Key Points
-
Provide an overview of flapless implant surgery and CBCT guided flapless implant surgery.
-
Describe the advantages, disadvantages, clinical indications, contraindications of using flapless implant surgery.
-
Provide the evidence on implant survival and complications associated with flapless implant surgery and CBCT guided implant surgery where possible.
Abstract
Flapless implant surgery is increasing in popularity, particularly due to advances and increased usage of cone beam computed tomography (CBCT) and dental implant treatment planning software allowing three-dimensional assessment of the implant site. It is the aim of the article to provide an overview of flapless implant surgery and CBCT guided flapless implant surgery and summarise the literature with regard to the effectiveness of this surgical technique.
Similar content being viewed by others
Introduction
The surgical placement of a dental implant fixture is constantly changing and in recent years, there has been some interest in developing techniques that minimise the invasive nature of the procedure, with flapless implant surgery being advocated. The original surgical protocol as proposed by Brånemark involved placing incisions in the oral vestibule and mucosa in an attempt to prevent infection by placing the incisions away from the implant fixture site. A mucoperiosteal flap was then raised to expose and visualise the underlying bone for implant placement, and then closed, burying the implant fixtures for a period of time to allow osseointegration to occur before restoration.1 Since then a variety of incisions and flap designs have been described in the literature for surgical implant placement to optimise soft tissue aesthetics and improve tissue healing to create a healthy and aesthetic peri-implant soft tissue profile.2,3,4,5,6,7,8 However, the raising of a mucoperiosteal flap has been associated with a degree of morbidity, discomfort and requires subsequent suturing. There is also evidence to demonstrate that bone resorption and subsequent soft tissue recession can occur as a result.9,10,11,12,13 Flapless implant surgery has been suggested to alleviate these issues and involves placing an implant fixture without elevation of the epithelium, connective tissue or periosteum covering the alveolar bone. In recent years, flapless implant surgery has increased in popularity as a result of technological advances in radiographic imagery such as cone beam cross-sectional tomography (CBCT) and implant planning software. These advances have allowed the clinician to place and even restore the dental implants virtually before surgical placement, with an ability to produce surgical guides transferring these planned CBCTs into the surgical field. A flapless implant surgical technique can be used to place single or multiple implants, with immediate, early and delayed implant placement and varying loading protocols being reported within the literature.14
It is the aim of this article to provide an overview of flapless implant surgery and CBCT guided flapless implant surgery and report on the advantages and disadvantages, implant survival rates, patient satisfaction and complications associated with this surgical technique.
Flapless surgical technique
Flapless implant surgery involves placing an implant fixture without elevation of the epithelium, connective tissue or periosteum overlying the alveolar bone. However, to place the implant fixture, surgical access to the underlying bone is required and a variety of soft tissue techniques have been utilised. These include, a soft tissue punch excision,15,16,17,18 a small/mini incision or by direct preparation through the soft tissue when preparing the osteotomy site.19,20
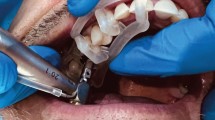
The soft tissue punch technique excises a small specific diameter of overlying soft tissue which corresponds to the planned diameter of the implant fixture. It is resective in nature and (Figs 1 and 2) is commonly carried out using a soft tissue punch or bur. Another resective method is the direct soft tissue technique and involves removal of the soft tissue during the preparation of the implant bed using the surgical osteotomy drills. As these techniques are both resective in nature they do not allow primary closure and submergence of the implant fixture and as such can only be used when a single stage surgical technique is desired and appropriate. Their resective nature means that careful assessment of the quality and quantity of the keratinised tissue is required. A minimum of 1.5 mm of circumferential peri-implant keratinised tissue is needed around the implant after surgery to provide epithelial and connective tissue elements for soft tissue integration and the development of biological width21 (Figs 3 and 4); it also provides tissues that are more stable and resistant to soft tissue recession which in turn helps facilitate good oral hygiene measures,22,23,24,25 thereby minimising the risk of peri-implant disease.26
Soft tissue management with resection of the soft tissue as part of a flapless implant surgical technique using a mucosa and tooth supported surgical guide (ImplantPilot system) constructed from a planned CBCT with immediate placement at the 12, 25 sites and delayed placement in the 26, 14 and 16 sites
The mini-incision technique is non-resective and involves placing a small incision to access the underlying alveolar bone. This incision should be of an adequate size to accommodate the osteotomy drills and allow placement of the implant fixture. Due to this being a non-resective technique it can be used as either a single or two-stage surgical procedure as the soft tissue is still present to cover the surgical site and submerge the implant fixture during healing. It is particularly useful when there is limited peri-implant keratinised tissue which is preserved using this technique and can alleviate the need for further surgical intervention such as a connective tissue graft.
