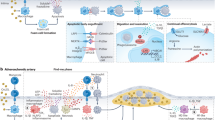
Abstract
Tissue plasminogen activator (t-PA) converts plasminogen into the serine protease plasmin, which in turn degrades fibrin clots. This study assessed whether an increase in shear stress is associated in humans in vivo with the release of t-PA in peripheral conduit arteries, the impact of high blood pressure and the role of NO and CYP450-derived epoxyeicosatrienoic acids (EETs). Local t-PA levels were quantified at baseline and during a sustained increase in radial artery wall shear stress induced by hand skin heating (from 34 to 44 °C) in a total of 25 subjects, among whom 8 were newly diagnosed essential hypertensive patients. The impact of the brachial infusion of NO synthase (L-NMMA) and CYP450 inhibitors (fluconazole) on t-PA release was assessed. The increase in shear stress induced by heating was associated with an increase in local t-PA release (from 3.0 ± 0.5 to 19.2 ± 5.5 ng/min, n = 25, P < 0.01). The magnitude of t-PA release was positively correlated with the increase in shear stress (r = 0.64, P < 0.001) and negatively correlated with mean blood pressure (r = −0.443, P = 0.027). These associations persisted after multiple adjustments for confounding factors. Finally, t-PA release was reduced by L-NMMA and to a larger extent by the combination of L-NMMA and fluconazole without a change in shear stress. The increase in wall shear stress in the peripheral conduit arteries induces a release of t-PA by a mechanism involving NO and EETs. The alteration of this response by high blood pressure may contribute to reducing the fibrinolytic potential and enhancing the risk of arterial thrombosis during exercise.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Gorog DA. Prognostic value of plasma fibrinolysis activation markers in cardiovascular disease. J Am Coll Cardiol. 2010;55:2701–9.
Muldowney JA, Vaughan DE. Tissue-type plasminogen activator release: new frontiers in endothelial function. J Am Coll Cardiol. 2002;40:967–9.
Oliver JJ, Webb DJ, Newby DE. Stimulated tissue plasminogen activator release as a marker of endothelial function in humans. Arterioscler Thromb Vasc Biol. 2005;25:2470–9.
Brown NJ. Blood pressure reduction and tissue-type plasminogen activator release. Hypertension. 2006;47:648–9.
Emeis JJ. Regulation of the acute release of tissue-type plasminogen activator from the endothelium by coagulation activation products. Ann N Y Acad Sci. 1992;667:249–58.
Diamond SL, Eskin SG, McIntire LV. Fluid flow stimulates tissue plasminogen activator secretion by cultured human endothelial cells. Science. 1989;243:1483–5.
Kawai Y, Matsumoto Y, Watanabe K, Yamamoto H, Satoh K, Murata M, et al. Hemodynamic forces modulate the effects of cytokines on fibrinolytic activity of endothelial cells. Blood. 1996;87:2314–21.
Sjögren LS, Gan L, Doroudi R, Jern C, Jungersten L, Jern S. Fluid shear stress increases the intra-cellular storage pool of tissue-type plasminogen activator in intact human conduit vessels. Thromb Haemost. 2000;84:291–8.
Li N, Wallén NH, Hjemdahl P. Evidence for prothrombotic effects of exercise and limited protection by aspirin. Circulation. 1999;100:1374–9.
Thrall G, Lane D, Carroll D, Lip GYH. A systematic review of the effects of acute psychological stress and physical activity on haemorheology, coagulation, fibrinolysis and platelet reactivity: Implications for the pathogenesis of acute coronary syndromes. Thromb Res. 2007;120:819–47.
Gkaliagkousi E, Gavriilaki E, Douma S. Effects of acute and chronic exercise in patients with essential hypertension: benefits and risks. Am J Hypertens. 2015;28:429–39.
Stein CM, Brown N, Vaughan DE, Lang CC, Wood AJ. Regulation of local tissue-type plasminogen activator release by endothelium-dependent and endothelium-independent agonists in human vasculature. J Am Coll Cardiol. 1998;32:117–22.
Brown NJ, Gainer JV, Stein CM, Vaughan DE. Bradykinin stimulates tissue plasminogen activator release in human vasculature. Hypertension. 1999;33:1431–5.
Hrafnkelsdóttir T, Wall U, Jern C, Jern S. Impaired capacity for endogenous fibrinolysis in essential hypertension. Lancet. 1998;352:1597–8.
Giannarelli C, De Negri F, Virdis A, Ghiadoni L, Cipriano A, Magagna A, et al. Nitric oxide modulates tissue plasminogen activator release in normotensive subjects and hypertensive patients. Hypertension. 2007;49:878–84.
