Key Points
-
Advances in cancer detection and therapy have dramatically increased the survival rates of patients with most cancers. For many patients, pain is the first sign of cancer and the majority of individuals will experience moderate to severe pain and/or neuropathy during the course of their disease and into survivorship.
-
Cancer pain has a considerable effect on the diagnosis, quality of life and survival of patients with cancer. During the past decade, preclinical and clinical data has begun to provide insight into the mechanisms that drive and mask cancer pain, and the mechanisms by which anti-neoplastic agents induce peripheral neuropathy.
-
Cancer pain seems to be modulated in the CNS by opioid-dependent mechanisms and, at least in an animal model of pancreatic cancer, endogenous opioid mechanisms seem to mask early- and mid-stage pancreatic cancer-related pain behaviours, which may contribute to the late diagnosis and lethality of this disease. Understanding the CNS mechanisms involved in masking and driving cancer pain might allow earlier detection of cancer and more effective therapies for controlling late-stage cancer pain.
-
Common anti-neoplastic agents such as the vinca alkaloids, taxanes and platinum-based compounds frequently induce a chemotherapy-induced peripheral neuropathy (CIPN) in which both large and small primary afferent sensory neurons are injured. As CIPN can affect both the quality of life, and in some cases the full delivery of the anti-neoplastic agent, the development of pre-emptive therapies to block or attenuate CIPN has the potential to improve both the quality of life and, in some cases, the survival of patients with cancer.
-
Tumour-induced cancer pain tends to increase with advancing disease, and can be driven by tumour-released products, acidosis and direct injury to sensory nerve fibres present at the site of the primary tumour or at the site of tumour metastasis.
-
An increase in our understanding of the thermal, chemical and mechanical transducers expressed by nociceptors, coupled with an increase in our knowledge of the interactions that occur at the nociceptor–tumour interface, have provided insights that could lead to the development of novel mechanism-based therapies to treat cancer pain.
-
In addition to reducing pain and/or neuropathy, commonly used analgesics such as the non-steroidal anti-inflammatory drugs (NSAIDS), cyclooxygenase 2 inhibitors and opiates may influence cancer disease progression. As patients with cancer continue to survive longer, it will be important to develop a mechanism-based understanding of the influence analgesics might have on the growth, vascularization and metastasis of tumours and their associated stromal cells.
-
By incorporating cancer pain research into mainstream cancer research it is possible that analgesic and cancer therapies can be simultaneously assessed with regard to how they affect the survival, overall health and quality of life of both patients with cancer and survivors.
Abstract
Cancer pain significantly affects the diagnosis, quality of life and survival of patients with cancer. During the past decade, preclinical and clinical data has begun to provide insight into the mechanisms that drive and mask cancer pain and the mechanisms by which anti-neoplastic agents induce peripheral neuropathy. Developing a mechanism-based understanding and mechanism-based therapies to treat cancer-associated pain and sensory neuropathy, and incorporating these into mainstream cancer research and therapy, will be crucial to improving the quality of life and survival of patients with cancer.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$189.00 per year
only $15.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Stewart, B. & Kleihues, P. World Cancer Report (International Agency for Research on Cancer, Lyon, 2003).
World Health Organization Cancer Control. <http://www.who.int./cancer>(2006).
Jemal, A. et al. Cancer statistics, 2006. CA Cancer J. Clin. 56, 106–130 (2006). An excellent source, published on a yearly basis, that reports changes in the incidence, survival and mortality of patients in the United States with different types of cancer.
Edwards, B. et al. Annual report to the nation on the status of cancer, 1975–2002, featuring population-based trends in cancer treatment. J. Natl Cancer Inst. 97, 1407–1427 (2005).
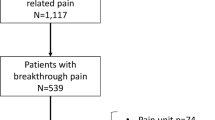
Portenoy, R. K., Payne, D. & Jacobsen, P. Breakthrough pain: characteristics and impact in patients with cancer pain. Pain 81, 129–134 (1999).
Mercadante, S. & Arcuri, E. Breakthrough pain in cancer patients: pathophysiology and treatment. Cancer Treat. Rev. 24, 425–432 (1998). A seminal review summarizing the pathological mechanisms and therapies for treating breakthrough pain in patients with cancer.
Meuser, T. et al. Symptoms during cancer pain treatment following WHO-guidelines: a longitudinal follow-up study of symptom prevalence, severity and etiology. Pain 93, 247–257 (2001).
Quasthoff, S. & Hartung, H. P. Chemotherapy-induced peripheral neuropathy. J. Neurol. 249, 9–17 (2002).
Mielke, S., Sparreboom, A. & Mross, K. Peripheral neuropathy: a persisting challenge in paclitaxel-based regimes. Eur. J. Cancer 42, 24–30 (2006).
