Abstract
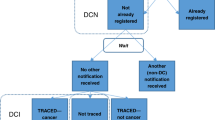
Merseyside and Cheshire Cancer Registry (MCCR) data quality was assessed by applying literature-based measures to 27,942 cases diagnosed in 1990 and 1991. Registrations after death (n = 8535) were also audited (n = 917) to estimate death certificate only (DCO) case accuracy and the proportion of registrations notified by death certificate (DC). Ascertainment appeared to be high from the registration/mortality ratio for lung [1.01:1] and to be low from capture-recapture estimates (59.4%), varying significantly with site from oesophagus [92.2% (95% CI 88.5-95.9)] to breast [47.5 (95% CI 41.8-53.2)]. The estimated DC-dependent proportion was 20% (5601 out of 27 942) with successful traceback in 3533 out of 5601 (63.1%) cases. DCO flagging (2497 out of 27,942, 8.9%) overestimated true DCO cases (2068 out of 27,942, 7.4%). The proportion of cases of unknown primary site was low (1.5%), varying significantly with age [0-4.2%, (95% CI 2.5-5.9)] and district [0.8% (95% CI 0.3-1.3) to 2.2% (95% CI 1.8-2.6)]. The median diagnosis to registration interval appeared to be good (10 weeks), varying significantly with site (P < 0.0001), age (P < 0.0001) and district (P < 0.0001). The proportion with a verified diagnosis was 77.3%, varying significantly with site [lung 55.2% (95% CI 53.7-56.7) to cervix 96.9% (95% CI 96.3-97.5)], age [45.2% (95% CI 40.9-49.5) to 97.5% (95% CI 96.4-98.6)] and district [71.8% (95% CI 69.9-73.8) to 82.5% (95% CI 80.7-84.3)]. The DCO percentages varied similarly by site [non-melanoma skin 0.4% (95% CI 0.2-0.6) to lung 22.6% CI (95% 19.9-25.3)], age [0.7(95% CI 0.1-1.4) to 23.0 (95% CI 19.4-26.6)] and district [6.9% (95% CI 5.7-8.1) to 13.9% (95% CI 12.9-15.0)]. MCCR data quality varied with age, site and district - inviting action - and apparently compares favourably with elsewhere, although deficiencies in published data hampered definitive assessment. Putting quality assurance into practice identified shortcomings in the scope, definition and application of existing measures, and absent standards impeded interpretation. Cancer registry quality assurance should henceforward be within an explicit framework of agreed and standardized measures.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Seddon, D., Williams, E. Data quality in population-based cancer registration: an assessment of the Merseyside and Cheshire Cancer Registry. Br J Cancer 76, 667–674 (1997). https://doi.org/10.1038/bjc.1997.443
Issue Date:
DOI: https://doi.org/10.1038/bjc.1997.443
This article is cited by
-
Bayesian estimation of a cancer population by capture-recapture with individual capture heterogeneity and small sample
BMC Medical Research Methodology (2015)
-
"Summary Page": a novel tool that reduces omitted data in research databases
BMC Medical Research Methodology (2010)
-
Breast cancer histological classification: agreement between the Office for National Statistics and the National Health Service Breast Screening Programme
Breast Cancer Research (2005)
-
Socioeconomic variation in colon cancer tumour factors associated with poorer prognosis
British Journal of Cancer (2003)
-
Concordance on the Recording of Cancer in the Saskatchewan Cancer Agency Registry, Hospital Charts and Death Registrations
Canadian Journal of Public Health (2000)