Abstract
Translation of drug candidates into clinical settings requires demonstration of preclinical efficacy and formal toxicology analysis for filling an Investigational New Drug (IND) application with the US Food and Drug Administration (FDA). Here, we investigate the membrane-associated glucose response protein 78 (GRP78) as a therapeutic target in leukemia and lymphoma. We evaluated the efficacy of the GRP78-targeted proapoptotic drug bone metastasis targeting peptidomimetic 78 (BMTP-78), a member of the D(KLAKLAK)2-containing class of agents. BMTP-78 was validated in cells from patients with acute myeloid leukemia and in a panel of human leukemia and lymphoma cell lines, where it induced dose-dependent cytotoxicity in all samples tested. Based on the in vitro efficacy of BMTP-78, we performed formal good laboratory practice toxicology studies in both rodents (mice and rats) and nonhuman primates (cynomolgus and rhesus monkeys). These analyses represent required steps towards an IND application of BMTP-78 for theranostic first-in-human clinical trials.
Similar content being viewed by others
Introduction
Human cancers are characterized by abnormal activation of stress-response chaperones to inhibit apoptosis and regulate senescence and autophagy.1 Stress-response chaperones consist of two families: heat-shock proteins and glucose-regulated proteins (GRP). Among the latter, GRP78 has been widely studied as a biomarker of endoplasmic reticulum stress and an activator of the unfolded protein response;2 these processes have been related to drug resistance in tumor cells.3, 4 Unexpectedly, GRP78 has been found associated with the cell membrane in many cancer types, a feature that enables specific targeting by circulating ligands.5, 6, 7, 8 In addition to our original discovery of cell-surface GRP78, we have recently reported that GRP78 is upregulated and systemically accessible in aggressive variants of human prostate and breast cancer, and can thereby be exploited for theranostic purposes.9, 10
High expression of GRP78 and its localization at the cell surface in human B-lineage acute lymphoblastic leukemia is associated with disease relapse and chemotherapy resistance.11 GRP78-knockout mice show reduced multiplication of hematopoietic stem cells, loss of lymphoid and myeloid progenitors, and decreased lymphoid cell populations.5 Conditional knockout in the hematopoietic system indicates that GRP78 plays a mechanistic role both in leukemogenesis12 and in hematopoietic stem cell survival.13In preclinical studies, GRP78 induces AKT oncogenic signaling and leukemogenesis in PTEN-null mice,12 and its cell-surface association with Cripto is functional in hematopoietic stem cell quiescence.
In this study, we provide evidence that GRP78 accumulates on the surface of cells from patients with acute myeloid leukemia (AML), as well as on human leukemia and lymphoma cell lines, where it can serve as an accessible molecular target. As a leukemia/lymphoma-targeting agent, we tested bone metastasis targeting peptidomimetic-78 (BMTP-78), a prototype drug composed by a GRP78-binding peptide, WIFPWIQL,5, 7, 15 fused to the proapoptotic enantiomer D(KLAKLAK)2, which disrupts the mitochondrial membrane causing cell death.5, 7, 16 Previous work from our group revealed that BMTP-78 inhibits tumor growth and prolongs survival in preclinical models of breast and prostate cancer.5, 7 Our current results indicate that BMTP-78 exerts a dose-dependent cytotoxicity in vitro in a panel of human leukemia and lymphoma cell lines, as well as primary cells from patients with AML. The overall positive outcome of BMTP-78 treatment in several preclinical models of human cancers prompted us to conduct exploratory good laboratory practice (GLP) toxicology studies in rodents and nonhuman primates towards formal application of an Investigational New Drug (IND) with the US Food and Drug Administration (FDA).
Materials and methods
Human leukemia and lymphoma cell lines
The human cell lines were obtained from the Leukemia Cell and Tissue Bank of the Department of Leukemia at The University of Texas MD Anderson Cancer Center (UTMDACC). The panel included MOLT-4 and CCRF-CEM (T-cell acute lymphoblastic leukemia, ALL), HL-60 (acute promyeolocytic leukemia, APML), OCI-AML3 (acute myeloid leukemia, AML), THP-1 (monocytic acute leukemia), K562 and KBM7 (chronic myelogenous leukemia (CML)), SR-786 (anaplastic large T-cell lymphoma), U937 and TUR (monocytic lymphomas), TF-1 (erythroleukemia) and RPMI-8226 (multiple myeloma). Cells were maintained in standard humidified hypoxia chambers (HeraCell 150; Thermo Electron Corporation, Waltham, MA, USA) with 5% CO2 and 5% O2 at 37 °C in RPMI-1640 containing 10% fetal bovine serum, L-glutamine (0.292 mg ml−1), penicillin (100 U ml−1), and streptomycin (100 U ml−1).
Patient-derived leukemia cells and non-malignant controls
Cells from peripheral blood were obtained from the Human Tissue Repository at the University of New Mexico Comprehensive Cancer Center (UNMCCC). All procedures were reviewed and approved by the Institutional Scientific Review Committee and Institutional Review Board.
