Abstract
Aberrant immune responses to environmental allergens including insect allergens from house dust mites and cockroaches contribute to allergic inflammatory diseases such as asthma in susceptible individuals. Airway epithelial cells (AECs) play a critical role in this process by sensing the proteolytic activity of allergens via protease-activated receptors (PAR2) to initiate inflammatory and immune responses in the airway. Elevation of cytosolic Ca2+ is an important signaling event in this process, yet the fundamental mechanism by which allergens induce Ca2+ elevations in AECs remains poorly understood. Here we find that extracts from dust mite and cockroach induce sustained Ca2+ elevations in AECs through the activation of Ca2+ release-activated Ca2+ (CRAC) channels encoded by Orai1 and STIM1. CRAC channel activation occurs, at least in part, through allergen mediated stimulation of PAR2 receptors. The ensuing Ca2+ entry then activates NFAT/calcineurin signaling to induce transcriptional production of the proinflammatory cytokines IL-6 and IL-8. These findings highlight a key role for CRAC channels as regulators of allergen induced inflammatory responses in the airway.
Similar content being viewed by others
Introduction
Asthma is a heterogeneous disease arising from a complex interplay of genetic, epigenetic and environmental factors and is believed to affect over 300 million people worldwide1,2. The disease is characterized by varying levels of bronchoconstriction, airway remodeling and infiltration of a variety of immune cells including eosinophils, basophils and CD4+ T cells, leading to chronic airway inflammation3,4. Atopy, which refers to allergic sensitization to inhaled allergens such as house dust mites, cockroaches, fungi, pollen and animal dander, is widely associated with asthma1,3. These allergens activate numerous signaling pathways through a variety of cell surface receptors that include the protease activated receptor type 2 (PAR2), promoting sensitization and culminating in exaggerated inflammatory effector responses1,5. Elucidation of these signaling cascades is incomplete but remains a major goal of current efforts for identifying new targets for blocking the inflammatory response.
Among the numerous immune and structural cells implicated in the allergen response, airway epithelial cells (AECs) are thought to play an early role in the process through direct interactions with allergens. Located at the interface of the host and the environment, AECs act not only as a mechanical barrier and a first line of defense against inhaled allergens, but also play a vital role in their early recognition and response using pattern recognition receptors such as toll-like receptors (TLRs) and PARs6,7. Following exposure to allergens, AECs produce inflammatory mediators that activate innate lymphocytic cells, prime dendritic cells to induce Th2 responses from T cells, and induce the production of IL-13 from T cells3,7 thus helping to shape the multistage immune response seen in asthma. For example, house dust mite (HDM) allergens induce the release of cytokines eotaxin, GM-CSF, CCL2, CCL20, IL-6 and IL-8; cockroach allergens have been shown to induce IL-6, IL-8 and GM-CSF and fungal allergens such as Alternaria have been implicated in the release of IL-6, GM-CSF and IL-33 from AECs8,9,10,11,12,13. However, the molecular mechanisms by which these factors are generated and released by AECs are not well-understood. In particular, many if not most allergens induce cytosolic Ca2+ elevations in AECs, which in principle could drive transcriptional and enzymatic cascades to induce cytokine production9,12,13,14. However, it is not clear whether allergen induced cytosolic Ca2+ fluxes arise primarily due to Ca2+ release from internal stores or if they also involve activation of specific Ca2+ channels on the plasma membrane. Given recent evidence implicating Ca2+ signaling in multiple effector functions in AECs15,16, a clear understanding of how AECs generate Ca2+ signals in response to allergens is needed to better understand how cytokine signaling pathways are induced in AECs and to translate this knowledge in the quest for identifying novel targets for therapy.
Store-operated Ca2+ release-activated Ca2+ (CRAC) channels are the primary mechanism for producing cytosolic Ca2+ elevations in many non-excitable cells17. CRAC channels are encoded by the Orai genes (Orai1-3) and activated by the ER Ca2+ sensors, STIM1-217,18,19,20. Mechanistically, it is now known that STIM1 and STIM2 sense the [Ca2+]ER, and, in response to ER Ca2+ store-depletion, translocate to the junctional ER to physically interact with Orai channels resulting in CRAC channel gating17,21. The resulting Ca2+ influx regulates a variety of functions including gene expression, cell proliferation and differentiation in many types of cells17,21.
We and others have shown that CRAC channels are a major mechanism for eliciting Ca2+ signals in AECs and are activated in response to PAR2 stimulation15,16. The ensuing Ca2+ elevation regulates the production of key inflammatory cytokines including IL-6, IL-8, and TSLP15. Given that many inhaled allergens produce Ca2+ elevations in AECs and are thought to mediate their inflammatory effects, at least in part, by stimulating PAR2 receptors9,11,12,13, we sought to investigate whether CRAC channels contribute to the downstream response to allergens in bronchial BEAS-2B cells9,11,12,13. We report here that cockroach and dust mite allergens activate CRAC channels through stimulation of PAR2 receptors. The ensuing Ca2+ signal induces the generation of IL-6 and IL-8. These results highlight an important role for CRAC channels as key regulators for early activation of allergic inflammation in AECs.