When considering surgical flap design for the surgical placement of dental implants, Sclar27 proposed a set criteria which is shown in Box 1. However, Sclar's criteria cannot be fully met when a flapless implant surgical technique is used and it is therefore imperative that surgeons are aware of the limitations that a flapless surgical technique has in comparison to raising a mucoperiosteal flap which should be considered very early in the planning stages of treatment to ensure optimal and predictable treatment outcomes are achieved.
Advantages and disadvantages of a flapless surgical technique
A number of advantages and disadvantages of using a flapless surgical technique over raising a mucoperiosteal flap have been proposed in the literature and are summarised in Table 1. The majority of the advantages of using a flapless technique pertain to the minimally invasive nature of the surgical technique and the majority of the disadvantages are related to the lack of direct visualisation of the surgical site at the time of the surgery.
CBCT-guided flapless implant surgery
The planning and placement of dental implants and their subsequent prosthodontic restoration needs to be carefully considered and planned three-dimensionally. With decreasing cost and increased access of CBCT imagery to dental practitioners this type of imagery is being readily used in implant dentistry. CBCT imagery allows a 3D volumetric image of potential implant sites to be visualised and allows a more accurate assessment of the bone quantity, quality and topography as well as the proximity to adjacent structures in comparison to conventional radiographs.39 Interactive CBCT implant planning software can be used to virtually plan the placement of implant fixtures to optimise their position and avoid adverse trauma to adjacent structures (Fig. 5). These planned CBCTs can then be transferred to the patient via surgical guides which are produced by a variety of automated manufacturing processes (CAD/CAM) (Figs 6 and 7). These surgical guides are manufactured in such a way that the location, trajectory, and depth of the planned implant fixture can be transferred from the planned CBCT to the surgical guides with a high degree of precision,40 and enables accurate and consistent positioning and orientation of the implants (Figs 8, 9, 10, 11, 12, 13). These guides can be used in the preparation of the implant bed (Figs 6, 14 and 16) and/or the placement of the implant fixtures (Figs 15 and 16).41,42,43 Use of computer-assisted surgery is advocated as being more predictable, precise and safer in flapless dental implantology,41,44 and has been the driving force behind the increasing use of this surgical technique.45 Despite this, however; these systems are not 100% accurate and errors in the positioning and angulation of the implant fixtures can occur.49,50 Tahmaseb et al.,49 (as part of the Fifth International Team of Implantology Consensus conference) reviewed the literature assessing the accuracy and clinical performance of static computer-assisted implant surgical guides and carried out a meta-analysis of a number of in-vitro and in-vivo studies. This meta-analysis revealed a total mean error in the position of the implant fixture of 1.12 mm at the entry point (with a maximum of 4.5 mm) and 1.39 mm at the apex (with a maximum of 7.1 mm). This working group also reported that of the 38 studies included, ten studies reported changes in the surgical plan at the time of surgery, with an overall implant incidence of 2.0%.49 These issues have also been reported by Van Assche et al.,50 who as part of a working group for the European Association of Osseointegration (EAO) carried out a review and a meta-analysis on the accuracy of computer-aided implant placement. The meta-analysis revealed a positioning mean error of 0.99 mm at the entry point (ranging from 0 to 6.5 mm) and 1.24 mm at the apex (ranging from 0 to 6.9 mm) at the apex with a mean angular deviation of 3.81° (ranging from 0 to 24.9°).50 The causes of such errors leading to inaccurate implant positioning when using a CBCT surgical implant guide can occur at any stage of treatment and include: the planning and diagnostic work up of the patient; the design and production of the surgical guide; and/or the surgical processes involved in the placement of the implant fixture. Greater deviations and inaccuracies in the positioning of the implant fixture are generally seen when the degree of the error is large or when multiple errors have occurred potentiating to a greater overall error.49 A number of causes leading to such errors have been proposed and are summarised in Box 2.13,40,49,50,51,52,53,54,55,56 Clinicians therefore need to be aware of the potential sources of error that can lead to inaccuracies and deviations in the placement of the implant fixtures when using a CBCT surgical guide and where possible minimise or reduce these potential errors. Clinicians should also consider the potential for inaccuracies and deviations in implant positioning during the planning and surgical stages of treatment46,47,48,49,50 as a failure to give due consideration to these potential issues can lead to a variety of surgical and prosthodontic complications including damage to vital structures.55,57,58
