Abstract
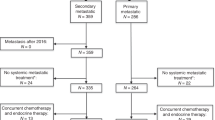
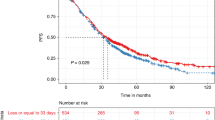
We retrospectively analyzed the effect of maintenance endocrine therapy (MET) after high-dose chemotherapy with hematopoietic progenitor cell transplant (HDCT) on the progression-free survival (PFS) of patients with hormone-dependent metastatic breast cancer (MBC). One hundred and nine consecutive patients with estrogen receptor (ER) and/or progesterone receptor (PgR)-positive MBC, who were progression free for at least 4 months after HDCT with cyclophosphamide, carmustine and thiotepa (CBT), were analyzed. Of these, 55 were non-randomly submitted to MET. After a median follow-up of 34.4 months (17.1–91.0), univariate analysis showed that MET was significantly associated with improved median PFS (31.1 vs 19.2 months, P = 0.022). Complete response to HDCT, pattern of metastatic spread, extent of the disease, single vs multiple metastatic sites, prior endocrine therapy for metastatic disease and prior exposure to any hormonal therapy (adjuvant and/or for the advanced disease) were also associated with PFS at univariate analysis. A multivariate Cox proportional hazard model was fitted to the data in order to correct the effect of MET for the other significant covariates. After correcting for these covariates, MET was still significant, predicting improved PFS (hazard ratio (HR) 0.580, 95% CI; 0.362–0.931). Administration of MET after optimal cytoreduction might result in increased efficacy of HDCT in hormone-dependent metastatic breast cancer.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Stadtmauer EA, O'Neill A, Goldstein LJ et al. Conventional-dose chemotherapy compared with high-dose chemotherapy plus autologous hematopoietic stem-cell transplantation for metastatic breast cancer. Philadelphia Bone Marrow Transplant Group New Engl J Med 2000 342: 1069 1076
Lotz JP, Cure H, Janvier M et al. Intensive chemotherapy and autograft of hematopoietic stem cells in the treatment of metastatic cancer: results of the national protocol Pegase 04 Hematol Cell Ther 1999 41: 71 74
Nieto Y, Champlin RE, Wingard JR et al. Status of high-dose chemotherapy for breast cancer: a review Biol Blood Marrow Transplant 2000 6: 476 495
Rizzieri DA, Vredenburgh JJ, Jones R et al. Prognostic and predictive factors for patients with metastatic breast cancer undergoing aggressive induction therapy followed by high-dose chemotherapy with autologous stem-cell support J Clin Oncol 1999 17: 3064 3074
Rowlings PA, Williams SF, Antman KH et al. Factors correlated with progression-free survival after high-dose chemotherapy and hematopoietic stem cell transplantation for metastatic breast cancer JAMA 1999 282: 1335 1343
Ayash LJ, Wheeler C, Fairclough D et al. Prognostic factors for prolonged progression-free survival with high-dose chemotherapy with autologous stem-cell support for advanced breast cancer J Clin Oncol 1995 13: 2043 2049
Williams SF, Gilewski T, Mick R et al. High-dose consolidation therapy with autologous stem-cell rescue in stage IV breast cancer: follow-up report J Clin Oncol 1992 10: 1743 1747
Dunphy FR, Spitzer G, Fornoff JE et al. Factors predicting long-term survival for metastatic breast cancer patients treated with high-dose chemotherapy and bone marrow support Cancer 1994 73: 2157 2167
Greenberg PA, Hortobagyi GN, Smith TL et al. Long-term follow-up of patients with complete remission following combination chemotherapy for metastatic breast cancer J Clin Oncol 1996 14: 2197 2205
Tomiak E, Piccart M, Mignolet F et al. Characterisation of complete responders to combination chemotherapy for advanced breast cancer: a retrospective EORTC breast group study Eur J Cancer 1996 32A: 1876 1887
Winer EP, Morrow M, Osborne KC, Harris JR . Malignant tumors of the breast. In: DeVita VT Jr, Hellman S, Rosenberg SA (eds) Cancer: Principles and Practice of Oncology Lippincott Williams & Wilkins: Philadelphia 2001 1651 1717