Results
A screen of allergen extracts reveals insect allergens as activators of store-operated Ca2+ entry in bronchial epithelial cells
Many studies have shown that allergen extracts from insects (HDM and cockroach) and fungi (Alternaria, Aspergillus) induce cytosolic Ca2+ signals in AECs8,13,22. A multitude of factors including activation of PAR28 or other proteolytic receptors and ATP induction23 have been implicated in the genesis of these Ca2+ signals, yet it is not clear whether they primarily arise due to Ca2+ release from internal stores or if they additionally involve Ca2+ influx across the plasma membrane. We and others have previously shown that store-operated calcium entry (SOCE) is a major mechanism of Ca2+ influx in bronchial epithelial cells and is stimulated by activation of PAR2 receptors15,16. However, whether allergens can activate CRAC channels in AEC is unknown. We therefore tested the ability of various allergen extracts to activate SOCE in bronchial BEAS-2B cells using fura-2 based Ca2+ imaging (Table 1). Specific allergens including HDM, cockroach extracts, chitinase from Streptomyces griseus and fungal extracts from Alternaria and Aspergillus were applied in a Ca2+-free medium followed by re-addition of extracellular Ca2+ to detect SOCE. This screen revealed that only a subset of allergens tested, limited to extracts from HDM and cockroach allergens, and, to a lesser extent, chitinase from Streptomyces griseus, activated store-operated Ca2+ signals and Ca2+ entry across the plasma membrane in the AECs (Table 1).
Cockroach extracts induce Ca2+ signals in AEC by activating CRAC channels
There is a strong correlation between sensitization and allergy to inhaled cockroach extracts and the incidence of acute asthmatic attacks24,25. In vitro and in vivo studies have shown that extracts from cockroach have proteinase activity and stimulate PAR2 receptors to mediate their inflammatory effects9,10. Induction of cytosolic Ca2+ fluxes in response to cockroach extracts has been shown in alveolar A549 cells26, cultured human keratinocytes27 and KNRK cells, a rat kidney cell line10. However, the pathways mediating these Ca2+ fluxes are unknown. We found that administration of cockroach extract to BEAS-2B cells in a 2 mM Ca2+ Ringer’s solution produced a biphasic rise in cytoplasmic Ca2+: a rapid initial spike followed by sustained Ca2+ signals that lasted more than 10 minutes (Fig. 1A). In most cells, the sustained component of the Ca2+ response consisted of an elevated baseline with an oscillating component superposed on the baseline. The sustained signals elicited by cockroach extract were almost completely abolished in a Ca2+ free Ringer’s solution, suggesting that Ca2+ influx across the plasma membrane was needed for this Ca2+ signal (Fig. 1B). Moreover, the CRAC channel inhibitor, BTP2, significantly inhibited both the plateau Ca2+ signals as well as the oscillating component (Fig. 1C), indicating that the sustained Ca2+ signals arise from the opening of CRAC channels. Fig. 1A–C show traces from individual cells, whereas the average [Ca2+]i changes and the integrated area under the curve during the time period of allergen treatment are summarized in Fig. 1D–F. To confirm the inhibitory effects of BTP2 on CRAC channel activation in BEAS-2B cells more directly, we activated SOCE using thapsigargin, a SERCA pump inhibitor that irreversibly depletes ER Ca2+ stores. SOCE was significantly inhibited by BTP2 at the same concentration that was used to inhibit allergen induced Ca2+ signal (Fig. 1G,H). Based on these results, we conclude that cockroach extracts induce long lasting Ca2+ signals in bronchial epithelial cells by activating SOCE through CRAC channels.
(A–C) [Ca2+i] imaging showing responses of individual BEAS-2B cells to cockroach allergen extracts (10 μg/mL) administered in (A) 2 mM Ca2+ ringer’s solution, (B) Ca2+ free ringer’s solution or (C) 2 mM Ca2+ ringer’s solution in the presence of the CRAC channel inhibitor BTP2 (500 nM). (D) Average [Ca2+i] response of the individual cells shown in (A–C). (E–F) Summary of the average rise in [Ca2+i] 600 seconds after addition of cockroach extract (E) and the integral of the [Ca2+]i signal during application of the allergen. (F). (G) Ca2+ imaging trace showing SOCE in BAES-2B cells. SOCE was induced by depleting ER Ca2+ stores with 1 µM thapsigargin in a Ca2+-free Ringer’s solution and readding 2 mM Ca2+ following store depletion. Pre-treating cells with BTP2 (500 nM) strongly inhibits SOCE. (H) Summary of average rise in cytosolic Ca2+ levels 200 seconds after re-addition of 2 mM Ca2+ ringer’s following store-depletion. Data are mean ± SEM of 34-47 cells. Representative of 5 independent experiments. **P < 0.01, ***P < 0.001, Ck. Ext, cockroach extract.
STIM1 and Orai1 mediate cockroach extract induced Ca2+ entry in bronchial epithelial cells
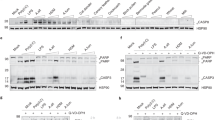
We have previously shown in AECs that SOCE is mediated by the CRAC channel proteins, STIM1 and Orai115. Knockdown of STIM1 and Orai1 using siRNA reduced expression of these proteins (Fig. 2A and Supplementary Fig. S1) and significantly reduced the amplitude of Ca2+ elevation induced by cockroach extract (Fig. 2B). Both the average amplitude of Ca2+ signal and the integrated Ca2+ signal over time was significantly attenuated in siSTIM1 and siOrai1 treated cells (Fig. 2C,D). Knockdown of STIM1 by siStim1 showed good specificity and did not have any effect on STIM2 expression (Supplementary Fig. S1). Interestingly, analysis of single cell Ca2+ responses revealed that a proportion of cells in both siSTIM1 and siOrai1 treated samples showed Ca2+ oscillations (Fig. 2F,G). It is likely that, given the incomplete knockdown of STIM1 and Orai1 by siRNA (Fig. 2A), these oscillatory signals are mediated by the residual CRAC channel machinery. In contrast, cells treated with the siRNA control showed a more heterogeneous response with individual cells showing a sustained increase in Ca2+ signal with oscillatory Ca2+ signals riding on top of the elevated baseline, which accounted for the higher average Ca2+ response (Fig. 2E). We also note that the average Ca2+ elevation in response to cockroach extracts seen in siControl treated cells was lower than in untransfected control cells (Fig. 1D) likely due to the cell stress induced by cell transfection with lipofectamine. Taken together, these results demonstrate that STIM1 and Orai1 make essential contributions to the Ca2+ elevations in AECs following exposure of the cells to cockroach extracts.
