Abstract
The complexity of endometrial receptivity at the molecular level needs to be explored in detail to improve the management of infertility. Here, differential expression of transcriptomes in receptive endometrial glands and stroma revealed Ectonucleotide Pyrophosphatase/Phosphodiesterase 3 (ENPP3) as a progesterone regulated factor and confirmed by various methods, both at mRNA and protein level. The involvement of ENPP3 in embryo attachment was tested in an in vitro model for human embryo implantation. Interestingly, there was high expression of ENPP3 mRNA in stroma but not protein. Presence of N-glycosylated ENPP3 in receptive phase uterine fluid in women confirms its regulation by progesterone and makes it possible to use in a non-invasive test of endometrial receptivity.
Similar content being viewed by others
Introduction
A significant cause of female infertility (10–15% globally) is the failure to establish a receptive endometrium, with the latter primarily driven by progesterone (P). Despite optimization of critical events in assisted reproductive technology, pregnancy rates do not exceed 30%1. Important limitations are the lack of knowledge about the implantation process, including endometrial receptivity and lack of reliable diagnosis of receptivity. Recent advances in omics technology, either by a genomic or proteomic approach, has yielded many molecules regulated during the receptive phase: integrins αvβ32, LIF, gp1303, nuclear pore proteins4, HB-EGF5, mucins6, heart and neural crest derivatives 27, homeobox genes8, Annexin A29, Annexin IV10, Calreticulum11, Stathmin 19 and Ezrin12, but no unequivocal receptivity marker is yet defined in humans.
Taking into consideration the dynamic nature of the endometrium, cellular and molecular signatures alter rapidly due to ovarian hormonal regulation in a given menstrual cycle13. Endometrial tissue sampling for identification of biomarkers in endometrial receptivity by microarray studies include divergent cohorts: normo-ovulatory women14,15,16,17,18,19,20,21,22, fertile donors23, fertile mid-secretory phase and infertile women24,25, natural and stimulated cycles16,26 and women with recurrent implantation failure or miscarriage27,28. The high degree of heterogenicity leads to difficulty in deriving conclusions for receptivity genes. Adding to this, the above studies were done using whole endometrial tissue, which constitutes diverse cell types in altered ratios with distinct genotypic and phenotypic expression, leading to different results.
The antiprogestin mifepristone administered on cycle day LH + 2 has previously been used to study P-regulated endometrial receptivity29,30,31. Potentially, this approach could also be used to identify a possible biomarker for endometrial receptivity. To overcome confounding factors such as tissue variability and to minimize subject-to-subject variations, we selectively isolated the mid-secretory phase glandular epithelium and stroma from fertile and infertile women by laser capture microdissection (LCMD), followed by microarray. The results were reconfirmed by real time PCR and immunohistochemistry. From our findings, we report here a P-regulated molecule, Ectonucleotide Pyrophosphatase/ Phosphodiesterase 3 (ENPP3) that can serve as a potential biomarker for progesterone regulated endometrial receptivity. Expression of this glycoprotein was also quantified in uterine fluid with the possible aim to develop a non-invasive endometrial receptivity assay.
Results
LCMD and gene expression analysis
The LCMD of approximately 200 cells yielded a minimum of 500 pg of RNA that was taken for amplification. Microarray data analysis showed 32 genes out of 47 were up-regulated and 15 genes down-regulated in the epithelial compartment, whereas in the stromal compartment, 79 out of 85 genes were up-regulated and 6 down-regulated with mifepristone treatment (Supplementary Table 1). A higher number of significantly downregulated genes were observed in the glands in comparison to stroma with mifepristone treatment (Fig. 1).
Heatmaps for hierarchical clustering of significant genes.
Genes regulated by progesterone in endometrial glandular (G, left panel) and stromal (S, right panel) compartments shown by heatmaps. Gene expression was studied in the receptive endometrium (C) in a non-treated cycle and non-receptive endometrium (T) with the treatment of progesterone receptor antagonist mifepristone. Each woman in the study acted as their own control.
Biological and molecular pathway analysis
The 132 significantly regulated (up or down) genes were analyzed for upstream regulators, canonical pathways and biological networks. The leading five canonical pathways obtained were NRF2-mediated oxidative stress response, ovarian cancer signaling, superoxide radicals dismutation, prostate cancer signaling and glioblastoma multiforme signaling, respectively. Ingenuity Pathway Analysis (IPA) predicts activation or inhibition of upstream regulators that may be responsible for gene expression changes observed in the experimental dataset, which aids in understanding the biological activities occurring in the tissues or cells. In the current dataset, transcription factor Chromobox Homolog 5 (CBX5) was predicted to be inhibited with an unbiased Z score of −2.236 and upstream regulator molecules. Colony stimulating factor 2 (CSF2) and early B cell factor 1 (EBF1) were predicted to be activated with a Z scores of 2.43 and 2.0, respectively.
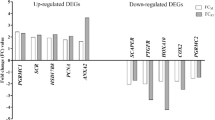
Validation of microarray by real-time PCR
Real-time PCR analysis was in line with the microarray study, as 13 and 11 differentially expressed genes respectively from the stromal and epithelial compartments were corroborated in both methods (supplementary Table 2). Secreted frizzled-related protein 4 (SFRP4) was up regulated by 8.76 fold (p = 0.013) in the stroma compartment and by 16.25 fold (p = 0.0001) in the epithelial compartment. Carboxypeptidase M (CPM) was up-regulated by 29 fold (p = 0.005) in the stromal compartment, while Ubiquitin-Conjugating Enzyme E2E 2 (UBE2E2) was up-regulated by 7 fold (p = 0.024) in the epithelial compartment. MT1G is down-regulated by 7 fold (p = 0.008) in stromal and 519 fold (p = 0.005) in epithelial compartments and MT2A was down-regulated by 3 fold (p = 0.031) in stromal and by 7 fold (p = 0.03) in epithelial compartments. ENPP3 was significantly down-regulated in both the stromal (−55.93 fold; p = 0.015) and epithelial (−9.46 fold; p = 0.035) compartments (Figs 2 and 3).
