Abstract
Nascent studies showed that patients with chronic medical illnesses such as diabetes mellitus (DM) and HIV/AIDS are highly vulnerable to face both treatment burden and regimen fatigue. However, an attempt made so far in this sphere in sub-Saharan African health care context is dearth. Thus, this study aimed to determine the level of treatment burden and regimen fatigue of diabetic and HIV patients attending adult diabetic and ART clinics of TASH and explore patients’ and health care workers’ propositions to reduce treatment burden and regimen fatigue. An explanatory sequential mixed methods study was conducted at the adult HIV and DM clinics of TASH, Addis Ababa, Ethiopia from February 01-March 30, 2022. Simple random and purposive sampling techniques were employed to select participants for quantitative and qualitative studies, respectively. Descriptive analysis was done to summarize the quantitative data. Logistic and linear regression analyses were performed to identify predictors of treatment burden and regimen fatigue, respectively. P value < 0.05 was considered statistically significant. Qualitative data was analyzed by using a thematic analysis. A total of 300 patients (200 diabetes and 100 HIV) were included in the quantitative study. For the qualitative study, 14 patients and 10 health care workers (six nurses and four medical doctors) were included. Participants' mean global Treatment Burden Questionnaire (TBQ) and Treatment Regimen Fatigue Scale (TRFS) score were 28.86 ± 22.13 and − 42.82 ± 17.45, respectively. Roughly, 12% of patients experienced a high treatment burden. The presence of two or more comorbidities (adjusted odds ratio [AOR] = 7.95, 95% confidence interval [CI] 1.59–39.08), daily ingestion of more than five types of prescribed medications (AOR = 6.81, 95%CI 1.59–29.14), and good knowledge about DM and/or HIV (AOR = 0.33, 95%CI 0.12–0.92) were predictors of treatment burden. Poor availability of medications (β = 0.951, p < 0.001) was the only predictor of regimen fatigue. Patients and health care workers primarily proposed to foster self-care efficacy, advance administrative services of the clinic and hospital, and improve healthcare system provision. The findings of this study unveiled that a considerable proportion of patients experienced low levels of treatment burden and regimen fatigue. This study showed that boosting the patients’ self-care efficacy, upgrading administrative services of the clinic and hospital, and promoting the healthcare system provision had enormous significance in reducing treatment burden and regimen fatigue. Therefore, when designing patient-specific healthcare interventions for both HIV and diabetic patients’ various factors affecting both treatment burden and regimen fatigue should be considered to achieve the desired goals of therapy.
Similar content being viewed by others
Introduction
Globally, chronic diseases like diabetes mellitus (DM) and HIV/AIDS are astoundingly increasing in almost epidemic proportions1. Unfortunately, adherence to lifelong complex treatment, continuous health care engagement, multiple lifestyle modifications, and adaptive coping skills are mandatory to adequately control these diseases2. In sub-Saharan Africa (SSA) countries including Ethiopia, these patients often face prodigious barriers such as out-of-pocket expenses, time spent traveling, attending clinical appointments, stigma, fear of disclosure, and drug stock-outs2,3. As a result, patients living with HIV and DM are highly vulnerable to facing treatment burden (TB) and regimen fatigue (TRF).
Treatment burden refers to the workload that a patient must manage to take care of their health and its impact on the patient’s daily life4,5. Treatment regimen fatigue refers to a decreased desire and motivation to maintain vigilance in adhering to a long-term treatment6. Both are novel clinical concepts that need to be well articulated in patients with DM and HIV/AIDS3. They can cause poor medication adherence which eventually leads to fatal clinical outcomes such as more hospitalizations, higher mortality, poorer health-related quality of life, worsening or recurrence of symptoms, and ineffective use of finite health resources7,8. Recent systematic review studies9,10 indicated that TB and TRF could be affected by numerous personal, disease, and treatment-related factors.
Although some qualitative studies11,12,13,14 in amalgamation with systematic reviews4,6,7 have been conducted to conceptualize TB and TRF in DM or HIV/AIDS, quantitative-based studies done on this sphere are dearth. Evidences indicated that TB and TRF had many common features, notwithstanding, they vary between specific countries and diseases as both are contextual concepts that depend on variety of factors such as personal characteristics like age gender, educational level, marital status, living condition, health literacy, and family support, illness duration or severity, treatment characteristics (e.g., medication type, number, and dose of medications), and financial cost of treatment2,15. So, direct extrapolation of findings from different Western countries is not a judicious option to apply in the SSA healthcare setup.