(A) Western blot showing STIM1 and Orai1 expression in BEAS-2B cells and the effects of siRNA knockdown of STIM1 or Orai1. (B) Ca2+ traces showing the effects of siRNA knockdown of STIM1 and Orai1 on cockroach allergen-induced Ca2+ signals. A scrambled siRNA sequence was used as control. (C,D) Summary of average cytosolic Ca2+ levels 798 seconds after addition of cockroach allergen extract (8 μg/mL) (C) and the integral [Ca2+] signal following addition of cockroach extract (D). (E–G) Ca2+ imaging traces of individual cells treated with either a scrambled control siRNA (E) or siRNA against Stim1 (F) or Orai1 (G) showing effects of the knockdown on cockroach allergen-induced Ca2+ signals. Data are mean ± SEM of 29–38 cells. Representative of 3 independent experiments. **P < 0.01.
Dust mite extracts induce Ca2+ signals in AECs by activating CRAC channels
Previous studies have shown that exposure to HDM can trigger allergic inflammation in asthmatic patients1,28,29. Components of HDM, including Der p1, Der p3 and Der p9 exhibit proteolytic activity that leads to activation of PAR2 receptors, which in turn plays a critical role in mediating the inflammatory effects of HDM8,30. HDM has also been shown to activate Ca2+ signals in airway epithelial cells in both primary epithelial cells and cell lines, and this is believed to occur through both PAR2-dependent and -independent mechanisms8,30,31. However, whether HDM can activate CRAC channels has not been studied. When administered in a Ca2+-free Ringer’s solution, HDM induced only a transient Ca2+ signal indicating that the extract causes Ca2+ release from internal stores (Supplementary Fig. S2). In the presence of extracellular Ca2+, however, HDM extracts activated a sustained Ca2+ signal in BEAS-2B cells that was inhibited by the CRAC channel inhibitor BTP2 (Fig. 3A–C, Supplementary Fig. S2). Further, knockdown of the CRAC channel proteins STIM1 and Orai1 significantly abrogated the average sustained Ca2+ signals seen in response to HDM (Fig. 3D–F). These results indicate that HDM allergens mobilize cellular Ca2+ elevations in bronchial epithelial cells by depleting ER Ca2+ stores and activating CRAC channels encoded by STIM1 and Orai1.
(A) HDM extract (nDerP, 18 μg/mL) induces a cytosolic Ca2+ signal that is blocked by BTP2. (B,C) Summary of the average rise in [Ca2+i] 200 seconds after addition of HDM extract (B) and the integral Ca2+ signal (D–F) Knockdown of STIM1 or Orai1 inhibits nDerP induced Ca2+ signals. (D) Average trace showing the effects of siRNA mediated knockdown of STIM1 and ORAI1 on HDM allergen-induced Ca2+ signals. Summary of (E) average cytosolic Ca2+ levels 540 seconds after addition of dust mite allergen extract and (F) integrated Ca2+ signal. Data are mean ± SEM of 32–57 cells. Representative of 3–5 independent experiments. **P < 0.01, ***P < 0.001, nDerP, dust mite extract.
Insect allergens mobilize Ca2+ signals by activating PAR2 receptors
Both HDM and cockroach allergens have been shown to activate PAR2 receptors on airway epithelial cells1,9,30,31. Whether this is the primary mechanism by which cellular Ca2+ signals are generated remains a contentious issue, with evidence for both PAR2 dependent and independent mechanisms8,30. We therefore studied the effect of siRNA mediated PAR2 receptor knockdown on allergen induced Ca2+ influx. Cytosolic Ca2+ elevations in response to type IX trypsin, a well characterized PAR2 agonist, was strongly inhibited in the siRNA treated cells, confirming knockdown of PAR2 in these cells (Fig. 4A–C). Importantly, Ca2+ influx seen in response to cockroach allergens was also significantly inhibited in siPAR2 treated cells, indicating that cockroach extracts induced Ca2+ signals by activating PAR2 receptors (Fig. 4D–F). This conclusion is further supported by the Ca2+ responses seen following paired application of the allergen and the PAR2 specific agonist, trypsin. Following application of the cockroach extract, administration of trypsin failed to elicit a Ca2+ signal, suggesting that trypsin and cockroach extract activate the same signal transduction pathway, and prior desensitization of the PAR2 receptor or immediate downstream signaling attenuates the response to a second challenge to PAR2 (Fig. 4G). By contrast, Ca2+ mobilization in response to P2Y receptor activation by UTP (therefore PAR2-independent) was unaffected following prior treatment with the allergen. Likewise, pre-application of the PAR2 agonist trypsin impaired a subsequent Ca2+ response to cockroach allergen but not to UTP. (Fig. 4H). These results are consistent with the interpretation that cockroach allergens activate PAR2 receptors in AECs. However, in contrast to the effects of the cockroach extracts, knockdown of PAR2 elicited only modest inhibition of the Ca2+ response to dust mite extract (Fig. 4I–K). This result suggests that the Ca2+ response to dust mite extracts is mediated by both PAR2-dependent as well as independent mechanisms.
