Abstract
The pathophysiology of negative affect states in older adults is complex, and a host of central nervous system and peripheral systemic mechanisms may play primary or contributing roles. We conducted an unbiased analysis of 146 plasma analytes in a multiplex biochemical biomarker study in relation to number of depressive symptoms endorsed by 566 participants in the Alzheimer's Disease Neuroimaging Initiative (ADNI) at their baseline and 1-year assessments. Analytes that were most highly associated with depressive symptoms included hepatocyte growth factor, insulin polypeptides, pregnancy-associated plasma protein-A and vascular endothelial growth factor. Separate regression models assessed contributions of past history of psychiatric illness, antidepressant or other psychotropic medicine, apolipoprotein E genotype, body mass index, serum glucose and cerebrospinal fluid (CSF) τ and amyloid levels, and none of these values significantly attenuated the main effects of the candidate analyte levels for depressive symptoms score. Ensemble machine learning with Random Forests found good accuracy (∼80%) in classifying groups with and without depressive symptoms. These data begin to identify biochemical biomarkers of depressive symptoms in older adults that may be useful in investigations of pathophysiological mechanisms of depression in aging and neurodegenerative dementias and as targets of novel treatment approaches.
Similar content being viewed by others
Introduction
The prevalence and incidence of clinically significant depressive symptoms increase with advancing age, especially among those with physical illness, cognitive decline and functional disability.1, 2, 3 In community-dwelling seniors, the prevalence of major depression is ∼10%, whereas the rate for ‘minor’, ‘subsyndromal’ or ‘subthreshold’ depression is ∼30%, but may be as high as 48% among those >75 years. Subsyndromal depression is not benign as it carries clinically significant disability, poorer quality of life and higher health-care costs.1, 4
The pathophysiology of late-life depression is complex, and a host of central nervous system and peripheral systemic mechanisms may play primary or contributing roles. Age-associated neurological illnesses such as Alzheimer's disease (AD), stroke and Parkinson's disease are well-known risk factors and may be associated with depression due to disruption of neural circuitries that mediate the experience and expression of negative emotions and behaviors by their defined neuropathological lesions and neurochemical changes.5, 6, 7 Cardiovascular disease, inflammatory conditions, cancer, metabolic and endocrine dysfunction also increase with age and are highly associated with depression. They are commonly thought to exert their effect via circulating factors such as inflammatory markers produced in the course of these chronic disease processes, although evidence to support this is still controversial.8, 9, 10, 11 Numerous hypothesis-based studies of depression in adulthood and late life have identified associations with glucocorticoids and other stress hormones,12 insulin resistance,13 inflammatory cytokines and chemokines14 and trophic factors15, 16, 17 that may be activated with normal and abnormal aging processes and/or in response to illness, injury and other stressors, although the data in older adults for all of these are relatively scarce. Whether alterations in these various age- and depression-associated factors are causative of depression or consequences thereof and how they interact are not established.
The identification and validation of biomarkers in psychiatry has been challenging but the task remains important to both better understand the pathophysiology of depression and better classify and treat this multifactorial syndrome in an era of personalized medicine. Here, we used data from a large multianalyte biochemical panel in plasma samples from older adult participants in the Alzheimer's Disease Neuroimaging Initiative (ADNI) in a discovery analysis to identify peripheral biochemical biomarkers that associate with depressive symptoms. Our findings provide further support for a role of several previously identified proteins in negative affect states and identify novel candidates for validation and investigation in future studies and other cohorts.
Subjects and methods
Description of the ADNI
The ADNI is a large, multicenter, longitudinal neuroimaging and biomarker study, launched in 2004,18, 19, 20 with a primary goal to characterize cognitive functioning and AD in older adults with longitudinal clinical assessments, multiple modality neuroimaging and blood, urine and cerebrospinal fluid (CSF) molecular and biochemical biomarkers. Participants received baseline and periodic physical and neurological examinations, standardized neuropsychological assessments, apolipoprotein E (APOE) genotyping and they provided biofluid samples throughout the study.21, 22 Imaging (magnetic resonance imaging and for a subset, 18F-fluorodeoxyglucose positron emission tomography and 11C-Pittsburgh compound B positron emission tomography) is performed at baseline and at regular intervals thereafter.20 The procedures for this study were approved by institutional review boards of all participating institutions. All subjects gave written, informed consent for all procedures before participation.
Participants
The total ADNI cohort includes 819 older adults, 55 to 90 years old, who met entry criteria for a clinical diagnosis of normal cognition, amnestic mild cognitive impairment (MCI) or probable AD.19 Participants with AD met National Institute of Neurological and Communication Disorders/Alzheimer's Disease and Related Disorders Association criteria for probable AD and had a Mini-Mental State Examination score between 20 and 26 and a global Clinical Dementia Rating (CDR) of 0.5 or 1.0 and, therefore, were only mildly impaired at baseline. Inclusion criteria for participants with MCI included memory complaint and abnormal memory score on the Wechsler Memory Scale, Mini-Mental Sate Examination score between 24 and 30 and a CDR of 0.5 with a Memory Box score of at least 0.5.
People with significant current psychiatric illness were ineligible to participate in ADNI and thus only participants with no more than mild depression, anxiety or other symptoms were enrolled. Specific exclusion criteria for all participants included major mood disorder within a year of screening, a score of ⩾6 on the Geriatric Depression Scale (GDS),23, 24 history of schizophrenia, alcohol or substance abuse within the past 2 years, and for AD and MCI participants, any psychosis, agitation or behavior problems. For a review and more details on inclusion and exclusion criteria, see Mueller et al.25 and http://www.adni-info.org/.
