Abstract
Background
Air pollution epidemiological studies usually rely on estimates of long-term exposure to air pollutants, which are difficult to ascertain. This problem is accentuated in settings where sources of personal exposure differ from those of ambient concentrations, including household air pollution environments where cooking is an important source.
Objective
The objective of this study was to assess the feasibility of estimating usual exposure to PM2.5 based on short-term measurements.
Methods
We leveraged three types of short-term measurements from a cohort of mother-child pairs in 26 communities in rural Ghana: (A) personal exposure to PM2.5 in mothers and age four children, ambient PM2.5 concentrations (B) at the community level, and (C) at a central site. Baseline models were linear mixed models with a random intercept for community or for participant. Lowest root-mean-square-error (RMSE) was used to select the best-performing model.
Results
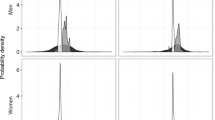
We analyzed 240 community-days and 251 participant-days of PM2.5. Medians (IQR) of PM2.5 were 19.5 (36.5) μg/m3 for the central site, 28.7 (41.5) μg/m3 for the communities, 70.6 (56.9) μg/m3 for mothers, and 80.9 (74.1) μg/m3 for children. The ICCs (95% CI) for community ambient and personal exposure were 0.30 (0.17, 0.47) and 0.74 (0.65, 0.81) respectively. The sources of variability differed during the Harmattan season. Children’s daily exposure was best predicted by models that used community ambient compared to mother’s exposure as a predictor (log-scale RMSE: 0.165 vs 0.325).
Conclusion
Our results support the feasibility of predicting usual personal exposure to PM2.5 using short-term measurements in settings where household air pollution is an important source of exposure. Our results also suggest that mother’s exposure may not be the best proxy for child’s exposure at age four.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 6 print issues and online access
$259.00 per year
only $43.17 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Vos T, Lim SS, Abbafati C, Abbas KM, Abbasi M, Abbasifard M, et al. Global burden of 369 diseases and injuries in 204 countries and territories, 1990–2019: a systematic analysis for the Global Burden of Disease Study 2019. Lancet. 2020;396:1204–22.
Landrigan PJ, Fuller R, Acosta NJR, Adeyi O, Arnold R, Basu N (Nil). The Lancet Commission on pollution and health. The Lancet. 2018;391(10119):462–512.
Garcia E, Rice MB, Gold DR. Air pollution and lung function in children. J Allergy Clin Immunol. 2021;148:1–14.
Rees N, UNICEF. Clear the air for the children: the impact of air pollution on children. New York: UNICEF; 2016 [cited 2021 Oct 30]. http://www.unicef.org/publications/files/UNICEF_Clear_the_Air_for_Children_30_Oct_2016.pdf.
Korten I, Ramsey K, Latzin P. Air pollution during pregnancy and lung development in the child. Paediatr Respiratory Rev. 2017;21:38–46.
Gauderman WJ, Urman R, Avol E, Berhane K, McConnell R, Rappaport E, et al. Association of improved air quality with lung development in children. N. Engl J Med. 2015;372:905–13.
Lee AG, Kaali S, Quinn A, Delimini R, Burkart K, Opoku-Mensah J, et al. Prenatal household air pollution is associated with impaired infant lung function with sex-specific effects. Evidence from GRAPHS, a cluster randomized cookstove intervention trial. Am J Respir Crit Care Med. 2019;199:738–46.
Gauderman WJ, Avol E, Gilliland F, Vora H, Thomas D, Berhane K, et al. The effect of air pollution on lung development from 10 to 18 years of age. N. Engl J Med. 2004;351:1057–67.
Perera F, Ashrafi A, Kinney P, Mills D. Towards a fuller assessment of benefits to children’s health of reducing air pollution and mitigating climate change due to fossil fuel combustion. Environ Res. 2019;172:55–72.
Suades-González E, Gascon M, Guxens M, Sunyer J. Air pollution and neuropsychological development: a review of the latest evidence. Endocrinology. 2015;156:3473–82.
Laden F, Schwartz J, Speizer FE, Dockery DW. Reduction in fine particulate air pollution and mortality: extended follow-up of the Harvard Six Cities study. Am J Respir Crit Care Med. 2006;173:667–72.
Pope CA, Ezzati M, Dockery DW. Fine-particulate air pollution and life expectancy in the United States. N. Engl J Med. 2009;360:376–86.
Clark ML, Peel JL, Balakrishnan K, Breysse PN, Chillrud SN, Naeher LP, et al. Health and household air pollution from solid fuel use: the need for improved exposure assessment. Environ Health Perspect. 2013;121:1120–8.
Milà C, Salmon M, Sanchez M, Ambrós A, Bhogadi S, Sreekanth V, et al. When, where, and what? Characterizing personal PM2.5 exposure in Periurban India by integrating GPS, wearable camera, and ambient and personal monitoring data. Environ Sci Technol. 2018;52:13481–90.
Ni K, Carter E, Schauer JJ, Ezzati M, Zhang Y, Niu H, et al. Seasonal variation in outdoor, indoor, and personal air pollution exposures of women using wood stoves in the Tibetan Plateau: Baseline assessment for an energy intervention study. Environ Int. 2016;94:449–57.
Adhvaryu A, Bharadwaj P, Fenske J, Nyshadham A, Stanley R, Dust and Death: evidence from the West African Harmattan. National Bureau of Economic Research; 2019 [cited 2020 Dec 23]. Report No.: w25937. https://www.nber.org/papers/w25937.
McCracken JP, Schwartz J, Bruce N, Mittleman M, Ryan LM, Smith KR. Combining individual- and group-level exposure information: child carbon monoxide in the guatemala woodstove randomized control trial. Epidemiology 2009;20:127–36.