Pasetto, L., D'Andrea, M., Rossi, E. & Monfardini, S. Oxaliplatin-related neurotoxicity: how and why? Crit. Rev. Oncol. Hematol. 59, 159–168 (2006).
Julius, D. & Basbaum, A. I. Molecular mechanisms of nociception. Nature 413, 203–210 (2001). A clear and comprehensive review of the cellular and molecular biology of nociceptors.
Mantyh, P. W. A mechanism based understanding of cancer pain. Pain 96, 1–2 (2002).
Mantyh, P. W., Clohisy, D. R., Koltzenburg, M. & Hunt, S. P. Molecular mechanisms of cancer pain. Nature Rev. Cancer 2, 201–209 (2002).
Dougherty, P. M., Cata, J. P., Cordella, J. V., Burton, A. & Weng, H. R. Taxol-induced sensory disturbance is characterized by preferential impairment of myelinated fiber function in cancer patients. Pain 109, 132–142 (2004). Evidence that large sensory fibres are preferentially affected in humans receiving intravenous admin-istration of paclitaxel as part of their cancer therapy.
Postma, T. J., Vermorken, J. B., Liefting, A. J., Pinedo, H. M. & Heimans, J. J. Paclitaxel-induced neuropathy. Ann. Oncol. 6, 489–494 (1995).
Einzig, A. I. et al. Phase I study of paclitaxel (taxol) and granulocyte colony stimulating factor (G-CSF) in patients with unresectable malignancy. Invest. New Drugs 16, 29–36 (1998).
Verstappen, C. C., Postma, T. J., Hoekman, K. & Heimans, J. J. Peripheral neuropathy due to therapy with paclitaxel, gemcitabine, and cisplatin in patients with advanced ovarian cancer. J. Neurooncol. 63, 201–205 (2003).
Jemal, A. et al. Annual report to the nation on the status of cancer, 1975–2001, with a special feature regarding survival. Cancer 101, 3–27 (2004).
Granville, C. A. & Dennis, P. A. An overview of lung cancer genomics and proteomics. Am. J. Respir. Cell Mol. Biol. 32, 169–176 (2005).
Barber, M. D., Ross, J. A. & Fearon, K. C. Changes in nutritional, functional, and inflammatory markers in advanced pancreatic cancer. Nutr. Cancer 35, 106–110 (1999).
Kelsen, D. P. et al. Pain and depression in patients with newly diagnosed pancreas cancer. J. Clin. Oncol. 13, 748–755 (1995).
Elli, M. et al. Considerations on early diagnosis of carcinoma of the pancreas. Hepatogastroenterology 50, 2205–2207 (2003).
Grahm, A. L. & Andren-Sandberg, A. Prospective evaluation of pain in exocrine pancreatic cancer. Digestion 58, 542–549 (1997).
Wong, G. Y. et al. Effect of neurolytic celiac plexus block on pain relief, quality of life, and survival in patients with unresectable pancreatic cancer: a randomized controlled trial. JAMA 291, 1092–1099 (2004).
Lindsay, T. H. et al. A quantitative analysis of the sensory and sympathetic innervation of the mouse pancreas. Neuroscience 137, 1417–1426 (2006).
Lindsay, T. H. et al. Pancreatic cancer pain and its correlation with changes in tumor vasculature, macrophage infiltration, neuronal innervation, body weight and disease progression. Pain 119, 233–246 (2005). The first paper to present an animal model of pancreatic cancer pain and demonstrate that, as in humans with pancreatic cancer, there is a disparity between the appearance of pancreatic pathology and the appearance of pain-related behaviours.
Porreca, F., Ossipov, M. H. & Gebhart, G. F. Chronic pain and medullary descending facilitation. Trends Neurosci. 25, 319–325 (2002). A review summarizing the evidence that descending modulation from higher brain centres can facilitate pain transmission in the spinal cord.
Ren, K. & Dubner, R. Descending modulation in persistent pain: an update. Pain 100, 1–6 (2002).
Sevcik, M. et al. Endogenous opioids inhibit early stage pancreatic pain in a mouse model of pancreatic cancer. Gastroenterology (in the press).
Borgbjerg, F. M., Frigast, C. & Madsen, J. B. Tonic endogenous opioid inhibition of visceral noxious information in rabbits. Gastroenterology 111, 78–84 (1996).
Basbaum, A. I. & Fields, H. L. Endogenous pain control systems: brainstem spinal pathways and endorphin circuitry. Annu. Rev. Neurosci. 7, 309–388 (1984). A seminal review of the original work demonstrating that higher centres of the brain can inhibit pain transmission in the spinal cord.
Smith, J. P., Conter, R. L., Demers, T. M., McLaughlin, P. J. & Zagon, I. S. Elevated levels of opioid growth factor in the plasma of patients with pancreatic cancer. Pancreas 21, 158–164 (2000).
