Abstract
Research question
Does dental trauma have impact on the oral health-related quality of life of children and adolescents?
Research protocol
Protocol was designed as per the best practices of evidence-based medicine, guidelines for umbrella reviews and registered in PROSPERO.
Literature search
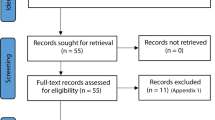
PubMed, Scopus, Embase, Web of Sciences and Lilacs were searched for studies meeting the inclusion criteria from start of databases to 15th July 2021. Grey literature and registries of systematic review protocols were also searched. Hand searching of the references of included articles was also performed. The literature search was updated on 15th October 2021. Scrutiny of the titles and abstracts and later full text was done as per the inclusion and exclusion criteria.
Data extraction
Self-designed pre-piloted form was used by two reviewers.
Quality appraisal
AMSTAR-2 was used to assess the quality of systematic reviews, PRISMA was used to check reporting-characteristics and citation-matrix was used to evaluate study-overlap. Quality of evidence was assessed by using Kohler’s-criteria.
Data analysis
Qualitative synthesis was performed for describing the study characteristics, details of sampling and the tool of OHRQoL used. The meta-analytic data was used for evaluating the evidence and its strength for each of the outcomes.
Results and interpretation
A significant impact of all types of TDI on OHRQoL in children and adolescents was observed. The effect of uncomplicated TDI on OHRQoL in children and all ages showed no difference from controls. Though the quality of evidence in these interpretations was weak.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Petti S, Glendor U, Andersson L. World traumatic dental injury prevalence and incidence, a meta-analysis—one billion living people have had traumatic dental injuries. Dent Traumatol. 2018;34:71–86.
Glendor U. Epidemiology of traumatic dental injuries—a 12 year review of the literature. Dent Traumatol. 2008;24:603–11.
Tewari N, Bansal K, Mathur VP. Dental trauma in children: a quick overview on management. Indian J Pediatr. 2019;86:1043–7.
da Silva RLC, Dias Ribeiro AP, Almeida JCF, Sousa SJL, Garcia FCP. Impact of dental treatment and the severity of traumatic dental injuries on the quality of life of Brazilian schoolchildren. Dent Traumatol. 2021;28. https://doi.org/10.1111/edt.12660.
Traebert J, Ryda U, Robertson A. Psychosocial aspects of traumatic dental injuries. In: Andreasen JO, Andreasen FM, Andersson L, editors. Textbook and color atlas of traumatic injuries to the teeth, 5th ed. Copenhagen: Wiley Blackwell; 2018:227–40.
Borges TS, Vargas-Ferreira F, Kramer PF, Feldens CA. Impact of traumatic dental injuries on oral health-related quality of life of preschool children: a systematic review and meta-analysis. PLoS One. 2017;12:e0172235.
Zaror C, Martínez-Zapata MJ, Abarca J, Díaz J, Pardo Y, Pont À, et al. Impact of traumatic dental injuries on quality of life in preschoolers and schoolchildren: a systematic review and meta-analysis. Community Dent Oral Epidemiol. 2018;46:88–101.
Lopez D, Waidyatillake N, Zaror C, Marino R, et al. Impact of uncomplicated traumatic dental injuries on the quality of life of children and adolescents: a systematic review and meta-analysis. BMC Oral Health. 2019;19:224.
Antunes LAA, Lemos HM, Milani AJ, Guimarães LS, Küchler EC, Antunes LS. Does traumatic dental injury impact oral health-related to quality of life of children and adolescents? Systematic review and meta-analysis. Int J Dent Hyg. 2020;18:142–62.
Wormald R, Evans J. What makes systematic reviews systematic and why are they the highest level of evidence? Ophthalmic Epidemiol. 2018;25:27–30.
Tewari N, Goel S, Rahul M, Mathur VP, Ritwik P, Haldar P, et al. Global status of knowledge for prevention and emergency management of traumatic dental injuries among school teachers: a systematic review and meta-analysis. Dent Traumatol. 2020;36:568–83.
