Key Points
-
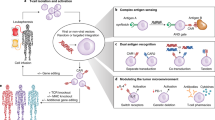
In principle, the goal of lymphocyte engineering is to pharmacologically enhance the function of the immune system, including specifying antigen recognition, improving lymphocyte survival, augmenting proliferative capacity, preventing apoptosis and/or inducing resistance to immune regulation.
-
Improved understanding of lymphocyte subsets has recently allowed adoptive transfer of CD4+ effector T cells, CD4+ regulatory T cells and CD8+ cytotoxic T cells. In addition to the previous clinical trials testing T cells expressing αβ T cell receptors, clinical protocols evaluating infusions of γδ T cells and invariant natural killer T cells have recently been completed.
-
For many years the only established method to engineer lymphocytes for clinical protocols used gammaretroviruses. Technological advances have produced lentiviral vectors and foamy virus vectors that have increased efficiency and potentially enhanced safety features, zinc-finger nucleases that allow site-specific modification and various other non-viral approaches such as transposons.
-
The most important questions currently facing the field are whether engineered lymphocytes are safe and, if so, under what conditions? Malignancies arising from retrovirally transduced haematopoietic stem cells have been reported in animal models and human gene therapy trials. Several hundred patients have been treated with engineered mature T cells for various indications including congenital immunodeficiency, cancer and AIDS following HIV infection. In contrast to stem cell engineering, to date there are no reported cases of transformation or leukaemia following engineered T cell transfer.
-
The first Phase III clinical study with engineered lymphocytes is currently testing whether allogeneic T cells can mediate immune reconstitution and antileukaemic effects and improve safety by triggering a conditional suicide gene comprised of herpes simplex virus thymidine kinase in the event of graft-versus-host disease.
Abstract
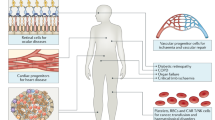
Cell-based therapies with various lymphocyte subsets hold promise for the treatment of several diseases, including cancer and disease resulting from inflammation and infection. The ability to genetically engineer lymphocyte subsets has the potential to improve the natural immune response and correct impaired immunity. In this Review we focus on the lymphocyte subsets that have been modified genetically or by other means for therapeutic benefit, on the technologies used to engineer lymphocytes and on the latest progress and hurdles in translating these technologies to the clinic.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Weiden, P. L. et al. Antileukemic effect of graft-versus-host disease in human recipients of allogeneic-marrow grafts. N. Engl. J. Med. 300, 1068–1073 (1979). This was the first study to indicate the potent antitumour effects of human T cells.
Rosenberg, S. A. et al. Gene transfer into humans — immunotherapy of patients with advanced melanoma, using tumor-infiltrating lymphocytes modified by retroviral gene transduction. N. Engl. J. Med. 323, 570–578 (1990). This was the first human gene transfer study.
Uchida, N., Cone, R. D., Freeman, G. J., Mulligan, R. C. & Cantor, H. High efficiency gene transfer into murine T cell clones using a retroviral vector. J. Immunol. 136, 1876–1879 (1986).
Naldini, L. et al. In vivo gene delivery and stable transduction of nondividing cells by a lentiviral vector. Science 272, 263–267 (1996).
Amado, R. G. & Chen, I. S. Lentiviral vectors — the promise of gene therapy within reach? Science 285, 674–676 (1999).
Ellis, J. Silencing and variegation of gammaretrovirus and lentivirus vectors. Hum. Gene Ther. 16, 1241–1246 (2005).
Wolf, D. & Goff, S. P. Host restriction factors blocking retroviral replication. Annu. Rev. Genet. 42, 143–163 (2008).
Russell, D. W. & Miller, A. D. Foamy virus vectors. J. Virol. 70, 217–222 (1996).
Beard, B. C. et al. Unique integration profiles in a canine model of long-term repopulating cells transduced with gammaretrovirus, lentivirus, or foamy virus. Hum. Gene Ther. 18, 423–434 (2007).
Rethwilm, A. Foamy virus vectors: an awaited alternative to gammaretro- and lentiviral vectors. Curr. Gene Ther. 7, 261–271 (2007).
Trobridge, G. D. et al. Foamy virus vector integration sites in normal human cells. Proc. Natl Acad. Sci. USA 103, 1498–1503 (2006).
Schroers, R. et al. Gene transfer into human T lymphocytes and natural killer cells by Ad5/F35 chimeric adenoviral vectors. Exp. Hematol. 32, 536–546 (2004).
Perez, E. E. et al. Establishment of HIV-1 resistance in CD4+ T cells by genome editing using zinc-finger nucleases. Nature Biotech. 26, 808–816 (2008). The first study to show that site-specific modification of cells can be accomplished at levels sufficient for therapeutic efficacy in an animal model.
Fratantoni, J. C., Dzekunov, S., Singh, V. & Liu, L. N. A non-viral gene delivery system designed for clinical use. Cytotherapy 5, 208–210 (2003).
Park, J. R. et al. Adoptive transfer of chimeric antigen receptor re-directed cytolytic T lymphocyte clones in patients with neuroblastoma. Mol. Ther. 15, 825–833 (2007).