So far, quite a few studies have sought patients’ perspectives and propositions to ameliorate treatment onerousness and regimen fatigue. Nonetheless, almost all these studies were done in developed nations and thus could not be inferred to the SSA health care context. Hence, further exploration is required2,16. Moreover, the health care worker’s perspectives on these issues remain untapped. So, the current study was designed to fill these gaps of knowledge. Hence, this study aimed to determine the level of treatment burden and regimen fatigue of diabetic and HIV patients attending adult diabetic and ART clinics of TASH and explore patients’ and health care workers’ propositions to reduce treatment burden and regimen fatigue.
Methods
Study setting, study design and study period
This study used an explanatory sequential mixed methods design. Consequently, a quantitative (cross-sectional) investigation was followed by a qualitative study. From February 1 to March 30, 2022, the study was conducted at TASH's ambulatory ART and diabetes clinics in Addis Ababa, Ethiopia. TASH is Ethiopia's largest government-owned tertiary care, specialized, referral, and teaching hospital. It has 51 specialty and sub-specialty out-patient clinics that serve around 500,000 patients per year17. The ART and DM clinics are part of a larger network of specialized clinics that offer full care, including treatment and follow-up. The DM clinic is open three days a week (Monday, Wednesday, and Friday), but the ART clinic is open five days a week (excluding weekends). Every day, on average, 70 diabetics and 50 HIV patients come for follow-up.
Study participants
All adult HIV and diabetes patients who visited TASH's respective ambulatory clinics on a regular basis and met the inclusion criteria during the study period were included. Patients were eligible for enrollment in this study if they were at least 18 years old, had been diagnosed with HIV or/and diabetes for at least 6 months prior to the study, had regular follow-up at TASH's ART and DM clinics, had been on treatment for at least 6 months, and could complete a written consent form. Patients with cognitive disabilities who may have difficulty understanding questions and critically sick patients who cannot tolerate interviews were excluded.
Sample size calculation and sample size determination
The sample size was estimated using a single population proportion calculation with a 95% confidence level, 5% margin of error, 50% proportion of TB and TRF, expected number of source population (N = 4240), and 5% non-response rate. As a result, a total sample size of 370 patients was determined. 70 patients (30 from the diabetic clinic and 40 from the ART clinic) were excluded, leaving 300 patients (200 from the diabetes clinic and 100 from the HIV clinic) in the final analysis. The main reasons for exclusion were unwillingness to participate in the study and intolerance to complete in-depth interview.
To identify study participants who met the stated inclusion criteria for the quantitative investigation, a simple random selection procedure was used. As a sampling framework, the nurse appointment logbook was used. Patients were included in the research at random during their drug refill appointment. Purposive sampling was used to collect detailed information from patients and health care staff for the qualitative investigation. As a result, from each clinic, 7 patients and 5 health care staff were chosen. The qualitative study included 14 patients (7 females) and 10 health care providers (6 females and 4 males).
Six experienced nurses and four medical doctors (1 senior endocrine specialist, 1 senior infectious disease specialist, 2 fellowship residents, and 1 chief R3 resident) made up the health care team. Patients were chosen for in-depth interviews based on their TBQ and TRFS global scores, whereas health care personnel were chosen for key informant interviews based on their experience and knowledge with diabetes and HIV/AIDS management. After a brief explanation of the study by the matrons of the two clinics, eligible patients and health care personnel were reached through oral invitation and invitation letter, respectively. The participants who had only accepted the invitation offer were then contacted by phone to set up a convenient date and time for the interviews.
Study variables
Dependent variables: (1) treatment burden, (2) treatment regimen fatigue. Independent variables: (1) sociodemographic characteristics include age, sex, place of residence, occupation status, monthly income level, marital status, education level, smoking habit, and living conditions. (2) Clinical characteristics include duration of DM/HIV/AIDS, duration of treatment, severity of DM/HIV, presence and number of comorbidities, travel time, number of appointments, number of hospitalizations during the past 12 month, knowledge about DM/HIV/AIDS, and health literacy. (3) Treatment-related characteristics include total number of prescribed medications/pills, medications source, medication type, costs of medications, availability of medications, and ADR.
Data collection instruments and procedure
The current investigation was divided into two basic parts. In phase I, standardized questionnaires were used to collect quantitative data on the patients' sociodemographic, clinical, and therapeutic features, as well as their level of TB and TRF. Patients' medical records were also checked to augment additional clinical data if needed. The Treatment Burden Questionnaire (TBQ-15) and Treatment Regimen Fatigue Scale (TRFS) were used to assess diabetic and HIV patients' treatment burden and regimen tiredness, respectively. The TBQ and TRFS were administered by two nurses having MSc degrees. On average, quantitative data gathering took 30 min.