Aromataris E, Fernandez R, Godfrey CM, Holly C, Khalil H, Tungpunkom P. Summarizing systematic reviews: methodological development, conduct and reporting of an umbrella review approach. Int J Evid Based Health. 2015;13:132–40.
Fusar-Poli P, Radua J. Ten simple rules for conducting umbrella reviews. Evid Based Ment Health. 2018;21:95–100.
Papatheodorou S. Umbrella reviews: what they are and why we need them. Eur J Epidemiol. 2019;34:543–6. https://doi.org/10.1007/s10654-019-00505-6.
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JPA, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ. 2009;339:b2700.
Tewari N, Mathur VP, Kaur A, Sardana D, Rahul M, Tamchos R, et al. Evidence mapping and quality assessment of systematic reviews in dental traumatology. Dent Traumatol. 2021;37:17–36.
Shea BJ, Reeves BC, Wells G, et al. AMSTAR 2: a critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. BMJ. 2017;358:j4008.
Pieper D, Antoine SL, Mathes T, Neugebauer EA, Eikermann M. Systematic review finds overlapping reviews were not mentioned in every other overview. J Clin Epidemiol. 2014;67:368–75. https://doi.org/10.1016/j.jclinepi.2013.11.007.
Köhler CA, Evangelou E, Stubbs B, Solmi M, Veronese N, Belbasis L, et al. Mapping risk factors for depression across the lifespan: an umbrella review of evidence from meta-analyses and Mendelian randomization studies. J Psychiatr Res. 2018;103:189–207. https://doi.org/10.1016/j.jpsychires.2018.05.020.
Bellou V, Belbasis L, Tzoulaki I, Middleton LT, Ioannidis JPA, Evangelou E. Systematic evaluation of the associations between environmental risk factors and dementia: An umbrella review of systematic reviews and meta-analyses. Alzheimers Dement. 2017;13:406–18. https://doi.org/10.1016/j.jalz.2016.07.152.
Magno MB, Nadelman P, Leite KLF, Ferreira DM, Pithon MM, Maia LC. Associations and risk factors for dental trauma: a systematic review of systematic reviews. Community Dent Oral Epidemiol. 2020;48:447–63.
Ioannidis JP. Integration of evidence from multiple meta-analyses: a primer on umbrella reviews, treatment networks and multiple treatments meta-analyses. CMAJ. 2009;181:488–93. https://doi.org/10.1503/cmaj.081086.
Kenny KP, Day PF, Sharif MO, Parashos P, Lauridsen E, Feldens CA, et al. What are the important outcomes in traumatic dental injuries? An international approach to the development of a core outcome set. Dent Traumatol. 2018;34:4–11.
Acknowledgements
None
Funding
None
Author information
Authors and Affiliations
Contributions
NT conceptualized the study, designed the protocol, performed the electronic searchers, analysed the data, supervised the stages of risk of bias analysis and grading of the evidence, prepared the initial draft of manuscript and revised it. VM designed the protocol supervised the data extraction and revised the manuscript, SG designed the protocol, performed the literature search, data extraction, risk of bias analysis, data extraction and revised the manuscript, MR designed the protocol performed the data analysis and revised the manuscript, SS designed the protocol, performed the data extraction and risk of bias assessment and grading of the evidence, FS designed the protocol, performed data extraction and revised the manuscript. FS developed the protocol, analysed the data and edited the manuscript, PH developed the protocol, supervised the data analysis, quality assessment and grading of the evidence, PR developed the protocol, supervised the quality assessment and edited the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tewari, N., Mathur, V.P., Goel, S. et al. Does dental trauma have impact on the oral health-related quality of life of children and adolescents?. Evid Based Dent 24, 41 (2023). https://doi.org/10.1038/s41432-023-00849-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41432-023-00849-9