t(8:21) in core-binding factor AML (CBF-AML) or t(15:17) in acute promyelocytic leukemia (APL) result in the formation of chimeric proteins (RUNX1-RUNX1T1 and PML-RARA, respectively), which alter the normal maturation process of myeloid precursor cells. In addition to large chromosomal rearrangements, molecular changes have also been implicated in the development of AML. In fact, genetic mutations are identified in more than 97% of cases,6 often in the absence of any large chromosomal abnormality.7 Studies of animal models at the turn of the century led to the development of a two-hit model of leukemogenesis, which offers a conceptual framework for classifying the various mutations associated with AML.8 According to this model, class I mutations which result in the activation of pro-proliferative pathways must occur in conjunction with class II mutations which impair normal hematopoietic differentiation in order for leukemia to develop.9, 10 Common class I mutations, such as FLT3 (internal tandem duplications, ITD, and tyrosine kinase domain mutations, TKD), K/NRAS, TP53 and c-KIT are found in ~28, 12, 8 and 4% of cases, respectively.7 Studies of solid and hematological malignancies have also highlighted the role of signal transducer and activator of transcription 3 (STAT3) in the stimulation of cellular proliferation and survival.11, 12, 13 Enhanced tyrosine phosphorylation of STAT3 whether due to increased secretion of cytokines, such as IL-6(ref. 14) or mutations in receptor tyrosine kinases (for example, FLT3 duplications15 or less frequently JAK2)16 is seen in up to 50% of AML cases and signifies a worse prognosis. Notable class II mutations include NPM1 and CEBPA, which are found in ~27% and 6% of cases, respectively, and confer a better prognosis.7 Alterations in genes involved in epigenetic regulation have recently emerged as a third class of mutations, with downstream effects on both cellular differentiation and proliferation. These include mutations in the DNA-methylation related genes DNMT3A, TET2, and IDH-1 and IDH-2,6, 7 which are found in more than 40% of AML cases.
Despite significant advances, much remains to be discovered on the exact contribution of these individual mutations to the development of AML. As suggested by the ‘two-hit model,’ the pathogenesis and behavior of AML depends heavily on the interactions between different somatic alterations and chromosomal rearrangements. Thus, the c-KIT mutation has been associated with t(8;21) or inv(16), and its presence carries significant implications regarding prognosis. Similarly, NMP1 (a class II mutation) frequently occurs in conjunction with the class I mutation FLT3-ITD, or mutations in the epigenetic genes DNMT3A and IDH-1 or IDH-2.6
Most of the clinical manifestations of AML reflect the accumulation of malignant, poorly differentiated myeloid cells within the bone marrow, peripheral blood and infrequently in other organs. The majority of patients presents with a combination of leukocytosis and signs of bone marrow failure such as anemia and thrombocytopenia. Fatigue, anorexia and weight loss are common complaints; lymphadenopathy and organomegaly are not typically seen. If left untreated, death usually ensues within months of diagnosis secondary to infection or bleeding. The diagnosis of acute leukemia is established by the presence of 20% or more blasts in the bone marrow or peripheral blood.17 AML is further diagnosed by demonstrating the myeloid origin of these cells through testing for myeloperoxidase activity, immunophenotyping or documenting the presence of Auer rods. The latter finding consists of azurophilic, often needle-shaped cytoplasmic inclusion bodies that are commonly seen in APL, acute myelomonocytic leukemia and the majority of AML with t(8;21). The diagnosis of AML can also be established in the presence of an extramedullary tissue infiltrate, or a documented t(8;21), inv(16) or t(15;17) in the appropriate clinical setting, regardless of the blast percentage.18
Classification
The French–American–British classification system represents the first attempt to distinguish between different types of AML. Established in 1976, it defines eight subtypes (M0 through M7) based on the morphological and cyto-chemical characteristics of the leukemic cells. In 2001, as part of an effort to integrate advances made in the diagnosis and management of AML, the World Health Organization (WHO) introduced a new classification system followed by a revised version in 2008.18 Later in 2016 a new revised version was released, the WHO classification of AML distinguishes itself by incorporating genetic information with morphology, immunophenotype and clinical presentation to define six major disease entities: AML with recurrent genetic abnormalities; AML with myelodysplasia-related features; therapy-related AML; AML not otherwise specified; myeloid sarcoma; and myeloid proliferation related to Down syndrome (Table 1).19 Among cases of AML with recurrent genetic abnormalities, 11 subtypes are further delineated according to distinct chromosomal translocations. In addition, the provisional entities AML with mutated NPM1 and AML with mutated CEBPA were introduced as part of the 2008 revision,18 while AML with BCR-ABL1 and AML with mutated RUNX1 were introduced as part of the 2016 revision.19 Genetic abnormalities also inform the diagnosis of AML with myelodysplasia-related changes: along with a history of MDS or morphological evidence of dysplasia in two or more myeloid cell lineages, the presence of myelodysplasia-related cytogenetic abnormalities such as monosomy 5 or 7, and deletion 5q or 7q identify cases of AML with myelodysplasia-related features.
Prognostic factors
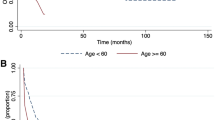
Accurate assessment of prognosis is central to the management of AML. By stratifying patients according to their risk of treatment resistance or treatment-related mortality (TRM), prognostic factors help guide the physician in deciding between standard or increased treatment intensity, consolidation chemotherapy or allogenic hematopoietic stem cell transplant, or more fundamentally in choosing between established or investigational therapies. Among clinical factors, increased age and poor performance status are both associated with lower rates of complete remission (CR) and decreased overall survival (OS).3, 20 Age and performance status at diagnosis similarly help to predict the risk of TRM, although multivariate model analyses suggest that other variables such as platelet count, serum creatinine or albumin rather than age itself account for most of the increased risk of TRM seen in older patients.21 Therapy-related AML and AML associated with a prior hematological malignancy also carry a significantly poorer prognosis.22 Although clinical factors have an important role in guiding therapy, cytogenetic changes constitute the single strongest prognostic factor for CR and OS in AML. Accordingly, cases of AML can be stratified into favorable, intermediate or adverse prognostic risk groups based on their cytogenetic profile alone. The chromosomal rearrangements t(8;21), t(15;17) or inv(16) all confer a favorable prognosis,17, 23 with a 3 year OS of 66% and 33% in patients younger and older than 60 years, respectively.24 In contrast, cytogenetic changes such as a complex karyotype (that is, three or more chromosomal abnormalities in the absence of any of the recurrent genetic abnormalities identified in the WHO 2008 classification), monosomy 5 or 7, t(6;9), inv(3) or 11q changes other than t(9;11) have all been associated with a significantly higher risk of treatment failure and death (Table 2).24 AML cases with an intermediate prognostic risk mainly constitute of patients with normal cytogenetics (CN-AML).17, 24
Gene mutations have helped further refine risk stratification based on cytogenetic changes alone. Among patients with t(8;21), the presence of a c-KIT mutation significantly increases the risk of relapse, and decreases OS to levels comparable to those of patient with intermediate-risk AML.6, 23, 25 Although there is some evidence that the presence of c-KIT mutations similarly lowers prognosis in patients with inv(16),26 recent studies have failed to show any prognostic impact in this subset of cases.6, 27, 28 Molecular changes have a particularly important role in refining the prognosis of patients with CN-AML, which includes nearly half of de novo AML cases. Thus CN-AML with a mutated CEBPA or a mutated NPM1 in the absence of FLT3-ITD has been identified as having a prognostic risk similar to that of AML with favorable cytogenetic changes.17, 29 The favorable prognostic impact of CEBPA mutations has been further refined to biallelic mutations only.30 On the other hand, multiple studies29, 31 including a meta-analysis of relapse-free survival (RFS) and OS in patients with CN-AML <60 years of age have consistently shown the presence of FLT3-ITD to be associated with a worsened prognosis.6, 32 This has led to the classification of CN-AML with FLT3-ITD into the adverse prognostic-risk group.23, 33 As with CEBPA mutations, the prognostic impact of FLT3-ITD may depend on the presence of biallelic mutations. Several studies have shown a significantly worse prognosis in patients with higher mutant to wild-type allelic ratios.34, 35 TP53 mutations, which are found in only 2– 8% of cases,6, 7 occur more frequently in cases with unfavorable cytogenetic and a complex karyotype.36 However regardless of the cytogenetic profile, TP53 mutations are associated with a very poor prognosis10 and may in fact represent the single worst genetic prognostic factor.36 Mutations in DNA-related genes also carry important implications for the prognosis and treatment of AML. The presence of a mutated DNA methyl transferase gene DNMT3A has been associated with a worsened prognosis in CN-AML and adverse-risk AML.37 Partial tandem duplications of KMT2A (previously known as MLL), which encodes a histone methyltransferase, have also been associated with a worse prognosis in CN-AML.6, 10, 36 The prognostic impact of IDH-1/IDH-2 mutations is less well established and is likely modified by co-occurring mutations. Among cases of FLT3-ITD-negative and NPM1-mutated CN-AML, IDH-1/IDH-2 mutations have been shown to improve OS.6 However a recent study of 826 patients with known IDH-1 and IDH-2 status found no prognostic impact on treatment response or OS.38 Further analysis is required to delineate the role of DNA-related genes in OS and treatment response. In addition to genetic profiling at the time of diagnosis, information gained after treatment initiation plays a growing role in refining patient prognosis: As could be expected, individuals who achieve CR (defined morphologically as a blast count of <5% of total nonerythroid cells in the bone marrow) after induction therapy have a significantly increased survival compared with patients with treatment resistant AML.39, 40 Survival among patients achieving CR is further influenced by the correction or persistence of thrombocytopenia, with a shorter duration of survival observed in the latter group.40 More recently, techniques such as real-time PCR and flow cytometry have been used to measure the presence of minimal residual disease among patients in CR. Persistently elevated levels of RUNX1-RUNX1T1 transcripts after induction therapy in patients with t(8;21) AML are thus associated with an increased incidence of relapse.41, 42 Similarly among patients with intermediate-risk disease, detection of minimal residual disease by flow cytometry is an independent predictor of relapse and survival43, 44 and carries important implications for management.45
