Abstract
Background
The relationship between maternal physical activity (PA)/sitting and birth defects is largely unexplored. We examined whether pre-pregnancy PA/sitting were associated with having a pregnancy affected by a birth defect.
Methods
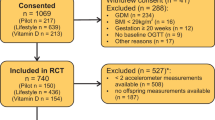
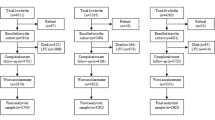
We used data from two United States population-based case–control studies: 2008–2011 deliveries from the National Birth Defects Prevention Study (NBDPS; 9 states) and 2014–2018 deliveries from the Birth Defects Study To Evaluate Pregnancy exposureS (BD-STEPS; 7 states). Cases with one of 12 non-cardiac birth defects (n = 3798) were identified through population-based registries. Controls (n = 2682) were live-born infants without major birth defects randomly sampled using vital/hospital records. Mothers self-reported pre-pregnancy PA/sitting. Unconditional logistic regression models estimated associations between PA/sitting categories and the 12 birth defects.
Results
Mothers engaging in pre-pregnancy PA was associated with a reduced odds of five (spina bifida, cleft palate, anorectal atresia, hypospadias, transverse limb deficiency) and a higher odds of two (anencephaly, gastroschisis) birth defects. Mothers spending less time sitting in pre-pregnancy was associated with a reduced odds of two (anorectal atresia, hypospadias) and a higher odds of one (cleft lip with or without cleft palate) birth defect.
Conclusions
Reasonable next steps include replication of these findings, improved exposure assessment, and elucidation of biologic mechanisms.
Impact
-
Using data from two population-based case–control studies, we found that mothers engaging in different types of physical activity in the 3 months before pregnancy had an infant with a reduced odds of five and a higher odds of two birth defects.
-
Mothers spending less time sitting in the 3 months before pregnancy had an infant with a reduced odds of two and a higher odds of one birth defect.
-
Clarification and confirmation from additional studies are needed using more precise exposure measures, distinguishing occupational from leisure-time physical activity, and elucidation of mechanisms supporting these associations.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 14 print issues and online access
$259.00 per year
only $18.50 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
Data availability
The study questionnaires and the process for accessing the data used in this study are described at https://www.cdc.gov/ncbddd/birthdefects/nbdps-public-access-procedures.html.
References
DiPietro, L. et al. Benefits of physical activity during pregnancy and postpartum: an umbrella review. Med. Sci. Sports Exerc. 51, 1292–1302 (2019).
US Department of Health and Human Services. Physical Activity Guidelines for Americans 2nd edn (US Department of Health and Human Services, 2018).
ACOG. Physical activity and exercise during pregnancy and the postpartum period: ACOG Committee Opinion, Number 804. Obstet. Gynecol. 135, e178–e188 (2020).
Mottola, M. F. et al. 2019 Canadian guideline for physical activity throughout pregnancy. Br. J. Sports Med. 52, 1339–1346 (2018).
Bull, F. C. et al. World Health Organization 2020 guidelines on physical activity and sedentary behaviour. Br. J. Sports Med. 54, 1451–1462 (2020).
Bo, K. et al. Exercise and pregnancy in recreational and elite athletes: 2016 evidence summary from the IOC expert group meeting, Lausanne. Part 1-exercise in women planning pregnancy and those who are pregnant. Br. J. Sports Med. 50, 571–589 (2016).
Evenson, K., Mottola, M. & Artal, R. Review of current physical activity guidelines during pregnancy to facilitate advice by health care providers. Obstet. Gynecol. Surv. 74, 481–489 (2019).
Simeone, R. M. et al. Diabetes and congenital heart defects: a systematic review, meta-analysis, and modeling project. Am. J. Prev. Med. 48, 195–204 (2015).
Correa, A. et al. Diabetes mellitus and birth defects. Am. J. Obstet. Gynecol. 199, 237.e231–237.e239 (2008).
Correa, A. et al. Lack of periconceptional vitamins or supplements that contain folic acid and diabetes mellitus-associated birth defects. Am. J. Obstet. Gynecol. 206, 218 e211–e213 (2012).
Waller, D. K. et al. Prepregnancy obesity as a risk factor for structural birth defects. Arch. Pediatr. Adolesc. Med. 161, 745–750 (2007).