Immunohistochemical analysis
Based on the literature review, microarray expression levels and availability of antibodies, we studied the protein expression of stanniocalcin 1 (STC1); Cathepsin C (CTSC); Secrteoglobin family 2A member2 (SCGB2A2); SWI/SNF related matrix associated actin-dependent regulator of chromatin subfamily a member 1 (SMARCA1); high-mobility group nucleosome binding domain 5 (HMGN5); and B-cell CLL/lymphoma 11A (zinc finger protein) (BCL11A). Immunodetection of ENPP3 was observed in all the tissues from healthy fertile women and differed significantly between the groups. The findings were in line with the microarray results (Fig. 4A–C).
Regulation of ENPP3 by progesterone.
The expression of ENPP3 was observed very specifically in the apical border of glands in P dominant mid-luteal phase as studied by immunohistochemistry (A,C,D) in women without mifepristone treatment (control). Downregulation of ENPP3 was observed in endometrial glands with the suppression of progesterone action by mifepristone treatment (B,C). In endometrium of women without mifepristone treatment, high level of ENPP3 was observed during P upregulated secretory phase, on comparing with proliferative phase of the menstrual cycle. Scale bar indicates 50 μm.
Expression of ENPP3 in endometrium
Microarray analysis showed down-regulation of ENPP3 by 59 fold in the epithelial compartment (p = 0.04) with P inhibition. Immunohistochemical analysis for ENPP3 showed expression specific to the apical surface of the epithelial compartment and glandular secretions, but was very scanty in the treatment group. The mean immunoreactive score (IRS ± SD) for the control group was 8.8 ± 4.41 and the treatment group was very low 0.42 ± 1.13 (p = 0.0007). Interestingly, the protein expression for ENPP3 was not seen in stroma in either group, although mRNA expression was seen in both groups as studied by western blot and immunohistochemistry. ENPP3 showed a cyclical expression highest in the mid-secretory phase and lowest in the proliferative phase with mean IRS ± SD scores respectively in proliferative, mid and late-secretory phases were 1.97 ± 2.21, 10.25 ± 3.88 and 7.12 ± 3.83, respectively. Higher expression of ENPP3 was observed in P dominant mid-secretory phase on comparing with the proliferative phase (p = 0.0001). There was no significant difference between mid- and late-secretory phases (Fig. 4D).
ENPP3 protein expression in uterine fluid and whole endometrial tissue lysates
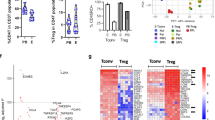
The uterine lavages from fertile women and the same women treated with a single dose of 200 mg of mifepristone on LH + 2 were collected on LH + 6/7 and tested for ENPP3 protein expression by the western blotting technique. A strong band was observed around 165 kd indicating glycosylated ENPP3 and showed a significant downregulation in P-inhibited group (AUC - control 17.85: mifepristone treatment: 9.47; p = 0.002) with a similar pattern to that of tissue ENPP3 (AUC -control 18.98: mifepristone treatment 11.94; p = 0.002). The expression of ENPP3 in endometrial tissue lysate was more abundant than in uterine fluid (Fig. 5).
Expression of ENPP3 in endometrium and uterine fluid.
Western blot analysis of ENPP3 in receptive phase endometrial tissue lysates (A,B) and uterine fluid (C,D) by Wes showed good expression levels of ENPP3 in control samples (lanes 2–7). Antiprogestin treatment (A,C): lanes 8–13) showed no detectable levels of ENPP3, both in endometrial tissue and uterine fluid, confirming the regulation of ENPP3 protein by progesterone. (B,D) show semiquantitative analysis of immunodetectable ENPP3 by Wes, expressed in log2 AUC (area under the curve). Lane 1: protein molecular weight marker.
Evaluation of ENPP3 as glycoprotein
The predicted molecular weight of ENPP3 is around 100 kd, but Western blot analysis showed a band at 165 kd, leading us to further investigate its glycosylation. We tested uterine fluid and endometrial tissue lysates after digesting with Peptide-N-Glycosidase F (PNGase F), which cleaves the glycoaminidase link between asparagine and N-acetylglucosamines. We observed a shift from 165 kD to 110 kD in the deglycosylated samples, confirming that ENPP3 is N-Glycosylated in the uterine fluid and endometria of healthy fertile women (Fig. 6).
N-glycosylated ENPP3 in human endometrium.
Deglycosylation of uterine fluid showed a shift of band from 165 kD to a single band at 110 kD, meaning that ENPP3 in the uterine fluid is present in its glycosylated form. The glycosylated (lanes 2–7) form of ENPP3 showed a band at 165 kD and the deglycosylated (lanes 8–13) form had a single band at 110 kD.
In vitro functional assay
Embryo attachment was studied in a previously-described three-dimensional endometrial cell culture model to study human implantation process in vitro32 and showed that 7 out of 10 blastocysts attached to the endometrial construct in the control group. In controls, a very good expression level of ENPP3 was seen as studied by real-time PCR. Exposure to mifepristone (0.5 μM) led to significant (p = 0.004; fisher’s exact test) down-regulation of ENPP3, with none of the embryos attached to the in vitro endometrial construct (p = 0.004, Fig. 7).
Embryo attachment and ENPP3 expression.