Zagon, I. S., Verderame, M. F. & McLaughlin, P. J. The biology of the opioid growth factor receptor (OGFr). Brain Res. Brain Res. Rev. 38, 351–376 (2002).
Apkarian, A. V., Bushnell, M. C., Treede, R. D. & Zubieta, J. K. Human brain mechanisms of pain perception and regulation in health and disease. Eur. J. Pain 9, 463–484 (2005).
Konsman, J. P., Vigues, S., Mackerlova, L., Bristow, A. & Blomqvist, A. Rat brain vascular distribution of interleukin-1 type-1 receptor immunoreactivity: relationship to patterns of inducible cyclooxygenase expression by peripheral inflammatory stimuli. J. Comp. Neurol. 472, 113–129 (2004).
Watkins, L., Maier, S. F. & Goehler, L. E. Immune activation: the role of pro-inflammatory cytokines in inflammation, illness responses and pathological pain states. Pain 63, 289–302 (1995).
Gebhart, G. F. Descending modulation of pain. Neurosci. Biobehav. Rev. 27, 729–737 (2004).
Ness, T. J. & Gebhart, G. F. Characterization of neuronal responses to noxious visceral and somatic stimuli in the medial lumbosacral spinal cord of the rat. J. Neurophysiol. 57, 1867–1892 (1987).
Granville, L. et al. Review and update of uncommon primary pleural tumors: a practical approach to diagnosis. Arch. Pathol. Lab. Med. 129, 1428–1443 (2005).
Aghajanian, C. et al. Phase II study of 'dose-dense' high-dose chemotherapy treatment with peripheral-blood progenitor-cell support as primary treatment for patients with advanced ovarian cancer. J. Clin. Oncol. 16, 1852–1860 (1998).
Pasini, F., Durante, E., De Manzoni, D., Rosti, G. & Pelosi, G. High-dose chemotherapy in small-cell lung cancer. Anticancer Res. 22, 3465–3472 (2002).
Cocconi, G. et al. Mature results of a prospective randomized trial comparing a three-weekly with an accelerated weekly schedule of cisplatin in advanced ovarian carcinoma. Am. J. Clin. Oncol. 22, 559–567 (1999).
Guastalla, J. P. et al. Efficacy and safety of the paclitaxel and carboplatin combination in patients with previously treated advanced ovarian carcinoma. A multicenter GINECO (Group d'Investigateurs Nationaux pour l'Etude des Cancers Ovariens) phase II study. Ann. Oncol. 9, 37–43 (1998).
Holmes, J. et al. Comparative neurotoxicity of oxaliplatin, cisplatin, and ormaplatin in a Wistar rat model. Toxicol. Sci. 46, 342–351 (1998).
Cavaletti, G. et al. Distribution of paclitaxel within the nervous system of the rat after repeated intravenous administration. Neurotoxicology 21, 389–393 (2000). A report showing that, compared with other peripheral tissues, the DRG preferentially accumulate intravenously infused paclitaxel.
Cavaletti, G. et al. Effects of different schedules of oxaliplatin treatment on the peripheral nervous system of the rat. Eur. J. Cancer 37, 2457–2463 (2001).
Screnci, D. et al. Relationships between hydrophobicity, reactivity, accumulation and peripheral nerve toxicity of a series of platinum drugs. Br. J. Cancer 82, 966–972 (2000).
Theiss, C. & Meller, K. Taxol impairs anterograde axonal transport of microinjected horseradish peroxidase in dorsal root ganglia neurons in vitro. Cell Tissue Res. 299, 213–224 (2000).
Cavaletti, G. et al. Effect on the peripheral nervous system of the short-term intravenous administration of paclitaxel in the rat. Neurotoxicology 18, 137–145 (1997).
Cliffer, K. D. et al. Physiological characterization of taxol-induced large-fiber sensory neuropathy in the rat. Ann. Neurol. 43, 46–55 (1998). One of the first animal models that allowed researchers to demonstrate that intravenous infusion of paclitaxel preferentially targets large primary afferent sensory neurons.
Mimura, Y., Kato, H., Eguchi, K. & Ogawa, T. Schedule dependency of paclitaxel-induced neuropathy in mice: a morphological study. Neurotoxicology 21, 513–520 (2000).
Persohn, E. et al. Morphological and morphometric analysis of paclitaxel and docetaxel-induced peripheral neuropathy in rats. Eur. J. Cancer 41, 1460–1466 (2005).
Peters, C. M. et al. Intravenous paclitaxel administration in the rat induces a peripheral sensory neuropathy characterized by macrophage infiltration and injury to sensory neurons and their supporting cells. Exp. Neurol. (in the press).
