Abstract
Although recent studies have shed insights on some of the potential causes of male infertility, new underlining molecular mechanisms still remain to be elucidated. Makorin-2 (Mkrn2) is an evolutionarily conserved gene whose biological functions are not fully known. We developed an Mrkn2 knockout mouse model to study the role of this gene, and found that deletion of Mkrn2 in mice led to male infertility. Mkrn2 knockout mice produced abnormal sperms characterized by low number, poor motility, and aberrant morphology. Disruption of Mkrn2 also caused failure of sperm release (spermiation failure) and misarrangement of ectoplasmic specialization (ES) in testes, thus impairing spermiogenesis and spermiation. To understand the molecular mechanism, we found that expression of Odf2, a vital protein in spermatogenesis, was significantly decreased. In addition, we found that expression levels of Odf2 were decreased in Mkrn2 knockout mice. We also found that MKRN2 was prominently expressed in the sperm of normal men, but was significantly reduced in infertile men. This result indicates that our finding is clinically relevant. The results of our study provided insights into a new mechanism of male infertility caused by the MKRN2 downregulation.
Similar content being viewed by others
Introduction
Infertility is a severe health problem leading to tremendous social consequences. Approximately 10–15% of all couples experience fertility-related problems during their childbearing years1 and around 50% of such cases are caused by male infertility2. Sperm carries paternal genetic information delivering heredity to offspring. Spermatogenesis can be divided into three stages: mitosis of spermatogonia, meiosis of spermatocytes, and spermiogenesis3,4,5. Although many genes, including more than 20 male germ cell-specific genes, have been identified to be essential for spermatogenesis6, the underlying mechanisms of spermatogenesis remain largely unknown.
The makorin (MKRN) gene family encodes putative ribonucleoproteins with a distinctive array of zinc finger domains7. Makorin-1 (MKRN1) is the most extensively studied member of this family of proteins7,8,9. Makorin-2 (MKRN2), formerly designated as HSPC070, is a new member of the Makorin family, which was first identified in human CD34+ hematopoietic stem/progenitor cells10. MKRN2 is a zinc finger protein containing the typical C3HC4 protein-protein interaction motif (termed the RING domain) found in most E3 ubiquitin ligases11,12. It is ubiquitously expressed in various tissues and cell lines10,13, but MKRN2 function is not known yet in mammals. We previously demonstrated that forced expression of Mkrn2 in Xenopus produced impaired tadpoles with dorso-posterior deficiencies and small-head/short-tail phenotype, whereas knockdown of Mkrn2 by morpholino antisense oligonucleotides induced a double-axis phenotype during neurogenesis14; however, further studies are required to fully determine the biological function of Mkrn2 in mammals.
To investigate the function of the MKRN2 gene, we generated Mkrn2-knockout mice. Based on the results of our previous study, we expected that deletion of Mkrn2 in mice may result indeficiency in the development of neurogenesis14. Surprisingly, Mkrn2-knockout mice were viable with detectable abnormal neurogenesis, but the male mice were sterile. As mice and human share similar process of spermiogenesis and spermiation15, these infertile Mkrn2-knockout mice could serve as an in vivo model to investigate the biological function of MKRN2 in human spermiogenesis and spermiation.
Results
Expression pattern of Mkrn2 in mouse testes
Mkrn2 mRNA and protein expression levels were evaluated using qRT-PCR and immunoblotting analysis, respectively, in different tissue samples of mice. The Mkrn2 mRNA levels were low in the brain, thymus, heart, lung, liver, spleen, kidney, ovary, uterus, and seminal vesicle; but were very high in the testis with 30-fold higher than those in the brain and heart tissues (Fig. 1a). Similarly, Mkrn2 protein was ubiquitously expressed at low levels in different tissues, but preferentially expressed in the testis (Fig. 1b), indicating that Mkrn2 may play a vital role in testes. Furthermore, immunohistochemical analysis revealed that Mkrn2 protein was mainly localized in the Sertoli cells and spermatids (Fig. 1c). These data implied that Mkrn2 may play an important role in spermiogenesis and spermiation.
Expression profile of Mkrn2 in mice tissues.
(a) Mkrn2 mRNA levels in different tissues were analyzed by RT-qPCR and normalized to those in liver tissue. Data in the figure are represented as means ± SE. from four mice. (b) The Mkrn2 protein levels in mouse organs were detected by immnuoblotting. β-Tubulin was used as a loading control. The blotting density was normalized to that of the liver. (c) The location of Mkrn2 inthe testis of 4-week mice was determined using immunohistochemistry. Scale bar = 20 μm.
MKRN2 expression in infertile human sperms
MKRN2 protein levels were lower in human sperm samples from patients of oligoasthenoteratozoospermia (OAT) than in the normal samples (Fig. 2a, Supplementary Figure S1). Similarly, the mRNA levels of MKRN2 in the OAT patient sperms were significantly lower by more than two-fold than those in the normal group (Fig. 2b). To validate this finding in an independent cohort, we obtained MKRN2 expression data from sperm samples (including 8 OAT patients and 13 normal subjects) of American populations which was submitted to the database of European Bioinformatics Institute (EBI) by Platts and colleagues (E-GEOD-6872)16. By analyzing the raw data, we found that the MKRN2 mRNA levels were significantly decreased by 5-fold in the OAT group than in the corresponding normal group (Fig. 2c). These two independent cohorts demonstrated that low MKRN2 expression levels in sperm are strongly correlated with human male infertility.
