Abstract
Thrombospondin-1 (TSP-1) is a multifunctional protein which is secreted into the extracellular matrix during inflammation, where it modulates numerous components of the immune infiltrate. Macrophages are a source of TSP-1, which they produce in response to TLR4 mediated signals. Their production of TSP-1 is regulated by environmental signals that establish a threshold for the level of protein secretion that can be induced by LPS stimulation. Th1 and Th2 cytokines raise this threshold which leads to less TSP-1 production, while signals that promote the generation of regulatory macrophages lower it. TSP-1 plays no direct role in the regulation of its own secretion. In vivo in uveitis, in the presence of TLR-4 ligands, TSP-1 is initially produced by recruited macrophages but this decreases in the presence of inflammatory cytokines. The adaptive immune system therefore plays a dominant role in regulating TSP-1 production in the target organ during acute inflammation.
Similar content being viewed by others
Introduction
Macrophages act as a bridge between innate and adaptive immunity, by responding to signals from pattern recognition receptors such as Toll-Like Receptors (TLRs) and modulating T helper cell stimulation. Extracellular cues drive a wide range of different but overlapping gene programs that are commonly used to define phenotype1,2. Resident macrophages, present in virtually all tissues of the body, play a sentinel role in the surveillance, compartmentalisation and presentation of pathogens3. Pathogen-associated danger signals stimulate and recruit macrophages, leading to the release of pro-inflammatory molecules, chemo-attractants and extracellular matrix-altering molecules that initiate and regulate inflammation and immune infiltrate4. One important effector molecule is thrombospondin-1, a protein that plays a role in a number of different organ specific autoimmune diseases5,6.
Thrombospondin-1 (TSP-1) is a multifunctional extracellular matrix protein. In adults its expression is restricted, but at sites of inflammation it modulates several components of the immune response. The effects of TSP-1 include, but are not limited to, neutrophil and monocyte chemotaxis7,8, phagocytosis of neutrophils9, regulation of T cell function via receptor ligation10, activation of latent TGF-β111 and the inhibition of angiogenesis12. The phenotype of the TSP-1 KO mouse has been well described, presenting in a way that is similar to, albeit less severe than TGF-β1 and TGF-βR KO mice13. Despite this chronic inflammatory phenotype characterised by systemic leukocytosis14, raised levels of pro-inflammatory cytokines and impaired wound healing15 and a Sjorgren's syndrome like ocular surface disease16 the TSP-1 KO mouse is resistant to some models of autoimmunity, such as Experimental Autoimmune Encephalomyelitis (EAE)6, while remaining susceptible to others, such as Experimental Autoimmune Uveoretinitis (EAU)5. The phenotype of the T cell response in both these models is the same (S.R. Morwood and L.B. Nicholson; unpublished data), which makes it difficult to understand how the outcomes of the diseases are divergent. Local factors in the eye may be important to the differences in outcome because of the critical role of TSP-1 in the regulation of angiogenesis17, since in chronic uveitis, TSP-1 KO animals develop significantly more retinal angiogenesis than WT controls and this is associated with alterations in the phenotype of the infiltrating macrophages18. It is therefore important to understand the regulation of TSP-1 by recruited macrophages, which are the dominant cell population during the early stages of uveitis and remain present throughout the course of disease.
In this paper we have characterised signals that induce TSP-1 production by macrophages. We demonstrate that the local environment sets a threshold for TSP-1 production with the highest levels of protein elicited by stimuli that favour a regulatory phenotype, consistent with the reported role of TSP-1 in tolerance19. Importantly we further show that the generation of TSP-1 is inhibited by Th1 and Th2, but not Th17 cytokines. The rapid down-regulation of TSP-1 production, in the presence of activated T cells is confirmed by in vivo observations, using the acute endotoxin induced uveitis model, in which the early production of TSP-1 in response to TLR4 ligation is reduced as T cells accumulate at the site of inflammation and by studies of acute inflammation in EAU.
Results
TLR4 dependent TSP-1 production by BM-MΦ is inhibited by Th1 and Th2 cytokines
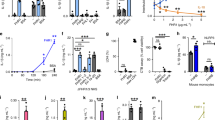
Under innate inflammatory conditions, macrophages upregulate the production of TSP-120 a response that can be induced by lipopolysaccharide (LPS)21. This can be detected at the protein level by intracytoplasmic staining of TSP-1. To recapitulate this observation in our system, we compared LPS with other ligands that engage pattern recognition receptors expressed on BM-MΦ, to confirm this effect on TSP-1 expression. Stimulation for 24 hours with, BLP a TLR2 ligand22 or CpG a TLR9 ligand did not increase TSP-1 protein production. In comparison, treatment with the LPS, a TLR4 ligand, increased expression of TSP-1 approximately 6 fold after 24 hours of treatment (Fig 1A). When cells were cultured for longer periods, up to 72 hours, TSP-1 expression was maintained and increased slightly until approximately 40% of cells produced TSP-1 (data not shown). To establish the requirement for TLR4 signalling more precisely, we then tested BM-MΦ from wild type or TLR4 knockout mice stimulated with LPS or ultrapure LPS and measured nitrite (NO) or TSP-1 production (Fig 1B). In this assay TLR4 knockout BM-MΦ were unable to upregulate TSP-1 in the presence of LPS.
TSP-1 expression by BM-MΦs is stimulated via TLR4.
(A) BM-MΦs were cultured for 24 hrs in media alone or in the presence of various innate ligands. To control for autofluorescence, TSP-1 production was always determined by comparison with comparably activated TSP-1 KO cells. LPS, but not BLP or CpG induced TSP-1. Results are representative of 3 independent experiments. (B) WT and TLR4 KO BM-MΦs were cultured in media alone or stimulated with LPS or ultrapure LPS for 24 hr and assayed for NO and TSP-1 production. Results are the averages of 3 separate experiments. ** p = <0.01, Mann-Whitney two-tailed test.
