Abstract
Combination targeted therapy is commonly used to treat acute myeloid leukemia (AML) patients, particularly in refractory/relapse (RR) population. However, concerns have been raised regarding the safety and patient tolerance of combination chemotherapy. It is critical to choose the appropriate treatment for precision therapy. We performed genome-wide RNA profiling using RNA-Seq to compare the RR group and the complete remission (CR) group (a total of 42 adult AML patients). The Hedgehog (Hh) and PI3K/AKT pathways were upregulated in the RR population, which was further confirmed by western blot and/or qPCR. Overexpression of GLI1 in AML cells led to increased AKT phosphorylation and decreased drug sensitivity, which was attenuated by GLI1 inhibition. By contrast, neither the expression of GLI1 nor apoptosis in response to Ara-C treatment of AML cells was significantly affected by PI3K inhibition. Furthermore, co-inhibition of GLI1 and PI3K induced apoptosis of hematopoietic stem/progenitor cells (HSPCs), which raised serious concerns about the side effects of this treatment. These results indicated that GLI1 inhibition alone, but not combined inhibition, is sufficient to enhance AML drug sensitivity, which provides a novel therapeutic strategy for AML treatment.
Similar content being viewed by others
Introduction
Acute myeloid leukemia (AML) is a hematological malignancy with high incidence and recurrence rates. The high recurrence of AML reflects the incomplete eradication of leukemia stem cells by conventional chemotherapy and Ara-C combination chemotherapy, which are the most commonly used treatments. Approximately 20% of adult patients with AML fail to achieve remission with initial induction chemotherapy, and approximately 50% ultimately experience relapse after achieving complete remission1,2,3. A major side effect of the current chemotherapy is toxicity to hematopoietic stem cells (HSCs). Although hematopoietic stem cell transplantation (HSCT) is a promising therapeutic strategy for AML, the absence of Human leukocyte antigen(HLA)-matched donors and the risk of post-transplantation rejection are major challenges. Additionally, the high cost and mortality rate limit its application in clinical practice. As new developments have been made in molecular biology and genetics, targeted therapy or combination targeted therapy has been shown to be a promising area of research for AML4,5.
As the pathogenesis of AML involves regulation of different signalling pathways, the interaction and feedback among different signalling pathways are expected to be involved in the clinical treatment of AML. It is therefore critical to understand the interactions of these signalling pathways to provide a precise diagnosis for patients. Genomic approaches have identified somatic mutations in coding genes that are associated with patients’ prognosis. In transcriptome research, microarrays have been extensively used to identify a number of differentially expressed genes6,7,8. Microarray techniques and, more recently, RNA sequencing (RNA-Seq) technology have been widely used to analyse the global transcriptome changes in different malignancies9,10.
The Hh pathway plays an important role in cell proliferation, differentiation, apoptosis and migration. It has been shown to cross-talk with other signalling pathways (such as PI3K/AKT, RAS, NOTCH and others) and has been identified as a major target in the treatment of hematological malignancies11,12,13. In chronic myeloid leukemia (CML), inhibition of the Hh pathway could reduce the number of leukemia stem cells and reverse drug resistance to imatinib14. Recently Zahreddine et al. also demonstrated that a key transcription factor of the Hh pathway, GLI1, affects drug resistance by inducing glucuronidation, which could be reversed by a Hh inhibitor15. In addition, several clinical studies have reported that the expression of GLI1 is closely related to the prognosis of acute myeloid leukemia (AML)16.
Meanwhile, sustained activation of the PI3K/AKT pathway has been identified in different types of leukemia, and this effect promotes cell cycle progression, inhibits cell apoptosis and facilitates invasion and metastasis of cancer cells17,18,19. Our group found that PTEN-regulated PI3K/AKT activation is closely related to the progression and drug resistance of adult AML20. In addition, it has been shown that combined inhibition of the Hh and PI3K/AKT pathways has synergistic anti-leukemia effects in AML and in chronic lymphocytic leukemia21,22,23.
However, whether there is cross-talk between the Hh and PI3K/AKT pathways in AML drug resistance/relapse and the potential risk of combined inhibition of these pathways in AML patients are still unknown. The possibility of using Hh and PI3K double inhibition in clinical AML treatment requires further study.