Established treatments
Eligible patients first undergo induction therapy to achieve CR. Unfortunately, minimal residual disease often persists in CR, and relapse will inevitably occur if treatment is discontinued. Therefore, a favorable response to induction therapy should be followed by consolidation therapy in order to eradicate any residual disease and achieve lasting remission. The mainstay of induction therapy consists of the ‘7+3’ regimen, which combines 7 days of continuous infusion cytarabine with 3 days of anthracycline. It is generally offered to patients with an intermediate to favorable prognosis and a low risk of TRM (for example, younger patients with good performance status, normal creatinine, albumin and platelet count).23 Studies of induction regimens using either daunorubicin at 60 or 90 mg/m2, or idarubicin at 12 mg/m2 have shown similar rates of CR and survival.23, 46, 47 A subset of patients with DNMT3A and KMT2A mutations, which represents a poor prognostic marker, may however benefit from higher doses of daunorubicin.6 Standard dosing of cytarabine consists of 100–200 mg/m2 daily administered as a continuous infusion over 7 days. Although studies have shown greater efficacy at higher doses, this added benefit is small and accrued at the cost of increased toxicity;23, 48, 49 induction therapy with high-dose cytarabine is generally reserved for refractory disease. The combination of fludarabine, cytarabine, G-CSF and idarubicin (FLAG-IDA), which was traditionally used for the treatment of relapse, has also been shown to be a reasonable alternative to standard induction regimens and results in similar CR rates and OS overall but higher rates of CR after a single course.50
An optimal approach to elderly patients with AML has not been established. Individuals over the age of 65 are more likely to present with an adverse cytogenetic-risk profile, are less likely to respond to chemotherapy and are often more susceptible to treatment-related toxicities. However despite a significantly worse prognosis, induction therapy improves survival in patients over the age of 65 when compared with supportive care and palliative chemotherapy,51 and should be pursued whenever possible. Hypomethylating agents, traditionally used for the treatment of myelodysplastic syndrome (MDS), have also shown efficacy in elderly patients with AML. Evidence of a therapeutic benefit was first demonstrated in post hoc analyses of patients with MDS who were retrospectively found to meet diagnostic criteria for AML under the WHO classification.52 A 2012 randomized trial of the hypomethylating agent decitabine versus supportive care or low-dose cytarabine in patients 65 years or older showed a significant improvement in OS with hypomethylating therapy (although this survival advantage failed to meet statistical significance in the primary analysis).53 A more recent trial comparing the hypomethylating agent azacitidine to supportive care, low-dose cytarabine or standard induction therapy in patients 65 years or older did not show any significant improvement in median OS.54 However among patients pre-selected to receive supportive care, a subgroup analysis suggested a benefit to azacitidine therapy. A similar benefit was seen among patients with adverse cytogenetic-risk profile or MDR-AML.54 These results suggest a promising role for the use of hypomethylating agents in older individuals, including as a bridge for induction chemotherapy with the goal of achieving CR.
Response to induction therapy should be evaluated 14 days after initiation of treatment with a bone marrow aspirate and core biopsy.17 Up to 25–50% of patients show persistent cytological evidence of disease after one cycle of standard induction therapy and require reinduction.55 Treatment options for such patients (as well as patients with a disease relapse) include a second cycle of standard dose cytarabine combined with an anthracycline, high-dose cytarabine alone or FLAG-IDA, with roughly similar CR rates of up to 50%.23, 56, 57 In addition, mitoxantrone-based regimens (in combination with etoposide and/or cytarabine) have been shown to achieve CR up to 40–60% of patients with recurrent or refractory AML.58, 59 Ultimately, around 60–80% of patients with de novo AML will achieve CR with induction therapy.60 Patients in remission should be offered consolidation therapy to eradicate residual disease and prevent relapse. Available options for consolidation include chemotherapy and allogeneic hematopoietic stem cell transplant (allo-HSCT). When choosing between these different options, the risk of TRM should be weighted against the risk of treatment failure or relapse. Intention-to-treat analyses (allocating patients to allo-HSCT or chemotherapy based on the availability of a related-donor) have found no benefit to allo-HSCT when compared with chemotherapy in patients with cytogenetically favorable AML in first CR.61, 62 Thus chemotherapy is a reasonable first-line consolidation choice for patients with a favorable prognosis. Regimens generally consist of intermediate-dose cytarabine (two to four cycles each consisting of six doses at 1.5–3 g/m2), which has been shown to be as effective as high-dose cytarabine48, 50, 63 or multi-agent regimens.50 The optimal choice of consolidation therapy for patients with an intermediate-risk cytogenetic profile but favorable genetic mutations is more controversial: several studies have found no benefit to transplantation in patients with NPM1-mutated, FLT3-ITD-negative CN-AML.64, 65 However in a recent intention-to-treat analysis, allo-HSCT was shown to improve RFS in this subset of patients.66 While these conflicting results may reflect differences in study design, the difference in observed outcomes may also reflect the modulating effect of co-occurring mutations, such as IDH-1/-2.6 On the other hand allo-HSCT significantly prolongs RFS and OS in some patients with intermediate-risk and in most with adverse-risk AML, and should be offered as a first-line consolidation therapy in eligible patients.62, 67, 68, 69 In addition, allo-HSCT has been shown to prolong RFS and improve OS in patients with CN-AML and a high FLT3-ITD allelic ratio.70
Novel agents
FLT3-ITD inhibitors
Inhibition of tyrosine kinase (TK) receptors has been used successfully in various solid and hematological malignancies, including Philadelphia-chromosome positive leukemias. Given the prognostic impact and the high rate of FLT3 mutations, inhibition of this TK has long been recognized as a potential therapeutic target in AML. Tested agents include the first-generation inhibitors sorafenib and midostaurin, as well as newer second-generation agents such as quizartinib and crenolanib.
Sorafenib
Sorafenib is a tyrosine kinase inhibitors (TKI) of RAF kinase, c-KIT, VGFR, PGFR and FLT3-ITD, which was first used for the treatment of hepatocellular and renal cell carcinoma. As early as 2008, phase I trials of sorafenib administered as a single agent n patients with FLT3-ITD-positive relapsed or refractory (r/r) AML demonstrated significant reductions in the number of leukemic cells both in the peripheral blood and bone marrow, achieving CR in several patients.71, 72, 73, 74 In a phase II trial of 13 patients with r/r FLT3-ITD-positive AML, single-agent sorafenib at doses of 200–400 mg twice daily established CR (including CR with insufficient hematologic recovery) in over 90% of cases. The agent was well-tolerated, with grades 3 to 4 adverse events consisting of hyperbilirubinemia (in 4/13 patients), elevated transaminases (5/13), diarrhea (4/13), rash (2/13), pancreatitis (1/13), colitis (1/13), pericarditis (1/13), hand and foot syndrome (2/13) and elevated creatinine (1/13). Yet despite a strong initial response, the majority of patients relapsed within 72 days of remission. Treatment failure was associated with the emergence of D835Y and D835H mutations within the FLT3 TKD. The addition of sorafenib to standard induction regimens has yielded similarly mixed results: although initial phases I and II trials of combination therapy were able to achieve longer periods of disease-free survival, relapse invariably ensued within several months of treatment.75, 76, 77 In one such study, the combination of sorafenib with cytarabine and idarubicin as induction and consolidation therapy was able to achieve CR (or CR with an incomplete platelet recovery) in 18 out of 18 patients with previously untreated FLT3-ITD-positive AML.75 However after a median follow-up of 9 months, more than half of these patients had relapsed. Interestingly, no new mutation was observed in the FLT3 TKD of the relapsed samples available for genetic sequencing. Alternative mechanisms of resistance, such as the increased levels of FLT3 receptor ligand seen in patients receiving standard chemotherapy, have been postulated to contribute to treatment failure.78 Combinations of sorafenib and hypomethylating agents, which have not been associated with an increase in FLT3 receptor ligand levels, are currently being investigated. An encouraging phase II trial of sorafenib and azacitidine in 43 patients with relapsed/refractory AML reported a response rate of 46%, including 16% CR and 27% CR with incomplete count recovery.79
The role of sorafenib as a first-line therapy in AML was further delineated in two recent randomized trials: In 2013, Serve et al. published the results of study, in which 201 patients 60 years or older with newly diagnosed AML were randomized to receive sorafenib or placebo in addition to standard chemotherapy. Even within the subset of patients with FLT3-ITD-positive disease, the addition of sorafenib did not result in an improved EFS or OS, and was instead associated with an increased incidence of adverse events.80 Most recently, Rollig et al.81 investigated the combination of sorafenib with standard chemotherapy in a multicenter randomized controlled phase II trial of 267 patients age 60 or younger with newly diagnosed AML. In this study, patients were randomly assigned to receive two cycles of standard ‘7+3’ induction therapy followed by three cycles of high-dose cytarabine as consolidation therapy in combination with either sorafenib (400 mg twice daily) or placebo. Patients assigned to the sorafenib group also received 12 months of sorafenib maintenance therapy after their last consolidation cycle. After 3 years the primary end point, event-free survival, was achieved in 40% of patients in the sorafenib group, versus 20% in the placebo group (with an unadjusted hazard ratio of 0.64).81 The occurrence of grades 3–5 diarrhea, rash, fever and bleeding were significantly increased among patients receiving sorafenib (occurring in 11, 7, 54 and 7%, respectively). Importantly, only 17% of the individuals enrolled in this study were positive for the FLT3-ITD mutation. The observed benefit in FLT3-ITD-negative AML may in part be explained by off-target inhibition of other tyrosine kinases, such as c-KIT, PGFR and RAF kinase. Alternatively as suggested by the observed increased in FLT3 receptor ligands level activation of wild-type FLT3 TK may become a driver of leukemogenesis in patients receiving standard chemotherapy.82 By targeting FLT3 TK in the period immediately after cytarabine or daunorubicin therapy, sorafenib may exert significant anti-leukemic activity even in FLT3-ITD-negative cells.