Having confirmed that LPS stimulated BM-MΦ TSP-1 production in a TLR4 dependent fashion, we wished to consider the control of TSP-1 expression by a more complex inflammatory microenvironment. During an adaptive immune response, activated T cells producing effector cytokines are present and central to the disease process23. Currently the three best characterised subsets of effector T cells, namely Th1, Th2 and Th17, are defined respectively by the production of IFN-γ, IL-4 and IL-17 cytokines. To address the TSP-1 response of macrophages encountering innate and cytokine signals together, we cultured BM-MΦ with LPS for 24 hours, before adding different effector T cell cytokines for a further 24 hours. The addition of Th1 or Th2 cytokines reduced TSP-1 production to that the level of unstimulated cells. In comparison IL-17 had no effect on TSP production, but when added in combination with IFN-γ, the effect of IFN-γ was dominant and TSP-1 production was suppressed (Fig. 2).
Effect of IFN-γ, IL-4 and IL-17 cytokines on BM-MΦ TSP-1 expression.
WT BM-MΦs were stimulated with LPS for 24 hrs followed by the addition of IFN-γ, IL-4, IL-17, or IFN-γ combined with IL-17 for a further 24 hrs. Cells stimulated with LPS alone for 48 hrs were used as controls. IFN-γ and IL-4 inhibited TSP-1 expression while IL-17 had no effect. Results are the averages from two independent experiments. Plots were gated on live F4/80+ cells. * p = <0.05 Mann-Whitney U test.
Environmental regulation of TSP-1 production
The effect of increasing the concentration of LPS to elicit TSP-1 production demonstrates a conventional dose response with a maximum of about 40% of the cells expressing protein. TSP-1 engages many cell surface ligands24, therefore we wished to determine whether this limit was reached because of TSP-1 dependent signals inhibited neighbouring cells from initiating TSP-1 production. To test this we stimulated mixed cultures of WT and TSP-1 KO BM-MΦ in different ratios, reasoning that if TSP-1 was necessary for inhibition to occur, then cultures in total numbers of WT BM-MΦ were lower would have a higher frequency of TSP-1 production i.e. more of the WT BM-MΦ cells would produce TSP-1 in compensation for the reduced total production in the culture. Using WT and TSP-1 KO cells that express different CD45 allelic markers, the individual cell populations and their TSP-1 production could be distinguished by flow cytometry.
The results from these mixed macrophage cultures demonstrated that the level of TSP-1 production is a property of individual cells and not related to environmental TSP-1 levels (Fig 3). When WT cell number is diluted by TSP-1 KO macrophages, the overall production of TSP-1 in the culture reduced to baseline levels, but within the WT population of macrophages, about 40% of the cells continue to produce TSP-1. We concluded that TSP-1 in the environment is not influencing the threshold at which macrophages can produce TSP-1.
TSP-1 secretion is independent of the response of neighbouring cells.
WT and TSP-1 KO BM-MΦ's were cultured together at different ratios and stimulated with LPS for 48 hrs. Expression of TSP-1 by WT (CD45.1 positive) cells was independent of the proportion of TSP-1 KO cells present. Results are the averages for two independent experiments. TSP-1 gates are based on the positivity of TSP-1 KO cells being less than 1%.
Although the fraction of cells producing TSP-1 is not affected by the presence of TSP-1 itself, the threshold of the macrophage TSP-1 response to LPS can be modified. External stimuli such as Th1 and Th2 cytokines inhibit TSP-1 expression (Fig. 2), furthermore, peritoneal macrophages (P-MΦ), obtained from normal mice and compared with BM-MΦ, respond to LPS stimulation by up-regulating TSP-1 expression in a greater proportion of cells (Fig 4A). Baseline and stimulated levels of TSP-1 production from P-MΦ was higher than BM-MΦ, as estimated by measuring frequency and mean fluorescence intensity of TSP-1 staining of cells (Fig 4B). Therefore factors that are independent of the level of TSP-1 protein regulate its production.
Peritoneal macrophages produce a soluble mediator that increases TSP-1 expression.
BM-MΦ or Peritoneal MΦs (P-MΦ) were cultured in media alone or stimulated with LPS. (A) P-MΦ produced greater amounts of TSP-1 as indicated by increased TSP-1+ percentage (B) TSP-1 protein levels were higher in P-MΦ. (C) About 28% of WT BM-MΦ, co-cultured with TSP-1 KO BM-MΦ (ratio 1:1) producedTSP-1. This increased to 48% when WT BM-MΦ were co-cultured with TSP-1 KOP-MΦ.
First we investigated whether the different frequencies of TSP-1 production by BM-MΦ versus P-MΦ were intrinsic to cells obtained from these different environments, or alternatively could be modified by environmental cues, WT BM-MΦ and TSP-1 KO P-MΦ or BM-MΦ were then combined and stimulated as mixed cultures with LPS. TSP-1 production was measured in the WT macrophage population. The results demonstrate that approximately 28% of the WT BM-MΦ produced TSP-1 when they were co-cultured with TSP-1 KO BM-MΦ, but when WT BM-MΦ were cultured with TSP-1 KO P-MΦ, the fraction of TSP-1 producing cells increased 2-fold (Fig 4C). We conclude that macrophages obtained from the peritoneum can interact with WT BM-MΦ and rapidly modify their threshold for TSP-1 secretion by in response to LPS stimulation.
It is well recognised that macrophages respond to a wide array of exogenous signals and a number of different stimuli have been described that modify macrophage activation25. For example, the ability of different signals to switch macrophages from a classically activated to a regulatory phenotype, has been intensively investigated26. In these experiments, it is often an innate signal in combination with a number of different second signals that alters the production of effector molecules, particularly IL-10. Because this response has been carefully documented we wished to investigate how the production of TSP-1 related to this paradigm. Because we have found that P-MΦ but not BM-MΦ include a population of cells competent to induce adenosine (JBF and LBN unpublished data) we tested the role of this mediator. In these experiments and congruent with this two stage signal model, the addition of adenosine or the selective A2A adenosine receptor agonist CGS, did not stimulate TSP-1 when administered alone, but when added in combination with LPS they enhanced TSP-1 production from BM-MΦ (Fig. 5A). The addition PGE2 could also potentiate TSP-1 production by LPS stimulated macrophages (Fig 5B) an effect that could be inhibited by indomethacin (data not shown). To assess the role of IL-10 in this process, we performed parallel experiments using WT and IL-10-deficient BM-MΦ. The absence of IL-10 had no impact on the enhanced TSP-1 production, indicating that this was not an IL-10 dependent response (Fig. 5B). We also considered the impact of TNFα signalling. LPS induces TNFα that signals through TNFR127 and we therefore tested the production of TSP-1 following LPS stimulation of TNFR1KO BM-MΦ. There was no deficit in the ability of these cells to produce TSP-1 in response LPS (Fig. 5C)
LPS in combination with adenosine or PGE2 increase TSP-1 expression.