The multi-analyte biochemical panel assays used here were conducted in a subsample of 566 ADNI participants, including 396 with MCI, 112 with AD and 58 with normal cognition. Subsampling was necessary because of budgetary constraints. Samples were selected to enrich for MCI cases and cases with additional biomarker end points (for example, CSF amyloid-β and -τ and amyloid neuroimaging) to be used in separate analyses. Table 1 presents demographic and clinical characteristics of the sample used here.
Assessments of depression and cognition
The primary outcome measure of depressive symptoms was the short version of the GDS.26 This 15-item self report form has demonstrated robust validity for depression in older adults,24, 26 including those with MCI,27 although its reliability may diminish in people with dementia.28 One item in the GDS asks if the subject feels he/she has more memory problems than most. Given the frequency of memory complaints in ADNI, this item was excluded from the total score that was used in analyses here.
The ADNI protocol includes a comprehensive assessment of cognitive functioning with particular emphasis on domains relevant to AD. A full description is available at http://www.adni-info.org/Scientists/CognitiveTesting.aspx. Clinical data from the baseline and 12-month assessments were used. To control for potentially confounding effects of cognitive syndrome on outcome measures of depression in participants with AD, MCI and normal cognition, the CDR Sum-of-Boxes score was included as a covariate in statistical analyses.29 The CDR is a structured interview assessing functional status in the domains of memory, orientation, judgment and problem solving, home and hobbies and personal care.
Plasma sampling and biochemical multi-analyte panel
Morning fasting plasma samples were obtained at baseline and 12-month assessments. Whole-blood samples were obtained in EDTA tubes, placed immediately on ice, spun down for plasma aliquoting and frozen at −80 °C, per ADNI lab standard operating protocols as reviewed recently.30
Plasma samples from the ADNI biospecimen repository at the University of Pennsylvania were sent to Rules-Based Medicine (RBM, Austin, TX, USA) for measurement of 190 protein analytes with a multiplex immunoassay panel. This panel was developed on the Luminex xMAP (Austin, TX, USA) platform to measure proteins previously reported to be altered in cancer, cardiovascular disease, metabolic disorders and inflammation. RBM also included additional analytes believed to be involved in cell signaling and previously reported to change in patients with AD.31 RBM has attempted to validate each of the 190 analytes up to CLIA (Clinical Laboratory Improvement Amendment) standards, but the assays themselves are not CLIA approved. Each analyte has an individual standard curve with between 6 and 8 reference standards. Each plate is run with three levels of quality control (QC) measures (low, medium and high dilutions). Each analyte has a validation report, including a dynamic range in young adults. Additional QC measures for almost all analytes were employed specifically for the ADNI plasma analysis by testing blank human plasmas spiked with extracts of cell cultures expressing the individual analytes. Samples from the total ADNI plasma cohort were run on 15 plates.
APOE genotyping
DNA was extracted from blood using commercial reagents (FlexiGene, Qiagen, Valencia, CA, USA). Two single-nucleotide polymorphisms (rs7412 and rs429358) in APOE were typed using allelic discrimination assays with TaqMan reagents (Applied Biosystems, Foster City, CA, USA) on an ABI 7500. The APOE genotypes (ɛ2, ɛ3 and ɛ4) were assigned by incorporating the genotyping results into an algorithm.
Statistical analyses and machine learning analyses
Analyses were conducted in the ‘ADNI Plasma QC Multiplex’ data set available for download at https://ida.loni.ucla.edu/login.jsp?project=ADNI. This data set contains the cleaned, quality-controlled data as described in the ADNI statistical analysis plan. Missing, ‘LOW’ or outlier values were imputed respectively as the mean of the nonmissing values, half the least detectable dose, or by a nearest neighbor or similar algorithm. Analytes for which missing/’LOW’ values were >25% of all samples were excluded, resulting in valid data for 146 of the total 190 analytes on the original panel.
Linear regression models evaluated the association of levels of each protein to GDS scores at baseline and month 12. Mixed-effect models examined if each protein is associated with change of depression symptoms by examining the interaction between follow-up time and each protein.32 This statistical procedure accounts for the correlations that are due to repeated measurements of depression symptoms in the same patient. All models adjusted for age, sex, education and CDR Sum-of-Boxes score as covariates. Analyses were conducted in SPSS Statistics 19 (IBM, Somers, NY, USA), SAS version 9.2 (SAS Institute, Cary, NC, USA) and JMP 8.0.1 (SAS). Secondary analyses incorporated terms for past depression or other psychiatric illness, antidepressant use and APOE genotype. All statistical tests were two sided. We did not conduct multiple testing adjustments except lowering the significance level to 0.01 and the ‘trend’ level to 0.05 because the current analyses are discovery in nature. Consequently, there is a chance of false discovery because of the number of statistical tests performed.
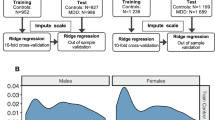
Finally, to assess the utility of such multiplex immunoassays as biomarker classifiers of depressive symptoms, we applied a machine learning ensemble classification method, Random Forests (using R package RandomForest, version 4.6-2; http://www.stat.berkeley.edu/~breiman/RandomForests/cc_home.htm). The samples were dichotomized into those with depressive symptoms (GDS ⩾2) versus those without depressive symptoms (GDS=0), with GDS=1 serving as a buffer. Analytes were first sorted by z-score (derived from variable importance score) obtained from Random Forests. The higher the score, the more significant the analyte is for discriminating between samples with and without depressive symptoms. The first selected analyte has the highest importance. This is then combined with all remaining analytes to find the second analyte, which in combination with the first one gives the best Out-of-Bag error estimation (used for deriving accuracy). Finally, to gauge the robustness of analytes’ association with depressive symptoms, we applied a fivefold cross-validation procedure to the analytes selected by Random Forests. In each of the five validations, 80% of the subjects were chosen for training and the remaining 20% were used for testing; the partition was done randomly while preserving the ratio of samples from the two categories. The procedure was repeated three times.