Hortobagyi GN . Treatment of breast cancer New Engl J Med 1998 339: 974 984
Swenerton KD, Legha SS, Smith T et al. Prognostic factors in metastatic breast cancer treated with combination chemotherapy Cancer Res 1979 39: 1552 1562
Miller AB, Hoogstraten B, Staquet M et al. Reporting results of cancer treatment Cancer 1981 47: 207 214
Berruti A, Zola P, Buniva T et al. Prognostic factors in metastatic breast cancer patients obtaining objective response or disease stabilization after first-line chemotherapy with epirubicin. Evidence for a positive effect of maintenance hormonal therapy on overall survival Anticancer Res 1997 17: 2763 2768
Kloke O, Klaassen U, Oberhoff C et al. Maintenance treatment with medroxyprogesterone acetate in patients with advanced breast cancer responding to chemotherapy: results of a randomized trial. Essen Breast Cancer Study Group Breast Cancer Res Treat 1999 55: 51 59
Hortobagyi GN . Progress in the endocrine therapy of breast cancer Cancer 1998 83: 1 6
Thürlimann B, Paridaens R, Serin D et al. Third-line hormonal treatment with exemestane in postmenopausal patients with advanced breast cancer progressing on aminoglutethimide: a phase II multicentre multinational study. Exemestane Study Group Eur J Cancer 1997 33: 1767 1773
Dombernowsky P, Smith I, Falkson G et al. Letrozole, a new oral aromatase inhibitor for advanced breast cancer: double-blind randomized trial showing a dose effect and improved efficacy and tolerability compared with megestrol acetate J Clin Oncol 1998 16: 453 461
Goss PE, Strasser K . Aromatase inhibitors in the treatment and prevention of breast cancer J Clin Oncol 2001 19: 881 894
Buzdar A, Douma J, Davidson N et al. Phase III, multicenter, double-blind, randomized study of letrozole, an aromatase inhibitor, for advanced breast cancer versus megestrol acetate J Clin Oncol 2001 19: 3357 3366
Nabholtz JM, Buzdar A, Pollak M et al. Anastrozole is superior to tamoxifen as first-line therapy for advanced breast cancer in postmenopausal women: results of a North American multicenter randomized trial J Clin Oncol 2000 18: 3758 3767
Bearman S, Vredenburgh J, Cagnoni P et al. High-dose therapy with autologous hematopoietic cell support as salvage treatment for patients with breast cancer who have relapsed after previous high-dose chemotherapy Bone Marrow Transplant 1999 24: 491 495
Acknowledgements
This work was presented in part at the EBMT International Conference on High-Dose Chemotherapy in Breast and Ovarian Cancer, 14–16 September 2000, Florence, Italy. FM was also supported by a grant from Institute for Cancer Research and Treatment, Ordine Mauriziano, Candiolo, Torino, Italy.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Montemurro, F., Rondón, G., Ueno, N. et al. Factors affecting progression-free survival in hormone-dependent metastatic breast cancer patients receiving high-dose chemotherapy and hematopoietic progenitor cell transplantation: role of maintenance endocrine therapy. Bone Marrow Transplant 29, 861–866 (2002). https://doi.org/10.1038/sj.bmt.1703555
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1703555
Keywords
This article is cited by
-
CHEOPS trial: a GINECO group randomized phase II assessing addition of a non-steroidal aromatase inhibitor to oral vinorelbine in pre-treated metastatic breast cancer patients
Breast Cancer (2023)
-
Long-term survival in patients with metastatic breast cancer receiving intensified chemotherapy and stem cell rescue: data from the Italian registry
Bone Marrow Transplantation (2013)
-
Cancer du sein méta-analyse en première ligne
Oncologie (2011)
-
High-dose chemotherapy and autologous peripheral blood stem cell transplantation for primary breast cancer refractory to neoadjuvant chemotherapy
Bone Marrow Transplantation (2006)