Abstract
Background
Early intervention and diagnosis of Metabolic Syndrome (MetS) are crucial for preventing adult cardiovascular disease. However, the optimal indicator for identifying MetS in adolescent remains controversial.
Methods
In total,1408 Chinese adolescents and 3550 American adolescents aged 12–17 years were included. MetS was defined according to the modified version for adolescents based on Adult Treatment Panel III (NCEP-ATP III) criteria. Areas under the curve (AUC) and corresponding 95% confidence interval (95% CI) of 8 anthropometric/metabolic indexes, such as waist circumference (WC), body mass index (BMI), a body shape index (ABSI), waist triglyceride index (WTI), were calculated to illustrate their ability to differentiate MetS. Sensitivity analysis using the other MetS criteria was performed.
Results
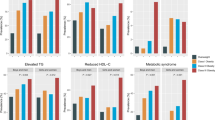
Under the modified NCEP-ATP III criteria, WTI had the best discriminating ability in overall adolescents, with AUC of 0.922 (95% CI: 0.900–0.945) in Chinese and 0.959 (95% CI: 0.949–0.969) in American. In contrast, ABSI had the lowest AUCs. Results of sensitivity analysis were generally consistent for the whole Chinese and American population, with the AUC for WC being the highest under some criteria, but it was not statistically different from that of WTI.
Conclusions
WTI had relatively high discriminatory power for MetS detection in Chinese and American adolescents, but the performance of ABSI was poor.
Impact
-
While many studies have compared the discriminatory power of some anthropometric indicators for MetS, there are few focused on pediatrics.
-
The current study is the first to compare the discriminating ability of anthropometric/metabolic indicators (WC, BMI, TMI, ABSI, WHtR, VAI, WTI, and TyG) for MetS in adolescents.
-
WTI remains the optimal indicator in screening for MetS in adolescents.
-
WC was also a simple and reliable indicator when screening for MetS in adolescents, but the performance of ABSI was poor.
-
This study provides a theoretical basis for the early identification of MetS in adolescents by adopting effective indicators.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 14 print issues and online access
$259.00 per year
only $18.50 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available in the CHNS and the NHANES repository, https://www.cpc.unc.edu/projects/china/data and https://wwwn.cdc.gov/nchs/nhanes/Default.aspx.
References
Medina, G. et al. Metabolic syndrome, autoimmunity and rheumatic diseases. Pharm. Res. 133, 277–288 (2018).
Xu, H., Li, X. P., Adams, H., Kubena, K. & Guo, S. D. Etiology of metabolic syndrome and dietary intervention. Int. J. Mol. Sci. 20, 128 (2019).
Engin, A. The definition and prevalence of obesity and metabolic syndrome. Adv. Exp. Med. Biol. 960, 1–17 (2017).
Weihe, P. & Weihrauch-Bluher, S. Metabolic syndrome in children and adolescents: diagnostic criteria, therapeutic options and perspectives. Curr. Obes. Rep. 8, 472–479 (2019).
Rodríguez-Colón, S. M. et al. Metabolic syndrome burden in apparently healthy adolescents is adversely associated with cardiac autonomic modulation—Penn State Children Cohort. Metabolism 64, 626–632 (2015).
Cook, S., Weitzman, M., Auinger, P., Nguyen, M. & Dietz, W. H. Prevalence of a metabolic syndrome phenotype in adolescents—findings from the Third National Health and Nutrition Examination Survey, 1988-1994. Arch. Pediatr. Adolesc. Med. 157, 821–827 (2003).
Zimmet, P. et al. The metabolic syndrome in children and adolescents—an Idf Consensus Report. Pediatr. Diabetes 8, 299–306 (2007).
Yang, H. R., Yi, D. Y. & Choi, H. S. Comparison between a pediatric health promotion center and a pediatric obesity clinic in detecting metabolic syndrome and non-alcoholic fatty liver disease in children. J. Korean Med. Sci. 29, 1672–1677 (2014).