Obata, K. et al. Contribution of injured and uninjured dorsal root ganglion neurons to pain behavior and the changes in gene expression following chronic constriction injury of the sciatic nerve in rats. Pain 101, 65–77 (2003).
Peters, C. M. et al. Tumor-induced injury of primary afferent sensory nerve fibers in bone cancer pain. Exp. Neurol. 193, 85–100 (2005).
Tsuzuki, K. et al. Differential regulation of P2X3 mRNA expression by peripheral nerve injury in intact and injured neurons in the rat sensory ganglia. Pain 91, 351–360 (2001).
Tsujino, H. et al. Activating transcription factor 3 (ATF3) induction by axotomy in sensory and motoneurons: a novel neuronal marker of nerve injury. Mol. Cell. Neurosci. 15, 170–182 (2000).
Jimenez-Andrade, J. M., Peters, C. M., Mejia, N. A., Ghilardi, J. R. & Mantyh, P. W. Sensory neurons and their supporting cells located in the trigeminal, thoracic and lumbar ganglia differentially express markers of injury following intravenous administration of paclitaxel in the rat. Neurosci. Lett. 405, 62–67 (2006).
Glantz, M. J. et al. Paclitaxel disposition in plasma and central nervous systems of humans and rats with brain tumors. J. Natl Cancer Inst. 87, 1077–1081 (1995).
Jacobs, J. M. Vascular permeability and neurotoxicity. Environ. Health Perspect. 26, 107–116 (1978).
Pettersson, C. A., Sharma, H. S. & Olsson, Y. Vascular permeability of spinal nerve roots. A study in the rat with Evans blue and lanthanum as tracers. Acta Neuropathol. (Berl.) 81, 148–154 (1990).
Grothey, A. Oxaliplatin-safety profile: neurotoxicity. Semin. Oncol. 30, 5–13 (2003).
Coleman, R. E. Skeletal complications of malignancy. Cancer 80, 1588–1594 (1997).
Mercadante, S. Malignant bone pain: pathophysiology and treatment. Pain 69, 1–18 (1997).
Bjurholm, A., Kreicbergs, A., Brodin, E. & Schultzberg, M. Substance P- and CGRP-immunoreactive nerves in bone. Peptides 9, 165–171 (1988).
Bjurholm, A., Kreicbergs, A., Terenius, L., Goldstein, M. & Schultzberg, M. Neuropeptide Y-, tyrosine hydroxylase- and vasoactive intestinal polypeptide-immunoreactive nerves in bone and surrounding tissues. J. Auton. Nerv. Syst. 25, 119–125 (1988).
Tabarowski, Z., Gibson-Berry, K. & Felten, S. Y. Noradrenergic and peptidergic innervation of the mouse femur bone marrow. Acta Histochem. 98, 453–457 (1996).
Coleman, R. E. Metastatic bone disease: clinical features, pathophysiology and treatment strategies. Cancer Treat. Rev. 27, 165–176 (2001).
Cherny, N. New strategies in opioid therapy for cancer pain. J. Oncol. Manag. 9, 8–15 (2000).
Hanks, G. W. et al. Morphine and alternative opioids in cancer pain: the EAPC recommendations. Br. J. Cancer 84, 587–593 (2001).
Portenoy, R. K. & Lesage, P. Management of cancer pain. Lancet 353, 1695–1700 (1999).
Foley, K. M. Misconceptions and controversies regarding the use of opioids in cancer pain. Anti-Cancer Drugs 6, 4–13 (1995).
Weber, M. & Huber, C. Documentation of severe pain, opioid doses, and opioid-related side effects in outpatients with cancer: a retrospective study. J. Pain Symptom Manage. 17, 49–54 (1999).
Davies, N. M. & Jamali, F. COX-2 selective inhibitors cardiac toxicity: getting to the heart of the matter. J. Pharm. Pharm. Sci. 7, 332–336 (2004).
Mukherjee, D., Nissen, S. E. & Topol, E. J. Risk of cardiovascular events associated with selective COX-2 inhibitors. JAMA 286, 954–959 (2001).
Mercadante, S. Problems of long-term spinal opioid treatment in advanced cancer patients. Pain 79, 1–13 (1999).
Honore, P. et al. Osteoprotegerin blocks bone cancer-induced skeletal destruction, skeletal pain and pain-related neurochemical reorganization of the spinal cord. Nature Med. 6, 521–528 (2000).
Luger, N. M. et al. Osteoprotegerin diminishes advanced bone cancer pain. Cancer Res. 61, 4038–4047 (2001).
Sabino, M. A. et al. Simultaneous reduction in cancer pain, bone destruction, and tumor growth by selective inhibition of cyclooxygenase-2. Cancer Res. 62, 7343–7349 (2002). A study in an animal model of bone cancer pain demonstrating that a COX2 inhibitor simultaneously reduces pain and tumour burden.