(A–C) The PAR2 agonist type IX trypsin (50 nM) mobilizes [Ca2+]i in BEAS-2B cells. This [Ca2+]i elevation is suppressed by siRNA knockdown of PAR2. (B). Summary of the average cytosolic [Ca2+] rise 150 seconds after addition of trypsin. Summary of the integral Ca2+ signal following application of trypsin. (D–F) Ca2+ responses to cockroach allergen (8 μg/mL) in cells treated with siControl or siPAR2. (E) Summary of the average [Ca2+] rise 100 seconds after addition of cockroach extract. Summary of the integrated Ca2+ signal following application of the extract. (G,H) Paired application of the PAR2 agonist trypsin and cockroach allergen shows that prior activation of PAR2 by trypsin diminishes the subsequent allergen response and vice versa. Subsequent response to a non-PAR2 agonist, UTP, is unaffected suggesting that the lack of response in the paired application is not due to depletion of ER-stores but rather due to receptor desensitization. (I–K) Response to dust mite allergens is partially inhibited by knockdown of PAR2. Mean ± SEM of 21–43 cells, 2 experiments. *P < 0.05, **P < 0.01; Tryp, trypsin.
Ca2+ responses to fungal and bacterial allergens
The ability of cockroach and dust mite extracts to stimulate SOCE led us to next consider whether this Ca2+ influx pathway might be a common feature of other allergenic pathways. Chitinase enzyme from fungal and insect sources has been implicated in airway inflammation and elevated expression of a mammalian chitinase enzyme has been noted in mouse models of asthma and in allergic asthma in humans22. Moreover, Hong et al. have noted that Chitinase stimulates Ca2+ flux in airway epithelial cells through a mechanism likely involving PAR2 receptors22. We found that chitinase extracts from Streptomyces griseus produced oscillatory Ca2+ signals in a significant fraction of BEAS-2B cells (Fig. 5A). These Ca2+ signals were inhibited by exposing cells to BTP2, suggesting that, like cockroach and HDM extracts, chitinase activates CRAC channels in AECs (Fig. 5A–C).
(A–C) Chitinase from Streptomyces griseus (30 μg/mL) induces oscillatory Ca2+ signal that is blocked by BTP2. (D–G) Effect of Alternaria alternata extracts on Ca2+ signaling in AECs (D) Alternaria alternata extracts (30 μg/mL) induce cytosolic Ca2+ elevations in AECs that is not blocked by BTP2 (E). (F) Summary of average Ca2+ rise at the 900 second time point. (G) Alternaria alternata extracts (30 μg/mL) do not cause ER store-release. (H,I) Extracts from Aspergillus fumigatus high molecular weight fraction (10 μg/mL) (H) and low molecular weight fraction (10 μg/mL) (I) fail to induce Ca2+ signals in BEAS-2B cells. (N = 17–34 cells, Mean ± SEM of 3 experiments). *P < 0.05, **P < 0.01 *P < 0.05, Alt, Alternaria alternata; Asp, Aspergillus fumigata; HMW, high molecular weight fraction; LMW. Low molecular weight fraction.
Allergens derived from the fungus Alternaria alternata have been shown to trigger a Th2 type response through the release of IL-33 from airway epithelial cells in a Ca2+ dependent manner32,47. Alternaria also induces the production of IL-6, IL-8 and GM-CSF from AEC13. We found that following treatment with Alternaria extracts, BEAS-2B cells showed a slow but progressive increase in their [Ca2+]i levels at concentrations of 30 μg/mL or above (Fig. 5D). However, this increase was not affected by pre-treatment with BTP2, ruling out involvement of CRAC channels in this process (Fig. 5E,F). Furthermore, Alternaria extracts did not evoke release of Ca2+ from internal stores (Fig. 5G). We did not observe concomitant reduction of fura 340 and 380 signal following addition of the fungal extracts, ruling out the possibility of proteolytic cell damage. These results indicate that the slow [Ca2+]i rises evoked by Alternaria extracts do not involve CRAC channels.
Another fungus that is commonly associated with inflammatory lung diseases including asthma, allergic sinusitis, bronchopulmonary aspergillosis, and chronic eosinophilic pneumonitis, is Aspergillus fumigatus33. Although some studies have implicated cross-talk between TLRs and PAR2 receptors in the response to this fungus, the basic mechanisms by which Aspergillus fumigatus triggers airway inflammation remain largely unknown. In our tests, neither low nor high molecular weight fractions of extracts from Aspergillus fumigatus induced Ca2+ signals in bronchial BEAS-2B cells (Fig. 5H,I). Thus, the ability of Aspergillus fumigatus extracts to modulate signaling pathways in AECs including inhibition of Jak-Stat signaling33 is likely not mediated by CRAC channels. Overall, these results suggest that the activation of Ca2+ influx through CRAC channels is confined to a specific subset of insect allergens that include cockroach, dust mites, and chitinase enzyme.
