Abstract
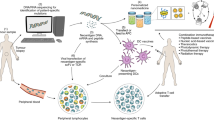
Clinical translation of cell therapies requires strategies that can manufacture cells efficiently and economically. One promising way to reproducibly expand T cells for cancer therapy is by attaching the stimuli for T cells onto artificial substrates with high surface area. Here, we show that a carbon nanotube–polymer composite can act as an artificial antigen-presenting cell to efficiently expand the number of T cells isolated from mice. We attach antigens onto bundled carbon nanotubes and combined this complex with polymer nanoparticles containing magnetite and the T-cell growth factor interleukin-2 (IL-2). The number of T cells obtained was comparable to clinical standards using a thousand-fold less soluble IL-2. T cells obtained from this expansion were able to delay tumour growth in a murine model for melanoma. Our results show that this composite is a useful platform for generating large numbers of cytotoxic T cells for cancer immunotherapy.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Change history
14 August 2014
In the version of this Article previously published, the name of the co-author Kevan C. Herold was spelt incorrectly. This has now been corrected in the online versions of the Article.
References
Waldmann, T. A. Immunotherapy: past, present and future. Nature Med. 9, 269–277 (2003).
Dudley, M. E. & Rosenberg, S. A. Adoptive-cell-transfer therapy for the treatment of patients with cancer. Nature Rev. Cancer 3, 666–675 (2003).
Zemon, H. An artificial solution for adoptive immunotherapy. Trends Biotechnol. 21, 418–420 (2003).
Brentjens, R. J. et al. CD19-targeted T cells rapidly induce molecular remissions in adults with chemotherapy-refractory acute lymphoblastic leukemia. Science Transl. Med. 5, 177ra38 (2013).
Robbins, P. F. et al. Tumor regression in patients with metastatic synovial cell sarcoma and melanoma using genetically engineered lymphocytes reactive with NY-ESO-1. J. Clin. Oncol. 29, 917–924 (2011).
Grupp, S. A. et al. Chimeric antigen receptor-modified T cells for acute lymphoid leukemia. N. Engl. J. Med. 368, 1509–1518 (2013).
Murphy, K., Travers, P. & Walport, M. Janeway's Immunobiology (Garland Science, 2008).
Kim, J. V., Latouche, J.-B., Rivière, I. & Sadelain, M. The ABCs of artificial antigen presentation. Nature Biotechnol. 22, 403–410 (2004).
Steenblock, E. R., Wrzesinski, S. H., Flavell, R. A. & Fahmy, T. M. Antigen presentation on artificial acellular substrates: modular systems for flexible, adaptable immunotherapy. Expert Opin. Biol. Ther. 9, 451–464 (2009).
Kropshofer, H. et al. Tetraspan microdomains distinct from lipid rafts enrich select peptide-MHC class II complexes. Nature Immunol. 3, 61–68 (2002).
Fooksman, D. R., Grönvall, G. K., Tang, Q. & Edidin, M. Clustering class I MHC modulates sensitivity of T cell recognition. J. Immunol. 176, 6673–6680 (2006).
Andersen, P. S., Menné, C., Mariuzza, R. A., Geisler, C. & Karjalainen, K. A response calculus for immobilized T cell receptor ligands. J. Biol. Chem. 276, 49125–49132 (2001).
González, P. A. et al. T cell receptor binding kinetics required for T cell activation depend on the density of cognate ligand on the antigen-presenting cell. Proc. Natl Acad. Sci. USA 102, 4824–4829 (2005).
Grakoui, A. et al. The immunological synapse: a molecular machine controlling T cell activation. Science 285, 221–227 (1999).
Monks, C. R., Freiberg, B. A., Kupfer, H., Sciaky, N. & Kupfer, A. Three-dimensional segregation of supramolecular activation clusters in T cells. Nature 395, 82–86 (1998).
Cemerski, S. et al. The stimulatory potency of T cell antigens is influenced by the formation of the immunological synapse. Immunity 26, 345–355 (2007).
Li, Q.-J. et al. CD4 enhances T cell sensitivity to antigen by coordinating Lck accumulation at the immunological synapse. Nature Immunol. 5, 791–799 (2004).