Dupuy, A. J., Akagi, K., Largaespada, D. A., Copeland, N. G. & Jenkins, N. A. Mammalian mutagenesis using a highly mobile somatic Sleeping Beauty transposon system. Nature 436, 221–226 (2005).
Huang, X. et al. Stable gene transfer and expression in human primary T-cells by the Sleeping Beauty transposon system. Blood 107, 483–491 (2006).
Singh, H. et al. Redirecting specificity of T-cell populations for CD19 using the Sleeping Beauty system. Cancer Res. 68, 2961–2971 (2008). References 16, 17 and 18 show the potential of transposon-based systems to engineer lymphocyte functions.
Rossi, J. J., June C. H. & Kohn, D. B. Genetic therapies for HIV/AIDS. Nature Biotech. 25, 1444–1454 (2007).
Wang, G. P. et al. Analysis of lentiviral vector integration in HIV+ study subjects receiving autologous infusions of gene modified CD4+ T cells. Mol. Ther. 17, 844–850 (2009).
Bushman, F. D. Retroviral integration and human gene therapy. J. Clin. Invest. 117, 2083–2086 (2007).
Zhao, Y. et al. High-efficiency transfection of primary human and mouse T lymphocytes using RNA electroporation. Mol. Ther. 13, 151–159 (2006).
Yoon, S. H. et al. Adoptive immunotherapy using human peripheral blood lymphocytes transferred with RNA encoding Her-2/neu-specific chimeric immune receptor in ovarian cancer xenograft model. Cancer Gene Ther. 16, 489–497 (2008).
Mitchell, D. A. et al. Selective modification of antigen-specific T cells by RNA electroporation. Hum. Gene Ther. 19, 511–521 (2008).
Rowley, J., Monie, A., Hung., C. F. & Wu, T. C. Expression of IL-15RA or an IL-15/IL-15RA fusion on CD8+ T cells modifies adoptively transferred T-cell function in cis. Eur. J. Immunol. 39, 491–506 (2009).
Wilber, A. et al. Messenger RNA as a source of transposase for sleeping beauty transposon-mediated correction of hereditary tyrosinemia type I. Mol. Ther. 15, 1280–1287 (2007).
Wang, W. et al. Chromosomal transposition of PiggyBac in mouse embryonic stem cells. Proc. Natl Acad. Sci. USA 105, 9290–9295 (2008).
Li, Q. J. et al. miR-181a is an intrinsic modulator of T cell sensitivity and selection. Cell 129, 147–161 (2007). This study was the first to indicate the potential of engineering microRNA to alter T cell function.
Merkenschlager, M. & Wilson, C. B. RNAi and chromatin in T cell development and function. Curr. Opin. Immunol. 20, 131–138 (2008).
Su, Z. et al. Telomerase mRNA-transfected dendritic cells stimulate antigen-specific CD8+ and CD4+ T cell responses in patients with metastatic prostate cancer. J. Immunol. 174, 3798–3807 (2005).
Murphy, K. M. & Reiner, S. L. The lineage decisions of helper T cells. Nature Rev. Immunol. 2, 933–944 (2002).
Wilson, C. B., Rowell, E. & Sekimata, M. Epigenetic control of T-helper-cell differentiation. Nature Rev. Immunol. 9, 91–105 (2009).
Jones, P. A. & Taylor, S. M. Cellular differentiation, cytidine analogs and DNA methylation. Cell 20, 85–93 (1980).
Holliday, R. & Pugh, J. E. DNA modification mechanisms and gene activity during development. Science 187, 226–232 (1975).
Ballas, Z. K. The use of 5-azacytidine to establish constitutive interleukin 2-producing clones of the EL4 thymoma. J. Immunol. 133, 7–9 (1984). This was the first study to show that epigenetic modification could alter T cell function.
Polansky, J. K. et al. DNA methylation controls Foxp3 gene expression. Eur. J. Immunol. 38, 1654–1663 (2008).
Guo, Z. S. et al. De novo induction of a cancer/testis antigen by 5-aza-2′-deoxycytidine augments adoptive immunotherapy in a murine tumor model. Cancer Res. 66, 1105–1113 (2006).
Tao, R. et al. Deacetylase inhibition promotes the generation and function of regulatory T cells. Nature Med. 13, 1299–1307 (2007).
Bolden, J. E., Peart, M. J. & Johnstone, R. W. Anticancer activities of histone deacetylase inhibitors. Nature Rev. Drug Discov. 5, 769–784 (2006).
Murakami, T. et al. Transcriptional modulation using HDACi depsipeptide promotes immune cell-mediated tumor destruction of murine B16 melanoma. J. Invest. Dermatol. 128, 1506–1516 (2008).
Blackwell, L., Norris, J., Suto, C. M. & Janzen, W. P. The use of diversity profiling to characterize chemical modulators of the histone deacetylases. Life Sci. 82, 1050–1058 (2008).
Schwarze, S. R., Ho, A., Vocero-Akbani, A. & Dowdy, S. F. In vivo protein transduction: delivery of a biologically active protein into the mouse. Science 285, 1569–1572 (1999).
Eguchi, A. et al. Efficient siRNA delivery into primary cells by a peptide transduction domain-dsRNA binding domain fusion protein. Nature Biotech. 27, 567–571 (2009).