Brauer M. How much, how long, what, and where. Proc Am Thorac Soc. 2010;7:111–5.
Özkaynak H, Baxter LK, Dionisio KL, Burke J. Air pollution exposure prediction approaches used in air pollution epidemiology studies. J Expo Sci Environ Epidemiol. 2013;23:566–72.
Dionisio KL, Howie SRC, Dominici F, Fornace KM, Spengler JD, Donkor S, et al. The exposure of infants and children to carbon monoxide from biomass fuels in The Gambia: a measurement and modeling study. J Exposure Sci Environ Epidemiol. 2012;22:173–81.
Baumgartner J, Schauer JJ, Ezzati M, Lu L, Cheng C, Patz J, et al. Patterns and predictors of personal exposure to indoor air pollution from biomass combustion among women and children in rural China. Indoor Air. 2011;21:479–88.
Jack DW, Asante KP, Wylie BJ, Chillrud SN, Whyatt RM, Ae-Ngibise KA. et al. Ghana randomized air pollution and health study (GRAPHS): study protocol for a randomized controlled trial. Trials. 2015;16:420
Van Vliet EDS, Asante K, Jack DW, Kinney PL, Whyatt RM, Chillrud SN, et al. Personal exposures to fine particulate matter and black carbon in households cooking with biomass fuels in rural Ghana. Environ Res. 2013;127:40–8.
Ofosu FG, Hopke PK, Aboh IJK, Bamford SA. Biomass burning contribution to ambient air particulate levels at Navrongo in the Savannah zone of Ghana. J Air Waste Manag Assoc. 2013;63:1036–45.
Chillrud SN, Ae-Ngibise KA, Gould CF, Owusu-Agyei S, Mujtaba M, Manu G, et al. The effect of clean cooking interventions on mother and child personal exposure to air pollution: results from the Ghana Randomized Air Pollution and Health Study (GRAPHS). J Exposure Sci Environ Epidemiol. 2021;1–16.
Gunnsteinsson S, Labrique AB, West KP, Christian P, Mehra S, Shamim AA, et al. Constructing Indices of rural living standards in northwestern Bangladesh. J Health Popul Nutr. 2010;28:509–19.
Owusu-Agyei S, Nettey OEA, Zandoh C, Sulemana A, Adda R, Amenga-Etego S, et al. Demographic patterns and trends in Central Ghana: baseline indicators from the Kintampo Health and Demographic Surveillance System. Glob Health Action. 2012;5:19033.
Koo TK, Li MY. A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med. 2016;15:155–63.
Smith KR, Bruce N, Balakrishnan K, Adair-Rohani H, Balmes J, Chafe Z, et al. Millions dead: how do we know and what does it mean? Methods used in the comparative risk assessment of household air pollution. Annu Rev Public Health. 2014 ;35(Mar):185–206.
Sanchez M, Milà C, Sreekanth V, Balakrishnan K, Sambandam S, Nieuwenhuijsen M, et al. Personal exposure to particulate matter in peri-urban India: predictors and association with ambient concentration at residence. J Expo Sci Environ Epidemiol. 2019 [cited 2020 May 7]; http://www.nature.com/articles/s41370-019-0150-5.
Keller JP, Clark ML. Estimating long-term average household air pollution concentrations from repeated short-term measurements in the presence of seasonal trends and crossover. Environ Epidemiol. 2022;6:e188.
Johannesson S, Gustafson P, Molnár P, Barregard L, Sällsten G. Exposure to fine particles (PM2.5 and PM1) and black smoke in the general population: personal, indoor, and outdoor levels. J Expo Sci Environ Epidemiol. 2007;17:613–24.
Armstrong JR, Campbell H. Indoor air pollution exposure and lower respiratory infections in young Gambian children. Int J Epidemiol. 1991;20:424–9.
de Francisco A, Morris J, Hall AJ, Armstrong Schellenberg JR, Greenwood BM. Risk factors for mortality from acute lower respiratory tract infections in young Gambian children. Int J Epidemiol. 1993;22:1174–82.
Schwartz J. Air pollution and children’s health. Pediatrics 2004;113:1037–43.
Nazif-Muñoz JI, Spengler JD, Arku RE, Oulhote Y. Solid fuel use and early child development disparities in Ghana: analyses by gender and urbanicity. J Exposure Sci Environ Epidemiol. 2020;30:698–706.
Acknowledgements
The authors acknowledge support from the National Institutes of Environmental Health Sciences grants R01 ES02699 and R01 ES019547. The authors acknowledge additional support from P30 ES009089. MD was supported by the Columbia World Project, Combating Household Air Pollution With Clean Energy, and AGL was supported by K23HL135349. The authors are grateful to study participants, without whom this study would not have been possible. The findings and conclusions in this report are those of the authors and do not necessarily represent the official position of the U.S. National Institutes of Health.
Author information
Authors and Affiliations
Contributions
MD, SC, DJ, and KP developed the study design. MM, SC, KS, and DJ led the exposure assessment work. MD conducted the literature review. MD was responsible for writing code and analyzing the data with input from all other authors. All authors contributed to the interpretation of findings, writing, and editing of manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Daouda, M., Mujtaba, M.N., Yang, Q. et al. Prediction of personal exposure to PM2.5 in mother-child pairs in rural Ghana. J Expo Sci Environ Epidemiol 32, 629–636 (2022). https://doi.org/10.1038/s41370-022-00420-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41370-022-00420-1
Keywords
This article is cited by
-
Geospatial determinants of maternal and child exposure to fine particulate matter in Kintampo, Ghana: Levels within the household and community, by surrounding building density and near roadways
Journal of Exposure Science & Environmental Epidemiology (2023)