Abstract
The expression levels and prognostic role of AP3M2 in colorectal adenocarcinoma (CRAC) have yet to be fully unveiled. Our study comprehensively investigated the clinical significance of AP3M2 in colorectal cancer through an extensive bioinformatics data mining process (TCGA, GEO, GEPIA, Timer, Ualcan, ROCPLOT, and David), followed by experimental validation. We found AP3M2 is a cancer gene, which can be used to distinguish between colorectal cancer and colorectal adenomas, liver metastasis, lung metastasis, colorectal polyp. Higher AP3M2 expression levels were associated with longer overall survival in colon adenocarcinoma. AP3M2 might be the primary biomarker for oxaliplatin in colon cancer and an acquired resistance biomarker for oxaliplatin and 5-fu. AP3M2 was positively associated with CD274, CTLA4. AP3M2 might be associated with T-cell, NF-kappaB transcription factor activity, and response to hypoxia. AP3M2 could predict chemotherapy effectiveness and prognosis for colon cancer patients. AP3M2 might inhibit tumor growth via influencing tumor-infiltrating immune cells in the context of Tumor microenvironment. AP3M2 plays as an oncogene in CRAC and is suggested as a new potential biotarget for therapy.
Similar content being viewed by others
Introduction
Colorectal cancer is a prevalent malignant neoplasm of the digestive system. With the increase in life expectancy and changes in drinking habits among Chinese individuals, both the incidence and mortality rates of colorectal cancer have been steadily rising1. Early detection and identification of novel biomarkers are crucial for effective management. Recently, AP3M2, previously associated with epilepsy and alcoholism2,3,4, has emerged as a potential prognostic marker for colorectal cancer5, It encodes a subunit of heterotetrameric adapter-associated protein complex 3 (AP-3), belonging to the medium subunit family of adaptor complexes involved in protein transport6. However, limited research exists on its specific relevance to colorectal cancer progression.
In this study, we explored the role of AP3M2 in colorectal cancer by using an extensive bioinformatics data mining process to determine the expression of AP3M2 in various cancers. We found the performance of AP3M2 in colon cancer (CC) and rectal cancer (RC) are quite different, to explore the role of AP3M2 gene in the survival, function and structure of CRAC, we used an extensive bioinformatics data mining process by several databases to analyze the clinical role of AP3M2 respectively.
Results
The expression of AP3M2 in colorectal adenocarcinoma (CRAC)
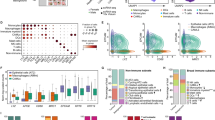
According to TCGA data from the TIMER database, the transcription level of AP3M2 across various cancer types showed statistical significance (p-value < 0.01). In colon cancer tissue, the expression level of AP3M2 was notably higher than in normal colon tissue (median 4.03 vs. 8.25 TPM—transcripts per million, p-value < 1E−12). Similarly, in adjacent tissue to carcinoma in rectal cancer, we observed comparable results (median 4.66 vs. 7.78 TPM, p-value < 7.51E−05). (Fig. 1). According to GSE database, the AP3M2 expression in colon cancer have no statistical significance (p-value < 0.05, |logFC|> 1) in trial results of colonic adenomas, liver metastasis, lung metastasis, colonic polyp. (colonic adenomas: GSE4183, p-value = 2.46E−01; GSE41258, p-value = 0.05; liver metastasis: GSE41258, p-value = 5.39E−01; lung metastasis: GSE41258, p-value = 8.98E−01; colonic polyp: GSE41258, p-value = 5.06E−05, logFC = 0.24; GSE68468, p-value = 1.36E−05, logFC = 3.19E−01). The expression levels of AP3M2 in colon cancer patients of different groups are similar to the expression level of rectal cancer, but they have no significantly relevant with age and gender (Supplemental Fig. 2). The expression level of AP3M2 in stage 1 to 4 colon cancer tissues was higher than that in adjacent normal tissue (stage 1 vs. stage 2 vs. stage 3 vs. stage 4: 7.95 vs. 8.51 vs. 8.42 vs. 7.40). The expression level of AP3M2 was uncorrelated between each stage. Which was also observed in rectal cancer. There were statistical significances in the AP3M2 expression levels between pathologic N0 (median 8.33), N1(median 7.28), N2 (median 9.19), and normal (median 3.94) in colon cancer. The same as rectal cancer (N0 (median 7.59), N1(median 7.27), N2 (median 8.82), and normal (median 4.58)). In addition, there were statistical significances in the AP3M2 expression levels between N1 and N2 in colon cancer (p-value < 0.05). The expression level of AP3M2 in different TP53 mutation status was higher than that in adjacent normal tissues (CC: normal vs. TP53 mutant vs. TP53 non-mutant: 4.03 vs. 8.45 vs. 7.97; RC: normal vs. TP53 mutant vs. TP53 non-mutant: 4.66 vs. 8.58 vs. 7.04). Nevertheless, it is correlated between the expression level of AP3M2 in different TP53 mutation status in rectal cancer while it is irrelevant in colon cancer (p-value < 0.05). (Fig. 2).
The relationship between AP3M2 expression and Tumor types: (a) The transcription level of AP3M2 in various cancer types (TIMER database) (p-value < 0.01). (b) The box plot comparing specific AP3M2 expression in normal (left plot) and colon cancer tissues (right plot) was derived from the ualcan database. (c) (p-value < 1E−12). The box plot comparing specific AP3M2 expression in normal (left plot) and rectal cancer tissue (right plot) was derived from ualcan database. (p-value < 7.51E−05).
