Abstract
The tumour suppressor gene, TES, is frequently methylated in many human tumours. Previously, we demonstrated that TES promoter methylation and transcriptional silencing was the most common molecular abnormality detected in childhood acute lymphoblastic leukaemia (ALL). Trp53-mutant mouse models predominantly develop B- and T-cell lymphomas, which are widely considered equivalent to childhood T and B ALL. In this study, we examined expression of Tes transcript and Testin protein in spontaneous tumours obtained from three Trp53-mutant mouse models. Using immunohistochemistry, we report that 47% of lymphomas lacked Testin protein compared to only 7% of non-lymphoid tumours. Further examination of the lymphomas from Trp53-null and Trp53-mΔpro homozygous mutant mice revealed that 63% and 69% respectively of the isolated lymphomas were Testin negative, which is similar to reported rates in childhood T-ALL. Surprisingly, lymphomas from Trp53-Δ122 mice were frequently Testin positive (> 60%), suggesting that the presence of the Trp53-Δ122 protein appeared to mitigate the requirement for Tes silencing in lymphomagenesis. Quantitative RT-PCR results confirmed that this lack of Testin protein was due to Tes transcriptional silencing, although bisulfite sequencing demonstrated that this was not due to promoter methylation. These results are consistent with the Testin protein having lymphoid tumour suppressor activity in both mice and humans.
Similar content being viewed by others
Introduction
Silencing of the TES gene is emerging as a common event during tumourigenesis with loss of TESTIN protein observed in many tumours, including glioblastoma1,2,3, gastric4, uterine5, ovarian6, prostate7 and breast5,8. Loss of TESTIN protein is predominantly the result of promoter methylation, with mutations of the TES coding sequence rarely reported. Previously, we reported that TES promoter methylation was a common event across all subtypes of childhood acute lymphoblastic leukaemia (ALL) and that dense, biallelic methylation of the TES promoter results in loss of transcription and absence of TESTIN protein9. In addition, re-expression of TESTIN in human ALL cell lines and other cancer cell lines resulted in suppression of anti-apoptotic proteins and induction of pro-apoptotic proteins10, resulting in increased cell death1,8,10,11,12,13,14, thus adding support for TES to be considered a tumour suppressor gene.
The high prevalence and clonal nature of TES silencing in paediatric ALL strongly suggests that TES silencing is either an early event or an epigenetic driver of leukaemia development. In this study, we investigated the role of TES expression in spontaneous tumours isolated from tumour-prone, Trp53-mutant mice. TP53 is a tumour suppressor that regulates the expression of multiple target genes and thereby can induce cell cycle arrest, DNA repair, apoptosis, senescence, or changes in metabolism in response to cellular stress15. TP53 gene mutations are common in human cancers and haematological neoplasms16. Trp53-mutant mice are susceptible to spontaneous T- or B-cell lymphomas development17,18,19, which are widely considered equivalent to childhood T and B ALL20. Of the three mouse models, the Trp53-null mice are unable to produce Trp53 protein and die rapidly, predominantly from T (56%) or B cell (18%) lymphomas21. The Trp53mΔpro mice produce a mutant Trp53 protein without the proline-rich domain (amino acids 58–88) and have a reduced lifespan compared to wild-type mice, succumbing to B-cell lymphomas (50%), osteosarcomas and T-cell lymphomas18. The third Trp53-mutant model produces the truncated Trp53-Δ122 protein, equivalent to the human Δ133p53 oncogenic isoform that has been observed in multiple tumours19,22. The Trp53-Δ122 protein promotes migration and actin polymerisation and Trp53-Δ122 mutant mice have an inflammatory phenotype, and succumb rapidly to B and T cell lymphomas18,23,24,25. As these Trp53-Δ122 mutant mice develop tumours more rapidly than Trp53-null mice, the Trp53-Δ122 protein is considered to be oncogenic.
