Abstract
Objective:
To compare infants’ discomfort, nursing-time and caregiver preference, and assess the clinical efficiency (as a secondary outcome) of hood versus facemask nebulization in infants with evolving bronchopulmonary dysplasia (BPD) in the neonatal intensive care unit.
Study Design:
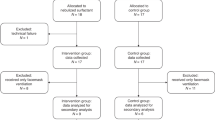
A prospective, open, randomized, controlled crossover clinical trial. In total, 10 infants with BPD who were on inhaled beta-agonist bronchodilators and corticosteroids were randomly assigned to receive their nebulized treatments either by a facemask, or by a hood for 2–3 days, and then crossover to receive the same treatments with the other technique for another 2–3 days. Infants’ discomfort, nursing-time, caregiver preference and clinical efficiency were compared.
Results:
At baseline there was no significant clinical difference between the groups. Nurse-time required for administering the hood nebulization (mean±s.e.m.: 1.9±0.1 min) was significantly shorter than the time for mask nebulization (12.0±0.6 min, P<0.0001). Infants’ discomfort score was significantly lower (0.1±0.04) for hood versus mask nebulization (2.5±0.2, P<0.0001). Nurses and parents unequivocally preferred the hood treatment. During both mask and hood nebulization therapies (2–3 days) clinical efficiency was comparable. While both methods caused an immediate (20 min post) clinical improvement, the immediate respiratory assessment change score was significantly greater for the hood versus the mask nebulization (0.62±0.27 versus 0.13±0.14, P<0.05).
Conclusions:
Nebulization of aerosolized medications in infants with evolving BPD by hood was less time-consuming for caregivers and was much better tolerated by the infants while being at least as effective as the conventional facemask nebulization.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Lister P, Iles R, Shaw B, Ducharme F . Inhaled steroids for neonatal chronic lung disease. Cochrane Database Syst Rev 2000; 3: CD002311.
Ng GY, da S, Ohlsson A . Bronchodilators for the prevention and treatment of chronic lung disease in preterm infants. Cochrane Database Syst Rev 2001; 3: CD003214.
Amirav I, Newhouse MT . Aerosol therapy with valved holding chambers in young children: importance of the facemask seal. Pediatrics 2001; 108: 389–394.
Everard MI, Clark AR, Milner AD . Drug delivery from jet nebulisers. Arch Dis Child 1992; 67: 586–591.
Cole CH . Special problems in aerosol delivery: neonatal and pediatric considerations. Respir Care 2000; 45: 646–651.
Fok TF, Monkman S, Dolovich M, Gray S, Coats G, Paes B et al. Efficiency of aerosol medication delivery from a metered dose inhaler versus jet nebuliser in infants with bronchopulmonary dysplasia. Pediatr Pulmonol 1996; 21: 301–309.
Amirav I, Balanov I, Gorenberg M, Groshar D, Luder AS, Newhouse MT . Nebulizer hood compared to mask in wheezy infants; aerosol therapy without tears. Arch Dis Child 2003; 88: 719–723.
Greenough A, Milner AD . Bronchopulmonary dysplasia. In: Arnold (ed). Neonatal respiratory disorders, 2nd edn, Hodder Headline Group: London; 2003, pp 400–422.
Klassen TP, Rowe PC, Suteliffe T, Ropp LJ, McDowell IW, Li MM . Randomized trial of albuterol in acute bronchiolitis. J Pediatr 1991; 118: 806–811.
Lowell DI, Lister G, Von Koss H, MacCarthy P . Wheezing in infants: the response to epinephrine. Pediatrics 1987; 79: 939–945.
Bertrand P, Aranibar H, Castro E, Sanchez I . Efficiency of nebulized epinephrine versus salbutamol in hospitalized infants with bronchiolitis. Pediatr Pulmonol 2001; 31: 284–288.
Postnatal corticosteroids to treat or prevent chronic lung disease in preterm infants. Committee on fetus and newborn. American Academy of Pediatrics and Canadian Paediatric Society. Pediatrics 2002; 109: 330–338.
Tal A, Golan H, Grauer N, Aviram M, Albin D, Quastral MR . Deposition pattern of radio labeled salbutamol inhaled from a metered-dose inhaler by means of a spacer with mask in young children with airway obstruction. J Pediatr 1996; 128: 479–484.
Murakami G, Igarashi T, Adachi Y, Matsuno M, Adachi Y, Sawai M et al. Measurement of bronchial hyperreactivity in infants and preschool children using a new method. Ann Allergy 1990; 64: 383–387.
Castro-Rodriguez JA, Rodrigo GJ . Beta agonists through metered-dose inhaler with valaved holding chamber versus nebulizer for acute exacerbation of wheezing or asthma in children under 5 years of age: a systematic review with meta-analysis. J Pediatr 2004; 145: 172–177.
Fok TF, Lam K, Ng PC, Leung TF, So HK, Cheung KL et al. Delivery of salbutamol to nonventilated preterm infants by metered dose inhaler, jet nebulizer, and ultrasonic nebulizer. Eur Respir J 1998; 12: 159–164.
Gappa M, Gartner M, Poets CF, Von der Hardt H . Effects of salbutamol delivery from a metered dose inhaler versus nebulizer on dynamic lung mechanics in very preterm infants with chronic lung disease. Pediatr Pulmonol 1997; 23: 442–448.
Fok TF, Lam K, Chan CK, Ng PC, Zhuang H, Wong W et al. Aerosol delivery to non-ventilated infants by metered dose inhaler; should a valved spacer be used? Pediatr Pulmonol 1997; 24: 204–212.
Acknowledgements
We thank Dr Mike Newhouse for his critical review and suggestions.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kugelman, A., Amirav, I., Mor, F. et al. Hood versus mask nebulization in infants with evolving bronchopulmonary dysplasia in the neonatal intensive care unit. J Perinatol 26, 31–36 (2006). https://doi.org/10.1038/sj.jp.7211434
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jp.7211434