Abstract
Our previous genome-wide miRNA microarray study revealed that miR-107 was upregulated in gastric cancer (GC). In this study we aimed to explore its biological role in the pathogenesis of GC. Integrating in silico prediction algorithms with western blotting assays revealed that miR-107 inhibition enhanced NF1 (neurofibromin 1) mRNA and protein levels, suggesting that NF1 is one of miR-107 targets in GC. Luciferase reporter assay revealed that miR-107 suppressed NF1 expression by binding to the first potential binding site within the 3′-UTR of NF1 mRNA. mRNA stable assay indicated this binding could result in NF1 mRNA instability, which might contribute to its abnormal protein expression. Functional analyses such as cell growth, transwell migration and invasion assays were used to investigate the role of interaction between miR-107 and its target on GC development and progression. Moreover, We investigated the association between the clinical phenotype and the status of miR-107 expression in 55 GC tissues, and found the high expression contributed to the tumor size and depth of invasion. The results exhibited that down regulation of miR-107 opposed cell growth, migration, and invasion, whereas NF1 repression promoted these phenotypes. Our findings provide a mechanism by which miR-107 regulates NF1 in GC, as well as highlight the importance of interaction between miR-107 and NF1 in GC development and progression.
Similar content being viewed by others
Introduction
Gastric cancer (GC) is the fourth most common cancer worldwide, with a total of 989,600 new cases and 738,000 deaths occurred in 20081. It is well accepted that gastric carcinogenesis is a multistep and multifactorial process involving genetic and epigenetic alterations in oncogenes and tumor suppressor genes2,3.
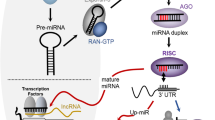
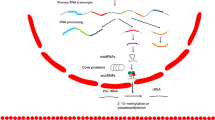
miRNAs, an important component of epigenetic mechanisms, comprise species of short noncoding RNA and post-transcriptionally modulate gene expression by negatively regulating the stability or translational efficiency of their target mRNAs4. miRNAs play a crucial role in a broad range of physiological and pathological process, and their aberrant expression has been observed in a variety of diseases, including neurodegenerative disease5, diabetes6 and tumors7. Increasing studies suggest miRNAs are promising biomarkers for cancer diagnosis, prognosis and therapeutic targets7,8.
Our previous genome-wide miRNA microarray study has identified 12 miRNAs including miR-107 significantly dysregulated in GC9. miR-107 has been reported to play a vital role in cell division, metabolism, stress response, and angiogenesis. Dysregulated of miR-107 is involved in multiple tumors development and progression10. miR-107 functions as a tumor suppressor by inducing cell cycle arrest in lung cancer and glioma via down-regulating the expression of CDK611,12. However, miR-107 serves as oncogene for promoting tumor invasion and metastasis in breast and gastric cancer through targeting DICER113,14. The role of miR-107 in tumors is contradictory and needed to be further addressed. In this study, we sought to determine the role of miR-107 underlying the pathogenesis of GC.
Methods and Materials
Cell lines and reagents
Human GC cell lines SGC7901 and MGC803 were purchased from the Shanghai Institute of Biochemistry and Cell Biology, Chinese Academy of Sciences (Shanghai, China). Cells were cultured in DMEM/10% fetal bovine serum and grown at 37 °C and 5% CO2.
Small interfering RNA
miR-107 inhibitor and negative control (designated si-107 and NC, respectively) were chemically synthesized by GenePharma Tech (Shanghai, China). The sequences of si-107 and NC were 5′-UGAUAGCCCUGUACAAUGCUGCU-3′ and 5′-CAGUAC UUUUGUGUAGUACA-3′, respectively; all the bases were 2′-OMe modified. Small interfering RNA (siRNA) specific for NF1 (sc-36036) and non-specific control siRNA (sc-37007) were purchased from Santa Cruz Biotechnology (Santa Cruz, CA, USA). In all functional analysis, NC and si-107 were used at a concentration of 50 nmol/L, while si-NF1 and its control at 10 nmol/L.
