Abstract
The prevalence of atherosclerotic cardiovascular disease is higher in patients with type 2 diabetes, a disorder characterized by hyperinsulinemia and insulin resistance. The role of hyperinsulinemia as an independent participant in the atherogenic process has been controversial. In the current study, we tested the effect of insulin and the insulin sensitizer, adiponectin, on human macrophage foam cell formation. We found that both insulin and adiponectin increased the expression of the type 2 scavenger receptor CD36 by approximately twofold and decreased the expression of the ATP-binding cassette transporter ABCA1 by >80%. In both cases regulation was post-transcriptional. As a consequence of these changes, we found that oxidized LDL (oxLDL) uptake was increased by 80% and cholesterol efflux to apolipoprotein A1 (apoA1) was decreased by ∼25%. This led to two- to threefold more cholesterol accumulation over a 16-h period. As reported previously in studies of murine systems, scavenger receptor-A (SR-A) expression on human macrophages was downregulated by insulin and adiponectin. Insulin and adiponectin did not affect oxLDL-induced secretion of monocyte attractant protein-1 (MCP-1) and interleukin-6 (IL-6). These studies suggest that hyperinsulinemia could promote macrophage foam cell formation and thus may contribute to atherosclerosis in patients with type 2 diabetes.
Similar content being viewed by others
Main
Cardiovascular disease is the leading cause of death in many developed countries, and atherosclerosis accounts for most of the major pathology.1, 2 Patients with type 2 diabetes mellitus, a condition characterized by insulin resistance and compensatory hyperinsulinemia, have a two- to threefold increased risk of atherosclerotic cardiovascular disease.3, 4, 5 Although there have been many studies that support the causative role of insulin resistance in cardiovascular disease from both epidemiologic and experimental perspectives,6, 7, 8, 9, 10, 11 there is very little evidence supporting a direct cause and effect relationship between hyperinsulinemia and atherosclerosis. Furthermore, the role of hyperinsulinemia as an independent risk factor has been controversial. Several prospective population studies including the Quebec Cardiovascular study showed an association of high plasma insulin levels with increased risk of coronary heart disease,12, 13, 14, 15, 16, 17 but other studies, such as that of Welin et al18 failed to show such an association.19 As hyperinsulinemia usually occurs in states of insulin resistance it is difficult to determine an independent role for hyperinsulinemia in the pathogenesis of atherosclerosis.
Excessive lipid accumulation by macrophages has a crucial role in the initiation and progression of atherosclerosis. Lipid laden macrophage foam cells accumulate in atheromatous plaque and promote inflammation by secreting cytokines that recruit other immune cells to the arterial intima. Foam cells are generated by uncontrolled uptake of modified LDL, especially oxidized LDL (oxLDL) and/or impaired cholesterol efflux.20, 21 Lipid homeostasis in macrophages is regulated by scavenger receptors, including CD36 and scavenger receptor-A (SR-A), which mediate uptake and specific ATP-binding cassette (ABC) family transporters that mediate cholesterol efflux to apolipoprotein A1 (apoA1) and high-density lipoprotein (HDL).22, 23, 24, 25 Thus, alteration in expression of these molecules in macrophages may affect foam cell formation and progression of atherosclerosis.
Adiponectin, also known as Acrp30, is an adipokine exclusively expressed and secreted by adipocytes that functions as an insulin sensitizer. Plasma concentrations of adiponectin are low in type 2 diabetic patients26, 27 and mice lacking adiponectin have hepatic insulin resistance.28 Administration of adiponectin improves insulin sensitivity in animal models of type 2 diabetes and insulin resistance.29, 30 The precise molecular mechanism by which adiponectin sensitizes cells to insulin signals has not been elucidated, however, it appears to include cross-talk between adiponectin and insulin receptor (IR) signaling pathways.31 Adiponectin was recently suggested to have an anti-atherogenic effect through regulation of SR-A and acyl-coenzyme A:cholesterol acyltransferase-1 (ACAT-1) expression in macrophages.32, 33
In the current study, we used human peripheral blood monocyte-derived macrophages to test the effect of insulin and adiponectin on macrophage expression of scavenger receptors and ABC transporter sub-family A member 1 (ABCA1) and on oxLDL uptake, cholesterol efflux and foam cell formation. We found that insulin and adiponectin upregulated CD36 expression and downregulated ABCA1 expression, resulting in enhanced oxLDL uptake, diminished cholesterol efflux and increased foam cell formation.
MATERIALS AND METHODS
Reagents
LDL prepared from human plasma was oxidatively modified as previously described using a myeloperoxidase, glucose oxidase, nitrite system.34 Bovine insulin was from Sigma and recombinant human adiponectin from R&D systems. Polyclonal antibody against human CD36 was from Cayman Chemical. Monoclonal anti-human CD36 IgG, phycoerythrin-conjugated anti-CD36 IgG and antibodies against SR-A, actin and α-tubulin were from Santa-Cruz Biotechnology. Antibodies against ABCA-1 and EMR1 (F4/80) were purchased from Abcam. C14-labeled cholesterol was purchased from American Radiolabeled Chemicals. ApoA1 protein was prepared as previously described.35 Quantikine Colorimetric Sandwich ELISA kits for IL-6 and monocyte chemoattractant protein-1 (MCP-1) were from R&D systems.