By comparing the clinical samples of AML-RR and AML-CR patients using RNA-Seq, we showed that both the Hh and PI3K/AKT pathways were upregulated in the AML-RR group. Moreover, overexpression of GLI1 decreased drug sensitivity in AML cells, which could be reversed by a GLI1 inhibitor. In addition, GLI1 inhibition blocked the PI3K/AKT pathway, whereas PI3K inhibition had no effect on GLI1 expression or AML cell drug sensitivity. This study describes a novel mechanism of Hh and PI3K/AKT pathway interaction in chemo-resistance and relapse of AML patients, which provides guidance to develop an efficient and safe combination targeted therapy for AML-RR patients.
Results
The Hh pathway is activated in AML-RR patients
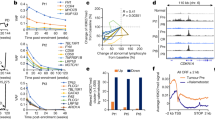
Forty-two AML patients were recruited in this study. Based on their clinical history, the patients were classified into two groups: the refractory/relapse (AML-RR) group and the complete remission (AML-CR) group (Tables 1 and 2). RNAs were isolated from mononuclear cells (MNCs) of these patients and analysed using RNA-Seq. To identify significant differences in the transcriptomic profiles of the two sample groups (AML-RR and AML-CR), we generated a pair wise scatter matrix by CummeRbund. This method compares and correlates the RPKM profile of all expressed genes in the two sample groups, and it also shows the density distribution of the RPKM for the expressed genes. The RPKM of all expressed genes ranged from 0.003 to 3000 (log10RPKM −2.5 to 3.5), with the majority of the genes ranging from 1 to 100 (log10RPKM 0 to 2). The majority of genes involved in the Hh pathway, such as GLI, SMO, SHH, and PTCH, (Fig. 1a–c, Table 3) were upregulated in the AML-RR group compared with the AML-CR group. qRT-PCR and western blot further confirmed the upregulation of GLI1, a key transcript of the Hh pathway, at the mRNA (Fig. 1d, P < 0.01) and protein (Fig. 1e,f, P < 0.05) levels in the AML-RR group. These results were consistent with the RNA-Seq results, which indicated that the Hh pathway may be related to the progression and prognosis of AML.
(a) Hh pathway-related gene expression in AML patients. (b) Core component Hh pathway gene expression in AML patients. (c) Fold-change of selected Hh-related genes in AML patients. (d) GLI1 transcript expression in AML-CR and AML-RR patients. (e,f) Western blot analysis and quantification of GLI1 protein expression in AML-CR and AML-RR patients. *P < 0.05, **P < 0.01.
The PI3K/AKT pathway is also activated in AML-RR patients
As previously noted, we also found that the majority of genes involved in the PI3K/AKT pathway, such as AKT1, AKT2, AKT3, and BTK (Fig. 2a–c, Table 3) were upregulated in the AML-RR group compared with the AML-CR group. Western blot validated the increased phosphorylation of AKT in the AML-RR group (Fig. 2d,e, P < 0.01). Together, these results suggested that the PI3K/AKT pathway is activated in the AML-RR group.
(a) Heatmap of PI3K/AKT-related genes. (b) Heatmap of selected PI3K/AKT-related genes. (c) Fold-change in the expression of selected PI3K/AKT-related genes in AML-CR and AML-RR patients. (d,e) Western blot analysis (d) and quantification of AKT and p-AKT protein expression (e) in AML-CR and AML-RR patients. *P < 0.05, **P < 0.01.
Overexpression of GLI1 upregulated p-AKT and this effect is abolished by a GLI1 inhibitor in acute myeloid leukemia cell lines
To explore the role of GLI1 and the relationship of Hh and the PI3K/AKT pathway in AML relapse and drug resistance, GLI1 was overexpressed in both HL60 and NB4 cells by a lentiviral vector carrying EGFP for selection. Seventy-two hours after infection, cells were sorted by FACS to establish new cell lines, which were named HL60/GLI1 and NB4/GLI1. The upregulation of GLI1 in HL60/GLI1 and NB4/GLI1 was also confirmed by both RT-PCR (Fig. 3a,b) and western blot (Fig. 3c,d). Interestingly, overexpression of GLI1 increased the p-AKT level. GANT61, a GLI1 inhibitor, could reverse the increase in p-AKT by GLI1 overexpression, suggesting that GLI1 functions upstream of p-AKT. LY294002, a PI3K inhibitor, did not inhibit the expression of GLI1 (Fig. 3a–d). These results indicate that GLI1 could regulate the expression of p-AKT and had a unidirectional regulatory effect on the PI3K/AKT pathway.