The relationship between AP3M2 expression and Clinical features: (a) The box plot comparing specific AP3M2 expression in different stages was derived from ualcan database in colon cancer. (b) The box plot comparing specific AP3M2 expression in different stages was derived from ualcan database in rectal cancer. (c)The box plot comparing specific AP3M2 expression in various pathologic Lymph node stages was derived from ualcan database in colon cancer. (d) The box plot comparing specific AP3M2 expression in various pathologic Lymph node stage was derived from ualcan database in rectal cancer. (e)The box plot comparing specific AP3M2 expression in different TP53 mutation status was derived from ualcan database in colon cancer. (f) The box plot comparing specific AP3M2 expression in different TP53 mutation status was derived from ualcan database in rectal cancer.
The relationship between the transcription level of AP3M2 and prognosis of colorectal adenocarcinoma (CRAC)
The relationship between the expression level of AP3M2 and patient prognosis was investigated in Colonic Neoplasm. It was observed that a higher AP3M2 expression level was significantly associated with unfavorable Overall Survival (OS) in colon cancer (p-value = 0.016, HR: 2), indicating a two-fold higher risk. However, no statistically significant difference was found in rectal adenocarcinoma (Fig. 3). Moreover, overexpression of AP3M2 was correlated with OS but showed no significant correlation with Disease-Free Survival (DFS). These findings suggest that elevated AP3M2 expression may serve as an indicator of poor OS specifically in colon cancer cases.
The relationship between AP3M2 expression and survival: (a) The relationship between AP3M2 expression and OS in colon cancer. (b) The relationship between AP3M2 expression and DFS in colon cancer. (c) The relationship between AP3M2 expression and OS in rectal cancer. (d) The relationship between AP3M2 expression and DFS in rectal cancer.
The expression of AP3M2 between acquired drug-resistant and parental cell lines
The predictive values of AP3M2 in CRAC
Based on the rocplot.plot analysis, in colon cancer patients, the expression level of AP3M2 was found to be higher in non-responders compared to responders who received oxaliplatin (AUC = 0.693, p-value = 2e−03). However, AP3M2 may not serve as a predictive marker for the effectiveness of 5-fluorouracil (AUC = 0.565, p = 0.081) and Irinotecan (AUC = 0.512, p-value = 0.42). Notably, a high level of AP3M2 might be associated with poor treatment response among colon cancer patients receiving oxaliplatin therapy. Conversely, no significant association between AP3M2 expression and drug response was observed among rectal cancer patients treated with oxaliplatin (AUC = 0.580, p-value = 0.230), 5-fluorouracil (AUC = 0.509, p-value = 0.440), or Irinotecan (AUC = 0.643, p-value = 280) (Fig. 4).
The relationship between AP3M2 expression and drug response: (a) The relationship between AP3M2 expression and oxaliplatin in colon cancer. (b) The relationship between AP3M2 expression and 5-fluorouracil in colon cancer. (c) The relationship between AP3M2 expression and Irinotecan in colon cancer. (d) The relationship between AP3M2 expression and oxaliplatin in rectal cancer. (e) The relationship between AP3M2 expression and 5-fluorouracil in rectal cancer. (f) The relationship between AP3M2 expression and Irinotecan in rectal cancer.
The expression of AP3M2 between acquired drug-resistant and parental cell lines
The acquisition of resistance biomarkers for trifluridine (GSE96787, logFC = 0.08, p-value = 0.868), oxaliplatin (GSE10405, logFC = 0.13, p-value = 0.36; GSE42387: HCT116: logFC = 0.10, p-value = 0.24; LoVo: logFC = 0.39, p-value = 5.39e02), BRAF inhibitor (GSE10405: HT29: logFC = 0.52, p-value = 0.29), trifluoro -thymidine (GSE18137: H630: logFC = 0.77, p-value = 0.12) and irinotecan (GSE42387: LoVo: logFC = 0.23, p-value = 0.33; GSE59501: LoVo:log FC = 0.59, p-value = 0.32; GSE42387: HCT116:log FC = 0.l7, p-value = 5.43e−02;G SE4238 HT29: logFC = 0.23, p-value = 6.94e−02) may not be applicable to AP3M2. However, AP3M2 could serve as an acquired resistance biomarker for fluorouracil in Hct-8 cell lines(GSE81008, Hct-8: logFC = 0.40, p-value = 1.99e−03)and oxaliplatin in HT29 cell lines(GSE42B7, HT29: logFC = 0.52, p-value = 9.30e−04).
AP3M2 might influence the prognosis of colon cancer via immune regulation
According to the KEGG7,8,9 and GO enrichment analysis of genes associated with AP3M2 (r > 1 or r < − 1, p-value < 0.05), we identified a potential association between AP3M2 and immune regulation, particularly T-cell immunity. In terms of biological processes, AP3M2 may be involved in T cell activation, lymph node development, positive regulation of NF-kappaB transcription factor activity, and response to hypoxia. Regarding cellular components, AP3M2 may play a role in the T cell receptor complex and alpha–beta T cell receptor complex Α-β. Additionally, the KEGG pathway analysis suggests an association between AP3M2 and the T cell receptor signaling pathway (Fig. 5a).
Among the genes related to T-cell immunity (biological process: GO:0042110, T cell activation; cellular component: GO:0042101, T cell receptor complex; GO:0042105, alpha–beta T cell receptor complex; KEGG pathway: hsa04660, T cell receptor signaling pathway), seven genes (CD3E, CD3G, CD247, CD3D, CD8A, CD8B, ZAP70) were found across all these categories. Furthermore,four genes(CD3E,CD3G,CD247,CD8A) showed significant associations with AP3M2 according to Timer database results(Fig. 5b).