Human embryo attached to the in vitro three-dimensional cell culture model with progesterone exposure (A). None of the 8 embryos in the anti-progestin treated group, where ENPP3 was significantly down regulated had attached. In the control group, 7 out of 10 blastocysts attached (B) to the construct, with very good expression of ENPP3 in the three-dimensional endometrial cell culture system.
Analysis of uterine fluid of receptive and non-receptive phase with nano-ESI-LC/MS/MS
We identified and quantified the expression of ENPP3 protein with 35 ENPP3 specific peptides obtaining 53.4% sequence coverage in the mass-spectrometry of uterine fluid. Based on total normalized protein intensities, ENPP3 protein was observed to be upregulated (mean fold change + 35.0, p = 0.003) during P dominant LH + 8, on comparing with early secretory phase (LH + 2) of the natural menstrual cycle (Fig. 8).
Expression of ENPP3 in the uterine fluid of receptive and non-receptive phase.
Tukey plot for the expression of ENPP3 quantified by nano-ESI-LC/MS in uterine fluids from early secretory phase (LH + 2) and mid-secretory phase (LH + 8) of the same set of women. A significant upregulation of ENPP3 (p = 0.0032) was observed in P dominant, receptive phase (LH + 8) on comparison with non-receptive phase (LH + 2).
Discussion
Our study systematically shows that ENPP3, a N-glycosylated protein regulated by P, is compartmentalized in endometrial glands as well as uterine secretions during the receptive phase. The regulation of ENPP3 by progesterone and the role in implantation process was tested using an in vitro human embryo implantation model, where exposure to a P receptor inhibitor inhibited human embryo attachment and thus the embryo implantation process along with the downregulation of ENPP3 expression. As the expression of ENPP3 in the endometrium correlated to that in uterine fluid, we propose that analysis of ENPP3 in uterine fluid may be used as a potential marker in non-invasive test for P regulated endometrial receptivity. Before the use in a clinical setup, we need to validate the data from women with recurrent implantation failure (RIF). This will demand a large number of samples to derive statistical significance to adjust for different factors contributing to RIF.
There are several studies conducted to identify endometrial transcriptome with array technology to explore endometrial receptivity markers with the aim of translating them to clinical use, mainly for diagnosis20,26,33,34. None of the above studies, including the studies that compared the mRNA as well as protein profiling between early (LH + 2) and mid (LH + 7 or 8) luteal phase have reported the expression of ENPP335,36,37. Here, for the first time we report that ENPP3 is highly expressed during progesterone dominant mid-luteal phase (LH + 8) compared with early luteal phase (LH + 2), when the level of P is less. Interestingly, a very recent study conducted to decipher the transcriptome profile of endometrium of RIF patients showed 303 predictive genes and ENPP5, a molecule that belong to ectonucleotide pyrophosphatase family38. Though, these reported data are of potential value to identify and develop array based predictive methods39,40, the functional role of these molecules still remains to be explored and for most of the transcripts, we do not know if they are further transcribed into their protein. In this study, we show the expression of ENPP3 both, at mRNA and protein level in the endometrium and also try to demonstrate its possible role in the process of human embryo implantation with the best available in vitro model to study human embryo implantation process. It will be important to further explore the molecular mechanism of ENPP3 in endometrial receptivity and implantation, particularly in female infertility.
Currently, endometrial receptivity array34,39 (ERA) claims to be a superior and more accurate method for endometrial receptivity evaluation compared to endometrial histological dating using Noyes criteria41. However, advanced technology with quality-controlled central laboratories are required for this analyses42. A recently developed method based on the expression of integrins43 (E-tegrity test®) may have potential but needs further clinical studies. It should be noted that both methods are invasive as an endometrial biopsy is required for analysis. The high impact of P on the expression of ENPP3 in the uterine fluid of a receptive endometrium, as reported in this study, is promising and supports its possible use in a receptivity test during the effectual cycle of embryo transfer. Collection of uterine fluid though requires insertion of flexible catheter into the uterine cavity, it does not cause injury to endometrium. More importantly, sampling of uterine fluid in an embryo transfer cycle does not reduce the implantation or pregnancy rate44. Hence, we propose that ENPP3 could be used as a marker for a non-invasive test of uterine fluid for progesterone regulated endometrial function. Such tests are not only important in identifying receptive endometrium before starting expensive fertility treatment, but also useful in personalized embryo transfer, that has given the possibility for some women with RIF to conceive45.
The novelty of this study compared with that of earlier reports lies in the fact that, we studied the gene expression of major cell types from a cohort of proven fertile women who were their own controls, minimizing the possible wide variations seen in idiopathic infertility. Secondly, stroma and glands in both receptive and non-receptive endometrium were isolated by laser capture microdissection, ruling out the possible global gene expression of different genes seen when using the whole endometrium. Most of the previously-published microarray-based gene expression studies were carried out using whole endometrial tissue14,15,20,21,23,46,47, giving the cumulative gene expression effect of all various cell types in the endometrium. We used microarray, a powerful technique to screen vast number of possible genes that are differently expressed. The expression of ENPP3 at transcriptome level was confirmed with a more sensitive and specific method, real time PCR. Further we looked into the expression and distribution of ENPP3 at protein level by Immunohistochemistry. As the expression level of ENPP3 was drastically downregulated with P inhibition, we looked for its expression in the uterine fluid, with the intention of further exploring the possibility of identifying a marker that could be used to develop a less invasive method. For this, we used one of the recently introduced sensitive and rapid method Wes48,49, that is suitable to analyse low level of protein in very small sample volume as only a very small quantity of protein and uterine fluid could be sampled from women. To study the expression of ENPP3 in receptive and non-receptive phase of the menstrual cycle, we used yet another highly sensitive label free protein analytic technology, nano-ESI-LC/MS/MS50. In the past, there are no reports on the functional role of the reported markers on endometrial receptivity as studies in humans are impossible due to ethical reasons. Here, we verified the functional role of ENPP3 in endometrial cells using a previously-described, well-established in vitro model for embryo attachment32.