Plasmids construction, transient transfection and luciferase assay
The NF1 Wild-type reporter plasmid was constructed by cloning a 490-bp DNA fragment of NF1 3′-untranslated region (UTR), which is containing the two predicted miR-107 target sites, into the HpaI site of the pGL3-promoter vector (Promega, WI, USA; Fig. 1C, upper panel). Based on the Wild plasmid, the Mut-1, Mut-2 and Mut-both mutant constructs were made by removing the first, second and both predicted miR-107 target sites of the NF1 3′-UTR fragment, respectively.
The plasmids or in combination with siRNAs were transiently transfected into cells using Lipofectamine 2000 (Invitrogen, CA, USA) following the manufacturer’s protocol. As an internal standard, all plasmids were cotransfected with 10 ng pRL-SV40, which contained the Renilla luciferase gene. The pGL3-promoter vector without an insert was used as a negative control. After transfection at 48 h, luciferase activity in lysates was measured with a Dual-Luciferase Reporter Assay System (Promega, WI, USA). The reporter assay was performed with three biological replicates and three technical replicates.
Real-time PCR analysis
Total RNA was isolated from cell lysates according to the instructions provided by the manufacturer of TRIZOL (Invitrogen, CA, USA). Reverse transcription was performed using the TaqMan MicroRNA Reverse Transcription Kit (ABI, CA, USA). The expression level of miR-107 was assessed using the specific TaqMan MicroRNA Assay kit (ABI, CA, USA), and normalized to U6. To determine the expression levels of NF1 mRNA, the cDNA was amplified by real-time PCR with SYBR Green RT-PCR kit (Takara, Japan). The expression of GAPDH was used as an internal control. The following primers were used for amplification: 5′- CGAATGGCACCGAGTCTT AC-3′ (F) and 5′-GACCAGTTGGACGAGCCC -3′ (R) for NF1; 5′- GCACCGTCA AGGCTGAGAAC -3′ (F) and 5′- TGGTGAAGACGCCAGTGGA -3′ (R) for GAPDH. Real-time PCR was performed in triplicate on ABI 7900HT Real-Time PCR System (ABI, CA, USA). Relative expression was calculated using the comparative Ct method. The Real-time PCR assay was performed with three biological replicates and three technical replicates.
Western blotting
The total cell lysates were prepared with a detergent lysis buffer (50 mM Tris, pH 7.4; 150 mM NaCl; 1% NP-40; 0.5% sodium deoxycholate; 0.1% SDS; 1 mM PMSF; and 1% phosphatase inhibitor cocktail (P2850, Sigma-Aldrich, MO, USA). Western blots were performed as previously reported15 using antibodies of NF1 (sc-67, Santa Cruz, CA, USA); α-tubulin, p-ERK1/2, and ERK1/2 (Cat. #2125, 9101, 9102, respectively; Cell Signaling, MA, USA).
Cell growth assay
The transfected MGC803 cells were seeded in 96-well plates. Cell culture was continued for 24 h, 36 h and 48 h and subsequently incubated with MTT reagent (5 mg/ml) at 37 °C for 4 h. MTT assay was performed as described elsewhere16.
Wound healing assay
The transfected MGC803 cells (5 × 105) were cultured in 6-well plates to monolayer. The cells were then starved in serum-free medium for 12 h before a wound approximately 2 mm in width was made with a cell scraper. The wound was allowed to heal for 3 d in a fresh medium containing 1% fetal bovine serum. The wounded monolayer was photographed at the indicated day using a fluorescent microscopy (IX70, Olympus, Japan) with a 10 × objective. Wound closure was measured as a percentage of original wound width.
