Abstract
Background/Objectives:
Optimal nutritional status is important in children with cancer, as it can influence clinical outcomes. To improve the nutritional health of children and adolescents receiving treatment for cancer residing in low income and middle-income countries (LMIC), we investigated nutrition practices among these nations’ institutions providing treatment for childhood cancer.
Subject/Methods:
A cross-sectional survey of nutrition practice was administered to staff members at institutions providing treatment for children with cancer between 2011 and 2012. Countries classified as low income and middle income were divided by geographical region. Final analysis was performed with 96 surveys, which included 27 institutions from Asia, 27 institutions from Latin America and Caribbean, 27 institutions from Africa and 15 institutions from Europe.
Results:
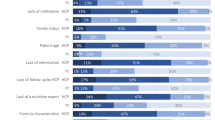
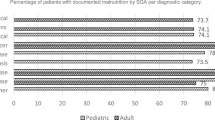
The study found that 55% of institutions had a dietician available on their service. Access to dieticians, lack of nutrition resources and lack of nutrition education of staff were the main barriers to providing nutrition care in LMIC. Half of the institutions performed nutritional assessment at diagnosis, and the methods used varied widely. Twenty-nine percent of all institutions used complementary and alternate therapies within their clinical practice, and 35% of institutions reported that nutrition education was provided to patients and families.
Conclusions:
Priority areas for improving the nutritional management in LMIC include the following: (1) improved nutrition education and assessment tools for doctors and nurses; (2) increased availability of nutrition education resources for families and patients; and (3) identification of the role of complementary and alternative therapies in closing gaps in symptom management in these institutions.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Ferlay J Shin HR Bray F Forman D Mathers C Parkin DM . GLOBOCAN 2008 v2.0-Cancer Incidence and Mortality Worldwide: IARC Cancer0. Base No 1. International Agency for Research on Cancer: Lyon, France, 2010.
Kellie SJ, Howard SC . Global child health priorities: what role for paediatric oncologists? Eur J Cancer 2008; 44: 2388–2396.
Magrath I, Steliarova-Foucher E, Epelman S, Ribeiro RC, Harif M, Li CK et al. Paediatric cancer in low-income and middle-income countries. Lancet Oncol 2013; 14: e104–e116.
Israëls T, van de Wetering MD, Hesseling P, van Geloven N, Caron HN, Molyneux EM . Malnutrition and neutropenia in children treated for Burkitt lymphoma in Malawi. Pediatr Blood Cancer 2009; 53: 47–52.
White M, Murphy AJ, Hallahan A, Ware RS, Fraser C, Davies PS . Survival in overweight and underweight children undergoing hematopoietic stem cell transplantation. Eur J Clin Nutr 2012; 66: 1120–1123.
Begum M, Jahan S, Tawfique M, Mannan MA . Out come of induction of remission in undernourished children with acute lymphoblastic leukaemia. Mymensingh Med J 2012; 21: 691–695.
Antillon F, Rossi E, Molina AL, Sala A, Pencharz P, Valsecchi MG et al. Nutritional status of children during treatment for acute lymphoblastic leukemia in Guatemala. Pediatr Blood Cancer 2013; 60: 911–915.
Sala A, Rossi E, Antillon F, Molina AL, de Maselli T, Bonilla M et al. Nutritional status at diagnosis is related to clinical outcomes in children and adolescents with cancer: a perspective from Central America. Eur J Cancer 2012; 48: 243–252.
Ladas ED, Sacks N, Brophy P, Rogers PC . Standards of nutritional care in pediatric oncology. Pediatr Blood Cancer 2006; 46: 339–344.
Selwood K, Ward E, Gibson F . Assessment and management of nutritional challenges in children’s cancer care: a survey of current practice in the United Kingdom. Eur J Oncol Nurs 2010; 14: 439–446.
Israëls T, Renner L, Hendricks M, Hesseling P, Howard S, Molyneux E et al. SIOP PODC: recommendations for supportive care of children with cancer in a low-income setting. Pediatr Blood Cancer 2013; 60: 899–904.
Ladas EJ, Mosby TT, Murphy AJ, Cohen J, Barr R, Rogers P . Meeting report: development of an International Committee on Nutrition & Health for Children with Cancer. Pediatr Blood Cancer 2012; 58: 1008–1009.
World Bank Country and Lending Groups Washington 2012. The World Bank. 2013. Available from http://data.worldbank.org/about/country-classifications/country-and-lending-groups.
United Nations Statistics Division. Composition of macro geographical (continental) regions, geographical sub-regions, and selected economic and other groupings. 2013. Available from http://unstats.un.org/unsd/methods/m49/m49regin.htm.
Mosby TT, Day S, Challinor J, Hernandez A, Garcia J, Velasquez S . Nutritional issues in pediatric oncology: an international collaboration between the American Nurses Cooperative and US-based dietary and nursing experts. Pediatr Blood Cancer 2008; 50: 1298–1300.
Israëls T, Chirambo C, Caron HN, Molyneux EM . Nutritional status at admission of children with cancer in Malawi. Pediatr Blood Cancer 2008; 51: 626–628.
World Health Organization United Nations Children’s Fund. WHO child growth standards and the identification of severe acute malnutrition in infants and children 2009.
de Onis M, Onyango AW, Borghi E, Siyam A, Nishida C, Siekmann J . Development of a WHO growth reference for school-aged children and adolescents. Bull World Health Org 2007; 85: 660–667.
Barr R, Collins L, Nayiager T, Doring N, Kennedy C, Halton J et al. Nutritional status at diagnosis in children with cancer. 2. An assessment by arm anthropometry. J Pediatr Hematol Oncol 2011; 33: e101–e104.
Murphy AJ, White M, Davies PS . The validity of simple methods to detect poor nutritional status in paediatric oncology patients. Br J Nutr 2009; 101: 1388–1392.
Kelly KM . Bringing evidence to complementary and alternative medicine in children with cancer: focus on nutrition-related therapies. Pediatr Blood Cancer 2008; 50: 490–493.
Ladas EJ, Rivas S, Ndao D, Damoulakis D, Bao YY, Cheng B et al. Use of traditional and complementary/alternative medicine (TCAM) in children with cancer in Guatemala. Pediatr Blood Cancer 2014; 61: 687–692.
Acknowledgements
We recognize the following agencies that supported the presented research: Queensland Children’s Medical Research Institute (AJM); The Tamarind Foundation, New York, NY (EJL); American Lebanese Syrian Associated Charities (TTM). We thank the Cure4kids management for distributing the survey through Cure4kids website. We also thank all participating sites for their time in completing the survey. The authors also recognize the International Pediatric Oncology Nutrition Group.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Murphy, A., Mosby, T., Rogers, P. et al. An international survey of nutritional practices in low- and middle-income countries: a report from the International Society of Pediatric Oncology (SIOP) PODC Nutrition Working Group. Eur J Clin Nutr 68, 1341–1345 (2014). https://doi.org/10.1038/ejcn.2014.122
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2014.122
This article is cited by
-
Health facility-based counselling and community outreach are associated with maternal dietary practices in a cross-sectional study from Tanzania
BMC Nutrition (2021)
-
The Impact of Fellowship in Dietetics on Clinical Practice
Journal of Cancer Education (2019)