Abstract
Objectives: To describe the first-week feeding patterns for breast- vs bottle-fed babies, and their association with sustained breast-feeding and infant weight gain at 6 weeks.
Design: A longitudinal cohort study.
Setting: Feeding diaries were completed by mothers in an urban UK community shortly after birth; follow-up weight and feeding data were collected at routine health checks.
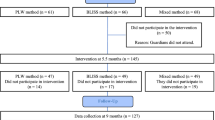
Subjects: Mothers of 923 full-term infants born during the recruiting period agreed to join the study. In all, 502 usable diaries were returned from 54% of the cohort.
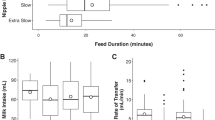
Results: Breast-fed infants were fed more frequently (2.71 h between feeds) than bottle-fed infants (3.25 h between feeds) and mixed-fed infants (3.14 h between feeds) (P<0.001) in the first week of life, while duration of feeds was similar. Only exclusive breast-feeding in the first week (P<0.001) and maternal education (P=0.004) were related to continued breast-feeding at 6 weeks. Greater first-week feeding frequency (as measured by feed-to-feed interval, h) was associated with higher weight gain at 6 weeks for breast-feeders, but no analysed factors were associated with higher weight gain for bottle-feeders.
Conclusions: This large-scale study of first-week feeding patterns sheds light on the important and complicated issues of breast-feeding continuation and infant weight gain, with implications for the feeding advice given to mothers. Supplementary bottle feeds were clearly associated with discontinued breast-feeding at 6 weeks. Over that period, higher weight gain was associated with more frequent feeding for breast-fed infants only.
Sponsorship: Henry Smith Charity, SPARKS, Child Growth Foundation.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Agras WS (1987): Does a vigorous feeding style influence early development of adiposity? J Pediatr 110, 799–804.
Dewey KG, Heinig MJ, Nommsen LA, Peerson JM & Lonnerdal B (1992): Growth of breast-fed and formula-fed infants from 0 to 18 months: the DARLING study. Pediatrics 89, 1035–1041.
Eriksson J, Forsen T, Tuomilehto J, Osmond C & Barker D (2001): Early Growth and coronary heart disease in later life: longitudinal study. BMJ 322, 949–953.
Foster K, Lader D & Cheesbrough S (1995): Infant feeding 1995: Results from a Survey Carried Out by the Social Survey Division of ONS on Behalf of the UK Health Departments. London: The Stationery Office.
Freeman JV, Cole TJ, Chinn S, Jones PRM, White EM & Preece MA (1995): Cross sectional stature and weight reference curves for the UK, 1990. Arch Dis Child 73, 17–24.
Health Education Authority (1998): Birth to five. London: Health Education Authority.
Hillervik-Lindquist C, Hofvander Y & Sjölin S (1991): Studies on perceived breast milk insufficiency. Acta Paediatr Scand 80, 297–303.
Hörnell A, Aarts C, Kylberg E, Hofvander Y & Gebre-Medhin M (1999): Breastfeeding patterns in exclusively breastfed infants: a longitudinal prospective study in Uppsala, Sweden. Acta Paediatr 88, 203–211.
Kramer MS, Guo T, Platt RW, Shapiro S, Collet JP, Chalmers B, Hodnett E, Sevkovskaya Z, Dzikovich I & Vanilovich I (2002): Breastfeeding and infant growth: biology or bias? Pediatrics 110, 343–347.
Millard AV (1990): The use of the clock in pediatric advice: rationales, cultural themes, and impediments to breastfeeding. Soc Sci Med 31, 211–221.
Mozingo J, Davis M, Droppleman PG & Meredith A (2000): It wasn’t working: women's experiences with short-term breastfeeding. Am J Matern Child Nurs 25, 120–126.
Nelson SE, Rogers RR, Ziegler EE & Fomon SJ (1989): Gain in weight and length during early infancy. Early Hum Dev 19, 223–239.
Quandt SA (1986): Patterns of variation in breast-feeding behaviors. Soc Sci Med 23, 445–453.
Righard L (1998): Are breastfeeding problems related to incorrect breastfeeding technique and the use of pacifiers and bottles? Birth 25, 40–44.
Salariya EM, Easton PM & Cater JI (1978): Duration of breast-feeding after early initiation and frequent feeding. Lancet 2 (8100), 1141–1143.
Townsend P, Phillimore P & Beattie A (1988): Health and deprivation: Inequality and the North. London: Croom Helm.
World Health Organization (2001): The Optimal Duration of Exclusive Breastfeeding: Report of an Expert Consultation, 28-30 March 2001. Geneva: WHO. Report No. WHO/FCH/CAH/01.24.
Wright CM, Matthews JNS, Waterson A & Aynsley-Green A (1994): What is a normal rate of weight gain in infancy? Acta Paediatr 83, 351–356.
Wright CM, Parker L, Lamont D & Craft AW (2001): Implications of childhood obesity for adult health: findings from the thousand families cohort study. BMJ 323, 1280–1284.
Wright P (1981): Development of feeding behaviour in early infancy: implications for obesity. Health Bull 39, 197–205.
Wright P (1986): Do breastfeeding mothers know how hungry their babies are? Midwifery 2, 86–92.
Wright P, Fawcett J & Crow R (1980): The development of differences in the feeding behaviour of bottle and breast fed human infants from birth to two months. Behav Process 5, 1–20.
Acknowledgements
The project support was provided by the Henry Smith Charity, SPARKS, and the Child Growth Foundation.
Author information
Authors and Affiliations
Contributions
Guarantor: RE Casiday.
Contributors: REC was the principal researcher responsible for data analysis and manuscript preparation. CMW was responsible for overseeing data collection and analysis, and manuscript preparation. CP-B was responsible for overseeing data analysis and manuscript preparation. KNP was responsible for data collection.
Corresponding author
Rights and permissions
About this article
Cite this article
Casiday, R., Wright, C., Panter-Brick, C. et al. Do early infant feeding patterns relate to breast-feeding continuation and weight gain? Data from a longitudinal cohort study. Eur J Clin Nutr 58, 1290–1296 (2004). https://doi.org/10.1038/sj.ejcn.1601964
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ejcn.1601964
Keywords
This article is cited by
-
The impact of reducing the frequency of night feeding on infant BMI
Pediatric Research (2022)
-
Zufüttern – ab wann, was und wie?
Pädiatrie & Pädologie (2019)