In an interesting parallel to the use of TKI in Philadelphia-chromosome-positive leukemias, inhibition of FLT3 TK has also shown a promising role in the post-allo-HSCT setting, either as maintenance therapy or treatment of relapse. This was explored recently by Chen et al.83 in a phase I trial of 22 patients with FLT3-ITD-positive disease who received sorafenib as maintenance therapy following allo-HSCT. In addition to establishing safety and feasibility, the authors of this study reported rates of PFS and OS which compared favorably to historical controls, particularly in the subset of patients in CR1 or CR2 at the time of transplant. In a retrospective analysis of six patients status post allo-HSCT, sorafenib as maintenance therapy (n=5) or treatment of relapse (n=1) resulted in a median PFS of 16 months, with all patients remaining in molecular remission (that is, FLT3-ITD-negative by PCR).84 Interestingly, skin graft-versus-host-disease occurred shortly after initiation of therapy in five out of these six patients. In addition to its action as a TKI, sorafenib may therefore possess an immunomodulatory role, which synergizes with the graft-versus-leukemia effect.85 Two phase I trials of sorafenib use in the peri-transplant setting are currently underway (NCT01398501 and NCT01578109).
Midostaurin
Midostaurin is another first-generation FLT3 TKI with significant but transient single-agent activity in patients with AML.86, 87 As with sorafenib, its effects are limited by the rapid emergence of resistance. Combinations of midostaurin and existing chemotherapy regimens are currently under investigation: results of a phase I and combined phase I/II trial of midostaurin and azacitidine have recently been published, demonstrating the tolerability and efficacy of this combination in patients with AML. In their cohort of 17 patients with a median age of 73, Cooper et al.88 established a MTD level of 75 mg PO twice daily with no observed dose-limiting toxicities. In another phase I/II trial of the combination of midostaurin and azacitidine was tested in patients with AML (primary or secondary) and MDS, Strati et al. reported a lower MTD of 50 mg PO twice daily. The combination achieved an overall response rate of 26%, with median remission duration of 20 weeks. Although no DLT were observed in this study, neutropenia, thrombocytopenia and anemia developed in 96, 94 and 61% of patients, as well as infections and a decreased left ventricular ejection fraction in 56 and 11% of patients, respectively.89 In a recent randomized, double-blind trial of 717 patients with previously untreated FLT3 (ITD and TKD) positive AML, Stone et al. explored the role of midostaurin in combination with a standard ‘7+3’ induction regimen and high-dose cytarabine consolidation therapy. Patients randomized to the midostaurin treatment arm also received midostaurin as maintenance therapy for one year. Although no difference in the rate of CR was observed between the midostaurin and placebo arms, patients receiving midostaurin had a significantly higher OS and EFS (with a hazard ratio of 0.77 and 0.80, respectively).90
Quizartinib
Second-generation inhibitors such as quizartinib have been designed to specifically target the FLT3 kinase, in order to reduce toxicity from off-target effects. In addition to this increased selectivity, quizartinib also possesses a good bioavailability and a half-life of more than 24 h, which allows for a more continuous FLT3 inhibition. A phase I study of oral quizartinib in 76 patients with relapsed/refractory AML was able to achieve a hematological response in 30% of patients, and a CR in 13% regardless of FLT3 mutational status. Among patients with FLT3-ITD, the rate of hematologic response increased to 53%, with ~23% of patients achieving CR. Patients were able to tolerate doses of up to 200 mg/day, with grade 3 QT interval prolongation as the only DLT.91 In one phase 2 trial, 137 patients with relapsed/refractory AML were given quizartinib monotherapy. The agent was administered in 28-day cycles at doses of 90 mg/day in females and 135 mg/day in males; the most common treatment toxicities were nausea and vomiting in 38 and 26% of patients, anemia in 29%, QT interval prolongation in 26%, febrile neutropenia in 25%, diarrhea in 20% and fatigue in 20%. The rate of composite CR (that is, CR, CR with incomplete platelet recovery and CR with incomplete hematological recovery) and the median OS were 34% and 25.6 months in FLT3-ITD-negative cases, and 44% and 23.1 months in FLT3-ITD positive cases. The observed benefit in FLT3-ITD-negative disease may be explained by off-target effects, or by the upregulation of the FLT3 TK pathway as suggested by the rise in FLT3 receptor ligand levels in patients receiving standard chemotherapy.92 Once again however, the response to FLT3 TKI is limited by the rapid emergence of resistance: the median duration of remission was only 5 weeks in patients with FLT3-ITD-positive AML.93 Interim analysis of a phase I/II trial of quizartinib in combination with azacitidine or cytarabine (NCT01892371) reported an overall response rate of 82% in FLT3-ITD-positive AML, MDS or chronic myelomonocytic leukemia.94 A phase III trial comparing quizartinib monotherapy to salvage chemotherapy in relapsed and refractory AML (NCT02039726) is similarly underway.
Crenolanib
Crenolanib besylate is an orally available second-generation FLT3 TKI, with activity against FLT3-ITD and FLT3-TKD mutants. Unlike other FLT3 TKIs, which are subject to the emergence of resistance conferring kinase domain mutations (such as D835Y), crenolanib appears to possess extensive ‘pan-kinase’ inhibition of secondary TKD mutations. Using concentrations far below the clinically achievable plasma levels, Smith et al. were unable to identify any single TKD mutation able to confer resistance to crenolanib.95 In a phase II study of 38 patients with FLT3-mutated AML (including relapsed and refractory patients), crenolanib administered at doses of 200 mg/m2 per day three times a day in 28 days cycle achieved a median EFS and OS of 8 and 19 weeks, respectively.96 Crenolanib is currently being studied in multiple clinical trials in AML patients, both with and without FLT3-mutated AMLs.
STAT inhibitors
STAT3 tyrosine phosphorylation is upregulated in up to 50% of AML cases and confers a worse prognosis. Activation of the STAT3 signaling pathway is also stimulated by the FLT3 receptor ligand,97 and may represent a key step in the development of FLT3 TKI resistance. Several small molecules of STAT3 inhibitors have been developed and are currently being investigated for the treatment of AML: in 2011, Redell et al. showed decreased STAT3 phosphorylation and induction of apoptosis in AML cell lines treated with the STAT3 inhibitor C188-9.98 More recently, the optimized compound MM-206 demonstrated a dose-dependent induction of apoptosis in AML cell lines cultured in the presence of bone marrow stromal cells. The anti-tumor activity of MM-206 was confirmed in vivo by reducing blast count and improving survival in AML-engrafted mice.99 OPB-31121 is a small molecule inhibitor of STAT3 and STAT5 phosphorylation, which has demonstrated activity in advanced solid tumors.100 Treatment of various leukemic cell lines with this compound resulted in significant growth inhibition, including FLT3-ITD-positive AML cells.101 Importantly, OPB-31121 was able to overcome FLT3 receptor ligand-induced STAT3 phosphorylation, and may help to prevent the emergence of resistance in patients receiving FLT3-ITD TKI. Other STAT3 inhibitors that work as antisense oligonucleotide (ASO) for STAT3 are in clinical trials in hematological malignancies including AML and will have to wait to see their efficacies in near future.