Cells
Human monocytes were isolated from peripheral blood by Ficoll-Hypaque centrifugation and were cultured in RPMI containing human AB serum (10%) for 7 days to allow for macrophage differentiation. The differentiation of the monocytes into macrophages was confirmed by flow cytometry with anti-EMR1(F4/80) antibody. Human peripheral blood was donated by non-diabetic healthy volunteers. Each sample was screened and the absence of hepatitis B, hepatitis C and HIV infection was confirmed.
Immunoblot Analyses
Human macrophages incubated with different concentrations of insulin (300 pM, 2 nM, 100 nM), adiponectin (2 μg/ml), oxLDL (50 μg/ml), LY294002 (10 μM) or wartmannin (100 nM) for 16 h were lysed with buffer containing 1% triton X-100. Lysates were separated by SDS–PAGE, transferred to PVDF membranes (Millipore) and probed with antibodies against CD36, ABCA-1, SR-A, actin or α-tubulin. Band intensities were quantified by ImageJ (http://rsbweb.nih.gov/ij/), Image-Pro Plus software (Media Cybernetics) and Gel-Pro Analyzer (MediaCybernetics).
Flow Cytometry
Human macrophages plated on serum-coated glass coverslips were incubated with insulin, adiponectin or oxLDL for 16 h, then fixed with 4% paraformaldehyde in PBS. Treated macrophages were gently scraped and collected in microtubes and then stained with PE-conjugated anti-CD36 or anti-SR-A IgG before measuring fluorescence intensity by flow cytometry with a Becton-Dickinson FACScan. Data were analyzed by FlowJo software (Tree Star). To assess oxLDL uptake, oxLDL was labeled with the fluorescent probe 1,1′-dioctadecyl-3,3,3′,3′-tetramethylindocarbocyanide perchlorate (diI; Molecular Probes) as previously described.36 Macrophages pre-incubated as above with insulin or adiponectin for 16 h were then exposed to diI-oxLDL (10 μg/ml) for 20 min and then fixed with 4% paraformaldehyde and analyzed by laser confocal microscopy. Fluorescence uptake was quantified using Image-Pro Plus software (Media Cybernetics).
RT-PCR
Total RNA was isolated by Tri reagent from human macrophages treated with insulin, adiponectin or oxLDL for 16 h and was converted into cDNA by reverse transcriptase (Roche) with oligo-dT primer. cDNAs were then used for PCR with the primers 5′-CAG AGG CTG ACA ACT TCA CAG-3′, 5′-AGG GTA CGG AAC CAA ACT CAA-3′ for CD36 or the primers 5′-AAC TCT ACA TCT CCC TT CCC G -3′, 5′-TGT CCT CAT ACC AGT TGA GAG AC-3′ for ABCA-1. PCR for actin was used as a reference with the primers 5′-GTG GGG CGC CCC AGG CAC CA-3′, 5′-CTC CTT AAT GTC ACG CAC GAT TTC-3′. PCR amplification was 22 cycles of 94°C for 1 min, 56°C for 1 min, and 72°C for 2 min for CD36, 28 cycles at the same temperature for ABCA-1 and 17 cycles for actin.
Cholesterol Efflux Assay
Macrophages plated on 24-well dishes were treated with insulin (2 nM, 100 nM) or adiponectin (2 μg/ml) with or without wartmannin (100 nM) for 16 h. OxLDL (50 μg/ml) was incubated with C14-labeled cholesterol (0.2 μCi/ml) at 37°C for 30 min and then loaded onto the macrophages. After 6 h, C14-cholesterol-labeled cells were washed with PBS and incubated with RPMI 1640 medium for 16 h. C14-cholesterol released from the cells into the medium was measured using scintillation counter. Cellular cholesterol was extracted by hexane:isopropanol (3:2 v/v), and C14 radioactivity in the extract solution was measured by scintillation counter. Efflux percentage was calculated as C14 radioactivity in medium/(C14 radioactivity in medium + C14 radioactivity in cells) × 100%.
Intracellular Cholesterol Measurement
Human macrophages plated in a 6-well dish were incubated with insulin (2 nM, 100 nM) or adiponectin (2 μg/ml) with or without LY294002 (10 μM). The cells were treated with oxLDL for 16 h and lysed by 0.5% triton X-100 containing buffer on ice. The lysates were centrifuged at 17 000 g for 30 min at 4°C and the supernatant was collected for cholesterol measurement. Cholesterol was measured using Cayman cholesterol assay kit (Cayman chemical). Briefly, the cell lysates were mixed with assay buffer containing cholesterol esterase, cholesterol oxidase, HRP and ADHP (10-acetyl-3,7-dihydroxyphenoxazine). Fluorescent product resorufin that was generated by the reaction between ADHP and hydrogen peroxide from cholesterol oxidation could be measured by fluorescence plate reader using excitation wavelengths of 530–580 nm and emission wavelengths of 585–595 nm. We also measured total cholesterol and free cholesterol of macrophages by using gas chromatography coupled with mass spectrometry (GC-MS). Human macrophages were incubated with insulin (2 nM, 100 nM) or adiponectin (2 μg/ml) with or without wartmannin (200 nM) and then treated with oxLDL (50 μg/ml) for 16 h. These cells were resuspended with 900 μl water and 100 μl of 1 μg/ml coprosternol in isopropanol and applied to the GC-MS as described previously.37 We recorded the total ion mass spectra of trimethylsilyl derivatives, extracted the GC chromatograms and calculated cholesterol content in each samples. The intracellular cholestserol of each sample was normalized by protein concentration of each sample.
