Abstract
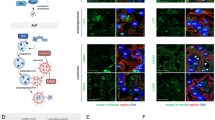
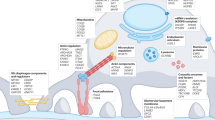
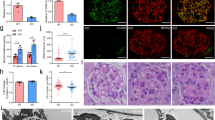
Podocyte dysfunction, represented by foot process effacement and proteinuria, is often the starting point for progressive kidney disease. Therapies aimed at the cellular level of the disease are currently not available. Here we show that induction of urokinase receptor (uPAR) signaling in podocytes leads to foot process effacement and urinary protein loss via a mechanism that includes lipid-dependent activation of αvβ3 integrin. Mice lacking uPAR (Plaur−/−) are protected from lipopolysaccharide (LPS)-mediated proteinuria but develop disease after expression of a constitutively active β3 integrin. Gene transfer studies reveal a prerequisite for uPAR expression in podocytes, but not in endothelial cells, for the development of LPS-mediated proteinuria. Mechanistically, uPAR is required to activate αvβ3 integrin in podocytes, promoting cell motility and activation of the small GTPases Cdc42 and Rac1. Blockade of αvβ3 integrin reduces podocyte motility in vitro and lowers proteinuria in mice. Our findings show a physiological role for uPAR signaling in the regulation of kidney permeability.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Zandi-Nejad, K., Eddy, A.A., Glassock, R.J. & Brenner, B.M. Why is proteinuria an ominous biomarker of progressive kidney disease? Kidney Int. Suppl. 66, S76–S89 (2004).
Kerjaschki, D. et al. A β1-integrin receptor for fibronectin in human kidney glomeruli. Am. J. Pathol. 134, 481–489 (1989).
Kreidberg, J.A. et al. α3β1 integrin has a crucial role in kidney and lung organogenesis. Development 122, 3537–3547 (1996).
Regele, H.M. et al. Glomerular expression of dystroglycans is reduced in minimal change nephrosis but not in focal segmental glomerulosclerosis. J. Am. Soc. Nephrol. 11, 403–412 (2000).
Reiser, J., Kriz, W., Kretzler, M. & Mundel, P. The glomerular slit diaphragm is a modified adherens junction. J. Am. Soc. Nephrol. 11, 1–8 (2000).
Faul, C., Asanuma, K., Yanagida-Asanuma, E., Kim, K. & Mundel, P. Actin up: regulation of podocyte structure and function by components of the actin cytoskeleton. Trends Cell Biol. 17, 428–437 (2007).
Tryggvason, K., Patrakka, J. & Wartiovaara, J. Hereditary proteinuria syndromes and mechanisms of proteinuria. N. Engl. J. Med. 354, 1387–1401 (2006).
Sever, S. et al. Proteolytic processing of dynamin by cytoplasmic cathepsin L is a mechanism for proteinuric kidney disease. J. Clin. Invest. 117, 2095–2104 (2007).
Reiser, J. et al. Induction of B7-1 in podocytes is associated with nephrotic syndrome. J. Clin. Invest. 113, 1390–1397 (2004).
Reiser, J. et al. Podocyte migration during nephrotic syndrome requires a coordinated interplay between cathepsin L and α3 integrin. J. Biol. Chem. 279, 34827–34832 (2004).
Asanuma, K. et al. Synaptopodin orchestrates actin organization and cell motility via regulation of RhoA signalling. Nat. Cell Biol. 8, 485–491 (2006).
Moeller, M.J. et al. Podocytes populate cellular crescents in a murine model of inflammatory glomerulonephritis. J. Am. Soc. Nephrol. 15, 61–67 (2004).
Seiler, M.W., Venkatachalam, M.A. & Cotran, R.S. Glomerular epithelium: structural alterations induced by polycations. Science 189, 390–393 (1975).
Van Den Berg, J.G., Van Den Bergh Weerman, M.A., Assmann, K.J.M., Weening, J.J. & Florquin, S. Podocyte foot process effacement is not correlated with the level of proteinuria in human glomerulopathies. Kidney Int. 66, 1901–1906 (2004).
Gadea, G., de Toledo, M., Anguille, C. & Roux, P. Loss of p53 promotes RhoA-ROCK–dependent cell migration and invasion in 3D matrices. J. Cell Biol. 178, 23–30 (2007).
Wei, Y. et al. Regulation of integrin function by the urokinase receptor. Science 273, 1551–1555 (1996).
Blasi, F. & Carmeliet, P. uPAR: a versatile signalling orchestrator. Nat. Rev. Mol. Cell Biol. 3, 932–943 (2002).
