Summary:
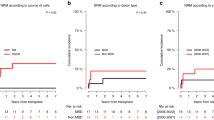
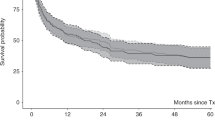
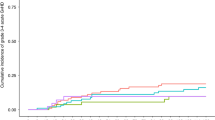
Myelofibrosis, either de novo or following pre-existing hematologic diseases, can be cured by allogeneic hematopoietic stem cell transplantation (SCT), but SCT is associated with significant morbidity and mortality, making the choice and timing of transplantation difficult. In all, 20 patients (seven female and 13 male), with a median age of 45 years (range 22–57 years), with idiopathic myelofibrosis (n=12), post-thrombocythemic (n=3) or post-polycythemic (n=2) myeloid metaplasia or leukemic transformation (n=3), underwent allogeneic SCT at our center between 1994 and 2003. With regard to the pre-transplant presence of risk factors such as hemoglobin levels ⩽10 mg/dl, grade III marrow fibrosis or peripheral blast counts >1%, patients were divided into high- and low-risk groups. The estimated 3-year survival post transplant was 38.5% for all patients. The 3-year probability of survival within the high-risk group (n=11) characterized by the presence of at least two risk factors was 16%. Low-risk patients (n=9) with at most one risk factor had an estimated 3-year survival of 67%. Thus, previously defined risk determinants for the outcome of allogeneic transplantation for myelofibrosis may provide useful information facilitating treatment strategies. Our data suggest that transplantation should be taken into consideration before poor prognostic variables develop.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Bouroncle B, Doan CA . Myelofibrosis: clinical, hematologic and pathologic study of 110 patients. Am J Med Sci 1962; 243: 697–715.
Tefferi A . Myelofibrosis with myeloid metaplasia. N Engl J Med 2000; 342: 1255–1265.
Jacobson RJ, Salo A, Fialkow PJ . Agnogenic myeloid metaplasia: a clonal proliferation of hemopoietic stem cells with secondary myelofibrosis. Blood 1978; 5: 189–194.
Rameshwar P, Denny TN, Stein D, Gascón P . Monocyte adhesion in patients with bone marrow fibrosis is required for the production of fibrogenic cytokines. J Immunol 1994; 153: 2819–2830.
Chagraoui H, Komura E, Tulliez M et al. Prominent role of TGF-beta 1 in thrombopoietin-induced myelofibrosis in mice. Blood 2002; 100: 3495–3503.
Cervantes F, Barosi G, Demory JL et al. Myelofibrosis with myeloid metaplasia in young individuals: disease characteristics, prognostic factors and identification of risk groups. Br J Haematol 1998; 102: 684–690.
Dupriez B, Morel P, Demory JL et al. Prognostic factors in agnogenic myeloid metaplasia: a report on 195 cases with a new scoring system. Blood 1996; 88: 1013–1018.
Cervantes F, Pereira A, Esteve J et al. Identification of ‘short-lived’ and ‘long-lived’ patients at presentation of idiopathic myelofibrosis. Br J Haematol 1997; 97: 635–640.
Rozman C, Giralt M, Feliu E et al. Life expectancy of patients with chronic nonleukemic myeloproliferative disorders. Cancer 1991; 67: 2658–2663.
Hoffman R, Silverstein MN . Agnogenic myeloid metaplasia. In: Hoffman R, Benz EJ, Shattil SJ, Furie B, Cohen HJ, Silberstein LE (eds). Hematology: Basic Principles and Practice, 2nd edn. Churchill Livingstone: New York, USA, 1995, pp 1160–1174.
Anderson JE, Sale G, Appelbaum FR et al. Allogeneic marrow transplantation for primary myelofibrosis and myelofibrosis secondary to polycythaemia vera or essential thrombocytosis. Br J Haematol 1997; 98: 1010–1016.
Guardiola P, Anderson JE, Bandini G et al. Allogeneic stem cell transplantation for agnogenic myeloid metaplasia: a European group for blood and marrow transplantation, société française de greffe de moelle, gruppo italiano per il trapianto midollo osseo, and Fred Hutchinson cancer research center. Blood 1999; 93: 2831–2838.