(A) BM-MΦs were cultured in media alone or stimulated with adenosine or CGS (a selective A2A agonist) alone or in combination with LPS. Adenosine and CGS alone did not up-regulate TSP-1 expression. The addition of Adenosine to LPS-stimulated cultures increased TSP-1 expression by about 1.5 fold, while the addition of CGS to LPS-stimulated culture increased TSP-1 expression 2 fold. (B) WT and IL-10 KO BM-MΦs were cultured in media alone or stimulated with LPS or LPS & PGE2 for 48 hrs. The addition of PGE2 increased TSP-1 expression 2-fold. (C) WT and TNFR1 KO BM-MΦs were cultured in media alone or stimulated with LPS for 48 hrs. The TSP-1 response is independent of the presence of TNFR1. Results are the averages for two independent experiments. * p = <0.05 Mann-Whitney U test. (D) WT BM-MΦs were stimulated with LPS + CGS for 24 hrs followed by the addition of IFN-γ, IL-4, IL-17, or IFN-γ & IL-17 for a further 24 hrs. IFN-γ and IL-4 reduced TSP-1 expression by 30-50%. IL-17 had no effect. Results are the averages from two independent experiments. *p = <0.05 Mann-Whitney U test.
It was then important to determine whether enhanced TSP-1 production was susceptible to inhibition by Th1 and Th2 cytokines. This addresses the outcome of a balance of signal in an adaptive versus an innate response. The addition of either IFN-γ or IL-4 resulted in reduced TSP-1 production by LPS+CGS stimulated BM-MΦ (Fig 5D). These experiments show that Th1 and Th2 cytokines modulate the threshold for TSP-1 production but IL-10 and IL-17 do not. We therefore then studied the impact of this regulation in the context of inflammation in vivo.
TSP-1 production in vivo
Inflammation precipitated by autoimmune disease involves the close collaboration of many cell types, including macrophages and T cells, that interact to establish a microenvironment that determines the fate of the organ in response to the pathological insult28. Investigating the source of TSP-1 mRNA up-regulation we found that this segregated to the macrophage compartment and not to T cells (Fig. 6A). This result is in conflict with data derived in human T cells, which are reported to produce TSP-129,30. We therefore addressed whether murine naive or effector T cells produce TSP-1 directly, using TCR transgenic T cells from OT-II mice, either immediately ex vivo (‘naive’) or differentiated to a Th1 or Th17 phenotype. When these cells were stimulated, either with an optimal concentration of anti-CD3 plus anti-CD28 (Fig 6B) or PMA Ionomycin (data not shown) and compared with TSP-1 KO T cells, they did not produce detectable levels of TSP-1 protein. We also examined in vitro generated dendritic cells (DCs), comparing the production of TSP-1 by immature and mature DCs with a BM-MΦ population and found that only the BM-MΦ upregulated their production of TSP-1 (Fig 6C). This raised the important question of under what circumstances would the balance of inflammatory signals lead in vivo inflammatory macrophages to produce TSP-1. To study this in ocular inflammation, we first assessed the retinas of young unimmunised TSP-1 KO mice and found that they were broadly normal, both clinically and histologically. There was no significant difference in apoptosis in the retina between WT and TSP-1 KO animals, as assessed by counting cleaved Caspase-3 positive cells in TSP-1 KO mice and their age matched controls up to 2 years of age. The only deficit we identified in non-manipulated TSP-1 KO mice was a slight thinning of nuclear layers at 2 years of age, (Fig 6D).
TSP-1 production and retinal architecture in TSP-1 KO animals.
(A) RNA was extracted from bone-marrow derived macrophages from WT mice stimulated as shown. (B) OT-II CD4+ T cells isolated from WT splenocytes were co-cultured with WT or TSP-1 KO KO macrophages, stimulated with peptide and/or LPS. TSP-1 mRNA is expressed by un-activated macrophages and is upregulated by LPS stimulation. IFN-γ down-regulates TSP-1 mRNA expression. In co-culture experiments TSP-1 mRNA was only detectable when WT (and not TSP-1 KO) macrophages where present. Furthermore TSP-1 mRNA was not detectable with the inclusion of WT T cells. Results are representative of >3 independent experiments. (B) Th1 and Th17 cells were generated from OT-II CD4+ T cells cultured in Th1- or Th17-polarising conditions. Th1 and Th17 cells were stimulated with αCD3/28 or PMA + Ionomycin. Neither naïve nor Th1 or Th17 differentiated T cells produced detectable TSP-1, despite the Th1 and Th17 cells producing significant amounts of their signature cytokines (Th1 = ~40% IFN-γ+, Th17 = ~60% IL-17+) upon stimulation. LPS-stimulated TSP-1 null and WT BM-MΦs were stained as a positive control (data not shown). (C) Dendritic cells were prepared from WT or TSP-1 KO mice by culture in GM-CSF and some were matured by the inclusion of LPS (1 µg/ml) for 18–20 hours. TSP-1 production in response to LPS was assessed in WT cells in comparison to TSP-1 KO DCs and BM-MΦs. Data is representative of 2 independent experiments. (D) The retinal thickness in 24-month-old TSP-1 KO mice was compared to their aged matched genetic background control animals. The average retinal thickness at the region 500µm from the optic disc margin is 199.0±20.3µm in WT mice (n = 10) and 168.7±19.1µm in TSP-1 KO mice (n = 9, **p<0.002, Students-T test). The thickness includes the retinal ganglia cell layer to the outer nuclear layer. The photoreceptor layer was excluded to avoid artefact.
