Abstract
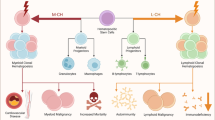
Childhood histiocytoses comprise two main diseases, Langerhans cell histiocytosis (LCH) and hemophagocytic lymphohistiocytosis (HLH). LCH is a rare disorder with obscure pathogenesis. Data on clonality suggested neoplastic origin, yet were not convincing. Dysregulation of cytokines and of DC trafficking and cross-talk are documented. Clinical manifestations and course are highly variable, ranging from self-healing solitary bone lesion to disseminated, multi-organ involvement with 20% fatality rate despite standard chemotherapy. HSCT has been applied in less than 50 cases, outside any trial, with good disease control but elevated early toxicity. The familial form of HLH (FHL) has been recognized as congenital immune deficiency, with mutations of PRF1, Munc13-4, syntaxin11 genes resulting in defective cellular cytotoxicity machinery. Chemo-immunotherapy allows temporary disease control, but HSCT holds as the only procedure with potential for cure. Rapid identification of genetic defects allows differential diagnosis from transient, virus-associated HLH, thus indicating early HSCT. The role of HSCT in childhood histiocytoses is thus very important. Better understanding of the pathogenesis, in particular of genetic and immune function defects, will help to tailor indications and, possibly less toxic, conditioning regimens, reducing treatment-related mortality, and thus disclosing the way to final cure.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Favara BE, Feller AC, Pauli M, Jaffe ES, Weiss LM, Arico M et al. Contemporary classification of histiocytic disorders. The WHO Committee on Histiocytic/Reticulum Cell Proliferations. Reclassification Working Group of the Histiocyte Society. Med Pediatr Oncol 1997; 29: 157–166.
Carstensen H, Ornvold K . The epidemiology of Langerhans cell histiocytosis in children in Denmark, 1975–1989. Med Pediatr Oncol 1993; 21: 387–388.
Arico M, Egeler RM . Clinical aspects of Langerhans cell histiocytosis. Hematol Oncol Clin North Am 1998; 12: 247–258.
Nezelof C, Basset F . An hypothesis Langerhans cell histiocytosis: the failure of the immune system to switch from an innate to an adaptive mode. Pediatr Blood Cancer 2004; 42: 398–400.
Beverley PC, Egeler RM, Arceci RJ, Pritchard J . The Nikolas symposia and histiocytosis. Nat Rev Cancer 2005; 5: 488–494.
Annels NE, da Costa CET, Prins FA, Willemze A, Hogendoorn PCW, Egeler RM . Aberrant chemokine receptor expression and chemokine production by Langerhans cells underlies the pathogenesis of Langerhans cell histiocytosis. J Exp Med 2003; 197: 1385–1390.
De Filippi P, Badulli C, Cuccia M, De Silvestri A, Dametto E, Pasi A et al. Specific polymorphisms of cytokine genes are associated with different risks to develop single-system or multi-system childhood Langerhans cell histiocytosis. Br J Haematol 2006; 132: 784–787.
Arico M, Nichols K, Whitlock JA, Arceci R, Haupt R, Mittler U et al. Familial clustering of Langerhans cell histiocytosis. Br J Haematol 1999; 107: 883–888.
Gadner H, Grois N, Arico M, Broadbent V, Ceci A, Jakobson A et al. Histiocyte Society. A randomized trial of treatment for multisystem Langerhans’ cell histiocytosis. J Pediatr 2001; 138: 728–734.
Gadner H, Grois N, Pötschger U, Minkov M, Aricò M, Braier J et al., for the Histiocyte Society. Improved outcome in multisystem Langerhans cell histiocytosis is associated with therapy intensification. Blood 2008; 111: 2556–2562.
Ringden O, Ahstrom L, Lonnqvist B, Baryd I, Svedmyr E, Gahrton G . Allogeneic bone marrow transplantation in a patient with chemotherapy-resistant progressive histiocytosis. N Engl J Med 1987; 316: 733–735.
Steiner M, Matthes-Martin S, Attarbaschi A, Minkov M, Grois N, Unger E et al. Improved outcome of treatment-resistant high-risk Langerhans cell histiocytosis after allogeneic stem cell transplantation with reduced-intensity conditioning. Bone Marrow Transplant 2005; 36: 215–225.
Farquhar J, Claireaux A . Familial haemophagocytic reticulosis. Arch Dis Child 1952; 27: 519–525.
Aricò M, Janka G, Fischer A, Henter JI, Blanche S, Elinder G et al. Hemophagocytic lymphohistiocytosis. Report of 122 children from the International Registry. FHL Study Group of the Histiocyte Society. Leukemia 1996; 10: 197–203.
Janka GE . Familial hemophagocytic lymphohistiocytosis. Eur J Pediatr 1983; 140: 221–230.
Aricò M, Allen M, Brusa S, Clementi R, Pende D, Maccario R et al. Haemophagocytic lymphohistiocytosis: proposal of a diagnostic algorithm based on perforin expression. Br J Haematol 2002; 119: 180–188.