Stereolithographic tooth supported Simplant surgical guides used to accommodate each osteotomy drill used in the drilling sequence for placement of Straumann implants (from planned CBCT Fig. 15)
Implant survival
High implant survival rates have been reported for flapless implant surgery with implant survival rates of over 90% reported in a number of studies9,29,31,37,59,60,61,62,63,64,65,66,67review and systematic review articles29,36,68,69 (see Tables 2 and 3). Two separate systematic reviews by Lin et al.,69 and Chracnovic et al.,36 reported on implant survival rates comparing conventional and flapless implant surgery. Both reported higher implant failure rates when using a flapless surgical technique with Lin et al.,69 reporting implant survival rates of; 97.0% for flapless implant surgery and 98.6% for conventional open flap surgery; however, this was not found to be statistically significant. Chracnovic et al.,36 reported a higher implant failure when using a flapless surgical technique in comparison to open flap surgery which was found to be statistically significant (P = 0.03). They also reported a risk ratio of 1.75 which implies that implants inserted using a flapless technique are 1.75 times likely to fail in comparison to those implants placed when using an open flap technique.36
Marginal bone loss
It has been suggested that marginal bone loss can be minimised around the implant fixture during the initial stages of healing by using a flapless implant surgical technique with this being attributed to a reduction in the disturbance of the blood supply at the surgical site. The vascularisation of bone at an edentate site is provided by blood vessels of the periosteum and the alveolar bone. A flapless technique reduces the disturbance to the periosteal blood supply (as a mucoperiosteal flap is not raised) and thus minimises bone resorption during the initial stages of healing9 with this being shown in both animal and human studies.70,71,72,73 When reviewing studies assessing marginal bone loss around implant fixtures placed using a flapless implant technique, the results are variable. Studies by Kan et al.,75, Becker et al.,20,31, Cosyn et al.,76, Sennerby et al.,59 and a systematic review by Moraschini et al.,68 all reported favourable minimal crestal bone loss when a flapless technique was used. Cosyn et al.,76 also concluded that there was enhanced papilla soft tissue regrowth which resulted in an improved aesthetic outcome in single implant placement when using a flapless technique.76 However, a comparative randomised control trial by Pisoni et al.,74 comparing conventional flap to flapless implant surgery reported no influence on bone resorption when comparing the two surgical techniques.74 Furthermore, a systematic review by Chrcanovic et al.,36 reported that five studies60,77,78,79,80 (included in their systematic review) reported increased marginal bone loss around the implant fixture when a flapless technique was used. The proposed explanation for this was that that the implant fixture could have been placed more apical than the desired position due to reduced visibility at the time of surgery,77,80 with the transmucosal portion of the implant being slightly below the crestal bone causing rearrangement/resorption of the peri-implant bone around the neck of the implant.80
Osseointegration and contamination of the implant fixture
It has been hypothetically proposed that osseointegration can be impaired when using a flapless surgical technique due to the risk of soft tissue contamination of the implant bed and/or implant fixture during the process of implant surgery due to the close proximity of the soft tissues during surgery.18,61 However, evidence for this is lacking and an animal study by Becker et al.,81 who evaluated the histology of implants placed using conventional and flapless implant surgery in dogs found no histological evidence of gingival tissue or foreign body intrusion at the implant site using either surgical technique.81
Irrigation of osteotomy site
Another concern of using a flapless implant surgical technique is the minimal and reduced surgical access for irrigation of the implant bed38 which is necessary to cool and prevent heat generation at the surgical site. This heat generation can lead to the risk of heat induced necrosis of the bone82 which can subsequently lead to bone resorption and implant failure. This may also be particularly true when a surgical drilling guide is used which can further impede and restrict delivery of irrigant to the osteotomy site (Figs 10 and 18 – the surgical guide design in Figure 18 also improves access for irrigation and visualisation at the implant bed site).45 There are a number of factors which can contribute to heat generation during the preparation of the implant bed which include; the presence and temperature of irrigant,82 the amount of bone being prepared,83 drill sharpness and design,84 the preparation time, the depth of the osteotomy,85 pressure on the drill,84 drill speed86 and the thickness of the cortical bone.87 On reviewing the literature relating to heat generation during the preparation of the implant bed using a flapless implant surgical technique, there are very few studies reporting on this. An in-vitro study by Jeong et al.,88 who assessed heat generation at implant osteotomy sites when using a surgical drilling guide comparing open flap and flapless implant surgery reported a greater temperature increase when a flapless surgical technique was used in comparison to open flap surgery, but this was not found to be statistically significant (This study however, only carried out 20 drilling procedures in total).
