Abstract
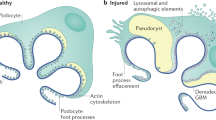
Focal segmental glomerulosclerosis (FSGS), a subtype of 'idiopathic nephrotic syndrome', is not a single disease, but a lesion that initially affects the glomerulus followed by the tubulointerstitium and renal vessels. The term 'FSGS' does not accurately encompass the various pathologic features of the glomerulus, which are not always focal, segmental or sclerotic. Particular variants of FSGS, such as collapsing glomerulopathy and the glomerular tip lesion, exemplify the nosologic uncertainty inherent in the classification of glomerular lesions. Pathologic variation notwithstanding, all pathologic processes that affect the podocyte lead to one of the histologic subtypes of FSGS. This specialized cell type has essential roles in maintaining the integrity of glomerular architecture, resisting endocapillary hydraulic pressure and hindering egress of proteins into the urinary space. Once initiated, podocyte lesions and ensuing fibrosis are usually irreversible, at least in human forms of FSGS. Remarkable progress has been made in unraveling the mechanisms of podocyte dysregulation that accompany the cellular variants of FSGS and in identifying genetic mutations affecting proteins of the slit diaphragm. Hopefully, this progress will drastically improve treatments for what is one of the most difficult therapeutic challenges to confront the nephrologist.
Key Points
-
The diverse histologic subtypes of focal segmental glomerulosclerosis (FSGS) are unified by the central pathophysiological role of the podocyte
-
Nuclear dysregulation, derangement of the cell cycle and morphologic changes are features of podocytes in FSGS
-
Podocyte dysregulation perturbs glomerular architecture leading to the primary clinical feature of FSGS—proteinuria
-
Evidence supports a central role for an elusive 'glomerular permeability factor' in pathogenesis of FSGS
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Pavenstädt H et al. (2003) Cell biology of the glomerular podocyte. Physiol Rev 83: 253–307
Meyrier A and Niaudet P (2005) Minimal changes and focal-segmental glomerulosclerosis. In: Oxford Textbook of Clinical Nephrology, 439–469, edn 3 (Eds AM Davison et al.) (vol 1). Oxford: Oxford University Press
Kerjaschki D (2001) Caught flat-footed: podocyte damage and the molecular bases of focal glomerulosclerosis. J Clin Invest 108: 1583–1587
Kriz W and Le Hir M (2005) Pathways to nephron loss starting from glomerular diseases—insights from animal models. Kidney Int 67: 404–419
Bertani T et al. (1982) Adriamycin-induced nephrotic syndrome in rats: sequence of pathologic events. Lab Invest 46: 16–23
Korbet SM et al. (1988) Recurrent nephrotic syndrome in renal allografts. Am J Kidney Dis 11: 270–276
Meyrier A (2003) E pluribus unum: the riddle of focal-segmental glomerulosclerosis. Semin Nephrol 23: 135–140
Fogo A et al. (1995) Is focal segmental glomerulosclerosis really focal? Distribution of lesions in adults and children. Kidney Int 47: 1690–1696
Fuiano G et al. (1996) Serial morphometric analysis of sclerotic lesions in primary „focal” segmental glomerulosclerosis. J Am Soc Nephrol 7: 49–55
Erkan E et al. (2005) Induction of renal tubular cell apoptosis in focal segmental glomerulosclerosis: roles of proteinuria and Fas-dependent pathways. J Am Soc Nephrol 16: 398–407
D'Agati VD et al. (2004) Pathologic classification of focal segmental glomerulosclerosis: a working proposal. Am J Kidney Dis 43: 368–382
Schwartz MM et al. (1999) Focal segmental glomerulosclerosis: prognostic implications of the cellular lesion. J Am Soc Nephrol. 10: 1900–1907
