Abstract
Major depressive disorder is a debilitating condition with a lifetime risk of ten percent. Most treatments take several weeks to achieve clinical efficacy, limiting the ability to bring instant relief needed in psychiatric emergencies. One intervention that rapidly alleviates depressive symptoms is sleep deprivation; however, its mechanism of action is unknown. Astrocytes regulate responses to sleep deprivation, raising the possibility that glial signaling mediates antidepressive-like actions of sleep deprivation. Here, we found that astrocytic signaling to adenosine (A1) receptors was required for the robust reduction of depressive-like behaviors following 12 hours of sleep deprivation. As sleep deprivation activates synaptic A1 receptors, we mimicked the effect of sleep deprivation on depression phenotypes by administration of the A1 agonist CCPA. These results provide the first mechanistic insight into how sleep deprivation impacts mood, and provide a novel pathway for rapid antidepressant development by modulation of glial signaling in the brain.
Similar content being viewed by others
Introduction
Current pharmacological treatments for major depressive disorder take weeks for clinical efficacy, limiting the ability to bring instant relief to suicidal patients. In contrast, a non-pharmacological intervention that rapidly alleviates symptoms of depression is a night of total sleep deprivation,1 which is effective in ∼60% of depressed patients.2, 3
A close relationship exists between major depressive disorder and sleep disorders. Symptoms of major depressive disorder involve altered sleep homeostasis that can be measured by changes in slow-wave activity.4 Pronounced changes in both sleep bout duration and the EEG spectrum have been shown to be hallmark changes in depressed patients. The reduction in depressive symptoms observed following sleep deprivation correlates with overnight dissipation of fronto-central slow-wave activity on baseline sleep, and with the rebound in right frontal all-night slow-wave activity during recovery sleep.4, 5 Selective slow-wave sleep deprivation promotes antidepressant actions in patients although the mechanism is also unknown.4, 5 Strong evidence suggests that the amplitude and slope of slow waves is related to the number, strength, and efficacy of the synaptic connections within the network.6 The idea of regulating synaptic strength in rapid therapies for depression is pertinent, given that another rapidly acting antidepressant, electroconvulsive therapy, may act via increasing synaptic strength in prefrontal cortex (PFC;7, 8). In addition, optogenetic stimulation of the prefrontal cortex, resulting in increased synaptic strength, exerts antidepressant effect in animal models.9
As the effects of sleep deprivation on depression are not long lasting, sleep deprivation is not always used clinically. However, if the mechanism mediating this action were identified, it might be possible to develop therapeutics that target this pathway as a new treatment for certain forms of depression. Although it is difficult to model all aspects of depression in mice, it is well known that stimuli, such as sleep deprivation and electroconvulsive therapy that are clinically effective, lead to robust changes in depressive-like behaviors in mice. We therefore used these tests, the forced-swim- and tail-suspension tests as a readout for the effects of sleep deprivation in order to identify the pathway that is required for sleep deprivation to exert its antidepressive effects. Subsequently, having identified the mechanism, we then validate our data using a third test, the sucrose-consumption test that models of a different aspect of depression, anhedonia.
Materials and methods
Animals and genetic strains
All procedures conducted were in strict accordance with the National Institutes of Health Guide for the Care and Use of Laboratory Animals, and were approved by the Tufts University Institutional Animal Care and Use Committee.
Sleep deprivation
Sleep deprivation of the mice is achieved using the Automated Sleep Deprivation System for Mice (Pinnacle technologies) used in two manners: first we used the EEG/EMG recording to trigger the movement of the bar when mice entered into NREM sleep; and as an alternate approach, we used randomly timed movements of the bar to prevent mice sleeping. Preliminary studies showed both to be effective methods for sleep deprivation.
Forced-Swim Test (FST) and Tail-Suspension Test (TST)
The forced-swim- and tail-suspension tests were performed in a quiet experimental room, as described in previous reports.10, 11, 12 Briefly, the forced-swim test (FST) involved placing a mouse into a clear cylinder (20 cm diameter) filled with water (22–25°C) ∼25-cm deep for a 6-min testing session. Each session was video recorded from above and digitized for analysis of immobility during the last 4 min using Noldus Ethovision software. For the tail-suspension test (TST), each mouse was suspended by its tail to a horizontal wooden bar located inside a white plastic box (40 × 46 × 40 cm), ∼35 cm above the floor. The mouse was secured to the bar by adhesive tape placed 1–1.5 cm from the tip of the tail, such that the mouse’s head was about 20 cm above the floor. The trial was conducted for 6 min (360 s) during which the behavior was video recorded, followed by digitizing and automated scoring using Ethovision. When mice were observed to climb their tails (>10% of total time), they were eliminated from further analyses.