IDH1/IDH2 small molecule inhibitors
Gain of function mutations in IDH-1 and IDH-2 enzymes are found in approximately 20% of cases.7 Recent attempts have been made to target these mutant enzymes as a potential treatment for AML. In 2013, Wang et al.102 published the results of AGI-6780, a small molecule inhibitor of the R140Q mutant IDH-2 enzyme. In an ex vivo model of primary human AML cells, treatment with AGI-6780 was able to overcome the differentiation block of leukemic cells. Recently, the IDH-2 inhibitor AG-221 was found to confer a dose-dependent survival benefits in a primary human IDH-2 mutant AML xenograft model. At a cellular level, AG-221 treatment was associated with an initial phase of CD45+ blast cells proliferation, followed by cellular differentiation.103 A phase I trial of AG-221 in IDH-2 mutant leukemia is currently underway (NCT01915498). IDH-1 mutant enzymes are also the targets of new therapeutic inhibitors: Preliminary results of a phase I trial of the small molecule inhibitor AG-120 (NCT02074839) demonstrated hematological response in 7 out of 14 IDH-1 positive patients, including 4 CR.104
Clofarabine
Clofarabine is a second-generation purine nucleoside analog approved for the treatment of relapsed or refractory pediatric acute lymphocytic leukemia. In AML, it has shown activity and tolerability as a single-agent, administered intravenously at doses of 20–30 mg/m2 for 5 days, with overall response rates of ~40%.105, 106 In a 2008 randomized study of 70 patients aged 60 years and older, it was reported a CR rate of 63% using the combination of clofarabine with low-dose cytarabine, compared with 31% with clofarabine alone.107 In a study of 320 patients over the age of 55 with relapsed/refractory AML, the combination of clofarabine and cytarabine achieved significantly higher rates of CR, CR with incomplete platelet count and DFS when compared with cytarabine alone.108 Although neither of these studies was able to show an improved OS, these results suggest a synergistic action between clofarabine and cytarabine, and have spurred interest in the combination of these two agents. Recently a study was published showing the results of a phase 2 trial of clofarabine and low-dose cytarabine in older patients with newly diagnosed AML.109 In this study, 118 patients age 60 or older (median age of 68 years) received induction therapy with clofarabine at 20 mg/m2 on day 1 through 5 and low-dose cytarabine at 20 mg subcutaneously twice daily on day 1 through 10. In an attempt to improve survival, this was followed by consolidation and maintenance therapy with up to 18 cycles of clofarabine and low-dose cytarabine alternating with decitabine. CR was achieved in 60% of cases, with a median OS of 11.1 months, and a median RFS of 14.1 months. The regimen was well-tolerated, with a 4-week mortality rate of 3%. The most common non-hematological toxicities reported in this study included nausea in 81% of cases, elevated liver transaminases and bilirubin in 64 and 47% of cases, as well as rash in 56% of cases. Clofarabine may thus represent a well-tolerated addition to low-dose cytarabine in elderly patients unable to receive standard chemotherapy or allo-HSCT for consolidation therapy. Clofarabine has shown similarly promising results in younger patients when combined with the standard ‘7+3’ induction regimen. In a study of 57 newly diagnosed patients under the age of 60, the combination of clofarabine (at 22.5 mg/m2 IV daily for 5 days) with idarubicin and cytarabine used as a frontline induction and consolidation therapy achieved CR rates of 74% and a median EFS of 13.5 months (the median OS and RFS had not been reached by a median follow-up of 10.9 months).110 A phase I/II study of frontline clofarabine, cytarabine and idarubicin in patients with intermediate and poor risk AML is currently underway (NCT00838240). The potential role of clofarabine in the peri-transplant setting is also currently under investigation. In a multicenter two-stage phase II trial, 84 patients with relapsed and refractory AML received clofarabine (at 30 mg/m2 for 5 days) in combination with cytarabine as salvage therapy, followed by 4 days of clofarabine and one dose of melphalan in chemo-responsive patients with HLA-compatible donors. Out of the 56 patients who underwent allo-HSCT, CR was achieved in 50 (including 11 CR with incomplete platelet recovery and 10 CR by chimerism). The 2-year OS of 43% compared favorably with historical controls.111 Although randomized controlled trials are needed to clearly delineate the role of clofarabine in AML these studies present promising results in support of this agent, particularly in combination with cytarabine in the elderly.
In addition to its activity as an intravenous agent, clofarabine has also captured interest as an oral agent for the treatment of AML. Unlike previous purine nucleoside analogs, clofarabine is able to resist acidic pH as well as phosphorolytic cleavage by gastrointestinal Escherichia coli. As a result it possesses a bioavailability of roughly 50%.112 In a phase I/II study of 35 patients 60 years or older with relapsed/refractory AML or high-risk MDS the feasibility and efficacy of oral clofarabine combined with low-dose cytarabine was investigated as a first-line therapy.113 At a MTD of oral clofarabine of 20 mg per day for 5 days, CR was achieved in 42% of patients (including CR with incomplete count recovery in 4%). Most importantly, more than 50% of cycles administered at the MTD were given in the outpatient setting. In a population at an increased risk of TRM, oral clofarabine may thus offer a valuable addition to reduced intensity chemotherapy.
Monoclonal antibodies
Monoclonal antibodies exert their anti-tumor activity through direct antibody-dependent cytotoxicity or through the conjugation of cytotoxic agents, which allows for the targeted delivery of potent chemotherapy to neoplastic cells. Gemtuzumab ozogamicin (GO) is a humanized recombinant antibody directed at CD33, a transmembrane protein expressed on cells of myeloid lineage. The antibody is conjugated to the DNA-cleaving cytotoxic agent calicheamicin, and is internalized by CD33-positive cells. GO received FDA approval in 2000 for the treatment of CD33-positive AML in patients 60 years or older at first relapse. However in 2009, interim analysis of a randomized clinical trial of 637 patients with newly diagnosed AML revealed increased fatal toxicity with no improvement in CR, disease-free survival or OS in patients receiving GO in combination with standard chemotherapy.114 The trial was prematurely terminated and FDA approval was rescinded. Despite its removal from the market, a 2014 meta-analysis of five randomized clinical trials demonstrated a decrease in relapse and improved survival in patients receiving GO in addition to standard chemotherapy.115 A subset analysis further revealed that this survival benefit was limited to patients with a favorable or intermediate cytogenetic-risk profile. Most recently, a randomized trial of 237 patients 60 years of age or older ineligible for intensive chemotherapy showed an improved OS (hazard ratio of 0.69) in those assigned to GO induction and consolidation compared with best supportive care.116 This survival benefit was again most pronounced in patients with an intermediate to favorable cytogenetic-risk profile. Although further studies are required to fully delineate the effects of gemtuzumab in the treatment of AML, these data suggest a benefit among elderly patients with favorable or intermediate cytogenetic-risk profile. CD37 is a transmembrane protein that is expressed in high levels on maturing B cells. Although its exact function has not yet been elucidated, it is upregulated in non-Hogkin lymphoma and chronic lymphocytic leukemia.117 Initially conceived as a therapy for B-cell malignancies, AGS67E is a fully human anti-CD37 IgG antibody that is conjugated with monomethyl auristatin E (MMAE), a potent microtubule-disrupting agent. AGS67E allows for the selective delivery of MMAE to CD37-positive malignant cells and results in apoptosis. Although CD37 is minimally expressed on normal myeloid stem cells it was recently demonstrated to have differential expression of CD37 on the surface of CD34+/CD38− AML stem cells. In vitro treatment of leukemic cells with nanomolar concentrations of AGS67E resulted in cytotoxicity, altered cell growth and apoptosis in seven out of 16 AML cell lines. The administration of AGS67E was further found to significantly decreased tumor engraftment in a murine xenograft model of AML, resulting in undetectable leukemic cell levels in three out of four AML samples. CD37 may thus represent a novel therapeutic target for the selective inhibition of leukemic cell growth. Although still at an early stage of its clinical development, AGS67E is a promising new therapy. More importantly, the identification of unique molecular markers expressed on the surface of leukemic cells is an emerging avenue for the discovery of novel targeted therapies against AML.
CART therapy
Chimeric antigen receptors are synthetic T-cell receptors with antibody-like specificity. They combine a single-chain variable fragment from a monoclonal antibody with the transmembrane and intracellular domains of a T-cell receptor. This allows for the creation of a host-derived population of chimeric antigen receptor-T (CART) cells, which can be directed at a pre-determined antigen. CD19-directed CART cell therapy has shown exciting efficacy in the treatment of acute lymphoblastic leukemia and B-cell lymphoma. Although this treatment does not distinguish between malignant and healthy CD19 cells, patients tolerate the depletion of CD19 lymphocytes with relatively little morbidity. In contrast to this, depletion of the normal cells of myeloid lineage is associated with unacceptable neutropenia, and attempts to apply CART cell therapy to the treatment of AML have had to focus on identifying an appropriate antigen to target malignant cells while sparing non-malignant myeloid cells. Kenderian et al. recently developed a CD33-specific CAR based on the single-chain variable fragment of gemtuzumab ozogamicin. They have reported potent in vitro activity of such CD33-specific CART cells against AML cell lines.118 CD33-specific CART therapy also prolonged survival in AML xenografts. However CD33 is expressed on normal cells of myeloid lineage and the reported anti-tumor effects were associated with profound cytopenias. Using electroporation of CD33-specific CAR mRNA into human T cells, the authors are able to induce the transient expression of anti-CD33 CAR,118 which may confer clinically significant anti-tumor activity while avoiding long-term myelosuppression. In an attempt to selectively target leukemic myeloid cells, others have focused instead on the β member of the folate receptor family (FRβ). This receptor subtype is primarily expressed on myeloid-lineage hematopoietic cells, and is upregulated in the setting of malignancy.119 FRβ is expressed in 70% of cases of primary AML, and its expression can be further upregulated following treatment with all-trans retinoic acid.120 In a recent publication the effect of FRβ-specific CART cells therapy in vitro as well as in AML xenograft was reported. The study demonstrated lytic activity against FRβ positive AML cell lines both in vitro and in vivo. Importantly, no evidence of toxic activity against healthy human CD34-positive stem cells was observed in vitro.121 Although still in its early stages, CART cell therapy may thus provide an alternative mechanism of treatment for patients with relapsed/refractory AML.