The results from KEGG and GO enrichment analyses regarding AP3M2(r > 1 or r < − 1, p-value < 0.05) in rectal cancer are presented in Fig, 6. There is no evidence suggesting an association with immune-related functions in rectal cancer.
Transcription factors of AP3M2
Through LASAGNA database, we found 86TFs associated with AP3M2, and UCSC database has 4 TFs, the intersection of the TFs are WT1 (p-value = 5.00E−05), CTF (p-value = 6.75E−04), TBP (p-value = 5.00E−05), NF-Y (p-value = 5.00E−05).
AP3M2 in tumor-infiltrating immune cells in CRAC
In order to reveal the relationship between AP3M2 and immune regulation in colon cancer, we then explore the gene and immune cell infiltration through TIMER database. AP3M2 was positively associated with CD8+ T cells (r = 0.14), CD4+ T cells (r = 0.16), Neutrophil cells (r = 0.22), B cells (r = 0.16), NK cells (r = 0.13), Tregs cells (r = 0.18), Monocyte cells(r = 0.28), macrophage M0 cells(r = 0.12), macrophage M1 cells (r = 0.23), macrophage M2 cells(r = 0.26), myeloid-derived suppressor cells(r = 0.16), but negatively associated with B cell memory (r = − 0.15), B cell plasma(r = − 0.13) (Fig. 7).
AP3M2 in tumor-infiltrating immune cells in colon cancer: (a) The relationship between AP3M2 and CD4+ T cells. (b) the relationship between AP3M2 and CD8+ T cells. (c) the relationship between AP3M2 and Neutrophil cell. (d) the relationship between AP3M2 and B cells. (e) the relationship between AP3M2 and NK cells. (f) The relationship between AP3M2 and Tregs cells. (g) The relationship between AP3M2 and Monocyte cells. (h) The relationship between AP3M2 and macrophage M0 cells. (i) The relationship between AP3M2 and macrophage M1 cells. (j) The relationship between AP3M2 and macrophage M2 cells. (k) The relationship between AP3M2 and myeloid-derived suppressor cells.
We also explore the gene and immune cell infiltration in rectal cancer through TIMER database. AP3M2 was positively associated with CD8+ T cells (r = 0.24), CD4+ T cells (r = 0.23), Monocyte cells (r = 0.35), macrophage M0 cells (r = 0.26), macrophage M2 cells (r = 0.24), myeloid-derived suppressor cells(r = 0.25), but negatively associated with B cell memory (r = − 0.22), B cell plasma(r = − 0.23) and not related with NK cell, Neutrophil cell, Tregs cell, macrophage M1 cell, B cell. (Fig. 8).
AP3M2 in tumor-infiltrating immune cells in rectal cancer: (a) the relationship between AP3M2 and CD4+ T cells. (b) The relationship between AP3M2 and CD8+ T cells. (c) The relationship between AP3M2 and Neutrophil cells. (d) The relationship between AP3M2 and B cells. (e) The relationship between AP3M2 and NK cell. (f) The relationship between AP3M2 and Tregs cells. (g) The relationship between AP3M2 and Monocyte cell. (h) The relationship between AP3M2 and macrophage M0 cells. (i) the relationship between AP3M2 and macrophage M1 cells. (j) The relationship between AP3M2 and macrophage M2 cells. (k) The relationship between AP3M2 and myeloid-derived suppressor cells.
The relationship of AP3M2 and other genes
Then we investigated genes associated with immune response through TIMER database, we found AP3M2 was positively related with FOXP3(r = 0.18), CD72(r = 0.16), RUNX1(r = 0.33), LAG3(r = 0.19), CTLA4(r = 0.24) PD-L1(CD274) (r = 0.27), CD20(MS4A1) (r = 0.13), PD1(CD279, PDCD1) (r = 0.15) and irrelated with CD19 in colon cancer. However, AP3M2 have no relationship with these genes except CD274(r = 0.33), RUNX1(r = 0.22), CTLA4(r = 0.27) in rectal cancer. (Figs. 9, 10).
Relationship of AP3M2 expression and other genes in colon cancer: (a) The relationship of AP3M2 expression and FOXP3. (b) The relationship of AP3M2 expression and CD72. (c) The relationship of AP3M2 expression and RUNX1. (d) The relationship of AP3M2 expression and LAG3. (e) The relationship of AP3M2 expression and CTLA4. (f) The relationship of AP3M2 expression and PD-L1. (g) The relationship of AP3M2 expression and CD20. (h) The relationship of AP3M2 expression and PD1. (i) The relationship of AP3M2 expression and CD19.
Relationship of AP3M2 expression and other genes in rectal cancer: (a) The relationship of AP3M2 expression and FOXP3. (b) The relationship of AP3M2 expression and CD72. (c) The relationship of AP3M2 expression and RUNX1. (d) The relationship of AP3M2 expression and LAG3. (e) The relationship of AP3M2 expression and CTLA4. (f) The relationship of AP3M2 expression and PD-L1. (g) The relationship of AP3M2 expression and CD20. (h) The relationship of AP3M2 expression and PD1. (i) The relationship of AP3M2 expression and CD19.
Moreover, we investigated the relationship between AP3M2 and ABCG2, which was confirmed the energetic association with oxaliplatin resistance. The relationship between AP3M2 and ABCG2 was positive in colon cancer (r = 0.12) and rectal cancer (r = 0.18). (Fig. 11).