Henter JI, Horne A, Arico M, Egeler RM, Filipovich AH, Imashuku S et al. HLH-2004: diagnostic and therapeutic guidelines for hemophagocytic lymphohistiocytosis. Pediatr Blood Cancer 2007; 48: 124–131.
Perez N, Virelizier JL, Arenzana-Seisdedos F, Fischer A, Griscelli C . Impaired natural killer activity in lymphohistiocytosis syndrome. J Pediatr 1984; 104: 569–573.
Arico M, Nespoli L, Maccario R, Montagna D, Bonetti F, Caselli D et al. Natural cytotoxicity impairment in familial haemophagocytic lymphohistiocytosis. Arch Dis Child 1988; 63: 292–296.
Stepp SE, Dufourcq-Lagelouse R, Le Deist F, Bhawan S, Certain S, Mathew PA et al. Perforin gene defects in familial hemophagocytic lymphohistiocytosis. Science 1999; 286: 1957–1959.
Feldmann J, Callebaut I, Raposo G, Certain S, Bacq D, Dumont C et al. Munc13-4 is essential for cytolytic granules fusion and is mutated in a form of familial hemophagocytic lymphohistiocytosis (FHL3). Cell 2003; 115: 461–473.
Santoro A, Cannella S, Bossi G, Gallo F, Trizzino A, Pende D et al. Novel Munc13-4 mutations in children and young adult patients with haemophagocytic lymphohistiocytosis. J Med Genet 2006; 43: 953–960.
zur Stadt U, Schmidt S, Kasper B, Beutel K, Diler AS, Henter JI et al. Linkage of familial hemophagocytic lymphohistiocytosis (FHL) type-4 to chromosome 6q24 and identification of mutations in syntaxin 11. Hum Mol Genet 2005; 14: 827–834.
Henter JI, Samuelsson-Horne A, Aricò M, Egeler RM, Elinder G, Filipovich AH et al. Histocyte Society. Treatment of hemophagocytic lymphohistiocytosis with HLH-94 immunochemotherapy and bone marrow transplantation. Blood 2002; 100: 2367–2373.
Janka GE, Schneider EM . Modern management of children with haemophagocytic lymphohistiocytosis. Br J Haematol 2004; 124: 4–14.
Jabado N, de Graeff-Meeder ER, Cavazzana-Calvo M, Haddad E, Le Deist F, Benkerrou M et al. Treatment of familial hemophagocytic lymphohistiocytosis with bone marrow transplantation from HLA genetically nonidentical donors. Blood 1997; 90: 4743–4748.
Durken M, Horstmann M, Bieling P, Erttmann R, Kabisch H, Loliger C et al. Improved outcome in haemophagocytic lymphohistiocytosis after bone marrow transplantation from related and unrelated donors: a single-centre experience of 12 patients. Br J Haematol 1999; 106: 1052–1058.
Horne A, Janka G, Egeler MR, Gadner H, Imashuku S, Ladisch S et al. Histiocyte Society. Haematopoietic stem cell transplantation in haemophagocytic lymphohistiocytosis. Br J Haematol 2005; 129: 622–630.
Cesaro S, Rondelli R, Porta F, Uderzo C, Lanino E, Pession A et al. Allogeneic haematopoietic stem cell transplantation in patients with haemophagocytic lymphohistiocytosis: a retrospective analysis of the Italian group for Paediatric Blood and Marrow Transplantation (AIEOP). Bone Marrow Transplant 2007; 39 (S1): S13.
Radhi M, Rumelhart S, Tatman D, Goldman F . Severe autoimmune hemolytic anemia after unrelated umbilical cord blood transplant for familial hemophagocytic lymphohistiocytosis: significant improvement after treatment with rituximab. J Pediatr Hematol Oncol 2007; 29: 125–127.
Mizumoto H, Hata D, Yamamoto K, Shirakawa R, Kumakura A, Shiota M et al. Familial hemophagocytic lymphohistiocytosis with the MUNC13-4 mutation: a case report. Eur J Pediatr 2006; 165: 384–388.
Imashuku S, Kohdera U, Teramura T, Ueda I, Morimoto A, Naya M et al. Sensorineural hearing loss in a case of familial hemophagocytic lymphohistiocytosis. Pediatr Blood Cancer 2007; 49: 856–858.
Kuroiwa Y, Suzuki N, Mizue N, Hori T, Endo T, Yoshida Y et al. Gastric antral vascular ectasia in 2-yr-old girl undergoing unrelated cord blood stem cell transplantation. Pediatr Transplant 2005; 9: 788–791.
Astigarraga I, Prats JM, Navajas A, Fernandez-Teijeiro A, Urberuaga A . Near fatal cerebellar swelling in familial hemophagocytic lymphohistiocytosis. Pediatr Neurol 2004; 30: 361–364.
Imashuku S, Teramura T, Tauchi H, Ishida Y, Otoh Y, Sawada M et al. Longitudinal follow-up of patients with Epstein–Barr virus-associated hemophagocytic lymphohistiocytosis. Haematologica 2004; 89: 183–188.
Imai C, Kakihara T, Iwabuchi H, Tanaka A, Furukawa T, Uchiyama M . Glomerular vasculopathy after unrelated cord blood transplantation. Pediatr Nephrol 2003; 18: 399–402.