Expression of MKRN2 in human sperm.
(a) MKRN2 protein expression levels from human sperm samples were subjected to immunoblotting analysis. (b) The MKRN2 mRNA levels from human sperm samples were measured by RT-qPCR. (c) MKRN2 mRNA expression levels of sperm samples from the US cohort were compared to available raw data extracted from the European Bioinformatics Institute (EBI) database. OAT, oligoasthenoteratozoospermia. * And ** significant difference at P < 0.05 and P < 0.01, respectively (two-tailed Student’s t test).
Generation of Mkrn2 knockout mice
Model animals are very useful tools to study the functions and mechanisms of target genes17. To better investigate the role of Mkrn2 gene in vivo, we generated Mkrn2 knockout mice using a Cre-LoxP system (Fig. 3a). The Mkrn2 gene in mice contains eight exons, in which the functional domains are mainly encoded by Exons 2–6. Thus, we disrupted Mkrn2 gene by deleting these exons and introducing frameshift mutations in Exons 7 and 8, thus obtaining maximum knockout effect. The mutant allele could be transmitted from both Mkrn2 heterozygous male and female mice, and homozygous mice could be obtained by interbreeding these heterozygous mice. Mkrn2 heterozygous and homozygous offspring were identified using a PCR-based genotyping assay (Fig. 3b). Immnuoblotting analysis using testis extracts verified the absence of Mkrn2 protein in Mkrn2 knockout mice (Fig. 3c). Amino acid sequence alignment showed that the MKRN2 protein in mice and human shared 88% identity (Supplementary Figure S2), suggesting that Mkrn2 knockout mice may be useful to explore the biological function of MKRN2 in human.
Generation of Mkrn2 knockout mice.
(a) Strategy for generating Mkrn2 knockout mice. Mkrn2-floxed mice whose Exons (numbered black boxes) 2–6 of the Mkrn2 gene were flanked by loxP sites (arrow) were crossed with EIIa-Cre transgenic mice to generate Mkrn2 knockout mice. E, exon; f, Floxed; +, wild-type; −, mutant. (b) Mkrn2 gene disruption was confirmed by PCR genotyping. Tail genomic DNA was amplified with specific primers for the wild-type (694 bp) and mutant (570 bp) Mkrn2 alleles. (c) Immunoblotting analysis showing the absence of Mkrn2 in the protein extracts of Mkrn2 knockout testes. β-Tubulin expression was used as an internal control to indicate equal amount of loading proteins. +/+, wild-type; +/−, heterozygous; −/−, homozygous (knockout).
Characteristics of Mkrn2 knockout mice
Both male and female Mkrn2 knockout mice were viable, and had no gross abnormalities except that their weights were lighter than wild-type counterparts (Supplementary Figure S3). Mkrn2 knockout male mice could mate with female mice, evidenced by the existing of vaginal plugs after mating. During the four-month duration of the mating test, the average litter size of wild-type male and female mice and Mkrn2 heterozygous male and female mice were 8.6 and 8.9 pups, respectively. However, no pups were born between Mkrn2 knockout male mice and female mice (including wild-type, heterozygous, and knockout), indicating that Mkrn2 knockout male mice were completely sterile (Table 1). Note that female Mkrn2 knockout mice were fertile, but displayed reduced fecundity with an average litter size of 5.9 pups. We then determined why Mkrn2 deletion leads to male infertility. First, the lower sperm-producing ability of male Mkrn2 knockout mice was confirmed by examining their cauda epididymis. Although a few of Mkrn2 knockout mice produced no sperm, most of them produced sperms, but with abnormal heads and tails (Fig. 4a).The abnormality rates in the sperm heads and tails of Mkrn2 knockout sperm were 13.2% and 38.9%, respectively, which were remarkably higher than the corresponding rates of 2.3% and 4.1% in wild-type sperms (Fig. 4b). Computer-assisted sperm analysis (CASA) showed that sperm amount was significantly reduced (Fig. 4c), and that approximately 70% of sperms lost motile ability (Fig. 4d) in the Mkrn2 knockout mice. Although the remaining 30% of the sperms in the Mkrn2 knockout group were motile, their mean, linear, and curvilinear velocities were significantly lower than those sperms from the wild-type mice (Fig. 4e). The observation of high rate of abnormality and low motile ability of Mkrn2 knockout sperms is very similar to those in the sperm samples obtained from OAT patients (Supplementary video 1 and 2). Thus, male Mkrn2 knockout mice produced abnormal sperms with a low count, reduced motility, and deformed morphology, which are similar to the most common type of male infertility in human18,19.
Mkrn2 knockout mouse sperm structure and characteristics.