The expression of AP3M2 in colon cancer samples and adjacent normal tissues.
Real-time PCR was used to assess the expression of AP3M2 in colon cancer
samples and adjacent normal tissues. The level of AP3M2 expression was higher in the tumor group compared to the normal group (p < 0.05) (Fig. 12).
Discussion
Diseases associated with AP3M2 include Farber Lipogranulomatosis and Generalized Epilepsy With Febrile Seizures Plus10. Several studies showed that AP3M2 lends credence to a functional role in alcohol preference and withdrawal through GABAergic transmission4,11,12. Few studies reveal its role in in tumorigenesis. AP3M2 plays different roles in various cancers, it is an oncogene in Breast invasive carcinoma, Cholangiocarcinoma, Stomach adenocarcinoma, Colon adenocarcinoma, Rectum adenocarcinoma, Esophageal carcinoma, Head and Neck squamous cell carcinoma, Liver hepatocellular carcinoma and Lung squamous cell carcinoma. Meanwhile, it plays an antioncogene role in Glioblastoma multiforme, Kidney Chromophobe and Thyroid carcinoma13,14.In our study, enhanced expression of AP3M2 predicts poor prognosis in patients with colon adenocarcinoma, but not rectal adenocarcinoma. Furthermore, AP3M2 might not be some clinic factor such as different stages, age groups, or gender of colorectal cancer. as well as prognostic in rectal cancer. But it is a prognostic biomarker for colon cancer. At the same time, AP3M2 seems can be a biomarker between colon cancer and colonic adenomas, liver metastasis, lung metastasis, colonic polyp. Available databases such as TCGA, GEO do not provide data on gene expression between rectal cancer and other rectal diseases,which prevents “validation” of our findings with clinical samples.
In the last 15 years, a significant progress in the management of CRC was achieved with several new agents licensed (irinotecan, oxaliplatin, capecitabine, bevacizumab, cetuximab and panitumumab)15,16. The chemotherapy agents of choice for adjuvant treatment of colorectal cancer with stage higher than T3N0M0 after resection are 5-fluorouracil (5-FU) and oxaliplatin. In the case of metastatic colorectal cancer (mCRC), oxaliplatin and irinotecan are considered as the most significant cytotoxic compounds17,76,19.
Resistance to oxaliplatin chemotherapy has become a significant cause for treatment failure and CRC-related death20. In our study, AP3M2 was found to be associated with oxaliplatin response in colon cancer. Moreover, we observed an association between AP3M2 and the NF-κB Signaling Pathway with a positive regulation. Studies have revealed NF-κB as one of the stem cell regulatory pathways frequently dysregulated in tumor cells, participating in the regulation of inflammation and leading to chemoresistance against anti-cancer drugs. One of the crucial factors in oxaliplatin resistance is NF-κB via autocrine signaling through IL-1 and IL-821,19,23. These findings suggest that AP3M2 could indicate oxaliplatin resistance through the NF-κB Signaling Pathway. Besides, overexpression of ABCG2 in oxaliplatin-resistant cells aims to escape from apoptosis induced by Hsi-Hsien Hsu24. AP3M2 expression is positively associated with ABCG2 in our study, we hypothesized that AP3M2 might affect the expression of ABCG2 in some way, influencing the acquired drug resistance of Oxaliplatin. However, oxaliplatin seems to induce immunogenic signals on the surface of cancer cells before apoptosis, triggering interferon-gamma production and interaction with toll-like receptor 4 on dendritic cells, resulting in the immunogenic death of cancer cells25. This contradicts our conclusion that the overexpression of AP3M2 is positively associated with dendritic cell infiltration in colon adenocarcinoma.
Tumor-infiltrating immune cells (TICs) in the context of tumor microenvironment (TME) are closely associated with clinical outcomes and can regulate tumor development in some way26 The promotion of tumor cell proliferation, growth and survival could be triggered by cytokines produced by immune cells27. Previous studies revealed that M2 macrophages exhibited pro-tumoral effects through interacting with with various cells, including T helper 2 cells, cancer-associated fibroblasts, cancer cells, regulatory T cells (Tregs), plasmacytoid dendritic cells, and myeloid-derived suppressor cells28. This further explains that AP3M2 is positively correlated with M2 macrophage levels and myeloid-derived suppressor cells in CRAC in our study. On the other hand, our studies revealed that AP3M2 is related with response to hypoxia, Tumor-tissue hypoxia can convert M1 macrophages to M2 macrophages29. Moreover, AP3M2 overexpression in colorectal adenocarcinoma can also increase the amount of immunosuppressive cells, such as regulatory T cells (Treg) and medullary inhibitory cells, to evade immune surveillance, the numbers of these immunosuppressive cells are closely related to a poor prognosis30,31. Recent advances in the field32 of tumor immunology reveals that Tregs are believed to promote tumor development by inefficient activation of the immune system against tumor cells. FOXP333,34, CD7235,36, RUNX137, LAG338, CTLA439,40 are related to Tregs in the presence of effector cells and contribute to their suppressive activity, suggesting that depletion of Tregs is believed to be a valid therapeutic approach in many cancer types. In our study, FOXP3(r = 0.179), CD72(r = 0.155), RUNX1(r = 0.327), LAG3(r = 0.194), CTLA4(r = 0.236) have a positive correlation with AP3M2 in Colon Neoplasm, but no irrelevancy in rectal tumor. Immune check point inhibitors with early Treg depletion might represent an effective strategy for the therapy of Colon Neoplasm32, and AP3M2 might be worth considering. This explains the different prognosis of AP3M2 in colon and rectal cancer.