Sucrose consumption
Sucrose consumption was conducted, as reported previously.13 After the acclimatization and habituation period, mice were given access to sucrose for 3 days (days 6–9) to establish baseline sucrose consumption levels. Mice were then given intracerebroventricular (i.c.v.) infusions of CCPA administered as a series of three bolus injections at Zeitgeber time (ZT)=0, 3, and 6, followed by the presentation of sucrose (day 10). The baseline (vehicle infusion) sucrose consumption (day 9) was then compared with the sucrose consumption following CCPA infusion (day 10).
Open-field behavior
The open-field test was performed in accordance with the EMPReSS resource phenotyping protocol.14 Recordings of open-field behavior of mice were imaged from above, digitized, stored, and subsequently assessed using Noldus Ethovision.
Rotorod
The rotorod was a rotating cylinder, 4 cm in diameter, fixed 35 cm above the ground and enclosed by transparent Plexiglas. The rotorod cylinder was covered in textured rubber coating, which facilitates traction. A small electric motor provided power to turn the rotorod via a rubber belt. The rotorod was set to rotate once every 5 s.
Intracerebroventricular cannula implantation
For cannula (Plastics One) implantation, mice are deeply anaesthetized and placed in a stereotaxic apparatus. Following opening, a hole is drilled at coordinates −1.0 mm AP, −1.0 mm ML relative to bregma for insertion of the cannula, and two additional holes were drilled nearby for anchoring screws. Cannulae were lowered into position using a stereotaxic attachment, and secured in place using dental cement. Following curing of the cement, the animal was sutured and allowed to recover for a minimum of 1 week before infusion and/or behavioral testing.
Histology and microscopy
For histology and immunohistochemistry, animals were transcardially perfused with a 4% solution of paraformaldehyde in PBS, followed by cryoprotection in 30% sucrose. Brains were then flash frozen and cut using a sliding microtome to a thickness of 40 μm. To evaluate EGFP signal in dnSNARE mice, sections were mounted on slides and cover slipped with fluoromount G before confocal microscopy on a Nikon Ti confocal microscope. To detect A1R, ABC-DAB immunohistochemistry was used and sections were visualized using a light microscope.
Preparation and extracellular recording of CA1 neurons in acute hippocampal slice
Slices were prepared as previously reported.15, 16 The brain was rapidly extracted in cold cutting solution that contained the following (in mM): 124 NaCl, 26 NaHCO3, 1 NaH2PO4, 10 glucose, 1 sodium pyruvate, 0.6 ascorbate, 2.9 KCl, 1 CaCl2, and 2 MgCl2 and bubbled continuously with a 95% O2 5% CO2 gas mixture. 310-μm-thick slices were cut using a vibratome (VT 1200S; Leica) and were transferred to a bath containing continuously oxygenated cutting solution and incubated at 30 °C for 1.5 h before recording. ZT corresponds to the time of sacrifice.
Electroencephalography
Mice were implanted with EEG and EMG electrodes under ketamine/xylazine anesthesia. After 5–7 days of postoperative recovery, lightweight recording cables were connected to the head implants and mice were placed in cylindrical polypropylene containers containing nest material, water, and food ad libitum. Mice were acclimated to the sleep chamber for 5–7 days (12:12 light–dark cycle; lights on at 0800 hours). EEGs and EMGs were then collected on a Pinnacle Technologies system and digitized at 1000 Hz. Following acclimation, baseline 24-h recordings were made.
Vigilance state scoring, and analyses
NREM sleep, REM sleep, and wake were determined by an experimenter blind to experimental condition. On the baseline day, we computed the amount of each state (expressed as a percentage of total recording time) and the duration of individual sleep and wake episodes. We also measured transitions between NREM sleep and REM sleep during the light phase. To investigate the beneficial effects of sleep deprivation on mice, we sleep deprived mice from 0800 to 1600 hours at the beginning of the major sleep period (light phase) using the Pinnacle sleep deprivation chamber. All EEG data were analyzed by normalizing each data point to the average power of the EEG from 0.5 to 40 Hz (Figure 4), and by normalizing each data point (+12 h, +36 h, +84 h, +108 h) to the corresponding vehicle data points (Supplementary Figure 3).
Statistical analysis
Data were expressed as mean±s.e.m. and the statistical significance of differences in mean values was assessed by t-test (sucrose consumption), or analysis of variance (ANOVA; two way (fluorescence quantification, forced-swim test, tail-suspension test, EEG) or repeated measures (EEG FFT)) with Bonferroni post hoc comparison, as appropriate. Differences among means were considered significant at values of *P⩽0.05, **P⩽0.01, ***P⩽0.001.