Results
Loss of Testin in Trp53-mutant lymphomas
Tumours from Trp53-mutant mice were collected and characterised using haematoxylin and eosin staining and immunohistochemistry (IHC) with antibodies to B cell (B220) and T-cell (CD3) surface markers. In addition, both lymphoid and non-lymphoid tumours were classified according to Testin protein status by IHC (see Fig. 1A for examples). Overall, the non-lymphoid tumours [osteosarcomas (n = 3), rhabdomyosarcoma (n = 1), malignant fibrous histiocytomas (n = 9), hamartoma (n = 1) and one undefined], were Testin-positive with only one testin-negative tumor [1 of 15 (7%); data not shown] compared to 42 of 88 (48%) lymphomas being negative for Testin protein (Fisher’s exact test; P = 0.0018) (Supplementary Table S1).
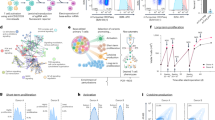
Testin immunohistochemistry of lymphomas. (A) Examples of immunohistochemistry results showing Testin-positive (right) and Testin-negative (left) lymphoma cells in tumours in the spleen (upper) and thymus (lower). (B) Pie-charts showing numbers of mice with lymphomas with respect to Testin status. (i) All lymphomas. (ii) B- or T-cell lymphomas. (iii) Trp53-mutant genotype of lymphomas. (Testin status: blue box negative; orange box positive; grey box mixed).
Closer examination of the IHC results revealed some interesting observations (Fig. 1B). Firstly, a similar proportion of B- and T-cell lymphomas were Testin-negative (42% of B-cell and 53% of T-cell lymphomas), which is in contrast to childhood ALL, where 94% of B-ALL and 71% of T-ALL were TESTIN negative9.
Secondly, Testin positive lymphomas were not observed at similar frequencies within the Trp53-mutant mice groups. For example, lymphomas isolated from Trp53-Δ122 mice were largely Testin positive or mixed (70%), whereas those from homozygous Trp53-null and homozygous Trp53-mΔpro mice were predominantly negative for Testin protein (63% and 69%, respectively).
Using Fisher’s exact test (2-tailed), the significance of the Testin status for each Trp53-mutant group with respect to the Trp53-Δ122 allele was calculated (Table 1). In brief, these results demonstrate that the Trp53-Δ122 allele was associated with the presence of Testin protein in the lymphomas, despite some comparisons failing to reach significance (P < 0.05). For example, the proportion of Testin positive and negative lymphomas isolated from Trp53-Δ122 was significantly different when compared to either homozygous Trp53-null (Group 1, P = 0.013) or homozygous Trp53-mΔpro (Group 2, P = 0.0044) mice, but not when compared to the small number of heterozygousTrp53-mΔpro/Trp53-Δ122 mice (Group 3, P = 0.7).
Comparing the heterozygous Trp53-mΔpro/Trp53-Δ122 mice with the homozygous Trp53-null (Group 4, P = 0.24) or with the Trp53-mΔpro mice (Group 5, P = 0.074), did not reveal significant differences in proportions of Tes-positive lymphomas, likely due to the low numbers of heterozygous mice present (n = 8).
To further investigate the effect of the Δ122 protein on Testin status, we combined the homozygous Trp53-Δ122 and heterozygous Trp53-mΔpro/Trp53-Δ122 mice into the “Δ122-any” cohort. Comparison of the proportion of the Tes-positive lymphomas between this “Δ122-any” cohort and the homozygous Trp53-null mice (Group 6, P = 0.0021) and between the homozygous Trp53-mΔpro mice (Group 7, P = 0.001) were highly significant. And finally, comparison of this “Δ122-any” cohort with the combined “non-Δ122 mice” (homozygous Trp53-null mice and homozygous Trp53-mΔpro) (Group 8, P = 0.0001) revealed highly significant differences in the proportions of Testin-positive lymphomas.
Firstly, these results confirm that silencing of Tes is frequently observed in lymphoid tumours and is likely required for lymphoma development. And secondly, that the presence of the Trp53-Δ122 allele increased the probability of a lymphoma being Testin-positive, suggesting that the presence of Trp53-Δ122 oncogenic protein reduced the requirement for Testin silencing in lymphoid tumour development.