Tanaka, Y., Dowdy, S. F., Linehan, D. C., Eberlein, T. J. & Goedegebuure, P. S. Induction of antigen-specific CTL by recombinant HIV trans-activating fusion protein-pulsed human monocyte-derived dendritic cells. J. Immunol. 170, 1291–1298 (2003).
Grube, M., Melenhorst, J. J. & Barrett, A. J. An APC for every occasion: induction and expansion of human Ag-specific CD4 and CD8 T cells using cellular and non-cellular APC. Cytotherapy 6, 440–449 (2004).
Melenhorst, J. J. et al. Robust expansion of viral antigen-specific CD4+ and CD8+ T cells for adoptive T cell therapy using gene-modified activated T cells as antigen presenting cells. J. Immunother. 29, 436–443 (2006).
Choi, J. M. et al. Intranasal delivery of the cytoplasmic domain of CTLA-4 using a novel protein transduction domain prevents allergic inflammation. Nature Med. 12, 574–579 (2006).
Choi, J. M. et al. Transduction of the cytoplasmic domain of CTLA-4 inhibits TcR-specific activation signals and prevents collagen-induced arthritis. Proc. Natl Acad. Sci. USA 105, 19875–19880 (2008).
Bargou, R. et al. Tumor regression in cancer patients by very low doses of a T cell-engaging antibody. Science 321, 974–977 (2008).
Chen, A., Zheng, G. & Tykocinski, M. L. Hierarchical costimulator thresholds for distinct immune responses: application of a novel two-step Fc fusion protein transfer method. J. Immunol. 164, 705–711 (2000).
Montini, E. et al. Hematopoietic stem cell gene transfer in a tumor-prone mouse model uncovers low genotoxicity of lentiviral vector integration. Nature Biotech. 24, 687–696 (2006).
Montini, E. et al. The genotoxic potential of retroviral vectors is strongly modulated by vector design and integration site selection in a mouse model of HSC gene therapy. J. Clin. Invest. 119, 964–975 (2009). References 51 and 52 describe potential genotoxicity of gammaretroviral and lentiviral vectors expressed in HSCs in tumour-prone mouse models.
Ho, W. Y., Blattman, J. N., Dossett, M. L., Yee, C. & Greenberg, P. D. Adoptive immunotherapy: engineering T cell responses as biologic weapons for tumor mass destruction. Cancer Cell 3, 431–437 (2003).
Bluestone, J. A., Thomson, A. W., Shevach, E. M. & Weiner, H. L. What does the future hold for cell-based tolerogenic therapy? Nature Rev. Immunol. 7, 650–654 (2007).
Moisini, I., Nguyen, P., Fugger, L. & Geiger, T. L. Redirecting therapeutic T cells against myelin-specific T lymphocytes using a humanized myelin basic protein-HLA-DR2-ζ chimeric receptor. J. Immunol. 180, 3601–3611 (2008).
Muul, L. M. et al. Persistence and expression of the adenosine deaminase gene for 12 years and immune reaction to gene transfer components: long-term results of the first clinical gene therapy trial. Blood 101, 2563–2569 (2003).
Ciceri, F. et al. Infusion of suicide-gene-engineered donor lymphocytes after family haploidentical haemopoietic stem-cell transplantation for leukaemia (the TK007 trial): a non-randomised phase I-II study. Lancet Oncol. 10, 489–500 (2009).
Cooper, L. J., Kalos, M., Lewinsohn, D. A., Riddell, S. R. & Greenberg, P. D. Transfer of specificity for human immunodeficiency virus type 1 into primary human T lymphocytes by introduction of T-cell receptor genes. J. Virol. 74, 8207–8212 (2000).
Varela-Rohena, A. et al. Control of HIV-1 immune escape by CD8 T cells expressing enhanced T-cell receptor. Nature Med. 14, 1390–1395 (2008).
Johnson, L. A. et al. Gene therapy with human and mouse T cell receptors mediates cancer regression and targets normal tissues expressing cognate antigen. Blood 114, 535–546 (2009). References 58–60 show the potential efficacy and toxicity of adoptive therapy with transgenic TCRs.
Gross, G., Waks, T. & Eshhar, Z. Expression of immunoglobulin-T-cell receptor chimeric molecules as functional receptors with antibody-type specificity. Proc. Natl Acad. Sci. USA 86, 10024–10028 (1989). The first study to show the activity of chimeric antigen receptors in T cells.
Sadelain, M., Brentjens, R. & Riviere, I. The promise and potential pitfalls of chimeric antigen receptors. Curr. Opin. Immunol. 21, 215–223 (2009).
Pule, M. A. et al. Virus-specific T cells engineered to coexpress tumor-specific receptors: persistence and antitumor activity in individuals with neuroblastoma. Nature Med. 14, 1264–1270 (2008). This study describes the first antitumour effects following the adoptive transfer of T cells modified to express chimeric antigen receptors in humans.
Maher, J., Brentjens, R. J., Gunset, G., Riviere, I. & Sadelain, M. Human T-lymphocyte cytotoxicity and proliferation directed by a single chimeric TCR ζ/CD28 receptor. Nature Biotech. 20, 70–75 (2002).