Conclusion
AML is a biologically and clinically heterogeneous disease. Although advances in supportive care and prognostic risk stratification have optimized established therapies, overall long-term survival remains poor. Elderly patients who account for the majority of newly diagnosed cases are more likely to present with an adverse cytogenetic profile. At the same time the increased risk of TRM often precludes this population of patients from receiving optimal chemotherapy or stem cell transplantation. Novel targeted therapies offer the promise of effective anti-leukemic activity with reduced toxicity from off-target effects. However given the molecular diversity of AML, it is unlikely that targeted therapies such as FLT3 tyrosine kinase inhibitors will provide a single ‘magic bullet’ against this disease. Rather the development of new treatments, in concert with improved genetic profiling and risk stratification, can be expected to result in incremental gains in remission and survival. Furthermore in addition to mutated enzymes and upregulated pathways, the identification of unique cell surface markers can provide a therapeutic target for recombinant monoclonal antibodies or chimeric antigen receptors. Here, the challenge lays in selectively targeting leukemic myeloid cells while sparing non-malignant myeloid precursors. Lastly, the development of well-tolerated oral therapies, such as clofarabine, will increasingly broaden the range of available treatment for elderly patients at a higher risk of mortality from standard chemotherapy regimens. We are looking to a new era in the treatment of AML to begin with novel agents so we can achieve better responses with prolong OS particularly for patients with relapsed or refractory diseases and poor cytogenetic features.
References
Yamamoto JF, Goodman MT . Patterns of leukemia incidence in the United States by subtype and demographic characteristics, 1997-2002. Cancer Causes Control 2008; 19: 379–390.
Siegel RL, Miller KD, Jemal A . Cancer statistics, 2015. CA Cancer J Clin 2015; 65:. 5–29.
Shah A, Andersson TM, Rachet B, Bjorkholm M, Lambert PC . Survival and cure of acute myeloid leukaemia in England, 1971-2006: a population-based study. Br J Haematol 2013; 162: 509–516.
Meyers J, Yu Y, Kaye JA, Davis KL . Medicare fee-for-service enrollees with primary acute myeloid leukemia: an analysis of treatment patterns, survival, and healthcare resource utilization and costs. Appl Health Econ Health Policy 2013; 11: 275–286.
Sill H, Olipitz W, Zebisch A, Schulz E, Wolfler A . Therapy-related myeloid neoplasms: pathobiology and clinical characteristics. Br J Pharmacol 2011; 162;792–805.
Patel JP, Gonen M, Figueroa ME, Fernandez H, Sun Z, Racevskis J et al. Prognostic relevance of integrated genetic profiling in acute myeloid leukemia. N Engl J Med 2012; 366: 1079–1089.
Cancer Genome Atlas Research Network. Genomic and epigenomic landscapes of adult de novo acute myeloid leukemia. N Engl J Med 2013; 368: 2059–2074.
Gilliland DG, Griffin JD . The roles of FLT3 in hematopoiesis and leukemia. Blood 2002; 100: 1532–1542.
Takahashi S . Current findings for recurring mutations in acute myeloid leukemia. J Hematol Oncol 2011; 4: 36.
Kihara R, Nagata Y, Kiyoi H, Kato T, Yamamoto E, Suzuki K et al. Comprehensive analysis of genetic alterations and their prognostic impacts in adult acute myeloid leukemia patients. Leukemia 2014; 28: 1586–1595.
Cook AM, Li L, Ho Y, Lin A, Li L, Stein A et al. Role of altered growth factor receptor-mediated JAK2 signaling in growth and maintenance of human acute myeloid leukemia stem cells. Blood 2014; 123: 2826–2837.
Ghoshal Gupta S, Baumann H, Wetzler M . Epigenetic regulation of signal transducer and activator of transcription 3 in acute myeloid leukemia. Leuk Res 2008; 32: 1005–1014.
Yamada O, Kawauchi K . The role of the JAK-STAT pathway and related signal cascades in telomerase activation during the development of hematologic malignancies. JAKSTAT 2013; 2: e25256.
Schuringa JJ, Wierenga AT, Kruijer W, Vellenga E . Constitutive Stat3, Tyr705, and Ser727 phosphorylation in acute myeloid leukemia cells caused by the autocrine secretion of interleukin-6. Blood 2000; 95: 3765–3770.
Spiekermann K, Bagrintseva K, Schwab R, Schmieja K, Hiddemann W . Overexpression and constitutive activation of FLT3 induces STAT5 activation in primary acute myeloid leukemia blast cells. Clin Cancer Res 2003; 9: 2140–2150.
Steensma DP, McClure RF, Karp JE, Tefferi A, Lasho TL, Powell HL et al. JAK2 V617F is a rare finding in de novo acute myeloid leukemia, but STAT3 activation is common and remains unexplained. Leukemia 2006; 20: 971–978.
Dohner H, Estey EH, Amadori S, Appelbaum FR, Buchner T, Burnett AK et al. Diagnosis and management of acute myeloid leukemia in adults: recommendations from an international expert panel, on behalf of the European LeukemiaNet. Blood 2010; 115: 453–474.
Vardiman JW, Thiele J, Arber DA, Brunning RD, Borowitz MJ, Porwit A et al. The 2008 revision of the World Health Organization (WHO) classification of myeloid neoplasms and acute leukemia: rationale and important changes. Blood 2009; 114:. 937–951.
Arber DA, Orazi A, Hasserjian R, Thiele J, Borowitz MJ, Le Beau MM et al. The 2016 revision to the World Health Organization (WHO) classification of myeloid neoplasms and acute leukemia. Blood 2016; 127: 2391–2405.
Kantarjian H, O'Brien S, Cortes J, Giles F, Faderl S, Jabbour E et al. Results of intensive chemotherapy in 998 patients age 65 years or older with acute myeloid leukemia or high-risk myelodysplastic syndrome: predictive prognostic models for outcome. Cancer 2006; 106: 1090–1098.
Walter RB, Othus M, Borthakur G, Ravandi F, Cortes JE, Pierce SA et al. Prediction of early death after induction therapy for newly diagnosed acute myeloid leukemia with pretreatment risk scores: a novel paradigm for treatment assignment. J Clin Oncol 2011; 29: 4417–4423.
Hulegardh E, Nilsson C, Lazarevic V, Garelius H, Antunovic P, Derolf A. Rangert et al. Characterization and prognostic features of secondary acute myeloid leukemia in a population-based setting: a report from the Swedish Acute Leukemia Registry. Am J Hematol 2015; 90: 208–214.
Estey EH . Acute myeloid leukemia: 2014 update on risk-stratification and management. Am J Hematol 2014; 89: 1063–1081.
Mrozek K, Marcucci G, Nicolet D, Maharry KS, Becker H, Whitman SP et al. Prognostic significance of the European LeukemiaNet standardized system for reporting cytogenetic and molecular alterations in adults with acute myeloid leukemia. J Clin Oncol 2012; 30: 4515–4523.
Qin YZ, Zhu HH, Jiang Q, Jiang H, Zhang LP, Xu LP et al. Prevalence and prognostic significance of c-KIT mutations in core binding factor acute myeloid leukemia: a comprehensive large-scale study from a single Chinese center. Leuk Res 2014; 38: 1435–1440.
Paschka P, Marcucci G, Ruppert AS, Mrozek K, Chen H, Kittles RA et al. Adverse prognostic significance of KIT mutations in adult acute myeloid leukemia with inv(16) and t(8;21): a Cancer and Leukemia Group B Study. J Clin Oncol 2006; 24: 3904–3911.
Park SH, Chi HS, Min SK, Park BG, Jang S, Park CJ . Prognostic impact of c-KIT mutations in core binding factor acute myeloid leukemia. Leuk Res 2011; 35: 1376–1383.
Park SH, Lee HJ, Kim IS, Kang JE, Lee EY, Kim HJ et al. Incidences and prognostic impact of c-KIT, WT1, CEBPA, and CBL mutations, and mutations associated with epigenetic modification in core binding factor acute myeloid leukemia: a multicenter study in a Korean population. Ann Lab Med 2015; 35: 288–297.
Dohner K, Schlenk RF, Habdank M, Scholl C, Rucker FG, Corbacioglu A et al. Mutant nucleophosmin (NPM1) predicts favorable prognosis in younger adults with acute myeloid leukemia and normal cytogenetics: interaction with other gene mutations. Blood 2005; 106: 3740–3746.