As Testin silencing was frequently observed in Trp53-mutant lymphomas, we speculated that the presence of Testin protein would be protective for lymphoma onset and mouse survival. However, no statistically significant difference in survival for the Testin negative or positive lymphomas was observed within the genotype groups or between the CD3+ and B220+ lymphomas, although the numbers of mice within these comparisons were small (Supplementary Table S2).
Testin protein is regulated by transcriptional control
To determine whether the absence of Testin protein in mouse lymphomas was due to transcriptional silencing as is observed in childhood ALL, Tes transcript levels were quantified in a separate cohort of lymphomas and normal control tissues (Fig. 2A for details). Small pieces (1 mm3) of lymphoma, containing both normal and tumour cell populations of unknown proportions, were used for nucleic acid purification. Total RNA from these small lymphoma samples were used to determine Tes mRNA expression and quantitative RT-PCR results demonstrated that Tes transcript was reduced in 4 of the 9 lymphomas tested (Fig. 2B). As normal cells express Tes transcript (Fig. 2B), these results confirm that mouse Tes RNA expression is reduced or absent in lymphomas.
Tes expression and promoter methylation in Trp53-mutant lymphomas. (A) Table showing the genotype for the Trp53-mutant lymphomas tested. (B) Quantitative RT-PCR results showing Tes mRNA expression levels calculated relative to Rps29 and β2m expression and normalised to spleen expression level for lymphomas and normal mouse tissues. Relative Tes expression levels are shown. (C) Methylation lollipop plots for normal tissues and lymphomas showing only the unique methylation patterns obtained. The observed frequency for each unique clone pattern is shown.
Testin protein is not regulated by Tes promoter methylation in murine lymphomas
In childhood ALL, RNA transcriptional silencing and lack of TESTIN protein results from dense, biallelic TES promoter methylation9. To investigate whether Tes expression is similarly controlled by promoter methylation in the mouse lymphomas, we designed bisulfite-specific primers to amplify the CpG island located in the orthologous region of the mouse promoter.
As lymphoma samples contained both normal and tumour cells, we investigated promoter methylation using clonal bisulfite sequencing (see “Methods”). From bisulfite sequencing analysis (Fig. 2C), mouse lymphomas were largely unmethylated at the Tes promoter, although low-level, sporadic methylation was observed. It is improbable that this observed low level of methylation (< 5%), which was neither clonal, dense or present at specific CpG sites, is able to silence Tes transcription in mouse lymphomas. Therefore, we conclude that the observed reduction in Tes transcription in these lymphomas is not mediated via promoter methylation.
Discussion
Promoter methylation and subsequent TES transcriptional silencing is observed in all molecular sub-types of childhood ALL9. TESTIN has been shown to inhibit cellular proliferation and increase apoptosis11 in ALL cells and other cancer cell lines1,8,10,11,12,13,14, confirming that TES is a tumour suppressor gene. The high prevalence and clonal nature of TES silencing in paediatric ALL strongly suggests that TES silencing is either an early event or an epigenetic driver of leukaemia development. To confirm the importance of TES transcriptional silencing in leukaemogenesis, we investigated Tes RNA and Testin protein expression in archived tumours isolated from tumour-prone mice.
In common with the prevalence of TES silencing observed in childhood ALL, we demonstrated that Tes-silencing and lack of Testin protein was common in spontaneous lymphomas isolated from Trp53-mutant mice, but was rare in non-lymphoid tumours. For the Trp53-null and Trp53-mΔpro homozygous mutant mice, 63% and 69% respectively of the isolated lymphomas were Testin negative, which is similar to reported rates in childhood T-ALL9. These results are consistent with Testin protein being a lymphoid tumour suppressor in both mice and humans.