Chun MJ et al. (2004) Focal segmental glomerulosclerosis in nephrotic adults: presentation, prognosis, and response to therapy of the histologic variants. J Am Soc Nephrol 8: 2169–2177
Korbet SM (2002) Treatment of primary focal segmental glomerulosclerosis. Kidney Int 62: 2301–2310
D'Agati V (2003) Pathologic classification of focal segmental glomerulosclerosis. Semin Nephrol 23: 117–134
D'Agati V (2005) Glomérulopathies avec „collapsus” du flocculus. In Actualités Néphrologiques Jean Hamburger Hôpital Necker 9–25 (Eds P Lesavre et al.) Paris: Médecine-Sciences Flammarion
Schwartz MM and Lewis EJ (1985) Focal segmental glomerular sclerosis. The cellular lesion. Kidney Int 28: 968–974
Haas M et al. (1995) Increasing incidence of focal-segmental glomerulosclerosis among adult nephropathies. Am J Kidney Dis 26: 740–750
Valeri A et al. (1996) Idiopathic collapsing focal segmental glomerulosclerosis. Kidney Int 50: 1734–1746
Braden GL et al. (2000) Changing incidence of glomerular diseases in adults. Am J Kidney Dis 35: 878–883
Filler G et al. (2003) Is there really an increase in non-minimal change nephrotic syndrome in children? Am J Kidney Dis 42: 1107–1113
Barri YM et al. (2004) Podocyte injury associated glomerulopathies induced by pamidronate. Kidney Int 65: 634–641
Herman ES and Klotman PE (2003) HIV-associated nephropathy: Epidemiology, pathogenesis and treatment. Semin Nephrol 23: 200–208
Tanawattanachaoren S et al. (2000) Parvovirus B 19 DNA in kidney tissue of patients with focal segmental glomerulosclerosis. Am J Kidney Dis 35: 1166–1174
Moudgil A et al. (2001) Association of parvovirus B 19 infection with idiopathic collapsing glomerulopathy. Kidney Int 59: 2126–2133
Li RM et al. (2002) Molecular identification of SV40 infection in human subjects and possible association with kidney disease. J Am Soc Nephrol 13: 2320–2330
Tomlinson L et al. (2003) Acute cytomegalovirus infection complicated by collapsing glomerulopathy. Nephrol Dial Transplant 18:187–189
Meyrier A (2004) Nephrotic focal segmental glomerulosclerosis in 2004: an update. Nephrol Dial Transplant 10: 2437–2444
Greenberg A et al. (1997) Focal segmental glomerulosclerosis associated with nephrotic syndrome in cholesterol atheroembolism: clinicopathological correlations. Am J Kidney Dis 29: 334–344
Thadani R et al. (1996) Preliminary description of focal segmental glomerulosclerosis in patients with renovascular disease. Lancet 347: 231–233
Stokes MB et al. (1999) Collapsing glomerulopathy in renal allografts: a morphologic pattern with diverse clinicopathologic associations. Am J Kidney Dis 33: 658–666
Meehan SM et al. (1998) De novo collapsing glomerulopathy in renal allografts Transplantation 65: 1192–1197
Nadasdy T et al. (2002) Zonal distribution of glomerular collapse in renal allografts: Possible role of vascular changes. Hum Pathol 33: 437–441
Howie AJ et al. (2005) Evolution of nephrotic-associated focal segmental glomerulosclerosis and relation to the glomerular tip lesion. Kidney Int 67: 987–1001
Stokes MB et al. (2004) Glomerular tip lesion: a distinct entity within the minimal change disease/focal segmental glomerulosclerosis spectrum. Kidney Int 65: 1690–1702
Haas M (2005) The glomerular tip lesion: what does it really mean? Kidney Int 67: 1188–1189
Shalhoub RJ (1974) Pathogenesis of lipoid nephrosis: a disorder of T cell function. Lancet 2: 556–559
Brenchley PEC (2003) Vascular permeability factors in steroid-sensitive nephrotic syndrome and focal segmental glomerulosclerosis. Nephrol Dial Transpl 18 (Suppl 6): vi21–vi25
Lagrue G et al. (1991) Transmission d'un syndrome néphrotique à deux nouveaux nés: régression spontanée. La Presse Médicale 20: 255–257