Transwell assay
Transwell assay was performed using 12-well Transwell chambers (Corning Costar, Cambridge, MA, USA) with a pore size of 8 μm. For Transwell migration, Cells (1 × 105) were seeded in serum-free medium in the upper chamber and incubated at 37 °C for 8 h. Afterward, the cells remained in the upper chamber were carefully removed with a cotton swab, whereas the cells having traversed to reverse face of the membrane were fixed in methanol, stained with crystal violet (0.04% in water), and counted. Transwell invasion assay was done under the same conditions as the Transwell migration assays, but in Matrigel-coated transwells (BD Biosciences, MA, USA) and incubation for 24 h.
Statistical analysis
Quantified data are presented as mean ± SEM. The difference between two independent means was assessed by t-test. All P-values are two-sided, and P < 0.05 was considered to statistically significant. Statistical analyses were carried out using SAS software (V.9.1.3; SAS Institute, Cary, NC, USA) and R software (V.2.15.0; The R Foundation for Statistical Computing).
Results
miR-107 is upregulated in GC tissues
We detected the expression of miR-107 in 55 paired of cancer and normal tissues. The expression level of miR-107 in cancer tissues was significantly increased compared with normal tissues (P = 0.0003, Fig. 1A). The same result was found in TCGA (Fig. 1B). As shown in Table 1, the aberrant miR-107 expression in GC tissues was associated with tumor sizes and depth of invasion.
NF1 is a target of miR-107
miRNA carries out its biological function via regulating the expression of its target genes through base-pairing with endogenous mRNAs. As an initial step to identify putative miR-107 targets, four commonly used algorithms (i.e., TargetScan, PicTar, Microcosm Targets v5, and miRanda) were applied to predict miR-107 target genes; and finally, there were 22 genes predicted by all four algorithms (Table 2). Among these 22 predicted target genes, NF1 (Neurofibromin 1) stood out for the presence of two evolutionarily conserved binding sites, suggesting collaborative binding and biologically effective interaction (Fig. 2A).
miR-107 targets NF1.
(A) Schematic diagram of the NF1 3′-UTR containing two putative miR-107 binding sites. Below, sequence of mature miR-107 aligned to the two binding sites, showing evolutionary conservation in the seed-pairing sequence between human and mouse. (B) Down-regulation of miR-107 by si-107 resulted in an increased NF1 expression in MGC803 cells. (C) Down-regulation of miR-107 by si-107 resulted in an increased NF1 expression in MGC803 cells. MGC803 cells pre-treated with NC or si-107 for 48 h were serum starved for 12 h, and exposed to 10% serum for increasing lengths of time (0–30 min), and thereafter the expression of NF1 was evaluated. a-tubulin was used as internal control. *P < 0.05.
NF1 is a tumor suppressor, and loss of NF1 expression has been linked to tumor development and progression17,18. To confirm that NF1 is a target of miR-107 in GC, the endogenous NF1 levels were measured in MGC803 cells at 48 h after miR-107 knockdown. The results showed that NF1 mRNA expression was significantly increased after miR-107 knockdown, compared with the negative control (Fig. 2B). Cichowski et al.19 reported that NF1 degradation could be rapidly triggered in response to growth factors and re-elevated shortly after growth factor treatment. Replicate growth factor treatment of MGC803 cells with 10% goat serum revealed that NF1 was rapidly degraded within 5 min and quickly re-elevated in the NC processing group, whereas evident degradation of NF1 was seen in 10 min in the si-107 treated group, possibly attributing to a rise in the expression of NF1 induced by miR-107 knockdown (Fig. 2C).