Delaisse, J. M. & Vaes, G. in Biology and Physiology of the Osteoclast (eds Rifkin, B. R. & Gay, C. V.) 289–314 (CRC, Ann Arbor, USA, 1992).
Clohisy, D. R., Perkins, S. L. & Ramnaraine, M. L. Review of cellular mechanisms of tumor osteolysis. Clin. Orthop. Rel. Res. 373, 104–114 (2000).
Berenson, J. R. et al. Zoledronic acid reduces skeletal-related events in patients with osteolytic metastases. Cancer 91, 1191–1200 (2001).
Fulfaro, F., Casuccio, A., Ticozzi, C. & Ripamonti, C. The role of bisphosphonates in the treatment of painful metastatic bone disease: a review of phase III trials. Pain 78, 157–169 (1998).
Major, P. P., Lipton, A., Berenson, J. & Hortobagyi, G. Oral bisphosphonates: a review of clinical use in patients with bone metastases. Cancer 88, 6–14 (2000).
Rogers, M. J. et al. Cellular and molecular mechanisms of action of bisphosphonates. Cancer 88, 2961–2978 (2000).
Gatti, D. & Adami, S. New bisphosphonates in the treatment of bone diseases. Drugs Aging 15, 285–296 (1999).
Rodan, G. & Martin, T. Therapeutic approaches to bone disease. Science 289, 1508–1514 (2000).
Hiraga, T., Tanaka, S., Yamamoto, M., Nakajima, T., Ozawa, H. Inhibitory effects of bisphosphonate YM175 on bone resorption induced by metastic bone tumor. Bone 18, 1–7 (1996).
Sasaki, A. et al. Bisphosphonate risedronate reduces metastic human breast cancer burden in bone in nude mice. Cancer Res. 55, 3551–3557 (1995).
Yoneda, T., Williams, P. J., Myoi, A., Michigami, T. & Mbalaviele, G. in Tumor Bone Diseases and Osteoporosis in Cancer Patients (ed. Body, J.-J.) 41–70 (Marcel Dekker, New York, 2000).
Sevcik, M. A. et al. Bone cancer pain: the effects of the bisphosphonate alendronate on pain, skeletal remodeling, tumor growth and tumor necrosis. Pain 111, 169–180 (2004).
Horton, A., Nesbitt, S., Bennett, J. & Stenbeck, G. in Principles of Bone Biology Vol. 1 (eds Bilezikian, J. P., Raisz L. G. & Rodan, G. A.) 265–286 (Academic, San Diego, 2002).
Tripathy, D., Body, J. J. & Bergstrom, B. Review of ibandronate in the treatment of metastatic bone disease: experience from phase III trials. Clin. Ther. 26, 1947–1959 (2004).
Simonet, W. S. et al. Osteoprotegerin: a novel secreted protein involved in the regulation of bone density. Cell 89, 309–319 (1997).
Rodan, G. A. & Martin, T. J. Therapeutic approaches to bone diseases. Science 289, 1508–1514 (2000).
Yasuda, H. et al. Identity of osteoclastogenesis inhibitory factor (OCIF) and osteoprotegerin (OPG): a mechanism by which OPG/OCIF inhibits osteoclastogenesis in vitro. Endocrinology 139, 1329–1337 (1998).
Sutherland, S., Cook, S. & McClesky, E. W. Chemical mediators of pain due to tissue damage and ischemia. Prog. Brain Res. 129, 21–38 (2000).
Olson, T. H., Riedl, M. S., Vulchanova, L., Ortiz-Gonzalez, X. R. & Elde, R. An acid sensing ion channel (ASIC) localizes to small primary afferent neurons in rats. Neuroreport 9, 1109–1113 (1998).
Caterina, M. J. et al. Impaired nociception and pain sensation in mice lacking the capsaicin receptor. Science 288, 306–313 (2000).
Tominaga, M. et al. The cloned capsaicin receptor integrates multiple pain-producing stimuli. Neuron 21, 531–543 (1998).
Bassilana, F. et al. The acid-sensitive ionic channel subunit ASIC and the mammalian degenerin MDEG form a heteromultimeric H+-gated Na+ channel with novel properties. J. Biol. Chem. 272, 28819–28822 (1997).
Griffiths, J. R. Are cancer cells acidic? Br. J. Cancer 64, 425–427 (1991).
Ghilardi, J. R. et al. Selective blockade of the capsaicin receptor TRPV1 attenuates bone cancer pain. J. Neurosci. 25, 3126–3131 (2005).
Alder, C.-P. Bone Diseases (Springer, Berlin, 2000).
Mundy, G. R. Bone Remodeling and its Disorders (Taylor Francis, London, 1999).