Noubiap, J. J. et al. Global, regional, and country estimates of metabolic syndrome burden in children and adolescents in 2020: a systematic review and modelling analysis. Lancet Child Adolesc. Health 6, 158–170 (2022).
Zong, X., Bovet, P. & Xi, B. A proposal to unify the definition of the metabolic syndrome in children and adolescents. Front. Endocrinol. 13, 925976 (2022).
GBD 2015 Obesity Collaborators, et al. Health effects of overweight and obesity in 195 countries over 25 years. N. Engl. J. Med. 377, 13–27 (2017).
Lo, K., Wong, M., Khalechelvam, P. & Tam, W. Waist-to-height ratio, body mass index and waist circumference for screening paediatric cardio-metabolic risk factors: a meta-analysis. Obes. Rev. 17, 1258–1275 (2016).
Kobo, O., Karban, A. M. I. R., Leiba, R. & Avizohar, O. Normal body mass index (BMI) can rule out metabolic syndrome. Eur. Heart J. 40, 3843–3843 (2019).
Peterson, C. M. et al. Tri-ponderal mass index vs body mass index in estimating body fat during adolescence. JAMA Pediatr. 171, 629–636 (2017).
Anoop, S., Krakauer, J., Krakauer, N. & Misra, A. A body shape index significantly predicts MRI-defined abdominal adipose tissue depots in non-obese Asian Indians with type 2 diabetes mellitus. BMJ Open Diab. Res. Care 8, e001324 (2020).
Vizzuso, S. et al. Visceral adiposity index (VAI) in children and adolescents with obesity: no association with daily energy intake but promising tool to identify metabolic syndrome (Mets). Nutrients 13, 413 (2021).
Tao, L. C., Xu, J. N., Wang, T. T., Hua, F. & Li, J. J. Triglyceride-glucose index as a marker in cardiovascular diseases: landscape and limitations. Cardiovasc. Diabetol. 21, 68 (2022).
Yang, R. F., Liu, X. Y., Lin, Z. & Zhang, G. Correlation study on waist circumference-triglyceride (Wt) index and coronary artery scores in patients with coronary heart disease. Eur. Rev. Med. Pharm. 19, 113–118 (2015).
Sekgala, M. D., Opperman, M., Mpahleni, B. & McHiza, Z. J. Anthropometric indices and cut-off points for screening of metabolic syndrome among South African taxi drivers. Front. Nutr. 9, 974749 (2022).
Li, Y. et al. Association between four anthropometric indexes and metabolic syndrome in US adults. Front. Endocrinol. 13, 889785 (2022).
Sun, J. H., Yang, R., Zhao, M., Bovet, P. & Xi, B. Tri-ponderal mass index as a screening tool for identifying body fat and cardiovascular risk factors in children and adolescents: a systematic review. Front. Endocrinol. 12, 694681 (2021).
Zhang, B., Zhai, F. Y., Du, S. F. & Popkin, B. M. The China health and nutrition survey, 1989-2011. Obes. Rev. 15, 2–7 (2014).
Volpe, M. & Patrono, C. Decline in blood pressure control trends in the US: a real step back: comment on National Health and Nutrition Examination Survey (NHANES) data. Eur. Heart J. 41, 3986–3987 (2020).
Margolis-Gil, M., Yackobovitz-Gavan, M., Phillip, M. & Shalitin, S. Which predictors differentiate between obese children and adolescents with cardiometabolic complications and those with metabolically healthy obesity? Pediatr. Diabetes 19, 1147–1155 (2018).
Yan, S. et al. The expanding burden of cardiometabolic risk in China: the China Health and Nutrition Survey. Obes. Rev. 13, 810–821 (2012).
Myers, G. L., Cooper, G. R., Winn, C. L. & Smith, S. J. The Centers for Disease Control-National-Heart-Lung-and-Blood-Institute Lipid Standardization Program—an approach to accurate and precise lipid measurements. Clin. Lab. Med. 9, 105–135 (1989).
Ji, M., Zhang, S. & An, R. Effectiveness of A body shape index (ABSI) in predicting chronic diseases and mortality: a systematic review and meta-analysis. Obes. Rev. 19, 737–759 (2018).