Carpenito, C. et al. Control of large established tumor xenografts with genetically re-targeted human T cells containing CD28 and CD137 domains. Proc. Natl Acad. Sci. USA 106, 3360–3365 (2009).
Muranski, P. & Restifo, N. P. Adoptive immunotherapy of cancer using CD4+ T cells. Curr. Opin. Immunol. 21, 200–208 (2009).
Muranski, P. et al. Tumor-specific Th17-polarized cells eradicate large established melanoma. Blood 112, 362–373 (2008).
Riley, J. L., June, C. H. & Blazar, B. R. Human T regulatory cell therapy: take a billion and call me in the morning. Immunity 30, 656–665 (2009).
Mekala, D. J. & Geiger, T. L. Immunotherapy of autoimmune encephalomyelitis with redirected CD4+CD25+ T lymphocytes. Blood 105, 2090–2092 (2005).
Eran, E., Nitzan, A., Tova, W. & Eshhar, Z. Amelioration of colitis by genetically engineered murine regulatory T cells redirected by antigen-specific chimeric receptor. Gastroenterology 136, 1721–1731 (2009).
Landmeier, S. et al. Gene-engineered varicella-zoster virus reactive CD4+ cytotoxic T cells exert tumor-specific effector function. Cancer Res. 67, 8335–8343 (2007).
Zhou, J. et al. Telomere length of transferred lymphocytes correlates with in vivo persistence and tumor regression in melanoma patients receiving cell transfer therapy. J. Immunol. 175, 7046–7052 (2005).
Lanzavecchia, A. & Sallusto, F. Understanding the generation and function of memory T cell subsets. Curr. Opin. Immunol. 17, 326–332 (2005).
Seder, R. A., Darrah, P. A. & Roederer, M. T-cell quality in memory and protection: implications for vaccine design. Nature Rev. Immunol. 211, 58–66 (2008).
Berger, C. et al. Adoptive transfer of effector CD8+ T cells derived from central memory cells establishes persistent T cell memory in primates. J. Clin. Invest. 118, 294–305 (2008).
Levine, B. L. et al. Effects of CD28 costimulation on long term proliferation of CD4+ T cells in the absence of exogenous feeder cells. J. Immunol. 159, 5921–5930 (1997).
Maus, M. V. et al. Extensive replicative capacity of human central memory T cells. J. Immunol. 172, 6675–6683 (2004).
Bondanza, A. et al. Suicide gene therapy of graft-versus-host disease induced by central memory human T lymphocytes. Blood 107, 1828–1836 (2006).
Pulle, G., Vidric, M. & Watts, T. H. IL-15-dependent induction of 4-1BB promotes antigen-independent CD8 memory T cell survival. J. Immunol. 176, 2739–2748 (2006).
Zhang, H. et al. 4-1BB is superior to CD28 costimulation for generating CD8+ cytotoxic lymphocytes for adoptive immunotherapy. J. Immunol. 179, 4910–4918 (2007).
Zhu, Y., Zhu, G., Luo, L., Flies, A. S. & Chen, L. CD137 stimulation delivers an antigen-independent growth signal for T lymphocytes with memory phenotype. Blood 109, 4882–4889 (2007).
Zhang, Y., Joe, G., Hexner, E., Zhu, J. & Emerson, S. G. Host-reactive CD8+ memory stem cells in graft-versus-host disease. Nature Med. 11, 1299–1305 (2005).
Ferrarini, M., Ferrero, E., Dagna, L., Poggi, A. & Zocchi, M. R. Human γδ T cells: a nonredundant system in the immune-surveillance against cancer. Trends Immunol. 23, 14–18 (2002).
Lopez, R. D. Human γδ-T cells in adoptive immunotherapy of malignant and infectious diseases. Immunol. Res. 26, 207–221 (2002).
Inman, B. A. et al. Questionable relevance of γδ T lymphocytes in renal cell carcinoma. J. Immunol. 180, 3578–3584 (2008).
Thedrez, A. et al. Self/non-self discrimination by human γδ T cells: simple solutions for a complex issue? Immunol. Rev. 215, 123–135 (2007).
Todaro, M. et al. Efficient killing of human colon cancer stem cells by γδ T lymphocytes. J. Immunol. 182, 7287–7296 (2009).
Brandes, M., Willimann, K. & Moser, B. Professional antigen-presentation function by human γδ T cells. Science 309, 264–268 (2005).
Kondo, M. et al. Zoledronate facilitates large-scale ex vivo expansion of functional γδ T cells from cancer patients for use in adoptive immunotherapy. Cytotherapy 10, 842–856 (2008).
Thedrez, A. et al. IL-21-mediated potentiation of antitumor cytolytic and proinflammatory responses of human Vγ9Vδ2 T cells for adoptive immunotherapy. J. Immunol. 182, 3423–3431 (2009).
Kabelitz, D., Wesch, D., Pitters, E. & Zoller, M. Characterization of tumor reactivity of human Vγ9Vδ2 γδ T cells in vitro and in SCID mice in vivo. J. Immunol. 173, 6767–6776 (2004).
Kobayashi, H. et al. Safety profile and anti-tumor effects of adoptive immunotherapy using γδ T cells against advanced renal cell carcinoma: a pilot study. Cancer Immunol. Immunother. 56, 469–476 (2007).