The quantity of the immune infiltrate is crucial for mounting an efficient antitumor response. In this regard, the transcriptional level of key genes involved in T cell, and B cell function may reveal deregulation41.We identified hub genes (CD3E, CD3G, CD247, CD8A, CD19, CD20(MS4A1),CTLA4,CD279) that were possibly synclastic related to AP3M2 and contribute to the immune response in Colonic Neoplasm. Studies have shown that the expression of CD3G, CD8A, CD19, MS4A1 is related to immune system activation and significantly associated with prognostic factors or disease survival42,40,41,42,46. These genes play a possible role in immune-mediated pathways to achieve the elimination of neoplastic cells, affecting the prognosis47. On the contrary, CTLA4 (Cytotoxic T lymphocyte antigen 4, CD152), PD1 (programmed cell death 1, CD279) receptors on the surface of activated T cells inhibit the activation of T cells by interacting with their ligands48,46,47,51. CD4+ memory activated and resting T cells and Tregs were negatively correlated with CD3E41. This supports the idea that AP3M2 affects prognosis through influencing the immune response. More notably, AP3M2 is independent of Immune Regulation in rectal cancer, which explains the different prognosis manifestation in the rectum instead.
Programmed death-ligand 1 (PD-L1, also known as B7-H1 and CD274) is one of the most critical immune checkpoints in CRAC. The binding of programmed cell death protein 1 (PD-1) and its ligand PD-L1 plays a negative regulatory role in the activation of T cells52,53. Previous studies have demonstrated that PD-L1 is overexpressed in various cancers including CRC54,55. PD-L1 expression is associated with a poor prognosis and inhibits cell proliferation56, migration, and invasion in CRC57. Besides, PDL1 may regulate immune-independent and intrinsic functions of tumor cells that include tumor cell apoptosis and autophagy58,59. Simultaneously, according to the current literature, the expression of PD-L1 is regulated by hypoxia-inducible factor-1 (HIF-1), which could bind to hypoxic response element (HRE) and upregulate the PD-L1 expression, simultaneously cause T-cell apoptosis and function inhibition60,61. NF-kB was also important transcription factors upregulating PD-L162,60,64. NK cell infiltration induces the expression of immune checkpoints such as PD‐1 with upregulated Th1 lymphocyte and cytotoxic T cell65. In our study, AP3M2 was found to be positively related to PD-L1(CD274), hypoxic response, NF-kB pathway, and NK cell infiltration in colorectal adenocarcinoma. Therefore, we speculate that AP3M2 plays a possible role in colorectal cancer immunotherapy.
Our study comprehensively analyzed the role of AP3M2 in colorectal adenocarcinoma, incorporating data from both TCGA and GEO. Nevertheless, our study has inherent limitations: first, all analyses were based on RNA sequence data. Second, population heterogeneity might exist across different datasets in this study. The absence of in vivo and in vitro experiments to validate our findings should be noted. Further research is warranted to investigate how AP3M2 affects drug effectiveness and colon cancer prognosis.
We hypothesize that AP3M2 functions as an oncogene in CRAC. AP3M2 could potentially predict chemotherapy effectiveness and prognosis for colon cancer patients. Moreover, AP3M2 might inhibit tumor growth by influencing tumor-infiltrating immune cells (TICs) in the context of the tumor microenvironment (TME). It is suggested as a novel potential biotarget for therapy.
Methods
Statistical analysis
Significance was defined as a p-value < 0.05 for gene expression, survival analysis, and protein–protein network relations.
Patients and data collection
Difference gene expression and clinical material of CRAC patients were downloaded from the TCGA database. Subsequently, the expression data were utilized to analyze mRNA expression levels in cancer tissue compared to normal tissue. (supplemental Fig. 1).
GEPIA, timer and ualcan database analysis
The transcription level of AP3M2 gene was identified by ualcan database (http://ualcan.path.uab.edu/index.html)66 and Timer database(http://timer.comp-genomics.org/)13,14,67 The relationship between AP3M2 expression and survival in CRAC was analyzed by GEPIA database (https://www.gepia.cancer-pku.cn/)68. The Promoter Methylation level of AP3M2 was also identified by ualcan database. Furthermore, the relationship between AP3M2 and immune regulation was identified by TIMER database.
ROC plot database analysis and GEO database
ROCPLOT database (http://www.rocplot.org/user/login)69 was used to analyze the predictive values of different drugs and the prognostic value of AP3M2 in CRAC. GEO database was used to analyze The Expression of AP3M2 between Acquired Drug-Resistant and Parental Cell Lines.
David database analysis
KEGG and GO enrichment analysis about AP3M2 was analyzed by David database (https://david.ncifcrf.gov/)70,71.
Other online database analysis
Transcription Factors of AP3M2 was found by LASAGNA database (https://biogrid-lasagna.engr.uconn.edu/)72, USSC database (http://genome.ucsc.edu/)73,miRDB database(http://mirdb.org/)74, targetscan database (http://www.targetscan.org/)75,76 and miRWalk database (http://mirwalk.umm.uni-heidelberg.de/) Other genes that might be associated with AP3M2 were explored using Cytoscape77based on available public databases.
Clinical specimen collection and ethics approval
Colon cancer samples and normal tissues were acquired from the Seventh Affiliated Hospital of Sun Yat-sen University. Ethical approval for this study was obtained from the Sun Yat-sen University Health Science Institution Review Board (No. KY-2022–051-02). Samples were collected for real-time PCR.