Giannarelli C, Virdis A, De Negri F, Magagna A, Duranti E, Salvetti A, et al. Effect of sulfaphenazole on tissue plasminogen activator release in normotensive subjects and hypertensive patients. Circulation. 2009;119:1625–33.
Robinson SD, Ludlam CA, Boon NA, Newby DE. Endothelial fibrinolytic capacity predicts future adverse cardiovascular events in patients with coronary heart disease. Arterioscler Thromb Vasc Biol. 2007;27:1651–6.
Brown NJ, Gainer JV, Murphey LJ, Vaughan DE. Bradykinin stimulates tissue plasminogen activator release from human forearm vasculature through B(2) receptor-dependent, NO synthase-independent, and cyclooxygenase-independent pathway. Circulation. 2000;102:2190–6.
Smith DT, Hoetzer GL, Greiner JJ, Stauffer BL, DeSouza CA. Endothelial release of tissue-type plasminogen activator in the human forearm: role of nitric oxide. J Cardiovasc Pharm. 2003;42:311–4.
Pretorius M, Brown NJ. Endogenous nitric oxide contributes to bradykinin-stimulated glucose uptake but attenuates vascular tissue-type plasminogen activator release. J Pharm Exp Ther. 2010;332:291–7.
Rahman AM, Murrow JR, Ozkor MA, Kavtaradze N, Lin J, De Staercke C, et al. Endothelium-derived hyperpolarizing factor mediates bradykinin-stimulated tissue plasminogen activator release in humans. J Vasc Res. 2014;51:200–8.
Bellien J, Iacob M, Gutierrez L, Isabelle M, Lahary A, Thuillez C, et al. Crucial role of NO and endothelium-derived hyperpolarizing factor in human sustained conduit artery flow-mediated dilatation. Hypertension. 2006;48:1088–94.
Bellien J, Iacob M, Remy-Jouet I, Lucas D, Monteil C, Gutierrez L, et al. Epoxyeicosatrienoic acids contribute with altered nitric oxide and endothelin-1 pathways to conduit artery endothelial dysfunction in essential hypertension. Circulation. 2012;125:1266–75.
Lorthioir A, Joannidès R, Rémy-Jouet I, Fréguin-Bouilland C, Iacob M, Roche C, et al. Polycystin deficiency induces dopamine-reversible alterations in flow-mediated dilatation and vascular nitric oxide release in humans. Kidney Int. 2015;87:465–72.
Eliasson M, Jansson JH, Nilsson P, Asplund K. Increased levels of tissue plasminogen activator antigen in essential hypertension. A population-based study in Sweden. J Hypertens. 1997;15:349–56.
Poli KA, Tofler GH, Larson MG, Evans JC, Sutherland PA, Lipinska I, et al. Association of blood pressure with fibrinolytic potential in the Framingham offspring population. Circulation. 2000;101:264–9.
Tarutani Y, Matsumoto T, Takashima H, Yamane T, Horie M. Brachial artery flow-mediated vasodilation is correlated with coronary vasomotor and fibrinolytic responses induced by bradykinin. Hypertens Res. 2005;28:59–66.
Bellien J, Remy-Jouet I, Iacob M, Blot E, Mercier A, Lucas D D, et al. Impaired role of epoxyeicosatrienoic acids in the regulation of basal conduit artery diameter during essential hypertension. Hypertension. 2012;60:1415–21.
Hrafnkelsdóttir T, Wall U, Jern C, Jern S. Impaired capacity for endogenous fibrinolysis in essential hypertension. Lancet. 1998;352:1597–8.
Ridderstråle W, Ulfhammer E, Jern S, Hrafnkelsdóttir T. Impaired capacity for stimulated fibrinolysis in primary hypertension is restored by antihypertensive therapy. Hypertension. 2006;47:686–91.
Acknowledgements
The authors thank Mrs Elizabeth Debray and Agnès Deshayes (Department of Hematology, Rouen University Hospital, France) for their technical help in the measurements of t-PA and PAP complex levels.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to disclose in relation to this manuscript.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Bellien, J., Iacob, M., Richard, V. et al. Evidence for wall shear stress-dependent t-PA release in human conduit arteries: role of endothelial factors and impact of high blood pressure. Hypertens Res 44, 310–317 (2021). https://doi.org/10.1038/s41440-020-00554-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-020-00554-5
Keywords
This article is cited by
-
Annual reports on hypertension research 2020
Hypertension Research (2022)
-
Numerical simulation of pulsatile blood flow: a study with normal artery, and arteries with single and multiple stenosis
Journal of Engineering and Applied Science (2021)