Dust mite and cockroach allergens induced generation of IL-6 and IL-8 through activation of CRAC channels
An important consequence of allergen sensing by the airways is the induction of pro-inflammatory mediators such as IL-6 and IL-8, which leads to the recruitment of various immune cells to the airway9,10,12. IL-8 plays an important role in the recruitment of neutrophils to the site of airway injury whereas IL-6 is a pleiotropic cytokine that is critical for B cell differentiation as well as T cell activation34. We found that exposure of BEAS-2B cells to cockroach allergens or HDM extracts resulted in the induction of IL-6 and IL-8 both at 6 and 24 hour time points (Fig. 6A–H). The induction of these cytokines was abolished by the CRAC channel antagonist, BTP2, indicating that Ca2+ entry through CRAC channels is essential for the generation of these cytokines (Fig. 6A–H). This result is consistent with our previous report demonstrating that activation of PAR2 receptors leads to induction of IL-6 and IL-8 in a CRAC channel dependent manner15. Moreover, cyclosporine A, a calcineurin inhibitor, impaired the generation of IL-6 and IL-8 following challenge by allergens, indicating that calcineurin/NFAT signaling is critical for the induction of IL-6 and IL-8 by allergens (Fig. 6A–H)35. Together, these results indicate that insect allergens stimulate the production of IL-6 and IL-8 via NFAT dependent gene expression that is driven by Ca2+ entry through CRAC channels.
(A–H) BEAS-2B cells were treated with cockroach (10 μg/mL) or and dust mite (18 μg/mL) allergen extracts for 6 or 24 hours. Cells were pre-treated with the CRAC channel inhibitor, BTP2 (500 nM) or the calcineurin inhibitor cyclosporine A (CsA, 500 nM) for 45 minutes before allergen treatment. After allergen treatment, cell culture supernatants were collected and examined for IL-6 and IL-8 using ELISA. Mean ± SEM of 2–3 experiments with three replicates for each expeirment. *P < 0.05, **P < 0.01.
Discussion
Interactions between common allergens found in ambient air such as insect (house dust mites, cockroach) or fungal (Aspergillus, Alternaria) allergens and the airway epithelium underlie the development of airway inflammation seen in allergic diseases like asthma36,37. The biological effect of these allergens is mediated, in part, by proteolytic activity contained within them, which produces epithelial cell damage and activates protease activated receptors to trigger signaling cascades that lead to production of several key inflammatory mediators from AECs5. A key signaling event in allergen induced cell signaling is the elevation in cytosolic Ca2+, which has been proposed to occur through both PAR2 dependent and independent pathways10,11,12,30. However, the specific Ca2+ entry pathways that mediate allergen-evoked Ca2+ signals have not been determined. In this study, we show that insect allergens derived from cockroach and dust mite extracts activate CRAC channels in bronchial epithelial cells. CRAC channel activation occurs, at least in part, through stimulation of PAR2 receptors and mediates an important role in the induction of the inflammatory modulators IL-6 and IL-8.
Our primary finding is that cockroach and dust mite allergens induce sustained and oscillatory Ca2+ signals in bronchial BEAS-2B cells by activating CRAC channels. Both pharmacological inhibition by BTP2 and knockdown of the canonical CRAC channel proteins STIM1 and Orai1 significantly abrogated insect allergen induced Ca2+ signals (Figs 2 and 3). For both allergens, while the sustained component of the Ca2+ signal was completely inhibited in Ca2+ free buffer (Fig. 1B and data not shown), some residual Ca2+ influx persisted in cells in which STIM1 and Orai1 were knocked down (Figs 2F and 3D). This is most likely due to the incomplete knockdown of CRAC channel proteins as seen in the Western blot (Fig. 2A). However, we cannot rule out that the possibility that other CRAC channel proteins (STIM2, Orai2, 3) also make some contribution to the allergen-induced Ca2+ signals. Interestingly, while the average [Ca2+]i rise following stimulation with cockroach extracts was lower in siSTIM1 and siOrai1 treated cells, a fraction of these cells showed Ca2+ oscillations (Fig. 2F,G). The specific nature of Ca2+ signals is often determined by complex interactions between the agonist, agonist receptor, IP3 receptors and Ca2+ channels38. It is possible that the reduced Ca2+ influx in the siSTIM1 and siOrai1 treated cells fundamentally affected feedback to IP3 receptors and changed the nature of Ca2+ signals to the oscillatory type. It would be interesting to test if the sustained Ca2+ signals seen in response to cockroach and dust mite allergens become oscillatory in nature when the concentration of the allergens is reduced in the external media, as has been shown for other agonists like ATP39. If true, this could have important implications for downstream signaling. For example, depending on the concentration of inhaled allergens in the airway, AEC might produce either oscillatory or sustained Ca2+ signals, with each producing a distinct biological response.
Several studies have established a role for PAR2 receptors in the induction of Ca2+ signals in response to cockroach and dust mite allergens9,10,12,40. While components of dust mite allergens such as Der p3 and Der p5 induce Ca2+ signals in kidney and alveolar epithelial cell lines through PAR2 receptors, other components such as Der p1 do not activate Ca2+ signals8,30. We found that knockdown of PAR2 receptors significantly inhibited Ca2+ signals in response to both cockroach and dust mites, though the inhibition of Ca2+ signal was incomplete, likely due to incomplete knockdown of the PAR2 protein (Fig. 4). However, given that the dust mite extract likely contains a combination of several serine proteases, and possibly many other undefined proteins, it is possible that additional PAR2 independent mechanisms also mediate the observed elevation of cellular Ca2+ signals. Future studies that examine the Ca2+ responses to specific purified or recombinant dust mite proteases (e.g., Der p1, 3, 5 and 9) will help to discern the contributions of precise components of the dust mite extracts to the observed Ca2+ signals.