The TBQ-15 is a well-validated universal psychometric instrument consisting of 15 items with scores ranging from 0 (no burden) to 10 (extremely high burden) that assesses the burden associated with medication management, self-monitoring, laboratory tests, doctor visits, the need for organization, administrative tasks, diet, physical activity, social impact, and financial burden of patients. It has five dimensions: medication-related hardship, administrative burden, financial burden, lifestyle modification burden, and social life-related burden18. The TRFS is a simple and reliable self-report psychometric instrument used to assess the amount of TRF in patients with chronic conditions who are on long-term treatment regimens. It consists of 22 items that examine three dimensions: treatment motivation, cynicism, and self-efficacy19.
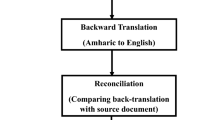
Permission to utilize the TBQ and TRFS, as well as authorization to translate them, were secured from the original developers via Mapi Research Trust (MRT) and the corresponding author, who conducted the initial validation research, respectively. As previously described in our pioneering published work, a strict translation approach was employed20. In the current study, the Cronbach alpha values for the Amharic for Ethiopia versions of TBQ-15 and TRFS were 0.76 and 0.81, respectively. However, other than internal consistency, no additional psychometric testing was performed.
In phase II, semi-structured interviews were used to collect qualitative data on patients' and health care staff' suggestions for reducing TB and TRF. In-depth and key informant interviews lasting around 30 min were conducted utilizing an interview guide adapted from diverse literatures. Face-to-face cognitive interviews with 10 patients and 5 health care personnel were used to ensure the comprehensibility of the opening question and the usability of potential reformulations and explanations. Furthermore, the face and content validity of the data collection devices were investigated by four highly qualified professionals in clinical research and diabetes/HIV/AIDS management. Two clinical pharmacists with master's degrees and extensive prior experience in qualitative-based health research conducted the interviews face-to-face in a separate quiet room adjacent to the DM clinic's matron's head station.
Principal investigators adequately trained data collectors for two consecutive days on the strict application of study criteria, explanation of study objectives, obtaining written consents, implementation of sampling techniques, uniform interpretation of questions, and the confidentiality of collected data. To record information from the interviews, voice recorders and notebooks were employed. Interviews were performed until the information was exhausted. Finally, the results of both phases I and II were evaluated to provide a thorough understanding of TB and TRF.
Data analysis
The quantitative data was input and cleaned in Epi Info version 4.6.0.2 before being exported and analyzed in the Statistical Package for the Social Sciences (SPSS) version 26. To summarize the categorical variables, frequencies and proportions were used. The mean, standard deviation, and/or median (IQR) of continuous variables were provided. Initially, normality tests utilizing plots and the Shapiro–Wilk test were used to choose relevant and robust statistical tests for continuous data. In addition, the variance inflation factor (VIF) was used to examine correlation among predictor variables. For excluding collinearity, a VIF of 10 was chosen as a cut point.
To analyze the relationship between treatment load and all independent variables and to identify candidates for multivariable analysis, binary logistic regression analysis was used. To find predictors of treatment burden, independent variables having p values less than 0.25 in univariable binary logistic regression analysis were re-entered into a multivariable binary logistic regression model. Statistical significance was defined as a p value of 0.05.
Univariable and multivariable linear regressions, on the other hand, were used to identify factors linked with regimen weariness. To begin, the statistical assumptions of linear regression analysis were put to the test. The Pearson R statistical test was used to calculate correlations between research variables. The multivariable linear regression analysis included all predictor variables with p values less than 0.25 in the univariable linear regression analysis. The overall model (F statistic, degrees of freedom, and p-value) was then reported, as was the variance explained by the overall model (adjusted r2) and any significant independent variables in the model (unstandardized beta coefficient, p-value).
Thematic analysis was used to assess the qualitative data. To aid with data analysis, the NVivo 12 qualitative data analysis program (QSR International Pty Ltd. Version 12, 2018) was employed. The data was first evaluated by verbatim transcribing the recorded data from Amharic to English, and then the transcript was classified and grouped into themes. Two investigators (OSM and MH) independently transcribed the audio recordings verbatim and read all of the participants' interview notes. The four investigators were in charge of coding, categorizing, and developing themes. Each theme's concepts were presented, narrated, and triangulated with quantitative findings.
Operational definitions
Treatment Burden Global Score—the sum of all items scores of the questionnaire with ‘does not apply’ and missing answer considered the lowest possible score (0) [scores ranging from 0 to 150]. No Treatment Burden—a score of 0 for each item in the TBQ. Low Treatment Burden—a TBQ global score of < 59. High Treatment Burden—a TBQ global score of ≥ 59. Treatment Regimen Fatigue—waning commitment to continue with a prescribed long-term treatment. Limited Health Literacy—if participants ‘sometimes’ or ‘often’ or ‘always’ need reading help for written health materials related to DM and HIV. Poor Medications Availability —if medications are available ‘sometimes’, ‘rarely’, ‘not at all’ as self-reported by the patient. Poor Knowledge of DM/HIV—if patients responded ‘insufficient’ or ‘very insufficient’ when asked about their knowledge about HIV/AIDS and Diabetes (e.g., symptoms, disease progression) and its treatment protocols (e.g., possible side effects, expected benefits, other treatment options). Poor family support—if patients does not obtain family/caregiver support (physical, psychological, financial) in self-management of their disease. Comorbidity—presence of two or more concurrent illnesses other than the primary diseases (HIV-AIDS and Diabetes Mellitus).