(a) Sperm obtained from the cauda epididymis were stained by hematoxylin and eosin (H&E). Sperm from Mkrn2 knockout mice were deformed: the sperm tails bent forward in the midpiece and the heads were round and irregular (arrow). Scale bar = 50 μm. (b) The proportions of abnormal sperm were calculated from five randomly selected microscopic fields in a double-blinded manner. Data are represented as the means ± SE. of five random microscopic fields. The sperm count (c),motility (d), and velocity (e) were measured by computer-assisted sperm analysis (CASA) from six different mice of corresponding phenotypes. Data are represented as the means ± SE. of six mice. Error bars represent SE. *P < 0.05, **P < 0.01 (two-tailed Student’s t test).
Failure of spermiation in the testes of Mkrn2 knockout mice
The internal organs of the mice were weighed and normalized to their body weight. The relative organ weights were similar between Mkrn2 knockout and wild-type mice in most of organs including brain, thymus, heart, lung, liver, spleen, kidney, and stomach (Supplementary Table S1); while the relative weights and volumes of testis were significantly lower in Mkrn2 knockout mice compared to those of the wild-type counterparts (Fig. 5a,b). In the testes of Mkrn2 knockout mice, all 12 stages of spermatogenesis were present (Supplementary Figure S4). In Stage VIII seminiferous tubules of Mkrn2 knockout mice, all cell types can be observed, but the number of round spermatids was significantly decreased (Supplementary Figure S5a,b). And elongated spermatids (EI) were lining in the center of the tubules prior to spermiation, similar to that observed in the testis of wild-type mice (Supplementary Figure S5a). However, a distinguishable defect was found in Mkrn2 knockout testes at Stage X (Fig. 5c). High-power magnification fields showed that Mkrn2 knockout seminiferous tubules retained elongated spermatids (termed as spermiation failure) among germ cells, which should be released at this stage like those in the Stage X seminiferous tubules of the wild-type mice. These data indicated that Mkrn2 is important in the regulation of spermiation.
Analysis of Mkrn2 knockout mouse testes.
(a) Macroscopic appearance of testes. Scale bar = 2 mm. (b) Testis weights. The net testis weight was normalized to body weight. Data arerepresented as the means ± SE. From six testes for each phenotype. Error bars represent SE. ** P < 0.01 (two-tailed Student’s t test). (c) Hematoxylin& eosin (H&E) staining sections of Stage X testicular tubules. Arrows indicate the spermiation failure spermatids in Mkrn2 knockout testes (right); these sperm should have been released at Stage X, as observed in the wild-type testes (left). Scale bar: Upper panel, 100 μm; Bottom panel, 20 μm.
Deletion of Mkrn2 damages arrangement of actin filaments in the ectoplasmic specialization
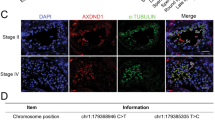
The ectoplasmic specialization (ES) is a specialized adhesion junction found in Sertoli cells at sites of attachment to elongated spermatids or neighboring Sertoli cells in the testes20. Spermiation failure can be indicative of disruption of ES21. We examined the ultrastructure of the testes using transmission electron microscopy (TEM). In normal testes, the ES synchronously stretches along with the acrosome, and is characterized by the presence of actin filament bundles sandwiched between endoplasmic reticulum (ER), and the two apposite plasma membranes of elongating spermid and Sertoli cells (Fig. 6a, left panel). In the Mkrn2 knockout testes, however, the ES arrangement was disrupted, as evidenced by desynchronization with the acrosome (Fig. 6a, left and middle panels). The ES broke across off the boundary of the acrosome, and extended further, preventing proper elongation of round spermatids by Sertoli cells in Mkrn2 knockout testes. We next examined the expression levels of the ES marker Espin. The Espin protein and mRNA levels in Mkrn2 knockout testes were decreased to one-third of the levels detected in the wild-type group (Fig. 6b,c). Immunohistochemical analysis revealed that Espin was expressed in the region between the ES and the heads of elongating/elongated spermatids in the wild-type group, but its expression was barely detected in Mkrn2 knockout testis (Fig. 6d). These data indicate that Mkrn2 regulates the accurate arrangement of the ES and Espin expression.
Analysis of Mkrn2 knockout mouse ectoplasmic specialization (ES) structure.
(a) TEM analysis of ES structure. Arrows indicate the boundary of the acrosome, and arrowheads indicate the improper arrangement of ES. Nu, nucleus; Ac, acrosome; ER, endoplasmic reticulum. Data are represented as means ± SE. From six different testis tissues for each phenotype. Error bars represent SE. **P < 0.01 (two-tailed Student’s t test). Scale bar = 1 μm. (b) Espin expression levels in the testes were analyzed by immunoblotting. β-Tubulin was used as the internal control. (c) The Espin mRNA levels in the testes were analyzed by RT-qPCR and normalized to that of β-Tubulin. Data are represented as means ± SE. From six different testis tissues for each phenotype. Error bars represent SE. **P < 0.01 (two-tailed Student’s t test). (d) Immunohistochemical staining of Espin in the testes shows co-localization of Espin at the apical ES and in the heads of elongated spermatids in wild-type testes (left), but no obvious staining can be observed in the tubules of the Mkrn2 knockout testes. Scale bar: Upper panel, 50 μm; Bottom panel, 20 μm.