Results
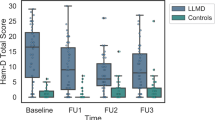
Of the 566 ADNI participants for whom at least baseline plasmas were analyzed, 165 (29.2%) had depressive symptoms (GDS 2–5) at baseline. In the subsequent year, there were some generally modest changes in GDS scores with a small increase in the proportion of participants with depressive symptoms (32.1% with GDS ⩾2 at month 12). This included 21 participants (4.1%) whose GDS scores increased into a more significant category of syndromal depression (⩾6, range 6–12).
There were no significant differences in age, gender or education among the normal, MCI and mild AD diagnostic groups at baseline. As expected, these groups differed in frequency of APOE genotype and in measures of cognition. Interestingly, although the diagnostic groups did not differ in GDS scores at baseline, there were highly significant differences in the frequency of past psychiatric illness, with MCI and AD participants respectively having ∼1.5-fold and 2.5-fold higher frequencies than those categorized as normal.
Linear regression models determined the statistical strengths of associations of analytes with depressive symptoms at baseline and at month 12. The top analytes are presented in Table 2 and statistics for the associations of all 146 plasma analytes with the main outcomes of interest are presented in the Supplementary Table S1. Associations were particularly strong for hepatocyte growth factor (HGF), several forms of insulin, pregnancy-associated plasma protein A (PAPPA), and vascular endothelial growth factor (VEGF).
To examine potentially confounding effects of other variables in the associations of the top analytes, we used separate linear regression models with additional terms for past history of psychiatric illness, antidepressant use, use of any psychotropic medicine, modified Hachinski Ischemic Score,33 APOE genotype, body mass index and serum glucose (baseline only). The associations were essentially the same (data not shown).
We also tested whether depressive symptoms were related to molecular signatures of AD pathology and whether these moderated the significant associations of depressive symptoms with biochemical analytes from the multi-analyte panel. We found no associations between baseline GDS scores and CSF total τ (F=2.06, d.f.=5, 351, P=0.15), p-τ181 (F=2.03, d.f.=5, 351, P=0.15), or Aβ (F=0.89, d.f.=5, 351, P=0.35), and no modifying effects.
Random Forest analyses were performed as a complementary analytic approach to assess the ability of sets of analytes to classify participants into those with (GDS ⩾2) or without (GDS=0) depressive symptoms. The set of analytes was first selected based on z-scores obtained from Random Forests. The final sets of analytes were then selected with the aim of obtaining the best classification accuracy. Two sets of experiments were performed on each of the baseline and month-12 data. At baseline, 140 people with depressive symptoms were compared with 225 with none. At month 12, 158 people had depressive symptoms whereas 210 had none. At baseline, the best set of analytes achieved an overall 75.4% accuracy in classifying presence or absence of depressive symptoms with a sensitivity of 62.8% and a specificity of 83.8%. At month 12, accuracy was 80.9% with a sensitivity of 59.5% and a specificity of 94.2%. The analytes selected by Random Forests at each assessment are presented in Table 3.
Finally, as a third approach to identify candidate biomarkers that may be pathophysiologically relevant to depressive symptoms, we used mixed-effects models to discern baseline plasma analytes that were associated with change in depressive symptoms from baseline through month 24. Adjusted for age, gender, education and CDR Sum of Boxes, the rate of change of depression symptoms was associated with three baseline analytes at the P<0.01 level, including angiopoietin 2, FAS ligand receptor and fatty acid-binding protein, and nine at the P<0.05 level, including HGF (see Supplementary Table S1 for statistical results for all analytes).
Discussion
Our data identified candidate plasma biomarkers of depressive symptoms in older adults, which may prove useful in investigations into the pathophysiology of negative affect across the lifespan. Previous biomarker studies of depression have focused on contemporaneous conceptualizations of depression pathophysiology.12, 13, 14, 15, 16, 17, 34, 35, 36 Here, we used an unbiased multiplex discovery interrogation of 146 known plasma analytes in a large cohort of well-characterized subjects. In particular, HGF, insulins, PAPPA and VEGF were identified as among the more robust and interesting candidates.
HGF (also known as scatter factor and hematopoietin A) is a 103 kDa heterodimeric protein first identified as a regeneration factor for hepatocytes after liver injury.37 It is a multifunctional trophic factor that signals through a tyrosine kinase signaling cascade after binding to MET, its proto-oncogenic receptor. HGF is produced by neurons and nonneuronal cells, whereas MET is especially highly expressed in neurons. During embryogenesis, HGF is a neural inducer, an interneuron motogen, an axonal chemoattractant, an angiogenic factor and a neuroprotective survival factor.38, 39 Its expression continues in adulthood and it is induced by ischemic injury40 and other disease processes, including AD.41 HGF enhances long-term potentiation,42 improves or attenuates ischemia-related memory deficits43 and Aβ-induced behavioral impairment,44 and has anxiolytic properties,45 whereas its suppression increases anxiety and depressive behaviors in rodents.46 To our knowledge, only two studies have investigated HGF in relation to depression in humans, one of which found significantly lower serum HGF levels among 26 people with major depression compared with 19 controls,47 whereas the other study found no difference in HGF levels in 12 women with major depression and borderline personality disorder.48 Higher serum levels of HGF have also been found in those patients with panic disorder who best responded to antidepressant medication.49 To this literature, we add our finding of an increase in plasma HGF levels with increasing depressive symptoms in older adults. Given the generally salutary effects of HGF, we speculate that such an increase may represent a compensatory mechanism in the setting of other depression-inducing pathophysiological mechanisms.