Results
We used C57Bl/6J mice that are known to exhibit depressive-like behaviors,10, 11, 17 to screen for therapeutic benefits resulting from sleep deprivation. We subjected mice to different durations of sleep deprivation using the Pinnacle apparatus (Supplementary Figure 1a) before a single period of either the forced-swim test, or the tail-suspension test. EEG monitoring during sleep deprivation demonstrated the effectiveness of the apparatus (Supplementary Figure 1b and c). In agreement with the human literature,18 12 h but not 72 h of sleep deprivation led to antidepressive-like effects revealed by reduced immobility time in both the forced-swim- and tail-suspension tests (Supplementary Figure 1d), without accompanying changes in locomotor activity measured in the open field (Supplementary Figure 2a).
Astrocytes are required for the beneficial effects of sleep deprivation
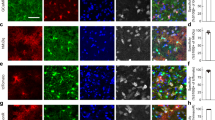
Astrocytes release chemical signals that modulate neurotransmission in a process termed gliotransmission.19 Gliotransmission is impaired in dnSNARE mice via conditional astrocyte-selective expression of the SNARE domain of the vesicle protein VAMP2.16 Astrocytic dnSNARE expression attenuates slow-wave activity of NREM sleep and impairs compensatory increases in sleep time that follow sleep deprivation, actions that are mediated by the ability of the astrocyte to regulate extracellular adenosine.20 Expression of dnSNARE and EGFP can be conditionally controlled by doxycycline (dox; Figure 1a). Confocal imaging and quantification of EGFP signal revealed expression of transgenes in regions of the nervous system thought to be important in contributing to depressive symptoms including the frontal cortex (Figures 1b and c), and hippocampus (Figure 1d).
Mice expressing a dominant negative-SNARE protein in astrocytes do not demonstrate beneficial effects of sleep deprivation on depressive-like behaviors. (a) Schematic diagram of tTA and tetO-driven expression of EGFP and dnSNARE. (b) Confocal images of EGFP expression in the frontal cortex of dnSNARE mice both off (left) and on (right) Dox. Quantification of EGFP intensity in frontal cortex (c) and hippocampal dentate gyrus (d). (e) Heat maps of wild-type and dnSNARE (± sleep deprivation) behavior in the last 4 min of the forced-swim task. (f) Time spent immobile in the last 4 min of the forced-swim task. (g) dnSNARE expression prevents sleep deprivation modulating immobile time in the tail-suspension test. (h) dnSNARE does not impair the ability of chronic (12 day) imiprimine from reducing immobility. ***P⩽0.001.
Adenosine signaling is implicated in the control of human sleep and humans with polymorphisms in the adenosine-metabolizing enzyme, adenosine deaminase, show reduced adenosine metabolism and exhibit more consolidated sleep.21, 22 Magnetic resonance spectroscopy has shown that brain purine levels are low in categories of depressed patients, suggesting that increasing brain adenosine levels may have antidepressive effects.23 In addition, compromised adenosine transport because of polymorphism in the nucleoside transporter gene SLC29A3 have been indentified in female patients predisposed to depression.24 We therefore asked whether the astrocytic control of adenosine signaling is required for the anti-depressive like effects of sleep deprivation.
Expression of astrocytic dnSNARE impaired the ability of 12 h of sleep deprivation to reduce immobility time in both the forced-swim- and tail-suspension tests (Figures 1e and g). In the forced-swim test, sleep deprivation reduced the immobility time from 140.813±6.97 to 28.83±5.70 s (P<0.001) in wild-type mice; whereas in dnSNARE mice, basal immobility (186.99±13.44 s) was not significantly affected by sleep deprivation (161.58±16.31 s; P=0.129; n=8 per group). In the tail-suspension test, basal immobility in dnSNARE mice (200.33±8.30 s) was not significantly reduced by sleep deprivation (206.67±21.31 s; P=0.748; n=10 per group). In contrast, when dnSNARE mice are maintained on dox to suppress expression of the dnSNARE transgene, sleep deprivation significantly decreased immobility time (dnSNARE: 186.99±13.44 s; dnSNARE+dox: 41.66±11.03s; n=8). Neither sleep deprivation in wild-type mice, nor dnSNARE expression affect locomotor activity assessed in the open field (Supplementary Figure 2a; n=8 per group), indicating that the antidepressant-like effects of sleep deprivation are mediated by an astrocyte-dependent dnSNARE-sensitive sleep homeostasis pathway.
To ask whether the astrocytic SNARE-dependent pathway converges on tricyclic antidepressant-sensitive systems, we examined the influence of chronic administration of imipramine (14 days) on immobility time. Both wild-type littermates (saline: 146.73±9.25s; imipramine: 80.67±7.16s; P<0.001) and dnSNARE mice (saline: 189.55±9.87s; imipramine: 97.77±18.10; P<0.001) showed a significant reduction in time spent immobile following chronic treatment (14 days) with imipramine (20 mg/kg; Figure 1h; n=10 per group). As immobility time of wild-type and dnSNARE mice was not differentially affected by imipramine treatment (P=0.316), we suggest that astrocytic signaling has a novel role in contributing to the beneficial effects of sleep deprivation on depressive-like symptoms.