Surgical technique: Free-hand, CBCT-guided and CBCT-guided and navigated flapless implant surgery
There are a variety of flapless implant surgical techniques which can be used for flapless implant surgery, these include, free hand, CBCT guided and CBCT guided and navigated flapless implant surgery. A systematic review by Voulgarakis et al.,89 compared the outcomes of these three different flapless surgical procedures assessing implant survival rates and marginal bone loss. Twenty-three studies with a minimum of 1-year follow-up were included. The following results were reported; free hand flapless implant surgery demonstrated implant survival rates of 98.3–100% and mean marginal bone loss of between 0.09 and 1.40 mm at 1-4 years after implant insertion. Flapless CBCT guided surgery (without 3D navigation) had an implant survival rate of between 91-100% and mean marginal bone loss of 0.89 mm after an observation period of 2-10 years and CBCT guided and navigated flapless surgery showed implant survival rates of between 89-100% and mean marginal bone loss of between 0.55-2.6 mm over a follow-up period of 1-5years. This systematic review concluded that there are several methods to facilitate implant placement via a flapless approach and that none of the methods demonstrated has advantages over the other with regard to implant survival and marginal bone loss.89 However, D'hase et al.,54 suggested that free hand flapless implant surgery can only be advocated in specific pre-planned cases by experienced surgeons where there is adequate bone volume.54
Loading protocols
Immediate, early and delayed loading protocols have been reported with flapless implant surgery. A systematic review by Xu et al.,14 compared immediate and early loading of implants placed using a flapless technique. The review reported on six articles which included four randomised controlled trials with 180 patients cumulatively included within their analysis. The review reported an implant failure rate of 0% to 3.3% for both immediate and early loaded implants when using a flapless surgical technique. The review reported no statistically significant outcome with regard to implant failure rates, peri-implant marginal bone levels or complications between the two groups. The only reported differences between the groups was that patients preferred immediate rather than early implant loading.14 A retrospective study by Doan et al.,103 reported on predictors for implant survival based on 1,241 consecutive implants placed using a flapless implant surgical technique. They reported on early (6-8 weeks and at 10-12 weeks) and delayed (at six months) loading protocols; however, the loading protocols were not reported as being predictors for implant survival.103 Additionally, a study by Oh et al.,104 reported on soft tissue changes on implants placed in the anterior maxilla using a flapless surgical technique comparing immediate and delayed loading (after four months). Patients were followed up for six months with no statistical significance in the soft tissue profile being found between the two groups. However, statistical significance in the papillary index score was found in the immediate loading group where score increased from baseline to month two which was maintained at month six and could indicate that creeping attachment (that is, soft tissue recovery) might occur within two months after immediate loading.104
Complications associated with flapless implant surgery
The most commonly reported complication when using a flapless implant surgical technique is the perforation or fenestration of the peri-implant bone during surgery.90,91 This is due to the procedure effectively being carried out blind without direct visualisation of the surgical site. A review by Brodala et al.,29 reported an overall incidence of intraoperative complications of 3.8% for flapless implant surgery. All of these were related to perforation or dehiscences, with four of the 16 studies included within this review reporting on such complications.29 Of these four studies, two used CBCT surgical stents for all patients,65,92 whilst the other two studies did not routinely use them;9,93 this demonstrates that this surgical complication can occur even with the use of CBCT surgical guides and should not be solely relied upon to alleviate this complication. There is also the strong possibility that the incidence of such events could be much higher due to such complications not being readily apparent to the clinician as a