Tinker S. C. et al. Specific birth defects in pregnancies of women with diabetes: National Birth Defects Prevention Study, 1997-2011. Am. J. Obstet. Gynecol. 222, 176.e1–176.e11 (2020).
Bo, K. et al. Exercise and pregnancy in recreational and elite athletes: 2016 evidence summary from the IOC expert group meeting, Lausanne. Part 2-the effect of exercise on the fetus, labour and birth. Br. J. Sports Med. 50, 1297–1305 (2016).
Marchi, J., Berg, M., Dencker, A., Olander, E. K. & Begley, C. Risks associated with obesity in pregnancy, for the mother and baby: a systematic review of reviews. Obes. Rev. 16, 621–638 (2015).
Parnell, A. S., Correa, A. & Reece, E. A. Pre-pregnancy obesity as a modifier of gestational diabetes and birth defects associations: a systematic review. Matern. Child Health J. 21, 1105–1120 (2017).
Flak, A. L., Yun Tark, J., Tinker, S. C., Correa, A. & Cogswell, M. E. Major, non-chromosomal, birth defects and maternal physical activity: a systematic review. Birth Defects Res. A Clin. Mol. Teratol. 94, 521–531 (2012).
Agopian, A. J. et al. Maternal occupational physical activity and risk for orofacial clefts. Am. J. Ind. Med. 60, 627–634 (2017).
Davenport, M. H. et al. Effects of prenatal exercise on incidence of congenital anomalies and hyperthermia: a systematic review and meta-analysis. Br. J. Sports Med. 53, 116–123 (2019).
Reefhuis, J. et al. The National Birth Defects Prevention Study: a review of the methods. Birth Defects Res. A Clin. Mol. Teratol. 103, 656–669 (2015).
Tinker, S. C. et al. Next steps for birth defects research and prevention: the birth defects study to evaluate pregnancy exposures (BD-STEPS). Birth Defects Res. A Clin. Mol. Teratol. 103, 733–740 (2015).
Rasmussen, S. A. et al. Guidelines for case classification for the National Birth Defects Prevention Study. Birth Defects Res. A Clin. Mol. Teratol. 67, 193–201 (2003).
Craig, C. et al. International physical activity questionnaire: 12-country reliability and validity. Med. Sci. Sports Exerc. 35, 1381–1395 (2003).
Sanda, B. et al. Reliability and concurrent validity of the International Physical Activity Questionnaire short form among pregnant women. BMC Sports Sci. Med. Rehabil. 9, 7 (2017).
Aittasalo, M., Pasanen, M., Fogelholm, M. & Ojala, K. Validity and repeatability of a short pregnancy leisure time physical activity questionnaire. J. Phys. Act. Health 7, 109–118 (2010).
Rittler, M. et al. Gastroschisis and young mothers: what makes them different from other mothers of the same age? Birth Defects Res. A Clin. Mol. Teratol. 103, 536–543 (2015).
Lin, S., Gensburg, L., Marshall, E. G., Roth, G. B. & Dlugosz, L. Effects of maternal work activity during pregnancy on infant malformations. J. Occup. Environ. Med. 40, 829–834 (1998).
Carmichael, S. L., Shaw, G. M., Neri, E., Schaffer, D. M. & Selvin, S. Physical activity and risk of neural tube defects. Matern. Child Health J. 6, 151–157 (2002).
Juhl, M., Kogevinas, M., Andersen, P. K., Andersen, A. M. & Olsen, J. Is swimming during pregnancy a safe exercise? Epidemiology 21, 253–258 (2010).
Nurminen, T., Lusa, S., Ilmarinen, J. & Kurppa, K. Physical work load, fetal development and course of pregnancy. Scand. J. Work Environ. Health 15, 404–414 (1989).
McDonald, A. D. et al. Congenital defects and work in pregnancy. Br. J. Ind. Med. 45, 581–588 (1988).
2018 Physical Activity Guidelines Advisory Committee. 2018 Physical Activity Guidelines Advisory Committee Scientific Report (Department of Health and Human Services, 2018).
Cogswell, M. E. et al. Control selection and participation in an ongoing, population-based, case-control study of birth defects: the National Birth Defects Prevention Study. Am. J. Epidemiol. 170, 975–985 (2009).
Tinker, S. C. et al. Challenges in studying modifiable risk factors for birth defects. Curr. Epidemiol. Rep. 2, 23–30 (2015).