Oelke, M. et al. Ex vivo induction and expansion of antigen-specific cytotoxic T cells by HLA-Ig-coated artificial antigen-presenting cells. Nature Med. 9, 619–624 (2003).
Prakken, B. et al. Artificial antigen-presenting cells as a tool to exploit the immune 'synapse'. Nature Med. 6, 1406–1410 (2000).
Zitvogel, L. et al. Eradication of established murine tumors using a novel cell-free vaccine: dendritic cell derived exosomes. Nature Med. 4, 594–600 (1998).
Steenblock, E. R. & Fahmy, T. M. A comprehensive platform for ex vivo T-cell expansion based on biodegradable polymeric artificial antigen-presenting cells. Mol. Ther. 16, 765–772 (2008).
Oosten, L. E. M. et al. Artificial antigen-presenting constructs efficiently stimulate minor histocompatibility antigen-specific cytotoxic T lymphocytes. Blood 104, 224–226 (2004).
Sabatos, C. A. et al. A synaptic basis for paracrine interleukin-2 signaling during homotypic T cell interaction. Immunity 29, 238–248 (2008).
Huse, M., Quann, E. J. & Davis, M. M. Shouts, whispers and the kiss of death: directional secretion in T cells. Nature Immunol. 9, 1105–1111 (2008).
Ye, Q. et al. Engineered artificial antigen presenting cells facilitate direct and efficient expansion of tumor infiltrating lymphocytes. J. Transl. Med. 9, 131 (2011).
Malek, T. R. The biology of interleukin-2. Annu. Rev. Immunol. 26, 453–479 (2008).
Fadel, T. R. & Fahmy, T. M. Immunotherapy applications of carbon nanotubes: from design to safe applications. Trends Biotechnol. 32, 198–209 (2014).
Zanello, L. P., Zhao, B., Hu, H. & Haddon, R. C. Bone cell proliferation on carbon nanotubes. Nano Lett. 6, 562–567 (2006).
Nayak, T. R. et al. Thin films of functionalized multiwalled carbon nanotubes as suitable scaffold materials for stem cells proliferation and bone formation. ACS Nano 4, 7717–7725 (2010).
Steenblock, E. R., Fadel, T., Labowsky, M., Pober, J. S. & Fahmy, T. M. An artificial antigen-presenting cell with paracrine delivery of IL-2 impacts the magnitude and direction of the T cell response. J. Biol. Chem. 286, 34883–34892 (2011).
Chen, Y. et al. Low-defect, purified, narrowly (n,m)-dispersed single-walled carbon nanotubes grown from cobalt-incorporated MCM-41. ACS Nano 1, 327–336 (2007).
Fadel, T. R. et al. Enhanced cellular activation with single walled carbon nanotube bundles presenting antibody stimuli. Nano Lett. 8, 2070–2076 (2008).
Fadel, T. R. et al. Adsorption of multimeric T cell antigens on carbon nanotubes: effect on protein structure and antigen-specific T cell stimulation. Small 9, 666–672 (2013).
Hogquist, K. A. et al. T cell receptor antagonist peptides induce positive selection. Cell 76, 17–27 (1994).
Fadel, T. R. et al. Clustering of stimuli on single-walled carbon nanotube bundles enhances cellular activation. Langmuir 26, 5645–5654 (2010).
Park, J. et al. Enhancement of surface ligand display on PLGA nanoparticles with amphiphilic ligand conjugates. J. Control. Rel. 156, 109–115 (2011).
Fahmy, T. M., Samstein, R. M., Harness, C. C. & Mark Saltzman, W. Surface modification of biodegradable polyesters with fatty acid conjugates for improved drug targeting. Biomaterials 26, 5727–5736 (2005).
Ragheb, R. R. T. et al. Induced clustered nanoconfinement of superparamagnetic iron oxide in biodegradable nanoparticles enhances transverse relaxivity for targeted theranostics. Magn. Reson. Med. 70, 1748–1760 (2013).