Bennouna, J. et al. Phase-I study of Innacell γδ, an autologous cell-therapy product highly enriched in Vγ9Vδ2 T lymphocytes, in combination with IL-2, in patients with metastatic renal cell carcinoma. Cancer Immunol. Immunother. 57, 1599–1609 (2008).
Rischer, M. et al. Human γδ T cells as mediators of chimaeric-receptor redirected anti-tumour immunity. Br. J. Haematol. 126, 583–592 (2004).
van der Veeken, L. T. et al. αβ T-cell receptor engineered γδ T cells mediate effective antileukemic reactivity. Cancer Res. 66, 3331–3337 (2006).
Schumacher, T. N. M. & Restifo, N. P. Adoptive T cell therapy of cancer. Curr. Opin. Immunol. 21, 187–189 (2009).
Kronenberg, M. Toward an understanding of NKT cell biology: progress and paradoxes. Annu. Rev. Immunol. 23, 877–900 (2004).
Tahir, S. M. et al. Loss of IFN-γ production by invariant NK T cells in advanced cancer. J. Immunol. 167, 4046–4050 (2001).
Rogers, P. R. et al. Expansion of human Vα24+ NKT cells by repeated stimulation with KRN7000. J. Immunol. Methods 285, 197–214 (2004).
Motohashi, S. et al. A phase I study of in vitro expanded natural killer T cells in patients with advanced and recurrent non-small cell lung cancer. Clin. Cancer Res. 12, 6079–6086 (2006).
Kunii, N. et al. Combination therapy of in vitro-expanded natural killer T cells and α-galactosylceramide-pulsed antigen-presenting cells in patients with recurrent head and neck carcinoma. Cancer Sci. 100, 1092–1098 (2009).
Harrington, K. & Vile, R. Virus smuggling, tax evasion and tumor assassination. Nature Med. 12, 507–509 (2006).
Zakrzewski, J. L. et al. Adoptive transfer of T-cell precursors enhances T-cell reconstitution after allogeneic hematopoietic stem cell transplantation. Nature Med. 12, 1039–1047 (2006).
de Pooter, R. F., Cho, S. K., Carlyle, J. R. & Zúñiga-Pflücker, J. C. In vitro generation of T lymphocytes from embryonic stem cell-derived prehematopoietic progenitors. Blood 102, 1649–1653 (2003).
Yang, L. & Baltimore, D. Long-term in vivo provision of antigen-specific T cell immunity by programming hematopoietic stem cells. Proc. Natl Acad. Sci. USA 102, 4518–4523 (2005).
van Lent, A. U. et al. Functional human antigen-specific T cells produced in vitro using retroviral T cell receptor transfer into hematopoietic progenitors. J. Immunol. 179, 4959–4968 (2007).
Papapetrou, E. P., Kovalovsky, D., Beloeil, L., Sant'Angelo, D. & Sadelain, M. Harnessing endogenous miR-181a to segregate transgenic antigen receptor expression in developing versus post-thymic T cells in murine hematopoietic chimeras. J. Clin. Invest. 119, 157–168 (2009).
Kay, M. A. et al. In vivo gene therapy of hemophilia B: sustained partial correction in factor IX-deficient dogs. Science 262, 117–119 (1993).
Zufferey, R. et al. Self-inactivating lentivirus vector for safe and efficient in vivo gene delivery. J. Virol. 72, 9873–9880 (1998).
Yang, L., Bailey, L., Baltimore, D. & Wang, P. Targeting lentiviral vectors to specific cell types in vivo. Proc. Natl Acad. Sci. USA 103, 11479–11484 (2006).
June, C. H. Adoptive T cell therapy for cancer in the clinic. J. Clin. Invest. 117, 1466–1476 (2007).
Rapoport, A. P. et al. Rapid immune recovery and GVHD-like engraftment syndrome following adoptive transfer of costimulated autologous T cells. Clin. Cancer Res. 15, 4499–4507 (2009).
Morgan, R. A. et al. Cancer regression in patients after transfer of genetically engineered lymphocytes. Science 314, 126–129 (2006).
Lamers, C. H. et al. Treatment of metastatic renal cell carcinoma with autologous T-lymphocytes genetically retargeted against carbonic anhydrase IX: first clinical experience. J. Clin. Oncol. 24, e20–e22 (2006).
Lamers, C. H. et al. Gene-modified T cells for adoptive immunotherapy of renal cell cancer maintain transgene-specific immune functions in vivo. Cancer Immunol. Immunother. 56, 1875–1883 (2007).
Hsu, C. et al. Cytokine-independent growth and clonal expansion of a primary human CD8+ T-cell clone following retroviral transduction with the IL-15 gene. Blood 109, 5168–5177 (2007).
Schumacher, T. N. T-cell-receptor gene therapy. Nature Rev. Immunol. 2, 512–519 (2002).
Li, Y. et al. Directed evolution of human T-cell receptors with picomolar affinities by phage display. Nature Biotech. 23, 349–354 (2005).
Varmus, H. Retroviruses. Science 240, 1427–1435 (1988).