Of surprise was the observation that lymphomas from mice expressing Trp53-Δ122 were frequently Testin positive (> 60%), suggesting that the presence of the Trp53-Δ122 protein appeared to mitigate the requirement for Tes silencing in lymphomagenesis. Trp53-Δ122 protein is considered to be oncogenic, as Trp53-Δ122 mice demonstrate increased cellular proliferation, increased inflammation and die earlier with more aggressive tumours than null mice19. Following these surprising results, we propose that Trp53 and Testin have complementary functions in lymphoid tumour development and that this may be mediated via interacting proteins. Two recent reports have identified proteins which interact with TESTIN and are able to modulate TP53 activity. Firstly, ELL2 is a binding partner for TESTIN26 and ELL proteins can bind to the transactivation domain of TP53 and inhibit transactivation activity27. Secondly, Zyxin, a known binding partner of TESTIN28, has been reported to modulate the TP53/HIPK2 pathway by stabilising the HIPK2 protein, which phosphorylates Ser46 of TP53 and induces apoptosis29. These observations confirm that the TESTIN protein may modulate TP53 activity via protein interactions. However, as the Trp53-Δ122 protein lacks both Ser46 and the transactivation domain, these reported interactions are unable to explain our results with the Trp53-Δ122 mice.
The lack of Testin silencing in tissues from the Trp53-Δ122 mice suggests that Trp53-Δ122 protein can override the mechanism of silencing. A possible explanation for this comes from a report that the human Δ133p53 isoform can overcome cell growth arrest induced by p53 family members, p63 and p7330. Thus, p63 and/or p73 could repress Testin expression, but when Δ133p53 is over-expressed, this repression is prevented. Preliminary data consistent with this explanation are shown in Supplementary Fig. S1. In three separate cohorts of haematopoietic tumors, p73 (but not p63 or p53) mRNA expression was negatively correlated with TES expression. There is also a p53/p63/p73 response element within the TES promoter31.
Previously, we demonstrated that silencing of TES transcription by promoter methylation is prevalent in childhood ALL9 and that re-expression of TESTIN in human ALL cell lines and other cancer cell lines resulted in increased cell death11, thus adding support for TES to be considered a tumour suppressor gene. In this study, we show that silencing of Tes transcription and subsequent lack of Testin protein is common in equivalent mouse tumours, supporting its proposed role in suppressing lymphoid tumour development.
Methods
Mouse husbandry and genotyping PCR
As homozygous Tp53-mutant mice were reported to have fertility problems32, all breeding crosses were performed with heterozygous Tp53-mutant mice. All mice were tail-tipped at weaning and tails were digested with proteinase K overnight. Tp53-specific PCR amplifications of crude tail-tip preparations were used to identify Tp53 genotypes (details available on request). Mutant mice were maintained under standard housing conditions and monitored for tumour development, such as morbidity, swelling of the abdomen and hunching. Mice were euthanised once tumours or morbidity were detected and tumors and normal tissues were collected and fixed in 10% neutral-buffered formalin or RNAlater (Life Technologies Ltd).
Mouse studies were approved and conducted in accordance with local guidelines and regulations under University of Otago Ethics Approvals—AEC 20/07, 21/07 and D118/09.
Immunotyping of lymphomas
Tissues and tumours were paraffin-embedded and sections were stained with haematoxylin and eosin. Tumours were classified by a mouse pathologist (GW) and T- and B-cell lymphomas were identified after immunohistochemistry with CD3 and B220 antibodies, respectively. Testin antibody (SC-100914 TES (AA-7), Global Science) was optimised on mouse spleen and human tonsil tissue sections (see Supplementary Fig. S2) and validated using tissues isolated from homozygous Tes-genetrap mice33 (data not shown). The Testin status of the tumours isolated from Tp53-mutant mice was determined using Testin antibody and immunohistochemistry, using the following scoring system: lymphomas with fewer than 10% of tumour cells positive for Testin antibody staining were classified as ‘negative’; whereas lymphomas with more than 80% of their tumour cells being Testin positive were classified as ‘positive’. Furthermore, the small number of lymphomas with less than 80%, but more than 20% of cells being positive for Testin antibody staining were labelled as ‘mixed’.