Blood samples were obtained from adult AML patients (n=3) and from healthy volunteers (n=3). Mononuclear cells were isolated using Ficoll-Paque Plus (GE Healthcare, Little Chalfont, UK).
Synthetic peptides
The peptides used in this study were synthesized by Polypeptide Laboratories under good manufacturing practice conditions, purified by high-performance liquid chromatography, and lyophilized. Reconstituted material was stable and maintained its potency through preparation and infusion. BMTP-78 is a synthetic peptidomimetic composed of the GRP78-binding motif WIFPWIQL fused to the proapoptotic enantiomer D(KLAKLAK)2 through a Gly-Gly linker.
Flow cytometry of cell lines
One hundred thousand cells were blocked in phosphate-buffered saline (PBS) containing 10 μg ml−1 human immunoglobulins (Sigma-Aldrich, St. Louis, MO, USA) for 30 min on ice. Cells were successively incubated with goat anti-GRP78 antibody (Santa Cruz Biotechnology, Dallas, TX, USA; Clone C-20 or N-20) in labeling buffer (PBS containing 0.2% bovine serum albumin, 0.1% sodium azide (NaN3) and 5% heat-inactivated donkey serum) on ice for 1 h, washed with washing buffer (PBS containing 0.2 bovine serum albumin and 0.1% NaN3) and incubated with a phycoerythrin-conjugated anti-goat antibody in labeling buffer for 30 min. After additional rinsing in washing buffer, cells were resuspended in PBS containing 0.2% bovine serum albumin and analyzed by flow cytometry (BD FACS Canto II, BD Bioscience, San Jose, CA, USA).
Flow cytometry of primary cells
Mononuclear cells were isolated from peripheral blood with Ficoll-Plaque PLUS (GE Heathcare, Little Chalfont, UK) and blocked in human immunoglobulins as described above. The mouse monoclonal anti-GRP78 (clone [10c3]; Abcam, Cambridge, UK) and control isotype antibodies were conjugated to phycoerythrin with the Lightning-Link R-Phycoerythrin Kit (Innova Biosciences, Cambridge, UK). Cells were double stained with anti-CD33 (conjugated to PercP-Cy5.5) and anti-CD34 (conjugated to allophycocyanin) antibodies (both eBioscience, Thermo Fisher Scientific, Waltham, MA, USA) for 1 h in the dark and on ice. Cells were analyzed with a BD Accuri C6 flow cytometer (BD Bioscience, San Jose, CA, USA). Data were processed with FlowJo software package (V.10.0.8; FlowJo LLC, Ashland, OR).
Cell viability and apoptosis assays
For the viability assays, cells were seeded in 96-well plates (2 × 104 cells per well) in complete medium, and incubated overnight at 37 °C with increasing concentrations of either BMTP-78 or an admixture of WIFPWIQL and D(KLAKLAK)2 at equimolar concentrations (negative control). Viability was determined by measuring the cytoplasmic lactate dehydrogenase enzymatic activity with DHL Cell Viability and Proliferation Assay Kit (AnaSpec, Fremont, CA, USA). For the apoptosis assays, OCI-AML cells were seeded in 6-well plates (2 × 105 cells per well), and incubated overnight at 37 °C with 20 μM of either BMTP-78 or the control admixture, followed by staining with FITC-conjugated Annexin V and propidium iodide (Sigma), and flow cytometry with a BD FACS Canto II (BD Bioscience, San Jose, CA, USA).
Statistical analysis
All data are reported as the average mean±s.e.m. Student’s t-test (unpaired) was used to determine statistical significance. P-values are represented as follows: *P<0.05 or **P<0.01.
BMTP-78 toxicology in rodents
Two studies were conducted with BMTP-78 in CD-1 female mice and Sprague–Dawley male rats at the UTMDACC Michale E Keeling Center for Comparative Medicine and Research (Bastrop, TX, USA). The preliminary 5-day range-finding study consisted of six groups of five CD-1 mice that received a single intravenous or subcutaneous dose of BMTP-78 (30, 100, or 200 mg kg−1). A 14-day single-dose range-finding study was performed in Sprague–Dawley rats. This study was designed as 5-day single dose (subcutaneous) followed by a 9-day recovery period, and consisted of four groups of five rats (5, 15, 50 or 150 mg kg−1). In both studies, the control group was treated with vehicle alone. All animals were observed before dose initiation, and on days 1, 5, 14, and 28. Daily observations for signs of toxicity and body weights were recorded. At termination, animals were killed and subjected to complete necropsy with histological evaluation of select tissues. The number of animals, doses and schedule for these studies are shown in Supplementary Table 1.