Ethical approval and informed consent
The study was approved by the Ethical Review Board (ERB) of Addis Ababa University, College of Health Sciences (25/03/2021; ERB No. 259/13/2021). The study protocol was performed in accordance with the Declaration of Helsinki. The aim and protocol of the current study were fully explained to all participants included in the study and written informed consent was obtained from all participants. All obtained data were treated confidentially.
Results
Sociodemographic characteristics of the study participants
A total of 300 patients (200 diabetes and 100 HIV) were included in the study. Out of the total, 162(54.0%) were female, 175(58.3%) were married, 115(38.3%) were unemployed, 253(84.3%) were from Addis Ababa, and 102(34.0%) had completed secondary school. The mean age of the participant was 49.76 ± 13.57 years (Table 1).
Clinical characteristics of the study participants
The median (IQR) duration of DM/HIV was 10 (6–16) years, and about 83.5% had type 2 DM. Most participants 212(70.7%) had to travel an hour and more to reach to the respective clinics. About 205(68.3%) of the participants were presented with other comorbid diseases (Table 2).
Treatment related characteristics of the study participants
Participants took an average of 4.19 ± 3.19 pills daily. With regards to ADR, 69(23.0%) of them reported adverse drug effects. Nearly half of the study participants (52.3%) obtained their refill medications via health insurance system. Majority of the participants 138(46.0%) had two or more comorbid conditions. Out of which, half of them (50.0%) were presented with hypertension, then followed by cardiac diseases (39.0%), and dyslipidemia (13.7%) (Table 3).
Description of treatment burden and treatment regimen fatigue
A mean global TBQ score of 28.86 (SD = 22.13) was reported by participants. Highest levels of treatment onerousness were reported in the administrative (mean = 9.05, SD = 9.42), medication (mean = 5.98, SD = 8.27) and social (mean = 5.93, SD = 6.10) domains. In contrast, lowest levels of treatment onerousness were displayed in the lifestyle change (mean = 4.06, SD = 5.05) and financial (mean = 3.84, SD = 4.22) domains (Table 4). About 265(88.3%) of the study participants exhibited low burden (TBQ score < 59), while only 35(11.7%) demonstrated high burden (TBQ score ≥ 59). With regard to regimen fatigue, participants’ self-reported mean global score of TRFS were − 42.82 (SD = 17.45).
Factors associated with treatment burden
The multivariable binary logistic regression model unveiled that presence of two and more comorbidities adjusted odd ratio [AOR] = 7.95, 95% CI 1.59–39.08), daily ingestion of more than five types of prescribed medications (AOR = 6.81, 95% CI 1.59–29.14), and good knowledge about DM/HIV and their treatment protocols (AOR = 0.33, 95% CI 0.12–0.92) were found to be predictors of higher burden of treatment (Table 5).
Factors associated with treatment regimen fatigue
Correlational analysis examining the association between potential antecedent factors and TRF indicated that number of comorbidities (r = 0.125; p = 0.030) was significantly correlated with TRF (see supplementary Table S1). The multivariable analysis demonstrated that eight percent of the variation in overall TRF was explained by the set of independent variables (adjusted R2 = 0.081, F (16, 283) = 2.655, p < 0.001). The only variable that made significant contribution (β = 0.951, 95% CI [0.49, 1.42], p < 0.001) to the prediction of TRF was poor medication availability (Table 6).
Qualitative analysis of patients’ and health care workers’ propositions to decrease treatment burden and regimen fatigue
Three major themes were extracted from patients and health care workers propositions on how burden of treatment and regimen fatigue could be ameliorated. (1) Fostering self-care efficacy, (2) Advancing the administrative services of the clinic and the hospital, and (3) Improving the healthcare system provision. Then, subthemes along with excerpts emerged in each key theme (see Supplementary Tables S4 and S5).
Theme 1: fostering self care efficacy
Patients proposed to modify the complexity of treatment regimens and contents of counseling tips as a means of developing self-care efficacy. To this end, one of the participants underscored that:
In the process of patient consultation for HIV patients, awareness campaigns should be incorporated with special emphasis on the topics of stigma and fear of disclosure (P-11).
Consonant to the patient’s perspective, health care workers advocate improving consultation content, providing patient education, establishing formalized patient support group system, and availing fixed-dose combination (FDC) medications to improve self-care management.