Alfano, M., Sidenius, N., Panzeri, B., Blasi, F. & Poli, G. Urokinase-urokinase receptor interaction mediates an inhibitory signal for HIV-1 replication. Proc. Natl. Acad. Sci. USA 99, 8862–8867 (2002).
Wei, Y. et al. Identification of the urokinase receptor as an adhesion receptor for vitronectin. J. Biol. Chem. 269, 32380–32388 (1994).
Madsen, C.D., Ferraris, G.M., Andolfo, A., Cunningham, O. & Sidenius, N. uPAR-induced cell adhesion and migration: vitronectin provides the key. J. Cell Biol. 177, 927–939 (2007).
Dewerchin, M. et al. Generation and characterization of urokinase receptor–deficient mice. J. Clin. Invest. 97, 870–878 (1996).
Carmeliet, P. et al. Biological effects of disruption of the tissue-type plasminogen activator, urokinase-type plasminogen activator, and plasminogen activator inhibitor-1 genes in mice. Ann. NY Acad. Sci. 748, 367–382 (1995).
Zheng, X., Saunders, T.L., Camper, S.A., Samuelson, L.C. & Ginsburg, D. Vitronectin is not essential for normal mammalian development and fertility. Proc. Natl. Acad. Sci. USA 92, 12426–12430 (1995).
Hodivala-Dilke, K.M. β3-integrin–deficient mice are a model for Glanzmann thrombasthenia showing placental defects and reduced survival. J. Clin. Invest. 103, 229–238 (1999).
Simons, K. & Toomre, D. Lipid rafts and signal transduction. Nat. Rev. Mol. Cell Biol. 1, 31–39 (2000).
Schmid, H. et al. Validation of endogenous controls for gene expression analysis in microdissected human renal biopsies. Kidney Int. 64, 356–360 (2003).
Nakamura, T., Ebihara, I., Shirato, I., Tomino, Y. & Koide, H. Modulation of basement membrane component gene expression in glomeruli of aminonucleoside nephrosis. Lab. Invest. 64, 640–647 (1991).
Kelley, V.E. & Cavallo, T. An ultrastructural study of the glomerular slit diaphragm in New Zealand black/white mice. Lab. Invest. 35, 213–220 (1976).
Mundel, P. et al. Synaptopodin: an actin-associated protein in telencephalic dendrites and renal podocytes. J. Cell Biol. 139, 193–204 (1997).
Shankland, S.J., Pippin, J.W., Reiser, J. & Mundel, P. Podocytes in culture: past, present, and future. Kidney Int. 72, 26–36 (2007).
Mauer, S.M. et al. Effects of kidney and pancreas transplantation on streptozotocin-induced malignant kidney tumors in rats. Cancer Res. 34, 1643–1645 (1974).
Mayer, G., Boileau, G. & Bendayan, M. Furin interacts with proMT1-MMP and integrin αv at specialized domains of renal cell plasma membrane. J. Cell Sci. 116, 1763–1773 (2003).
Moeller, M.J., Sanden, S.K., Soofi, A., Wiggins, R.C. & Holzman, L.B. Podocyte-specific expression of cre recombinase in transgenic mice. Genesis 35, 39–42 (2003).
Velasco, B. et al. Vascular gene transfer driven by endoglin and ICAM-2 endothelial-specific promoters. Gene Ther. 8, 897–904 (2001).
Zeisberg, E.M. et al. Endothelial-to-mesenchymal transition contributes to cardiac fibrosis. Nat. Med. 13, 952–961 (2007).
Arnaout, M.A., Mahalingam, B. & Xiong, J.P. Integrin structure, allostery, and bidirectional signaling. Annu. Rev. Cell Dev. Biol. 21, 381–410 (2005).
Chaurasia, P. et al. A region in urokinase plasminogen receptor domain III controlling a functional association with α5β1 integrin and tumor growth. J. Biol. Chem. 281, 14852–14863 (2006).
Wei, Y. et al. Urokinase receptors are required for α5β1 integrin–mediated signaling in tumor cells. J. Biol. Chem. 282, 3929–3939 (2007).
Degryse, B., Resnati, M., Czekay, R.P., Loskutoff, D.J. & Blasi, F. Domain 2 of the urokinase receptor contains an integrin-interacting epitope with intrinsic signaling activity: generation of a new integrin inhibitor. J. Biol. Chem. 280, 24792–24803 (2005).
Pelletier, A.J., Kunicki, T. & Quaranta, V. Activation of the integrin αvβ3 involves a discrete cation-binding site that regulates conformation. J. Biol. Chem. 271, 1364–1370 (1996).
Honda, S. et al. Topography of ligand-induced binding sites, including a novel cation-sensitive epitope (AP5) at the amino terminus, of the human integrin β3 subunit. J. Biol. Chem. 270, 11947–11954 (1995).