The regulation of ENPP3 in endometrial cells is intriguing, as the transcription was downregulated to an extent of 55 times in stromal compartments in non-receptive endometria, but without any detectable levels in protein. This was studied using two different antibodies, both by immunohistochemistry and Western immunoblot. Moreover, the mRNA expression of ENPP3 was more than double in the stromal compartment when compared with the glandular compartment. This high level of mRNA with no protein expression in the stromal compartment for ENPP3 not only reflects post-translational mechanisms at the protein level, but may have a significant biological role, which needs to be studied extensively. In endometrial epithelial cells, ENPP3 is regulated by P, as high levels were observed in the secretory phase of the menstrual cycle in comparison to the proliferative phase. However, we do not see a statistical significance between mid and late secretory phases, though there is a decrease in their mean values. This could be that the threshold level of P required to produce ENPP3 is less and though P is downregulated in the late secretory phase, still a basal level of P exists and this may be enough to produce significant level of ENPP3 that is observed in late luteal phase. In the endometrium, there are reports that ENPP3 is expressed in the epithelial glands as seen by quantitative mass spectrometry analysis in premenopausal women51.
We tried to characterize ENPP3, found in the endometrium and uterine fluid. For ENPP3, an immunoblot band is expected around the molecular weight of 100 kd. Surprisingly, a higher molecular weight band around 165 kd was observed, which on further investigation was found to be the glycosylated form present in the uterine fluid samples. We confirmed that this high molecular weight band is the glycosylated form of ENPP3, as treatment of receptive endometrial uterine fluid samples with N-Glycanase resulted in a loss of the immunoblot band at 165 kd and its presence at 100 kd. The expression of ENPP3 in the uterine fluid and endometrial tissue during the receptive phase of the menstrual cycle from proven fertile women had a similar pattern to the glycosylated ENPP3 form. The presence of ENPP3 in glandular secretions as exosomes has been reported earlier as it is present in human parotid glandular secretions encapsulated in exosomes52.
ENPP3 is one of the newly described molecules and thus less studied. The expression of ENPP3 in general is mainly reported in basophil and mast cells53. ENPP3 is a type II transmembrane protein and lacks the di-leucine that is characteristic of membrane proteins54. This is in line with our observation of the endometrium, as ENPP3 is seen only in the apical surface of epithelial cells. The only ENPP family of protein reported in human endometrium is ENPP5, a type I transmembrane protein and there are no report on its function38. It would be interesting to study the biological function of ENPP3, especially in relation to its expression and understanding in cases of RIF. One of the challenges in deriving a statistical significance to show the role of ENPP3 in RIF at endometrial level, we may require a large number of samples, as wide range of molecules may contribute individually or collectively to RIF.
The ENPP3 ectoenzyme is involved in extracellular nucleotide hydrolysis and possesses both ATPase and ATP pyrophosphatase activity. It cleaves a variety of phosphodiester and phosphosulfate bonds including deoxynucleotides, nucleotide sugars and NAD55,56,57. Recently it was shown that ENPP3 regulates the glycosyltransferase activity, which facilitates the glycosylation of many proteins by inhibiting an intrinsic factor for N-acetylglucosaminyltransferase GnT-IX (GnT-Vb) in murine neuroblastoma Neuro 2a cells58. Interestingly, the work of Korekane et al. shows that ENPP3 can either increase or decrease the activity of glycans59 and glycans are present both in the endometrium and uterine secretions, having an important role in the regulation of endometrial receptivity. The expression of Le(Y) oligosaccharide during the receptive period is known to be down-regulated by the inhibition of early luteal phase P by mifepristone in monkey endometria60. It is also known that the expression of MUC16 disappears from the endometrium at the time of embryo implantation, coinciding with the period of ENPP3 expression61. We do not know the specific glycans regulated by ENPP3 in the endometrium, but this is worth further exploring with regard to its regulation in different gynaecological conditions.
Based on our results we conclude that ENPP3 could be used as a molecular marker for progesterone action at the endometrial level in women. With further studies, this may be used to develop a less invasive method to screen women seeking IVF for endometrial receptivity using uterine fluid, before the planned embryo transfer. On the other hand, it may also be possible to develop an inhibitor or molecule that could alter the function of ENPP3 so it can be used for fertility control. For this, the first step may be to screen the molecular libraries to identify a potent inhibitor. A detailed study to understand the physiological function of this molecule in the endometrium and uterine fluid is essential.
Methods
Ethical permissions
All experiments were carried out in accordance with the approved guidelines. The experimental protocols including tissue sampling were approved by Karolinska University Hospital and the regional ethics committee (EPN), Stockholm, Sweden. The Ethical Committee from University of Tartu had approved the permission to collect and perform analysis of uterine fluid collected at their center. Informed and written consent was obtained from all the volunteers participated in the study and the documents were filed as per institutional documentation guidelines.