Kemper MJ et al. (2001) Transmission of glomerular permeability factor from a mother to her child. N Engl J Med 344: 386–387
Zimmerman SW (1984) Increased urinary protein excretion in the rat produced by serum from a patient with recurrent focal glomerular sclerosis after renal transplantation. Clin Nephrol 22: 32–38
Dantal J et al. (1994) Effect of plasma protein adsorption on protein excretion in kidney-transplant recipients with recurrent nephrotic syndrome. N Engl J Med 330: 7–14
Le Berre L et al. (2000) Effect of plasma fractions from patients with focal and segmental glomerulosclerosis on rat proteinuria. Kidney Int 58: 2502–2511
Savin VJ et al. (1996) Circulating factor associated with increased glomerular permeability to albumin in recurrent focal segmental sclerosis. N Engl J Med 334: 878–882
Esnault VL et al. (1999) Effect of protein A immunoadsorption in nephrotic syndrome of various etiologies. J Am Soc Nephrol 10: 2014–2017
Kraft SW et al. (2004) Glomerular podocytopathy in patients with systemic lupus erythematosus. J Am Soc Nephrol 16: 175–179
Coward RJ et al. (2005) Nephrotic plasma alters slit diaphragm dependent signaling and translocates nephrin, podocin and CD2 associated protein in cultured human podocytes. J Am Soc Nephrol 16: 629–637
McCarthy ET et al. (2004) Sera from patients with collapsing focal segmental glomerulosclerosis increase albumin permeability of isolated glomeruli. J Lab Clin Med 143: 225–229
Ghiggeri GM et al. (2001) Permeability plasma factors in nephrotic syndrome: more than one factor, more than one inhibitor. Nephrol Dial Transplant 16: 882–885
Deen WM (2004) What determines glomerular capillary permeability? J Clin Invest 114: 1412–1414
Hara M et al. (2001) Urinary podocytes in primary focal segmental glomerulosclerosis. Nephron 89: 342–347
Hara M et al. (2005) Apical cell membranes are shed into urine from injured podocytes: a novel phenomenon of podocyte injury. J Am Soc Nephrol 16: 408–416
Bariety J et al. (1998) Podocytes undergo phenotypic changes and express macrophagic-associated markers in idiopathic collapsing glomerulopathy. Kidney Int 53: 918–928
Barisoni L et al. (1999) The dysregulated podocyte phenotype: a novel concept in the pathogenesis of collapsing idiopathic focal segmental glomerulosclerosis and HIV-associated nephropathy. J Am Soc Nephrol 10: 51–61
Bariety J et al. (2001) Post-transplantation relapse of FSGS is characterized by glomerular epithelial cell transdifferentiation. J Am Soc Nephrol 12: 261–274
Nagata M et al. (1998) Cell cycle regulation and differentiation in the human podocyte lineage. Am J Pathol 153: 1511–1520
Shankland SJ et al. (2000) Differential expression of cyclin-dependent kinase inhibitors in human glomerular disease: role in podocyte proliferation and maturation. Kidney Int 58: 674–683
Conlon PJ et al. (1999) Spectrum of disease in familial focal and segmental glomerulosclerosis. Kidney Int 56: 1863–1871
Winn MP (2003) Approach to the evaluation of heritable diseases and update on familial focal segmental glomerulosclerosis. Nephrol Dial Transplant 18 (Suppl 6): vi14–vi20
Benzing T (2004) Signaling at the slit diaphragm. J Am Soc Nephrol 15: 1382–1391
Patrakka J et al. (2000) Congenital nephrotic syndrome (NPHS1): features resulting from different mutations in Finnish patients. Kidney Int 58: 972–980
Fuchshuber A et al. (1996) Congenital nephrotic syndrome of the Finnish type: linkage to the locus in non-Finnish population. Pediatr Nephrol 10: 135–138
Boute N et al. (2000) NPHS2, encoding the glomerular protein podocin, is mutated in autosomal recessive steroid-resistant nephrotic syndrome. Nat Genet 24: 349–354