Sleep deprivation elevates astrocyte-derived adenosine
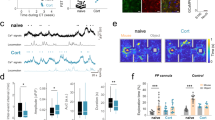
As astrocytic SNARE-dependent signaling activates neuronal A1 receptors,16, 20, 25 we asked whether sleep deprivation leads to an elevation of extracellular adenosine. A relative measure of the extracellular adenosine level can be obtained by determining the proportional enhancement of synaptic transmission in response to the application of the A1R antagonist 8-cyclopentyltheophylline (CPT; 200 nM),15, 20 an approach that has been validated using electrochemical biosensors.26 At zeitgeber time 0 (ZT=0), which corresponds with the time of lights on (onset of sleep cycle), CPT causes a 481.70±85.04 % increase in field excitatory postsynaptic potential fEPSP; whereas at the end of the light phase (ZT=12), the proportional enhancement of fEPSP declined to 128.15±28.91% consistent with a light phase and sleep-dependent reduction in adenosine tone (Figure 2; n=7 per group). This adenosine tone is regulated from an astrocytic source because conditional expression of dnSNARE significantly reduced the adenosine tone (ZT=0: 61.98±16.80%; ZT=12: 27.91±5.10%; P<0.001). Transient total sleep deprivation performed between ZT 0 and ZT 12 prevented the normal diurnal decline in adenosine tone (367.61±24.95%; P=0.028).
Adenosine A1R signaling is elevated by 12 h of sleep deprivation. (a) Representative field excitatory postsynaptic potentials (fEPSP) measured at the Schaeffer collateral synapse before (black) or following (red) the application of 8-cyclopentyltheophylline (CPT, 200 nM). (b) Adenosine tone increases following wakefulness (ZT=0) and declines during sleep (ZT=12) in slices from wildtype but not dnSNARE or A1R knockout (A1R−/−) mice. Transient sleep deprivation (12 h s.d.) maintains the wakefulness-dependent increase in adenosine tone that is impaired by astrocytic dnSNARE. **P⩽0.01, ***P⩽0.001.
Although 12 h of sleep deprivation promoted antidepressive-like behavioral responses, 72 h of sustained sleep deprivation was ineffective (Supplementary Figure 1e). The inability of sustained sleep deprivation to promote antidepressive-like actions was paralleled by an inability to elevate adenosine tone (Figure 2). These data demonstrate a significant correlation between the ability of sleep deprivation to both activate A1R signaling pathways and to promote antidepressive effects: 12 h but not 72 h of sleep deprivation leads to elevated A1R signaling and antidepressive-like actions.
Adenosine A1Rs are required for antidepressive effects of sleep deprivation
A1R−/− mice27 do not express A1R mRNA transcripts, do not show immunoreactivity for A1R (Figure 3a), do not respond to A1R agonists, but are viable and without gross anatomical abnormalities. Sleep deprivation failed to reduce the immobility time of A1R−/− mice (Figures 3b and d). In the forced-swim test, sleep deprivation reduced the immobility time from 141.74±13.75 to 34.15±6.09 s (P<0.001) in wild-type mice, whereas in A1R−/− mice, basal immobility (177.50±18.18s) was not significantly affected by sleep deprivation (155.52±19.21s; P=0.292; n=9 per group). Similarly sleep deprivation did not significantly reduce the immobility time in A1R−/− mice tested using the tail-suspension test (A1R−/−: 204.75±8.36s; A1R−/−+ sleep deprivation: 215.67±16.71s; P=0.476; n=10 per group).
Adenosine A1R are required for the beneficial effects of sleep deprivation on depressive-like behavior. (a) A1R immunohistochemistry in +/+ and A1R−/− brain. (b) Heat maps of representative performance of +/+, A1R−/− and i.c.v. CPT-treated mice during the last 4 min of the forced-swim test. Knockout of A1R, or i.c.v. CPT, prevents the beneficial effects of sleep deprivation on depressive-like behavior in the forced swim (c) and tail-suspension tests (d). ***P⩽0.001.
To determine whether central A1Rs mediate effects of sleep deprivation, we introduced the A1R antagonist CPT (4 mM) via i.c.v. administration. Neither i.c.v. implantation, vehicle infusion (data not shown), nor CPT itself influenced forced-swim task (Figures 3b and d). Mice treated with i.c.v. CPT did not demonstrate the beneficial effects of sleep deprivation on immobility (Figures 3b and d). In the forced-swim test, sleep deprivation reduced the immobility time from 141.74±13.75 to 34.15±6.09 s (P<0.001) in wild-type mice. I.c.v. treatment with CPT did not affect the basal immobility (183.67±13.58 s), but prevented sleep deprivation from reducing immobility in the forced swim (166.50±12.93s; P=0.423; n=9 per group) and tail-suspension tests (CPT, basal immobility 187.60±11.46s, sleep deprivation 204.00±3.58s; P=0.318; n=10 per group).