Endometrial biopsies
Endometrial biopsies were collected from proven healthy fertile women (n = 9) aged 22–37 years from the upper part of the endometrial cavity with a Pipelle aspirator (Prodimed, Neuilly en Thelle, France). These women were free from any gynaecological disorders and were not taking any hormonal contraception or had any intrauterine devices for a minimum of three months before the biopsy. All the subjects self-examined LH peak in urine samples collected twice a day from approximately cycle day 10 to LH + 2 by using a rapid self-test (Clearplan, Searle Unipath Ltd., Bedford, UK). Biopsies were obtained from each woman on cycle day LH + 7 in a control cycle and thereafter in a treatment cycle. In the treatment cycle, women received a single dose of 200 mg mifepristone on LH + 2. Each biopsy was divided into two portions, with one fixed in 4% paraformaldehyde for immunohistochemistry and the other snap frozen in liquid nitrogen for laser microdissection and RNA extraction. Endometrial samples from healthy women (n = 27) were also obtained during the proliferative, mid-secretory and late-secretory phases of the menstrual cycle, with nine endometrial samples for each group.
In order to confirm the protein expression of ENPP3 during the receptive phase, 6 endometrial biopsies from control and treatment cycle (200 mg mifepristone on LH + 2) were collected during LH + 6 to LH + 9 from healthy women and were snap frozen in liquid nitrogen till further use. For in vitro functional assay by three-dimensional cell cultures, endometrial biopsies were collected from proven fertile women (n = 30) on LH + 4, followed by isolation of stromal and epithelial cells by well-established protocols as previously described62.
Endometrial cell isolation
Briefly, the tissue was minced into 1 × 1 mm in Ham F10 (Life Technologies, Sweden) and incubated with pancreatin-trypsin EDTA (0.05 g/ml of trypsin-EDTA solution) for 30 minutes at 4 °C followed by digestion with Collagenase 4 (125 IU/ml, Worthington Biochemical, Lakewood NJ) and DNAse (40 μg/ml final concentration, Sigma, Sweden) and filtered through a 40-micron mesh cell strainer that allowed stromal cells to pass through and epithelial glands to remain in the strainer. Epithelial glands were digested with collagenase 3 (45 IU/ml, Worthington Biochemical, Lakewood, NJ) and DNAse and filtrated through a 40-micron mesh cell strainer. Stromal and epithelial cells were then separated in a recovery cell culture medium (Life Technologies) and preserved in liquid nitrogen until thawed for the endometrial co-culture.
Blastocysts
The embryos/blastocysts (n = 18) for this study were acquired through standard in vitro fertilization (IVF) or intracytoplasmic sperm injection (ICSI). The embryos used in this study were of at least grade 3BB (Gardner’s classification) and clinically valid for embryo transfer.
Three-dimensional endometrial cell cultures
Endometrial cell cultures were conducted as described by Lalitkumar et al.63. After five days of culturing, one group of cultures was treated with mifepristone concentration (Sigma Aldrich) of 0.5 μM (n = 8) and control group was treated with only the vehicle ethanol (n = 10). One embryo was added to each culture on the same day that mifepristone treatment started. The culture medium was changed every two days under light microscope and cultures were examined for attachment of the embryos. On day five after embryo introduction, attachment rates were noted after mechanical testing by shaking the cultures and washing them with PBS twice. Before termination of cultures, any attached or non-attached embryos were removed. After termination, the cultures were detached from the cell inserts and dissolved in 1 ml of Trizol reagent (Invitrogen) and stored at −80 °C prior to RNA extraction.
Uterine fluid
Uterine fluid was collected from proven fertile women on LH + 7 with or without mifepristone treatment. Two ml of injection grade water (Gibco) was infused into the uterine cavity using a modified feeding catheter (Nutrisafe 2, Fr-L.75 cm, Vycon Value Life, Ecouen, France) fixed to a 10 ml syringe. With the help of the syringe, about 1 ml was sucked back along with the uterine lavage and centrifuged at 200 g for 10 minutes to remove any cells or cell debris. The supernatant was lyophilized and reconstituted in 50 μl sterile water and taken for further analysis.
In another set of fertile women (n = 6; University of Tartu, Estonia), uterine fluid was collected in the same cycle, during early secretory phase (LH + 2) and progesterone dominant mid-secretory (LH + 8) phase to perform label-free proteomic analysis for ENPP3 expression.
Automated western blot
A completely automated western blot was performed using Simple Wes (Protein Simple, San Jose, CA) as per the manufacturer’s instructions. Briefly, 2 μg of protein from the tissue lysates or uterine fluid was added to the standard fluorescent mastermix and loaded into corresponding wells of the prefilled Wes assay plate, along with antibody diluent (Protein Simple), anti-ENPP3 antibody (1:50 dilution Sigma LifeSciences, HPA043772), anti-rabbit secondary antibody (Protein Simple) and Streptavidin, followed by luminol peroxide mix. The imaging and analysis were done with compass software (Protein Simple).
Label-free proteomic analysis by Nano-ESI-LC/MS/MS
The uterine fluids were separated into six fractions based on its molecular weight using SDS-PAGE (Invitrogen). Proteins were then reduced, alkylated and in-gel digested with dimethylated porcine trypsin (Sigma) followed by analysis with nano-ESI-LC/MS/MS (Dionex Ultimate 3000 RSLC and Q Exactive MS/MS, Thermo Fisher Scientific at University of Tartu) using 2 h reversed phase gradients and a top-10 data-dependent acquisition method. The obtained label-free mass-spectrometric data were identified and quantified with MaxQuant software package64 (UniProtKB human reference proteome database, 2014 September version). Label-free data were normalized with the MaxLFQ algorithm50 and compared with paired or unpaired two-tailed t-test.
Fluorescence-activated cell sorting (FACS)
Stromal cells were selectively isolated from the pool of endometrial cells by negative selection with FACS. Briefly, the cells were washed and stained for epithelial cells with EPCAM/CD326 for 30 minutes and were sorted using MoFLOW® XDP flow cell activated cell sorter (Beckman Coulter, USA).