Regarding role of patient education, an experienced infectious disease fellow specialist serving in the HIV clinic iterated that:
I think counseling on prescribed medication adherence along with its potential merits outweighs mere prescribing (HCP-2).
Theme 2: advancing the administrative services of the clinic and the hospital
Major issues emphasized by participants to upgrade the administrative services of the clinic or hospital include improving waiting area of the clinics, enhancing medication availability, reducing patient flow, promoting infrequent changing of physicians, and availing functional laboratory tests.
Most patients repeatedly iterated the importance of availing fully functional laboratory tests and hiring qualified laboratory technicians. To this end, one of the participants asserted that:
Surprisingly, crucial laboratory tests like HgbA1c, thyroid function tests, and viral load are unavailable in this big referral hospital causing us to look forward to other high-priced private institutions capable of undergoing these tests (P-12).
In conformity to the above statement, another participant stated that:
The queue for undergoing lab tests is prodigious but the number of working lab technicians are few (usually not more than two). Owing to this, the service provided is quite slow. To overcome this, competent lab technicians should be hired (P-2).
In conformity to the patients’ proposition, health care workers proposed to extend follow-up schedule and improve laboratory services of the hospital. To this end, an experienced endocrine fellow specialist serving in the diabetic clinic underscored as follows:
I heard frequent complaints from patients pertaining to the service provided in the hospital’s laboratory. To surmount this, many competent and well qualified lab technicians should be employed. If possible, because the diabetic clinic is one of the heavily burdened clinics in TASH, it is good to establish a separate lab for the clinic where only DM related tests will be performed (HCP-1).
Theme 3: improving the health care system provision
Patients conceived that the ripest way for boosting health care system provision is via obtaining social support, developing communication skills of non-medical staffs, and strengthening health insurance system. Regarding social support, one participant claimed that:
I believe that social help from a government and/or sponsoring organization in the form of financial aid or job opportunity is a weapon for transforming the health care system (P-3).
As reiterated by the health care workers, establishing a link between health insurance office and Kenema pharmacy, advancing the electronic record (I-Care) system, launching a well-organized health insurance system, and providing financial support have paramount role to upgrade the provision of the health care system.
With respect to the I-care system, one of the nurses who had 10-year work experience in the diabetic clinic asserted that:
The updated I-Care software prescription has no empty space for writing patients’ medical diagnosis and putting prescriber signature. As a result of this, dispensing pharmacists often considered it as incomplete prescription and return patients to respective physician for rectification (HCP-2).
Discussion
This study is the pioneer to explore the treatment burden and regimen fatigue of patients with HIV/AIDS and DM from the perspective of both health care workers and patients in SSA health care context, particularly in Ethiopia, using a mixed method study approach. Unfortunately, quite a few quantitative based-studies are available to compare our results owing to the novelty of conceptualizing and measuring TB and TRF in the aforementioned disease contexts.
The current study finding revealed a mean global TBQ of 28.86 (SD = 22.13). This finding is consonant with the findings of a study conducted in Switzerland (mean = 26.8, SD = 18.6)21. Though the specific disease context is different (heart failure), the finding is consistent with a recent study done in Ethiopia using similar patient-reported outcome measure [TBQ] (mean = 27.2, SD = 19.4)20. Conversely, it is smaller as compared to the studies conducted in USA, Cleveland State, (mean = 37.0, SD = 24.5)22, Australia (mean = 56.5, SD = 34.5)23, Qatar (Median = 40.5, IQR = 38)24, Côte d’Ivoire (mean = 33.3, SD = 19.6)2, and larger than a study done in USA, Ohio State, (mean = 22.8, SD = 24.6)25. The incongruity might be ascribed to the differences in the quality of health care provided, fragmented, and disorganized health care system provision, and varied economic capability. Our study determined the level of TB/TRF solely from the perspective of HIV and diabetic population alone.
In this study, highest level of TB was reported in administrative (mean = 9.05, SD = 9.4), medication (mean = 5.98, SD = 8.2) and social (mean = 5.93, SD = 6.1) domains, while lowest value of TB was displayed by lifestyle change (mean = 4.06, SD = 5.0) and financial (mean = 3.84, SD = 4.2) domains. This finding is incongruent with studies done in Australia23 that reported highest TB on financial, lifestyle, social, administrative, and medication domains, respectively and in Qatar24 that showed highest TB on medication, lifestyle, administrative, social and financial domain, respectively and in Ethiopia20 that showed administrative, financial, lifestyle, social, and medication domains, respectively. The possible reason behind such discrepancies could be attributed to the differences in the quality of the health care provided, disorganized healthcare system, economic factors, and specific disease context.