(a,b) The transcript expression of GLI1 in both wild-type and GLI1 overexpressing HL60 cells (a) and NB4 cells (b) treated with 20 μM GANT61 or 20 μM LY294002. (c,d) The protein expression of GLI1 and p-AKT in both wild-type and GLI1 overexpressing HL60 cells (c) and NB4 cells (d) treated with 20 μM GANT61 or 20 μM LY294002. *P < 0.05, **P < 0.01.
Inhibition of GLI1 could inhibit AML cell growth
Ara-C was assessed for its ability to inhibit AML cell growth and apoptosis. Ara-C inhibited the growth of HL60 and NB4 cells in a dose-dependent manner with an IC50 of 4 μM for the HL60 cells (Fig. 4a) and an IC50 of 25 μM for the NB4 cells (Fig. 4b). A time course experiment was used to optimize the timing and dose of Ara-C. HL60 and NB4 cells were treated with different concentration up to 48 h. The growth inhibition rate did not increase significantly when cells were treated with Ara-C at concentrations higher than 10 μM at both 24 h and 48 h (Fig. 4a–c). We found that the cell growth inhibition rates in both HL60/GLI1 and NB4/GLI1 cells were significantly lower than the wild-type cells. However, GANT61 treatment could compensate for this difference, suggesting that GLI1 is both sufficient and necessary to decrease drug sensitivity of Ara-C. Consistent with the previous results showing that LY294002 does not affect GLI1 expression, LY294002 inhibited neither HL60/GLI1 nor NB4/GLI1 cell growth (Fig. 4d,e). Besides, there was no difference in growth inhibition rate between the treatment of GANT61 or LY294002 in wild-type cells (Supplementary Fig. S4a). A major safety concern for AML is that the chemotherapy drugs also lead to severe bone marrow depression, which is related to the inhibition of proliferation in human HSPCs. Here, we tested the effect of GANT61 (20 μM), LY294002 (20 μM), and GANT61 + LY294002 (20 μM) on HSPCs. Surprisingly, the cell growth inhibition rate of the HSPCs in the GANT61 + LY294002 (20 μM) treatment group was higher than 90% (Fig. 4f), which raises the serious safety concern that the combination treatment may impair the human hematopoietic system.
(a) Growth inhibition rate of HL60 cells with Ara-C, IC50 (half maximal inhibitory concentration) = 4 μM. (b) Growth inhibition rate of NB4 cells with Ara-C, IC50 = 25 μM. (c) Growth inhibitory curve of HL60 and NB4 cells in their IC50 values. (d) The growth inhibition rate in both wild-type and GLI1 overexpressing HL60 cells treated with Ara-C and GANT61/LY294002. (e) The growth inhibition rate in both wild-type and GLI1 overexpressing NB4 cells treated with Ara-C and GANT61/LY294002. (f) The growth inhibition rate in HSPCs treated with Ara-C (4 μM) and GANT61/LY294002. The results are shown as the mean of three independent experiments ± s.d. *P < 0.05.
Inhibition of GLI1 could enhance acute myeloid leukemia cell drug sensitivity
To test drug sensitivity, both wild-type and GLI1 overexpressing cells were treated with Ara-C only, Ara-C + GANT61 (20 μM), and Ara-C + LY294002 (20 μM) separately for 48 hours, and cell apoptosis was assessed using Annexin V assays (Fig. 5a,d). Consistent with the cell growth inhibitory results, GANT61 significantly enhanced the drug sensitivity of HL60 and NB4 cells, whereas LY294002 failed to do so (Fig. 5b,c). While, there was no difference in cell death rate between the treatment of GANT61 or LY294002 in wild-type cells (Supplementary Fig. S4b). Moreover, we found that the apoptosis rate of HSPCs with both inhibitors was significantly higher than that in the control group, which raises a serious concern about the safety of the combination treatment (Fig. 5e,f).