Li HY, Deng DH, Huang Y, Ye FH, Huang LL, Xiao Q et al. Favorable prognosis of biallelic CEBPA gene mutations in acute myeloid leukemia patients: a meta-analysis. Eur J Haematol 2015; 94: 439–448.
Frohling S, Schlenk RF, Breitruck J, Benner A, Kreitmeier S, Tobis K et al. Prognostic significance of activating FLT3 mutations in younger adults (16 to 60 years) with acute myeloid leukemia and normal cytogenetics: a study of the AML Study Group Ulm. Blood 2002; 100: 4372–4380.
Port M, Bottcher M, Thol F, Ganser A, Schlenk R, Wasem J et al. Prognostic significance of FLT3 internal tandem duplication, nucleophosmin 1, and CEBPA gene mutations for acute myeloid leukemia patients with normal karyotype and younger than 60 years: a systematic review and meta-analysis. Ann Hematol 2014; 93: 1279–1286.
Cagnetta A, Adamia S, Acharya C, Patrone F, Miglino M, Nencioni A et al. Role of genotype-based approach in the clinical management of adult acute myeloid leukemia with normal cytogenetics. Leuk Res 2014; 38: 649–659.
Gale RE, Green C, Allen C, Mead AJ, Burnett AK, Hills RK et al. The impact of FLT3 internal tandem duplication mutant level, number, size, and interaction with NPM1 mutations in a large cohort of young adult patients with acute myeloid leukemia. Blood 2008; 111: 2776–2784.
Schnittger S, Bacher U, Haferlach C, Alpermann T, Kern W, Haferlach T . Diversity of the juxtamembrane and TKD1 mutations (exons 13-15) in the FLT3 gene with regards to mutant load, sequence, length, localization, and correlation with biological data. Genes Chromosomes Cancer 2012; 51: 910–924.
Grossmann V, Schnittger S, Kohlmann A, Eder C, Roller A, Dicker F et al. A novel hierarchical prognostic model of AML solely based on molecular mutations. Blood 2012; 120: 2963–2972.
Shivarov V, Gueorguieva R, Stoimenov A, Tiu R . DNMT3A mutation is a poor prognosis biomarker in AML: results of a meta-analysis of 4500 AML patients. Leuk Res 2013; 37: 1445–1450.
DiNardo CD, Ravandi F, Agresta S, Konopleva M, Takahashi K, Kadia T et al. Characteristics, clinical outcome, and prognostic significance of IDH mutations in AML. Am J Hematol 2015; 90: 732–736.
Chen X, Xie H, Wood BL, Walter RB, Pagel JM, Becker PS et al. Relation of clinical response and minimal residual disease and their prognostic impact on outcome in acute myeloid leukemia. J Clin Oncol 2015; 33: 1258–1264.
Walter RB, Kantarjian HM, Huang X, Pierce SA, Sun Z, Gundacker HM et al. Effect of complete remission and responses less than complete remission on survival in acute myeloid leukemia: a combined Eastern Cooperative Oncology Group, Southwest Oncology Group, and M. D. Anderson Cancer Center Study. J Clin Oncol 2010; 28: 1766–1771.
Hoyos M, Nomdedeu JF, Esteve J, Duarte R, Ribera JM, Llorente A et al. Core binding factor acute myeloid leukemia: the impact of age, leukocyte count, molecular findings, and minimal residual disease. Eur J Haematol 2013; 91: 209–218.
Yin JA, O'Brien MA, Hills RK, Daly SB, Wheatley K, Burnett AK . Minimal residual disease monitoring by quantitative RT-PCR in core binding factor AML allows risk stratification and predicts relapse: results of the United Kingdom MRC AML-15 trial. Blood 2012; 120: 2826–2835.
Buccisano F, Maurillo L, Del Principe MI, Del Poeta G, Sconocchia G, Lo-Coco F et al. Prognostic and therapeutic implications of minimal residual disease detection in acute myeloid leukemia. Blood 2012; 119: 332–341.
Buckley SA, Appelbaum FR, Walter RB . Prognostic and therapeutic implications of minimal residual disease at the time of transplantation in acute leukemia. Bone Marrow Transplant 2013; 48: 630–641.
Vidriales MB, Perez-Lopez E, Pegenaute C, Castellanos M, Perez JJ, Chandia M et al. Minimal residual disease evaluation by flow cytometry is a complementary tool to cytogenetics for treatment decisions in acute myeloid leukaemia. Leuk Res 2015; 40: 1–9.
Gong Q, Zhou L, Xu S, Li X, Zou Y, Chen J . High doses of daunorubicin during induction therapy of newly diagnosed acute myeloid leukemia: a systematic review and meta-analysis of prospective clinical trials. PLoS One 2015; 10: e0125612.
Li X, Xu S, Tan Y, Chen J The effects of idarubicin versus other anthracyclines for induction therapy of patients with newly diagnosed leukaemia. Cochrane Database Syst Rev 2015; 6: CD010432.
Lowenberg B . Sense and nonsense of high-dose cytarabine for acute myeloid leukemia. Blood 2013; 121: 26–28.
Lowenberg B, Pabst T, Vellenga E, van Putten W, Schouten HC, Graux C et al. Cytarabine dose for acute myeloid leukemia. N Engl J Med 2011; 364: 1027–1036.
Burnett AK, Russell NH, Hills RK, Hunter AE, Kjeldsen L, Yin J et al. Optimization of chemotherapy for younger patients with acute myeloid leukemia: results of the medical research council AML15 trial. J Clin Oncol 2013; 31: 3360–3368.
Lowenberg B, Zittoun R, Kerkhofs H, Jehn U, Abels J, Debusscher L et al. On the value of intensive remission-induction chemotherapy in elderly patients of 65+ years with acute myeloid leukemia: a randomized phase III study of the European Organization for Research and Treatment of Cancer Leukemia Group. J Clin Oncol 1989; 7: 1268–1274.
Fenaux P, Mufti GJ, Hellstrom-Lindberg E, Santini V, Gattermann N, Germing U et al. Azacitidine prolongs overall survival compared with conventional care regimens in elderly patients with low bone marrow blast count acute myeloid leukemia. J Clin Oncol 2010; 28: 562–569.
Kantarjian HM, Thomas XG, Dmoszynska A, Wierzbowska A, Mazur G, Mayer J et al. Multicenter, randomized, open-label, phase III trial of decitabine versus patient choice, with physician advice, of either supportive care or low-dose cytarabine for the treatment of older patients with newly diagnosed acute myeloid leukemia. J Clin Oncol 2012; 30: 2670–2677.
Dombret H, Seymour JF, Butrym A, Wierzbowska A, Selleslag D, Jang JH et al. International phase 3 study of azacitidine vs conventional care regimens in older patients with newly diagnosed AML with >30% blasts. Blood 2015; 126: 291–299.
Fernandez HF, Sun Z, Yao X, Litzow MR, Luger SM, Paietta EM et al. Anthracycline dose intensification in acute myeloid leukemia. N Engl J Med 2009; 361: 1249–1259.
Carella AM, Cascavilla N, Greco MM, Melillo L, Sajeva MR, Ladogana S et al. Treatment of "poor risk" acute myeloid leukemia with fludarabine, cytarabine and G-CSF (flag regimen): a single center study. Leuk Lymphoma 2001; 40: 295–303.
Herzig RH, Lazarus HM, Wolff SN, Phillips GL, Herzig GP . High-dose cytosine arabinoside therapy with and without anthracycline antibiotics for remission reinduction of acute nonlymphoblastic leukemia. J Clin Oncol 1985; 3: 992–997.
Amadori S, Arcese W, Isacchi G, Meloni G, Petti MC, Monarca B et al. Mitoxantrone, etoposide, and intermediate-dose cytarabine: an effective and tolerable regimen for the treatment of refractory acute myeloid leukemia. J Clin Oncol 1991; 9: 1210–1214.
Daenen S, Lowenberg B, Sonneveld P, van Putten WL, Verhoef G, Verdonck LF et al. Efficacy of etoposide and mitoxantrone in patients with acute myelogenous leukemia refractory to standard induction therapy and intermediate-dose cytarabine with amsidine. Dutch Hematology-Oncology Working Group for Adults (HOVON). Leukemia 1994; 8: 6–10.
Buchner T, Schlenk RF, Schaich M, Dohner K, Krahl R, Krauter J et al. Acute myeloid leukemia (AML): different treatment strategies versus a common standard arm—combined prospective analysis by the German AML Intergroup. J Clin Oncol 2012; 30: 3604–3610.
Koreth J, Schlenk R, Kopecky KJ, Honda S, Sierra J, Djulbegovic BJ et al. Allogeneic stem cell transplantation for acute myeloid leukemia in first complete remission: systematic review and meta-analysis of prospective clinical trials. JAMA 2009; 301: 2349–2361.
Yanada M, Matsuo K, Emi N, Naoe T . Efficacy of allogeneic hematopoietic stem cell transplantation depends on cytogenetic risk for acute myeloid leukemia in first disease remission: a metaanalysis. Cancer 2005; 103:. 1652–1658.
Weick JK, Kopecky KJ, Appelbaum FR, Head DR, Kingsbury LL, Balcerzak SP et al. A randomized investigation of high-dose versus standard-dose cytosine arabinoside with daunorubicin in patients with previously untreated acute myeloid leukemia: a Southwest Oncology Group study. Blood 1996; 88: 2841–2851.