BMTP-78 study in nonhuman primates
Five GLP toxicology studies were conducted in cynomolgus monkeys (Macaca fascicularis) and rhesus monkeys (Macaca mulatta) at the UTMDACC Michale E Keeling Center for Comparative Medicine and Research (Bastrop, TX, USA). Initial average animal weight was 5–9 kg; all animals were initially healthy with no history of chronic illness or injury. BMTP-78 was administered as a single infusion or multiple doses through a peripheral venous catheter. The number of animals, doses and schedules are shown in Table 1. Over the course of the study, the animals were observed two times daily for clinical signs of toxicity, including observations at 1 and 2 h postinfusion on the days of BMTP-78 administration. Body weights were measured weekly, and blood and urine were collected for clinicopathological analysis. At the time of killing, all monkeys were subjected to full necropsy, with tissues collected and processed for histopathological evaluation. Tissues were fixed in 10% neutral-buffered formalin, processed and embedded in paraffin, sectioned at 4–5 μm and stained with hematoxylin and eosin. Eyes were fixed in Davidson’s solution (30 ml of 95% ethyl alcohol, 20 ml of 10% neutral-buffered formalin, 10 ml glacial acetic acid, 30 ml of water), before processing and paraffin embedding. All GLP studies (rodents and primates) were registered with the FDA.
Results
Expression of the surface-associated GRP78 in peripheral blood cells of AML patients
To evaluate GRP78 as a potential target in leukemia, we analyzed its expression on the membrane of patient-derived cells by flow cytometry. The amount of surface-associated GRP78 on peripheral blood cells was markedly increased in all AML samples (46.6±3.9%) in comparison with normal healthy donors (3.6±1.0%) (Figure 1a). To investigate the tumor cell populations expressing GRP78, we used CD33 and CD34 in double staining with an anti-GRP78 antibody. CD33 is a specific myeloid receptor expressed in leukemic blasts and stem cells in AML,17, 18 and CD34 is a marker of immature leukemic cells and leukemic stem cells.19, 20
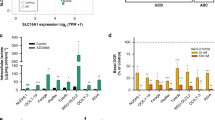
Detection of cell surface-associated glucose response protein 78 (GRP78) in leukemia. (a) The expression of GRP78 was studied in mononuclear cells isolated from peripheral blood of patients with acute myeloid leukemia (AML) compared with healthy donors. Ficoll-purified cells were stained with phycoerythrin (PE)-conjugated anti-GRP78 or control isotype antibody. Cells were double-stained with PE-conjugated anti-GRP78 plus (b) PercP-Cy5.5-conjugated anti-human CD33 or (c) allophycocyanin (APC)-conjugated anti-human CD34 antibody. (d) Leukemia cell lines (OCI-AML3, K562 and KBM-7) were stained with PE-conjugated anti-GRP78 or control isotype antibody and analyzed by flow cytometry. Non-stained cells were used as a negative control. The percentage of double-stained cells is represented. *P<0.05; **P<0.01.
In patients with AML, 26.6±3.3% of the peripheral blood cells positive for CD33 were also positive for GRP78 (Figure 1b). In healthy donors, the percentage of CD33+/GRP78+ cells was as low as 1.4±0.4%. AML patients showed elevated numbers of CD34+ cells, which were specifically costained for GRP78 (37.3±9.4%; compare with healthy donors, 1.4±0.6%) (Figure 1c). Given the presence of GRP78 on the surface of leukemia cells from patients, we evaluated its expression in leukemia cell lines, including OCI-AML3 cells derived from the primary blast of an AML patient,21 and K562 and KBM-7 cells from patients with chronic myelogenous leukemias. All cells showed specific staining for surface GRP78 (Figure 1d). These results show that GRP78 is expressed on the surface of human primary AML cells and leukemia cell lines, confirming previous studies where overexpression of unfolded protein response genes, including GRP78, was reported in AML patients.22
BMTP-78 reduces the viability of human leukemia and lymphoma cells
We have previously demonstrated that BMTP-78 selectively kills breast and prostate cancer cells, reducing both primary tumor growth and secondary spreading to the lungs and bones in mouse models.7 Here, we tested whether GRP78 could serve as a target for BMTP-78 in a panel of human leukemia and lymphoma cell lines. All the cell lines tested were highly sensitive to BMTP-78: markedly reduced cell viability was observed at low molar concentrations, and, in most cases, the maximum cytotoxic effect was reached at⩽10 μM (Figure 2). No detectable effect was observed with the control, which consisted of an equimolar admixture of WIFPWIQL and D(KLAKLAK)2. The effect of BMTP-78 on cell viability was also evaluated in primary cells from patients with AML. Three specimens of peripheral blood with 65–78% blasts were incubated with increasing molar concentrations of BMTP-78 or control peptides (Figure 3). Notably, higher molar concentrations of BMTP-78 were necessary to decrease cell viability in primary human leukemia cells compared with the above-described cell lines: a complete loss of cell viability was observed at 10–30 μM. The negative control admixture had no detectable effects. Collectively, these results demonstrate the efficacy of BMTP-78 in reducing cell viability of established leukemia and lymphoma cell lines as well as of peripheral blasts from AML patients.
Effect of bone metastasis targeting peptidomimetic 78 (BMTP-78) on cell viability. A panel of human leukemia and lymphoma cell lines was treated with increasing concentrations of BMTP-78 or control peptides. Cell viability was measured by lactate dehydrogenase (LDH) activity. Results represent the average of three independent experiments. Acute myeloid leukemia (AML), acute lymphoblastic leukemia (ALL) and chronic myelogenous leukemia (CML).