consequence of the lack of direct visualisation of the surgical site at the time of implant placement. To minimise the risk of this occurring, care must be taken when planning and placing the implants to ensure correct positioning and angulation. This is particularly true at high risk sites such as those with reduced alveolar ridge width and where bony concavities are present which commonly occur on the lingual aspect of the posterior mandible and the buccal aspect of the anterior maxilla.94 Where such anatomical risks are present and in the presence of inadequate bone volume,9 a flapless technique is not recommended. CBCT guided implant surgery can be used to minimise such risks, however, as discussed earlier these risks can and do still occur and should not be solely relied on to alleviate such risks.46,47,49,95 Other reported complications include: reduced primary stability of the implant fixture; sub-optimal implant positioning and angulation; implant failure; challenges in restoring the implant fixtures; fracture of surgical guide and complications associated with the implant prosthesis,68 however, such complications also occur when a conventional surgical technique is utilised with a review article by Brodala et al.,29 reporting that the immediate postoperative and delayed complications appear to be similar for both flap and flapless implant surgery.29
Training and experience
There are a number of articles that state that there is a learning curve to achieving treatment success when using a flapless implant surgical technique.9,68 This was reported by Campelo et al.,9 who attributed their improved implant survival rate over a ten-year follow up period to their increased clinical experience of using a flapless surgical technique.9 This was also suggested by Jain et al.,96 who stated that placing implants without raising a mucoperiosteal flap requires a certain level of experience, fine motor skills, and sensitivity of the surgeon's hand, which only can come with practice.96 Clinical experience has also been reported as being vital when using CBCT implant surgical guides for flapless implant surgery by Höckl et al.,97 stating that 'in the hands of an inexperienced clinician there can be a blind reliance on surgical guides when using a flapless technique.'97 It makes perfect sense that clinicians with less clinical experience of using such surgical techniques are more likely to have a lack of insight to identify any potential issues or errors and also a lack of experience to be able to alleviate or deal with these as they present themselves, with this being particular true in clinicians with limited implant surgery experience.97 For example, one of the ways to deal with a surgical complication may be to abandon a flapless surgical technique and to raise a mucoperiosteal flap to visualise the site.
Patient satisfaction and perceived pain
A flapless implant surgical technique is minimally invasive in comparison to conventional flap surgery and has been shown to have improved rates of healing due to reduced surgical trauma and, with this, reduced postoperative complications such as pain, infection, swelling or dehiscence. It has also been suggested that bleeding is reduced both at the time of surgery (allowing a clean surgical field) and also postoperatively.98 When assessing patients' satisfaction with using a flapless technique, a review article by Poomer et al.,99 reporting on patients' preferences towards minimally invasive treatment alternatives for implant rehabilitation of edentulous jaws reported that patient satisfaction was high for implant surgery (average 91% [range: 77 to 100%]).99 when using a flapless surgical technique.99 This was also reported by Youk et al.,100 who reported that patients who had undergone computer-guided flapless implant surgery employing a surgical template felt less pain and had higher satisfaction than those who had undergone conventional implant surgery.100 When assessing patients' perceived pain and discomfort, studies by Nkenke et al.,101 and Fortin et al.,18 both reported reduced patient morbidity and a reduction in the intensity of pain for shorter periods of time when using a flapless technique.18,101 This is weakly backed up by a Cochrane systematic review by Esposito et al.,102 who concluded that there is limited weak evidence to suggest that flapless implant surgery shows reduced postoperative discomfort in adequately selected patients.102
Conclusion
Flapless implant surgery is increasing in popularity with its use being driven by advances in CBCT guided implant surgery. However, this surgical technique requires further education, training and experience to enable clinicians to learn and apply the requisite skills necessary for this surgical approach as there is a learning curve to achieving treatment success.9,68 Clinicians using CBCT surgical guides should have a good understanding of the system being used and appreciate potential inaccuracies and deviations (both average and maximal) for each specific system used and consider this in the planning and surgical stages of treatment to minimise potential risks and complications occurring.