miR-107 downregulates NF1 expression by directly targeting its 3′-UTR
To establish a direct interaction between miR-107 and the 3′-UTR of NF1, we cloned the NF1 3′-UTR portion containing the two miR-107 target sites into a firefly luciferase reporter construct, designated as Wild-type Reporter (Fig. 3A), and used it for transient transfection into MGC803 cells. A significant reduction (87%) in the luciferase activity of the Wild-type Reporter was observed compared with the pGL3-promoter reporter (Fig. 3B). To evaluate whether the reduction of luciferase activity was associated with miR-107 targeting, the Wild-type Reporter was co-transfected with si-107 (miR-107 inhibitor) or NC (negative control) into the SGC7901 and MGC803 cells. The results demonstrated a significant increase in luciferase activity in both cell lines (1.48-fold for SGC7901 and 1.71-fold for MGC803) treated with si-107 compared with their NC-treated counterparts (Fig. 3C), indicating a direct interaction between miR-107 and the NF1 3′-UTR. As mentioned above, there are two potential miR-107 target sites within the NF1 3′-UTR. In order to identify the bona fide miR-107 target site, we mutated the first, second and both predicted target sites of the Wild-type Reporter, designated as Mut-1, Mut-2 and Mut-both reporter. Likewise, the three mutated reporters were co-transfected with si-107 or NC into MGC803 and SGC7901 cells, respectively, while the Wild-type Reporter was used as a positive control. The results revealed that in both cell lines, the luciferase activities were only increased in the cells co-transfected with the Wild and Mut-2 reporters after miR-107 knockdown compared with their NC-treated counterparts (Fig. 3D), indicating that the first predicted target site is the authentic miR-107 target site.
miR-107 negatively regulates NF1 expression by directly targeting its 3′-UTR.
(A) Partial sequences of NF1 3′-UTR containing wild or mutated putative miR-107 target sites were fused to the firefly luciferase coding sequence. Bars, predicted miR-107 seed-pairing sequences. (B) The pGL3-NF1 3′-UTR reporter (Wild) and pGL3-promoter plasmids were transfected into MGC803 cells respectively to compare their luciferase activity. (C) The Wild plasmid was co-transfected into MGC803 cells with NC or si-107. (D) The Wild and three mutated plasmids (Mut-1, Mut-2 and Mut-both) were respectively co-transfected into SGC7901 and MGC803 cells with NC or si-107. Luciferase activity was normalized to a simultaneously transfected Renilla expression plasmid. *P < 0.05, **P < 0.01 and ***P < 0.001.
Regulation by miR-107 results in NF1 mRNA degradation
NF1 3′-UTR sequence analysis revealed that there is an AU-rich element (ARE element, ATTTA) adjacent to the second predicted miR-107 target site (Fig. 4A). It was reported that miRNA could regulate the mRNA stability through binding to the ARE element in the 3′-UTR of mRNA20. In order to determine whether the increased expression of NF1 mRNA was a consequence of the enhanced mRNA stability after miR-107 knockdown, we measured the mRNA stability of NF1. As shown in Fig. 4B, the remaining NF1 mRNA expression was more in the si-107 treated group than in NC-treated group (1.08 ± 0.11 vs. 0.66 ± 0.09, P < 0.05) after ActD treatment for 2 h, implying that si-107 treatment significantly increased the stability of NF1 mRNA in contrast with the negative control (NC) and miR-107 may have an effect on NF1 mRNA decay and subsequent protein expression.
miR-107 regulates cell proliferation, migration and invasion by targeting NF1
It has reported that NF1 acts as a tumor suppressor to arrest cell growth, migration, and invasion18,21. We next examined the role of the interaction between miR-107 and NF1 on cell growth, migration, and invasion of GC cells. Apart from si-107 and its negative control, the MGC803 cells were further treated with si-NF1 (Fig. 5A, left panel) to evaluate whether the biological effect of miR-107 is through directly targeting NF1. The cell growth assay indicated that the cells treated with si-107 illustrated a moderate reduction in cell growth (25%) compared with its negative control (Fig. 5A, right panel). Furthermore, the cells with miR-107 knockdown displayed a significant reduction in cell migration using wound healing (46%, Fig. 5B) and Transwell migration (44%; Fig. 5C, panel a) assays. A strong decrease in invasive ability of the cells transfected with si-107 was also observed by Transwell invasion assay (70%; Fig. 5C, panel b). It was noteworthy that si-NF1 could reverse inhibition of cell proliferation (Fig. 4A, right panel), migration and invasion (Fig. 5, panel a and b, respectively) by miR-107 knockdown, indicating that miR-107 exerted its function by directly targeting NF1.
miR-107 knockdown inhibits cell growth, migration and invasion through NF1 upregulation.