Ethics statement
Research have been performed in accordance with the Declaration of Helsinki. All methods were performed in accordance with the relevant guidelines and regulations. All patients provided their informed consent in writing preoperatively.
Real-time PCR analysis
Total RNA was extracted from colon cancer and adjacent normal tissues using AG RNAex Pro RNA reagent (Accurate Biology, CAT#AG21102) according to the manufacturer's instructions. cDNA was synthesized using the Evo M-MLV reverse transcription Master Mix (Accurate Biology, CAT# AG11706). RT-qPCR was performed with a SYBR Green Pro Tag HS premixed qPCR kit (Accurate Biology, CAT# AG11701). The relative expression of total RNA was calculated using the 2-ΔΔCt method. The primer sequences for all the RNAs used for qPCR are recorded in Supplementary Table 1.
Data availability
The datasets presented in this study can be found in online repositories. The names of the repository/repositories and accession number(s) can be found in the article/Supplementary Material.
References
Siegel, R. L., Miller, K. D. & Jemal, A. Cancer statistics, 2020. CA Cancer J. Clin. 70(1), 7–30 (2020).
Huang, M.-C. et al. Mutation screening of AP3M2 in Japanese epilepsy patients. Brain Dev. 29(8), 462–467 (2007).
Sullivan, S. E. et al. Candidate-based screening via gene modulation in human neurons and astrocytes implicates FERMT2 in Aβ and TAU proteostasis. Hum. Mol. Genet. 28(5), 718–735 (2019).
Bubier, J. A. et al. Identification of a QTL in Mus musculus for alcohol preference, withdrawal, and Ap3m2 expression using integrative functional genomics and precision genetics. Genetics 197(4), 1377–1393 (2014).
Cui, M. et al. Screening of biomarkers associated with diagnosis and prognosis of colorectal cancer. Genes Genet. Syst. 97(3), 101–110 (2022).
Stelzer, G. et al. The GeneCards suite: From gene data mining to disease genome sequence analyses. Current Protoc. Bioinform. 54, 1–30 (2016).
Kanehisa, M. & Goto, S. KEGG: Kyoto encyclopedia of genes and genomes. Nucleic Acids Res. 28(1), 27–30 (2000).
Kanehisa, M. Toward understanding the origin and evolution of cellular organisms. Protein Sci. Publ. Protein Soc. 28(11), 1947–1951 (2019).
Kanehisa, M. et al. KEGG for taxonomy-based analysis of pathways and genomes. Nucleic Acids Res. 51(D1), D587–D592 (2023).
Rappaport, N. et al. MalaCards: An amalgamated human disease compendium with diverse clinical and genetic annotation and structured search. Nucleic Acids Res. 45(D1), D877–D887 (2017).
Nakatsu, F. et al. Defective function of GABA-containing synaptic vesicles in mice lacking the AP-3B clathrin adaptor. J. Cell Biol. 167(2), 293–302 (2004).
Misawa, H. et al. Aberrant trafficking of the high-affinity choline transporter in AP-3-deficient mice. Eur. J. Neurosci. 27(12), 3109–3117 (2008).
Li, T. et al. TIMER: A web server for comprehensive analysis of tumor-infiltrating immune cells. Cancer Res. 77(21), e108–e110 (2017).
Li, T. et al. TIMER2.0 for analysis of tumor-infiltrating immune cells. Nucleic Acids Res. 48(W1), W509–W514 (2020).
Schmiegel, W. et al. Colorectal carcinoma: The management of polyps, (neo)adjuvant therapy, and the treatment of metastases. Deutsch. Arztebl. Int. 106(51–52), 843–848 (2009).
Rosen, A. W., Degett, T. H. & Gögenur, I. Individualized treatment of colon cancer. Ugeskrift Laeger 178(31), V11150916 (2016).
Colorectal cancer. The Lancet 394(10207), 1467–1480. https://doi.org/10.1016/S0140-6736(19)32319-0 (2019).
Colon cancer version 2.2021 NCCN clinical practice guidelines in oncology. J. Natl. Compr. Canc. Netw. 19(3) 329–359. https://doi.org/10.6004/jnccn.2021.0012 (2021).
Rectal Cancer Version 2.2022 NCCN Clinical Practice Guidelines in Oncology. JJ. Natl. Compr. Canc. Netw. 20(10), 1139–1167. https://doi.org/10.6004/jnccn.2022.0051 (2022).
Zhou, W. et al. Thioredoxin domain-containing protein 9 (TXNDC9) contributes to oxaliplatin resistance through regulation of autophagy-apoptosis in colorectal adenocarcinoma. Biochem. Biophys. Res. Commun. 524(3), 582–588 (2020).
Iliopoulos, D., Hirsch, H. A. & Struhl, K. An epigenetic switch involving NF-kappaB, Lin28, Let-7 MicroRNA, and IL6 links inflammation to cell transformation. Cell 139(4), 693–706 (2009).
Abdullah, L. N. & Chow, E.K.-H. Mechanisms of chemoresistance in cancer stem cells. Clin. Transl. Med. 2(1), 3 (2013).
Wilson, C. et al. Chemotherapy-induced CXC-chemokine/CXC-chemokine receptor signaling in metastatic prostate cancer cells confers resistance to oxaliplatin through potentiation of nuclear factor-kappaB transcription and evasion of apoptosis. J. Pharmacol. Exp. Ther. 327(3), 746–759 (2008).