Cheng, L. E., Ohlén, C., Nelson, B. H. & Greenberg, P. D. Enhanced signaling through the IL-2 receptor in CD8+ T cells regulated by antigen recognition results in preferential proliferation and expansion of responding CD8+ T cells rather than promotion of cell death. Proc. Natl Acad. Sci. USA 99, 3001–3006 (2002).
Labowsky, M. & Fahmy, T. M. Diffusive transfer between two intensely interacting cells with limited surface kinetics. Chem. Eng. Sci. 74, 114–123 (2012).
Janas, M. L., Groves, P., Kienzle, N. & Kelso, A. IL-2 regulates perforin and granzyme gene expression in CD8+ T cells independently of its effects on survival and proliferation. J. Immunol. 175, 8003–8010 (2005).
Rabinovich, G. A., Gabrilovich, D. & Sotomayor, E. M. Immunosuppressive strategies that are mediated by tumor cells. Annu. Rev. Immunol. 25, 267–296 (2007).
Pardoll, D. M. Spinning molecular immunology into successful immunotherapy. Nature Rev. Immunol. 2, 227–238 (2002).
Suter, D. M. & Krause, K-H. Neural commitment of embryonic stem cells: molecules, pathways and potential for cell therapy. J. Pathol. 215, 355–368 (2008).
McIntosh, K. et al. The immunogenicity of human adipose-derived cells: temporal changes in vitro. Stem Cells 24, 1246–1253 (2006).
Acknowledgements
This work was supported in part by a National Science Foundation Career Award (0747577) to T.M.F. and in part by a National Institutes of Health Autoimmunity Center of Excellence Pilot Award (U19 AI056363, to T.M.F. and K.H.) and a Yale Specialized Programs of Research Excellence (SPORE) Investigator Pilot Award (to T.M.F.) and in part by the Yale SPORE in Skin Cancer (grant no. 1 P50 CA121974). The authors thank J. Alderman and R. Flavell for helpful critique, and M. Sznol, R. Tigelaar and M. Bosenberg (Yale Cancer Center), as well as P. De Sousa (University of Edinburgh), for technical comments regarding adoptive therapy. The authors also thank P. Van Tassel for technical advice regarding CNT preparation.
Author information
Authors and Affiliations
Contributions
T.R.F. and T.M.F. designed all of the experiments for this study. R.R synthesized the magnetite and fabricated the polymer nanoparticles. N.L. synthesized the carbon nanotubes. S.J. synthesized the biotinylated MHC-I. T.R.F., L.D.P. and G.L.H. characterized the carbon nanotubes. T.R.F. and R.R. characterized the particles and the CNP system. R.R. characterized the magnetic properties of the PLGA nanoparticles and CNPs. T.R.F. performed inverted, fluorescence and FRET imaging. T.R.F. performed in vitro characterization experiments and FACS analyses. T.R.F., F.S. and E.H. performed the studies on T-cell cytotoxicity. T.R.F., F.S. and D.K. characterized the tumour-infiltrating lymphocytes. F.S., N.V., and J.G. performed the human T cell expansion experiments. T.R.F. and D.K. performed the in vivo experiments. T.M.F. conceived the formulations. T.R.F. wrote the manuscript. T.M.F., R.R., D.K., F.S., E.H., L.D.P., and K.C.H. edited the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary information
Supplementary Information (PDF 9764 kb)
Rights and permissions
About this article
Cite this article
Fadel, T., Sharp, F., Vudattu, N. et al. A carbon nanotube–polymer composite for T-cell therapy. Nature Nanotech 9, 639–647 (2014). https://doi.org/10.1038/nnano.2014.154
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nnano.2014.154
This article is cited by
-
Optimizing the manufacturing and antitumour response of CAR T therapy
Nature Reviews Bioengineering (2023)
-
Multimodal targeting of glioma with functionalized nanoparticles
Cancer Cell International (2022)
-
Nanoparticle-based modulation of CD4+ T cell effector and helper functions enhances adoptive immunotherapy
Nature Communications (2022)
-
Insights on functionalized carbon nanotubes for cancer theranostics
Journal of Nanobiotechnology (2021)
-
Considerations for designing preclinical cancer immune nanomedicine studies
Nature Nanotechnology (2021)