The present study findings revealed that about 265(88.3%) of participants reported low burden, and only 35(11.7%) indicated high burden. This finding is incongruent to Tran’s et al.26 study, where roughly 47% experienced low, 28% moderate, and 24% high onerousness. Contrary to our finding, Bekalu’ et al.27 recently found moderate (58.9%) to high (26.2%) level of medication related burden and Baah-Nyarkoh et al.28 indicated 69.3% patients as having minimal burden in diabetic patients. The inconsistency could be attributed to variations in the characteristics of the study subjects. For instance, Tran's and Bekalu’s incorporated a large sample comprised of slightly older, and highly educated subjects. The discrepancy could also be colligated to difference on the cut-off value used to label patients as low and high burden. Unlike most previous studies that reckoned TBQ as a continuous variable, ours considered it as dichotomous categorical variable [low vs High] by referring the current scoring interpretation developed by the original developers. Nonetheless, this finding is in keeping with Pedersen et al.29 and Hassen et al.20 studies that revealed 13% and 12% patients exhibited high treatment burden.
With regard to TRF, the finding of this study reported a mean global TRFS of − 42.82 (SD = 17.45). This finding is in conformity with Claborne et al. that reported an overall low level of TRF (mean = − 41.28, SD = 21.08)19. Claborn et al.’ s mean level of TRF was only 2 points greater than the mean observed from the current study.
According to the finding of this study, patients who presented with two and more concurrent illnesses have higher TB compared with their counterparts. This finding is consonant with previous studies by Sav et al.23, Morris et al.30, Al-mansouri et al.24, and Schreiner et al.25 which unveiled that as the number of concurrent illnesses increases the level of treatment onerousness increases proportionally. This is possibly due to the need of polypharmacy, complex treatment regimens, erratic medication taking behavior, and uninterrupted motivation. This study revealed that more intake of prescribed medications (> 5 types) was strongly linked with higher TB. Similar observations were noted in studies by Morris et al., and Hassen et al., which showed that high TB was strongly associated with more prescribed regular medications20,30.
Furthermore, this study unveiled that having sufficient knowledge about DM/HIV and its treatment protocol and availability of medications was strongly associated with lower TB. This finding in agreement with Hassen et al., study20 though the specific disease context is different (DM/HIV vs Heart Failure). Even with differences in disease context, knowledge and medication availability have massive impact for both diseases owing to their chronic nature. Moreover, this finding is consistent with previous qualitative studies31,32.
Regarding TRF, the finding of this study demonstrated that poor availability of medications was significantly associated with TRF of HIV and diabetic patients. This finding is novel because so far, the available studies did not quantitatively examine its association with TRF. However, this finding was supported by previous qualitative studies by Claborne et al.33, and Crowford et al.34, which showed that TRF may be precipitated by the agglomerative effects of treatment, physical, psychosocial, cognitive, and economical-related factors.
As evidenced from the qualitative finding of this study, patients genuinely proposed for boosting self-care efficacy, administrative services of the clinic and/or the hospital, and health care system provision to alleviate and/or prevent the occurrence of TB and TRF. This finding is in line with a previous study by Ting et al., which indicated that patients suggestions to ameliorate treatment onerousness were focused on better provision of health care services and access, and rendering a less burdensome regimen32. Perhaps, this finding is supported by a study by Tran et al. which unveiled that patient proposed to improve personal care and the hospital’s organization and the health care system2. Apparently, the present study found that health care workers perspectives on decreasing TB and TRF strongly aligns with patients’ perspectives, especially concerning to the laboratory set-up and service.
Unfortunately, some of the propositions raised by patients in the current study were comparable as those underscored by patients residing in developed countries though clear difference was noted in terms of the magnitude of their impact on patients’ lives. For example, financial constraints associated with transportation and refilling medications was unbearable in this study and thus most patients emphasized having social and/or financial support and availing of less costly medications. In contrary, in developed countries like France and Chile, health care services are delivered free of charge to ambulatory patients presenting with any chronic diseases. Indeed, the variety of patients and health care workers propositions spotlighted that there is no ‘one-size-fits-all’ approach to minify TB and TRF and healthcare must be tailored to fit each patient’s context.
Finally, this study has some limitations that need to be acknowledged. First, it investigated TB and TRF at a single point in time cross-sectionally. Second, some variables such as smoking habit, disease duration, daily number of pills were obtained directly from patients which may cause social desirability and recall bias. Third, interviewer administration approach was applied to collect the quantitative data using TBQ and TRFS that may eventually lead to social desirability bias. To trim this risk, all data collectors strictly followed the interview protocols and avoided any personal knowledge, beliefs, and influences. Fourth, it was confined to HIV and diabetic patients who could speak Amharic language only and thus may not be generalized to other cultures or countries with other types of chronic medical illnesses. Fifth, the TBQ-15 and TRFS tools were culturally adapted and implemented, however, except internal consistency no further psychometric testing was done.
