Abstract
Flavonoids and lignans are polyphenol classes with anticarcinogenic activities against colorectal cancer (CRC). However, very limited epidemiological evidence exists on their effects on CRC prognosis. This study aimed to evaluate the association between flavonoid and lignan intakes with the risk of CRC recurrence and overall survival in CRC patients. The study followed incident histologically confirmed CRC cases in Barcelona (Spain). Validated dietary questionnaires and lifestyle information were collected at recruitment. An ad hoc food composition database on flavonoids and lignans was compiled by using data from the US Department of Agriculture and Phenol-Explorer databases. Adjusted hazards ratios (HR) and 95% confidence intervals (CIs) were estimated using multivariable Cox models. After 8.6 years of mean follow-up, 133 of 409 (32.5%) participants died and 77 of 319 (24.1%) had a CRC recurrence. Total flavonoids were associated neither with CRC recurrence (HR comparing extreme tertiles 1.13, 95% CI 0.64–2.02; P-trend 0.67) nor with overall survival (HRT3vsT1 1.06, 95% CI 0.69–1.65; P-trend 0.78) in the multivariable models. No associations were also observed with either total lignans or any flavonoid subclass intake. In conclusion, the results of the current study do not support a role of flavonoid and lignan intake in the CRC prognosis.
Similar content being viewed by others
Introduction
Flavonoids and lignans are classes of polyphenols found in plant-based foods, such as fruits, vegetables, tea, wine, chocolate and cereal products1. They have been largely investigated due to their anticarcinogenic properties including their ability to induce differentiation and apoptosis and inhibit metabolic carcinogen activation, cell proliferation, tumor cell adhesion and invasion and angiogenesis2,3. Flavonoid and lignan intakes have been inversely associated with colorectal cancer (CRC) risk in several case-control studies, but not in cohort studies1,4,5,6. Only one epidemiological study has evaluated the potential effect of flavonoids with respect to CRC prognosis7. The Polyp Prevention Trial suggested that high intakes of flavonols and isoflavones, two flavonoid subclasses, were related to a decreased risk in advanced colorectal adenoma recurrence7. To the best of our knowledge, no studies has been performed to evaluate the association between lignan intake and CRC prognosis.
In the current study, we prospectively investigated the association between the intake of total flavonoids, lignans and flavonoid subclasses and the risk of colorectal recurrence and overall survival in the Belvitge Colorectal Cancer Study.
Methods
Subjects and study design and ethics
Incident histologically confirmed CRC cases were recruited at the University Hospital of Bellvitge, Barcelona, Spain, from January 1996 to December 1998, as described elsewhere8. A total of 523 histologically confirmed CRC cases were identified, of whom 424 participated in the study (81% participation rate). For this analysis of prognosis, 15 patients were excluded because died within 60 days of surgery due to complications or chemotherapy toxicity, thus 409 will be analyzed. The study was performed in accordance with relevant guidelines and regulations. All participants gave written consent and the Ethics Committee of the Bellvitge University Hospital approved the study protocol.
Dietary and lifestyle assessment
Data collection included a validated dietary history enquiring about usual intakes in the previous 12 months, anthropometric data and questionnaires on sociodemographic factors, lifestyles and health history. Intakes of dietary flavonoid and lignan aglycones were estimated as described previously8 using the US Department Agriculture9, Phenol-Explorer10 and the United Kingdom Food Standards Agency11 databases. Furthermore, our database was expanded using retention factors, recipes and estimations based on similar food or food group items and logical zeros. The final database contained 1,877 food items and only 10% of missing values.
Outcome assessment
Health outcome data was collected through active follow-up. Oncologists updated electronic clinical records at the stablished follow-up visits, recording recurrence events. Mortality events were extracted from the hospital administrative database, with biannually updates. The end points of interest were overall survival, which included death related to CRC and CRC recurrence. The analysis of recurrence was restricted to patients with R0 resection (without residual tumor after surgery) and excluded patients with metastasis at diagnosis that could not be resected (stage IV), thus only 319 patients were considered. Patients with no events of interest were censored at date of last information (up to November 2014). More than 75% of the patients had at least 5 years of follow-up.