Immunohistochemistry
The 5 μm paraffin-embedded endometrial tissue samples were deparaffinized using a 2100-retriever autoclave (Histolab, Gothenburg, Sweden) and antigen retrieval done with a Diva Decloaker (Biocare Medical, Concord, CA). After peroxidase quenching, the sections were incubated with Background Sniper (Biocare Medical) followed by incubation with the primary antibodies (Supplementary Table 3) overnight at 4 °C. The primary antibodies were diluted in the diluent DaVinci Green (Biocare Medical, Concord, CA). The biotin-free detecting system Rabbit/Mouse HRP polymer kit MACH 3TM (Biocare Medical, Concord, CA) was used for detection. The reaction was developed with the Betazoid DAB Chromogen kit (Biocare Medical, Concord, CA). The counterstained hematoxylin (Vector Laboratories, Inc., Burlingame, CA) sections were mounted using the xylene-based medium Pertex® (Histolab, Gothenburg, Sweden) and analyzed in a Zeiss Axiovert 200 M microscope (Zeiss, Göttingen, Germany)62. All the slides were blinded and scored by two independent observers. The semi-quantitative IRS-score65 was used to assess the percentage of the positive cells (PC) and the staining intensity (SI). On disparity between the two observers, a third independent observer analysed the blinded slides and the average score of the two closest results was taken for further analysis.
Deglycosylation
Endometrial tissue lysates and uterine fluid samples were subjected to mild denaturation with 0.2% Rapigest SF Surfactant (Waters, 186001861) and DTT (5 mM) and the samples were denatured for 5 minutes at 95 °C. Iodoacetamide (15 mM final concentration) was added and incubated for 30 minutes in dark and in-solution enzymatic digestion was done by incubation with 1 μl/sample PNGase F (Roche, 11365169001) for 2 hours at 37 °C and analyzed by Simple Wes.
Statistical analysis
The paired T-test and SAM methods were performed to analyze microarray data by MultiExperiment Viewer. The Mann-Whitney U test was applied to compare immunohistochemical staining between the control and treatment groups. Based on the statistical assumptions, either an unpaired T-test or Mann Whitney test was performed for analyzing the real time PCR and western blot data. Fisher’s exact test was performed to analyze blastocyst attachment rate. All the statistical analysis was done with XLSTAT 2015 (Addinsoft) and Prism 6 (GraphPad Software).
Additional Information
Accession code: Microarray data, GEO repository accession number GSE59447.
How to cite this article: Boggavarapu, N. R. et al. Compartmentalized gene expression profiling of receptive endometrium reveals progesterone regulated ENPP3 is differentially expressed and secreted in glycosylated form. Sci. Rep. 6, 33811; doi: 10.1038/srep33811 (2016).
References
Pandian, Z., Bhattacharya, S., Vale, L. & Templeton, A. In vitro fertilisation for unexplained subfertility. Cochrane Database Syst Rev, CD003357 (2005).
Lessey, B. A. et al. Use of integrins to date the endometrium. Fertility and sterility 73, 779–787 (2000).
Tawfeek, M. A., Eid, M. A., Hasan, A. M., Mostafa, M. & El-Serogy, H. A. Assessment of leukemia inhibitory factor and glycoprotein 130 expression in endometrium and uterine flushing: a possible diagnostic tool for impaired fertility. BMC Womens Health 12, 10.
Guffanti, E. et al. Nuclear pore complex proteins mark the implantation window in human endometrium. J Cell Sci 121, 2037–2045.
Xie, H. et al. Maternal heparin-binding-EGF deficiency limits pregnancy success in mice. Proceedings of the National Academy of Sciences of the United States of America 104, 18315–18320.
Meseguer, M. et al. Human endometrial mucin MUC1 is up-regulated by progesterone and down-regulated in vitro by the human blastocyst. Biology of reproduction 64, 590–601 (2001).
Li, Q. et al. The antiproliferative action of progesterone in uterine epithelium is mediated by Hand2. Science 331, 912–916.
Lim, H., Ma, L., Ma, W. G., Maas, R. L. & Dey, S. K. Hoxa-10 regulates uterine stromal cell responsiveness to progesterone during implantation and decidualization in the mouse. Molecular endocrinology 13, 1005–1017.
Dominguez, F. et al. Proteomic analysis of the human receptive versus non-receptive endometrium using differential in-gel electrophoresis and MALDI-MS unveils stathmin 1 and annexin A2 as differentially regulated. Human reproduction 24, 2607–2617.
Li, J. et al. [Study of altered expression of annexin IV and human endometrial receptivity]. Zhonghua Fu Chan Ke Za Zhi 41, 803–805 (2006).
Parmar, T. et al. Protein profiling of human endometrial tissues in the midsecretory and proliferative phases of the menstrual cycle. Fertility and sterility 92, 1091–1103.
Heng, S. et al. Proprotein convertase 5/6 is critical for embryo implantation in women: regulating receptivity by cleaving EBP50, modulating ezrin binding and membrane-cytoskeletal interactions. Endocrinology 152, 5041–5052.
Chabbert Buffet, N., Djakoure, C., Maitre, S. C. & Bouchard, P. Regulation of the human menstrual cycle. Front Neuroendocrinol 19, 151–186 (1998).
Borthwick, J. M. et al. Determination of the transcript profile of human endometrium. Molecular human reproduction 9, 19–33 (2003).
Carson, D. D. et al. Changes in gene expression during the early to mid-luteal (receptive phase) transition in human endometrium detected by high-density microarray screening. Molecular human reproduction 8, 871–879 (2002).