Stelljes M, Krug U, Beelen DW, Braess J, Sauerland MC, Heinecke A et al. Allogeneic transplantation versus chemotherapy as postremission therapy for acute myeloid leukemia: a prospective matched pairs analysis. J Clin Oncol 2014; 32: 288–296.
Schlenk RF, Dohner K, Krauter J, Frohling S, Corbacioglu A, Bullinger L et al. Mutations and treatment outcome in cytogenetically normal acute myeloid leukemia. N Engl J Med 2008; 358: 1909–1918.
Rollig C, Bornhauser M, Kramer M, Thiede C, Ho AD, Kramer A et al. Allogeneic stem-cell transplantation in patients with NPM1-mutated acute myeloid leukemia: results from a prospective donor versus no-donor analysis of patients after upfront HLA typing within the SAL-AML 2003 trial. J Clin Oncol 2015; 33: 403–410.
Cornelissen JJ, van Putten WL, Verdonck LF, Theobald M, Jacky E, Daenen SM et al. Results of a HOVON/SAKK donor versus no-donor analysis of myeloablative HLA-identical sibling stem cell transplantation in first remission acute myeloid leukemia in young and middle-aged adults: benefits for whom? Blood 2007; 109: 3658–3666.
Schetelig J, Schaich M, Schafer-Eckart K, Hanel M, Aulitzky WE, Einsele H et al. Hematopoietic cell transplantation in patients with intermediate and high-risk AML: results from the randomized Study Alliance Leukemia (SAL) AML 2003 trial. Leukemia 2015; 29:. 1060–1068.
Li D, Wang L, Zhu H, Dou L, Liu D, Fu L et al. Efficacy of allogeneic hematopoietic stem cell transplantation in intermediate-risk acute myeloid leukemia adult patients in first complete remission: a meta-analysis of prospective studies. PLoS One 2015; 10: e0132620.
Schlenk RF, Kayser S, Bullinger L, Kobbe G, Casper J, Ringhoffer M et al. Differential impact of allelic ratio and insertion site in FLT3-ITD-positive AML with respect to allogeneic transplantation. Blood 2014; 124: 3441–3449.
Zhang W, Konopleva M, Shi YX, McQueen T, Harris D, Ling X et al. Mutant FLT3: a direct target of sorafenib in acute myelogenous leukemia. J Natl Cancer Inst 2008; 100: 184–198.
Borthakur G, Kantarjian H, Ravandi F, Zhang W, Konopleva M, Wright JJ et al. Phase I study of sorafenib in patients with refractory or relapsed acute leukemias. Haematologica 2011; 96: 62–68.
Crump M, Hedley D, Kamel-Reid S, Leber B, Wells R, Brandwein J et al. A randomized phase I clinical and biologic study of two schedules of sorafenib in patients with myelodysplastic syndrome or acute myeloid leukemia: a NCIC (National Cancer Institute of Canada) Clinical Trials Group Study. Leuk Lymphoma 2010; 51: 252–260.
Pratz KW, Cho E, Levis MJ, Karp JE, Gore SD, McDevitt M et al. A pharmacodynamic study of sorafenib in patients with relapsed and refractory acute leukemias. Leukemia 2010; 24: 1437–1444.
Al-Kali A, Cortes J, Faderl S, Jones D, Abril C, Pierce S et al. Patterns of molecular response to and relapse after combination of sorafenib, idarubicin, and cytarabine in patients with FLT3 mutant acute myeloid leukemia. Clin Lymphoma Myeloma Leuk 2011; 11: 361–366.
Man CH, Fung TK, Ho C, Han HH, Chow HC, Ma AC et al. Sorafenib treatment of FLT3-ITD(+) acute myeloid leukemia: favorable initial outcome and mechanisms of subsequent nonresponsiveness associated with the emergence of a D835 mutation. Blood 2012; 119: 5133–5143.
Ravandi F, Cortes JE, Jones D, Faderl S, Garcia-Manero G, Konopleva MY et al. Phase I/II study of combination therapy with sorafenib, idarubicin, and cytarabine in younger patients with acute myeloid leukemia. J Clin Oncol 2010; 28: 1856–1862.
Konig H, Levis M . Targeting FLT3 to treat leukemia. Expert Opin Ther Targets 2015; 19: 37–54.
Ravandi F, Alattar ML, Grunwald MR, Rudek MA, Rajkhowa T, Richie MA et al. Phase 2 study of azacytidine plus sorafenib in patients with acute myeloid leukemia and FLT-3 internal tandem duplication mutation. Blood 2013; 121: 4655–4662.
Serve H, Krug U, Wagner R, Sauerland MC, Heinecke A, Brunnberg U et al. Sorafenib in combination with intensive chemotherapy in elderly patients with acute myeloid leukemia: results from a randomized, placebo-controlled trial. J Clin Oncol 2013; 31: 3110–3118.
Rollig C, Serve H, Huttmann A, Noppeney R, Muller-Tidow C, Krug U et al. Addition of sorafenib versus placebo to standard therapy in patients aged 60 years or younger with newly diagnosed acute myeloid leukaemia (SORAML): a multicentre, phase 2, randomised controlled trial. Lancet Oncol 2015; 16: 1691–1699.
Sato T, Yang X, Knapper S, White P, Smith BD, Galkin S et al. FLT3 ligand impedes the efficacy of FLT3 inhibitors in vitro and in vivo. Blood 2011; 117: 3286–3293.
Chen YB, Li S, Lane AA, Connolly C, Del Rio C, Valles B et al. Phase I trial of maintenance sorafenib after allogeneic hematopoietic stem cell transplantation for fms-like tyrosine kinase 3 internal tandem duplication acute myeloid leukemia. Biol Blood Marrow Transplant 2014; 20: 2042–2048.
Antar A, Kharfan-Dabaja MA, Mahfouz R, Bazarbachi A . Sorafenib maintenance appears safe and improves clinical outcomes in FLT3-ITD acute myeloid leukemia after allogeneic hematopoietic cell transplantation. Clin Lymphoma Myeloma Leuk 2015; 15: 298–302.
Metzelder SK, Schroeder T, Finck A, Scholl S, Fey M, Gotze K et al. High activity of sorafenib in FLT3-ITD-positive acute myeloid leukemia synergizes with allo-immune effects to induce sustained responses. Leukemia 2012; 26: 2353–2359.
Fischer T, Stone RM, Deangelo DJ, Galinsky I, Estey E, Lanza C et al. Phase IIB trial of oral Midostaurin (PKC412), the FMS-like tyrosine kinase 3 receptor (FLT3) and multi-targeted kinase inhibitor, in patients with acute myeloid leukemia and high-risk myelodysplastic syndrome with either wild-type or mutated FLT3. J Clin Oncol 2010; 28: 4339–4345.
Stone RM, DeAngelo DJ, Klimek V, Galinsky I, Estey E, Nimer SD et al. Patients with acute myeloid leukemia and an activating mutation in FLT3 respond to a small-molecule FLT3 tyrosine kinase inhibitor, PKC412. Blood 2005; 105: 54–60.
Cooper BW, Kindwall-Keller TL, Craig MD, Creger RJ, Hamadani M, Tse WW et al. A phase I study of midostaurin and azacitidine in relapsed and elderly AML patients. Clin Lymphoma Myeloma Leuk 2015; 15: 428–432, e2.
Strati P, Kantarjian H, Ravandi F, Nazha A, Borthakur G, Daver N et al. Phase I/II trial of the combination of midostaurin (PKC412) and 5-azacytidine for patients with acute myeloid leukemia and myelodysplastic syndrome. Am J Hematol 2015; 90: 276–281.
Stone RM, Mandrekar S, Sanford BL, Geyer S, Bloomfield CD, Dohner K et al57th Annual Meeting & Exposition. The Multi-Kinase Inhibitor Midostaurin (M) Prolongs Survival Compared with Placebo (P) in Combination with Daunorubicin (D)/Cytarabine (C) Induction (ind), High-Dose C Consolidation (consol), and As Maintenance (maint) Therapy in Newly Diagnosed Acute Myeloid Leukemia (AML) Patients (pts) Age 18-60 with FLT3 Mutations (muts): An International Prospective Randomized (rand) P-Controlled Double-Blind Trial. Am Soc Hematol 2015 Orlando, FL, USA, 5–8 December 2015.
Cortes JE, Kantarjian H, Foran JM, Ghirdaladze D, Zodelava M, Borthakur G et al. Phase I study of quizartinib administered daily to patients with relapsed or refractory acute myeloid leukemia irrespective of FMS-like tyrosine kinase 3-internal tandem duplication status. J Clin Oncol 2013; 31: 3681–3687.
Levis M, Ravandi F, Wang ES, Baer MR, Perl A, Coutre S et al. Results from a randomized trial of salvage chemotherapy followed by lestaurtinib for patients with FLT3 mutant AML in first relapse. Blood 2011; 117: 3294–3301.