Baum, C., Kustikova, O., Modlich, U., Li, Z. & Fehse, B. Mutagenesis and oncogenesis by chromosomal insertion of gene transfer vectors. Hum. Gene Ther. 17, 253–263 (2006).
Faschinger, A. et al. Mouse mammary tumor virus integration site selection in human and mouse genomes. J. Virol. 82, 1360–1367 (2008).
Lewinski, M. K. et al. Genome-wide analysis of chromosomal features repressing human immunodeficiency virus transcription. J. Virol. 79, 6610–6619 (2005).
Friedmann, T. A brief history of gene therapy. Nature Genet. 2, 93–98 (1992).
Chang, A. H. & Sadelain, M. The genetic engineering of hematopoietic stem cells: the rise of lentiviral vectors, the conundrum of the LTR, and the promise of lineage-restricted vectors. Mol. Ther. 15, 445–456 (2007).
Hacein-Bey-Abina, S. et al. Insertional oncogenesis in 4 patients after retrovirus-mediated gene therapy of SCID-X1. J. Clin. Invest. 118, 3132–3142 (2008).
Heslop, H. E. et al. Long-term restoration of immunity against Epstein-Barr virus infection by adoptive transfer of gene-modified virus-specific T lymphocytes. Nature Med. 2, 551–555 (1996).
Deeks, S. et al. A phase II randomized study of HIV-specific T-cell gene therapy in subjects with undetectable plasma viremia on combination anti-retroviral therapy. Mol. Ther. 5, 788–797 (2002).
Newrzela, S. et al. Resistance of mature T cells to oncogene transformation. Blood 112, 2278–2286 (2008). This study compares the relative susceptibility of HSCs and T cells to genotoxicity after transduction with gammaretroviral vectors.
Min, B., Yamane, H., Hu-Li, J. & Paul, W. E. Spontaneous and homeostatic proliferation of CD4 T cells are regulated by different mechanisms. J. Immunol. 174, 6039–6044 (2005).
Goldman, D. P., Clarke, A. E. & Garber, A. M. Creating the costliest orphan. The Orphan Drug Act in the development of Ceredase. Int. J. Technol. Assess. Health Care. 8, 583–597 (1992).
Smiddy, W. E. Economic implications of current age-related macular degeneration treatments. Ophthalmology 116, 481–487 (2009).
Dedes, K. J. et al. Bevacizumab in combination with paclitaxel for HER-2 negative metastatic breast cancer: an economic evaluation. Eur. J. Cancer 45, 1397–1406 (2009).
Chamberlain, M. C. Bevacizumab plus irinotecan in recurrent glioblastoma. J. Clin. Oncol. 26, 1012–1013 (2008).
Capecchi, M. R. Altering the genome by homologous recombination. Science 244, 1288–1292 (1989).
Tan, S. et al. Zinc-finger protein-targeted gene regulation: genomewide single-gene specificity. Proc. Natl Acad. Sci. USA 100, 11997–12002 (2003).
Porteus, M. H. & Carroll, D. Gene targeting using zinc finger nucleases. Nature Biotech. 23, 967–973 (2005).
Santiago, Y. et al. Targeted gene knockout in mammalian cells by using engineered zinc-finger nucleases. Proc. Natl Acad. Sci. USA 105, 5809–5814 (2008).
Urnov, F. D. et al. Highly efficient endogenous human gene correction using designed zinc-finger nucleases. Nature 435, 646–651 (2005).
Dotti, G. et al. Human cytotoxic T lymphocytes with reduced sensitivity to Fas-induced apoptosis. Blood 105, 4677–4684 (2005).
Guttinger, M. et al. Adoptive immunotherapy by avidin-driven cytotoxic T lymphocyte-tumor bridging. Cancer Res. 60, 4211–4215 (2000).
Tykocinski, M. L., Chen, A., Huang, J. H., Weber, M. C. & Zheng, G. New designs for cancer vaccine and artificial veto cells: an emerging palette of protein paints. Immunol. Res. 27, 565–574 (2003).
Hacein-Bey-Abina, S. et al. LMO2-associated clonal T cell proliferation in two patients after gene therapy for SCID-X1. Science 302, 415–419 (2003).
Donahue, R. E. et al. Helper virus induced T cell lymphoma in nonhuman primates after retroviral mediated gene transfer. J. Exp. Med. 176, 1125–1135 (1992).
Levine, B. L. et al. Gene transfer in humans using a conditionally replicating lentiviral vector. Proc. Natl Acad. Sci. USA 103, 17372–17377 (2006).
Dropulic, B., Hermankova, M. & Pitha, P. M. A conditionally replicating HIV-1 vector interferes with wild-type HIV-1 replication and spread. Proc. Natl Acad. Sci. USA 93, 11103–11108 (1996). References 144 and 145 describe the development of the first lentiviral vector tested in humans, given as an adoptive transfer of engineered CD4+ T cells.
Matheson, R. I Am Legend. (Walker, New York, 1954).
Riddell, S. R. & Greenberg, P. D. The use of anti-CD3 and anti-CD28 monoclonal antibodies to clone and expand human antigen-specific T cells. J. Immunol. Methods 128, 189–201 (1990).
Oelke, M. et al. Ex vivo induction and expansion of antigen-specific cytotoxic T cells by HLA-Ig coated artificial antigen presenting cells. Nature Med. 9, 619–625 (2003).