Quantitative RT-PCR for Tes transcript
A small, separate cohort of lymphomas (Supplementary Table S1) containing both normal and tumour cells were collected into RNAlater and stored at − 20 °C. Genomic DNA and total RNA was isolated (MN RNA Isolation kit) from small biopsies (1 mm3) of these lymphomas and from fresh, normal tissues. RNA was reverse-transcribed to cDNA using the High Capacity cDNA Reverse Transcription kit (ThermoFisher Ltd). Quantitative RT-PCR was performed in triplicate for Tes (IDT PrimeTime assay-Mm.Pt.56a.43509122 (exons 6–7); Integrated DNA Technologies), β2-microglobin (IDT PrimeTime assay-N009735.1.pt; Integrated DNA Technologies) and Rps29 (TaqMan assay-Mm02342448_gH; Applied Biosystems Ltd)) using Takara 2 × qPCR mix and a LightCycler real-time PCR machine. Tes expression was quantified using the ΔΔCt calculation method with Rps29 and β2M expression as reference genes and normalised to mouse spleen expression levels.
Bisulfite sequencing of the murine Tes promoter
In order to investigate DNA methylation at the mouse Tes promoter, we designed bisulfite-specific primers to the orthologous region previously investigated in the human gene9. Genomic DNA from lymphomas and normal tissues were bisulfite-treated using EZ DNA Methylation Gold Kit (Zymo Research Ltd). Tes promoter regions were amplified with bisulfite-specific primers (forward: GGG TTA TTT ATT TTT TTT GGT TTG TT; reverse: TTT AAT TTC CAA ATC CAT ACT AAA C; product is 451 bp in length) and KAPA HiFi Hotstart Ready Mix, using the following program (98 °C for 45 s; 98 °C for 15 s, 56.7 °C for 30 s, 72 °C for 30 s, for 35 cycles; 72 °C for 5 min). PCR products were cloned using the TOPO Cloning kit (Life Technologies Ltd) and DH5α competent cells. Plasmid DNA was prepared (Zyppy Plasmid miniprep kit, Zymo Research Ltd) from bacterial colonies and sequenced according to established protocols.
Data availability
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- IHC:
-
Immunohistochemistry
- RT-PCR:
-
Reverse-transcriptase polymerase chain reaction
- ALL:
-
Acute lymphoblastic leukaemia
References
Bai, Y., Zhang, Q. G. & Wang, X. H. Downregulation of TES by hypermethylation in glioblastoma reduces cell apoptosis and predicts poor clinical outcome. Eur. J. Med. Res. 19, 66. https://doi.org/10.1186/s40001-014-0066-4 (2014).
Mueller, W. et al. Downregulation of RUNX3 and TES by hypermethylation in glioblastoma. Oncogene 26, 583–593. https://doi.org/10.1038/sj.onc.1209805 (2007).
Skiriutė, D. et al. Promoter methylation of AREG, HOXA11, hMLH1, NDRG2, NPTX2 and Tes genes in glioblastoma. J. Neurooncol. 113, 441–449. https://doi.org/10.1007/s11060-013-1133-3 (2013).
Ma, H. et al. Extensive analysis of D7S486 in primary gastric cancer supports TESTIN as a candidate tumor suppressor gene. Mol. Cancer 9, 190. https://doi.org/10.1186/1476-4598-9-190 (2010).
Sarti, M. et al. Adenoviral transduction of TESTIN gene into breast and uterine cancer cell lines promotes apoptosis and tumor reduction in vivo. Clin. Cancer Res. 11, 806–813 (2005).
Qiu, H. et al. Frequent hypermethylation and loss of heterozygosity of the testis derived transcript gene in ovarian cancer. Cancer Sci. 101, 1255–1260. https://doi.org/10.1111/j.1349-7006.2010.01497.x (2010).
Chene, L. et al. Extensive analysis of the 7q31 region in human prostate tumors supports TES as the best candidate tumor suppressor gene. Int. J. Cancer 111, 798–804. https://doi.org/10.1002/ijc.20337 (2004).