Wang, X. J. et al. Use of tri-ponderal mass index in predicting late adolescent overweight and obesity in children aged 7-18. Front. Nutr. 9, 785863 (2022).
Xi, B. et al. International waist circumference percentile cutoffs for central obesity in children and adolescents aged 6 to 18 years. J. Clin. Endocrinol. Metab. 105, e1569–e1583 (2020).
Xi, B. et al. Establishing international blood pressure references among nonoverweight children and adolescents aged 6 to 17 years. Circulation 133, 398–408 (2016).
de Winter, J. C., Gosling, S. D. & Potter, J. Comparing the Pearson and Spearman correlation coefficients across distributions and sample sizes: A tutorial using simulations and empirical data. Psychol. Methods 21, 273–290 (2016).
Wang, L., Du, Z. H., Qiao, J. M. & Gao, S. Association between metabolic syndrome and endometrial cancer risk: a systematic review and meta-analysis of observational studies. Aging 12, 9825–9839 (2020).
Dipietro, L. et al. Physical activity and cardiometabolic risk factor clustering in young adults with obesity. Med. Sci. Sports Exerc. 52, 1050–1056 (2020).
Magge, S. N., Goodman, E. & Armstrong, S. C. The metabolic syndrome in children and adolescents: shifting the focus to cardiometabolic risk factor clustering. Pediatrics 140, e20171603 (2017).
Ma, C. M. et al. Three novel obese indicators perform better in monitoring management of metabolic syndrome in type 2 diabetes. Sci. Rep. 7, 9843 (2017).
Neeland, I. J., Poirier, P. & Després, J. P. Cardiovascular and metabolic heterogeneity of obesity: clinical challenges and implications for management. Circulation 137, 1391–1406 (2018).
Wildman, R. P. et al. The obese without cardiometabolic risk factor clustering and the normal weight with cardiometabolic risk factor clustering: prevalence and correlates of 2 phenotypes among the US population (NHANES 1999-2004). Arch. Intern. Med. 168, 1617–1624 (2008).
Ross, R. et al. Waist circumference as a vital sign in clinical practice: a consensus statement from the IAS and ICCR Working Group on visceral obesity. Nat. Rev. Endocrinol. 16, 177–189 (2020).
Smith, U. Abdominal obesity: a marker of ectopic fat accumulation. J. Clin. Investig. 125, 1790–1792 (2015).
Al-Shami, I. et al. Assessing metabolic syndrome prediction quality using seven anthropometric indices among Jordanian adults: a cross-sectional study. Sci. Rep. 12, 21043 (2022).
Shin, K. A. & Kim, Y. J. Usefulness of surrogate markers of body fat distribution for predicting metabolic syndrome in middle-aged and older Korean populations. Diabetes Metab. Syndr. Obes. 12, 2251–2259 (2019).
Author information
Authors and Affiliations
Contributions
Conceptualization: Jieyun Yin, Jia Hu, Xuan Hu, and Zhuoqiao Yang; Methodology: Xuan Hu and Zhuoqiao Yang; Formal analysis and investigation: Xuan Hu and Zhuoqiao Yang; Writing—original draft preparation: Xuan Hu and Zhuoqiao Yang; Writing—review and editing: Wenxin Ge, Yaling Ding, Yi Zhong, Jianing Long, Xiaoyan Zhu, Jia Hu, and Jieyun Yin; Supervision: Jieyun Yin and Jia Hu.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
Consent was obtained from all individual participants included in the study. Ethics approval was accepted by the institutional review board of the National Center for Health Statistics (NCHS), Chinese Center for Disease Control and Prevention (CCDC) and National Institute for Nutrition and Health (NINH).
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hu, X., Yang, Z., Ge, W. et al. Evaluating eight indicators for identifying metabolic syndrome in Chinese and American adolescents. Pediatr Res (2024). https://doi.org/10.1038/s41390-024-03247-8
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41390-024-03247-8