To investigate the response to inflammation we then studied two models of uveitis. Endotoxin-induced uveitis (EIU), which results from by the injection of LPS31,32 provides a strong TLR-4 dependent signal in the local tissue. It produces an acute disease of about seven days duration, which is accompanied by a breakdown in the blood-retinal and blood-aqueous barriers and an influx of inflammatory leukocytes. Experimental autoimmune uveoretinitis (EAU) is a prototypical autoimmune disease that produces a pathogenic adaptive autoimmune response in which retinal antigen specific T cells traffic to the eye and produce inflammation in the retina28. In this model, TLR-4 signals are present at the site of immunisation, but not in the target organ.
When EIU was induced, WT and TSP-1 KO mice both developed an anterior uveitis and the infiltrating cell population in both mouse strains was dominated in the early phase by neutrophils (Ly6G+ cells), which do not express TSP-1 (data not shown). The other cell populations present in the early phase, 12 hours following LPS administration included both macrophages (CD11b+ Ly6G-) and T cells (CD3ε+). The CD45+ infiltrating cells were examined by flow cytometry to establish into which population TSP-1 production segregated and we found that it localised to the non-CD3ε+ compartment in wild type mice with approximately equal numbers of infiltrating cells in either model (Fig 7A & B). Analysis of the CD11b+ Ly6G- cellular fraction expressing TSP-1, revealed that for the first 36 hours greater than 30% of these cells were producing TSP-1, but by 60 hours this proportion had fallen by two thirds (Fig 7C). Over the same period there was a reciprocal increase in the fraction of CD3+ T cells present (Fig 7D).
TSP-1 expression during acute inflammation segregates to the macrophage population and is reduced in the presence of activated T cells.
Animals with Endotoxin-Induced Uveitis were sacrificed at different time points after disease induction. Cells released from the eyes were analysed by flow cytometry. (A) TSP-1 expression in macrophages (CD45+, CD11b+, 1A8(Ly6G)- cells) at 12 hours after treatment. (B) CD45+ cell infiltrate was detectable throughout the course of the experiment and peaked at 36 hours. WT and TSPKO animals had similar levels of infiltrate (C) The level of TSP-1 production fell rapidly and significantly over the first 60 hours of the disease course (D) The T cell content of the infiltrate increased significantly with time to 60 hours after the induction of disease. Results are representative of two individual experiments, n = ≥3 mice. *p = <0.05 Mann-Whitney U test.
When EAU was induced in WT and TSP-1 KO mice, clinical disease developed a little more rapidly in the TSP-1 KO animals compared with WT controls, but followed similar kinetics and reached a similar maximum disease score (Fig 8A). We analysed CD11b+ TSP-1 production (Fig. 8B) which is much lower than seen at early time points in EIU. T cell cytokine production tested at day 26 was similar in PMA/Ionomycin stimulated from T cells obtained from both WT and TSP-1 KO animals and included about 12% IFNγ positive cells (Fig. 8C). The low level of TSP-1 (Fig 8B) expression was comparable to that we detected in the EIU model following the maximum influx of CD3ε+ T cells at 60 hours and also the background levels of production that we have shown in vitro. Therefore we conclude that in acute inflammation, TSP-1 can be produced by inflammatory macrophages in vivo in response to LPS, but that this synthesis is relatively short lived and sub-ordinate to regulation that is associated with the local accumulation of Th1 lymphocytes.
TSP-1 expression during acute inflammation experimental autoimmune uveoretinitis.
(A) Clinical EAU assessed by TEFI was slightly advanced compared to the WT control group. The peak of clinical disease ant the kinetics of disease in the first 30 days were similar. (B) Infiltrating macrophages (CD11b+ cells) expressed low levels of TSP-1 at day 26. (C) Infiltrating T cells stimulated with PMA/Ionomycin produced comparable levels of IFNγ and IL-17 at day 26. Disease scores for WT and TSP-1 KO mice up to day 32. n = 10 per group. Cytokine measurements average of cells from 7-8 individual eyes from two independent experiments.
Discussion
Macrophages that have been exposed to a variety of pro-inflammatory stimuli are known as a source of induced TSP-120. In this paper we have elucidated the mechanisms by which the level of TSP-1 protein production is regulated and shown that in an acute inflammatory environment, this production is inversely correlated with the accumulation of CD3+ T cells. Our results demonstrate that BM-MΦ can integrate a number of different environmental cues to establish a threshold for TSP-1 production, which is revealed should they also encounter a TLR4 mediated signal. Th1 and Th2 cytokines raise the threshold for TSP-1 production and inhibit ongoing protein synthesis, even from cells that have already encountered LPS (Fig. 2). Importantly and in contrast with Th1 and Th2 environments, in the presence of IL-17 alone, macrophages can continue to produce TSP-1. Since one function of TSP-1 is the activation of TGFβ1, a cytokine known to play a role in Th17 cell differentiation33 continued TSP-1 secretion and/or the presence of TSP-1 closely associated with the differentiating T cell may favour Th17 cell development.
However, other signals can lower the threshold for TSP-1 secretion and this indicates that different populations of macrophages can respond to the same TLR4 stimulus with altered levels of TSP-1 production, defined as either the frequency or amount of protein (Fig. 4). Differences in local cues are present in the healthy normal environment, as shown by the different responses of BM-MΦ versus P-MΦ. This threshold is not directly regulated by the local concentration of TSP-1 (Fig. 3), which means that the TSP-1 response by macrophages is independent of local TSP-1 accumulation. TSP-1 has a relatively long half-life (540 minutes when measured in the circulation34), which means it has the potential to shape the responses of cells entering the inflammatory microenvironment over relatively long periods of time, compared with short acting effects of pro-inflammatory cytokines such as TNF-α.