Conclusion
The findings of this study unveiled that a considerable proportion of patients faced low levels of TB and TRF. Our finding revealed that the presence of two or more comorbidities, daily intake of more than five types of prescribed medications, and disease knowledge were found to have statistically significant associations with high TB. This study also showed that poor medication availability was significantly associated with TRF. The qualitative findings of this study unveiled that fostering self-care efficacy, administrative services of the clinic/hospital, and the health care provision had paramount importance in reducing TB and TRF. Multiple factors that increase TB and TRF should be considered when designing specific healthcare interventions toward HV and diabetic patients to achieve the desired goals of therapy.
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author upon reasonable request.
Abbreviations
- AIDS:
-
Acquired immune deficiency syndrome
- ART:
-
Antiretroviral therapy
- DM:
-
Diabetes mellitus
- FDC:
-
Fixed dose combination
- HIV:
-
Human immune deficiency virus
- MRT:
-
Mapi research trust
- SPSS:
-
Statistical package for social scientists
- TASH:
-
Tikur Anbessa specialized hospital
- TBQ:
-
Treatment burden questionnaire
- TRFS:
-
Treatment regimen fatigue scale
- VIF:
-
Variance inflation factor
References
Sav, A., Salehi, A., Mair, F. S. & McMillan, S. S. Measuring the burden of treatment for chronic disease: Implications of a scoping review of the literature. BMC Med. Res. Methodol. 17(1), 140 (2017).
Tran, V.-T., Messou, E., Djima, M. M., Ravaud, P. & Ekouevi, D. K. Patients’ perspectives on how to decrease the burden of treatment: A qualitative study of HIV care in sub-Saharan Africa. BMJ Qual. Saf. 28(4), 266–275 (2019).
Heckman, B. W., Mathew, A. R. & Carpenter, M. J. Treatment burden and treatment fatigue as barriers to health. Curr. Opin. Psychol. 5, 31–36 (2015).
Gallacher, K. et al. Qualitative systematic reviews of treatment burden in stroke, heart failure and diabetes-methodological challenges and solutions. BMC Med. Res. Methodol. 13(1), 10 (2013).
Mair, F. S. & May, C. R. Thinking about the burden of treatment. BMJ Br. Med. J. 349, g6680 (2014).
Claborn, K. R., Meier, E., Miller, M. B. & Leffingwell, T. R. A systematic review of treatment fatigue among HIV-infected patients prescribed antiretroviral therapy. Psychol. Health Med. 20(3), 255–265 (2015).
Eton, D. T. et al. A systematic review of patient-reported measures of burden of treatment in three chronic diseases. Patient Relat. Outcome Meas. 4, 7 (2013).
Spencer-Bonilla, G., Quiñones, A. R. & Montori, V. M. Assessing the burden of treatment. J. Gen. Intern. Med. 32(10), 1141–1145 (2017).
Sav, A. et al. ‘You say treatment, I say hard work’: Treatment burden among people with chronic illness and their carers in Australia. Health Soc. Care Community 21(6), 665–674 (2013).
Sav, A. et al. Burden of treatment for chronic illness: A concept analysis and review of the literature. Health Expect. 18(3), 312–324 (2015).
Drabe, N. et al. Perception of treatment burden, psychological distress, and fatigue in thyroid cancer patients and their partners–effects of gender, role, and time since diagnosis. Psychooncology 25(2), 203–209 (2016).
Gallacher, K. et al. Uncovering treatment burden as a key concept for stroke care: A systematic review of qualitative research. PLoS Med. 10(6), e1001473 (2013).
Karamanidou, C., Weinman, J. & Horne, R. A qualitative study of treatment burden among haemodialysis recipients. J. Health Psychol. 19(4), 556–569 (2014).
Li, L., Ji, G., Ding, Y., Tian, J. & Lee, A. Perceived burden in adherence of antiretroviral treatment in rural China. AIDS care. 24(4), 502–508 (2012).
Tran, V.-T., Barnes, C., Montori, V. M., Falissard, B. & Ravaud, P. Taxonomy of the burden of treatment: A multi-country web-based qualitative study of patients with chronic conditions. BMC Med. 13(1), 115 (2015).
Gallacher, K., May, C. R., Montori, V. M. & Mair, F. S. Understanding patients’ experiences of treatment burden in chronic heart failure using normalization process theory. Ann. Family Med. 9(3), 235–243 (2011).
Abate, D., Aman, M. A., Nasir, B. B., Gebremariam, G. T. & Fentie, A. M. Assessment of quality of care using information on patient satisfaction at adult oncology center of Tikur Anbessa Specialized Hospital, Ethiopia: A cross-sectional study. Patient Pref. Adher. 14, 847 (2020).