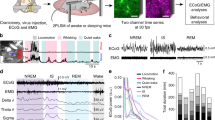
Adenosine agonists cause a sustained enhancement of delta power during wakefulness
As a final step in testing the antidepressive actions of adenosine, we determined whether activation of A1Rs was sufficient to mimic the effects of sleep deprivation on depressive-like behaviors. We delivered an A1R agonist i.c.v. to cause a sustained (6–12 h) activation of the A1R because our sleep deprivation studies showed that 12, but not 6 h of sleep deprivation is required for the antidepressive effects of forced wakefulness. The adenosine receptor agonist 2-chloro-N(6)-cyclopentyladenosine (CCPA; 500 nM) was delivered i.c.v while performing EEG/EMG recordings. A single i.c.v. infusion of CCPA caused a transient decrease in the percentage of time that the animals were awake. Three consecutive CCPA infusions (ZT=0, 3, and 6) caused mice to sleep for a significantly greater time from ZT 1 through 10 compared with vehicle (Figure 4a; P<0.002; n=6 per group). By ZT 12, when we normally assess depressive-like behaviors, animals exhibited normal homecage and open-field behaviors (Supplementary Figure 2a) and spent a significantly greater percentage of time awake than during vehicle administration or at 36 h following administration (Supplementary Figure 2b).
The adenosine receptor agonist 2-chloro-N(6)-cyclopentyladenosine(CCPA) alters network patterns of electrical activity and sleep architecture. (a) The percent time awake is decreased during CCPA administration (arrows). (b) Normalized power spectrum at ZT=12 during wakefulness at hours 12, 36, 84, and 108 after initial drug administration. Data are normalized to the total power of the EEG between 0.5 and 40 Hz. (c) Normalized power spectrum from 0.5 to 4.0 Hz for wake states at 12, 36, 84, and 108 h after initial drug administration. (d) Normalized power during wake of the delta (.5–4 Hz), theta (5–8 Hz) alpha (9–13 Hz), and gamma (20–40 Hz). *P⩽0.05, **P⩽0.01, ***P⩽0.001.
Once mice awoke from the somnogenic effects of CCPA, we noted that there was a prominent increase in delta power (0.5–4 Hz.; P<0.001) during wakefulness that was sustained for 36 h (P<0.001) following the onset of CCPA administration (Figures 4b–d). This increase in delta power is probably because of a long-lasting change in brain function, rather than due to the lingering presence of CCPA because (i) the acute effect of CCPA was to reduce delta power, (ii) effects of CCPA on sleep had reversed by ZT=11, which is 5 h following the last administration of CCPA (at ZT=6).
Activation of A1R leads to sustained antidepressive-like behaviors
CCPA administration (ZT=0, 3, and 6) caused a reduction in immobility time when mice were tested at ZT=12 in the forced-swim test (Figures 5a and b; n=8 per group) without accompanying changes in locomotor activity assessed in both the open field and the rotorod (Supplementary Figure 2a, c; n=8 per group). Because of the complicated nature of using animal models of depression, we sought an independent test to validate this result and used sucrose consumption that models anhedonia, a component of depression symptoms that is often incorporated in the evaluation for clinical diagnosis.28 I.c.v. administration of CCPA (51.45±6.35 g/kg) significantly increased sucrose consumption compared with the levels measured during the vehicle baseline (30.55±3.60 g/kg; P=0.008; Figure 5c; n=10 per group). Thus, in addition to the symptoms of despair or hopelessness modeled by the forced-swim test, CCPA also has beneficial effects on the lack of interest in pleasure modeled by the sucrose consumption test.
Activation of A1R with CCPA leads to sustained antidepressive-like behaviors. (a) Representative heatmaps showing dwell time during the last 4 min of the forced-swim test following CCPA treatment and sleep deprivation (12 h). (b) CCPA significantly reduces immobility in the forced-swim test, an effect that is sustained for 36 h following the onset of CCPA administration. (c) Validation of forced-swim test results using an additional test of depressive-like symptoms, the sucrose consumption test. *P⩽0.05, **P⩽0.01.