Disruption of Mkrn2 results in sperm abnormalities
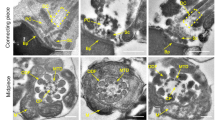
To further define the nature of the abnormalities in Mkrn2 knockout sperms, we compared the ultrastructure of sperm from the Mkrn2 knockout and wild-type groups using TEM. Results revealed that spermatozoa were normal with well-shaped heads and tails in the wild-type mice (Fig. 7a,i). However, sperms from the Mkrn2 knockout mice showed deformed heads, disorganized axonemal structure, and disorganized flagellar structure (Fig. 7a, ii–iv). The shapes of the sperm heads were aberrant, resulting in abnormal or missing acrosomes (Fig. 7a, ii, asterisk). Normal sperm tails contain a highly ordered structure termed the “9 + 2” axoneme22. The “9 + 2” axoneme arrangement in the tail flagellae of Mkrn2-deficient sperm exhibited two types of abnormalities (Fig. 7a, iii-iv, arrows): First, complete loss of the axoneme doublets in one side of the fibrous sheath; and second, disordered assembly of the “9+2” arrangement. These data demonstrated that Mkrn2 is required for the normal sperm development.
Analysis of Mkrn2 knockout mouse sperm structures and Odf2 expression.
(a) TEM analysis of epididymal sperm. i, Note the normal head and axoneme with typical “9 + 2” microtubule structure (nine pairs of peripheral and two central microtubules) in wild-type mice. ii–iv, Abnormalities in Mkrn2 knockout mouse sperm were evaluated by the appearance of deformed heads (ii, asterisk), deformed “9 + 2” structures with missing and/or misarranged microtubules (iii-iv, arrows) and lack of Odf (iv, arrowhead). Scale bar = 1 μm. (b) The Odf2 protein levels in wild-type and Mkrn2 knockout mouse sperm and testes, respectively. β-Tubulin was used as the loading control. (c) The Odf2 mRNA expression levels in the testes were determined by RT-qPCR and normalized to that of β-Tubulin. Data are represented as the means ± SE. From six different testes tissue samples for each phenotype. Error bars represent SE. *P < 0.05 (two-tailed Student’s t test).
Next, we investigated the molecular mechanism of Mkrn2 deficiency leading to male infertility. Interestingly, we found that the outer dense fiber (Odf), which is an important component of flagellae (Fig. 7a, iv, arrowheads), was either absent or improperly arranged in the Mkrn2 knockout epididymal sperms. This finding is consistent with the reduced expression of Odf2 protein, which is important for the regulation of sperm morphology (Fig. 7b). In addition, Odf2 mRNA and protein levels were significantly lower in Mkrn2 knockout sperms and testes than those of the wild-type (Fig. 7b,c). This result suggest that Mkrn2 is required for both Odf2 protein and mRNA expression.
Discussion
Mkrn2 is a new member of the highly evolutionarily conserved makorin family, and it maybe originally created by gene duplication of MKRN1 approximately 450 million years ago13. MKRN1 plays multiple functions such as modulating gene transcription, controlling protein stabilization, and regulating tumorigenesis23,24,25. However, the biological function of Mkrn2 in mammals still remains unknown. We previously found that Xenopus mkrn2 inhibited neurogenesis during early embryonic development14. To further explore the in vivo biological function of Mkrn2, we generated a strain of Mkrn2 knockout mice by using EIIa-Cre method. EIIa-Cre is widely expressed and highly efficient in gene knockout because it is expressed as early as the zygote stage26,27. Since the biological function of Mkrn2 is largely unknown, we firstly employed EIIa-Cre method to efficiently delete Mkrn2 in the whole body of mice, and to investigate the phenotype caused by Mkrn2 knockout. According to our previous study on a Xenopus model, we anticipated that disruption of Mkrn2 would result in prenatal death or deficiency in neurogenesis in mice. Surprisingly, Mkrn2 knockout mice were viable with no obvious phenotype associated with neurodeficiency. After fecundity tests, male Mkrn2 knockout mice were found to be sterile, and no pups were born during the 4-month period of mating with female mice. This finding revealed potential role of Mkrn2 in fertility of male mice. Further analysis indicated that Mkrn2 knockout mice either did not have sperm, or produced sperm with a low count, poor motility, and/or abnormal shapes. This condition is termed oligoasthenoteratozoospermia (OAT) in human, which is the most common cause of infertility in human. Mice are commonly used to study human diseases because of the genetic similarities between human and mice15,28,29. Nevertheless, the results from the animal model studies need to be confirmed in human. In this study, we showed that human MKRN2 protein and mRNA levels in the infertile OAT sperm were lower than those in the fertile sperm from a human cohort. This finding was validated by the results of the second cohort of sperm samples obtained from the EBI, in which the MKRN2 mRNA levels were downregulated in OAT sperm compared to their normospermic counterparts in the same cohort. These two independent cohorts provide direct evidence indicating that MKRN2 is significantly correlated with infertility in men. Together, the results obtained from both Mkrn2 knockout mice and human cohorts suggest that MKRN2 is important for regulating fertility and that Mkrn2 knockout mice may serve as a useful animal model for further studies.