Drug activity of bone metastasis targeting peptidomimetic 78 (BMTP-78) in primary human leukemia cells. Peripheral blood cells purified from three acute myeloid leukemia (AML) patients were incubated with increasing concentrations of BMTP-78 or control peptides. Cell viability was measured via lactate dehydrogenase (LDH) enzymatic activity.
BMTP-78 induces apoptosis in human leukemia cells
We next evaluated morphologic changes in OCI-AML3 cells incubated for 16 h with 20 μM of either BMTP-78 or the control admixture of WIFPWIQL plus D(KLAKLAK)2. On microscopic analysis, cells treated with the control peptides showed a regular morphology, as opposed to cells treated with BMTP-78, which appeared ‘shrunken’ and fragmented into characteristic apoptotic bodies (Figure 4). The double positivity for annexin V and propidium iodide in >70% of BMTP-78-treated cells confirmed the microscopic assessments. In contrast, cells treated with the control admixture exhibited only background levels of cell death (~5%). We concluded that BMTP-78 induces apoptosis in leukemia cells by specifically targeting cell surface-associated GRP78.
Effect of bone metastasis targeting peptidomimetic 78 (BMTP-78) on cell death by apoptosis. OCI-AML3 cells were treated for 16 h with BMTP-78 or control peptides (20 μM), followed by staining with Annexin V/propidium iodide (PI) to detect the percentage of apoptotic cells by flow cytometry. Untreated OCI-AML3 cells served to determine background levels of cell death under the same experimental conditions.
Toxicology studies with BMTP-78 in rodents
An initial dose range-finding study of BMTP-78 was performed in female CD-1 mice (n=5 animals per group) dosed at 30, 100 and 200 mg kg−1 (intravenously or subcutaneously). Two control groups were injected intravenously or subcutaneously with vehicle only (PBS). Similar signs of toxicity were noted in all treatment groups regardless of the administration route. Affected organs/tissues were: injection sites, lymphoid tissues, lungs, kidneys and gastrointestinal tract. The lesions were characterized as degenerative, regenerative and/or inflammatory in nature. In most cases, renal and/or immune failure was considered as the cause of death after BMTP-78 administration. Body weights decreased in all mice treated with BMTP-78 (Supplementary Table 1). All mice in control groups appeared normal during the study.
Successively, we performed a 5-day single dose followed by a 9-day recovery period in Sprague–Dawley male rats (n=5 animals per group) administered subcutaneously with BMTP-78 at 5, 15, 50 and 150 mg kg−1. In each group, two animals were killed at day 5, and three at day 14. The incidence and severity of BMTP-78-related lesions occurred in a dose-dependent manner, and were more severe in the two high-dose groups (50 and 150 mg kg−1), where all animals were dead or moribund at day 3. The 15 mg kg−1 dose appeared to be the midpoint of BMTP-78-related toxicity: three out of five animals were found dead by day 3. All animals in the 5 mg kg−1 treatment group survived to study termination with minimal lesions. Body weights in the high-dose groups (50 and 150 mg kg−1) were lower compared with the low-dose (5 mg kg−1) and vehicle groups. Most affected were the kidneys, but alterations were also seen in the spleen, lymph nodes and at injection sites. Kidney lesions were generally degenerative/necrotic in nature in the high-dose groups and regenerative in the low-dose groups. Renal failure was considered a cause of spontaneous death in these rats. Given the promising toxicology profile of BMTP-78 at low doses observed in rodents, we used these results to enable a dose-range selection for subsequent studies in nonhuman primates.
Toxicology studies with BMTP-78 in nonhuman primates
Within the class of D(KLAKLAK)2-containing compounds, we have previously evaluated GLP toxicities of agents against obesity (adipotide23, 24) and cancer (BMTP-11; refs 25, 26). We reported that these BMTP-78-like compounds induce reversible renal toxicity and no adverse side effects in monkeys.24, 26 Inspired by these findings and by the above-described efficacy in vitro and in animal models, we evaluated BMTP-78 toxicology profiles in nonhuman primates. Five studies were designed, including single and multiple dose regimens, along with dose-range determination and repeated infusion for the assessment of BMTP-78 safety (Table 1).
Preliminarily, a dose-escalating study (study no. 1) was performed in cynomolgus monkeys (n=3) serially dosed with BMTP-78 at 0.3, 3, 100 and 200 mg kg−1 via subcutaneous administration every 3 days for 2 weeks. The study was terminated after the administration of 100 mg kg−1 dose due to BMTP-78-related toxicity at the injection site and in the kidneys of all monkeys. In the subsequent study (study no. 2), cynomolgus monkeys (n=3) were scheduled to receive weekly intravenous doses (n=4) of BMTP-78 at 3 mg kg−1. Two animals had complications and were killed after receiving a single dose of BMTP-78; one received all doses, but presented with necrotizing and inflammatory lesions at the intravenous injection site. Kidney lesions (cortical tubular necrosis) were also observed in one of the monkeys after a single dose. A substantially lower dose (0.75 mg kg−1) of BMTP-78 was administered to cynomolgus monkeys (n=2) (study no. 3) and no adverse effects were detected.