Dormond, O., Foletti, A., Paroz, C. & Ruegg, C. NSAIDs inhibit αvβ3 integrin–mediated and Cdc42/Rac-dependent endothelial-cell spreading, migration and angiogenesis. Nat. Med. 7, 1041–1047 (2001).
Cai, W. & Chen, X. Anti-angiogenic cancer therapy based on integrin αvβ3 antagonism. Anticancer Agents Med. Chem. 6, 407–428 (2006).
Schwarz, K. et al. Podocin, a raft-associated component of the glomerular slit diaphragm, interacts with CD2AP and nephrin. J. Clin. Invest. 108, 1621–1629 (2001).
Keller, P. & Simons, K. Cholesterol is required for surface transport of influenza virus hemagglutinin. J. Cell Biol. 140, 1357–1367 (1998).
Butta, N. et al. Disruption of the β3 663–687 disulfide bridge confers constitutive activity to beta3 integrins. Blood 102, 2491–2497 (2003).
Pampori, N. et al. Mechanisms and consequences of affinity modulation of integrin αvβ3 detected with a novel patch-engineered monovalent ligand. J. Biol. Chem. 274, 21609–21616 (1999).
Hughes, P.E. et al. Breaking the integrin hinge. A defined structural constraint regulates integrin signaling. J. Biol. Chem. 271, 6571–6574 (1996).
de Jong, P.E. & Brenner, B.M. From secondary to primary prevention of progressive renal disease: the case for screening for albuminuria. Kidney Int. 66, 2109–2118 (2004).
Silberman, S., Janulis, M. & Schultz, R.M. Characterization of downstream Ras signals that induce alternative protease-development invasive phenotypes. J. Biol. Chem. 272, 5927–5935 (1997).
Gugliucci, A. & Bendayan, M. Reaction of advanced glycation endproducts with renal tissue from normal and streptozotocin-induced diabetic rats: an ultrastructural study using colloidal gold cytochemistry. J. Histochem. Cytochem. 43, 591–600 (1995).
Acknowledgements
Antibody to WOW-1 fragment (Fab) was a gift from S. Shattil (University of California, San Diego, La Jolla, California). Rabbit polyclonal antibody and NPHS2 promoter vector p2.5 cDNA were gifts from L. Holzman (University of Michigan). Vtn−/− mice were a gift from D. Ginsburg (University of Michigan) and Itgb3−/− mice were obtained from R. Kalluri (Beth Israel Deaconess Medical Center, Harvard Medical School, Boston). PLAURD262A 37 cDNA was a gift from Y. Wei and H.A. Chapman (University of California, San Francisco). J.R. was supported by the KMD Foundation and the Kidney-Urology Foundation of America–American Society of Nephrology (KUFA-ASN) Research. This work was supported by US National Institutes of Health (NIH) grants DK073495 (to J.R.), DK057683, DK062472 and the George M. O'Brien Kidney Center DK064236 (to P.M.). C.W. is the Halpin Scholar of the American Society of Nephrology. C.C.M. was supported by a scholarship of the German Academic Exchange Service. M.M.A. was supported by NIH training grant T32DK007540. Gene expression studies of uPAR in human disease were performed in the framework of the European renal cDNA bank. We thank all members of the European Renal cDNA Bank and their patients for their support (for participating centers at the time of the study, see ref. 26). Part of the electron microscopy work was performed in the Microscopy Core facility of the Massachusetts General Hospital Program in Membrane Biology and was supported by an NIH Program Project grant (DK38452).
Author information
Authors and Affiliations
Corresponding author
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–4, Supplementary Table 1 and Figure Legends (PDF 3660 kb)
Rights and permissions
About this article
Cite this article
Wei, C., Möller, C., Altintas, M. et al. Modification of kidney barrier function by the urokinase receptor. Nat Med 14, 55–63 (2008). https://doi.org/10.1038/nm1696
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm1696
This article is cited by
-
Predictive value of suPAR in AKI: a systematic review and meta-analysis
Clinical and Experimental Nephrology (2023)
-
Urokinase-type plasminogen activator receptor (uPAR) as a therapeutic target in cancer
Journal of Translational Medicine (2022)
-
Soluble urokinase plasminogen activator receptor (suPAR) and glomerular disease in children: a narrative review
Egyptian Pediatric Association Gazette (2022)
-
Upregulation of OASIS/CREB3L1 in podocytes contributes to the disturbance of kidney homeostasis
Communications Biology (2022)
-
Anti-ANGPTL3-FLD monoclonal antibody treatment ameliorates podocyte lesions through attenuating mitochondrial damage
Cell Death & Disease (2022)