Deeg J, Gooley TA, Flowers ME et al. Allogeneic hematopoietic stem cell transplantation for myelofibrosis. Blood 2003; 102: 3912–3918.
Laszlo J . Myeloproliferative disorders (MPD): myelofibrosis, myelosclerosis, extramedullary hematopoiesis, undifferentiated MPD, and hemorrhagic thrombocythemia. Semin Hematol 1975; 12: 409–432.
Murphy S, Peterson P, Iland H, Laszlo J . Experience of the polycythemia study group with essential thrombocythemia: a final report on diagnostic criteria, survival, and leukemic transition by treatment. Semin Hematol 1997; 34: 29–39.
Thiele J, Kvasnicka HM, Fischer R . Histochemistry and morphometry on bone marrow biopsies in chronic myeloproliferative disorders – aids to diagnosis and classification. Ann Hematol 1999; 78: 495–506.
Glucksberg H, Storb R, Fefer A et al. Clinical manifestations of graft-versus-host disease in human recipient of marrow from HLA-matched sibling donors. Transplantation 1974; 18: 295–304.
Thomas E, Storb R, Clift RA et al. Bone-marrow transplantation. N Engl J Med 1975; 292: 832–843.
Elmaagacli AH, Runkel K, Steckel N et al. A comparison of chimerism and minimal residual disease between four different allogeneic transplantation methods in patients with chronic myelogenous leukemia in first chronic phase. Bone Marrow Transplant 2001; 27: 809–815.
Kaplan EL, Meier P . Nonparametric estimation from incomplete observations. J Am Stat Assoc 1958; 53: 457.
Gratwohl A, Hermans J, Goldman JM et al. Risk assessment for patients with chronic myeloid leukemia before allogeneic blood or marrow transplantation. Chronic Leukemia Working Party of the European Group for Blood and Marrow Transplantation. Lancet 1998; 352: 1087.
Ottinger HD, Ferencik S, Beelen DW et al. Hematopoietic stem cell transplantation: contrasting the outcome of transplantations from HLA-identical siblings, partially HLA-mismatched related donors, and HLA-matched unrelated donors. Blood 2003; 102: 1131–1137.
Soll E, Massumoto C, Clift RA et al. Relevance of marrow fibrosis in bone marrow transplantation: a retrospective analysis of engraftment. Blood 1995; 86: 4667–4673.
Cervantes F, Rovira M, Urbano-Ispizua A et al. Complete remission of idiopathic myelofibrosis following donor lymphocyte infusion after failure of allogeneic transplantation: demonstration of a graft-versus-myelofibrosis effect. Bone Marrow Transplant 2000; 26: 697–699.
Anderson JE, Trefferi A, Craig F et al. Myeloablation and autologous peripheral blood stem cell rescue results in hematologic and clinical responses in patients with myeloid metaplasia with myelofibrosis. Blood 2001; 98: 586–593.
Tanner ML, Hoh CK, Bashey A et al. FLAG chemotherapy followed by allogeneic stem cell transplant using nonmyeloablative conditioning induces regression of myelofibrosis with myeloid metaplasia. Bone Marrow Transplant. 2003; 32: 581–585.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ditschkowski, M., Beelen, D., Trenschel, R. et al. Outcome of allogeneic stem cell transplantation in patients with myelofibrosis. Bone Marrow Transplant 34, 807–813 (2004). https://doi.org/10.1038/sj.bmt.1704657
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1704657
Keywords
This article is cited by
-
The role of JAK inhibitors in hematopoietic cell transplantation
Bone Marrow Transplantation (2022)
-
Indication and management of allogeneic stem cell transplantation in primary myelofibrosis: a consensus process by an EBMT/ELN international working group
Leukemia (2015)
-
Indications and outcomes of reduced-toxicity hematopoietic stem cell transplantation in adult patients with hematological malignancies
International Journal of Hematology (2013)
-
How to manage the transplant question in myelofibrosis
Blood Cancer Journal (2012)
-
Allogeneic hemopoietic SCT for patients with primary myelofibrosis: a predictive transplant score based on transfusion requirement, spleen size and donor type
Bone Marrow Transplantation (2010)