Depressive symptoms were positively associated with levels of insulin polypeptides, in support of a growing literature linking insulin resistance to depression.13, 50, 51, 52, 53 The nature of this association is complex as some evidence indicates a bidirectional relationship; that is, depression increases the risk for subsequent development of type 2 diabetes mellitus,54 whereas the presence of type 2 diabetes mellitus increases risk for incident depression.52 One mechanism that has been proposed to account for insulin resistance in depression is dysregulation of the hypothalamic–pituitary–adrenal axis with abnormal circulating levels of glucocorticoids.12, 55 Others have invoked the effects on insulin signaling by inflammatory cytokines14 and some trophic factors15, 16, 17 that may also be activated in depression. Conversely, insulin activates diverse, multifunctional signaling cascades (for example, Akt and glycogen synthase kinase 3) that are believed to play important roles in mood.56, 57
As further support for an insulin link to depression, we observed an association of PAPPA with depressive symptoms. PAPPA is a secreted metalloproteinase that cleaves insulin-like growth factor-binding proteins, increasing their bioavailability.58 To our knowledge, its expression or activity in the brain have not been studied.
VEGF was also found to be elevated in relation to depressive symptoms in the ADNI cohort. Previous studies have reported VEGF gene polymorphisms associated with major depression,59, 60 increased leukocyte VEGF mRNA expression in refractory depression61 and increased serum or plasma VEGF levels in depression in two studies48, 62 but not a third one.63 VEGF (specifically VEGF-A measured here) is a 232-amino-acid protein with multiple isoforms that bind to three high-affinity receptor tyrosine kinases. It is widely expressed and is best known for its growth factor activity in angiogenesis, vasculogenesis and endothelial cell growth.64 Analogous to insulin, after binding to its receptors, VEGF activates numerous downstream signaling proteins including protein kinase C, phospholipase C-γ, phosphatidylinositol 3-kinase, Akt and mammalian target of rapamycin. VEGF increases the permeability of the blood–brain barrier,65 facilitates neurogenesis and proliferation of neurons in the adult hippocampus,66 plays a role in synaptic neurotransmission67 and synaptic plasticity in hippocampus-dependent learning and memory68 and has anxiolytic and antidepressant activity in rodent models.66
Our data should be interpreted in light of the strengths of the ADNI study design as well as its weaknesses. Foremost, the ADNI study incorporates an extraordinary array of biomarker approaches that characterize many aspects of the functional, anatomic, physiological, biochemical and molecular health of the aging brain. It is longitudinal, thus allowing both cross-sectional and dynamic monitoring of phenomenology and biology that may better elucidate disease processes. Future analyses will investigate the relationships of biochemical biomarkers of depressive symptoms identified here in relation to other neuroimaging and longitudinal outcome data.
On the other hand, the principal outcome of interest of the ADNI is cognitive functioning, not emotional functioning, and its clinical assessments of mood and other psychiatric symptoms are limited. The assessment of depressive symptoms is by the interviewer-administered GDS with the research participant, and thus may lack the depth and accuracy of a structured psychiatric interview or observer ratings. Although the GDS is among the most well-validated and widely used scales for depressive symptoms in the elderly, its sensitivity wanes in people with dementia in comparison with other ‘gold-standard’ expert rater-based scales of depression in dementia.27 As well, ADNI was designed to recruit older adults who are typical of participants in clinical trials of AD and MCI. These focus on cognitive function unconfounded by depression or other illnesses that are common in general older populations. Indeed, eligibility in ADNI was restricted to participants with no active psychiatric illness and no more than very mild depressive symptoms at baseline. Despite these limitations, the sample size and expanding range of depressive symptoms over time did allow us to discern candidate biomarkers of depressive symptoms that are also biologically plausible. However, given the exclusion of subjects with any clinically significant depression at the time of enrollment in ADNI, it is important to recognize that our analyses may have failed to detect depression-related analytes that would be found in people with more severe symptoms or that our findings may be specific only to subsyndromal depressive symptoms in older adults and not major or minor depression in general.
There have been very few biomarker discovery investigations of psychiatric disorders that employ multi-analyte panels such as ours. Simon et al.69 tested a chronic inflammation hypothesis of major depressive disorder using a 22-plex cytokine/chemokine panel on a Luminex platform in 49 patients and 49 controls and found significant differences in most of the analytes, thus supporting their hypothesis. More recently, Domenici et al.70 used a 79-plex analyte panel from RBM to profile plasmas from 245 patients with recurrent major depressive disorder, 229 patients with schizophrenia and 254 nonpsychiatric controls. Many of the analytes in their panel were also measured in ours. In univariate analyses, the analyte that showed the greatest difference between depressed and control groups was insulin.
There is substantial evidence that higher levels of inflammatory biomarkers, such as tumor necrosis factor-α, various interleukins and transforming growth factor-β are present in major depression as well as AD.71, 72 Our analyses did not find any association between depressive symptoms and these inflammatory cytokines. However, it is important to again note the differences in subjects used in these studies, where ADNI specifically excludes participants with major depression.