Maus, M. V. et al. Ex vivo expansion of polyclonal and antigen-specific cytotoxic T lymphocytes by artificial APCs expressing ligands for the T cell receptor, CD28 and 4-1BB. Nature Biotech. 20, 143–148 (2002).
Exley, M. A. et al. Selective activation, expansion, and monitoring of human iNKT cells with a monoclonal antibody specific for the TCR α-chain CDR3 loop. Eur. J. Immunol. 38, 1756–1766 (2008).
Miller, A. D. & Rosman, G. J. Improved retroviral vectors for gene transfer and expression. Biotechniques 7, 980–990 (1989).
Dull, T. et al. A third-generation lentivirus vector with a conditional packaging system. J. Virol. 72, 8463–8471 (1998).
Switzer, W. M. et al. Frequent simian foamy virus infection in persons occupationally exposed to nonhuman primates. J. Virol. 78, 2780–2789 (2004).
Bauer, T. R. Jr et al. Successful treatment of canine leukocyte adhesion deficiency by foamy virus vectors. Nature Med. 14, 93–97 (2008).
Stevenson, S. C., Rollence, M., Marshall-Neff, J. & McClelland, A. Selective targeting of human cells by a chimeric adenovirus vector containing a modified fiber protein. J. Virol. 71, 4782–4790 (1997).
Takayama, K. et al. A mosaic adenovirus possessing serotype Ad5 and serotype Ad3 knobs exhibits expanded tropism. Virology 309, 282–293 (2003).
Stecher, H., Shayakhmetov, D. M., Stamatoyannopoulos, G. & Lieber, A. A capsid-modified adenovirus vector devoid of all viral genes: assessment of transduction and toxicity in human hematopoietic cells. Mol. Ther. 4, 36–44 (2001).
Mori, Y. Recent topics related to human herpesvirus 6 cell tropism. Cell. Microbiol. 11, 1001–1006 (2009).
Romi, H., Singer, O., Rapaport, D. & Frenkel, N. Tamplicon-7, a novel T-lymphotropic vector derived from human herpesvirus 7. J. Virol. 73, 7001–7007 (1999).
Borenstein, R., Singer, O., Moseri, A. & Frenkel, N. Use of amplicon-6 vectors derived from human herpesvirus 6 for efficient expression of membrane-associated and -secreted proteins in T cells. J. Virol. 78, 4730–4743 (2004).
Finney, H. M., Akbar, A. N. & Lawson, A. D. G. Activation of resting human primary T cells with chimeric receptors: costimulation from CD28, inducible costimulator, CD134, and CD137 in series with signals from the TCRζ chain. J. Immunol. 172, 104–113 (2004).
Till, B. G. et al. Adoptive immunotherapy for indolent non-Hodgkin lymphoma and mantle cell lymphoma using genetically modified autologous CD20-specific T cells. Blood 112, 2261–2271 (2008).
Acknowledgements
C.H.J. is grateful for support by the US National Institutes of Health (NIH) (grants 5R01CA105216, 1R01CA120409, 5P01CA066726 and 1U19AI082628) and the Alliance for Cancer Gene Therapy. B.R.B. acknowledges direct support of this work by the US NIH (grants 2R01HL56067, R01AI34495, R01CA72669, P01CA142106 and P01AI056299) as well as a Leukemia and Lymphoma Translational Research Award. J.L.R. receives support from the US NIH (grants P30AI045008, R01AI057838, R01CA113783, R41CA130547, U19AI066290, U19AI082628 and P01AI080192) as well as from the JDRF Center on Cord Blood Therapies for Type 1 Diabetes.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Carl H. June and James L. Riley receive research funding from Tmune Therapeutics, Inc. This is managed in compliance with the policies established at the University of Pennsylvania.
Supplementary information
Supplementary information S1 (figure)
Metabolic pathways that guide activation of human Vγ9Vδ2 T cells. (PDF 173 kb)
Related links
Related links
FURTHER INFORMATION
Clinicaltrials.gov identifier NCT00842634
Glossary
- Adoptive transfer
-
A form of immunotherapy in which effector lymphocytes are transfused. Allogeneic adoptive transfer is usually referred to as donor lymphocyte infusion and autologous lymphocyte adoptive transfer is referred to as adoptive transfer therapy.
- Therapeutic window
-
The range of concentrations of a drug, or numbers of immune cells, that will achieve therapeutic effects in most patients with adverse effects in only a small percentage. In cell-based therapies, the condition of the host and the dose and schedule of administration can alter the therapeutic window.
- Adeno-associated virus
-
(AAV). A replication-defective non-enveloped virus that is a member of the Parvovirus family. Vectors derived from AAV are useful because AAV does not cause disease and they can mediate long-term gene transfer in both dividing and non-dividing cells.
- Gammaretrovirus
-
A genus of the retroviridae family. Vectors using gammaretroviruses were the first integrating vectors to be used clinically. Most vectors are derived from endogenous retroviruses isolated from mice such as the murine leukaemia virus.
- Transposon
-
Mobile DNA elements that can relocate within the genome of their hosts. Transposons can be used for various applications, including insertional mutagenesis, gene identification, gene tagging and DNA sequencing.