Haouzi, D. et al. Gene expression profile of human endometrial receptivity: comparison between natural and stimulated cycles for the same patients. Human reproduction 24, 1436–1445.
Kao, L. C. et al. Globzal gene profiling in human endometrium during the window of implantation. Endocrinology 143, 2119–2138.
Kuokkanen, S. et al. Genomic profiling of microRNAs and messenger RNAs reveals hormonal regulation in microRNA expression in human endometrium. Biology of reproduction 82, 791–801.
Ponnampalam, A. P., Weston, G. C., Trajstman, A. C., Susil, B. & Rogers, P. A. Molecular classification of human endometrial cycle stages by transcriptional profiling. Molecular human reproduction 10, 879–893.
Riesewijk, A. et al. Gene expression profiling of human endometrial receptivity on days LH+2 versus LH+7 by microarray technology. Molecular human reproduction 9, 253–264 (2003).
Talbi, S. et al. Molecular phenotyping of human endometrium distinguishes menstrual cycle phases and underlying biological processes in normo-ovulatory women. Endocrinology 147, 1097–1121.
Tseng, L. H. et al. Genome-based expression profiling as a single standardized microarray platform for the diagnosis of endometrial disorder: an array of 126-gene model. Fertility and sterility 94, 114–119.
Mirkin, S. et al. In search of candidate genes critically expressed in the human endometrium during the window of implantation. Human reproduction 20, 2104–2117.
Altmae, S. et al. Endometrial gene expression analysis at the time of embryo implantation in women with unexplained infertility. Molecular human reproduction 16, 178–187.
Koler, M. et al. Disrupted gene pattern in patients with repeated in vitro fertilization (IVF) failure. Human reproduction 24, 2541–2548.
Ruiz-Alonso, M., Blesa, D. & Simon, C. The genomics of the human endometrium. Biochimica et biophysica acta 1822, 1931–1942.
Ledee, N. et al. Specific and extensive endometrial deregulation is present before conception in IVF/ICSI repeated implantation failures (IF) or recurrent miscarriages. The Journal of pathology 225, 554–564.
Othman, R. et al. Microarray profiling of secretory-phase endometrium from patients with recurrent miscarriage. Reprod Biol 12, 183–199 (2012).
Cameron, S. T., Critchley, H. O., Buckley, C. H., Kelly, R. W. & Baird, D. T. Effect of two antiprogestins (mifepristone and onapristone) on endometrial factors of potential importance for implantation. Fertility and sterility 67, 1046–1053 (1997).
Danielsson, K. G., Marions, L. & Bygdeman, M. Effects of mifepristone on endometrial receptivity. Steroids 68, 1069–1075 (2003).
Spitz, I. M. Mifepristone: where do we come from and where are we going? Clinical development over a quarter of a century. Contraception 82, 442–452.
Danielsson, K. G. et al. Effect of low daily doses of mifepristone on ovarian function and endometrial development. Human reproduction 12, 124–131 (1997).
Bhagwat, S. R. et al. Endometrial receptivity: a revisit to functional genomics studies on human endometrium and creation of HGEx-ERdb. PLoS One 8, e58419.
Diaz-Gimeno, P. et al. The accuracy and reproducibility of the endometrial receptivity array is superior to histology as a diagnostic method for endometrial receptivity. Fertility and sterility 99, 508–517.
Chan, C. et al. Discovery of biomarkers of endometrial receptivity through a minimally invasive approach: a validation study with implications for assisted reproduction. Fertility and sterility 100, 810–817.
Haouzi, D. et al. Identification of new biomarkers of human endometrial receptivity in the natural cycle. Human reproduction 24, 198–205.
Horcajadas, J. A. et al. Global gene expression profiling of human endometrial receptivity. Journal of reproductive immunology 63, 41–49.
Koot, Y. E. et al. An endometrial gene expression signature accurately predicts recurrent implantation failure after IVF. Sci Rep 6, 19411.
Diaz-Gimeno, P. et al. A genomic diagnostic tool for human endometrial receptivity based on the transcriptomic signature. Fertility and sterility 95, 50–60, 60 e51-15.
Garrido-Gomez, T. et al. Profiling the gene signature of endometrial receptivity: clinical results. Fertility and sterility 99, 1078–1085.
Noyes, R. W., Hertig, A. T. & Rock, J. Dating the endometrial biopsy. American journal of obstetrics and gynecology 122, 262–263 (1975).
Lessey, B. A. The pathologists are free to go, or are they? Fertility and sterility 99, 350–351.
Lessey, B. A., Castelbaum, A. J., Sawin, S. W. & Sun, J. Integrins as markers of uterine receptivity in women with primary unexplained infertility. Fertility and sterility 63, 535–542 (1995).
Brosens, J. J. et al. Uterine selection of human embryos at implantation. Sci Rep 4, 3894.
Ruiz-Alonso, M. et al. The endometrial receptivity array for diagnosis and personalized embryo transfer as a treatment for patients with repeated implantation failure. Fertility and sterility 100, 818–824.
Horcajadas, J. A. et al. Effect of controlled ovarian hyperstimulation in IVF on endometrial gene expression profiles. Molecular human reproduction 11, 195–205.
Luna, J. J. et al. Gene expression pattern and immunoreactive protein localization of LGR7 receptor in human endometrium throughout the menstrual cycle. Molecular human reproduction 10, 85–90 (2004).
Goldsworthy, M. et al. Haploinsufficiency of the Insulin Receptor in the Presence of a Splice-Site Mutation in Ppp2r2a Results in a Novel Digenic Mouse Model of Type 2 Diabetes. Diabetes 65, 1434–1446.
Thorpe, C. T. et al. Anatomical heterogeneity of tendon: Fascicular and interfascicular tendon compartments have distinct proteomic composition. Sci Rep 6, 20455.