Rubert, C. K., Henshaw, R. M. & Malawer, M. M. in Tumor Bone Disease and Osteoporosis in Cancer Patients (ed. Body, J.-J.) 305–356 (Marcel Dekker, New York, 2000).
Galasko, C. S. Diagnosis of skeletal metastases and assessment of response to treatment. Clin. Orthop. Relat. Res. 312, 64–75 (1995).
Nielsen, O. S., Munro, A. J. & Tannock, I. F. Bone metastases: pathophysiology and management policy. J. Clin. Oncol. 9, 509–524 (1991).
DeLeo, J. A. & Yezierski, R. P. The role of neuroinflammation and neuroimmune activation in persistent pain. Pain 90, 1–6 (2001).
Nadler, R. B. et al. IL-1β and TNF-α in prostatic secretions are indicators in the evaluation of men with chronic prostatitis. J. Urol. 164, 214–218 (2000).
Watkins, L. R., Maier, S. F. & Goehler, L. E. Immune activation: the role of pro-inflammatory cytokines in inflammation, illness responses and pathological pain states. Pain 63, 289–302 (1995).
Davar, G. Endothelin-1 and metastatic cancer pain. Pain Med. 2, 24–27 (2001).
Nelson, J., Bagnato, A., Battistini, B. & Nisen, P. The endothelin axis: emerging role in cancer. Nature Rev. Cancer 3, 110–116 (2003).
DeLeo, J. A., Colburn, R. W., Nichols, M. & Malhotra, A. Interleukin-6-mediated hyperalgesia/allodynia and increased spinal IL-6 expression in a rat mononeuropathy model. J. Interferon Cytokine Res. 16, 695–700 (1996).
Opree, A. & Kress, M. Involvement of the proinflammatory cytokines tumor necrosis factor-α, IL-1 β, and IL-6 but not IL-8 in the development of heat hyperalgesia: effects on heat-evoked calcitonin gene-related peptide release from rat skin. J. Neurosci. 20, 6289–6293 (2000).
Stoscheck, C. M. & King, L. E. Jr. Role of epidermal growth factor in carcinogenesis. Cancer Res. 46, 1030–1037 (1986).
Radinsky, R. Growth factors and their receptors in metastasis. Semin. Cancer Biol. 2, 169–177 (1991).
Silver, B. J. Platelet-derived growth factor in human malignancy. Biofactors 3, 217–227 (1992).
Kundu, N., Yang, Q. Y., Dorsey, R. & Fulton, A. M. Increased cyclooxygenase-2 (cox-2) expression and activity in a murine model of metastatic breast cancer. Int. J. Cancer 93, 681–686 (2001).
Molina, M. A., Sitja-Arnau, M., Lemoine, M. G., Frazier, M. L. & Sinicrope, F. A. Increased cyclooxygenase-2 expression in human pancreatic carcinomas and cell lines: growth inhibition by nonsteroidal anti-inflammatory drugs. Cancer Res. 59, 4356–4362 (1999).
Vasko, M. R. Prostaglandin-induced neuropeptide release from spinal cord. Prog. Brain Res. 104, 367–380 (1995).
Pilbeam, C. C., Harrison, J. R. & Raisz, L. G. in Principles of Bone Biology (eds Bilezikian, J. P., Raisz L. G. & Rodan, G. A.) (Academic, San Diego, 2002).
Gupta, R. A. & Dubois, R. N. Colorectal cancer prevention and treatment by inhibition of cyclooxygenase-2. Nature Rev. Cancer 1, 11–21 (2001).
Thun, M. J., Henley, S. J. & Patrono, C. Nonsteroidal anti-inflammatory drugs as anticancer agents: mechanistic, pharmacologic, and clinical issues. J. Natl Cancer Inst. 94, 252–266 (2002).
Iniguez, M. A., Rodriguez, A., Volpert, O. V., Fresno, M. & Redondo, J. M. Cyclooxygenase-2: a therapeutic target in angiogenesis. Trends Mol. Med. 9, 73–78 (2003). An excellent review showing that different types of NSAID can have an effect on neovascularization both in vivo and in vitro.
Williams, C. S., Tsujii, M., Reese, J., Dey, S. K. & DuBois, R. N. Host cyclooxygenase-2 modulates carcinoma growth. J. Clin. Invest. 105, 1589–1594 (2000).
Masferrer, J. L. et al. Antiangiogenic and antitumor activities of cyclooxygenase-2 inhibitors. Cancer Res. 60, 1306–1311 (2000).
Carducci, M. A. et al. Atrasentan, an endothelin-receptor antagonist for refractory adenocarcinomas: safety and pharmacokinetics. J. Clin. Oncol. 20, 2171–2180 (2002).
Nelson, J. B. & Carducci, M. A. The role of endothelin-1 and endothelin receptor antagonists in prostate cancer. BJU Int. 85, 45–48 (2000).