To understand why disruption of Mkrn2 impairs fertility, we examined the distribution of Mkrn2 in mouse organs. While Mkrn2 was expressed at low levels in all the organs examined, it was preferentially overexpressed in the testis with up to 30-fold higher mRNA levels than those in other organ tissues. Furthermore, Mkrn2 was expressed in Sertoli cells and spermatids. Based on these results, we speculated that Mkrn2 may play an important role in testis development and in the process of spermatogenesis. As expectedly, the sizes and weights of the testes in Mkrn2 knockout mice were lower than those in normal mouse testes. TEM analysis revealed that impaired ES structure in Mkrn2 knockout mice20,30,31. ES is mainly characterized by the presence of a unique junction plaque containing parallel actin bundles sandwiched between the plasma membrane of Sertoli cells and affiliated endoplasmic reticulum32,33. ES is considered important for orienting the positions and shapes of the spermatid head and for regulating spermiation34,35, thus playing a vital role in spermiogenesis and spermiation. Histological examination revealed abnormal spermiogenesis and spermiation in the Stage X seminiferous tubules of the knockout mice, observed by retention of elongated spermatids and sloughing in the different compartments of germ cells. This is a very interesting phenomenon termed spermiation failure, which can be indicative of changes in the components of the ES21,36. Ultrastructure analyses revealed that the ES in the knockout mouse testes was desynchronized with the acrosome and stretched beyond the boundary of the acrosome. Immunoblot analysis showed that Espin was rarely detected in Mkrn2 knockout mouse testis, indicating that the ES was severely impaired in these mice. As a specialized structure formed by Sertoli cells, ES plays a vital role in spermiogenesis and spermiation. Our results indicated that deletion of Mkrn2 in the testes, especially in Sertoli cells, impaired ES functions, thus leading to sperm abnormalities.
Except for some cases where the Mkrn2 knockout male mice produced no sperm, most knockout mice were capable of producing lower numbers of sperm. The low sperm count maybe due to the reduced number of round spermatids in Stage VIII and/or the spermiation failure in stage X seminiferous tubules. Furthermore, deletion of the Mkrn2 gene led to severe impairment of sperm motility, which strongly indicated abnormality in sperm tails. The same phenomenon was observed in the sperm of human patients with OAT. Sperm from the Mkrn2 knockout group were morphologically abnormal, with deformed heads and tails bent toward the head at the principle piece. Ultrastructure analyses of cauda epididymal sperm revealed a drastically deformed nucleus and improperly arranged sperm flagellae in Mkrn2 knockout mice. The “9 + 2” structure was partially lost or disordered. These results implied that deletion of Mkrn2 in the testes, especially in germ cells, would impair some essential components during sperm flagellar assembly. After further exploration, we found that Odf was not assembled correctly. Odf2, an important member of Odf family, has been reported to be associated with flagellar assembly37,38. The Odf2 expression levels were greatly reduced both in the sperm and testes of Mkrn2 knockout mice, indicating that Mkrn2 may control the expression of Odf2 directly or indirectly, consequently modulating sperm flagellar assembly. It was reported that Odf2 KO results in preimplantation lethality, suggesting that Odf2 may be an important downstream protein of MKRN2 for spermiogenesis and spermiation39.
This study uses an Mkrn2 knockout mouse model and two independent cohorts of human sperm samples to demonstrate the important role of Mkrn2 in male fertility. Our results demonstrate that Mkrn2 is essential for spermiogenesis and spermiation. We found that deletion of Mkrn2 in somatic Sertoli cells results in disruption of ES, leading to abnormalities in sperm heads and spermiation failure. This deletion also suppresses Odf2 expression in germ cells, disrupting the flagellar assembly of sperm tails. Furthermore, the Mkrn2 expression levels were significantly downregulated in the infertile male subjects in our study. Mkrn2 knockout mice may serve as a model for investigating the involvement of Mkrn2 in spermiogenesis and spermiation in the future.
Material and Methods
Sperm sample collection and analysis
Human sperm samples have been collected for several years by the Center of Clinical Reproductive Medicine, the First Affiliated Hospital of Nanjing Medical University. Informed consents were obtained from all subjects participating in the study. Ejaculates were evaluated according to World Health Organization criteria40. These sperm samples and other related samples have been kept in the tissue bank of the First Affiliated Hospital of Nanjing Medical University. These samples have been prepared for cases in the First Affiliated Hospital of Nanjing Medical University biorepository, and clinical annotation is available through a database using caBIG. Cases will be classified and selected based on diagnosis using the CoPath Anatomic Pathology system as well as caBIG. No information regulated by The Health Insurance Portability and Accountability Act was included in the study, which qualifies for the status of NIH Exemption # 4. The sperm samples based on the database containing 33 infertile men diagnosed as having oligoasthenoteratozoospermia (OAT) and 33 fertile men were used for this study, and the results are showed in Supplementary Figure S1.
Ethics statement
All animal experiments were approved by the Committee of Laboratory Animal Experimentation of Nanjing Medical University. All methods were performed in accordance with the relevant guidelines and regulations. The mice used in this study were housed in a controlled specific pathogen-free (SPF) environment and cared according to the approved protocol.