Interestingly, we failed to detect the involvement of CRAC channels in the Ca2+ elevation evoked by extracts of the Alternaria fungus. A previous study that used a high concentration of Alternaria extracts (200 μg/mL) found that the extracts cause Ca2+ elevations acting through the autocrine stimulation of purinergic receptors by ATP23. Here, we employed a lower concentration of the extract (30 μg/mL) and found that while the extract induced Ca2+ elevations in the presence of extracellular Ca2+, no response occurred in Ca2+-free Ringer’s buffer, arguing against activation of purinergic receptors, at least in the concentration range we tested. Moreover, the observed Ca2+ influx seen in the presence of extracellular Ca2+ was not dependent on CRAC channels as the CRAC channel inhibitor BTP2 had no effect. These results indicate that Alternaria evokes Ca2+ influx through other Ca2+ influx pathways whose identity remains to be determined.
In conclusion, we provide evidence showing that bronchial epithelial cells sense cockroach and dust mite allergens through the activation of cell surface PAR2 receptors, which in turn leads to the opening of store-operated CRAC channels. The ensuing Ca2+ signal is known to play an important role in the induction of the cytokines IL-6 and IL-8 through an NFAT dependent mechanism. These results demonstrate that CRAC channels may have a central role as effectors of allergen signaling in the airway epithelium.
Methods
Cells and media
The bronchial epithelial cell line BEAS-2B, a kind gift from Curtis C. Harris (National Cancer Institute), was cultured in DMEM/F12 medium (CellGro) containing 5%FBS (Hyclone), 50 U/mL penicillin and 50 mg/mL Streptomycin and was maintained at 37 °C and in 5% CO2. Cells from passage 44-51 were used for experiments.
Plasmids and transfections
siRNAs used to down regulate STIM1, STIM2, Orai1 and PAR2 protein expression along with scrambled siRNA negative control were purchased from Ambion, Life Technologies (SilencerSelect predesigned siRNA). siRNA constructs were transfected into BEAS-2B cells using Lipofectamine2000 (Invitrogen) according to manufacturer instructions. Cells were used for experiments 48–72 hours after transfection.
Reagents and chemicals
The standard extracellular Ringers solution had the following composition (in mM): 150 NaCl, 4.5 KCl, 10 D-glucose, 1 MgCl2, 2 CaCl2 and 5 Na-HEPES. pH was adjusted to 7.4 using NaOH. For the Ca2+ free Ringers solution, CaCl2 was excluded from the above composition and MgCl2 was increased to 3 mM. Stock solutions of BTP2, thapsigargin (TG) and cyclosporinA (CsA) were made in DMSO. PAR2-agonist type IX trypsin (Sigma) was constituted in water. Dust mite allergen extract (nDer p) was from Indoor Biotechnologies Inc, Charlottesville, VA. Cockroach extract was purchased from HollisterStier Allergy, Spokane, WA. CRAC channel inhibitor BTP2 was from Millipore, Billerica, MA. All other compounds were from Sigma Aldrich, St. Louis, MO.
Intracellular Ca2+ measurements
BEAS-2B cells were grown on poly-L lysine coated glass bottom dishes (MatTek Corp, Ashland, MA). Cells were loaded with 2.5 μM Fura-2 AM (Thermo Scientific Fisher, Waltham, MA) in DMEM/F12 and 5% FBS culture media for 40 minutes at room temperature. Excess fura2 was washed off and cells were incubated in media for an additional 10 minutes before imaging. Single cell [Ca2+]i measurements were done according to the protocol described previously41. Image acquisition and analysis was performed using IPLab (Scanalytics, Rockville, MD, USA) and Slidebook. For analysis, regions of interest were drawn around single cells and following background subtraction, the F340/F380 intensity ratio was obtained as a function of time. The ratios were converted to [Ca2+]I using the formula

where R is the F340/F380 fluoresce intensity ratio and Rmax (9.645) and Rmin (0.268) were determined by in-vitro calibration of FURA242. β (20.236) was determined from the Fmin/Fmax ratio at 380 nm and Kd is the apparent dissociation constant of fura-2 binding to Ca2+ (135 nM).
Western blots
BEAS-2B cells were cultured in 6-well plates. At 70% confluency, cells were washed with cold PBS and lysed in a solution containing 150 mM NaCl, 50 mM Tris, 1% Triton-X-100, 0.1% SDS and 1x Protease Inhibitor Cocktail (Sigma) for 45 minutes. Cell lysates were obtained using a cell scraper, lysates were spun down at 4 °C for 30 minutes and supernatants were collected and stored at −80 °C. For Western blotting, samples were heated to 99 °C for 5 minutes in Laemmli Sample Buffer (Bio-Rad) containing 0.1% β-mercaptoethanol, run on 10% SDS-PAGE gels, and transferred to nitrocellulose membrane. Orai1, STIM1, and STIM2 proteins were detected using an affinity purified polyclonal antibodies and peroxidase labelled secondary antibodies43,44.
Analysis of cytokine secretion
BEAS-2B cells were cultured on 24 well plates in DMEM/F12 media with 5% FBS. 24–48 hours later, cells were pre-treated with CRAC channel inhibitor BTP2 (500 nM) or calcineurin inhibitor Cyclosporin A (500 nM) for 45–60 min before being stimulated with dust mite and cockroach allergens for 6 or 24 hours. Supernatants were collected and stored at −80 deg. C. Levels of inflammatory mediators IL-6 and IL-8 was measured using ELISA kits (RayBiotech for IL-6, and LifeTechnologies for IL-8).
Data analysis
Average cytosolic Ca2+ traces and bar graphs summarizing the data are reported as mean ± SEM. For data sets involving more than two groups, initial statistical analysis was performed using ANOVA with a confidence interval of 5%. This was followed by two-tailed paired student t-test for comparing different treatment conditions within the set.