Statistical analyses
Cox proportional hazards models were used to estimate hazards ratios (HRs) with 95% confidence intervals (CI) for the association between flavonoid and lignan intakes and CRC recurrence risk and overall survival. Proportional hazards assumption was assessed using a test of the interaction of effects with time. Also graphs based on Schoenfeld residuals were used, which showed no evidence of deviation. The intakes of total and subclasses of flavonoids and lignans were analyzed as tertiles using both absolute amounts adjusted for energy and as density variables (mg/1000 kcal*d), with similar results (data not shown). Multivariable models were adjusted for sex, age (tertiles), total energy (tertiles) and CRC stage (I, II, III, IV). BMI, smoking status, physical activity, intake of alcohol, fruits, vegetables, red and processed meat were not included in final models because they did not change effect estimates >10%. We calculated P-value in the risk categories analysis by the trend test. Interactions with sex, age, BMI, tobacco consumption and physical activity were examined but were not significant. Data were analyzed with the statistical software R version 3.1.2 (R Foundation for Statistical Computing, Vienna, Austria).
Power calculation
Using Power (version 3.0, 1999, National Cancer Institute, Bethesda, MD), we calculated that, given our size and α = 0.05, our study had 80% power to detect an HR ≥ 2.0.
Results
After 8.6 years of mean follow-up, 133 of 409 (32.5%) participants died and 77 of 319 (24.1%) had a CRC recurrence. The median (interquartile range) intake of total flavonoids and lignans were 196.4 (119.8–308.4) mg/d and 0.7 (0.5–1.0) mg/d, respectively. Flavanols were the most important contributor (76.0%, including flavan-3-ol monomers and proanthocyanidins) to total flavonoid intake, followed by flavanones (9.2%), flavonols (7.6%), anthocyanidins (6.0%), flavones (1.1%) and isoflavones (0.1%). The richest food sources of total flavonoids were fruits (65.1%), wine (14.4%), legumes (6.3%) and vegetables (4.4%). For lignans, the main contributors were fruits (32.3%), vegetables (31.2%) and cereal products (10.7%). Baseline characteristics of the participants are shown in Table 1.
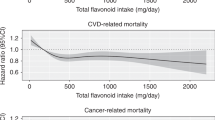
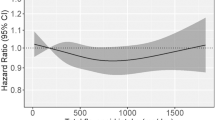
Total flavonoid intake was not associated with either CRC recurrence risk ((hazard ratio comparing third to first tertile (HRT3–T1) 0.97, 95% CI: 0.60–1.56; P trend = 0.89) or overall survival (HRT3–T1 0.87, 95% CI: 0.47–1.62; P trend = 0.71) in the multivariable models (Table 2). The results obtained for total lignan or flavonoid subclasses did not show any association either.
Discussion
The present prospective study shows no association between the intake of total flavonoid, flavonoid subclasses and the CRC recurrence. Similar results were observed in the Polyp Prevention Trial between any colorectal adenoma recurrence and total flavonoid and flavonoid subclass intake7. However, they suggested inverse associations between flavonol and isoflavone intakes and advanced adenoma recurrence7. These findings may not be generalizable to other populations, as it was well discussed by Bobe et al., because most of the participants were healthy conscious7. Moreover, the flavonol intake was greater in the trial than in the standard United States population12, although it was much lower than the European intakes13. Despite of that, in the Bellvitge colorectal cancer case-control study, we did not find any association between flavonol and isoflavone intake and CRC risk8. No association between total lignan intake and CRC recurrence was found in the current study, which is the first one evaluating this topic.
To the best of our knowledge, this is the first study evaluating the association between flavonoid and lignan intakes and the survival of CRC patients. In the present study, no association was observed with the intake of both total flavonoids and lignans and any flavonoid subclass. Similar results have been shown in the Spanish EPIC study, where the cancer mortality was not related to the intake of flavonoids and lignans14. The main strength of the current study is the prospective design, with active long follow-up of recurrence events. Inherent to prospective studies, we had some lost of follow-up, but more than 75% of the patients had at least 5 years of information. Probably the major limitations of the study are related to the potential measurement error in the dietary intake assessment, which may have produced an underestimation of the effects. However, dietary questionnaires were previously validated for some flavonoid-rich foods, such as fruits, vegetables, tea and wine15. Moreover, our database was expanded with the most comprehensive databases on flavonoids and lignans9,10,11. Another limitation is the potential modification of diet related to cancer diagnosis or during the follow-up of the study, which cannot be considered because only diet prior to cancer diagnosis was assessed by the questionnaire.
In summary, our results do not support a role of flavonoid and lignan intake in the CRC prognosis, suggesting that they are not associated with an improvement in both the overall survival and CRC recurrences in CRC patients.