Generation of Mkrn2 knockout mice
To generate Mkrn2 floxed mice, a targeting vector containing Mkrn2 exons 2–6 flanked by Loxp sites was linearized by digestion with NotI was introduced into embryonic stem cells derived from mice with a 129P2/OlaHsd background by electroporation. Southern blotting analysis was used to confirm the resulting cells harboring floxed alleles of Mkrn2. The targeted embryonic stem cell clones were microinjected into C57BL/6 J blastocysts of female mice, which gave birth to chimeric mice. The offspring were subsequently crossed with C57BL/6 J mice to generate F1 Mkrn2-floxed offspring.
To generate Mkrn2 knockout mice, Mkrn2-floxed mice that had been backcrossed with C57BL/6 J for more than five generations were crossed with transgenic EIIa-cre mice with a C57BL/6 J background (Jackson Laboratory) to obtain mosaic mice with the Mkrn2+/f/−·EIIa-cre genotype. The resulting mice were crossed with C57BL/6 J to obtain Mkrn2 heterozygotes. Mkrn2 knockout mice were generated by sibmating of heterozygotes. Genomic DNA isolated from the tails was genotyped with oligonucleotides listed in Supplementary Table S2, yielding 694-bp (wild-type) and 570-bp (mutant) products.
Morphological and immunohistochemical analysis
The testes and epididymis tissues were dissected, fixed in Bouin’s fixatives overnight, and embedded in paraffin. Sections were stained by hematoxylin and eosin (H&E) for histological examination or immunohistochemically using antibodies against MKRN2 (Novus Biologicals) and Espin (BD Biosciences). The epididymis sections were dissected, incubated in PBS, and epididymal sperm morphology was analyzed by observing the sections on a slide with methanol fixation and H&E staining.
Sperm analysis
Sperm motility and count were measured using a CASA system as described previously41. Mature sperm were isolated from the cauda epididymis dissected from sexually mature mice. The tissue was incised at four sites and placed in 0.5 mL of PBS for 15 min in a 37 °C incubator. Debris was removed, and 20 μL aliquots of sperm were placed in an 80-μm-deep chamber for the assessment of sperm motility, and the sperm count was obtained by CASA using an IVOS Sperm Analyzer (Hamilton Thorne Biosciences).
Ultrastructure analysis
For electron microscopy, testicular and cauda epididymal sperm from adult mice were fixed in 5% (v/v) and 2.5% (v/v) glutaraldehyde at 4 °C, respectively. The specimens were embedded according to standard procedures, sectioned, and examined with a JEM-1010 transmission electron microscope (JEOL).
RNA analysis
Total RNAs were prepared using TRIzol reagent (Invitrogen) according to the manufacturer’s instructions. First-strand cDNAs were synthesized and subjected to real-time RT-PCR analysis (Vazyme). The relative amounts of target genes were calculated by the comparative threshold cycle (Ct) method. β-Tubulin mRNA levels were used as the internal control. The oligonucleotide primer sequences used here are listed in Supplemental Table 2.
Immunoblotting
Tissues were homogenized in ice-cold RIPA buffer supplemented with protease inhibitor cocktail (Sigma). The cell suspensions were centrifuged for 15 minutes at 15,000 rpm at 4 °C. The sperm samples were collected and homogenized in lysis buffer containing 7 M urea (Thermal Scientific), 2 M thiourea (Sigma-Aldrich), 4% (w/v) CHAPS (Sigma-Aldrich), 65 mM dithiothreitol (SunShine Biotechnology), and 1% (v/v) Protease Inhibitor Cocktail for sperm protein analysis, as described in a previous study42. Briefly, homogenates were subjected to four repetitions of ultrasound every 15 minutes, and then centrifuged for 1 h at 15,000 rpm at 4 °C. The extracted proteins were subjected to immnuoblot analysis for detecting MKRN2 (Novus Biologicals), Espin or Odf2 (BD Biosciences). β-Tubulin (Cell Signaling Technology) was used as the loading control.
Statistical analysis
Data were presented as the means ± SE. of at least three independent experiments unless otherwise indicated. The Student’s unpaired t test was used for comparison of the wild-type and knockout mice. Values were considered significantly different at P < 0.05.
Additional Information
How to cite this article: Qian, X. et al. Deficiency of Mkrn2 causes abnormal spermiogenesis and spermiation, and impairs male fertility. Sci. Rep. 6, 39318; doi: 10.1038/srep39318 (2016).
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
De Kretser, D. M. & Baker, H. W. Infertility in men: recent advances and continuing controversies. The Journal of clinical endocrinology and metabolism 84, 3443–3450, doi: 10.1210/jcem.84.10.6101 (1999).
Hirsh, A. Male subfertility. Bmj 327, 669–672, doi: 10.1136/bmj.327.7416.669 (2003).
Eddy, E. M. Male germ cell gene expression. Recent progress in hormone research 57, 103–128 (2002).
Zhang, Z. et al. MEIG1 is essential for spermiogenesis in mice. Proceedings of the National Academy of Sciences of the United States of America 106, 17055–17060, doi: 10.1073/pnas.0906414106 (2009).
Alves, M. G. et al. Molecular mechanisms beyond glucose transport in diabetes-related male infertility. Biochimica et biophysica acta 1832, 626–635, doi: 10.1016/j.bbadis.2013.01.011 (2013).