Caridi G et al. (2003) Broadening the spectrum of diseases related to podocin mutations. J Am Soc Nephrol 14: 1278–1286
Niaudet P (2004) Podocin and nephrotic syndrome: implications for the clinician. J Am Soc Nephrol 15: 832–834
Huber TB et al. (2003) Molecular basis of the functional podocin–nephrin complex: mutations in the NPHS2 gene disrupt nephrin targeting to lipid raft microdomains. Hum Mol Genet 12: 3397–3405
Schultheiss M et al. (2004) No evidence for genotype/phenotype correlation in NPHS1 and NPHS2 mutations. Pediatr Nephrol 19: 1340–1348
Tsukagushi H et al. (2002) NPHS2 mutations in late-onset focal segmental glomerulosclerosis: R229Q is a common disease allele. J Clin Invest 110: 1659–1666
Kaplan JM et al. (2000) Mutations in ACTN4, encoding α-actinin-4, cause familial focal segmental glomerulosclerosis. Nat Med 24: 251–256
Kim JM et al. (2003) CD2-associated protein haploinsufficiency is linked to glomerular disease susceptibility. Science 300: 1298–1300
Scharnhorst V et al. (2001) WT1 proteins: functions in growth and differentiation Gene 273: 141–161
Gubler MC (2002) WT1, a multiform protein. Contribution of genetic models to the understanding of its various functions. J Am Soc Nephrol 13: 2192–2194
Wagner N et al. (2004) The major podocyte protein nephrin is transcriptionally activated by the Wilm's tumor suppressor WT1. J Am Soc Nephrol 15: 3044–3051
McTaggart SJ et al. (2001) Clinical spectrum of Denys–Drash and Frasier syndrome. Pediatr Nephrol 16: 335–339
Little S et al. (2005) A WT1 exon 1 mutation in a child diagnosed with Denys–Drash syndrome. Pediatr Nephrol 20: 81–85
Yang Y et al. (1999) WT1 and PAX-2 podocyte expression in Denys–Drash syndrome and isolated diffuse mesangial sclerosis. Am J Pathol 154: 181–192
Scott DA et al. (2005) Congenital diaphragmatic hernia in WAGR syndrome. Am J Med Genet 134: 430–433
Orloff MS et al. (2005) Variants in the Wilms' tumor gene are associated with focal segmental glomerulosclerosis in the African American population. Physiol Genomics 21: 212–221
Guéry B et al. (2003) The spectrum of systemic involvement in adults presenting with renal lesions and mitochondrial tRNA (Leu) mutation. J Am Soc Nephrol 14: 2099–2108
Boerkel CF et al. (2002) Mutant chromatin remodeling protein SMARCAL1 causes Schimke immuno-osseous dysplasia. Nat Genet 30: 215–220
Acknowledgements
I am greatly indebted to Jean Bariéty MD, Professor Emeritus, Paris-Descartes University, for kindly providing the histopathologic images and critically reviewing the text.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The author declares no competing financial interests.
Rights and permissions
About this article
Cite this article
Meyrier, A. Mechanisms of Disease: focal segmental glomerulosclerosis. Nat Rev Nephrol 1, 44–54 (2005). https://doi.org/10.1038/ncpneph0025
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/ncpneph0025
This article is cited by
-
Genotype–phenotype correlations and nephroprotective effects of RAAS inhibition in patients with autosomal recessive Alport syndrome
Pediatric Nephrology (2021)
-
Focal segmental glomerulosclerosis with heterozygous apolipoprotein E5 (Glu3Lys)
CEN Case Reports (2018)
-
Endothelin and endothelin antagonists in chronic kidney disease
Kidney International (2014)
-
A study of interobserver reproducibility of morphologic lesions of focal segmental glomerulosclerosis
Virchows Archiv (2013)
-
A spectrum of morphologic lesions of focal segmental glomerulosclerosis by Columbia criteria in human immunodeficiency virus infection
Virchows Archiv (2012)