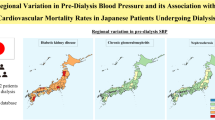
Abstract
Blood pressure (BP) is reportedly a predictor of mortality in hemodialysis (HD) patients; however, it is unclear whether pre- or postdialysis BP has greater predictive power. To evaluate the association of pre- and postdialysis BP with patient survival in Japanese HD patients, we enrolled the entire phase 3 and 4 Japan Dialysis Outcomes and Practice Patterns Study populations. Among 3176 patients, 486 were excluded because of missing data. The remaining 2690 patients were divided into five groups according to pre- or postdialysis systolic BP (SBP): <100, 100–119, 120–139, 140–159, and ≥160 mmHg; diastolic BP (DBP): <60, 60–79, 80–89, 90–99, and ≥100 mmHg; or pulse pressure (PP): <50, 50–59, 60–69, 70–79, and ≥80 mmHg. The hazard ratios for all-cause and cardiovascular mortalities were estimated according to pre- and postdialysis SBP, DBP, and PP using a Cox proportional hazards model. During the follow-up period, 495 and 193 subjects died because of any cause and cardiovascular disease (CVD), respectively. In the multivariable-adjusted Cox proportional hazards model, U-shaped associations of postdialysis SBP and PP with mortality rates were observed, but no significant associations were observed with predialysis SBP or PP. A stratified analysis showed significant interactions between history of CVD and postdialysis SBP with all-cause and cardiovascular mortality. Compared with predialysis values, postdialysis SBP and PP are better predictors of all-cause and cardiovascular mortality, showing U-shaped associations with these outcomes in Japanese HD patients.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Vasan RS, Larson MG, Leip EP, Evans JC, O'Donnell CJ, Kannel WB, et al. Impact of high-normal blood pressure on the risk of cardiovascular disease. N Engl J Med. 2001;345:1291–7.
Port FK, Hulbert-Shearon TE, Wolfe RA, Bloembergen WE, Golper TA, Agodoa LY, et al. Predialysis blood pressure and mortality risk in a national sample of maintenance hemodialysis patients. Am J Kidney Dis. 1999;33:507–17.
Zager PG, Nikolic J, Brown RH, Campbell MA, Hunt WC, Peterson D, et al. "U" curve association of blood pressure and mortality in hemodialysis patients. Medical Directors of Dialysis Clinic, Inc. Kidney Int. 1998;54:561–9.
Kalantar-Zadeh K, Kilpatrick RD, McAllister CJ, Greenland S, Kopple JD. Reverse epidemiology of hypertension and cardiovascular death in the hemodialysis population: the 58th annual fall conference and scientific sessions. Hypertension. 2005;45:811–7.
Hara M, Tanaka S, Taniguchi M, Fujisaki K, Torisu K, Masutani K, et al. Prognostic value of pre-dialysis blood pressure and risk threshold on clinical outcomes in hemodialysis patients: the Q-Cohort Study. Medicine. 2018;97:e13485.
Klassen PS, Lowrie EG, Reddan DN, DeLong ER, Coladonato JA, Szczech LA, et al. Association between pulse pressure and mortality in patients undergoing maintenance hemodialysis. JAMA. 2002;287:1548–55.
Moriya H, Oka M, Maesato K, Mano T, Ikee R, Ohtake T, et al. Weekly averaged blood pressure is more important than a single-point blood pressure measurement in the risk stratification of dialysis patients. Clin J Am Soc Nephrol. 2008;3:416–22.
Myers OB, Adams C, Rohrscheib MR, Servilla KS, Miskulin D, Bedrick EJ, et al. Age, race, diabetes, blood pressure, and mortality among hemodialysis patients. J Am Soc Nephrol. 2010;21:1970–8.
Alborzi P, Patel N, Agarwal R. Home blood pressures are of greater prognostic value than hemodialysis unit recordings. Clin J Am Soc Nephrol. 2007;2:1228–34.
Agarwal R, Peixoto AJ, Santos SF, Zoccali C. Pre- and postdialysis blood pressures are imprecise estimates of interdialytic ambulatory blood pressure. Clin J Am Soc Nephrol. 2006;1:389–98.
Agarwal R, Brim NJ, Mahenthiran J, Andersen MJ, Saha C. Out-of-hemodialysis-unit blood pressure is a superior determinant of left ventricular hypertrophy. Hypertension. 2006;47:62–8.
Mapes DL, Lopes AA, Satayathum S, McCullough KP, Goodkin DA, Locatelli F, et al. Health-related quality of life as a predictor of mortality and hospitalization: the Dialysis Outcomes and Practice Patterns Study (DOPPS). Kidney Int. 2003;64:339–49.