- Chimeric antigen receptor
-
Also known as chimeric immune receptor. Non-MHC-restricted chimeric antigen receptors combine antigen specificity and T cell-activating properties in a single fusion molecule. Most chimeric antigen receptors use an antibody-derived antigen-binding motif to recognize surface-expressed targets, in contrast to T cell receptors, which usually recognize peptide antigens presented by MHC molecules.
- MicroRNAs
-
Single-stranded RNA molecules approximately 21–23 nucleotides in length that are thought to regulate the expression of other genes.
- Epigenetic marks
-
Chemical modifications of chromatin that retain an intact DNA sequence and can modify gene expression. Examples are methylation of cytosine residues and histone modification by acetylation.
- Regulatory T (TReg) cell
-
A specialized type of CD4+ T cell that can suppress the responses of other T cells. TReg cells provide a crucial mechanism for the maintenance of peripheral self tolerance and a subset of these cells is characterized by the expression of CD25 and FOXP3.
- Protein transduction domains
-
(PTDs). Peptides derived from several viruses, such as the HIV Tat PTD, that can enhance cellular uptake of proteins or polynucleotides. In general, the PTD must be covalently attached to the protein.
- Small interfering RNA
-
(siRNA). Synthetic RNA molecules of 19–23 nucleotides that are used to 'knock down' (that is, silence the expression of) a specific gene. This approach is known as RNA interference (RNAi) and is mediated by the sequence-specific degradation of mRNA.
- Insertional mutagenesis
-
Genotoxicity from DNA-based engineering that can result in cellular transformation through various mechanisms. DNA insertion can result in mutations that lead to the activation of oncogenes or to the inactivation of tumour suppressor genes.
- Zinc-finger nucleases
-
(ZFNs). Chimeric proteins comprised of engineered zinc-finger proteins fused to the catalytic domain of a restriction endonuclease that can bind and cleave DNA specifically at a unique and predetermined site in the human genome.
- Target product profile
-
A prospective and dynamic summary of the ideal characteristics of a drug or biological product to ensure that the desired quality, and hence the safety and efficacy, of a drug product is achieved. The target product profile forms the basis of design for the development of the product.
- T helper 17 (TH17) cells
-
A subset of CD4+ T helper cells that produce interleukin-17 (IL-17) and that are thought to be important in inflammatory and autoimmune diseases. Their generation involves IL-23 and IL-21, as well as the transcription factors RORγt (retinoic acid receptor-related orphan receptor-γt) and STAT3 (signal transducer and activator of transcription 3).
- Experimental autoimmune encephalomyelitis
-
An experimental model of multiple sclerosis that is induced by immunization of susceptible animals with myelin-derived antigens, such as myelin basic protein, proteolipid protein or myelin oligodendrocyte glycoprotein.
- Central memory T (TCM) cells
-
Antigen-experienced T cells that express cell surface receptors required for homing to secondary lymphoid organs. These cells are generally thought to be long-lived and can serve as the precursors to effector T cells for recall responses.
- Effector memory T (TEM) cells
-
Terminally differentiated T cells that lack lymph node-homing receptors but express receptors that enable them to home to inflamed tissues. TEM cells can exert immediate effector functions without the need for further differentiation.
- Vγ9Vδ2+ T cells
-
Vγ9Vδ2+ T cell receptors are expressed by γδ T cells. Vγ9Vδ2+ T cells are unique to humans and primates and are a minor fraction of the leukocyte population in peripheral blood (0.5–5%).
- SCID mouse
-
A naturally occurring mouse mutant with severe combined immune deficiency due to an inability to rearrange antigen receptor chain genes.
- Natural killer T (NKT) cells
-
A subpopulation of T cells that expresses both NK cell and T cell markers. In the C57BL/6 mouse strain, NKT cells express the NK1.1 (NKRP1C) molecule and the T cell receptor (TCR). Some NKT cells recognize CD1d-associated lipid antigens and express a restricted repertoire of TCRs. After TCR stimulation of naive mice, NKT cells rapidly produce interleukin-4 and interferon-γ.
- Replication-competent lentivirus
-
A lentivirus vector that produces infectious virions. Lentiviral vectors are designed to support only one infections cycle however mutations can induce replication competency.
Rights and permissions
About this article
Cite this article
June, C., Blazar, B. & Riley, J. Engineering lymphocyte subsets: tools, trials and tribulations. Nat Rev Immunol 9, 704–716 (2009). https://doi.org/10.1038/nri2635
Issue Date:
DOI: https://doi.org/10.1038/nri2635
This article is cited by
-
Chimeric antigen receptor-based natural killer cell immunotherapy in cancer: from bench to bedside
Cell Death & Disease (2024)
-
Chimeric antigen receptor-natural killer cells: a promising sword against insidious tumor cells
Human Cell (2023)
-
Chimeric antigen receptor natural killer (CAR-NK) cell design and engineering for cancer therapy
Journal of Hematology & Oncology (2021)
-
Efficient Editing of an Adenoviral Vector Genome with CRISPR/Cas9
Indian Journal of Microbiology (2021)
-
Photothermal nanofibres enable safe engineering of therapeutic cells
Nature Nanotechnology (2021)