A second dose-ranging study (1–9 mg kg−1) in rhesus monkeys (study no. 4) included four animals that were scheduled to receive four weekly intravenous doses of BMTP-78. The animal that received the highest dose (9 mg kg−1) completed only two infusions and was killed shortly after the second week of treatment; the necropsy revealed a cardiac lesion not seen in the previous GLP toxicology studies. The lesion was present in the myocardium of the intraventricular septum and was degenerative and fibrotic. Although the animals that received the low (1 mg kg−1), mid-low (3 mg kg−1) and mid-high (6 mg kg−1) doses completed the 4 weeks of treatment, kidney toxicity was observed in the animals treated with 3 and 6 mg kg−1 of BMTP-78, including tubular necrosis/degeneration and/or regeneration. Few necrotic foci were observed in the mid-low dose (3 mg kg−1), minimal necrotic changes in the mid-high dose (6 mg kg−1) and mild necrotic changes in the high dose (9 mg kg) animal. Similar to the monkeys in study no. 2, lesions were also observed at the injection site of the monkeys in the mid-low and mid-high doses. A description of protocols and the summary of results are presented in Table 1.
Finally, we tested BMTP-78 safety in a large cohort of female rhesus monkeys (n=20), with four intravenous infusions over a 22-day period, followed by a 29-day recovery period (study no. 5, Supplementary Table 2). The 20 animals were randomized in one control group (45% saline) and low (3 mg kg−1) to high (30 mg kg−1) dose groups. Each monkey was scheduled to receive BMTP-78 as a 2-h infusion once weekly. Two animals in the high dose group (30 mg kg−1) presented with fatal cardiac arrhythmias shortly after the initial injection. A third animal received a single dose of 15 mg kg−1 and also developed heart arrhythmia with irreversible cardiac arrest. Two additional animals receiving the mid-high dose (9 mg kg−1) of BMTP-78 developed fatal arrhythmias, one after the first infusion and one after the third. The other animals in the group developed tachycardia during all four infusions. At the low dose (3 mg kg−1), all five animals displayed sinus tachycardia after the fourth infusion. In contrast with higher doses, this sinus tachycardia did not convert to life-threatening ventricular arrhythmias. Owing to the severe heart toxicity and the risk of fatal cardiac arrhythmias, the GLP toxicology studies were terminated early in an abrogated manner, as required by the FDA.
Altogether these studies led to the conclusion that, despite the promising antitumor effect of BMTP-78 in vitro and in preclinical cancer models, the current formulation is not suitable to be pursued for cancer treatment because of unexpected cardiac toxicity resulting in unanticipated morbidity and mortality.
Discussion
The expression of stress-related proteins has been reported in many solid tumors as a response to unfavorable microenvironment conditions such as hypoxia and glucose deprivation.1, 27 In the bone marrow, low oxygen levels are observed in the endosteal area where hematopoietic stem cells are maintained in a quiescent niche while maintaining a pluripotent state.28 This phenomenon results from the activation of hypoxia-inducible factor 1 and other targets including VEGFA, CXCR4 and the Cripto/GRP78 complex.14, 29, 30 The levels of surface-associated GRP78 have been used to distinguish two populations of hematopoietic stem cells: one, characterized as GRP78+/CD34−, seems to be a myeloid-biased lineage with slow engraft reconstitution ability, while the other (GRP78−/CD34−) tends to generate a compromised lymphoid lineage.31 In hematopoietic malignancies, disease progression has been linked to vast expansion of hypoxic areas within the bone marrow and overexpression of the GRP78-binding partner Cripto32 to form a supramolecular complex on the cell surface. Consistent with these findings, elevated expression of surface-associated GRP78 has been described in several tumor types,5, 6, 7, 8, 9, 10, 33 most of which are characterized by a hypoxic microenvironment. The mechanism of GRP78 relocation from the ER to the plasma membrane seems to be dependent on hypoxia and nutrient deprivation;34 therefore, its association with coreceptors that trigger cell proliferation and prevent apoptosis is considered a hallmark of cancer cells.
Here we report the expression of surface-associated GRP78 in cells from patients with AML, as well as in different human leukemia cell lines. Our results explore whether GRP78 would be an accessible molecular target for drug delivery, by extending previous results in which expression of surface-associated GRP78 was shown in B-cell acute lymphoblastic leukemia11 and chronic lymphocytic leukemia.35 To address this hypothesis, we tested the GRP78-targeted peptidomimetic BMTP-78 in vitro in a panel of human leukemia and lymphoma cell lines and primary cells from patients with AML. BMTP-78 reduced cell viability in all conditions tested and at a lower concentration (<10 μM) than BMTP-11 (60–80 μM36), an IL11-Rα-targeting drug that has been recently evaluated in a first-in-man clinical trial.26 BMTP-78 treatment resulted in apoptosis, confirming that this compound, like BMTP-1125, 26 and adipotide,23, 24 induces cell death by a ligand-specific pathway.