Pisoni RL, Gillespie BW, Dickinson DM, Chen K, Kutner MH, Wolfe RA. The Dialysis Outcomes and Practice Patterns Study (DOPPS): design, data elements, and methodology. Am J Kidney Dis. 2004;44:7–15.
Foley RN, Herzog CA, Collins AJ. United States Renal Data System. Blood pressure and long-term mortality in United States hemodialysis patients: USRDS Waves 3 and 4 Study. Kidney Int. 2002;62:1784–90.
Agarwal R. Blood pressure and mortality among hemodialysis patients. Hypertension. 2010;55:762–8.
Stidley CA, Hunt WC, Tentori F, Schmidt D, Rohrscheib M, Paine S, et al. Medical Directors of Dialysis Clinic I. Changing relationship of blood pressure with mortality over time among hemodialysis patients. J Am Soc Nephrol. 2006;17:513–20.
Nongnuch A, Campbell N, Stern E, El-Kateb S, Fuentes L, Davenport A. Increased postdialysis systolic blood pressure is associated with extracellular overhydration in hemodialysis outpatients. Kidney Int. 2015;87:452–7.
Yotsueda R, Taniguchi M, Tanaka S, Eriguchi M, Fujisaki K, Torisu K, et al. Cardiothoracic ratio and all-cause mortality and cardiovascular disease events in hemodialysis patients: the Q-Cohort Study. Am J Kidney Dis. 2017;70:84–92.
Tozawa M, Iseki K, Iseki C, Takishita S. Pulse pressure and risk of total mortality and cardiovascular events in patients on chronic hemodialysis. Kidney Int. 2002;61:717–26.
Briet M, Boutouyrie P, Laurent S, London GM. Arterial stiffness and pulse pressure in CKD and ESRD. Kidney Int. 2012;82:388–400.
Georgianos PI, Pikilidou MI, Liakopoulos V, Balaskas EV, Zebekakis PE. Arterial stiffness in end-stage renal disease-pathogenesis, clinical epidemiology, and therapeutic potentials. Hypertens Res. 2018;41:309–19.
Hirakata H, Nitta K, Inaba M, Shoji T, Fujii H, Kobayashi S, et al. Japanese Society for Dialysis Therapy guidelines for management of cardiovascular diseases in patients on chronic hemodialysis. Ther Apher Dial. 2012;16:387–435.
Workgroup KD. K/DOQI clinical practice guidelines for cardiovascular disease in dialysis patients. Am J Kidney Dis. 2005;45:S1–153.
Hoshide S, Kario K, Tomitani N, Kabutoya T, Chia YC, Park S, et al. Highlights of the 2019 Japanese Society of Hypertension Guidelines and perspectives on the management of Asian hypertensive patients. J Clin Hypertens. 2019. https://doi.org/10.1111/jch.13763.
Shoji T, Tsubakihara Y, Fujii M, Imai E. Hemodialysis-associated hypotension as an independent risk factor for two-year mortality in hemodialysis patients. Kidney Int. 2004;66:1212–20.
Liu W, Wang L, Huang X, Yuan C, Li H, Yang J. Orthostatic blood pressure reduction as a possible explanation for memory deficits in dialysis patients. Hypertens Res. 2019;42:1049–56.
Amari Y, Morimoto S, Iida T, Yurugi T, Oyama Y, Aoyama N, et al. Characteristics of visit-to-visit blood pressure variability in hemodialysis patients. Hypertens Res. 2019;42:1036–48.
Acknowledgements
We would like to thank the Arbor Research Collaborative for Health, Ann Arbor, MI, USA, for administering the J-DOPPS and express our appreciation for the support of Kyowa Hakko Kirin, without restrictions on publication. The DOPPS.org website lists the full details. We also thank the study nurses, physicians, and medical directors for all the time and attention that they devoted to our study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
KT has received speaker’s fees, consultant fees, and a research grant from Kyowa Kirin. EK has been a member of a biostatistics support group for the J-DOPPS program, which is supported by Kyowa Kirin. TN is a current employee of Kyowa Kirin. KI has received speaker’s fee from Kyowa Kirin. HH has received speaker’s fees from Kyowa Kirin.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Tsuruya, K., Kanda, E., Nomura, T. et al. Postdialysis blood pressure is a better predictor of mortality than predialysis blood pressure in Japanese hemodialysis patients: the Japan Dialysis Outcomes and Practice Patterns Study. Hypertens Res 43, 791–797 (2020). https://doi.org/10.1038/s41440-020-0425-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-020-0425-1
Keywords
This article is cited by
-
Seasonal variation and predictors of intradialytic blood pressure decline: a retrospective cohort study
Hypertension Research (2021)
-
Intradialytic systolic blood pressure variation can predict long-term mortality in patients on maintenance hemodialysis
International Urology and Nephrology (2021)
-
We can have it all, but we just cannot have it all at once
Hypertension Research (2020)