To test the longevity of the beneficial effects of CCPA administration, we used separate cohorts of mice and tested them at 12 h (ZT=12), 36 h, 84 h, and 108 h after first CCPA treatment. The beneficial effects of only one subjective night of CCPA treatment on immobility measured in the forced-swim test last for up to 36 h (Figure 5b). Thus CCPA can have rapid and moderately long-lasting effects on depressive-like symptoms modeled in mice, which correspond with the duration of change in EEG delta power observed following CCPA administration (Figures 4b–d, Supplementary Figure 3).
Discussion
We have investigated the mechanisms underlying the robust improvement observed in human depression patients following sleep deprivation. Using pharmacology and molecular genetics, we have modulated astrocyte-to-neuron signaling pathways, and show that the beneficial effects of sleep deprivation on depressive-like behaviors require an astrocyte-dependent signaling pathway. We have used multiple methods to both screen and model behavior while being aware of the inherent limitations of using animal models to study psychiatric disorders. By using these models and knowing that sleep deprivation is highly effective for treating human depression, we demonstrate the critical importance of A1R signaling for these beneficial effects: A1R receptors are required as A1R−/− mice, as well as mice in which the A1R antagonist CPT was delivered centrally, both fail to respond to sleep deprivation with reduced immobility in the forced-swim- and tail-suspension tests. In addition, support for A1R signaling mediating antidepressive effects are provided by the observation that sustained sleep deprivation (72 h) leads to both an inactivation of the A1R pathway and to a loss of the antidepressive effects of sleep deprivation. As exogenous, central activation of A1R using CCPA led to antidepressive effects, our results lead us to suggest that glial-derived adenosine acting through A1R mediates the antidepressive effects of sleep deprivation.
One potential confound is the role that the endogenous A1R plays in the brain along with the possibility that animals lacking this receptor would be prone to seizure activity. Stenberg et al.29 have shown that both baseline and sleep deprived A1R−/− mice show no significant differences in their EEG from wild-type animals.29 Further, after the i.c.v. injection of the A1 antagonist CPT animals were monitored extensively for seizure and aberrant electrophysiological activity. As previously reported, CPT did not cause any large changes in the spectrum of the EEG and no seizures were observed.
Animal models of specific symptoms of human depression have proven to be essential tools in revealing the mechanisms of psychiatric diseases. In relation to depression, two tests that are well characterized, robust, and respond to many antidepressive drugs are the forced-swim test and the tail-suspension test. The strain of mice used in this study, C57Bl6, has been consistently shown to have high levels of depressive-like behavior compared with other inbred strains.10, 11, 17 Before interpreting changes in immobility in these two behavioral despair tasks as being relevant to depression, we provided further validation by showing that 14 days of treatment with a tricyclic antidepressant, imipramine, reduces immobility (Figure 1h), as described previously,30, 31 and that sleep deprivation, a powerful and rapid acting antidepressant treatment in the clinical population, reduces immobility in these tasks. Final validation was provided by an additional behavioral test of anhedonia that was performed using the sucrose consumption test. It is important when studying animal models to not use a single task to measure effects, and consequently, we have used multiple tasks to increase our research validity. Taken together, this validation provides strong support to our thesis that activation of the glial-dependent adenosine pathway contributes to antidepressive effects of sleep deprivation.
Whether antidepressive effects of A1R activation converge on pathways recruited by other treatments is unknown. However, there are common observations concerning the modulation of delta power of the EEG. EEG measurements revealed a significant increase in delta power during wakefulness that decayed in a temporally coincident manner with the antidepressive effects of this ligand: CCPA caused a significant increase in delta power for up to 36 h, following onset of administration of this A1R ligand (Figures 4b–d) and antidepressive effects for the same time period (Figure 5b). Other fast-acting antidepressant treatments are also known to increase delta power including ketamine,32, 33 deep brain stimulation,34, 35 transcranial magnetic stimulation,36, 37 and electroconvulsive therapy38, 39 raising the possibility of convergent mechanisms of action.3
Traditional therapeutics for depression are limited by the delayed onset of beneficial effects. In contrast, the adenosine signaling pathway activated by sleep deprivation is rapidly beneficial and represents a novel strategy to bring relief to suicidal patients where a delay in therapeutic benefits could be devastating. Although adenosinergic pharmacology can alleviate depressive-like behaviors in mice, it could not become a therapeutic strategy for humans because of the well-known systemic side effects resulting from the activation of A1Rs. That being said, the results of this study provide a highly novel and innovative future strategy of targeting glial specific receptors to influence adenosine signaling. One can envision the potential of developing therapeutic agents that act on these receptors to control adenosine and as a consequence depressive-like behaviors without the normal peripheral side effects of adenosine pharmacology.
References
Germain A, Buysse DJ, Nofzinger E . Sleep-specific mechanisms underlying posttraumatic stress disorder: integrative review and neurobiological hypotheses. Sleep Med Rev 2008; 12: 185–195.