Levis MJ, Perl AE, Dombret H, Döhner H, Steffen B, Rousselot P et al. Final results of a phase 2 Open-label, monotherapy efficacy and safety study of quizartinib (AC220) in patients with FLT3-ITD positive or negative relapsed/refractory acute myeloid leukemia after second-line chemotherapy or hematopoietic stem cell transplantation. Blood 2012; 120: 673 ASH abstract 673.
Borthakur G, Kantarjian HM, O'Brien S, Garcia-Manero G, Jabbour E, Daver N et al. The combination of Quizartinib with Azacitidine or low dose Cytarabine is highly active in patients (Pts) with FLT3-ITD mutated myeloid leukemias: interim report of a phase I/II trial. Blood 2014; 124: 388–388.
Smith CC, Lasater EA, Lin KC, Wang Q, McCreery MQ, Stewart WK et al. Crenolanib is a selective type I pan-FLT3 inhibitor. Proc Natl Acad Sci USA 2014; 111: 5319–5324.
Randhawa JK, Kantarjian H, Borthakur G, Thompson PA, Konopleva M, Daver N et al57th Annual Meeting & Exposition. Results of a phase II study of crenolanib in relapsed/refractory acute myeloid leukemia patients (Pts) with activating FLT3 mutations. Am Soc Hematol 2014, San Francisco, CA, USA.
Zhou J, Bi C, Janakakumara JV, Liu SC, Chng WJ, Tay KG et al. Enhanced activation of STAT pathways and overexpression of survivin confer resistance to FLT3 inhibitors and could be therapeutic targets in AML. Blood 2009; 113: 4052–4062.
Redell MS, Ruiz MJ, Alonzo TA, Gerbing RB, Tweardy DJ . Stat3 signaling in acute myeloid leukemia: ligand-dependent and -independent activation and induction of apoptosis by a novel small-molecule Stat3 inhibitor. Blood 2011; 117: 5701–5709.
Krueger MJ, Minus M, Liu W, Long X, Stevens AM, Kolosov MI et al57th Annual Meeting & Exposition. A novel STAT3 inhibitor has potent activity in preclinical models of acute myeloid leukemia that incorporate the stromal environment. Am Soc Hematol 2015, Orlando, FL, USA.
Oh DY, Lee SH, Han SW, Kim MJ, Kim TM, Kim TY et al. Phase I study of OPB-31121, an oral STAT3 inhibitor, in patients with advanced solid tumors. Cancer Res Treat 2015; 47: 607–615.
Hayakawa F, Sugimoto K, Harada Y, Hashimoto N, Ohi N, Kurahashi S et al. A novel STAT inhibitor, OPB-31121, has a significant antitumor effect on leukemia with STAT-addictive oncokinases. Blood Cancer J 2013; 3: e166.
Wang F, Travins J, DeLaBarre B, Penard-Lacronique V, Schalm S, Hansen E et al. Targeted inhibition of mutant IDH2 in leukemia cells induces cellular differentiation. Science 2013; 340: 622–626.
Ellwood-Yen K, Wang F, Travins J, Chen Y, Yang H, Straley K et al AG-221 offers a survival advantage in a primary human IDH2 mutant AML xenograft model. in AACR Annual Meeting. 2014. San Diego, CA.
Pollyea DA, Botton Sd, Fathi AT, Stein EM, Tallman MS, Agresta S et al. Clinical safety and activity in a phase I trial of AG-120, a first in class, selective, potent inhibitor of the IDH1-mutant protein, in patients with IDH1 mutant positive advanced hematologic malignancies. Eur J Cancer 2014; 50: 195.
Burnett AK, Russell NH, Hunter AE, Milligan D, Knapper S, Wheatley K et al. Clofarabine doubles the response rate in older patients with acute myeloid leukemia but does not improve survival. Blood 2013; 122: 1384–1394.
Kantarjian HM, Erba HP, Claxton D, Arellano M, Lyons RM, Kovascovics T et al. Phase II study of clofarabine monotherapy in previously untreated older adults with acute myeloid leukemia and unfavorable prognostic factors. J Clin Oncol 2010; 28: 549–555.
Faderl S, Ravandi F, Huang X, Garcia-Manero G, Ferrajoli A, Estrov Z et al. A randomized study of clofarabine versus clofarabine plus low-dose cytarabine as front-line therapy for patients aged 60 years and older with acute myeloid leukemia and high-risk myelodysplastic syndrome. Blood 2008; 112: 1638–1645.
Faderl S, Wetzler M, Rizzieri D, Schiller G, Jagasia M, Stuart R et al. Clofarabine plus cytarabine compared with cytarabine alone in older patients with relapsed or refractory acute myelogenous leukemia: results from the CLASSIC I Trial. J Clin Oncol 2012; 30: 2492–2499.
Kadia TM, Faderl S, Ravandi F, Jabbour E, Garcia-Manero G, Borthakur G et al. Final results of a phase 2 trial of clofarabine and low-dose cytarabine alternating with decitabine in older patients with newly diagnosed acute myeloid leukemia. Cancer 2015; 121: 2375–2382.
Nazha A, Kantarjian H, Ravandi F, Huang X, Choi S, Garcia-Manero G et al. Clofarabine, idarubicin, and cytarabine (CIA) as frontline therapy for patients ⩽60 years with newly diagnosed acute myeloid leukemia. Am J Hematol 2013; 88: 961–966.
Middeke JM, Herbst R, Parmentier S, Bug G, Hanel M, Stuhler G et al. Clofarabine salvage therapy before allogeneic hematopoietic stem cell transplantation in patients with relapsed or refractory AML: results of the BRIDGE trial. Leukemia 2015; 30: 261–267.
Bonate PL, Cunningham CC, Gaynon P, Jeha S, Kadota R, Lam GN et al. Population pharmacokinetics of clofarabine and its metabolite 6-ketoclofarabine in adult and pediatric patients with cancer. Cancer Chemother Pharmacol 2011; 67: 875–890.
Buckley SA, Mawad R, Gooley TA, Becker PS, Sandhu V, Hendrie P et al. A phase I/II study of oral clofarabine plus low-dose cytarabine in previously treated acute myeloid leukaemia and high-risk myelodysplastic syndrome patients at least 60 years of age. Br J Haematol 2015; 170: 349–355.
Petersdorf SH, Kopecky KJ, Slovak M, Willman C, Nevill T, Brandwein J et al. A phase 3 study of gemtuzumab ozogamicin during induction and postconsolidation therapy in younger patients with acute myeloid leukemia. Blood 2013; 121: 4854–4860.
Hills RK, Castaigne S, Appelbaum FR, Delaunay J, Petersdorf S, Othus M et al. Addition of gemtuzumab ozogamicin to induction chemotherapy in adult patients with acute myeloid leukaemia: a meta-analysis of individual patient data from randomised controlled trials. Lancet Oncol 2014; 15: 986–996.
Amadori S, Suciu S, Selleslag D, Aversa F, Gaidano G, Musso M et al. Gemtuzumab Ozogamicin versus best supportive care in older patients with newly diagnosed acute myeloid leukemia unsuitable for intensive chemotherapy: results of the randomized phase III EORTC-GIMEMA AML-19 Trial. J Clin Oncol 2016; 34: 972–979.
Moore K, Cooper SA, Jones DB . Use of the monoclonal antibody WR17, identifying the CD37 gp40-45 Kd antigen complex, in the diagnosis of B-lymphoid malignancy. J Pathol 1987; 152: 13–21.
Kenderian SS, Ruella M, Shestova O, Klichinsky M, Aikawa V, Morrissette JJ et al. CD33-specific chimeric antigen receptor T cells exhibit potent preclinical activity against human acute myeloid leukemia. Leukemia 2015; 29: 1637–1647.
Ross JF, Wang H, Behm FG, Mathew P, Wu M, Booth R et al. Folate receptor type beta is a neutrophilic lineage marker and is differentially expressed in myeloid leukemia. Cancer 1999; 85: 348–357.
Wang H, Zheng X, Behm FG, Ratnam M . Differentiation-independent retinoid induction of folate receptor type beta, a potential tumor target in myeloid leukemia. Blood 2000; 96: 3529–3536.
Lynn RC, Poussin M, Kalota A, Feng Y, Low PS, Dimitrov DS et al. Targeting of folate receptor beta on acute myeloid leukemia blasts with chimeric antigen receptor-expressing T cells. Blood 2015; 125: 3466–3476.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
De Kouchkovsky, I., Abdul-Hay, M. ‘Acute myeloid leukemia: a comprehensive review and 2016 update’. Blood Cancer Journal 6, e441 (2016). https://doi.org/10.1038/bcj.2016.50
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/bcj.2016.50
This article is cited by
-
METTL1 mediated tRNA m7G modification promotes leukaemogenesis of AML via tRNA regulated translational control
Experimental Hematology & Oncology (2024)
-
Venetoclax efficacy on acute myeloid leukemia is enhanced by the combination with butyrate
Scientific Reports (2024)
-
Inflammatory recruitment of healthy hematopoietic stem and progenitor cells in the acute myeloid leukemia niche
Leukemia (2024)
-
Development and validation of a cuproptosis-related prognostic model for acute myeloid leukemia patients using machine learning with stacking
Scientific Reports (2024)
-
Oncogenic lncRNA FAM215A promotes the malignant cell phenotypes of acute myeloid leukemia (AML) cell lines
Journal of Molecular Histology (2024)