Nelson, J. B. et al. Identification of endothelin-1 in the pathophysiology of metastatic adenocarcinoma of the prostate. Nature Med. 1, 944–949 (1995).
Pomonis, J. D., Rogers, S. D., Peters, C. M., Ghilardi, J. R. & Mantyh, P. W. Expression and localization of endothelin receptors: implications for the involvement of peripheral glia in nociception. J. Neurosci. 21, 999–1006 (2001).
Davar, G., Hans, G., Fareed, M. U., Sinnott, C. & Strichartz, G. Behavioral signs of acute pain produced by application of endothelin-1 to rat sciatic nerve. Neuroreport 9, 2279–2283 (1998).
Peters, C. M. et al. Endothelin and the tumorigenic component of bone cancer pain. Neuroscience 126, 1043–1052 (2004).
Couture, R., Harrisson, M., Vianna, R. M. & Cloutier, F. Kinin receptors in pain and inflammation. Eur. J. Pharmacol. 429, 161–176 (2001).
Fox, A. et al. Regulation and function of spinal and peripheral neuronal B1 bradykinin receptors in inflammatory mechanical hyperalgesia. Pain 104, 683–691 (2003).
Sevcik, M. A. et al. Analgesic efficacy of bradykinin B1 antagonists in a murine bone cancer pain model. J. Pain 6, 771–775 (2005).
Averill, S., McMahon, S. B., Clary, D. O., Reichardt, L. F. & Priestley, J. V. Immunocytochemical localization of trkA receptors in chemically identified subgroups of adult rat sensory neurons. Eur. J. Neurosci. 7, 1484–1494 (1995).
Donnerer, J., Schuligoi, R. & Stein, C. Increased content and transport of substance P and calcitonin gene-related peptide in sensory nerves innervating inflamed tissue: evidence for a regulatory function of nerve growth factor in vivo. Neuroscience 49, 693–698 (1992).
Ji, R. R., Samad, T. A., Jin, S. X., Schmoll, R. & Woolf, C. J. p38 MAPK activation by NGF in primary sensory neurons after inflammation increases TRPV1 levels and maintains heat hyperalgesia. Neuron 36, 57–68 (2002).
Ramer, M. S., Bradbury, E. J. & McMahon, S. B. Nerve growth factor induces P2X3 expression in sensory neurons. J. Neurochem. 77, 864–875 (2001).
Rueff, A. & Dray, A. Sensitization of peripheral afferent fibres in the in vitro neonatal rat spinal cord-tail by bradykinin and prostaglandins. Neuroscience 54, 527–535 (1993).
Verge, V. M. K., Tetzlaff, W., Bisby, M. A. & Richardson, P. M. Influence of nerve growth factor on neurofilament gene expression in mature primary sensory neurons. J. Neurosci. 10, 2018–2025 (1990).
Gould, H. J. et al. A possible role for nerve growth factor in the augmentation of sodium channels in models of chronic pain. Brain Res. 854, 19–29 (2000).
Heumann, R., Korsching, S., Bandtlow, C. & Thoenen, H. Changes of nerve growth factor synthesis in nonneuronal cells in response to sciatic nerve transection. J. Cell Biol. 104, 1623–1631 (1987).
Halvorson, K. G. et al. A blocking antibody to nerve growth factor attenuates skeletal pain induced by prostate tumor cells growing in bone. Cancer Res. 65, 9426–9435 (2005).
Sevcik, M. A. et al. Anti-NGF therapy profoundly reduces bone cancer pain and the accompanying increase in markers of peripheral and central sensitization. Pain 115, 128–141 (2005).
Walsh, G. S., Krol, K. M. & Kawaja, M. D. Absence of the p75 neurotrophin receptor alters the pattern of sympathosensory sprouting in the trigeminal ganglia of mice overexpressing nerve growth factor. J. Neurosci. 19, 258–273 (1999).
Woodham, P., Anderson, P. N., Nadim, W. & Turmaine, M. Satellite cells surrounding axotomised rat dorsal root ganglion cells increase expression of a GFAP-like protein. Neurosci. Lett. 98, 8–12 (1989).
Hu, P. & McLachlan, E. M. Macrophage and lymphocyte invasion of dorsal root ganglia after peripheral nerve lesions in the rat. Neuroscience 112, 23–38 (2002).
Maindrault-Goebel, F. et al. High-dose intensity oxaliplatin added to the simplified bimonthly leucovorin and 5-fluorouracil regimen as second-line therapy for metastatic colorectal cancer (FOLFOX 7). Eur. J. Cancer 37, 1000–1005 (2001).
Stewart, J. M. Bradykinin antagonists as anti-cancer agents. Curr. Pharm. Des. 9, 2036–2042 (2003).