Like any aspect of implant surgery, careful patient selection, proper diagnosis and appropriate treatment planning29 are key factors in achieving predictable treatment outcomes;9,29,31 this is particularly true for flapless implant surgery as this technique is effectively a 'blind procedure'. It has been suggested that a flapless implant surgical technique should only be considered where there is sufficient bone volume, adequate keratinised soft tissue, (when resection of the soft tissue is planned), an absence of significant hard tissue undercuts5,9,16,75 and when the clinician is appropriately aware of the anatomy and location of vital structures.31
This surgical technique has promise, however, for more definite conclusions further well-designed long-term clinical trials need to be carried out to determine the real effect of flapless implant surgery on patient outcome variables. Further research and development is also needed to improve the accuracy of CBCT surgical guides with this improvement being predicted to increase the usage and uptake of this surgical technique by dental practitioners.
References
Brånemark P I, Hansson B O, Adell R, Breine U, Lindström J, Hallén O . Osseointegrated implants in the treatment of the edentulous jaw. Experience from a 10-year period. Scand J Plast Reconstr Surg Suppl 1977; 16: 1–132.
Han T J, Park K B, Klokkevold P R . Standard implant surgical procedures. In: Carranza's Clinical Periodontology. 10th ed. pp. 1120–1132. St.Louis: Saunders, 2006.
Cranin A N, Sirakian A, Russell D, Klein M . The role of incision design and location in the healing processes of alveolar ridges and implant host sites. Int J Oral Maxillofac Implants 1998; 13: 483–491.
Cranin A N . Implant surgery: The management of soft tissues. J Oral Implantol 2002; 28: 230–237.
Sclar A G . Guidelines for flapless surgery. J Oral Maxillofac Surg 2007; 65: 20–32.
Gomez-Roman G . Influence of flap design on peri-implant interproximal crestal bone loss around single tooth implants. Int J Oral Maxillofac Implants 2001; 16: 61–67.
Takei H H, Han T J, Carranza FA Jr, Kenney E B, Lekovic V . Flap technique for periodontal bone implants: papilla preservation technique. J Periodontol 1985; 56: 204–210.
Rosenquist B . A comparison of various methods of soft tissue management following the immediate placement of implants into extraction sockets. Int J Oral Maxillofac Implants 1997; 12: 43–51.
Campelo L D, Camara J R . Flapless implant surgery: A 10-year clinical retrospective analysis. Int J Oral Maxillofac Implants 2002; 17: 271–276.
Van der Zee E, Oosterveld P, Van Waas M A . Effect of GBR and fixture installation on gingiva and bone levels at adjacent teeth. Clin Oral Implants Res 2004; 15: 62–65.
Wood D L, Hoag P M, Donnenfeld O W, Rosenfeld L D . Alveolar crest reduction following full and partial thickness flaps. J Periodontol 1972; 43: 141–144.
Van der Zee E, Oosterveld P, Van Waas M A . Effect of GBR and fixture installation on gingiva and bone levels at adjacent teeth. Clin Oral Implants Res 2004; 15: 62–65.
Staffileno H . Significant differences and advantages between the full thickness and split thickness flaps. J Periodontol 1974; 45: 421–425.
Xu L, Wang X, Zhang Q, Yang W, Zhu W, Zhao K . Immediate versus early loading of flapless placed dental implants: a systematic review. J Prosthet Dent 2014; 112: 760–769.
Campelo L D, Camara J R . Flapless implant surgery: A 10-year clinical retrospective analysis. Int J Oral Maxillofac Implants 2002; 17: 271–276.