Hsu, H.-H. et al. Oxaliplatin resistance in colorectal cancer cells is mediated via activation of ABCG2 to alleviate ER stress induced apoptosis. J. Cell. Physiol. 233(7), 5458–5467 (2018).
Tesniere, A. et al. Immunogenic death of colon cancer cells treated with oxaliplatin. Oncogene 29(4), 482–491 (2010).
Fridman, W. H. et al. The immune contexture in human tumours: impact on clinical outcome. Nat. Rev. Cancer 12(4), 298–306 (2012).
Markman, J. L. & Shiao, S. L. Impact of the immune system and immunotherapy in colorectal cancer. J. Gastrointest. Oncol. 6(2), 208–223 (2015).
Najafi, M. et al. Macrophage polarity in cancer: A review. J. Cell. Biochem. 120(3), 2756–2765 (2019).
Lewis, C. & Murdoch, C. Macrophage responses to hypoxia: Implications for tumor progression and anti-cancer therapies. Am. J. Pathol. 167(3), 627–635 (2005).
Hanahan, D. & Weinberg, R. A. Hallmarks of cancer: The next generation. Cell 144(5), 646–674 (2011).
Diaz-Montero, C. M. et al. Increased circulating myeloid-derived suppressor cells correlate with clinical cancer stage, metastatic tumor burden, and doxorubicin-cyclophosphamide chemotherapy. Cancer Immunol. Immunother. CII 58(1), 49–59 (2009).
Fantini, M. C. et al. Tumor infiltrating regulatory T cells in sporadic and colitis-associated colorectal cancer: The red little riding hood and the wolf. Int. J. Mol. Sci. 21(18), 6744 (2020).
Fontenot, J. D., Gavin, M. A. & Rudensky, A. Y. Foxp3 programs the development and function of CD4+CD25+ regulatory T cells. Nat. Immunol. 4(4), 330–336 (2003).
Hori, S., Nomura, T. & Sakaguchi, S. Control of regulatory T cell development by the transcription factor Foxp3. Science (New York, N.Y.) 299(5609), 1057–1061 (2003).
Allard, B. et al. The ectonucleotidases CD39 and CD73: Novel checkpoint inhibitor targets. Immunol. Rev. 276(1), 121–144 (2017).
Sundström, P. et al. Regulatory T cells from colon cancer patients inhibit effector T-cell migration through an adenosine-dependent mechanism. Cancer Immunol. Res. 4(3), 183–193 (2016).
Ono, M. et al. Foxp3 controls regulatory T-cell function by interacting with AML1/Runx1. Nature 446(7136), 685–689 (2007).
Yan, Y. et al. IDO upregulates regulatory T cells via tryptophan catabolite and suppresses encephalitogenic T cell responses in experimental autoimmune encephalomyelitis. J. Immunol. (Baltimore, Md.: 1950) 185(10), 5953–5961 (2010).
Qureshi, O. S. et al. Trans-endocytosis of CD80 and CD86: A molecular basis for the cell-extrinsic function of CTLA-4. Science (New York, N.Y.) 332(6029), 600–603 (2011).
Walker, L. S. K. & Sansom, D. M. Confusing signals: recent progress in CTLA-4 biology. Trends Immunol. 36(2), 63–70 (2015).
Sivan, A. et al. Commensal bifidobacterium promotes antitumor immunity and facilitates anti-PD-L1 efficacy. Science (New York, N.Y.) 350(6264), 1084–1089 (2015).
Tagliabue, M. et al. A role for the immune system in advanced laryngeal cancer. Sci. Rep. 10(1), 18327 (2020).
West, N. R. et al. Tumor-infiltrating lymphocytes predict response to anthracycline-based chemotherapy in estrogen receptor-negative breast cancer. Breast Cancer Res. BCR 13(6), R126 (2011).
Leonard, B. et al. APOBEC3G expression correlates with T-cell infiltration and improved clinical outcomes in high-grade serous ovarian carcinoma. Clin. Cancer Res. Off. J. Am. Assoc. Cancer Res. 22(18), 4746–4755 (2016).
Lin, Z. et al. Tumor infiltrating CD19 B lymphocytes predict prognostic and therapeutic benefits in metastatic renal cell carcinoma patients treated with tyrosine kinase inhibitors. Oncoimmunology 7(10), e1477461 (2018).
Wang, M., Windgassen, D. & Papoutsakis, E. T. Comparative analysis of transcriptional profiling of CD3+, CD4+ and CD8+ T cells identifies novel immune response players in T-cell activation. BMC Genomics 9, 225 (2008).
Reshetnikova, E. et al. B cell-specific protein FCRLA is expressed by plasmacytoid dendritic cells in humans. Cytom. Part B Clin. Cytom. 94(4), 683–687 (2018).
Kishore, C. & Bhadra, P. Current advancements and future perspectives of immunotherapy in colorectal cancer research. Eur. J. Pharmacol. 893, 173819 (2021).
Buchbinder, E. I. & Desai, A. CTLA-4 and PD-1 pathways: Similarities, differences, and implications of their inhibition. Am. J. Clin. Oncol. 39(1), 98 (2016).
Rowshanravan, B., Halliday, N. & Sansom, D. M. CTLA-4: A moving target in immunotherapy. Blood 131(1), 58–67 (2018).
Mizuno, R. et al. PD-1 primarily targets TCR signal in the inhibition of functional T cell activation. Front. Immunol. 10, 630 (2019).