Additional Information
How to cite this article: Zamora-Ros, R. et al. Dietary flavonoids, lignans and colorectal cancer prognosis. Sci. Rep. 5, 14148; doi: 10.1038/srep14148 (2015).
References
Zamora-Ros, R., Touillaud, M., Rothwell, J. A., Romieu, I. & Scalbert, A. Measuring exposure to the polyphenol metabolome in observational epidemiologic studies: current tools and applications and their limits. Am J Clin Nutr. 101, 1854–1865 (2014).
de Kok, T. M., van Breda, S. G. & Manson, M. M. Mechanisms of combined action of different chemopreventive dietary compounds: a review. Eur J Nutr. 47 Suppl 2, 51–59 (2008).
Pierini, R., Gee, J. M., Belshaw, N. J., Johnson, I. T. Flavonoids and intestinal cancers. Br J Nutr. 99E-Suppl. 1, ES53–ES59 (2008).
Woo, H. D. & Kim, J. Dietary flavonoid intake and risk of stomach and colorectal cancer. World J Gastroenterol. 19, 1011–1019 (2013).
Kocic, B., Kitic, D., Brankovic, S. Dietary flavonoid intake and colorectal cancer risk: evidence from human population studies. J BUON. 18, 34–43 (2013).
Jin, H., Leng, Q., Li C. Dietary flavonoid for preventing colorectal neoplasms. Cochrane Database Syst Rev. 8, CD009350 (2012).
Bobe, G. et al. Dietary flavonoids and colorectal adenoma recurrence in the Polyp Prevention Trial. Cancer Epidemiol Biomarkers Prev. 17, 1344–1353 (2008).
Zamora-Ros, R. et al. Association between habitual dietary flavonoid and lignan intake and colorectal cancer in a Spanish case-control study (the Bellvitge Colorectal Cancer Study). Cancer Causes Control. 24, 549–557 (2012).
U.S. Departament of Agriculture. USDA Database for the Flavonoid Content of Selected Foods. Beltsville: MD (USDA, 2007).
Neveu, V. et al. Phenol-Explorer: an online comprehensive database on polyphenol contents in foods. Database (Oxford) 2010:bap024 (2010).
Ward, H. A. et al. Breast, colorectal and prostate cancer risk in the European Prospective Investigation into Cancer and Nutrition-Norfolk in relation to phytoestrogen intake derived from an improved database. Am J Clin Nutr. 91, 440–448 (2010).
Chun, O. K., Chung, S. J. & Song, W. O. Estimated dietary flavonoid intake and major food sources of US adults. J Nutr. 137, 1244–1252 (2007).
Zamora-Ros, R. et al. Estimated dietary intakes of flavonols, flavanones and flavones in the European Prospective Investigation into Cancer and Nutrition (EPIC) 24-h dietary recall cohort. Br J Nutr. 106, 1915–1925 (2011).
Zamora-Ros, R. et al. Dietary flavonoid and lignan intake and mortality in a Spanish cohort. Epidemiology. 24, 726–733 (2013).
EPIC Group of Spain. Relative validity and reproducibility of a diet history questionnaire in Spain. I. Foods. Int J Epidemiol. 26 Suppl. 1, S91–S99 (1997).
Acknowledgements
Grant support: This study was supported by the Spanish Instituto de Salud Carlos III and European Regional Development Fund (ERDF) (CIBERESP CB07/02/2005 and grants PS09-1037 and PI11-01439 and RTICCC RD06/0020) and also from the Spanish Association Against Cancer (AECC) Scientific Foundation, the Catalan Government DURSI grant 2014SGR647.
Author information
Authors and Affiliations
Contributions
R.Z.-R. and V.M. designed the research; A.S. and M.B. contributed to recruit, assess clinical data and follow-up of patients. E.G. and H.A. performed the statistical analysis; R.Z.-R., C.V., M.B, A.S. and V.M. interpreted the results; R.Z.-R. and V.M. wrote the manuscript; All authors read, critically reviewed and approved the final manuscript.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Zamora-Ros, R., Guinó, E., Henar Alonso, M. et al. Dietary flavonoids, lignans and colorectal cancer prognosis. Sci Rep 5, 14148 (2015). https://doi.org/10.1038/srep14148
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep14148
This article is cited by
-
Flavonoids: structure–function and mechanisms of action and opportunities for drug development
Toxicological Research (2021)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.