(A) MGC803 cells were transfected with NC or si-107, or si-107 in combination with si-NF1. At 48 h post-transfection, cells were seeded in 96-well plates and their growth was evaluated by MTT assay at indicated time points (right panel). Left panel, the interference effect of si-NF1 on NF1 expression. (B) MGC803 cells pre-treated with si-107 or NC for 48 h migrated into the wounded area. Left panel shows representative images; right panel shows the quantification of migration rate. (C) Transwell migration (a) and invasion (b) assays were performed in MGC803 cells pre-treated with NC, si-107, or si-107 in combination with si-NF1 for 48 h. Means ± SEM from three independent experiments. *P < 0.05, **P < 0.01, and ***P < 0.001.
Discussion
Recent study indicates that the role of miR-107 in tumor development and progression is contradictory and differs in a context-dependent manner. miR-107 could function as tumor suppressor gene by inducing cell cycle arrest in lung cancer and glioma11,12, whereas serve as oncogene for promoting tumor invasion and metastasis in breast and gastric cancer13,14.
In GC, Li et al.14 found that miR-107 was upregulated in GC and promoted tumor invasion and metastasis by negatively regulating DICER1. Song et al.22 showed that miR-107 was capable of advancing proliferation of GC cells by targeting CDK8. However, Feng et al.23 reported an opposite role of miR-107 that it was down-regulated in GC and acted as a tumor suppressor to oppose proliferation and invasion of GC cells. In our present study, functional analyses revealed that miR-107 stimulated cell growth, migration, and invasion, in agreement with Li et al.14 and Song et al.22, indicating that miR-107 could function as onco-miRNA in GC through multiple targets, including Dicer, CDK8, and NF1. The biological processes and molecular mechanisms underlying miR-107 still remain unclear in GC, and further functional studies are warranted to address these unsolved issues.
NF1 is a GTPase which converts active Ras-GTP to its inactive form, thereby negatively regulating Ras signaling24. Loss of NF1 expression by mutation25, copy number alteration26, or miRNA regulation18 can result in constitutive activation of Ras, which can mediate signal transduction via multiple pathways, including Ras/Raf/MEK/ERK pathway, leading to various cancer phenotypes like decreased apoptosis and increased proliferation and migration27. It is biologically plausible that the observed miR-107 phenotype in GC may be attributable to ERK activation induced by decreased NF1 expression. Recently, Lenarduzzi et al.18 reported that miR-193b enhanced tumor progression via down regulation of NF1, which in turn leading to activation of ERK, resulting in proliferation, migration, invasion, and tumor formation.
miRNAs exert their function by repressing translation and/or triggering degradation of mRNA targets28. It is reported that miRNA is involved in the ARE-mediated mRNA instability20. By bioinformatics analysis, we identified an ARE element adjacent to the second predicted miR-107 target site in NF1 3′-UTR. Our results showed that NF1 mRNA stability was enhanced after miR-107 knockdown. We proposed that miR-107 was involved in the ARE-mediated mRNA instability. Further studies on the role of direct interaction between miR-107 and ARE element in the regulation of NF1 mRNA stability are warranted. There is a predicted HuR binding site adjacent to the second predicted miR-107 target site in NF1 3′-UTR (Fig. 3A). Haeussler et al.29 found that mRNA binding protein HuR could interact with ARE element in the 3′-UTR of NF1, thereby negatively regulating the expression of mRNA on the posttranscriptional level. Therefore, the role of HuR in the regulation of NF1 mRNA stability by miR-107 also merits further investigation.
Some limitations in this study should be addressed. First, the function of miR-107 was evaluated through miR-107 knockdown in a loss-of-function model. Gain-of-function studies via overexpression of miR-107 in GC cell lines are needed to verify our findings. Second, future in vivo studies are needed to validate the role of miR-107 in tumor development and progression. It is reported by Li et al. that silencing the expression of miR-107 could suppress the migration and invasion of GC cell in nude mice30. We propose that the miR-107 may play an important role in vivo in GC carcinogenesis through multiple targets including NF1.