Jamsai, D. & O’Bryan, M. K. Mouse models in male fertility research. Asian journal of andrology 13, 139–151, doi: 10.1038/aja.2010.101 (2011).
Omwancha, J. et al. Makorin RING finger protein 1 (MKRN1) has negative and positive effects on RNA polymerase II-dependent transcription. Endocrine 29, 363–373, doi: 10.1385/ENDO:29:2:363 (2006).
Kim, J. H. et al. Ubiquitin ligase MKRN1 modulates telomere length homeostasis through a proteolysis of hTERT. Genes & development 19, 776–781, doi: 10.1101/gad.1289405 (2005).
Ko, A. et al. Acceleration of gastric tumorigenesis through MKRN1-mediated posttranslational regulation of p14ARF. Journal of the National Cancer Institute 104, 1660–1672, doi: 10.1093/jnci/djs424 (2012).
Zhang, Q. H. et al. Cloning and functional analysis of cDNAs with open reading frames for 300 previously undefined genes expressed in CD34+ hematopoietic stem/progenitor cells. Genome research 10, 1546–1560 (2000).
Deshaies, R. J. & Joazeiro, C. A. RING domain E3 ubiquitin ligases. Annual review of biochemistry 78, 399–434, doi: 10.1146/annurev.biochem.78.101807.093809 (2009).
Riley, B. E. et al. Structure and function of Parkin E3 ubiquitin ligase reveals aspects of RING and HECT ligases. Nature communications 4, 1982, doi: 10.1038/ncomms2982 (2013).
Gray, T. A. et al. Phylogenetic conservation of the makorin-2 gene, encoding a multiple zinc-finger protein, antisense to the RAF1 proto-oncogene. Genomics 77, 119-126, doi: 10.1006/geno.2001.6627 (2001).
Yang, P. H. et al. Makorin-2 is a neurogenesis inhibitor downstream of phosphatidylinositol 3-kinase/Akt (PI3K/Akt) signal. The Journal of biological chemistry 283, 8486–8495, doi: 10.1074/jbc.M704768200 (2008).
Church, D. M. et al. Lineage-specific biology revealed by a finished genome assembly of the mouse. PLoS biology 7, e1000112, doi: 10.1371/journal.pbio.1000112 (2009).
Platts, A. E. et al. Success and failure in human spermatogenesis as revealed by teratozoospermic RNAs. Human molecular genetics 16, 763–773, doi: 10.1093/hmg/ddm012 (2007).
Baddack, U. et al. A chronic model of arthritis supported by a strain-specific periarticular lymph node in BALB/c mice. Nature communications 4, 1644, doi: 10.1038/ncomms2625 (2013).
Wei, T. C., Huang, W. J., Lin, A. T. & Chen, K. K. The role of hormones on semen parameters in patients with idiopathic or varicocele-related oligoasthenoteratozoospermia (OAT) syndrome. Journal of the Chinese Medical Association: JCMA 76, 624–628, doi: 10.1016/j.jcma.2013.07.005 (2013).
Jungwirth, A. et al. European Association of Urology guidelines on Male Infertility: the 2012 update. European urology 62, 324–332, doi: 10.1016/j.eururo.2012.04.048 (2012).
Parreira, G. G., Melo, R. C. & Russell, L. D. Relationship of sertoli-sertoli tight junctions to ectoplasmic specialization in conventional and en face views. Biology of reproduction 67, 1232–1241 (2002).
Borg, C. L., Wolski, K. M., Gibbs, G. M. & O’Bryan, M. K. Phenotyping male infertility in the mouse: how to get the most out of a ‘non-performer’. Human reproduction update 16, 205–224, doi: 10.1093/humupd/dmp032 (2010).
Porter, M. E. & Sale, W. S. The 9 + 2 axoneme anchors multiple inner arm dyneins and a network of kinases and phosphatases that control motility. The Journal of cell biology 151, F37–42 (2000).
Lee, E. W. et al. Differential regulation of p53 and p21 by MKRN1 E3 ligase controls cell cycle arrest and apoptosis. The EMBO journal 28, 2100–2113, doi: 10.1038/emboj.2009.164 (2009).
Miroci, H. et al. Makorin ring zinc finger protein 1 (MKRN1), a novel poly(A)-binding protein-interacting protein, stimulates translation in nerve cells. The Journal of biological chemistry 287, 1322–1334, doi: 10.1074/jbc.M111.315291 (2012).
Shimada, H. et al. Identification of Makorin 1 as a novel SEREX antigen of esophageal squamous cell carcinoma. BMC cancer 9, 232, doi: 10.1186/1471-2407-9-232 (2009).
Holzenberger, M. et al. Cre-mediated germline mosaicism: a method allowing rapid generation of several alleles of a target gene. Nucleic acids research 28, E92 (2000).
Lakso, M. et al. Efficient in vivo manipulation of mouse genomic sequences at the zygote stage. Proceedings of the National Academy of Sciences of the United States of America 93, 5860–5865 (1996).
Cox, R. D. & Brown, S. D. Rodent models of genetic disease. Current opinion in genetics & development 13, 278–283 (2003).