Additional Information
How to cite this article: Jairaman, A. et al. Allergens stimulate store-operated calcium entry and cytokine production in airway epithelial cells. Sci. Rep. 6, 32311; doi: 10.1038/srep32311 (2016).
References
Gandhi, V. D. & Vliagoftis, H. Airway epithelium interactions with aeroallergens: role of secreted cytokines and chemokines in innate immunity. Front. Immunol. 6, 147 (2015).
Olin, J. T. & Wechsler, M. E. Asthma: pathogenesis and novel drugs for treatment. BMJ 349, g5517 (2014).
Holgate, S. T. & Polosa, R. Treatment strategies for allergy and asthma. Nature Rev. Immunol. 8, 218–230 (2008).
Holtzman, M. J., Byers, D. E., Alexander-Brett, J. & Wang, X. The role of airway epithelial cells and innate immune cells in chronic respiratory disease. Nature Rev. Immunol. 14, 686–698 (2014).
Reed, C. E. & Kita, H. The role of protease activation of inflammation in allergic respiratory diseases. J. Allergy Clin. Immunol. 114, 997–1008 (2004).
Kato, A. & Schleimer, R. P. Beyond inflammation: airway epithelial cells are at the interface of innate and adaptive immunity. Curr. Opin. Immunol. 19, 711–720 (2007).
Lambrecht, B. N. & Hammad, H. The airway epithelium in asthma. Nature Med. 18, 684–692 (2012).
Kauffman, H. F., Tamm, M., Timmerman, J. A. & Borger, P. House dust mite major allergens Der p 1 and Der p 5 activate human airway-derived epithelial cells by protease-dependent and protease-independent mechanisms. Clin. Mol. Allergy 4, 5 (2006).
Wada, K., Matsuwaki, Y., Moriyama, H. & Kita, H. Cockroach induces inflammatory responses through protease-dependent pathways. Int. Arch. Allergy Immunol. 155, 135–141 (2011).
Arizmendi, N. G. et al. Mucosal allergic sensitization to cockroach allergens is dependent on proteinase activity and proteinase-activated receptor-2 activation. J. Immunol. 186, 3164–3172 (2011).
Kauffman, H. F., Tomee, J. F., van de Riet, M. A., Timmerman, A. J. & Borger, P. Protease-dependent activation of epithelial cells by fungal allergens leads to morphologic changes and cytokine production. J. Allergy Clin. Immunol. 105, 1185–1193 (2000).
Lee, K. E. et al. Regulation of German cockroach extract-induced IL-8 expression in human airway epithelial cells. Clin. Exp. Allergy 37, 1364–1373 (2007).
Matsuwaki, Y., Wada, K., White, T., Moriyama, H. & Kita, H. Alternaria fungus induces the production of GM-CSF, interleukin-6 and interleukin-8 and calcium signaling in human airway epithelium through protease-activated receptor 2. Int. Arch Allergy Immunol. 158, 19–29 (2012).
Asokananthan, N. et al. Activation of protease-activated receptor (PAR)-1, PAR-2, and PAR-4 stimulates IL-6, IL-8, and prostaglandin E2 release from human respiratory epithelial cells. J. Immunol. 168, 3577–3585 (2002).
Jairaman, A., Yamashita, M., Schleimer, R. P. & Prakriya, M. Store-Operated Ca2+ Release-Activated Ca2+ Channels Regulate PAR2-Activated Ca2+ Signaling and Cytokine Production in Airway Epithelial Cells. J. Immunol. 195, 2122–2133 (2015).
Samanta, K., Bakowski, D. & Parekh, A. B. Key role for store-operated Ca2+ channels in activating gene expression in human airway bronchial epithelial cells. PLoS One 9, e105586 (2014).
Prakriya, M. & Lewis, R. S. Store-Operated Calcium Channels. Physiol. Rev. 95, 1383–1436 (2015).
Liou, J. et al. STIM is a Ca2+ sensor essential for Ca2+-store-depletion-triggered Ca2+ influx. Curr. Biol.: CB 15, 1235–1241 (2005).
Parekh, A. B. Store-operated CRAC channels: function in health and disease. Nature reviews. Nature Rev. Drug Discov. 9, 399–410 (2010).
Prakriya, M. et al. Orai1 is an essential pore subunit of the CRAC channel. Nature 443, 230–233 (2006).
Hogan, P. G., Lewis, R. S. & Rao, A. Molecular basis of calcium signaling in lymphocytes: STIM and ORAI. Annu. Rev. Immunol. 28, 491–533 (2010).
Hong, J. H. et al. Chitinase activates protease-activated receptor-2 in human airway epithelial cells. Am. J. Respir. Cell Mol. Biol. 39, 530–535 (2008).
O’Grady, S. M. et al. ATP release and Ca2+ signalling by human bronchial epithelial cells following Alternaria aeroallergen exposure. J. Physiol. 591, 4595–4609 (2013).
Gelber, L. E. et al. Sensitization and exposure to indoor allergens as risk factors for asthma among patients presenting to hospital. Am. Rev. Respir. Dis. 147, 573–578 (1993).
Kang, B. C., Wilson, M., Price, K. H. & Kambara, T. Cockroach-allergen study: allergen patterns of three common cockroach species probed by allergic sera collected in two cities. J. Allergy Clin. Immunol. 87, 1073–1080 (1991).
Hong, J. H. et al. German cockroach extract activates protease-activated receptor 2 in human airway epithelial cells. J. Allergy Clin. Immunol. 113, 315–319 (2004).