(a,d) Flow cytometry scatter plot of both wild-type and GLI1 overexpressing HL60 cells (a) or NB4 cells (d) treated with Ara-C and GLI1 inhibitor or the PI3K inhibitor. (b,c) Cell death rate in both wild-type and GLI1 overexpressing HL60 (b) or NB4 (c) cells treated with Ara-C and GLI1 inhibitor or PI3K inhibitor. (e,f) Flow cytometry scatter plot and cell death rate of HSPCs with both inhibitors of GLI1 and PI3K. *P < 0.05.
Discussion
As the morbidity and mortality of leukemia are increasing every year, developing effective and safe treatment strategies is of great urgency. In recent years, targeted therapy, which is considered to be one of the most promising treatments for AML, has been extensively researched. However, only a few targeted drugs have been successful in clinical practice, such as all trans-retinoic acid and imatinib24,25,26. Therefore, new targets and associated drugs are necessary for future treatment of AML.
In this study, by comparing gene expression profiles of clinical bone marrow samples from AML-CR and AML-RR patients using RNA-Seq technology, we found that the Hh and PI3K/AKT pathways were upregulated in the AML-RR group. Consistent with the results of RNA-Seq, RT-PCR and western blot analyses also showed upregulated expression of GLI1 and p-AKT in the AML-RR patients. An in vitro study showed that inhibition of GLI1 depressed p-AKT activation and increased Ara-C sensitivity in leukemia cells, which is consistent with previous reports12,15,27. These results indicated that these pathways might play important roles in the progression and drug resistance of leukemia. Nevertheless, the expression of GLI1 in AML cells was not significantly affected by the PI3K inhibitor LY294002. Recently, several studies have reported that combined inhibition of the Hh and PI3K/AKT pathways can effectively inhibit the growth of cancer cells and has a synergistic anticancer effect on various tumours, such as rhabdomyosarcoma, pancreatic cancer, ovarian cancer and others28,29,30. These reports provided a basis for combination therapies targeting the Hh/GLI and PI3K pathways. However, the feasibility of clinical application has yet to be fully defined. In addition, our results showed that the both inhibitors had an irreversible and severe cytotoxicity to HSPCs, which raised the question of how to maximize the anti-leukemia effect of combined inhibition while minimizing the side effects to normal cells.
Other groups have shown that the AKT1 promoter possesses two GLI1 binding sites (BS1 and BS2) and proved the expression of AKT1 was regulated at the transcriptional level by GLI131. Our results suggested that for AML patients with both GLI1 and AKT activation, the GLI1 inhibitor alone is sufficient, which will significantly decrease the unnecessary side effects of the combination therapy using Hh and PI3K inhibitors. The GLI1 inhibitor would provide a potential targeted therapy to AML cells, which have been reported in other hematonosis32. Additional studies are needed to identify the feasibility of clinical application by using GLI1 inhibitor in refractory/relapse population of AML patients.
Our study characterizes the Hh and PI3K/AKT interaction in AML drug sensitivity, which may provide a theoretical basis for further research of targeted therapy.
Materials and Methods
Cell culture and transfection
HL60 and NB4 cells were obtained from the Cell Resource Centre (Xiangya Medical College, Central South University, Hunan, China). The cell lines were maintained in RPMI-1640 medium (Corning Inc., Corning, NY, USA) containing 10% foetal bovine serum (Corning Inc.) and 1% antibiotic solution of penicillin/streptomycin (Sigma, MO, USA) in a 37 °C incubator with a humidified atmosphere of 5% CO2 (Supplementary Fig. S2). To overexpress GLI1, AML cells were infected with lentivirus containing the GLI1 open reading frame (MOI: 50–100). After 72 h of infection, HL60 and NB4 lines were allowed to recover for 24 h with fresh media and were referred to as HL60/GLI1 and NB4/GLI1 cells (Supplementary Fig. S3). To evaluate the response to drug treatment, 1 × 106 HL60/GLI1 and NB4/GLI1 cells were seeded in 6-well culture plates and incubated with either 20 μM GANT61 (Adooq Bioscience, A13252) or 20 μM LY294002 (Adooq Bioscience, A10547) for 72 h prior to subsequent measurements.