The signals that lower the threshold for TSP-1 production (e.g. LPS plus PGE2) are the same as those often associated with the generation of regulatory macrophages26. Macrophages derived from the peritoneal cavity, which have blunted nitric oxide responses to LPS stimulation, produce elevated amounts of TSP-1 (Fig. 4). Furthermore, in a corneal transplantation model the absence of TSP-1 potentiated graft rejection35. This presents a consistent picture, indicating that TSP-1 is induced in circumstances where it plays an anti-inflammatory role. However this interpretation cannot completely explain findings in some autoimmune disease models.
Organ specific autoimmune disease is the product of a CD4+ T cell immune response, directed at self-proteins within the target organ and recruiting a complex mixture of leukocytes28. Many targeted mutations modify the expression of disease and these effects are often consistent across a number of different models, for example IFN-γ knockout mice develop more severe EAE and EAU36,37. The TSP-1 knockout mouse is an exception to this, as it is resistant to experimental autoimmune encephalomyelitis (EAE) but susceptible to experimental autoimmune uveoretinitis (EAU)5,6. Since we have shown that IL-17, but not IFNγ or IL-4, is permissive for the continued production of TSP-1, we propose that this allows Th17 cells to maintain a microenvironment that favours their differentiation. These cells would in turn limit the expansion of Th1 cells. This hypothesis is supported by the finding that in the corneal transplantation model discussed above, there is an expansion of Th1 cells associated with the TSP-1 knockout phenotype. The ability of Th17 cells to solicit TSP-1 from antigen presenting cells may be critical in the early expansion of this cell population, especially in the EAE model when it is induced under sub-optimal conditions. The critical importance of Th17 cells in the development of EAE has been highlighted in recent studies of IL-17 reporter mice38, while for EAU both Th1 and Th17 cell populations can induce disease independently of the presence of the reciprocal cytokine14,39. Therefore EAE in the C57BL/6 model may be a more Th17 dependent disease than EAU in the same strain.
The interaction between lymphocytes and macrophages in the regulation of TSP-1 production is clearly seen in another model of inflammation in vivo, in which LPS is used to induce a model of acute uveitis. Here, there is an inverse correlation between the production of TSP-1 and the accumulation of CD3+ T cells (Fig 7). Because this occurs relatively quickly, it likely reflects an active process rather than the exhaustion of the macrophages. Taking our data together with other studies6,35 we conclude that the major effects of TSP-1 in acute inflammation occur early and in response to innate stimuli that act via TLR4. In the presence of an adaptive immune response, that is associated with the induction of Th1 and/or Th2 cytokines, infiltrating macrophages will no longer synthesise TSP-1, even with continued TLR4 ligation. Only in a strongly Th17 biased environment will TSP-1 be produced.
In chronic EAU the presence of TSP-1 plays a role in controlling the development of angiogenesis. When the retina is examined in animals four months after the induction of EAU, retinal neovascular membranes can be detected. These are markedly increased in the absence of TSP-118. Therefore conditioning of the macrophages to produce TSP-1 is likely to be more significant late in the disease process and acutely a deficit of macrophage TSP-1 production does not lead to a loss of other functional outcome measures of macrophage conditioning, implying that TSP-1 expression per se does not directly signal a switch in macrophage phenotype. TSP-1 production by macrophages is therefore subject to both acute and chronic conditioning that has a significant impact on the outcome of organ specific autoimmunity.
Methods
Animals
C57BL/6 mice were obtained from Harlan UK Limited (Oxford, UK) and thrombospondin-1 deficient (TSP-1 KO) mice (C57BL/6 background) mice were originally from Jack Lawler14 and maintained in our facility at BC10. Toll-like receptor 4 deficient (TLR4KO) mice (C57BL/6 background) were originally obtained from the Research Institute for Microbial Diseases, Osaka University (Osaka, Japan) and generously donated by Dr. Clare Bryant (University of Cambridge, Cambridge, UK). B10.PL wild-type and IL-10KO mice were a kind gift of Prof. David C. Wraith (Cellular & Molecular Medicine, University of Bristol, UK). All breeding colonies were established within the Animal Service Unit at Bristol University (Bristol, UK). Animals were housed in specific pathogen free conditions. Experiments were carried out in compliance with University of Bristol institutional guidelines and under the authority of a project licence from the UK Home Office.
Generation of Bone Marrow Derived Macrophages and Dendritic cells
Bone marrow cells were isolated from the femurs and tibia of mice by flushing with Dulbecco's modified Eagle medium (DMEM). Single-cell suspensions were cultured for 8 days in hydrophobic Teflon bags (supplied by Dr. M. Munder, University of Heidelberg, Heidelberg, Germany40) with DMEM containing 10% heat-inactivated foetal calf serum (FCS), 5% normal horse serum, 1 mM sodium pyruvate, 2 mM L-glutamine, 100 U/ml penicillin-streptomycin (all obtained from PAA Laboratories, Somerset, UK), 50 mM 2-mercaptoethanol (Invitrogen, Paisley, UK) and 50 pg/ml macrophage-colony stimulating factor (M-CSF) generated from L929 fibroblast-conditioned media. Bone marrow-derived macrophages (BM-MΦs) were then harvested and washed in DMEM prior to plating. Greater than 95% of cells were positive for the macrophage markers F4/80 and CD11b.
Monocyte-derived Dendritic Cells were prepared from bone marrow cells. To deplete macrophages, the cells were centrifuged at 500 g for 10 minutes, re-suspended in 20 ml complete media with GM-CSF and then transferred into tissue culture flask (Corning, NY, USA) through 40 µm cell strainer (BD Biosciences, Oxford, UK) before cultured in a 5% vol./vol. CO2 incubator at 37°C for 2 hours. Adherent cells were left in the flask whereas non-adherent cells were removed and centrifuged at 500 g for 5 minutes. Cells were then re-suspended in GM-CSF medium (4 ng/ml) and plated in 6-well tissue culture plates (Corning). Each well contained 2x106 cells per 5 ml GM-CSF medium. The plates were then incubated in a 5% vol./vol. CO2 incubator at 37°C and 2 ml of the media was changed with fresh GM-CSF medium on days 3, 6 and 8. On day 9, 1 µg/ml of LPS (from E.coli 026:B6 (Sigma-Aldrich, Dorset, UK) was added to some wells in order to generate matured DCs and left for 18–20 hours in the 5% vol./vol. CO2 incubator. On day 10, cells were harvested and washed with DMEM.
