Abstract
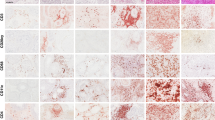
Early detection of testicular leukaemia and the identification of residual leukaemic cells in treated patients are important aims in the management of males with acute lymphoblastic leukaemia (ALL). In most cases of ALL ( greater than 95%) the blast cells express terminal deoxynucleotidyl transferase (TdT), a nuclear enzyme. We have therefore standardized the immuno-fluorescence and -peroxidase techniques (using anti-Tdt antibodies) for identifying TdT cells in the normal thymus, as well as in samples of testis with heavy leukaemic infiltrates (positive controls). TdT cells can be identified in formalin (but not in Bouin's or Carnoy's) fixed paraffin-embedded tissues, and the preservation of morphological details is excellent. The method is nevertheless difficult to standardize and also requires the use of deoxyribonuclease (DNase) for the digestion of sections. However, in frozen tissue sections, stronger staining of TdT cells was found, even without DNase treatment. Good morphology was preserved when cut sections were fixed immediately in the cryostat. In the second part of the study 15 samples from treated boys were analysed to see whether the technique is suitable to identify residual minimal leukaemic infiltrates. In 5 patients scanty disseminated TdT cells were detected, and in 2 patients small clumps of TdT cells were seen. The results indicate that the immunohistological identification of TdT ALL blasts may be the method of choice.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Rights and permissions
About this article
Cite this article
Thomas, J., Janossy, G., Eden, O. et al. Nuclear terminal deoxynucleotidyl transferase in leukaemic infiltrates of testicular tissue. Br J Cancer 45, 709–717 (1982). https://doi.org/10.1038/bjc.1982.112
Issue Date:
DOI: https://doi.org/10.1038/bjc.1982.112