Zhu, J. et al. Testin is a tumor suppressor and prognostic marker in breast cancer. Cancer Sci. 103, 2092–2101. https://doi.org/10.1111/cas.12020 (2012).
Weeks, R. J., Kees, U. R., Song, S. & Morison, I. M. Silencing of TESTIN by dense biallelic promoter methylation is the most common molecular event in childhood acute lymphoblastic leukaemia. Mol. Cancer 9, 163. https://doi.org/10.1186/1476-4598-9-163 (2010).
Li, H. et al. TES inhibits colorectal cancer progression through activation of p38. Oncotarget 7, 45819–45836. https://doi.org/10.18632/oncotarget.9961 (2016).
Weeks, R. J., Ludgate, J. L., LeMee, G. & Morison, I. M. TESTIN induces rapid death and suppresses proliferation in childhood B acute lymphoblastic leukaemia cells. PLoS One 11, e0151341. https://doi.org/10.1371/journal.pone.0151341 (2016).
Gu, Z. et al. TESTIN suppresses tumor growth and invasion via manipulating cell cycle progression in endometrial carcinoma. Med. Sci. Monit. 20, 980–987. https://doi.org/10.12659/MSM.890544 (2014).
Wang, M. et al. Testin is a tumor suppressor in non-small cell lung cancer. Oncol. Rep. 37, 1027–1035. https://doi.org/10.3892/or.2016.5316 (2017).
Zhong, Z., Zhang, F. & Yin, S.-C. Effects of TESTIN gene expression on proliferation and migration of the 5–8F nasopharyngeal carcinoma cell line. Asian Pac. J. Cancer Prev. 16, 2555–2559. https://doi.org/10.7314/apjcp.2015.16.6.2555 (2015).
Levine, A. J. & Oren, M. The first 30 years of p53: Growing ever more complex. Nat. Rev. Cancer 9, 749–758. https://doi.org/10.1038/nrc2723 (2009).
Olivier, M., Hollstein, M. & Hainaut, P. TP53 mutations in human cancers: Origins, consequences, and clinical use. Cold Spring Harb Perspect. Biol. 2, a001008. https://doi.org/10.1101/cshperspect.a001008 (2010).
Donehower, L. A. et al. Mice deficient for p53 are developmentally normal but susceptible to spontaneous tumours. Nature 356, 215–221. https://doi.org/10.1038/356215a0 (1992).
Slatter, T. L. et al. p53-mediated apoptosis prevents the accumulation of progenitor B cells and B-cell tumors. Cell Death Differ. 17, 540–550. https://doi.org/10.1038/cdd.2009.136 (2010).
Slatter, T. L. et al. Hyperproliferation, cancer, and inflammation in mice expressing a Delta133p53-like isoform. Blood 117, 5166–5177. https://doi.org/10.1182/blood-2010-11-321851 (2011).
Morse, H. C. Bethesda proposals for classification of lymphoid neoplasms in mice. Blood 100, 246–258. https://doi.org/10.1182/blood.V100.1.246 (2002).
Jacks, T. et al. Tumor spectrum analysis in p53-mutant mice. Curr. Biol. 4, 1–7. https://doi.org/10.1016/s0960-9822(00)00002-6 (1994).
Joruiz, S. M. & Bourdon, J. C. p53 isoforms: Key regulators of the cell fate decision. Cold Spring Harb. Perspect. Med. 6, 20. https://doi.org/10.1101/cshperspect.a026039 (2016).
Sawhney, S. et al. Alpha-enolase is upregulated on the cell surface and responds to plasminogen activation in mice expressing a 133p53alpha mimic. PLoS One 10, e0116270. https://doi.org/10.1371/journal.pone.0116270 (2015).
Campbell, H. G. et al. Does Delta133p53 isoform trigger inflammation and autoimmunity?. Cell Cycle 11, 446–450. https://doi.org/10.4161/cc.11.3.19054 (2012).