Isolation of Resident Peritoneal Macrophages
Mice were sacrificed and the peritoneal cavity washed with 5 mls of ice-cold phosphate-buffered saline (PBS) containing 5% FCS. The peritoneal cavity was gently agitated for 3 minutes before retrieval of peritoneal fluid. Peritoneal cells were washed in DMEM and then plated in DMEM containing 1% FCS, 1 mM sodium pyruvate, 2 mM L-glutamine and 100 U/ml penicillin-streptomycin for 2 hrs at 37°C. Non-adherent cells were removed by gentle washing with media. Approximately 70% of adherent cells were positive for the macrophage markers F4/80 and CD11b.
Stimulation of Macrophages
BM-MΦs were cultured at a concentration of 2x106/ml in DMEM containing 1% FCS, 1 mM sodium pyruvate, 2 mM L-glutamine and 100 U/ml penicillin-streptomycin. Resident peritoneal macrophages (P-MΦs) were cultured at a concentration of 2.6x106/ml in DMEM containing 1% FCS, 1 mM sodium pyruvate, 2 mM L-glutamine and 100 U/ml penicillin-streptomycin. In co-culture experiments, wild-type BM-MΦs were cultured with TSP-1 KO P-MΦs or the equivalent number of TSP-1 KO BM-MΦs as controls. Both BM-MΦ and P-MΦ were plated 2 hours prior to stimulation, ensuring that both populations were activated simultaneously. LPS or combinations of LPS and adenosine, the adenosine receptor agonist CGS21680 or prostaglandin E2 (PGE2) were used to stimulate macrophage TSP-1 production. Cell suspensions of 500 μl were applied to 24-well flat bottom culture plates and harvested after 24 or 48 hours of culture. LPS (100 ng/ml), Adenosine (1μM), CGS21680 (1μM), IFN-γ (100 U/ml), IL-17 (200 ng/ml) and PGE2 (1 ng/ml) were purchased from Sigma-Aldrich. IL-4 (25 U/ml) was purchased from Peprotech.
Quantification of nitric oxide (NO) production
NO generation was measured in culture supernatants after 24 hours of culture under varying experimental conditions. NO was assayed by detection of the stable reaction product nitrite quantified using a sodium nitrite standard in a Griess assay27.
Staining of cells for analysis by flow cytometry
All staining protocols were performed on ice, in staining buffer (PBS containing 1% FCS and 0.1% sodium azide). Macrophages were harvested and pre-incubated with 24G2 cell supernatant for 10 min before incubation with primary mAb at 4°C for 20 min. Intracellular staining was carried out using a cytofix/cytoperm kit (BD Biosciences). For intracellular staining, brefeldin A was added for the final 3 hours of cell culture. For TSP-1 staining, a biotinylated anti-TSP-1 mAb (Clone:D4.6; Thermoscientific, USA) was added for 30 minutes, followed by a secondary streptavidin-fluorochrome conjugate for 30 minutes. Cell viability was assessed using LIVE/DEAD fixable dead cell stain kit following the manufacturer's protocol (Invitrogen, UK). TSP-1 staining was detected intracytoplasmically but not extracellularly with this protocol (JBF and LBN, data not shown). All mAbs were purchased from BD Biosciences unless otherwise stated. Data sets were acquired with a LSR II flow cytometer (BD Cytometry Systems) and analysis carried out using FlowJo software (Tree Star, San Carlos, CA).
Isolation of CD4+ T cells
Single-cell suspensions were prepared from whole spleens and CD4+ cells were isolated from splenocytes by negative selection using a MACS separation kit (Miltenyi Biotec).
Generation of Th1 and Th17 cell lines
T cell lines were prepared using a protocol adapted from Cox et al.41. Briefly, CD4+ T cells were purified from OT-II TCR transgenic mice and activated with irradiated antigen presenting cells in RPMI medium (10% FCS) in the presence of peptide (ovalbumin323–339, 10 µg/ml) and either anti-IL-4 (11B11) and IL-12 (Th1 cells) or anti-IFNγ (XMG1.2) and IL-4 (Th2 conditions), or anti-IL-4 plus anti- IFNγ with human TGFβ and IL-6. Cultures were maintained with medium containing IL-2 and after one week re-stimulated with 2 µg/ml (Th1) or 10 µg/ml (Th2 and Th17) OVA peptide and IL-12 (Th1), IL-4 and anti- IFNγ (Th2) or TGFβ, IL-6 and IL-23 with anti-IL-4 plus anti- IFNγ.
Stimulation of CD4+ T cells
CD4+ T cells were cultured in flat-bottom 96-well plates for 24 hours in DMEM containing 1% FCS, 1 mM sodium pyruvate, 2 mM L-glutamine and 100 U/ml penicillin-streptomycin. Stimulation was with PMA (50 ng/ml) & ionomycin (25 ng/ml) (Sigma Aldrich) for the last 3 hours of culture or with CD3/28-mediated in plates with α-CD3 Abs (10 μg/ml) and α-CD28 Abs (5 μg/ml) (BD Pharmingen) in PBS under sterile conditions 24 hrs prior to use.
TSP-1 mRNA detection by RT-PCR
For TSP-1 message detection, RNA was isolated from macrophages using Trizol reagent according to the manufacturers instructions. cDNA was synthesised using the improm II Reverse transcription system with random primers (Promega). TSP-: TSP-Forward: 5′-GCG TCC TTG TCC TTC ACT TC-3′; TSP- Reverse: 5′-TGC ACC TCC AAT GAG TTC AA-3′.