RESULTS
Insulin and Adiponectin Alter Scavenger Receptor Expression in Human Monocyte-Derived Macrophages
Immunoblots for CD36 showed that insulin at 2 and 100 nM and adiponectin at 2 μg/ml increased CD36 expression in macrophages. The adiponectin concentration used was the one that increased phosphorylation of Akt Ser473 to the same extent as did 100 nM insulin (data not shown). The increase in CD36 was prevented by pre-treatment of the cells with the PI3-kinase inhibitors LY294002 or wartmannin (Figure 1a). The inhibitors themselves had no effect (Figure 1a), unlike what was previously reported for murine macrophages.38 Although the magnitude of effect on CD36 expression induced by insulin or adiponectin varied among cells from different donors, cumulative data from 15 different subjects showed a mean increase of twofold (Figure 1b; P<0.05).
Insulin and adiponectin increase CD36 expression in human monocyte-derived macrophages. (a) Macrophages were pre-treated with indicated concentrations of insulin or adiponectin for 16 h and then lysed and assessed by western blot for CD36 expression. In some cases, cells were also treated with LY294002 (10 μM) or wartmannin (100 nM). Blots were stripped and re-probed with anti-tubulin antibody and fold change in CD36 band density was determined from scanned images. Image is representative of n=15. (b) Means±s.d. of data from 15 different donors normalized as in panel a; *P<0.05. (c) Flow cytometry histogram of cells treated with insulin or adiponectin and then stained with PE-conjugated anti-CD36 IgG. (d) Mean fluorescence intensity was assessed by flow cytometry as described in panel c. The bar graph of comparison was generated from experiments using macrophages from five different subjects; *P<0.001. (e) mRNA isolated from cells treated with insulin or adiponectin was assessed by RT-PCR using specific primers for CD36 and actin. (f) Macrophages pre-treated with insulin or adiponectin along with or without oxidized LDL (oxLDL) were assessed by western blot for CD36 expression as described in panel a.
Using flow cytometry we showed that the increase in total CD36 protein levels induced by insulin or adiponectin were associated with a significant, dose-dependent increase in macrophage cell surface CD36 expression (Figure 1c). Cumulative data from five different subjects showed that 100 nM of insulin and 2 μg/ml of adiponectin induced mean increases of 1.36-fold and 1.47-fold, respectively (Figure 1d; P<0.001). CD36 mRNA levels measured by RT-PCR did not change after macrophages were exposed to insulin or adiponectin (Figure 1e), suggesting that CD36 regulation was post-transcriptional. OxLDL, known to upregulate CD36,39, 40 had additive effect in CD36 increase when combined with insulin or adiponectin (Figure 1f).
SR-A, the other major scavenger receptor on macrophages for modified LDL,41 was also regulated by insulin, but in the opposite direction to CD36. Immunoblots revealed that insulin induced a dramatic, dose-dependent decrease in the expression of SR-A (Figure 2a). Immunofluorescence flow cytometry showed that insulin downregulated SR-A surface expression and that adiponectin also downregulated SR-A expression (Figures 2b and c). Interestingly, oxLDL, which is known to upregulate CD36,39, 40 decreased the expression of SR-A in human monocyte-derived macrophages (Figures 2a–c) and had an additive effect when combined with insulin (Figure 2a).
Insulin and adiponectin decrease expression of scavenger receptor-A (SR-A) in human monocyte-derived macrophages. Macrophages were pre-treated with insulin, adiponectin, oxidized LDL (oxLDL) or insulin plus oxLDL for 16 h and analyzed by immunoblot (a) or flow cytometry (b) as in Figure 1 using a monoclonal antibody specific for SR-A. Experiments were repeated with macrophages from three different donors, respectively. (c) Mean fluorescence intensity was assessed by flow cytometry in panel b. The bar graph of comparison was generated from experiments using macrophages from three different subjects; *P<0.05.
Insulin and Adiponectin Decrease ABCA-1 Expression in Human Monocyte-Derived Macrophages
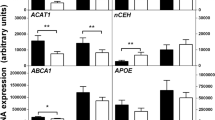
Immunoblots for the cholesterol transporter ABCA-1 revealed that insulin and adiponectin decreased ABCA-1 expression in macrophages by up to 80% (Figure 3a). Interestingly, PI3-kinase inhibition by LY294002 had no effect on adiponectin-mediated downregulation and only a partial effect on insulin (Figure 3a). Insulin and adiponectin also induced downregulation of ABCA-1 in the presence of oxLDL (Figure 3b), which by itself has been shown to increase ABCA-1 expression.42 These data suggest that the regulatory mechanism of insulin and adiponectin on ABCA-1 expression may be distinct from the liver X receptor/retinoid X receptor regulatory pathway activated by oxLDL.42 This is further supported by analysis of mRNA levels (Figure 3c), which showed no change in ABCA-1 levels after macrophages were exposed to insulin or adiponectin, in contrast to the 4.4-fold increase seen after exposure to oxLDL.