Patient characteristics
Liquid bone marrow samples from 42 patients between 18 and 64 years old, who were diagnosed with AML according to the 2008 WHO criteria and treated at Xiangya Hospital of Central South University, Hunan, China, were included in the AML group (Tables 1 and 2, Supplementary Fig. S1). For comparison, 15 healthy candidate donors were included as normal controls. The experimental protocols were approved by the ethical committee of Xiangya Hospital, Central South University. The informed consent was obtained from all the research subjects. All the bone marrow samples were collected into sterile tubes with anticoagulant (heparin sodium). Mononuclear cells (MNCs) were enriched by density centrifugation over Ficoll-Paque (Sigma, St. Louis, MO, USA) and stored at −80 °C.
RNA-Seq
RNA sample quality was analysed, and the cDNA libraries were synthesized and sequenced using BGI technology. In brief, the quality of the RNA samples was assessed by an Agilent Bioanalyzer (Agilent). cDNA libraries were generated using TruSeq RNA Sample Preparation (Illumina). Each library was sequenced using single-reads on a HiSeq2000/1000 (Illumina). Gene expression levels were measured in RPKM using Cufflinks33,34.
Quantitative RT-PCR and RT-PCR
RNA was isolated from 1 × 106 cells using TRIzol reagent (TaKaRa, Japan, Cat#9109). Total RNA (500 ng) was reverse transcribed into first strand cDNA using a PrimeScriptTM RT Reagent Kit (TaKaRa, Japan, Cat#RR047A). cDNA was amplified in a total volume of 10 μl using SYBR qPCR Mix (Toy-obo, TOYOBO, Japan, Lot:266400), and the amplification was performed by ABI StepOnePlus (Applied Biosystems, Foster City, CA, USA) with specific primers (Table 4). The thermal cycler conditions were as follows: 95 °C for 2 min, followed by 40 cycles of 95 °C for 10 s, 58 °C for 20 s, and 68 °C for 50 s.
Western blot analysis
Equal amounts of protein were solubilized in sample buffer and electrophoresed on denaturing SDS-polyacrylamide gels and then transferred to polyvinylidene fluoride (PVDF) membranes (Millipore, Billerica, MA, USA). The membranes were saturated in TBST containing 5% BSA (Bio Sharp Sigma A-4612) for an hour at room temperature and incubated with the primary antibodies overnight at 4 °C. After incubation with secondary antibody, the blots were then washed and detected with a ChemiDoc MP System (Bio-Rad Laboratories. Inc., Hercules, CA, USA). The antibodies were used as follows: mAb rabbit anti-GLI1 (C68H3) (Cell Signaling, 3538), mAb rabbit anti-phospho-AKT (Ser473) (Cell Signaling, 4060), mAb rabbit anti-AKT (Cell Signaling, 9272), anti-GAPDH (Santa Cruz, CA, USA), and horseradish peroxidase (HRP)-conjugated goat anti-rabbit IgG (Santa Cruz, CA, USA).
CCK8 assay
The inhibition effect of cell proliferation was measured by a Cell Counting Kit-8 assay (7sea biotech, China) using different concentrations of Ara-C (Solarbio, Lot. No. 317B002) according to the protocol provided by the manufacturer. Then, 2 × 104 cells were seeded in 96-well culture plates in 100 μL of medium per well and treated with Ara-C at IC50 (half maximal inhibitory concentration) and GANT61/LY294002 (20 μm) for 24 h. Finally, 10 μl CCK8 solution was added to each well, and the cells were incubated further for 3 h at 37 °C. Cell viability was evaluated based on the absorbance at 450 nm compared with 630 nm. The growth inhibition rate = (1 − OD value of treatment/OD value of control) × 100%.
Annexin V APC assay
In each well, 1 × 106 cells were seeded in 6-well culture plates and treated with Ara-C at its IC50 and GANT61/LY294002 (20 μm). After 24 h of culture, cells were analysed by flow cytometry with an Annexin V-APC kit (Beyotime Institute) to determine the cell death rate.
Statistical analysis
All experiments were repeated independently at least three times, and the data were represented as the mean ± SD of the vehicle controls. All groups were compared using the Statistical Package for the Social Sciences (SPSS) version 20.0. The differences between the populations were assessed by analysis of covariance (ANCOVA). The diagrams were generated by GraphPad Prism 6 software. Significance was defined as *P < 0.05, **P < 0.01, ***P < 0.001, and ****P < 0.0001.
Ethical approval
The experimental protocols and methods were performed in accordance with relevant guidelines and regulations. The informed consent was obtained from all the research subjects.