Tran, V.-T. et al. Adaptation and validation of the Treatment Burden Questionnaire (TBQ) in English using an internet platform. BMC Med. 12(1), 109 (2014).
Claborn, K. R., Miller, M. B. & Meier, E. Initial validation of the HIV treatment regimen fatigue scale for adults prescribed antiretroviral therapy. J. Assoc. Nurses AIDS Care. 26(4), 308–315 (2015).
Hassen, M., Mekonnen, D. & Muhammed, O. S. Treatment burden among patients with heart failure attending cardiac clinic of Tikur Anbessa Specialized Hospital: An explanatory sequential mixed methods study. Sci. Rep. 12(1), 18899 (2022).
Herzig, L. et al. Factors associated with patients’ and GPs’ assessment of the burden of treatment in multimorbid patients: A cross-sectional study in primary care. BMC Family Pract. 20(1), 1–11 (2019).
Schreiner, N. & Daly, B. A pilot study exploring treatment burden in a skilled nursing population. Rehabil. Nurs. 45(3), 158 (2020).
Sav, A. et al. Treatment burden and chronic illness: Who is at most risk?. Patient-Patient-Centered Outcomes Res. 9(6), 559–569 (2016).
Al-Mansouri, A. et al. Assessment of treatment burden and its impact on quality of life in dialysis-dependent and pre-dialysis chronic kidney disease patients in Qatar. Res. Soc. Admin. Pharm. 1, 1 (2021).
Schreiner, N., Perazzo, J., Currie, J., Daly, B. & Webel, A. A descriptive, cross-sectional study examining treatment burden in people living with HIV. Appl. Nurs. Res. 46, 31–36 (2019).
Tran, V.-T. et al. Development and description of measurement properties of an instrument to assess treatment burden among patients with multiple chronic conditions. BMC Med. 10(1), 68 (2012).
Bekalu, A. F., Yenit, M. K., Tekile, M. T. & Birarra, M. K. Medication-related burden and associated factors among diabetes mellitus patients at Felege Hiwot Comprehensive Specialized Hospital in northwest Ethiopia. Front. Clin. Diabetes Healthcare. 3, 977216 (2022).
Baah-Nyarkoh, E., Alhassan, Y., Dwomoh, A. K. & Kretchy, I. A. Medicated-related burden and adherence in patients with co-morbid type 2 diabetes mellitus and hypertension. Heliyon. 9(4), 1 (2023).
Pedersen, M. H. et al. Patient-perceived treatment burden: The first study in a general population–Denmark 2017. Eur. J. Public Health. 28(4), 214 (2018).
Morris, J. E. et al. Treatment burden for patients with multimorbidity: Cross-sectional study with exploration of a single-item measure. Br. J. Gen. Pract. 71(706), e381–e390 (2021).
Spencer-Bonilla, G. et al. Patient work and treatment burden in type 2 diabetes: A mixed-methods study. Mayo Clin. Proc. Innov. Qual. Outcomes. 5(2), 359–367 (2021).
Ting, N. C., El-Turk, N., Chou, M. S. & Dobler, C. C. Patient-perceived treatment burden of tuberculosis treatment. Plos One. 15(10), e0241124 (2020).
Claborn, K., Miller, M. B., Meier, E. & Carbone, S. Development of a conceptual etiological model of treatment regimen fatigue among patients engaged in HIV care: A qualitative study. J. Assoc. Nurs. AIDS Care. 28(4), 479–490 (2017).
Crawford, A., Jewell, S., Mara, H., McCatty, L. & Pelfrey, R. Managing treatment fatigue in patients with multiple sclerosis on long-term therapy: The role of multiple sclerosis nurses. Patient Pref. Adher. 8, 1093 (2014).
Acknowledgements
We wish to extend our utmost gratitude to Addis Ababa University for sensitization to develop and support this adaptive problem-solving project. We would also like to sincerely thank all the nurses and medical doctors working in the ambulatory adult HIV and DM clinics of TASH for their warm welcome and unwavering support and their immense cooperation in the data collection process. Lastly, we unfeignedly thank the study participants for their eager involvement in the study.
Funding
This study was funded by Addis Ababa University.
Author information
Authors and Affiliations
Contributions
O.S.M. and M.H. conceptualized and designed the study, wrote the original manuscript, performed analysis and interpretation of data. M.T. and E.B. assisted in the content validation of the data instruments, study design, and manuscript evaluation. All authors have made an intellectual contribution to the work and have approved the final version of the manuscript for submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Muhammed, O.S., Hassen, M., Taye, M. et al. Treatment burden and regimen fatigue among patients with HIV and diabetes attending clinics of Tikur Anbessa specialized hospital. Sci Rep 14, 5221 (2024). https://doi.org/10.1038/s41598-024-54609-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-024-54609-5
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.