Hahn J . Single-stage, immediate loading, and flapless surgery. J Oral Implantol 2000; 26: 193–198.
Casap N, Tarazi E, Wexler A, Sonnenfield U, Lustmann J . Intraoperative computerized navigation for flapless implant surgery and immediate loading in the edentulous mandible. Int J Oral Maxillofac Implants 2005; 20: 92–98.
Fortin T, Bosson J L, Isidori M, Blanchet E . Effect of flapless surgery on pain experienced in implant placement using an image-guided system. Int J Oral Maxillofac Implants 2006; 21: 298–304.
Al-Ansari B H, Morris R R . Placement of dental implants without flap surgery: A clinical report. Int J Oral Maxillofac Implants 1998; 13: 861–865.
Becker W, Wikesjo U M, Sennerby L et al. Histologic evaluation of implants following flapless and flapped surgery: A study in canines. J Periodontol 2006; 77: 1717–1722.
Berglundh T, Lindhe J : Dimension of the peri-implant mucosa: Biologic width revisited. J Clin Periodontol 1996; 23: 971.
Schroeder A, van der Zypen E, Stich H, Sutter F . The reactions of bone, connective tissue, and epithelium to endosteal implants with titanium-sprayed surfaces. J Maxillofac Surg 1981; 9: 15–25.
Buser D, Weber H P, Lang N P . Tissue integration of non-submerged implants. 1-year results of a prospective study with 100 ITI hollow-cylinder and hollow-screw implants. Clin Oral Implants Res 1990; 1: 33–40.
Meffert R M, Langer B, Fritz M E . Dental implants: a review. J Periodontol 1992; 63: 859–870.
ten Bruggenkate C M, Krekeler G, van der Kwast W A, Oosterbeek H S . Palatal mucosa grafts for oral implant devices. Oral Surg Oral Med Oral Pathol 1991; 72: 154–158.
Block M S, Kent J N . Factors associated with soft-and hard-tissue compromise of endosseous implants. J Oral Maxillofac Surg 1990; 48: 1153–1160.
Sclar A G : Surgical techniques for management of peri-implant soft tissues. In Motamedi M Soft Tissue and Esthetic Considerations in Implant Therapy. P. 43. Chicago, I L: Quintessence, 2003.
Bidra A S . Consequences of insufficient treatment planning for flapless implant surgery for a mandibular overdenture: a clinical report. J Prosthet Dent 2011; 105: 286–291.
Brodala N . Flapless surgery and its effect on dental implant outcomes. Int J Oral Maxillofac Implants 2009; 24: 118–125.
Turkyilmaz I . Immediate provisional restoration of implant placed using flapless surgery and ridge mapping. N Y State Dent J 2011; 77: 21–23.
Becker W, Goldstein M, Becker B E, Sennerby L . Minimally invasive flapless implant surgery: a prospective multicentre study. Clin Implant Dent Relat Res 2005; 7: S21–S27.
Sclar A G . Guidelines for flapless surgery. J Oral Maxillofac Surg 2007; 65: 20–32.
Fortin T, Bosson J L, Isidori M, Blanchet E . Effect of flapless surgery on pain experienced in implant placement using an image-guided system. Int J Oral Maxillofac Implants 2006; 21: 298–304.
Komiyama A, Klinge B, Hultin M . Treatment outcome of immediately loaded implants installed in edentulous jaws following computer-assisted virtual treatment planning and flapless surgery. Clin Oral Implants Res 2008; 19: 677–685.
Rocci A, Martignoni M, Gottlow J . Immediate loading in the maxilla using flapless surgery, implants placed in predetermined positions, and prefabricated provisional restorations: a retrospective 3-year clinical study. Clin Implant Dent Relat Res 2003; 5 Suppl 1: 29–36.
Chrcanovic B R, Albrektsson T, Wennerberg A . Flapless versus conventional flapped dental implant surgery: a meta-analysis. PLoS One 2014; e100624.
Sunitha R V, Sapthagiri E . Flapless implant surgery: a 2-year follow-up study of 40 implants. Oral Surg Oral Med Oral Pathol Oral Radiol 2013; 116: e237–e243.