Additional Information
How to cite this article: Liang, H. et al. Targeting the PI3K/AKT pathway via GLI1 inhibition enhanced the drug sensitivity of acute myeloid leukemia cells. Sci. Rep. 7, 40361; doi: 10.1038/srep40361 (2017).
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
Breems, D. A. et al. Prognostic index for adult patients with acute myeloid leukemia in first relapse. J. Clin. Oncol. 23, 1969–1978 (2005).
Ravandi, F. et al. Characteristics and outcome of patients with acute myeloid leukemia refractory to 1 cycle of high-dose cytarabine-based induction chemotherapy. Blood 116, 5818–5823, quiz 6153 (2010).
Walter, R. B. et al. Effect of complete remission and responses less than complete remission on survival in acute myeloid leukemia: a combined Eastern Cooperative Oncology Group, Southwest Oncology Group, and M. D. Anderson Cancer Center Study. J. Clin. Oncol. 28, 1766–1771 (2010).
Thomas, X. & Cannas, G. Leukemia stem cells and new strategies to overcome resistance to therapy. Curr Stem Cell Res Ther 5, 277–286 (2010).
Wang, Z. et al. Glycogen synthase kinase 3 in MLL leukaemia maintenance and targeted therapy. Nature 455, 1205–1209 (2008).
Klein, U. et al. Gene expression profiling of B cell chronic lymphocytic leukemia reveals a homogeneous phenotype related to memory B cells. J. Exp. Med. 194, 1625–1638 (2001).
Haslinger, C. et al. Microarray gene expression profiling of B-cell chronic lymphocytic leukemia subgroups defined by genomic aberrations and VH mutation status. J. Clin. Oncol. 22, 3937–3949 (2004).
Rosenwald, A. et al. Relation of gene expression phenotype to immunoglobulin mutation genotype in B cell chronic lymphocytic leukemia. J. Exp. Med. 194, 1639–1647 (2001).
Ren, S. et al. RNA-seq analysis of prostate cancer in the Chinese population identifies recurrent gene fusions, cancer-associated long noncoding RNAs and aberrant alternative splicings. Cell Res. 22, 806–821 (2012).
Shah, S. P. et al. The clonal and mutational evolution spectrum of primary triple-negative breast cancers. Nature 486, 395–399 (2012).
Irvine, D. A. & Copland, M. Targeting hedgehog in hematologic malignancy. Blood 119, 2196–2204 (2012).
Zhao, C. et al. Hedgehog signalling is essential for maintenance of cancer stem cells in myeloid leukaemia. Nature 458, 776–779 (2009).
Campbell, V. & Copland, M. Hedgehog signaling in cancer stem cells: a focus on hematological cancers. Stem Cells Cloning 8, 27–38 (2015).
Dierks, C. et al. Expansion of Bcr-Abl-positive leukemic stem cells is dependent on Hedgehog pathway activation. Cancer Cell 14, 238–249 (2008).
Zahreddine, H. A. et al. The sonic hedgehog factor GLI1 imparts drug resistance through inducible glucuronidation. Nature 511, 90–93 (2014).
Wellbrock, J. et al. Expression of Hedgehog Pathway Mediator GLI Represents a Negative Prognostic Marker in Human Acute Myeloid Leukemia and Its Inhibition Exerts Antileukemic Effects. Clin. Cancer Res. 21, 2388–2398 (2015).
Xu, Q. et al. Survival of acute myeloid leukemia cells requires PI3 kinase activation. Blood 102, 972–980 (2003).
Samuels, Y. et al. High frequency of mutations of the PIK3CA gene in human cancers. Science 304, 554 (2004).
Kubota, Y. et al. Constitutive activation of PI3K is involved in the spontaneous proliferation of primary acute myeloid leukemia cells: direct evidence of PI3K activation. Leukemia 18, 1438–1440 (2004).
Huang, F. F. et al. Inactivation of PTEN increases ABCG2 expression and the side population through the PI3K/Akt pathway in adult acute leukemia. Cancer Lett. 336, 96–105 (2013).
Lin, T. L. et al. Self-renewal of acute lymphocytic leukemia cells is limited by the Hedgehog pathway inhibitors cyclopamine and IPI-926. PLoS One 5, e15262 (2010).
Hou, X. et al. Inhibition of hedgehog signaling by GANT58 induces apoptosis and shows synergistic antitumor activity with AKT inhibitor in acute T cell leukemia cells. Biochimie 101, 50–59 (2014).