Insulin and adiponectin decrease ATP-binding cassette transporter sub-family A member 1 (ABCA-1) expression in human monocyte-derived macrophages. (a) Macrophages were pre-treated for 16 h with insulin or adiponectin in the presence or absence of LY294002 (10 μM) and then lysed and analyzed by immunoblot for ABCA-1 expression. Blots were stripped and re-probed with anti-actin antibody and fold change in ABCA-1 band density was determined from scanned images. Image is representative of three repetitive blots. (b) Cells were exposed to oxidized LDL (oxLDL; 50 μg/ml) with or without insulin or adiponectin and analyzed as in panel a. (c) RT-PCR for ABCA-1 mRNA of macrophages treated as described in panel b.
Insulin and Adiponectin Enhance oxLDL-Induced Lipid Accumulation in Human Monocyte-Derived Macrophages
Having shown that insulin and adiponectin increased the expression of CD36 and decreased the expression of ABCA-1 in human macrophages, we next examined their effect on oxLDL uptake, cholesterol efflux and foam cell formation. To assess oxLDL uptake, we added diI-labeled oxLDL to macrophages that had been exposed to insulin (100 nM) or adiponectin (2 μg/ml) for 16 h and then measured intracellular fluorescence after 20 min using confocal microscopy. As shown in Figure 4a, insulin increased uptake by ∼80% (P<0.05) whereas adiponectin had no effect (Figure 4a).
Insulin and adiponectin enhance oxidized LDL (oxLDL)-mediated cholesterol loading of human mononcyte-derived macrophages. (a) Macrophages were pre-treated with insulin (100 nM) or adiponectin (2 μg/ml) for 16 h and then exposed to 1,1′-dioctadecyl-3,3,3′,3′-tetramethylindocarbocyanide perchlorate (diI)-labeled oxLDL for 20 min at 37°C. Fluorescence uptake was quantified by digital confocal microscopy using Imge-Pro software. The graph represents mean±s.d. of five experiments analyzing 50–100 cells each (*P<0.05). (b) Macrophages were pre-treated with insulin or adiponectin for 16 h and then exposed to oxLDL-containing C14-labeled cholesterol for 6 h. C14-labeled cholesterol effluxed to apolipoprotein A1 (apoA1) was measured by scintillation counting. The graph shows mean±s.d. from separate assays using macrophages from three different donors (*P<0.05). (c) Macrophages were pre-treated with insulin or adiponectin as above and then exposed to oxLDL (50 μg/ml) for 16 h at 37°C. Intracellular cholesterol was measured by the cholesterol oxidation reaction method. The graph shows mean±s.d. from experiments using macrophages from three different donors (*P<0.001). Macrophages pre-treated with insulin or adiponectin were exposed to oxLDL (50 μg/ml). Free (d) or total (e) cholesterol was measured by gas chromatography combined with mass spectrometry (GC-MS).
To evaluate the effect of insulin and adiponectin on cholesterol efflux from macrophages, we loaded cells with oxLDL-containing C14-labeled cholesterol and then measured the rate of C14 efflux to apoA1 in the culture medium. Pre-treatment with either insulin or adiponectin decreased the efflux by ∼25% (Figure 4b; P<0.05).
We hypothesized that the increased macrophage uptake of oxLDL and impaired cholesterol efflux induced by insulin or adiponectin would result in intracellular accumulation of excessive lipoprotein derived cholesterol and ultimately in foam cell formation.43 Figure 4c shows that after 16 h of cell exposure to oxLDL, intracellular cholesterol content measured by enzymatic cholesterol assay was increased by threefold in macrophages pre-treated with insulin or adiponectin, compared with untreated cells. Total cholesterol and free cholesterol of macrophages measured by GC-MS also showed that free and total intracellular cholesterol of macrophages were increased by pre-treatment with insulin or adiponectin (Figures 4d and e).
OxLDL is known to induce secretion of cytokines such as MCP-1 and IL-6 from mouse macrophages.44 Here we show that oxLDL also increased the secretion of IL-6 and MCP-1 from human monocyte-derived macrophages (Supplementary Figure 1), and that neither insulin nor adiponectin affected baseline or oxLDL-induced cytokine secretion.
DISCUSSION
Hyperinsulinemia was first suggested as a risk factor for atherosclerosis more than 30 years ago, based on the observation that insulin levels are higher than normal in patients with ischemic heart disease.45 Since then, there have been many clinical and experimental studies revealing that high levels of insulin precede development of arterial diseases in diabetic and non-diabetic patients.12, 13, 14, 15, 16, 17, 46, 47, 48 However, the role of hyperinsulinemia as an independent risk factor for atherosclerotic coronary disease has been controversial. Mostly, hyperinsulinemia occurs with insulin resistance in type 2 diabetes and is regarded as a compensatory mechanism of insulin resistance. Many studies suggest insulin resistance as a risk factor for atherosclerosis based on its pathological effects on dyslipidemia, hypertension, and a hypercoagulable state, which accelerate atherosclerosis.6, 7, 8, 9, 10, 11, 49 Therefore, it is difficult to determine whether the link between hyperinsulinemia and atherosclerosis is causative, and this compels more experimental studies.