There is growing recognition that chronic psychological distress is a risk factor for cognitive decline and aging-related dementias.73, 74, 75, 76 Consonant with this, we observed a >1.5-fold higher rate of past psychiatric illness among ADNI participants with MCI at baseline and an almost 2.5-fold higher rate in those with AD compared with those with normal cognition. The mechanism(s) by which depression and other facets of psychological distress increase dementia risk is not clear. Overall, post-mortem clinicopathological studies have not found associations between psychological distress and the defining pathologies of neurodegenerative dementias such as Aβ plaque or neurofibrillary τ tangle densities, α-synuclein Lewy bodies or cerebral infarcts.77, 78 Here as well, we saw no association between CSF τ or Aβ levels (as proxies for brain AD pathology) and depressive symptoms. Thus, it will be important to further investigate the candidate biomarkers associated with depressive symptoms identified in this study for their relationship to subsequent cognitive decline, to neuroimaging evidence of atrophy and other evidence of neurodegeneration and to post-mortem neuropathological findings as these become available.
References
Meeks TW, Vahia IV, Lavretsky H, Kulkarni G, Jeste DV . A tune in “a minor” can “b major”: a review of epidemiology, illness course, and public health implications of subthreshold depression in older adults. J Affect Disord 2010; 129: 126–142.
Thielke SM, Diehr P, Unutzer J . Prevalence, incidence, and persistence of major depressive symptoms in the Cardiovascular Health Study. Aging Ment Health 2010; 14: 168–176.
Dozeman E, van Marwijk HW, van Schaik DJ, Stek ML, van der Horst HE, Beekman AT et al. High incidence of clinically relevant depressive symptoms in vulnerable persons of 75 years or older living in the community. Aging Ment Health 2010; 14: 828–833.
Lyness JM, Heo M, Datto CJ, Ten Have TR, Katz IR, Drayer R et al. Outcomes of minor and subsyndromal depression among elderly patients in primary care settings. Ann Intern Med 2006; 144: 496–504.
Aznar S, Knudsen GM . Depression and Alzheimer's disease: is stress the initiating factor in a common neuropathological cascade? J Alzheimers Dis 2011; 23: 177–193.
Rodriguez-Oroz MC, Jahanshahi M, Krack P, Litvan I, Macias R, Bezard E et al. Initial clinical manifestations of Parkinson's disease: features and pathophysiological mechanisms. Lancet Neurol 2009; 8: 1128–1139.
Fang J, Cheng Q . Etiological mechanisms of post-stroke depression: a review. Neurol Res 2009; 31: 904–909.
Flicker L . Cardiovascular risk factors, cerebrovascular disease burden, and healthy brain aging. Clin Geriatr Med 2010; 26: 17–27.
Bremmer MA, Beekman AT, Deeg DJ, Penninx BW, Dik MG, Hack CE et al. Inflammatory markers in late-life depression: results from a population-based study. J Affect Disord 2008; 106: 249–255.
Penninx BW, Kritchevsky SB, Yaffe K, Newman AB, Simonsick EM, Rubin S et al. Inflammatory markers and depressed mood in older persons: results from the Health, Aging and Body Composition study. Biol Psychiatry 2003; 54: 566–572.
Forti P, Rietti E, Pisacane N, Olivelli V, Mariani E, Chiappelli M et al. Blood inflammatory proteins and risk of incident depression in the elderly. Dement Geriatr Cogn Disord 2010; 29: 11–20.
Bremmer MA, Deeg DJ, Beekman AT, Penninx BW, Lips P, Hoogendijk WJ . Major depression in late life is associated with both hypo- and hypercortisolemia. Biol Psychiatry 2007; 62: 479–486.
Amato L, Paolisso G, Cacciatore F, Ferrara N, Canonico S, Rengo F et al. Non-insulin-dependent diabetes mellitus is associated with a greater prevalence of depression in the elderly. The Osservatorio Geriatrico of Campania Region Group. Diabetes Metab 1996; 22: 314–318.
Lee KS, Chung JH, Lee KH, Shin MJ, Oh BH, Lee SH et al. Simultaneous measurement of 23 plasma cytokines in late-life depression. Neurol Sci 2009; 30: 435–438.
Diniz BS, Teixeira AL, Talib LL, Mendonca VA, Gattaz WF, Forlenza OV . Serum brain-derived neurotrophic factor level is reduced in antidepressant-free patients with late-life depression. World J Biol Psychiatry 2010; 11: 550–555.
Shi Y, You J, Yuan Y, Zhang X, Li H, Hou G . Plasma BDNF and tPA are associated with late-onset geriatric depression. Psychiatry Clin Neurosci 2010; 64: 249–254.
Lang UE, Hellweg R, Gallinat J . BDNF serum concentrations in healthy volunteers are associated with depression-related personality traits. Neuropsychopharmacology 2004; 29: 795–798.
Mueller SG, Weiner MW, Thal LJ, Petersen RC, Jack C, Jagust W et al. The Alzheimer's disease neuroimaging initiative. Neuroimaging Clin N Am 2005; 15: 869–877, xi–xii..
Aisen PS, Petersen RC, Donohue MC, Gamst A, Raman R, Thomas RG et al. Clinical Core of the Alzheimer's Disease Neuroimaging Initiative: progress and plans. Alzheimers Dement 2010; 6: 239–246.