Kern, D. et al. Hedgehog/GLI and PI3K signaling in the initiation and maintenance of chronic lymphocytic leukemia. Oncogene 34, 5341–5351 (2015).
Castaigne, S. et al. All-trans retinoic acid as a differentiation therapy for acute promyelocytic leukemia. I. Clinical results. Blood 76, 1704–1709 (1990).
Talpaz, M. et al. Imatinib induces durable hematologic and cytogenetic responses in patients with accelerated phase chronic myeloid leukemia: results of a phase 2 study. Blood 99, 1928–1937 (2002).
Druker, B. J. et al. Efficacy and safety of a specific inhibitor of the BCR-ABL tyrosine kinase in chronic myeloid leukemia. N. Engl. J. Med. 344, 1031–1037 (2001).
Lu, F. L. et al. Sonic hedgehog antagonists induce cell death in acute myeloid leukemia cells with the presence of lipopolysaccharides, tumor necrosis factor-alpha, or interferons. Invest New Drugs 31, 823–832 (2013).
Park, S. et al. Role of the PI3K/AKT and mTOR signaling pathways in acute myeloid leukemia. Haematologica 95, 819–828 (2010).
Sandhofer, N. et al. Dual PI3K/mTOR inhibition shows antileukemic activity in MLL-rearranged acute myeloid leukemia. Leukemia 29, 828–838 (2015).
Graab, U., Hahn, H. & Fulda, S. Identification of a novel synthetic lethality of combined inhibition of hedgehog and PI3K signaling in rhabdomyosarcoma. Oncotarget 6, 8722–8735 (2015).
Agarwal, N. K. et al. Transcriptional regulation of serine/threonine protein kinase (AKT) genes by glioma-associated oncogene homolog 1. J. Biol. Chem. 288, 15390–15401 (2013).
Geng, L. et al. GLI1 inhibitor GANT61 exhibits antitumor efficacy in T-cell lymphoma cells through down-regulation of p-STAT3 and SOCS3. Oncotarget (2016).
Trapnell, C. et al. Transcript assembly and quantification by RNA-Seq reveals unannotated transcripts and isoform switching during cell differentiation. Nat. Biotechnol. 28, 511–515 (2010).
Trapnell, C. et al. Differential gene and transcript expression analysis of RNA-seq experiments with TopHat and Cufflinks. Nat Protoc 7, 562–578 (2012).
Acknowledgements
This study was supported by National Natural Science Foundation of China (Grant No. 81100328), the Doctoral Fund of Ministry of Education of China (Grant No. 20110162120010), and the Excellent Doctoral Dissertation of Hunan Province to H. Z. We are also very grateful to Dr. Lei Tan for a critical reading of the manuscript.
Author information
Authors and Affiliations
Contributions
H.Z., F.C., X.C., S.C. and W.L. designed the project; H.L., Q.Z., P.F. and J.Z. performed experiments; T.Z. performed the bioinformatics analysis; H.Z., S.C. and M.G. analysed data; H.Z., S.C., W.L. and H.L. wrote the manuscript; C.R. performed the additional experiments; and H.Z. approved the final version.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Liang, H., Zheng, QL., Fang, P. et al. Targeting the PI3K/AKT pathway via GLI1 inhibition enhanced the drug sensitivity of acute myeloid leukemia cells. Sci Rep 7, 40361 (2017). https://doi.org/10.1038/srep40361
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep40361
This article is cited by
-
High GLI-1 Expression is a Reliable Indicator of Bad Prognosis in Newly Diagnosed Acute Leukemia Patients
Indian Journal of Hematology and Blood Transfusion (2023)
-
GANT61/BI-847325 combination: a new hope in lung cancer treatment
Medical Oncology (2022)
-
PRICKLE1, a Wnt/PCP signaling component, is overexpressed and associated with inferior prognosis in acute myeloid leukemia
Journal of Translational Medicine (2021)
-
GLI1 reduces drug sensitivity by regulating cell cycle through PI3K/AKT/GSK3/CDK pathway in acute myeloid leukemia
Cell Death & Disease (2021)
-
Identifying subpathway signatures for individualized anticancer drug response by integrating multi-omics data
Journal of Translational Medicine (2019)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.