Jeong, S. K. et al. Mite and cockroach allergens activate protease-activated receptor 2 and delay epidermal permeability barrier recovery. J. Invest. Derm. 128, 1930–1939 (2008).
Korsgaard, J. House-dust mites and asthma. A review on house-dust mites as a domestic risk factor for mite asthma. Allergy 53, 77–83 (1998).
Milian, E. & Diaz, A. M. Allergy to house dust mites and asthma. P. R. Health Sci. J. 23, 47–57 (2004).
Adam, E. et al. The house dust mite allergen Der p 1, unlike Der p 3, stimulates the expression of interleukin-8 in human airway epithelial cells via a proteinase-activated receptor-2-independent mechanism. J. Biol. Chem. 281, 6910–6923 (2006).
Post, S. et al. House dust mite-induced calcium signaling instigates epithelial barrier dysfunction and CCL20 production. Allergy 68, 1117–1125 (2013).
Snelgrove, R. J. et al. Alternaria-derived serine protease activity drives IL-33-mediated asthma exacerbations. J. Allergy Clin. Immunol. 134, 583–592.e586 (2014).
Bhushan, B. et al. Suppression of epithelial signal transducer and activator of transcription 1 activation by extracts of Aspergillus fumigatus. Am. J. Respir. Cell Mol. Biol. 53, 87–95 (2015).
Hirota, J. A. & Knight, D. A. Human airway epithelial cell innate immunity: relevance to asthma. Curr. Opin. Immunol. 24, 740–746 (2012).
Hogan, P. G., Chen, L., Nardone, J. & Rao, A. Transcriptional regulation by calcium, calcineurin, and NFAT. Genes Dev. 17, 2205–2232 (2003).
Baldacci, S. et al. Allergy and asthma: Effects of the exposure to particulate matter and biological allergens. Respir. Med. 109, 1089–1104 (2015).
Lambrecht, B. N. & Hammad, H. Allergens and the airway epithelium response: gateway to allergic sensitization. J. Allergy Clin. Immunol. 134, 499–507 (2014).
Dupont, G., Combettes, L., Bird, G. S. & Putney, J. W. Calcium oscillations. Cold Spring Harb. Perspect. Biol. 3, pii: a004226 (2011).
Evans, J. H. & Sanderson, M. J. Intracellular calcium oscillations induced by ATP in airway epithelial cells. Am. J. Physiol. 277, L30–41 (1999).
Page, K., Ledford, J. R., Zhou, P., Dienger, K. & Wills-Karp, M. Mucosal sensitization to German cockroach involves protease-activated receptor-2. Respir. Res. 11, 62 (2010).
McNally, B. A., Somasundaram, A., Yamashita, M. & Prakriya, M. Gated regulation of CRAC channel ion selectivity by STIM1. Nature 482, 241–245 (2012).
Grynkiewicz, G., Poenie, M. & Tsien, R. Y. A new generation of Ca2+ indicators with greatly improved fluorescence properties. J. Biol. Chem. 260, 3440–3450 (1985).
Gwack, Y. et al. Hair loss and defective T- and B-cell function in mice lacking ORAI1. Mol. Cell Biol. 28, 5209–5222 (2008).
Oh-Hora, M. et al. Dual functions for the endoplasmic reticulum calcium sensors STIM1 and STIM2 in T cell activation and tolerance. Nature Immunol. 9, 432–443 (2008).
Davidson, C. E. et al. Proteinase-activated receptor-2 activation participates in allergic sensitization to house dust mite allergens in a murine model. Clin. Exp. Allergy 43, 1274–1285 (2013).
Moretti, S. et al. The contribution of PARs to inflammation and immunity to fungi. Mucosal Immunol. 1, 156–168 (2008).
Kouzaki, H., Iijima, K., Kobayashi, T., O’Grady, S. M. & Kita, H. The danger signal, extracellular ATP, is a sensor for an airborne allergen and triggers IL-33 release and innate Th2-type responses. J. Immunol. 186, 4375–4387 (2011).
Acknowledgements
We would like to thank Tetsuya Homma from the Schleimer lab for help with reagents and members of the Prakriya lab for helpful discussions. This work was supported by NIH grant R01 NS057499 and funds from the Northwestern Skin Disease Research Center (SDRC) to M. Prakriya and in part by Grants R37HL068546 and U19AI106683 (Chronic Rhinosinusitis Integrative Studies Program (CRISP)), and by the Ernest S. Bazley Foundation to R. Schleimer. This work used resources of the Northwestern University Structural Biology Facility which is generously supported by NCI CCSG P30 CA060553.
Author information
Authors and Affiliations
Contributions
A.J. designed and performed research, analyzed data, and wrote the paper. C.H.M. designed research and performed research and analyzed the data. R.P.S. helped design research and contributed reagents and helped edit the paper. M.P. designed research, analyzed data, and wrote the paper. All authors read and approved the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Jairaman, A., Maguire, C., Schleimer, R. et al. Allergens stimulate store-operated calcium entry and cytokine production in airway epithelial cells. Sci Rep 6, 32311 (2016). https://doi.org/10.1038/srep32311
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep32311
This article is cited by
-
Gene expression of TMEM178, which encodes a negative regulator of NFATc1, decreases with the progression of asthma severity
Clinical and Translational Allergy (2019)
-
Cockroach protease allergen induces allergic airway inflammation via epithelial cell activation
Scientific Reports (2017)
-
Tight junctions in pulmonary epithelia during lung inflammation
Pflügers Archiv - European Journal of Physiology (2017)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.