Macrophages perform a crucial role in the atherogenic process by generating lipid laden foam cells.20 Macrophages are known to express most insulin signaling molecules except IR substrate 1 (IRS1) and glucose transporter type 4.50, 51 Even though insulin activates the IR/IRS2/PI3K/Akt pathway in macrophages as in other types of insulin-responsive cells, there have been few studies investigating the biological functions of insulin signaling in macrophages. In the current study, we evaluated if insulin affects macrophage foam cell formation and found that insulin increased the expression of CD36 and decreased ABCA-1 expression, which may promote cholesterol accumulation in human monocyte-derived macrophages. Although the mechanism is not clear, the insulin-mediated regulatory mechanism of CD36 and ABCA-1 appear to be post-transcriptional based on our results from RT-PCR. A recent study showing that insulin increased CD36 expression in Chinese hamster ovary or HEK 293 cells via regulating CD36 turnover52 supports our observation and permits a possible expectation that a similar regulatory pathway may be activated in macrophages. The mechanisms of insulin regulation of CD36 and ABCA-1 need to be studied and it appears to be that these proteins are regulated via different pathways.
Adiponectin is known to enhance insulin sensitivity, however, the signaling mechanism by which adiponectin sensitizes insulin is not clear. In our study, adiponectin showed an overlapping signaling with insulin. Low concentration of adiponectin increased the phosphorylation of Akt (Ser436) by the same degree as insulin and had the same modulating effect on CD36 and ABCA-1 as insulin (Figures 1 and 3). Previous studies showed that adiponectin had an anti-atherogenic property in apolipoprotein E-deficient mice53 and one of the suggested mechanisms was an inhibitory effect of adiponectin on SR-A expression and acetylated LDL (acLDL) uptake.54 In our current study, we reproduced the previous finding and showed that both insulin and adiponectin decreased SR-A expression in macrophages. However, the net effect of adiponectin resulted in increased intracellular cholesterol accumulation, which was opposite of previous reports. In addition to SR-A, adiponectin is known to downregulate ACAT-1 that catalyzes cholesteryl ester (CE) formation33 and therefore, adiponectin treatment decreased acLDL-induced CE accumulation in macrophages.33, 55 These intriguing results may be due to the different sources of cholesterol for lipid uptake assays, different concentrations of adiponectin and different modes of adiponectin activities. In our study using MPO-modified LDL (oxLDL), which is known to be a specific ligand for CD36,56 adiponectin increased the uptake of oxLDL via increased expression of CD36, whereas in the previous studies performed with acLDL, a specific ligand for SR-A,57 adiponectin, decreased acLDL uptake via a decrease in SR-A. Therefore, the effect of adiponectin in vivo may be determined by the specificity of modified LDL for different scavenger receptors.
Changes in the protein levels of CD36 and ABCA-1 induced by insulin and adiponectin appear to be regulated by PI3-kinase. Our study showed that PI3-kinase inhibitor prevented the increase of CD36 expression induced by insulin and adiponectin (Figure 1) while it minimally blocked the effect of these reagents on the expression of ABCA-1 (Figure 3). The functional effect of PI3-kinase blockade on the intracellular cholesterol of macrophages was varied among macrophages from different donors (Figure 4). As expected, based on the minimal blockade of ABCA-1 decrease, the PI-3 kinase inhibitor had no effect on cholesterol efflux of macrophages (Figure 4b) but partially prevented the increase of intracellular cholesterol by blocking increased CD36 expression.
Atherosclerosis and type 2 diabetes share similar pathological mechanisms including elevation in cytokines like MCP-1 and interleukin-6 (IL-6), which contribute to underlying inflammation of both.58 OxLDL is abundant in both of these conditions and is known to induce secretion of these proinflammatory cytokines in macrophages.59 Previous studies have suggested anti-inflammatory activities of insulin by showing that insulin infusion to diabetic patients suppressed mononuclear cell expression of toll-like receptor (TLR)-2 and TLR-4.60 However, another study showed that prolonged exposure to insulin accentuated tumor necrosis factor-α-induced transcription of proinflammatory genes while short-term exposure inhibited the transcription.61 In our current study, insulin and adiponectin, also known to have anti-inflammatory activity,62 did not affect oxLDL-induced secretion of MCP-1 and IL-6 in macrophages.
In the current study, we propose evidence that insulin facilitates macrophage foam cell formation, although this is a topic of controversy. It is sometimes suggested that hyperinsulinemia in the presence of insulin resistance may not be metabolically effective, however, it is possible that one pathway may remain active when the other pathway is blocked by insulin resistance. Therefore, more studies are needed to show how insulin activates different pathways and may be involved in different biological functions specifically affected by insulin resistance. The risk of cardiovascular disease is 10-fold higher than normal in patients with type 1 diabetes.63 Even though type 1 diabetes is characterized by impaired insulin secretion, it does not rule out the possible pathological effect of hyperinsulinemia. Indeed, many patients with type 1 diabetes have hyperinsulinemia from excessive dose of insulin, resulting insulin resistance.64 Furthermore, hyperinsulinemia appears to drive insulin resistance.65 Therefore, for the proper management of patients with type 1 and type 2 diabetes, more investigation about the role of hyperinsulinemia is required.