Roth, I. et al. The Delta133p53 isoform and its mouse analogue Delta122p53 promote invasion and metastasis involving pro-inflammatory molecules interleukin-6 and CCL2. Oncogene 35, 4981–4989. https://doi.org/10.1038/onc.2016.45 (2016).
Arumemi, F., Bayles, I., Paul, J. & Milcarek, C. Shared and discrete interacting partners of ELL1 and ELL2 by yeast two-hybrid assay. Adv. Biosci. Biotechnol. 04, 774–780. https://doi.org/10.4236/abb.2013.47101 (2013).
Wiederschain, D., Kawai, H., Gu, J., Shilatifard, A. & Yuan, Z. M. Molecular basis of p53 functional inactivation by the leukemic protein MLL-ELL. Mol. Cell. Biol. 23, 4230–4246. https://doi.org/10.1128/mcb.23.12.4230-4246.2003 (2003).
Hadzic, E. et al. Delineating the tes interaction site in zyxin and studying cellular effects of its disruption. PLoS One 10, e0140511. https://doi.org/10.1371/journal.pone.0140511 (2015).
Crone, J. et al. Zyxin is a critical regulator of the apoptotic HIPK2-p53 signaling axis. Cancer Res. 71, 2350–2359. https://doi.org/10.1158/0008-5472.CAN-10-3486 (2011).
Mehta, S. Y. et al. Regulation of the interferon-gamma (IFN-gamma) pathway by p63 and Delta133p53 isoform in different breast cancer subtypes. Oncotarget 9, 29146–29161. https://doi.org/10.18632/oncotarget.25635 (2018).
Sbisa, E. et al. p53FamTaG: A database resource of human p53, p63 and p73 direct target genes combining in silico prediction and microarray data. BMC Bioinform. 8(Suppl 1), S20. https://doi.org/10.1186/1471-2105-8-S1-S20 (2007).
Hu, W., Feng, Z., Teresky, A. K. & Levine, A. J. p53 regulates maternal reproduction through LIF. Nature 450, 721–724. https://doi.org/10.1038/nature05993 (2007).
Crompton, L. A., Du Roure, C. & Rodriguez, T. A. Early embryonic expression patterns of the mouse Flamingo and Prickle orthologues. Dev. Dyn. 236, 3137–3143. https://doi.org/10.1002/dvdy.21338 (2007).
Gao, J. M. T. et al. The cbioportal for cancer genomics: An intuitive open-source platform for exploration, analysis and visualization of cancer genomics data. AACR 20, 20 (2018).
Acknowledgements
The study received histology technical assistance from Amanda Fisher, Ms Shanna Trollip and Alisa Shaw (Histology Unit, Dunedin School of Medicine). Statistical advice was provided by Dr. Michel de Lange (University of Otago).
Funding
This work was supported by the Health Research Council NZ, Cancer Society NZ and by the Dean’s Bequest Fund (Dunedin School of Medicine, University of Otago, Dunedin).
Author information
Authors and Affiliations
Contributions
R.J.W., J.L.L., G.L.M. and T.L.S. were involved in mouse husbandry, tissue collection and genotyping. R.J.W. and R.K. performed the qRT-PCR and bisulfite sequencing. G.W. analysed the IHC experiments and classification of the mouse tumours. R.J.W., T.L.S., A.W.B. and I.M.M. were involved in study concept and design. R.J.W., G.W., A.W.B. and T.L.S. performed the mouse lymphoma data analysis. A.W.B. and S.M. analysed the haematopoietic tumor cohort data (Supplementary Fig. S1). R.J.W. wrote the first draft of the manuscript. All authors contributed to the editing and had final approval of the submitted version.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Weeks, R.J., Ludgate, J.L., Le Mée, G. et al. Silencing of Testin expression is a frequent event in spontaneous lymphomas from Trp53-mutant mice. Sci Rep 10, 16255 (2020). https://doi.org/10.1038/s41598-020-73229-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-020-73229-3
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.