Despite the promising antitumor effects of BMTP-78 in vitro and in preclinical tumor models,5, 7 and a favorable toxicity profile in rodents at low doses, its current formulation has shown unexpected side effects in primates, thereby deeming this drug candidate unsuitable for clinical testing. Of note, BMTP-78-related toxicity was not observed in therapeutic studies with tumor-bearing mice, probably due the dose used (15 mg kg−1).6, 8 Toxic effects in mice were observed at 30 mg kg−1 and above, although in rats 15 mg kg−1 was already considered a midpoint for the drug test. Interestingly, no cardiac abnormalities were observed in any toxicology studies performed in rodents. The D(KLAKLAK)2 proapoptotic moiety has been extensively used by us5, 7, 16, 37 and others38, 39, 40, 41 to develop ligand-directed therapeutics, and two of our most advanced D(KLAKLAK)2-based formulations have been successfully granted safe-to-proceed and translated into FDA-approved clinical trials.24, 26 These observations allow excluding a causative involvement of D(KLAKLAK)2 in the observed adverse events. We speculate that the biochemical features of WIFPWIQL, for example, its high content in hydrophobic residues (Ile, Phe, Pro, Leu, Trp) might contribute to its insolubility and tissue-specific toxicity. Of note, WIFPWIQL was originally identified by an in silico analysis,15 as opposed to other targeting peptides that our group has selected via in vivo screenings and that have been exploited in formulations compatible with preclinical and/or clinical studies. Further investigation is needed to assess a potential toxicity profile of WIFPWIQL. Meanwhile, we have recently identified a new GRP78-targeting motif from an in vivo phage display selection in a patient-derived xenograft model of prostate cancer.10, 42, 43 This peptide, SNTRVAP, might therefore resolve the toxicity issues of the current BMTP-78 formulation.
In the present work, we describe and confirm the presence of membrane-associated GRP78 in human leukemia cells and investigate the targeting of GRP78 with BMTP-78. We conclude that the first generation of BMTP-78 should no longer be pursued in clinical testing because of its unacceptable toxicity profile in nonhuman primates. However, several aspects merit further comment. First, BMTP-78 will likely still be useful as a molecular imaging probe, because the molar doses used would be several orders of magnitude lower. As such, a study of WIFPWIQL conjugated to 1,4,7,10-tetraazacyclododecane-1,4,7,10-tetraacetic acid (DOTA) for PET imaging is currently under planning with the lead-labeled compound already synthesized in good manufacturing practice grade (unpublished observations). Moreover, as mentioned, a next-generation GRP78 ligand has been selected and validated for therapeutic applications.10, 42 Collectively, this GLP toxicology study serves as a cautionary note in which species-specific toxicity must be taken into account during preclinical drug development. The fact that the toxicity profile of BMTP-78 in rodents was essentially indistinguishable from adipotide24 and BMTP-11,26 but the nonhuman primate study showed unexpected cardiac toxicity in the form of lethal heart arrhythmias, is quite remarkable and should give pause to drug development efforts. Nevertheless, despite the toxicity of BMTP-78 described herein, the accessibility of GRP78 and its potential as a target remain a path to be pursued for the treatment of hematopoietic malignancies.
References
Li J, Lee AS . Stress induction of GRP78/BiP and its role in cancer. Curr Mol Med 2006; 6: 1 45–54.
Lee AS . The ER chaperone and signaling regulator GRP78/BiP as a monitor of endoplasmic reticulum stress. Methods 2005; 35: 373–381.
Ranganathan AC, Zhang L, Adam AP, Aguirre-Ghiso JA . Functional coupling of p38- induced up-regulation of BiP and activation of RNA-dependent protein kinase-like endoplasmic reticulum kinase to drug resistance of dormant carcinoma cells. Cancer Res 2006; 66: 1702–1711.
Reddy RK, Mao C, Baumeister P, Austin RC, Kaufman RJ, Lee AS . Endoplasmic reticulum chaperone protein GRP78 protects cells from apoptosis induced by topoisomerase inhibitors: role of ATP binding site in suppression of caspase-7 activation. J Biol Chem 2003; 278: 20915–20924.
Arap MA, Lahdenranta J, Mintz PJ, Hajitou A, Sarkis AS, Arap W et al. Cell surface expression of the stress response chaperone GRP78 enables tumor targeting by circulating ligands. Cancer Cell 2004; 6: 275–284.
Liu Y, Steiniger SC, Kim Y, Kaufmann GF, Felding-Habermann B, Janda KD . Mechanistic studies of a peptidic GRP78 ligand for cancer cell-specific drug delivery. Mol Pharm 2007; 4: 435–447.
Miao YR, Eckhardt BL, Cao Y, Pasqualini R, Argani P, Arap W et al. Inhibition of established micrometastases by targeted drug delivery via cell surface-associated GRP78. Clin Cancer Res 2013; 19: 2107–2116.