Michel, M. et al. The role of p53 dysfunction in colorectal cancer and its implication for therapy. Cancers 13(10), 2296 (2021).
Iwai, Y. et al. Involvement of PD-L1 on tumor cells in the escape from host immune system and tumor immunotherapy by PD-L1 blockade. Proc. Natl. Acad. Sci. U. S. A. 99(19), 12293–12297 (2002).
Enwere, E. K. et al. Expression of PD-L1 and presence of CD8-positive T cells in pre-treatment specimens of locally advanced cervical cancer. Mod. Pathol. 30(4), 577–586 (2017).
Lee, K. S. et al. Prognostic relevance of programmed cell death ligand 1 expression in glioblastoma. J. Neuro-oncol. 136(3), 453–461 (2018).
Zhang, M. et al. Cancer-associated fibroblasts promote cell growth by activating ERK5/PD-L1 signaling axis in colorectal cancer. Pathol. Res. Pract. 216(4), 152884 (2020).
Shi, S.-J. et al. B7–H1 expression is associated with poor prognosis in colorectal carcinoma and regulates the proliferation and invasion of HCT116 colorectal cancer cells. PloS ONE 8(10), e76012 (2013).
Azuma, T. et al. B7–H1 is a ubiquitous antiapoptotic receptor on cancer cells. Blood 111(7), 3635–3643 (2008).
Clark, C. A. et al. Tumor-intrinsic PD-L1 signals regulate cell growth, pathogenesis, and autophagy in ovarian cancer and melanoma. Cancer Res. 76(23), 6964–6974 (2016).
Barsoum, I. B. et al. A mechanism of hypoxia-mediated escape from adaptive immunity in cancer cells. Cancer Res. 74(3), 665–674 (2014).
Noman, M. Z. et al. PD-L1 is a novel direct target of HIF-1α, and its blockade under hypoxia enhanced MDSC-mediated T cell activation. J. Exp. Med. 211(5), 781–790 (2014).
Ju, X. et al. Regulation of PD-L1 expression in cancer and clinical implications in immunotherapy. Am. J. Cancer Res. 10(1), 1 (2020).
Gao, Y. et al. Cancer-associated fibroblasts promote the upregulation of PD-L1 expression through Akt phosphorylation in colorectal cancer. Front. Oncol. 11, 748465 (2021).
Cortez, M. A. et al. PDL1 regulation by p53 via miR-34. J. Natl. Cancer Inst. 108(1), djv303 (2016).
Payandeh, Z. et al. PD-1/PD-L1-dependent immune response in colorectal cancer. Journal Cell. Physiol. 235(7–8), 5461–5475 (2020).
Lujan, H. J. et al. Advantages of robotic right colectomy with intracorporeal anastomosis. Surg. Laparosc. Endosc. Percutan Tech. 28(1), 36–41 (2018).
Li, B. et al. Comprehensive analyses of tumor immunity: Implications for cancer immunotherapy. Genome Biol. 17(1), 174 (2016).
Tang, Z. et al. GEPIA: a web server for cancer and normal gene expression profiling and interactive analyses. Nucleic Acids Res. 45(W1), W98 (2017).
Fekete, J. T. & Győrffy, B. ROCplot.org: Validating predictive biomarkers of chemotherapy/hormonal therapy/anti-HER2 therapy using transcriptomic data of 3104 breast cancer patients. Int. J. Cancer 145(11), 3140–3151 (2019).
Huang, D. W., Sherman, B. T. & Lempicki, R. A. Bioinformatics enrichment tools: paths toward the comprehensive functional analysis of large gene lists. Nucleic Acids Res. 37(1), 1–3 (2009).
Huang, D. W., Sherman, B. T. & Lempicki, R. A. Systematic and integrative analysis of large gene lists using DAVID bioinformatics resources. Nat. Protoc. 4(1), 44–57 (2009).
Lee, C. & Huang, C.-H. LASAGNA-search: An integrated web tool for transcription factor binding site search and visualization. BioTechniques 54(3), 141–153 (2013).
Navarro Gonzalez, J. et al. The UCSC genome browser database: 2021 update. Nucleic Acids Res. 49(D1), D1046–D1057 (2021).
Chen, Y. & Wang, X. miRDB: An online database for prediction of functional microRNA targets. Nucleic Acids Res. 48(D1), D127–D131 (2020).
Lewis, B. P. et al. Prediction of mammalian microRNA targets. Cell 115(7), 787–798 (2003).
Lewis, B. P., Burge, C. B. & Bartel, D. P. Conserved seed pairing, often flanked by adenosines, indicates that thousands of human genes are microRNA targets. Cell 120(1), 15–20 (2005).
Shannon, P. et al. Cytoscape: A software environment for integrated models of biomolecular interaction networks. Genome Res. 13(11), 2498–2504 (2003).
Acknowledgements
We thank the public databases, including GEPIA, Timer, Ualcan, ROCPLOT, and David, for providing open access.
Author information
Authors and Affiliations
Contributions
Q.J. and Y.K. designed this study. Q.J. and J.F. extracted the information from the databases and analyzed the data. Y.K. and Y.Y. supervised the entire study. Y.Y. finished the experimental part. Qianqian Jin and Yong Kuang wrote the manuscript. All authors contributed to the article and approved the submitted version.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Jin, Q., Feng, J., Yan, Y. et al. Prognostic and immunological role of adaptor related protein complex 3 subunit mu2 in colon cancer. Sci Rep 14, 483 (2024). https://doi.org/10.1038/s41598-023-50452-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-023-50452-2
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.