Hemmeter U, Bischof R, Hatzinger M, Seifritz E, Holsboer-Trachsler E . Microsleep during partial sleep deprivation in depression. Biol Psychiatry 1998; 43: 829–839.
Hemmeter UM, Hemmeter-Spernal J, Krieg JC . Sleep deprivation in depression. Expert Rev Neurother 2010; 10: 1101–1115.
Goldstein MR, Plante DT, Hulse BK, Sarasso S, Landsness EC, Tononi G et al. Overnight changes in waking auditory evoked potential amplitude reflect altered sleep homeostasis in major depression. Acta Psychiatr Scand 2011; 125: 468–477.
Landsness EC, Ferrarelli F, Sarasso S, Goldstein MR, Riedner BA, Cirelli C et al. Electrophysiological traces of visuomotor learning and their renormalization after sleep. Clin Neurophysiol 2011; 122: 2418–2425.
Hanlon EC, Vyazovskiy VV, Faraguna U, Tononi G, Cirelli C . Synaptic potentiation and sleep need: clues from molecular and electrophysiological studies. Curr Top Med Chem 2011; 11: 2472–2482.
Duman RS, Vaidya VA . Molecular and cellular actions of chronic electroconvulsive seizures. J ECT 1998; 14: 181–193.
Lavergne F, Jay TM . A new strategy for antidepressant prescription. Front neurosci 2010; 4: 192.
Covington HE, Lobo MK, Maze I, Vialou V, Hyman JM, Zaman S et al. Antidepressant effect of optogenetic stimulation of the medial prefrontal cortex. J Neurosci 2010; 30: 16082–16090.
Bai F, Li X, Clay M, Lindstrom T, Skolnick P . Intra- and interstrain differences in models of "behavioral despair". Pharmacol Biochem Behav, [Comparative Study] 2001; 70: 187–192.
Cryan JF, Mombereau C . In search of a depressed mouse: utility of models for studying depression-related behavior in genetically modified mice. Mol Psychiatry 2004; 9: 326–357.
Porsolt RD, Le Pichon M, Jalfre M . Depression: a new animal model sensitive to antidepressant treatments. Nature 1977; 266: 730–732.
Papp M, Willner P, Muscat R . An animal model of anhedonia: attenuation of sucrose consumption and place preference conditioning by chronic unpredictable mild stress. Psychopharmacology (Berl) 1991; 104: 255–259.
Brown SD, Chambon P, de Angelis MH . EMPReSS: standardized phenotype screens for functional annotation of the mouse genome. Nat Genet 2005; 37: 1155.
Manzoni OJ, Manabe T, Nicoll RA . Release of adenosine by activation of NMDA receptors in the hippocampus. Science 1994; 265: 2098–2101.
Pascual O, Casper KB, Kubera C, Zhang J, Revilla-Sanchez R, Sul JY et al. Astrocytic purinergic signaling coordinates synaptic networks. Science 2005; 310: 113–116.
Miller BH, Schultz LE, Gulati A, Su AI, Pletcher MT . Phenotypic characterization of a genetically diverse panel of mice for behavioral despair and anxiety. PLoS one 2010; 5: e14458.
Wu JC, Bunney WE . The biological basis of an antidepressant response to sleep deprivation and relapse: review and hypothesis. Am J psychiatry 1990; 147: 14–21.
Haydon PG . GLIA: listening and talking to the synapse. Nat Rev Neurosci 2001; 2: 185–193.
Halassa MM, Florian C, Fellin T, Munoz JR, Lee SY, Abel T et al. Astrocytic modulation of sleep homeostasis and cognitive consequences of sleep loss. Neuron 2009; 61: 213–219.
Bachmann V, Klaus F, Bodenmann S, Schafer N, Brugger P, Huber S et al. Functional ADA polymorphism increases sleep depth and reduces vigilant attention in humans. Cereb Cortex 2012; 22: 962–970.
Mazzotti DR, Guindalini C, Pellegrino R, Barrueco KF, Santos-Silva R, Bittencourt LR et al. Effects of the adenosine deaminase polymorphism and caffeine intake on sleep parameters in a large population sample. Sleep 2011; 34: 399–402.
Renshaw PF, Parow AM, Hirashima F, Ke Y, Moore CM, Frederick Bde B et al. Multinuclear magnetic resonance spectroscopy studies of brain purines in major depression. Am J Psychiatry 2001; 158: 2048–2055.
Gass N, Ollila HM, Utge S, Partonen T, Kronholm E, Pirkola S et al. Contribution of adenosine related genes to the risk of depression with disturbed sleep. J Affect Disord 2010; 126: 134–139.
Fellin T, Halassa MM, Terunuma M, Succol F, Takano H, Frank M et al. Endogenous nonneuronal modulators of synaptic transmission control cortical slow oscillations in vivo. Proc Natl Acad Sci USA 2009; 106: 15037–15042.