In conclusion, we provide evidence that hyperinsulinemia may promote atherosclerosis by promoting macrophage foam cell formation in the setting of abundant oxLDL, which has specific affinity to CD36.
References
Lusis AJ . Atherosclerosis. Nature 2000;407:233–241.
Marray CJ, Lopez AD . Global mortality, disability, and the contribution of risk factors; Global Burden of Disease Study. Lancet 1997;349:1436–1442.
Kannel WB, McGee DL . Diabetes and glucose tolerance as risk factors for cardiovascular disease: the Framingham Study. Diabetes Care 1979;2:120–126.
Pyörälä K, Laakso M, Uusitupa M . Diabetes and atherosclerosis: an epidemiologic view. Diabetes Metab Dev 1987;3:463–524.
Haffner SM, Lehto S, Ronnemaa T, et al. Mortality from coronary heart disease in subjects with type 2 diabetes and in nondiabetic subjects with and without prior myocardial infarction. N Engl J Med 1998;339:229–234.
Reaven GM . Banting lecture. Role of insulin resistance in human disease. Diabetes 1988;37:1595–1607.
Rutter MK, Meigs JB, Sullivan LM, et al. Insulin resistance, the metabolic syndrome, and incident cardiovascular events in the Framingham Offspring Study. Diabetes 2005;54:3252–3257.
Hanley AJ, Williams K, Stern MP, et al. Homeostasis model assessment of insulin resistance in relation to the incidence of cardiovascular disease: the San Antonio Heart Study. Diabetes Care 2002;25:1177–1184.
DeFronzo RA . Is insulin resistance atherogenic? Possible mechanisms. Atheroscler suppl 2006;7:11–15.
Bonora E, Formentini G, Calcaterra F, et al. HOMA-estimated insulin resistance is an independent predictor of cardiovascular disease in type 2 diabetic subjects: prospective data from the Cerona Diabetes Complications Study. Diabetes Care 2002;25:1135–1141.
Reddy KJ, Singh M, Bangit JR, et al. The role of insulin resistance in the pathogenesis of atherosclerotic cardiovascular disease: an updated review. J Cardiovasc Med 2010;11:633–647.
Pyörälä K . Relationship of glucose tolerance and plasma insulin to the incidence of coronary heart disease: results from two population studies in Finland. Diabetes Care 1979;2:131–141.
Welborn TA, Wearne K . Coronary heart disease incidence and cardiovascular mortality in Busselton with reference to glucose and insulin concentrations. Diabetes Care 1979;2:154–160.
Ducimetiere D, Eschwege E, Papoz L, et al. Relationship of plasma insulin levels to the incidence of myocardial infarction and coronary heart disease mortality in middle-aged population. Diabetologia 1980;19:205–210.
Pyörälä K, Savolainen E, Kankola S, et al. Plasma insulin as coronary heart disease risk factor: relationship to other risk factors and predictive value during 9 ½ year follow-up of the Helsinki Policemen Study population. Acta Med Scand 1985;701 (suppl 1):38–52.
Eschwege E, Richard JL, Thibault N, et al. Coronary heart disease mortality in relation with diabetes, blood glucose and plasma insulin levels. The Paris Prospective Study, ten years later. Horm Metab Res 1985;15(suppl):41–46.
Haffner SM, Stern MP, Hazuda HP, et al. Hyperinsulinemia in a population at high risk for non-insulin-dependent diabetes mellitus. N Engl J Med 1986;315:220–224.
Welin L, Eriksson H, Larsson B, et al. Hyperinsulinemia is not a major coronary risk factor in elderly men. The study of men born in 1913. Diabetologia 1992;35:766–770.
Ferrara A, Barrett-Connor EL, Edelstein SL . Hyperinsulinemia does not increase the risk of fatal cardiovascular disease in elderly men or women without diabetes: the Rancho Bernardo Study, 1984–1991. Am J Epidemiol 1994;140:857–869.
Li AC, Glass CK . The macrophage foam cell as a target for therapeutic intervention. Nat Med 2002;8:1235–1242.
Kleemann R, Zadelaar S, Kooistra T . Cytokines and atherosclerosis: a comprehensive review of studies in mice. Cardiovasc Res 2008;79:360–376.
Febbraio M, Podrez EA, Smith JD, et al. Targeted disruption of the class B scavenger receptor CD36 protects against atherosclerotic lesion development in mice. J Clin Invest 2000;105:1049–1056.
de Winther MP, Hofker MH . Scavenging new insights into atherogenesis. J Clin Invest 2000;105:1039–1041.
Terpstra V, Kondratenko N, Steinberg D . Macrophages lacking scavenger receptor A show a decrease in binding and uptake of acetylated low-density lipoprotein and of apoptotic thymocytes, but not of oxidatively damaged red blood cells. Proc Natl Acad Sci USA 1997;94:8127–8131.
Van Eck M, Pennings M, Hoekstra M, et al. Scavenger receptor B1 and ATP-binding cassette transporter A1 in reverse cholesterol transport and atherosclerosis. Curr Opin Lipidol 2005;16:307–315.