Weiner MW, Aisen PS, Jack Jr CR, Jagust WJ, Trojanowski JQ, Shaw L et al. The Alzheimer's disease neuroimaging initiative: progress report and future plans. Alzheimers Dement 2010; 6: 202–211, e207.
Petersen RC, Aisen PS, Beckett LA, Donohue MC, Gamst AC, Harvey DJ et al. Alzheimer's Disease Neuroimaging Initiative (ADNI): clinical characterization. Neurology 2010; 74: 201–209.
Shaw LM . PENN Biomarker Core of the Alzheimer's Disease Neuroimaging Initiative. Neurosignals 2008; 16: 19–23.
Yesavage JA, Brink TL, Rose TL, Lum O, Huang V, Adey M et al. Development and validation of a geriatric depression screening scale: a preliminary report. J Psychiatr Res 1982; 17: 37–49.
Almeida OP, Almeida SA . Short versions of the geriatric depression scale: a study of their validity for the diagnosis of a major depressive episode according to ICD-10 and DSM-IV. Int J Geriatr Psychiatry 1999; 14: 858–865.
Mueller SG, Weiner MW, Thal LJ, Petersen RC, Jack CR, Jagust W et al. Ways toward an early diagnosis in Alzheimer's disease: the Alzheimer's Disease Neuroimaging Initiative (ADNI). Alzheimers Dement 2005; 1: 55–66.
Friedman B, Heisel MJ, Delavan RL . Psychometric properties of the 15-item geriatric depression scale in functionally impaired, cognitively intact, community-dwelling elderly primary care patients. J Am Geriatr Soc 2005; 53: 1570–1576.
Debruyne H, Van Buggenhout M, Le Bastard N, Aries M, Audenaert K, De Deyn PP et al. Is the geriatric depression scale a reliable screening tool for depressive symptoms in elderly patients with cognitive impairment? Int J Geriatr Psychiatry 2009; 24: 556–562.
Burke WJ, Roccaforte WH, Wengel SP . The short form of the geriatric depression scale: a comparison with the 30-item form. J Geriatr Psychiatry Neurol 1991; 4: 173–178.
Morris JC . The Clinical Dementia Rating (CDR): current version and scoring rules. Neurology 1993; 43: 2412–2414.
Trojanowski JQ, Vandeerstichele H, Korecka M, Clark CM, Aisen PS, Petersen RC et al. Update on the biomarker core of the Alzheimer's Disease Neuroimaging Initiative subjects. Alzheimers Dement 2010; 6: 230–238.
Ray S, Britschgi M, Herbert C, Takeda-Uchimura Y, Boxer A, Blennow K et al. Classification and prediction of clinical Alzheimer's diagnosis based on plasma signaling proteins. Nat Med 2007; 13: 1359–1362.
Laird NM, Ware JH . Random-effects models for longitudinal data. Biometrics 1982; 38: 963–974.
Rosen WG, Terry RD, Fuld PA, Katzman R, Peck A . Pathological verification of ischemic score in differentiation of dementias. Ann Neurol 1980; 7: 486–488.
Carroll BJ, Martin FI, Davies B . Resistance to suppression by dexamethasone of plasma 11-O.H.C.S. levels in severe depressive illness. Br Med J 1968; 3: 285–287.
Belmaker R, Beckmann H, Goodwin F, Murphy D, Pollin W, Buchsbaum M et al. Relationships between platelet and plasma monoamine oxidase, plasma dopamine-beta-hydroxylase, and urinary 3-methoxy-4-hydroxy phenylglycol. Life Sci 1975; 16: 273–280.
Karege F, Perret G, Bondolfi G, Schwald M, Bertschy G, Aubry JM . Decreased serum brain-derived neurotrophic factor levels in major depressed patients. Psychiatry Res 2002; 109: 143–148.
Nakamura T, Mizuno S . The discovery of hepatocyte growth factor (HGF) and its significance for cell biology, life sciences and clinical medicine. Proc Jpn Acad Ser B Phys Biol Sci 2010; 86: 588–610.
Jung W, Castren E, Odenthal M, Vande Woude GF, Ishii T, Dienes HP et al. Expression and functional interaction of hepatocyte growth factor-scatter factor and its receptor c-met in mammalian brain. J Cell Biol 1994; 126: 485–494.
Powell EM, Campbell DB, Stanwood GD, Davis C, Noebels JL, Levitt P . Genetic disruption of cortical interneuron development causes region- and GABA cell type-specific deficits, epilepsy, and behavioral dysfunction. J Neurosci 2003; 23: 622–631.
Nagayama T, Nagayama M, Kohara S, Kamiguchi H, Shibuya M, Katoh Y et al. Post-ischemic delayed expression of hepatocyte growth factor and c-Met in mouse brain following focal cerebral ischemia. Brain Res 2004; 999: 155–166.
Fenton H, Finch PW, Rubin JS, Rosenberg JM, Taylor WG, Kuo-Leblanc V et al. Hepatocyte growth factor (HGF/SF) in Alzheimer's disease. Brain Res 1998; 779: 262–270.
Akimoto M, Baba A, Ikeda-Matsuo Y, Yamada MK, Itamura R, Nishiyama N et al. Hepatocyte growth factor as an enhancer of nmda currents and synaptic plasticity in the hippocampus. Neuroscience 2004; 128: 155–162.
Date I, Takagi N, Takagi K, Kago T, Matsumoto K, Nakamura T et al. Hepatocyte growth factor improved learning and memory dysfunction of microsphere-embolized rats. J Neurosci Res 2004; 78: 442–453.