Mintz PJ, Kim J, Do KA, Wang X, Zinner RG, Cristofanilli M et al. Fingerprinting the circulating repertoire of antibodies from cancer patients. Nat Biotechnol 2003; 21: 57–63.
Ferrara F, Staquicini DI, Driessen WH, D'Angelo S, Dobroff AS, Barry M et al. Targeted molecular-genetic imaging and ligand-directed therapy in aggressive variant prostate cancer. Proc Natl Acad Sci USA 2016; 113: 12786–12791.
Dobroff AS, D'Angelo S, Eckhardt BL, Ferrara F, Staquicini DI, Cardó-Vila M et al. Towards a transcriptome-based theranostic platform for unfavorable breast cancer phenotypes. Proc Natl Acad Sci USA 2016; 113: 12780–12785.
Uckun FM, Qazi S, Ozer Z, Garner AL, Pitt J, Ma H et al. Inducing apoptosis in chemotherapy-resistant B-lineage acute lymphoblastic leukaemia cells by targeting HSPA5, a master regulator of the anti-apoptotic unfolded protein response signalling network. Br J Haematol 2011; 153: 741–752.
Wey S, Luo B, Tseng CC, Ni M, Zhou H, Fu Y et al. Inducible knockout of GRP78/BiP in the hematopoietic system suppresses Pten-null leukemogenesis and AKT oncogenic signaling. Blood 2012; 119: 817–825.
Wey S, Luo B, Lee AS . Acute inducible ablation of GRP78 reveals its role in hematopoietic stem cell survival, lymphogenesis and regulation of stress signaling. PLoS ONE 2012; 7: e39047.
Miharada K, Karlsson G, Rehn M, Rorby E, Siva K, Cammenga J et al. Cripto regulates hematopoietic stem cells as a hypoxic-niche-related factor through cell surface receptor GRP78. Cell Stem Cell 2011; 9: 330–344.
Blond-Elguindi S, Cwirla SE, Dower WJ, Lipshutz RJ, Sprang SR, Sambrook JF et al. Affinity panning of a library of peptides displayed on bacteriophages reveals the binding specificity of BiP. Cell 1993; 75: 717–728.
Ellerby HM, Arap W, Ellerby LM, Kain R, Andrusiak R, Rio GD et al. Anti-cancer activity of targeted pro-apoptotic peptides. Nat Med 1999; 5: 1032–1038.
Dinndorf PA, Andrews RG, Benjamin D, Ridgway D, Wolff L, Bernstein ID . Expression of normal myeloid-associated antigens by acute leukemia cells. Blood 1986; 67: 1048–1053.
Taussig DC, Pearce DJ, Simpson C, Rohatiner AZ, Lister TA, Kelly G et al. Hematopoietic stem cells express multiple myeloid markers: implications for the origin and targeted therapy of acute myeloid leukemia. Blood 2005; 106: 4086–4092.
Bonnet D, Dick JE . Human acute myeloid leukemia is organized as a hierarchy that originates from a primitive hematopoietic cell. Nat Med 1997; 3: 730–737.
Warner JK, Wang JC, Takenaka K, Doulatov S, McKenzie JL, Harrington L et al. Direct evidence for cooperating genetic events in the leukemic transformation of normal human hematopoietic cells. Leukemia 2005; 19: 1794–1805.
Wang C, Curtis JE, Minden MD, McCulloch EA . Expression of a retinoic acid receptor gene in myeloid leukemia cells. Leukemia 1989; 3: 264–269.
Schardt JA, Weber D, Eyholzer M, Mueller BU, Pabst T . Activation of the unfolded protein response is associated with favorable prognosis in acute myeloid leukemia. Clin Cancer Res 2009; 15: 3834–3841.
Kolonin MG, Saha PK, Chan L, Pasqualini R, Arap W . Reversal of obesity by targeted ablation of adipose tissue. Nat Med 2004; 10: 625–632.
Barnhart KF, Christianson DR, Hanley PW, Driessen WH, Bernacky BJ, Baze WB et al. A peptidomimetic targeting white fat causes weight loss and improved insulin resistance in obese monkeys. Sci Transl Med 2011; 3: 108ra112.
Cardó-Vila M, Marchiò S, Sato M, Staquicini FI, Smith TL, Bronk JK et al. Interleukin-11 Receptor Is a Candidate Target for Ligand-Directed Therapy in Lung Cancer: Analysis of Clinical Samples and BMTP-11 Preclinical Activity. Am J Pathol 2016; 186: 2162–2170.
Pasqualini R, Millikan RE, Christianson DR, Cardó-Vila M, Driessen WH, Giordano RJ et al. Targeting the interleukin-11 receptor alpha in metastatic prostate cancer: A first-in-man study. Cancer 2015; 121: 2411–2421.
Lee AS . Glucose-regulated proteins in cancer: molecular mechanisms and therapeutic potential. Nat Rev Cancer 2014; 14: 263–276.
Semenza GL . Oxygen-dependent regulation of mitochondrial respiration by hypoxia-inducible factor 1. Biochem J 2007; 405: 1–9.