Lindsay RS, Funahashi T, Hanson RL, et al. Adiponectin and development of type 2 diabetes in the Pima Indian population. Lancet 2002;360:57–58.
Deepa SS, Dong LQ . APPL1: role in adiponectin signaling and beyond. Am J Physiol Endocrinol Metab 2009;296:E22–E36.
Nawrocki AR, Rajala MW, Tomas E, et al. Mice lacking adiponectin show decreased hepatic insulin sensitivity and reduced responsiveness to peroxisome proliferator-activated receptor γ agonists. J Biol Chem 2006;281:2654–2660.
Yamauchi T, Kamon J, Waki H, et al. The fat-derived hormone adiponectin reverses insulin resistance associated with both lipoatrophy and obesity. Nat Med 2001;7:941–946.
Hotta K, Funahashi T, bodkin NL, et al. Circulating concentrations of the adipocyte protein adiponectin are decreased in parallel with reduced insulin sensitivity during the progression to type 2 diabetes in rhesus monkeys. Diabetes 2001;50:1126–1133.
Wang C, Mao X, Wang L, et al. Adiponectin sensitizes insulin signaling by reducing p70 S6 kinase-mediated serine phosphorylation of IRS-1. J Biol Chem 2007;282:7991–7996.
Ouchi N, Kihara S, Arita Y, et al. Adipocyte-derived plasma protein, adiponectin, suppresses lipid accumulation and class A scavenger receptor expression in human monocyte-derived macrophages. Circulation 2001;103:1057–1063.
Furukawa K, Hori M, Ouchi N, et al. Adiponectin down-regulates acyl-coenzyme A:cholesterol acyltransferase-1 in cultured human monocyte-derived macrophages. Biochem Biophys Res Commun 2004;317:831–836.
Podrez EA, Schmitt D, Hoff HF, et al. Myeloperoxidase-generated reactive nitrogen species convert LDL into an atherogenic form in vitro. J Clin Invest 1999;103:1547–1560.
Rye KA, Garrety KH, Barter PJ . Changes in the size of reconstituted high density lipoproteins during incubation with cholesteryl ester transfer protein: the role of apolipoproteins. J Lipid Res 1992;33:215–224.
Rahaman SO, Lennon DJ, Febbraio M, et al. A CD36-dependent signaling cascade is necessary for macrophage foam cell formation. Cell Metab 2006;4:211–221.
Robinet P, Wang Z, Hazen SL, et al. A simple and sensitive enzymatic method for cholesterol quantification in macrophages and foam cells. J Lipid Res 2010;51:3364–3369.
Liang CP, Han S, Okamoto H, et al. Increased CD36 protein as a response to defective insulin signaling in macrophages. J Clin Invest 2004;113:764–773.
Han J, Hajjar DP, Febbraio M, et al. Native and modified low density lipoproteins increase the functional expression of the macrophage class B scavenger receptor, CD36. J Biol Chem 1997;272:21654–21659.
Nagy L, Tontonoz P, Alvarez J, et al. Oxidized LDL regulates macrophage gene expression through ligand activation of PPARγ. Cell 1998;93:229–240.
Sugano R, Yamamura T, Harada-Shiba M, et al. Uptake of oxidized low-density lipoprotein in a THP-1 cell line lacking scavenger receptor A. Atherosclerosis 2001;158:351–357.
Tang CK, Yi GH, Yang JH, et al. Oxidized LDL upregulated ATP binding cassette transporter-1 in THP-1 macrophages. Acta Pharmacol Sin 2004;25:581–586.
Zhao Y, Van Berkel TJ, Van Eck M . Relative roles of various efflux pathways in net cholesterol efflux from macrophage foam cells in atherosclerotic lesions. Curr Opin Lipidol 2010;21:441–453.
Janabi M, Yamashita S, Hirano K, et al. Oxidized LDL-induced NF-kappa B activation and subsequent expression of proinflammatory genes are defective in monocyte-derived macrophages from CD36-deficient patients. Arterioscler Thromb Vasc Biol 2000;20:1953–1960.
Stout RW, Vallance-Owen J . Insulin and atheroma. Lancet 1969;i:1078–1080.
Ronnemaa T, Laakso M, Pyorala K, et al. High fasting plasma insulin is an indicator of coronary heart disease in non-insulin-dependent diabetic patients and nondiabetic subjects. Arterioscler Thromb 1991;11:80–90.
Standl E, Janka HU . High serum insulin concentrations in relation to other cardiovascular risk factors in macrovascular disease of type 2 diabetes. Horm Metab Res 1985;15 (Suppl):46–51.
Uusitupa MIJ, Niskanen LK, Siitonen O, et al. 5-year incidence of atherosclerotic vascular disease in relation to general risk factors, insulin level, and abnormalities in lipoprotein composition in non-insulin-dependent diabetic and nondiabetic subjects. Circulation 1990;82:27–36.
Plutzky J, Viberti G, Haffner S . Atherosclerosis in type 2 diabetes mellitus and insulin resistance: mechanistic links and therapeutic targets. J Diabetes Complications 2002;16:401–415.