Induction of Endotoxin-induced Uveoretinitis (EIU) and Experimental autoimmune uveoretinitis (EAU)
Local administration of LPS was performed by intravitreal injection in adult mice. Mice were anesthetized by i.p. injection of 150 ul of Vetelar (ketamine hydrochloride 100 mg/ml; Pfizer, Sandwich, UK) and Rompun (xylazine hydrochloride 20 mg/ml; Bayer, Newbury, UK) mixed with sterile water in the ratio 0.6:1:84. The pupils of all animals were dilated using topical 1% tropicamide and 2.5% phenylepherine (Chauvin Pharmaceuticals, Kingston-Upon-Thames, Surrey, UK). Intravitreal injection of 100 ng LPS in 4 ul of PBS was performed under direct control of a surgical microscope with the tip of a 12 mm 33-gaugue hypodermic needle. The injection site was treated once with chloramphenicol ointment. To induce EAU, mice were immunised subcutaneously with peptide (RBP-3-1-20 (GPTHLFQPSLVLDMAKVLLD) 500 µg) emulsified in complete Freud's adjuvant that was supplemented with Mycobacterium tuberculosis (MTb) H37Ra (75 µg BD Biosciences). Mice were coinjected with Bordetella pertussis toxin (Sigma, Poole, UK) intraperitoneally 1.5 µg per mouse.
Isolation of Ocular infiltrate
Infiltrating cells were isolated as previously described42. In brief, retina, ciliary body and choroid were removed and digested in HBSS supplemented with 0.5 mg/ml collagenase D (Roche, Lewes, UK) and 750 U/ml DNase (Sigma) for 15 min at 37°C. After this time, any remaining tissue was disrupted through a 70-µm cell strainer (BD Falcon) and the resulting single cell suspension washed and resuspended in staining buffer.
Retinal thickness measurement
24-month-old thrombospondin-1 knockout (TSP-1 KO) mice and same age matched genetic background controls C57Bl/6J mice were used. Eyecups were embedded in the optimal cutting temperature compound (OCT, R. Lamb) and frozen in liquid nitrogen until used. Only sections including optic nerves were included and images of retina were taken at 500 µm distance to optic disc margin. Retinal thickness measurement (x3) was carried out in 40x images using ImageJ software (NIH) from the inner edge of retinal ganglion cell layer to the outer edge of the outer nuclear layer. To avoid the artifact of artificial retinal detachment, the photoreceptor layer was excluded in this measurement.
References
Medzhitov, R. & Horng, T. Transcriptional control of the inflammatory response. Nat Rev Immunol 9, 692–703 (2009).
Krausgruber, T. et al. IRF5 promotes inflammatory macrophage polarization and TH1-TH17 responses. Nat Immunol 12, 231–238 (2011).
Desmedt, M., Rottiers, P., Dooms, H., Fiers, W. & Grooten, J. Macrophages induce cellular immunity by activating Th1 cell responses and suppressing Th2 cell responses. Journal of Immunology 160, 5300–5308 (1998).
Fujihara, M. et al. Molecular mechanisms of macrophage activation and deactivation by lipopolysaccharide: roles of the receptor complex. Pharmacology & Therapeutics 100, 171–194 (2003).
Zamiri, P., Masli, S., Kitaichi, N., Taylor, A. W. & Streilein, J. W. Thrombospondin Plays a Vital Role in the Immune Privilege of the Eye. Investigative Ophthalmology Visual Science 46, 908–919 (2005).
Yang, K. et al. Deficiency of thrombospondin-1 reduces Th17 differentiation and attenuates experimental autoimmune encephalomyelitis. Journal of Autoimmunity 32, 94–103 (2009).
Mansfield, P. J. & Suchard, S. J. Thrombospondin promotes chemotaxis and haptotaxis of human peripheral blood monocytes. J Immunol 153, 4219–4229 (1994).
Mansfield, P. J. & Suchard, S. J. Thrombospondin promotes both chemotaxis and haptotaxis in neutrophil- like HL-60 cells. J Immunol 150, 1959–1970 (1993).
Savill, J., Hogg, N., Ren, Y. & Haslett, C. Thrombospondin cooperates with CD36 and the vitronectin receptor in macrophage recognition of neutrophils undergoing apoptosis. J Clin Invest 90, 1513–1522 (1992).
Lamy, L. et al. Interactions between CD47 and Thrombospondin Reduce Inflammation. Journal of Immunology 178, 5930–5939 (2007).
Crawford, S. E. et al. Thrombospondin-1 is a major activator of TGF-beta1 in vivo. Cell 93, 1159–1170 (1998).
Streit, M. et al. Overexpression of Thrombospondin-1 Decreases Angiogenesis and Inhibits the Growth of Human Cutaneous Squamous Cell Carcinomas. Am J Pathol 155, 441–452 (1999).
Daniel, C., Schaub, K., Amann, K., Lawler, J. & Hugo, C. Thrombospondin-1 Is an Endogenous Activator of TGFβ in Experimental Diabetic Nephropathy In Vivo. Diabetes 56, 2982–2989, 10.2337/db07-0551 (2007).
Lawler, J. et al. Thrombospondin-1 is required for normal murine pulmonary homeostasis and its absence causes pneumonia. J Clin Invest 101, 982–992 (1998).
Streit, M. et al. Thrombospondin-1 suppresses wound healing and granulation tissue formation in the skin of transgenic mice. EMBO J 19, 3272–3282 (2000).
Turpie, B. et al. Sjogren's syndrome-like ocular surface disease in thrombospondin-1 deficient mice. American Journal of Pathology 175, 1136–1147 (2009).
Cursiefen, C. et al. Roles of Thrombospondin-1 and -2 in Regulating Corneal and Iris Angiogenesis. Investigative Ophthalmology & Visual Science 45, 1117–1124, 10.1167/iovs.03-0940 (2004).
Chen, M. et al. Persistent Inflammation Subverts Thrombospondin-1–Induced Regulation of Retinal Angiogenesis and Is Driven by CCR2 Ligation. The American journal of pathology 180, 235–245 (2012).
Masli, S., Turpie, B. & Streilein, J. W. Thrombospondin orchestrates the tolerance-promoting properties of TGFβ-treated antigen-presenting cells. International Immunology 18, 689–699 (2006).
