Abstract
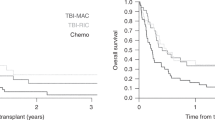
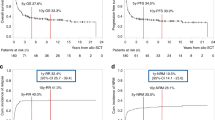
High MRD levels before transplantation in children receiving T cell-depleted unrelated grafts for relapsed ALL were associated with a 100% relapse risk. We report on two children with relapsed ALL who underwent non T cell-depleted BMT from unrelated donors. Despite a high residual tumor load pre- transplant and the occurrence of only aGVHD grade I, they are still in second complete remission 2.7 and 5.2 years after transplantation, respectively. Thus, we propose that the transplant regimens influence the prognostic significance of high MRD levels pre-BMT.
Bone Marrow Transplantation (2001) 28, 1087–1089.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Van Dongen JJM, Seriu T, Panzer-Grümayer ER et al. Prognostic value of minimal residual disease in acute lymphoblastic leukaemia in childhood Lancet 1998 352: 1731–1738
Cave H, van der Werff ten Bosch J, Suciu S et al. Clinical significance of minimal residual disease in childhood acute lymphoblastic leukaemia New Engl J Med 1998 339: 591–597
Coustan-Smith E, Behm FG, Sanchez J et al. Immunological detection of minimal residual disease in children with acute lymphoblastic leukaemia Lancet 1998 351: 550–554
Knechtli CJC, Goulden NJ, Hancock JP et al. Minimal residual disease status before allogeneic bone marrow transplantation is an important determinant of successful outcome for children and adolescents with acute lymphoblastic leukaemia Blood 1998 92: 4072–4079
Schrappe M, Reiter A, Zimmermann M et al. Long-term results of four consecutive trials in childhood ALL performed by the ALL-BFM study group from 1981 to 1995 Leukemia 2000 14: 2205–2222
Pongers-Willemse MJ, Seriu T, Stolz F et al. Primers and protocols for standardized detection of minimal residual disease in acute lymphoblastic leukemia using immunoglobulin and T cell receptor gene rearrangements and TAL1 deletions as PCR targets: report of the Biomed-1 concerted action: investigation of minimal residual disease in acute leukemia Leukemia 1999 13: 110–118
Eiermann TH, Lambrecht P, Zander AR . Monitoring anti-thymocyte globulin (ATG) in bone marrow recipients Bone Marrow Transplant 1999 23: 779–781
Maraninchi D, Gluckman E, Blaise D et al. Impact of T cell depletion on outcome of allogeneic bone-marrow transplantation for standard risk leukaemias Lancet 1987 25: 175–178
Vettenranta K, Saarinen-Pihkala UM, Cornish J et al. Pediatric marrow transplantation for acute leukaemia using unrelated donors and T-replete or -deplete grafts: a case-matched analysis Bone Marrow Transplant 2000 25: 395–399
Uzunel M, Mattson J, Jaksch M et al. The significance of graft-versus-host disease and pretransplantation minimal residual disease status to outcome after allogeneic stem cell transplantation in patients with acute lymphoblastic leukemia Blood 2001 98: 1982–1984
Acknowledgements
This work was supported by a grant from the FWF 13757-Med to ERP-G.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Schneider, M., Hettinger, K., Matthes-Martin, S. et al. Influence of transplantation regimen on prognostic significance of high-level minimal residual disease before allogeneic stem cell transplantation in children with ALL. Bone Marrow Transplant 28, 1087–1089 (2001). https://doi.org/10.1038/sj.bmt.1703286
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1703286