Kamberov, Y. G. et al. Modeling recent human evolution in mice by expression of a selected EDAR variant. Cell 152, 691–702, doi: 10.1016/j.cell.2013.01.016 (2013).
O’Donnell, L., Nicholls, P. K., O’Bryan, M. K., McLachlan, R. I. & Stanton, P. G. Spermiation: The process of sperm release. Spermatogenesis 1, 14–35, doi: 10.4161/spmg.1.1.14525 (2011).
Li, M. W., Mruk, D. D., Lee, W. M. & Cheng, C. Y. Connexin 43 is critical to maintain the homeostasis of the blood-testis barrier via its effects on tight junction reassembly. Proceedings of the National Academy of Sciences of the United States of America 107, 17998–18003, doi: 10.1073/pnas.1007047107 (2010).
Cheng, C. Y. & Mruk, D. D. A local autocrine axis in the testes that regulates spermatogenesis. Nature reviews. Endocrinology 6, 380–395, doi: 10.1038/nrendo.2010.71 (2010).
Bartles, J. R., Wierda, A. & Zheng, L. Identification and characterization of espin, an actin-binding protein localized to the F-actin-rich junctional plaques of Sertoli cell ectoplasmic specializations. Journal of cell science 109 (Pt 6), 1229–1239 (1996).
Yan, H. H., Mruk, D. D., Lee, W. M. & Cheng, C. Y. Ectoplasmic specialization: a friend or a foe of spermatogenesis? BioEssays: news and reviews in molecular, cellular and developmental biology 29, 36–48, doi: 10.1002/bies.20513 (2007).
Mruk, D. D. & Cheng, C. Y. Cell-cell interactions at the ectoplasmic specialization in the testis. Trends in endocrinology and metabolism: TEM 15, 439–447, doi: 10.1016/j.tem.2004.09.009 (2004).
Lee, N. P. & Cheng, C. Y. Ectoplasmic specialization, a testis-specific cell-cell actin-based adherens junction type: is this a potential target for male contraceptive development? Human reproduction update 10, 349–369, doi: 10.1093/humupd/dmh026 (2004).
Tarnasky, H. et al. Gene trap mutation of murine outer dense fiber protein-2 gene can result in sperm tail abnormalities in mice with high percentage chimaerism. BMC developmental biology 10, 67, doi: 10.1186/1471–213X-10–67 (2010).
Mariappa, D. et al. Inhibition of tyrosine phosphorylation of sperm flagellar proteins, outer dense fiber protein-2 and tektin-2, is associated with impaired motility during capacitation of hamster spermatozoa. Molecular reproduction and development 77, 182–193, doi: 10.1002/mrd.21131 (2010).
Salmon, N. A., Reijo Pera, R. A. & Xu, E. Y. A gene trap knockout of the abundant sperm tail protein, outer dense fiber 2, results in preimplantation lethality. Genesis 44, 515–522, doi: 10.1002/dvg.20241 (2006).
Menkveld, R. Clinical significance of the low normal sperm morphology value as proposed in the fifth edition of the WHO Laboratory Manual for the Examination and Processing of Human Semen. Asian journal of andrology 12, 47–58, doi: 10.1038/aja.2009.14 (2010).
Yildiz, Y. et al. Mutation of beta-glucosidase 2 causes glycolipid storage disease and impaired male fertility. The Journal of clinical investigation 116, 2985–2994, doi: 10.1172/JCI29224 (2006).
Guo, X. et al. Proteomic analysis of proteins involved in spermiogenesis in mouse. Journal of proteome research 9, 1246–1256, doi: 10.1021/pr900735k (2010).
Acknowledgements
This work was supported in part by grants from the National Key Basic Research Program of China (2011CB944304, 2011CB504003), and by the Chinese Natural Science Funds (81270736, 81222006, 81302182, 81472944, 81320108019), and by the National Institutes of Health grant R01ES020868 and R01CA193511. We thank Model Animal Research Center of Nanjing University for generation of the Mkrn2 floxed mice.
Author information
Authors and Affiliations
Contributions
X.Q. L.W. and B.Z. designed and performed experiments, analyzed data and wrote the manuscript; L.W., Z.M.S., X.G. and C.F.J. maintained mice and performed IHC and qRT-PCR assay; Y.C.Q., D.M.L., X.L., W.L., Y.Y. and J.T.Z. acquired data, reporter assay and immunoblotting analysis; H.S., M.W, M.L. and X.J.G. analyzed TEM data and did statistical analysis; J.H. and L.Z.L. prepared the manuscript. J.H.S. and B.H.J. designed and supervised the project.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Qian, X., Wang, L., Zheng, B. et al. Deficiency of Mkrn2 causes abnormal spermiogenesis and spermiation, and impairs male fertility. Sci Rep 6, 39318 (2016). https://doi.org/10.1038/srep39318
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep39318
This article is cited by
-
ANGPTL4 regulates ovarian cancer progression by activating the ERK1/2 pathway
Cancer Cell International (2024)
-
LCRMP-1 is required for spermatogenesis and stabilises spermatid F-actin organization via the PI3K-Akt pathway
Communications Biology (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.