Miknyoczki, S. J. et al. The neurotrophin–trk receptor axes are critical for the growth and progression of human prostatic carcinoma and pancreatic ductal adenocarcinoma xenografts in nude mice. Clin. Cancer Res. 8, 1924–1931 (2002).
Fenwick, S. W., Toogood, G. J., Lodge, J. P. & Hull, M. A. The effect of the selective cyclooxygenase-2 inhibitor rofecoxib on human colorectal cancer liver metastases. Gastroenterology 125, 716–729 (2003).
Gupta, K. et al. Morphine stimulates angiogenesis by activating proangiogenic and survival-promoting signaling and promotes breast tumor growth. Cancer Res. 62, 4491–4498 (2002). A paper showing that morphine promotes neovascularization when human breast cancer cells are injected subcutaneously in nude mice.
Singleton, P. A., Lingen, M. W., Fekete, M. J., Garcia, J. G. & Moss, J. Methylnaltrexone inhibits opiate and VEGF-induced angiogenesis: role of receptor transactivation. Microvasc. Res. 72, 3–11 (2006). A recent report suggesting that a peripherally restricted μ-opioid receptor antagonist can inhibit both opiate and VEGF-induced angiogenesis.
Smith, T. J. & Coyne, P. J. Implantable drug delivery systems (IDDS) after failure of comprehensive medical management (CMM) can palliate symptoms in the most refractory cancer pain patients. J. Palliat. Med. 8, 736–742 (2005).
Fields, H. State-dependent opioid control of pain. Nature Rev. Neurosci. 5, 565–575 (2004).
Acknowledgements
This work is supported by the National Institute of Neurological Disorders and Stroke, and a Veterans Administration Merit Review. The author would like to thank J. R. Ghilardi, K. G. Halvorson, J. M. Jimenez-Andrade and C. M. Peters for their invaluable comments and suggestions to this review.
Author information
Authors and Affiliations
Ethics declarations
Competing interests
The author declares no competing financial interests.
Glossary
- Neuropathy
-
Dysfunction of the cranial or spinal nerves.
- Nociceptor
-
A primary afferent sensory neuron that is activated by stimuli related to tissue damage. Nociceptors terminate in free nerve endings with peripheral terminals that are devoid of specialized cell types.
- Peripheral sensitization
-
An altered state of nociceptor function that is characterized by a lowered threshold of activation and an increased response to suprathreshold stimuli.
- Hyperalgesia
-
An increased response to a stimulus that is normally painful.
- Allodynia
-
Pain due to a stimulus that does not normally provoke pain.
- Myalgia
-
Aching of the muscles and joints.
- Paresthesia
-
An abnormal sensation such as burning, pricking or tingling that can be spontaneous or evoked.
- Dysesthesia
-
Impairment of sensation and/or a condition in which an unpleasant sensation is produced by ordinary stimuli.
- Central sensitization
-
Increased responsiveness to pain transmission by neurons in the spinal cord. This is usually caused by neurochemical changes in the spinal cord, brainstem or forebrain.
- Disease-free survival from cancer
-
Length of time after treatment during which no cancer is found.
- Sickness behaviour
-
Constellation of physiological and behavioural responses observed in animals after the administration of inflammatory agents or specific proinflammatory cytokines. These symptoms observed in animals are similar to those observed in cancer patients, and include pain, diarrhoea, nausea, cachexia, fatigue, anxiety and depression.
- Cold block
-
The interruption of spinal cord neuron action potential propagation that results from decreasing the temperature of the spinal cord by 7–10°C.
- Glove and stocking distribution
-
A pattern of sensory abnormalities that occurs with peripheral neuropathies in which the distal extremities (hands and feet) exhibit the most severe symptoms.
- Neuropathic pain
-
Pain initiated or caused by a primary lesion or dysfunction in the nervous system.
Rights and permissions
About this article
Cite this article
Mantyh, P. Cancer pain and its impact on diagnosis, survival and quality of life. Nat Rev Neurosci 7, 797–809 (2006). https://doi.org/10.1038/nrn1914
Issue Date:
DOI: https://doi.org/10.1038/nrn1914
This article is cited by
-
Kinin B1 and B2 receptors mediate cancer pain associated with both the tumor and oncology therapy using aromatase inhibitors
Scientific Reports (2023)
-
Cancer–nerve interplay in cancer progression and cancer-induced bone pain
Journal of Bone and Mineral Metabolism (2023)
-
The Effect of Exercise on Pain in People with Cancer: A Systematic Review with Meta-analysis
Sports Medicine (2023)
-
A Compound Mitigates Cancer Pain and Chemotherapy-Induced Neuropathic Pain by Dually Targeting nNOS-PSD-95 Interaction and GABAA Receptor
Neurotherapeutics (2021)