Welham MJ, Bone H, Levings M, et al. Insulin receptor substrate-2 is the major 170-kDa protein phosphorylated on tyrosine in response to cytokines in murine lymphohematopoietic cells. J Biol Chem 1997;272:1377–1381.
Malide D, Davies-Hill TM, Levine M, et al. Distinct localization of GLUT-1, -3, and -5 in human monocyte-derived macrophages: effects of cell activation. Am J Physiol 1998;274:E516–E526.
Smith J, Su X, El-Maghrabi R, et al. Opposite regulation of CD36 ubiquitination by fatty acids and insulin: effects on fatty acid uptake. J Biol Chem 2008;283:13578–13585.
Okamoto Y, Kihara S, Ouchi N, et al. Adiponectin reduces atherosclerosis in apolipoprotein E-deficient mice. Circulation 2002;106:2767–2770.
Ouchi N, Kihara S, Arita Y, et al. Adipocyte-derived plasma protein, adiponectin, suppresses lipid accumulation and class A scavenger receptor expression in human monocyte-derived macrophages. Circulation 2001;103:1057–1063.
Tian L, Luo N, Klein RL, et al. Adiponectin reduces lipid accumulation in macrophage foam cells. Atheroscler 2009;202:152–161.
Podrez EA, Schmitt D, Hoff HF, et al. Myeloperoxidase-generated reactive nitrogen species convert LDL into an atherogenic form in vitro. J Clin Invest 1999;103:1547–1560.
Goldstein JL, Ho YK, Basu SK, et al. Binding site on macrophages that mediates uptake and degradation of acetylated low density lipoprotein, producing massive cholesterol deposition. Proc Nat Acad Sci 1979;76:333–337.
Fernández-Real JM, Ricart W . Insulin resistance and chronic cardiovascular inflammatory syndrome. Endocr Rev 2003;24:278–301.
Miller YI, Viriyakosol S, Worrall DS, et al. Toll-like receptor 4-dependent and -independent cytokine secretion induced by minimally oxidized low-density lipoprotein in macrophages. Arterioscler Thromb Vasc Biol 2005;25:1213–1219.
Ghanim H, Mohanty P, Deopurkar R, et al. Acute modulation of toll-like receptors by insulin. Diabetes Care 2008;31:1827–1831.
Iwasaki Y, Nishiyama M, Taguchi T, et al. Insulin exhibits short-term anti-inflammatory but long-term proinflammatory effects in vitro. Mol Cell Endocrinol 2009;298:25–32.
Ohashi K, Parker JL, Ouchi N, et al. Adiponectin promotes macrophage polarization toward an anti-inflammatory phenotype. J Biol Chem 2010;285:6153–6160.
Laing SP, Swerdlow AJ, Slater SD, et al. Mortality from heart disease in a cohort of 23 000 patients with insulin-treated diabetes. Diabetologia 2003;46:760–765.
Conway B, Costacou T, Orchard T . Is glycaemia or insulin dose the stronger risk factor for coronary artery disease in type 1 diabetes? Diab Vasc Dis Res 2009;6:223–230.
Shanik MH, Xu Y, Skrha J, et al. Insulin resistance and hyperinsulinemia: is hyperinsulinemia the cart or the horse? Diabetes Care 2008;31 (Suppl 2):S262–S268.
Acknowledgements
We are grateful to David Schmitt, Dr Xin-Min Li and Robert Koeth in Dr Stanley Hazen's laboratory at the Cleveland Clinic for helping us perform the cholesterol efflux assay and GC-MS. This study was supported by NIH P01 HL087018 (RLS) and a KL2 award (SK) from the Case Western Reserve University Clinical Translational Research Award UL1RR024989.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Laboratory Investigation website
The role of hyperinsulinemia in atherosclerosis has been controversial. Insulin and adiponectin are now shown to promote human macrophage foam cell formation by inducing cholesterol accumulation via increased CD36 expression and decreased ATP-binding cassette transporter ABCA1 expression. Therefore, hyperinsulinemia may contribute to atherosclerosis in patients with type 2 diabetes.
Supplementary information
Rights and permissions
About this article
Cite this article
Park, Y., R Kashyap, S., A Major, J. et al. Insulin promotes macrophage foam cell formation: potential implications in diabetes-related atherosclerosis. Lab Invest 92, 1171–1180 (2012). https://doi.org/10.1038/labinvest.2012.74
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.2012.74
Keywords
This article is cited by
-
Insulin Rescued MCP-1-Suppressed Cholesterol Efflux to Large HDL2 Particles via ABCA1, ABCG1, SR-BI and PI3K/Akt Activation in Adipocytes
Cardiovascular Drugs and Therapy (2022)
-
The “discordant doppelganger dilemma”: SGLT2i mimics therapeutic carbohydrate restriction - food choice first over pharma?
Journal of Human Hypertension (2021)
-
Analysis of Low Molecular Weight Substances and Related Processes Influencing Cellular Cholesterol Efflux
Pharmaceutical Medicine (2019)
-
CD36 overexpression: a possible etiopathogenic mechanism of atherosclerosis in patients with prediabetes and diabetes
Diabetology & Metabolic Syndrome (2017)
-
Multiple-stressor effects in an apex predator: combined influence of pollutants and sea ice decline on lipid metabolism in polar bears
Scientific Reports (2017)