Minegishi M, Ohashi Y, Kumaki S, Sasahara Y, Hayashi T, Asada H et al. Successful umbilical cord blood transplantation from an unrelated donor for a patient with Epstein–Barr virus-associated hemophagocytic lymphohistiocytosis. Bone Marrow Transplant 2001; 27: 883–886.
Tanaka Y, Hosoi G, Ishii T, Shimoyama T, Fujimura Y, Sako M . Successful engraftment of unrelated cord blood stem cells for familial erythrophagocytic lymphohistiocytosis. Kinki Cord Blood Bank. Bone Marrow Transplant 1998; 22: 511–513.
Schwinger W, Urban C, Lackner H, Benesch M, Kerbl R, Dornbusch HJ et al. Unrelated 5/6-locus matched umbilical cord blood transplantation in a 23-month-old child with hemophagocytic lymphohistiocytosis. Bone Marrow Transplant 1998; 22: 393–396.
Arico M, Danesino C, Pende D, Moretta L . Pathogenesis of haemophagocytic lymphohistiocytosis. Br J Haematol 2001; 114: 761–769.
Janka GE . Familial and acquired hemophagocytic lymphohistiocytosis. Eur J Pediatr 2007; 166: 95–109.
Arico M, Imashuku S, Clementi R, Hibi S, Teramura T, Danesino C et al. Hemophagocytic lymphohistiocytosis due to germline mutations in SH2D1A, the X-linked lymphoproliferative disease gene. Blood 2001; 15: 1131–1133.
Scappaticci S, Danesino C, Rossi E, Klersy C, Fiori GM, Clementi R et al. Cytogenetic abnormalities in PHA-stimulated lymphocytes from patients with Langerhans cell histocytosis. AIEOP–Istiocitosi Group. Br J Haematol 2000; 111: 258–262.
Coury F, Annels N, Rivollier A, Olsson S, Santoro A, Speziani C et al. Langerhans cell histiocytosis reveals a new IL-17A-dependent pathway of dendritic cell fusion. Nat Med 2008; 14: 81–87.
Ringdén O, Ahström L, Lönnqvist B, Båryd I, Svedmyr E, Gahrton G . Allogeneic bone marrow transplantation in a patient with chemotherapy-resistant progressive histiocytosis X. N Engl J Med 1987; 316: 733–735.
Stoll M, Freund M, Schmid H, Deicher H, Riehm H, Poliwoda H et al. Allogeneic bone marrow transplantation for Langerhans’ cell histiocytosis. Cancer 1990; 66: 284–288.
Greinix HT, Storb R, Sanders JE, Petersen FB . Marrow transplantation for treatment of multisystem progressive Langerhans cell histiocytosis. Bone Marrow Transplant 1992; 10: 39–44.
Conter V, Reciputo A, Arrigo C, Bozzato N, Sala A, Aricò M . Bone marrow transplantation for refractory Langerhans’ cell histiocytosis. Haematologica 1996; 81: 468–471.
Frost JD, Wiersma SR . Progressive Langerhans cell histiocytosis in an infant with Klinefelter syndrome successfully treated with allogeneic bone marrow transplantation. J Pediatr Hematol Oncol 1996; 18: 396–400.
Kinugawa N, Imashuku S, Hirota Y, Yamada K, Yamamoto A, Akazai A et al. Hematopoietic stem cell transplantation (HSCT) for Langerhans cell histiocytosis (LCH) in Japan. Bone Marrow Transplant 1999; 24: 935–938.
Akkari V, Donadieu J, Piguet C, Bordigoni P, Michel G, Blanche S et al., French Langerhans Cell Study Group. Hematopoietic stem cell transplantation in patients with severe Langerhans cell histiocytosis and hematological dysfunction: experience of the French Langerhans Cell Study Group. Bone Marrow Transplant 2003; 31: 1097–1103.
Ingram W, Desai SR, Gibbs JS, Mufti G . Reduced-intensity conditioned allogeneic haematopoietic transplantation in an adult with Langerhans’ cell histiocytosis and thrombocytopenia with absent radii. Bone Marrow Transplant 2006; 37: 713–715.
Author information
Authors and Affiliations
Consortia
Corresponding author
Additional information
Conflict of interest
Neither of the authors declared any financial interests.
Rights and permissions
About this article
Cite this article
Caselli, D., Aricò, M. & on behalf of the EBMT Paediatric Working Party. The role of BMT in childhood histiocytoses. Bone Marrow Transplant 41 (Suppl 2), S8–S13 (2008). https://doi.org/10.1038/bmt.2008.46
Published:
Issue Date:
DOI: https://doi.org/10.1038/bmt.2008.46
Keywords
This article is cited by
-
Improved outcome of refractory Langerhans cell histiocytosis in children with hematopoietic stem cell transplantation in Japan
Bone Marrow Transplantation (2010)
-
Outcome of pediatric patients with Langerhans cell histiocytosis treated with 2 chlorodeoxyadenosine: a nationwide survey in Japan
International Journal of Hematology (2010)