Takeuchi D, Sato N, Shimamura M, Kurinami H, Takeda S, Shinohara M et al. Alleviation of Abeta-induced cognitive impairment by ultrasound-mediated gene transfer of HGF in a mouse model. Gene Therapy 2008; 15: 561–571.
Isogawa K, Akiyoshi J, Kodama K, Matsushita H, Tsutsumi T, Funakoshi H et al. Anxiolytic effect of hepatocyte growth factor infused into rat brain. Neuropsychobiology 2005; 51: 34–38.
Wakatsuki M, Akiyoshi J, Ichioka S, Tanaka Y, Tsuru J, Matsushita H et al. Administration of antisense DNA for hepatocyte growth factor causes an depressive and anxiogenic response in rats. Neuropeptides 2007; 41: 477–483.
Russo AJ . Decreased serum hepatocyte growth factor (HGF) in individuals with depression correlates with severity of disease. Biomark Insights 2010; 5: 63–67.
Kahl KG, Bens S, Ziegler K, Rudolf S, Kordon A, Dibbelt L et al. Angiogenic factors in patients with current major depressive disorder comorbid with borderline personality disorder. Psychoneuroendocrinology 2009; 34: 353–357.
Kanehisa M, Ishitobi Y, Ando T, Okamoto S, Maruyama Y, Kohno K et al. Serum hepatocyte growth factor levels and the effects of antidepressants in panic disorder. Neuropeptides 2010; 44: 431–435.
Okamura F, Tashiro A, Utumi A, Imai T, Suchi T, Tamura D et al. Insulin resistance in patients with depression and its changes during the clinical course of depression: minimal model analysis. Metabolism 2000; 49: 1255–1260.
Pouwer F, Beekman AT, Nijpels G, Dekker JM, Snoek FJ, Kostense PJ et al. Rates and risks for co-morbid depression in patients with Type 2 diabetes mellitus: results from a community-based study. Diabetologia 2003; 46: 892–898.
Pan A, Lucas M, Sun Q, van Dam RM, Franco OH, Manson JE et al. Bidirectional association between depression and type 2 diabetes mellitus in women. Arch Intern Med 2010; 170: 1884–1891.
Weber-Hamann B, Gilles M, Lederbogen F, Heuser I, Deuschle M . Improved insulin sensitivity in 80 nondiabetic patients with MDD after clinical remission in a double-blind, randomized trial of amitriptyline and paroxetine. J Clin Psychiatry 2006; 67: 1856–1861.
Knol MJ, Twisk JW, Beekman AT, Heine RJ, Snoek FJ, Pouwer F . Depression as a risk factor for the onset of type 2 diabetes mellitus. A meta-analysis. Diabetologia 2006; 49: 837–845.
Vogelzangs N, Suthers K, Ferrucci L, Simonsick EM, Ble A, Schrager M et al. Hypercortisolemic depression is associated with the metabolic syndrome in late-life. Psychoneuroendocrinology 2007; 32: 151–159.
Lute BJ, Khoshbouei H, Saunders C, Sen N, Lin RZ, Javitch JA et al. PI3K signaling supports amphetamine-induced dopamine efflux. Biochem Biophys Res Commun 2008; 372: 656–661.
Robertson SD, Matthies HJ, Owens WA, Sathananthan V, Christianson NS, Kennedy JP et al. Insulin reveals Akt signaling as a novel regulator of norepinephrine transporter trafficking and norepinephrine homeostasis. J Neurosci 2010; 30: 11305–11316.
Conover CA, Bale LK, Overgaard MT, Johnstone EW, Laursen UH, Fuchtbauer EM et al. Metalloproteinase pregnancy-associated plasma protein A is a critical growth regulatory factor during fetal development. Development 2004; 131: 1187–1194.
Viikki M, Anttila S, Kampman O, Illi A, Huuhka M, Setala-Soikkeli E et al. Vascular endothelial growth factor (VEGF) polymorphism is associated with treatment resistant depression. Neurosci Lett 2010; 477: 105–108.
Tsai SJ, Hong CJ, Liou YJ, Chen TJ, Chen ML, Hou SJ et al. Haplotype analysis of single nucleotide polymorphisms in the vascular endothelial growth factor (VEGFA) gene and antidepressant treatment response in major depressive disorder. Psychiatry Res 2009; 169: 113–117.
Iga J, Ueno S, Yamauchi K, Numata S, Tayoshi-Shibuya S, Kinouchi S et al. Gene expression and association analysis of vascular endothelial growth factor in major depressive disorder. Prog Neuropsychopharmacol Biol Psychiatry 2007; 31: 658–663.
Takebayashi M, Hashimoto R, Hisaoka K, Tsuchioka M, Kunugi H . Plasma levels of vascular endothelial growth factor and fibroblast growth factor 2 in patients with major depressive disorders. J Neural Transm 2010; 117: 1119–1122.
Ventriglia M, Zanardini R, Pedrini L, Placentino A, Nielsen MG, Gennarelli M et al. VEGF serum levels in depressed patients during SSRI antidepressant treatment. Prog Neuropsychopharmacol Biol Psychiatry 2009; 33: 146–149.
Ferrara N, Gerber HP, LeCouter J . The biology of VEGF and its receptors. Nat Med 2003; 9: 669–676.
Rigau V, Morin M, Rousset MC, de Bock F, Lebrun A, Coubes P et al. Angiogenesis is associated with blood-brain barrier permeability in temporal lobe epilepsy. Brain 2007; 130 (Pt 7): 1942–1956.