Schmitt LI, Sims RE, Dale N, Haydon PG . Wakefulness affects synaptic and network activity by increasing extracellular astrocyte-derived adenosine. J Neurosci 2012; 32: 4417–4425.
Sun D, Samuelson LC, Yang T, Huang Y, Paliege A, Saunders T et al. Mediation of tubuloglomerular feedback by adenosine: evidence from mice lacking adenosine 1 receptors. Proc Natl Acad Sci USA 2001; 98: 9983–9988.
El Yacoubi M, Bouali S, Popa D, Naudon L, Leroux-Nicollet I, Hamon M et al. Behavioral, neurochemical, and electrophysiological characterization of a genetic mouse model of depression. Proc Natl Acad Sci USA 2003; 100: 6227–6232.
Stenberg D, Litonius E, Halldner L, Johansson B, Fredholm BB, Porkka-Heiskanen T . Sleep and its homeostatic regulation in mice lacking the adenosine A1 receptor. J Sleep Res 2003; 12: 283–290.
Fukui M, Rodriguiz RM, Zhou J, Jiang SX, Phillips LE, Caron MG et al. Vmat2 heterozygous mutant mice display a depressive-like phenotype. J Neurosci 2007; 27: 10520–10529.
Sanchez C, Meier E . Behavioral profiles of SSRIs in animal models of depression, anxiety and aggression. Are they all alike? Psychopharmacology (Berl) 1997; 129: 197–205.
Freye E, Partecke LB, Levy JV . Increase in delta- and beta-wave activity of the EEG during rapid opiate detoxification (ROD)-reversal by administration of the non-specific NMDA-antagonist S+ ketamine. Neurophysiol Clin 2005; 35: 25–32.
Murrough JW, Perez AM, Mathew SJ, Charney DS . A case of sustained remission following an acute course of ketamine in treatment-resistant depression. J Clin Psychiatry 2011; 72: 414–415.
Kennedy SH, Giacobbe P, Rizvi SJ, Placenza FM, Nishikawa Y, Mayberg HS et al. Deep brain stimulation for treatment-resistant depression: follow-up after 3 to 6 years. Am J Psychiatry 2011; 168: 502–510.
Mayberg HS, Lozano AM, Voon V, McNeely HE, Seminowicz D, Hamani C et al. Deep brain stimulation for treatment-resistant depression. Neuron 2005; 45: 651–660.
Griskova I, Ruksenas O, Dapsys K, Herpertz S, Hoppner J . The effects of 10 Hz repetitive transcranial magnetic stimulation on resting EEG power spectrum in healthy subjects. Neurosci Lett 2007; 419: 162–167.
Spronk D, Arns M, Bootsma A, van Ruth R, Fitzgerald PB . Long-term effects of left frontal rTMS on EEG and ERPs in patients with depression. Clini EEG Neurosci 2008; 39: 118–124.
Fink M, Kahn RL . Relation of electroencephalographic delta activity to behavioral response in electroshock; quantitative serial studies. AMA Arch Neurol Psychiatry 1957; 78: 516–525.
Sackeim HA, Luber B, Katzman GP, Moeller JR, Prudic J, Devanand DP et al. The effects of electroconvulsive therapy on quantitative electroencephalograms. Relationship to clinical outcome. Arch Gen Psychiatry 1996; 53: 814–824.
Acknowledgements
We thank Dr Michael Halassa, for his careful reading of this paper and his comments. Grant support for these studies was provided by the NIMH to PGH.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Dr Haydon is co-founder and President of GliaCure Inc., which has licensed a pending patent application concerning the signaling cascades described in this paper.
Additional information
Supplementary Information accompanies the paper on the Translational Psychiatry website
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-Share Alike 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-sa/3.0/
About this article
Cite this article
Hines, D., Schmitt, L., Hines, R. et al. Antidepressant effects of sleep deprivation require astrocyte-dependent adenosine mediated signaling. Transl Psychiatry 3, e212 (2013). https://doi.org/10.1038/tp.2012.136
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/tp.2012.136
Keywords
This article is cited by
-
Sleep-mediated regulation of reward circuits: implications in substance use disorders
Neuropsychopharmacology (2023)
-
The antidepressant-like effect of guanosine involves the modulation of adenosine A1 and A2A receptors
Purinergic Signalling (2023)
-
Astrocytes: new evidence, new models, new roles
Biophysical Reviews (2023)
-
Rapid-acting antidepressants and the circadian clock
Neuropsychopharmacology (2022)
-
A Pattern to Link Adenosine Signaling, Circadian System, and Potential Final Common Pathway in the Pathogenesis of Major Depressive Disorder
Molecular Neurobiology (2022)