Takubo K, Goda N, Yamada W, Iriuchishima H, Ikeda E, Kubota Y et al. Regulation of the HIF-1alpha level is essential for hematopoietic stem cells. Cell Stem Cell 2010; 7: 391–402.
Benito J, Zeng Z, Konopleva M, Wilson WR . Targeting hypoxia in the leukemia microenvironment. Int J Hematol Oncol 2013; 2: 279–288.
Miharada K, Karlsson G, Rehn M, Rorby E, Siva K, Cammenga J et al. Hematopoietic stem cells are regulated by Cripto, as an intermediary of HIF-1alpha in the hypoxic bone marrow niche. Ann NY Acad Sci 2012; 1266: 55–62.
Wellmann S, Guschmann M, Griethe W, Eckert C, von Stackelberg A, Lottaz C et al. Activation of the HIF pathway in childhood ALL, prognostic implications of VEGF. Leukemia 2004; 18: 926–933.
Dong D, Ko B, Baumeister P, Swenson S, Costa F, Markland F et al. Vascular targeting and antiangiogenesis agents induce drug resistance effector GRP78 within the tumor microenvironment. Cancer Res 2005; 65: 5785–5791.
Zhang Y, Liu R, Ni M, Gill P, Lee AS . Cell surface relocalization of the endoplasmic reticulum chaperone and unfolded protein response regulator GRP78/BiP. J Biol Chem 2010; 285: 15065–15075.
Huergo-Zapico L, Gonzalez-Rodriguez AP, Contesti J, Gonzalez E, Lopez-Soto A, Fernandez-Guizan A et al. Expression of ERp5 and GRP78 on the membrane of chronic lymphocytic leukemia cells: association with soluble MICA shedding. Cancer Immunol Immunother 2012; 61: 1201–1210.
Karjalainen K, Jaalouk DE, Bueso-Ramos C, Bover L, Sun Y, Kuniyasu A et al. Targeting IL11 receptor in leukemia and lymphoma: a functional ligand-directed study and hematopathology analysis of patient-derived specimens. Clin Cancer Res 2015; 21: 3041–3051.
Karjalainen K, Jaalouk DE, Bueso-Ramos CE, Zurita AJ, Kuniyasu A, Eckhardt BL et al. Targeting neuropilin-1 in human leukemia and lymphoma. Blood 2011; 117: 920–927.
Burns KE, McCleerey TP, Thevenin D . pH-selective cytotoxicity of pHLIP-antimicrobial peptide conjugates. Sci Rep 2016; 6: 28465.
Daquinag AC, Tseng C, Zhang Y, Amaya-Manzanares F, Florez F, Dadbin A et al. Targeted proapoptotic peptides depleting adipose stromal cells inhibit tumor growth. Mol Ther 2016; 24: 34–40.
Mai JC, Mi Z, Kim SH, Ng B, Robbins PD . A proapoptotic peptide for the treatment of solid tumors. Cancer Res 2001; 61: 7709–7712.
Marks AJ, Cooper MS, Anderson RJ, Orchard KH, Hale G, North JM et al. Selective apoptotic killing of malignant hemopoietic cells by antibody-targeted delivery of an amphipathic peptide. Cancer Res 2005; 65: 2373–2377.
Mandelin J, Cardó-Vila M, Driessen WH, Mathew P, Navone NM, Lin SH et al. Selection and identification of ligand peptides targeting a model of castrate-resistant osteogenic prostate cancer and their receptors. Proc Natl Acad Sci USA 2015; 112: 3776–3781.
Li ZG, Mathew P, Yang J, Starbuck MW, Zurita AJ, Liu J et al. Androgen receptor-negative human prostate cancer cells induce osteogenesis in mice through FGF9-mediated mechanisms. J Clin Invest 2008; 118: 2697–2710.
Acknowledgements
This work was supported by the Specialized Program in Research Excellence (SPORE) in Leukemia from The University of Texas MD Anderson Cancer Center (to RP and WA), the Gillson-Longenbaugh Foundation (to RP and WA) and The Kimberly Patterson Fellowship for Leukemia Research (to DEJ).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
RP and WA are founders and equity stockholders of Alvos Therapeutics (Arrowhead Pharmaceuticals Research Corporation, Pasadena, CA, USA). Arrowhead Pharmaceuticals has licensed rights to patents and technologies described in this article. RP and WA are inventors on patent applications and intellectual property related to this work and will be entitled to standard royalties if licensing and/or commercialization occur. The University of New Mexico Health Sciences Center manages and monitors these arrangements, along with the University of Texas MD Anderson Cancer Center. The other authors declare that they have no competing interests.
Additional information
Supplementary Information accompanies the paper on the The Pharmacogenomics Journal website
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Staquicini, D., D'Angelo, S., Ferrara, F. et al. Therapeutic targeting of membrane-associated GRP78 in leukemia and lymphoma: preclinical efficacy in vitro and formal toxicity study of BMTP-78 in rodents and primates. Pharmacogenomics J 18, 436–443 (2018). https://doi.org/10.1038/tpj.2017.46
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/tpj.2017.46