Jaffe, E. A., Ruggiero, J. T. & Falcone, D. J. Monocytes and macrophages synthesize and secrete thrombospondin. Blood 65, 79–84 (1985).
Dipietro, L. A. & Polverini, P. J. Angiogenic macrophages produce the angiogenic inhibitor thrombospondin-1. American Journal of Pathology 143, 678–684 (1993).
Zhang, Q. et al. Bacterial lipoproteins differentially regulate human primary and memory CD4+ T and B cell responses to pneumococcal protein antigens through Toll-like receptor 2. Journal of Infectious Diseases 201, 1753–1763 (2010).
Kuchroo, V. K., Sarvetnick, N., Hafler, D. A. & Nicholson, L. B. Cytokines and Autoimmune Diseases. Vol. 1st (Humana Press, 2002).
Adams, J. C. & Lawler, J. The thrombospondins. Int J Biochem Cell Biol 36, 961-968 (2004).
Nicholson, L. B., Raveney, B. J. E. & Munder, M. Monocyte Dependent Regulation of Autoimmune Inflammation. Current Molecular Medicine 9, 23–29 (2009).
Mosser, D. M. & Edwards, J. P. Exploring the full spectrum of macrophage activation. Nat Rev Immunol 8, 958–969 (2008).
Calder, C. J., Nicholson, L. B. & Dick, A. D. A selective role for the TNFp55 receptor in autocrine signalling following IFN-gamma stimulation in Experimental Autoimmune Uveoretinitis. Journal of Immunology 175, 6286–6293 (2005).
Kerr, E. C., Copland, D. A., Dick, A. D. & Nicholson, L. B. The Dynamics of Leukocyte Infiltration in Experimental Autoimmune Uveoretinitis. Progress in Retinal and Eye Research 27, 527–535 (2008).
Li, S. S. et al. T lymphocyte expression of thrombospondin-1 and adhesion to extracellular matrix components. Eur J Immunol 32, 1069–1079 (2002).
Li, S. S., Liu, Z., Uzunel, M. & Sundqvist, K.-G. Endogenous thrombospondin-1 is a cell-surface ligand for regulation of integrin-dependent T-lymphocyte adhesion. Blood 108, 3112–3120 (2006).
Rosenbaum, J. T., McDevitt, H. O., Guss, R. B. & Egbert, P. R. Endotoxin-induced uveitis in rats as a model for human disease. Nature 286, 611–613 (1980).
Forrester, J. V., Worgul, B. V. & Merriam, G. R., Jr Endotoxin-induced uveitis in the rat. Albrecht Von Graefes Archiv fur Klinische und Experimentelle Ophthalmologie 213, 221–233 (1980).
Bettelli, E., Korn, T. & Kuchroo, V. K. Th17: the third member of the effector T cell trilogy. Current Opinion in Immunology 19, 652–657, DOI: 10.1016/j.coi.2007.07.020 (2007).
Morwood, S. R. & Nicholson, L. B. Modulation of the immune response by extracellular matrix proteins. Archivum Immunologiae et Therapiae Experimentalis 54, 1–8 (2006).
Saban, D. R., Bock, F., Chauhan, S. K., Masli, S. & Dana, R. Thrombospondin-1 Derived from APCs Regulates Their Capacity for Allosensitization. The Journal of Immunology 185, 4691–4697, 10.4049/jimmunol.1001133 (2010).
Jones, L. S. et al. IFN-gamma-deficient mice develop experimental autoimmune uveitis in the context of a deviant effector response. Journal of Immunology 158, 5997–6005 (1997).
Krakowski, M. & Owens, T. Interferon-gamma confers resistance to experimental allergic encephalomyelitis. European Journal of Immunology 26, 1641–1646 (1996).
Hirota, K. et al. Fate mapping of IL-17-producing T cells in inflammatory responses. Nat Immunol 12, 255–263 (2011).
Luger, D. et al. Either a Th17 or a Th1 effector response can drive autoimmunity: conditions of disease induction affect dominant effector category. Journal of Experimental Medicine 205, 799-810 (2008).
Munder, P. G., Modolell, M. & Wallach, D. F. Cell propagation on films of polymeric flurocarbon as a means to regulate pericellular pH and pO2 in cultured monolayers. FEBS letters 15, 191–196 (1971).
Cox, C. A. et al. Both Th1 and Th17 Are Immunopathogenic but Differ in Other Key Biological Activities. The Journal of Immunology 180, 7414–7422 (2008).
Kerr, E. C., Raveney, B. J. E., Copland, D. A., Dick, A. D. & Nicholson, L. B. Analysis of Retinal Cellular Infiltrate in Experimental Autoimmune Uveoretinitis Reveals Multiple Regulatory Cell Populations. Journal of Autoimmunity 31, 354–361 (2008).
Acknowledgements
The authors acknowledge the support of the National Eye Research Centre and the MRC (SRM).
Author information
Authors and Affiliations
Contributions
JBF, SRM, JH, LPS and DAC carried out experiments. JBF, ADD and LBN designed experiments. JBF and LBN drafted the manuscript.
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-No Derivative Works 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Fordham, J., Hua, J., Morwood, S. et al. Environmental conditioning in the control of macrophage thrombospondin-1 production. Sci Rep 2, 512 (2012). https://doi.org/10.1038/srep00512
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/srep00512
This article is cited by
-
Candida albicans Elicits Pro-Inflammatory Differential Gene Expression in Intestinal Peyer’s Patches
Mycopathologia (2019)
-
Hypoxia inducible factors are dispensable for myeloid cell migration into the inflamed mouse eye
Scientific Reports (2017)
-
Thrombospondin-1 Production Regulates the Inflammatory Cytokine Secretion in THP-1 Cells Through NF-κB Signaling Pathway
Inflammation (2017)
-
Angiogenic inhibitors delivered by the type III secretion system of tumor-targeting Salmonella typhimurium safely shrink tumors in mice
AMB Express (2016)
-
Pleiotropic action of CpG-ODN on endothelium and macrophages attenuates angiogenesis through distinct pathways
Scientific Reports (2016)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.