In summary, our data demonstrated that miR-107 targeted NF1, and suppression of miR-107 enhanced proliferation, migration and invasion of GC, whereas repression of NF1 promoted these phenotypes. We propose that miR-107 may serve as a useful therapeutic strategy for advanced GC.
Additional Information
How to cite this article: Wang, S. et al. miR-107 regulates tumor progression by targeting NF1 in gastric cancer. Sci. Rep. 6, 36531; doi: 10.1038/srep36531 (2016).
References
Jemal, A. et al. Global cancer statistics. CA Cancer J Clin 61, 69–90 (2011).
Tahara, E. Genetic pathways of two types of gastric cancer. IARC Sci Publ . 327–349 (2004).
You, J. S. & Jones, P. A. Cancer genetics and epigenetics: two sides of the same coin? Cancer Cell 22, 9–20 (2012).
Ambros, V. The functions of animal microRNAs. Nature 431, 350–355 (2004).
Wang, W. X. et al. miR-107 regulates granulin/progranulin with implications for traumatic brain injury and neurodegenerative disease. Am J Pathol. 177, 334–345 (2010).
Trajkovski, M. et al. MicroRNAs 103 and 107 regulate insulin sensitivity. Nature 474, 649–653 (2011).
Grady, W. M. & Tewari, M. The next thing in prognostic molecular markers: microRNA signatures of cancer. Gut 59, 706–708 (2010).
Di Leva, G. & Croce, C. M. miRNA profiling of cancer. Curr Opin Genet Dev. 23, 3–11 (2013).
Wang, S. et al. A common genetic variation in the promoter of miR-107 is associated with gastric adenocarcinoma susceptibility and survival. Mutat Res Fundam Mol Mech Mutagen 35–41, doi: 10.1016/j.mrfmmm.2014.1007 1002 (2014).
Finnerty, J. R. et al. The miR-15/107 group of microRNA genes: evolutionary biology, cellular functions, and roles in human diseases. J Mol Biol. 402, 491–509 (2010).
Chen, L. et al. P53-induced microRNA-107 inhibits proliferation of glioma cells and down-regulates the expression of CDK6 and Notch-2. Neurosci Lett. 534, 327–332 (2013).
Takahashi, Y. et al. MiR-107 and MiR-185 can induce cell cycle arrest in human non small cell lung cancer cell lines. PLoS One 4, e6677 (2009).
Martello, G. et al. A MicroRNA targeting dicer for metastasis control. Cell 141, 1195–1207 (2010).
Li, X. et al. MicroRNA-107, an oncogene microRNA that regulates tumour invasion and metastasis by targeting DICER1 in gastric cancer. J Cell Mol Med. 15, 1887–1895 (2011).
Wang, M. et al. A novel functional polymorphism C1797G in the MDM2 promoter is associated with risk of bladder cancer in a Chinese population. Clin Cancer Res. 14, 3633–3640 (2008).
Ye, J., Li, A., Liu, Q., Wang, X. & Zhou, J. Inhibition of mitogen-activated protein kinase kinase enhances apoptosis induced by arsenic trioxide in human breast cancer MCF-7 cells. Clin Exp Pharmacol Physiol. 32, 1042–1048 (2005).
Dai, C. et al. Loss of tumor suppressor NF1 activates HSF1 to promote carcinogenesis. J Clin Invest 122, 3742–3754 (2012).
Lenarduzzi, M. et al. MicroRNA-193b enhances tumor progression via down regulation of neurofibromin 1. PLoS One 8, e53765 (2013).
Cichowski, K., Santiago, S., Jardim, M., Johnson, B. W. & Jacks, T. Dynamic regulation of the Ras pathway via proteolysis of the NF1 tumor suppressor. Genes Dev. 17, 449–454 (2003).