Benavides, E., Lupo, P. J., Langlois, P. H. & Schraw, J. M. A comprehensive assessment of the associations between season of conception and birth defects, Texas, 1999-2015. Int. J. Environ. Res. Public Health 17, 7120 (2020).
Benavides, E. et al. Urban-rural residence and birth defects prevalence in Texas: a phenome-wide association study. Pediatr. Res. 91, 1587–1594 (2022).
Herdt-Losavio, M. L. et al. Maternal occupation and the risk of birth defects: an overview from the National Birth Defects Prevention Study. Occup. Environ. Med. 67, 58–66 (2010).
Lin, S. et al. Maternal occupation and the risk of major birth defects: a follow-up analysis from the National Birth Defects Prevention Study. Int. J. Hyg. Environ. Health 216, 317–323 (2013).
Lee, L. J. et al. Data linkage between the National Birth Defects Prevention Study and the Occupational Information Network (O*NET) to assess workplace physical activity, sedentary behaviors, and emotional stressors during pregnancy. Am. J. Ind. Med. 59, 137–149 (2016).
Sun, S. et al. Associations between air pollution exposure and birth defects: a time series analysis. Environ. Geochem. Health 43, 4379–4394 (2021).
Rzewnicki, R., Vanden Auweele, Y., De & Bourdeaudhuij, I. Addressing overreporting on the International Physical Activity Questionnaire (IPAQ) telephone survey with a population sample. Public Health Nutr. 6, 299–305 (2003).
Lerman, Y., Jacubovich, R. & Green, M. S. Pregnancy outcome following exposure to shortwaves among female physiotherapists in Israel. Am. J. Ind. Med. 39, 499–504 (2001).
Taskinen, H., Kyyronen, P. & Hemminki, K. Effects of ultrasound, shortwaves, and physical exertion on pregnancy outcome in physiotherapists. J. Epidemiol. Community Health 44, 196–201 (1990).
Kyyronen, P., Taskinen, H., Lindbohm, M. L., Hemminki, K. & Heinonen, O. P. Spontaneous abortions and congenital malformations among women exposed to tetrachloroethylene in dry cleaning. J. Epidemiol. Community Health 43, 346–351 (1989).
Iszatt, N., Nieuwenhuijsen, M. J., Nelson, P., Elliott, P. & Toledano, M. B. Water consumption and use, trihalomethane exposure, and the risk of hypospadias. Pediatrics 127, e389–e397 (2011).
Judge, C. M., Chasan-Taber, L., Gensburg, L., Nasca, P. C. & Marshall, E. G. Physical exposures during pregnancy and congenital cardiovascular malformations. Paediatr. Perinat. Epidemiol. 18, 352–360 (2004).
Clapp, J. F. 3rd The effects of maternal exercise on early pregnancy outcome. Am. J. Obstet. Gynecol. 161, 1453–1457 (1989).
Clapp, J. F. 3rd Exercise and fetal health. J. Dev. Physiol. 15, 9–14 (1991).
Acknowledgements
The authors thank Sarah Tinker and Kathy Wisniewski for their contributions to the writing and analysis, the California Department of Public Health Maternal Child and Adolescent Health Division for providing data for these analyses, and the reviewers for their helpful comments.
Funding
This project was supported through funding from the Centers for Disease Control and Prevention (CDC) to the North Carolina Center for Birth Defects Research and Prevention at the University of North Carolina at Chapel Hill (grant number U01DD001231), and CDC cooperative agreements under PA #96043, PA #02081, FOA #DD09–001, FOA #DD13–003, and NOFO #DD18–001 to the Centers for Birth Defects Research and Prevention participating in the National Birth Defects Prevention Study (NBDPS) and/or the Birth Defects Study To Evaluate Pregnancy exposureS (BD-STEPS). S.M. was supported by the National Institutes of Health (NIH), National Institute of Child Health Development #T32 HD52468. The findings and conclusions in this report are those of the authors and do not necessarily represent the official position of the CDC, the NIH, or the California Department of Public Health.
Author information
Authors and Affiliations
Consortia
Contributions
All authors provided (1) substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; (2) drafting the article or revising it critically for important intellectual content; and (3) final approval of the version to be published.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
The study participants signed a written consent.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Evenson, K.R., Mowla, S., Olshan, A.F. et al. Maternal physical activity, sitting, and risk of non-cardiac birth defects. Pediatr Res 95, 334–341 (2024). https://doi.org/10.1038/s41390-023-02768-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-023-02768-y