Udo H, Yoshida Y, Kino T, Ohnuki K, Mizunoya W, Mukuda T et al. Enhanced adult neurogenesis and angiogenesis and altered affective behaviors in mice overexpressing vascular endothelial growth factor 120. J Neurosci 2008; 28: 14522–14536.
McCloskey DP, Croll SD, Scharfman HE . Depression of synaptic transmission by vascular endothelial growth factor in adult rat hippocampus and evidence for increased efficacy after chronic seizures. J Neurosci 2005; 25: 8889–8897.
Cao L, Jiao X, Zuzga DS, Liu Y, Fong DM, Young D et al. VEGF links hippocampal activity with neurogenesis, learning and memory. Nat Genet 2004; 36: 827–835.
Simon NM, McNamara K, Chow CW, Maser RS, Papakostas GI, Pollack MH et al. A detailed examination of cytokine abnormalities in major depressive disorder. Eur Neuropsychopharmacol 2008; 18: 230–233.
Domenici E, Wille DR, Tozzi F, Prokopenko I, Miller S, McKeown A et al. Plasma protein biomarkers for depression and schizophrenia by multi analyte profiling of case-control collections. PLoS One 2010; 5: e9166.
Dowlati Y, Herrmann N, Swardfager W, Liu H, Sham L, Reim EK et al. A meta-analysis of cytokines in major depression. Biol Psychiatry 2010; 67: 446–457.
Swardfager W, Lanctot K, Rothenburg L, Wong A, Cappell J, Herrmann N . A meta-analysis of cytokines in Alzheimer's disease. Biol Psychiatry 2010; 68: 930–941.
Wilson RS, Arnold SE, Schneider JA, Kelly JF, Tang Y, Bennett DA . Chronic psychological distress and risk of Alzheimer's disease in old age. Neuroepidemiology 2006; 27: 143–153.
Wilson RS, Barnes LL, Mendes de Leon CF, Aggarwal NT, Schneider JS, Bach J et al. Depressive symptoms, cognitive decline, and risk of AD in older persons. Neurology 2002; 59: 364–370.
Yaffe K, Vittinghoff E, Lindquist K, Barnes D, Covinsky KE, Neylan T et al. Posttraumatic stress disorder and risk of dementia among US veterans. Arch Gen Psychiatry 2010; 67: 608–613.
Crowe M, Andel R, Pedersen NL, Gatz M . Do work-related stress and reactivity to stress predict dementia more than 30 years later? Alzheimer Dis Assoc Disord 2007; 21: 205–209.
Wilson RS, Arnold SE, Schneider JA, Li Y, Bennett DA . Chronic distress, age-related neuropathology, and late-life dementia. Psychosom Med 2007; 69: 47–53.
Milwain EJ, Nagy Z . Depressive symptoms increase the likelihood of cognitive impairment in elderly people with subclinical Alzheimer pathology. Dement Geriatr Cogn Disord 2005; 19: 46–50.
Acknowledgements
The principal sources of support for this work were NIH AG10124, AG033101 and AG10161, the Marian S Ware Alzheimer's Program, Burroughs Wellcome Career Award for medical scientists, the Benaroya Fund and the Penn-Pfizer Alliance. Data collection and sharing for this project was funded by the Alzheimer's Disease Neuroimaging Initiative (ADNI; National Institutes of Health Grant U01 AG024904). ADNI is funded by the National Institute on Aging, the National Institute of Biomedical Imaging and Bioengineering, and through generous contributions from the following: Abbott, AstraZeneca AB, Bayer Schering Pharma AG, Bristol-Myers Squibb, Eisai Global Clinical Development, Elan Corporation, Genentech, GE Healthcare, GlaxoSmithKline, Innogenetics, Johnson and Johnson, Eli Lilly, Medpace, Merck, Novartis AG, Pfizer, F Hoffman-La Roche, Schering-Plough and Synarc, as well as from non-profit partners such as the Alzheimer's Association and Alzheimer's Drug Discovery Foundation, with participation from the US Food and Drug Administration. Private sector contributions to ADNI are facilitated by the Foundation for the National Institutes of Health (www.fnih.org). The grantee organization is the Northern California Institute for Research and Education, and the study is coordinated by the Alzheimer's Disease Cooperative Study at the University of California, San Diego. ADNI data are disseminated by the Laboratory for Neuro Imaging at the University of California, Los Angeles. This research was also supported by the NIH Grants P30 AG010129, K01 AG030514, and the Dana Foundation.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Translational Psychiatry website
Supplementary information
Rights and permissions
This work is licensed under the Creative Commons Attribution-NonCommercial-No Derivative Works 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Arnold, S., Xie, S., Leung, YY. et al. Plasma biomarkers of depressive symptoms in older adults. Transl Psychiatry 2, e65 (2012). https://doi.org/10.1038/tp.2011.63
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/tp.2011.63
Keywords
This article is cited by
-
Alteration of transthyretin and thyroxine-binding globulin in major depressive disorder: multiple reaction monitoring-based proteomic analysis
Journal of Translational Medicine (2021)
-
Depression Augments Plasma APOA4 without Changes of Plasma Lipids and Glucose in Female Adolescents Carrying G Allele of APOA4 rs5104
Journal of Molecular Neuroscience (2021)
-
Reduced plasma Fetuin-A is a promising biomarker of depression in the elderly
European Archives of Psychiatry and Clinical Neuroscience (2020)
-
Serum proteomic profiles of depressive subtypes
Translational Psychiatry (2016)
-
Identification of genes and gene pathways associated with major depressive disorder by integrative brain analysis of rat and human prefrontal cortex transcriptomes
Translational Psychiatry (2015)