Jing, Q. et al. Involvement of microRNA in AU-rich element-mediated mRNA instability. Cell 120, 623–634 (2005).
Banerjee, S. et al. The neurofibromatosis type 1 tumor suppressor controls cell growth by regulating signal transducer and activator of transcription-3 activity in vitro and in vivo. Cancer Res. 70, 1356–1366 (2010).
Song, Y. Q. et al. MicroRNA-107 promotes proliferation of gastric cancer cells by targeting cyclin dependent kinase 8. Diagn Pathol. 9, 164 (2014).
Feng, L., Xie, Y., Zhang, H. & Wu, Y. miR-107 targets cyclin-dependent kinase 6 expression, induces cell cycle G1 arrest and inhibits invasion in gastric cancer cells. Med Oncol. 29, 856–863 (2012).
Brems, H., Beert, E., de Ravel, T. & Legius, E. Mechanisms in the pathogenesis of malignant tumours in neurofibromatosis type 1. Lancet Oncol. 10, 508–515 (2009).
Boudry-Labis, E. et al. Neurofibromatosis-1 gene deletions and mutations in de novo adult acute myeloid leukemia. Am J Hematol. 88, 306–311 (2013).
Maertens, O. et al. Molecular pathogenesis of multiple gastrointestinal stromal tumors in NF1 patients. Hum Mol Genet 15, 1015–1023 (2006).
Dhillon, A. S., Hagan, S., Rath, O. & Kolch, W. MAP kinase signalling pathways in cancer. Oncogene 26, 3279–3290 (2007).
Carthew, R. W. & Sontheimer, E. J. Origins and Mechanisms of miRNAs and siRNAs. Cell 136, 642–655 (2009).
Haeussler, J. et al. Tumor antigen HuR binds specifically to one of five protein-binding segments in the 3′-untranslated region of the neurofibromin messenger RNA. Biochem Biophys Res Commun. 267, 726–732 (2000).
Li, X. et al. MicroRNA-107, an oncogene microRNA that regulates tumourinvasion and metastasis by targeting DICER1 in gastric cancer. J Cell Mol Med. 15(9), 1887–1895 (2011).
Acknowledgements
This study was partly supported by National Natural Science Foundation of China (81230068, 81373091, 81302502, 81302490, and 81473049), Natural Science Foundation of Jiangsu Province (BK2012842, BK20130641 and BK2011194), the Key Program for Basic Research of Jiangsu Provincial Department of Education (12KJA330002), Specialized Research Fund for the Doctoral Program of Higher education of China (20130092120063), Jiangsu Provincial Science and Technology Innovation Team, Collaborative Innovation Center For Cancer Personalized Medicine and the Priority Academic Program Development of Jiangsu Higher Education Institutions (Public Health and Preventive Medicine).
Author information
Authors and Affiliations
Contributions
Z.Z. and M.W. conceived and designed the experiments. S.W., G.M., H.Z., and N.T. performed the experiments. C.L., D.W., and H.C. analyzed the data. F.Q., W.G., Q.Z., G.T. and J.Z. contributed reagents/materials/analysis tools. S.W wrote the paper.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Wang, S., Ma, G., Zhu, H. et al. miR-107 regulates tumor progression by targeting NF1 in gastric cancer. Sci Rep 6, 36531 (2016). https://doi.org/10.1038/srep36531
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep36531
This article is cited by
-
MicroRNAs are involved in the development and progression of gastric cancer
Acta Pharmacologica Sinica (2021)
-
MicroRNAs’ role in the environment-related non-communicable diseases and link to multidrug resistance, regulation, or alteration
Environmental Science and Pollution Research (2021)
-
MicroRNA-107 enhances radiosensitivity by suppressing granulin in PC-3 prostate cancer cells
Scientific Reports (2020)
-
MicroRNA Expression Profiles in Gastric Carcinogenesis
Scientific Reports (2018)
-
MiR-107 suppresses cell proliferation and tube formation of Ewing sarcoma cells partly by targeting HIF-1β
Human Cell (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.