Cox, J. et al. Accurate proteome-wide label-free quantification by delayed normalization and maximal peptide ratio extraction, termed MaxLFQ. Mol Cell Proteomics 13, 2513–2526.
Hood, B. L. et al. Proteomics of the human endometrial glandular epithelium and stroma from the proliferative and secretory phases of the menstrual cycle. Biology of reproduction 92, 106.
Gonzalez-Begne, M. et al. Proteomic analysis of human parotid gland exosomes by multidimensional protein identification technology (MudPIT). J Proteome Res 8, 1304–1314.
Buhring, H. J., Streble, A. & Valent, P. The basophil-specific ectoenzyme E-NPP3 (CD203c) as a marker for cell activation and allergy diagnosis. Int Arch Allergy Immunol 133, 317–329.
Meerson, N. R. et al. Intracellular traffic of the ecto-nucleotide pyrophosphatase/phosphodiesterase NPP3 to the apical plasma membrane of MDCK and Caco-2 cells: apical targeting occurs in the absence of N-glycosylation. J Cell Sci 113 Pt 23, 4193–4202 (2000).
Bollen, M., Gijsbers, R., Ceulemans, H., Stalmans, W. & Stefan, C. Nucleotide pyrophosphatases/phosphodiesterases on the move. Crit Rev Biochem Mol Biol 35, 393–432.
Jin-Hua, P., Goding, J. W., Nakamura, H. & Sano, K. Molecular cloning and chromosomal localization of PD-Ibeta (PDNP3), a new member of the human phosphodiesterase I genes. Genomics 45, 412–415.
Stefan, C., Jansen, S. & Bollen, M. NPP-type ectophosphodiesterases: unity in diversity. Trends Biochem Sci 30, 542–550.
Korekane, H. et al. Identification of ectonucleotide pyrophosphatase/phosphodiesterase 3 (ENPP3) as a regulator of N-acetylglucosaminyltransferase GnT-IX (GnT-Vb). The Journal of biological chemistry 288, 27912–27926.
Genbacev, O. D. et al. Trophoblast L-selectin-mediated adhesion at the maternal-fetal interface. Science 299, 405–408.
Ghosh, D., Liu, N., Zhu, Z. M. & Sengupta, J. Immunolocalization of Le(y) oligosaccharide in endometrium during menstrual cycle and effect of early luteal phase mifepristone administration on its expression in implantation stage endometrium of the rhesus monkey. Human reproduction 13, 1374–1379 (1998).
Gipson, I. K. et al. MUC16 is lost from the uterodome (pinopode) surface of the receptive human endometrium: in vitro evidence that MUC16 is a barrier to trophoblast adherence. Biology of reproduction 78, 134–142.
Lalitkumar, S. et al. Polyethylene glycated leukemia inhibitory factor antagonist inhibits human blastocyst implantation and triggers apoptosis by down-regulating embryonic AKT. Fertility and sterility 100, 1160–1169.
Lalitkumar, P. G. et al. Mifepristone, but not levonorgestrel, inhibits human blastocyst attachment to an in vitro endometrial three-dimensional cell culture model. Human reproduction 22, 3031–3037.
Cox, J. & Mann, M. MaxQuant enables high peptide identification rates, individualized p.p.b.-range mass accuracies and proteome-wide protein quantification. Nature biotechnology 26, 1367–1372.
Remmele, W. & Stegner, H. E. Recommendation for uniform definition of an immunoreactive score (IRS) for immunohistochemical estrogen receptor detection (ER-ICA) in breast cancer tissue. Pathologe 8, 138–140 (1987).
Acknowledgements
The authors are grateful to researchers Eva Broberg (midwife/coordinator) and Dr Ingrid Sääv, Karolinska University Hospital and Karolinska Institutet, Stockholm Sweden, for their help with endometrial biopsies and care of the subjects. This study was funded by the Swedish Research Council (K2013-54X-14212-12-5), Joint grant from Stockholm County Council and Karolinska University Hospital (ALF). S.K. and A.S. were supported by the Estonian Ministry of Education and Research (IUT34-16), Enterprise Estonia (EU48695) and Horizon 2020 innovation programme (WIDENLIFE, 692065). A joint grant was received from European Union’s FP7 Marie Curie Industry-Academia Partnerships and Pathways (IAPP, SARM, EU324509) for this study.
Author information
Authors and Affiliations
Contributions
N.R.B. designed, performed experiments, interpreted the results, prepared the manuscript draft. S.L. designed, performed experiments, interpreted the results, wrote and edited the manuscript draft. V.J.B. performed the microarray analysis, edited the manuscript. S.K. and A.S. did the MS studies and edited the manuscript. P.G.L. designed the study, performed experiments, interpreted the results, edited the manuscript with critical intellectual input, responsible for experimental work and co-funded the study. K.G.D. designed the study, collected samples, gave intellectual comments, edited the manuscript with critical input, funded the study and was overall responsible for the study.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Electronic supplementary material
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Boggavarapu, N., Lalitkumar, S., Joshua, V. et al. Compartmentalized gene expression profiling of receptive endometrium reveals progesterone regulated ENPP3 is differentially expressed and secreted in glycosylated form. Sci Rep 6, 33811 (2016). https://doi.org/10.1038/srep33811
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep33811
This article is cited by
-
Comparative transcriptome analysis of the human endocervix and ectocervix during the proliferative and secretory phases of the menstrual cycle
Scientific Reports (2019)
-
Crystal structure and substrate binding mode of ectonucleotide phosphodiesterase/pyrophosphatase-3 (NPP3)
Scientific Reports (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.