De Bruyn H, Atashkadeh M, Cosyn J, van de Velde T . Clinical outcome and bone preservation of single TiUnite™ implants installed with flapless or flap surgery. Clin Implant Dent Relat Res 2011; 13: 175–183.
Orentlicher G, Abboud M . Guided surgery for implant therapy. Dent Clin North Am 2011; 55: 715–744.
Chrcanovic B R, Oliveira D R, Custodio A L . Accuracy evaluation of computed tomography-derived stereolithographic surgical guides in zygomatic implant placement in human cadavers. J Oral Implantol 2010; 36: 345–355.
Lindeboom J A, van Wijk A J . A comparison of two implant techniques on patient-based outcome measures: a report of flapless vs. conventional flapped implant placement. Clin Oral Implants Res 2010; 21: 366–370.
Soares M M, Harari N D, Cardoso E S, Manso M C, Conz M B, Vidigal G M Jr . An in vitro model to evaluate the accuracy of guided surgery systems. Int J Oral Maxillofac Implants 2012; 27: 824–831.
Brief J, Edinger D, Hassfeld S, Eggers G . Accuracy of image-guided implantology. Clin Oral Implants Res 2005; 16: 495–501.
Van Assche N, van Steenberghe D, Quirynen M, Jacobs R . Accuracy assessment of computer-assisted flapless implant placement in partial edentulism. J Clin Periodontol 2010; 37: 398–403.
Sclar A G . Guidelines for flapless surgery. J Oral Maxillofac Surg 2007; 65: 20–32.
D'haese J, Van De Velde T, Elaut L, De Bruyn H . A prospective study on the accuracy of mucosally supported stereolithographic surgical guides in fully edentulous maxillae. Clin Implant Dent Relat Res 2012; 14: 293–303.
Di Giacomo GA, da Silva JV, da Silva A M, Paschoal G H, Cury P R, Szarf G . Accuracy and complications of computer-designed selective laser sintering surgical guides for flapless dental implant placement and immediate definitive prosthesis installation. J Periodontol 2012; 83: 410–419.
D'haese J, Van De Velde T, Komiyama A, Hultin M, De Bruyn H . Accuracy and complications using computer-designed stereolithographic surgical guides for oral rehabilitation by means of dental implants: a review of the literature. Clin Implant Dent Relat Res 2012; 14: 321–335.
Tahmaseb A, Wismeijer D, Coucke W, Derksen W . Computer technology applications in surgical implant dentistry: a systematic review. Int J Oral Maxillofac Implants 2014; 29 Suppl: 25–42.
Van Assche N, Vercruyssen M, Coucke W, Teughels W, Jacobs R, Quirynen M . Accuracy of computer-aided implant placement. Clin Oral Implants Res 2012; 23 Supp 6: 112–123.
Lee D H, An S A, Hong M H, Jeon K B, Lee K B . Accuracy of a direct drill-guiding system with minimal tolerance of surgical instruments used for implant surgery: a prospective clinical study. J Adv Prosthodont 2016; 8: 207–213.
Ozan O, Turkyilmaz I, Yilmaz B . A preliminary report of patients treated with early loaded implants using computerized tomography-guided surgical stents: flapless versus conventional flapped surgery. J Oral Rehabil 2007; 34: 835–840.
Turbush S K, Turkyilmaz I . Accuracy of three different types of stereolithographic surgical guide in implant placement: an in vitro study. J Prosthet Dent 2012; 108: 181–188.
D'haese J, Ackhurst J, Wismeijer D, De Bruyn H, Tahmaseb A . Current state of the art of computer-guided implant surgery. Periodontol 2000 2017; 73: 121–133.
Pettersson A, Komiyama A, Hultin M, Näsström K, Klinge B . Accuracy of virtually planned and template guided implant surgery on edentate patients. Clin Implant Dent Relat Res 2012; 14: 527–537.
Behneke A, Burwinkel M, Behneke N . Factors influencing transfer accuracy of cone beam CT-derived template-based implant placement. Clin Oral Implants Res 2012; 23: 416–423.
Schneider D, Marquardt P, Zwahlen M, Jung R E . A systematic review on the accuracy and the clinical outcome of computer-guided template-based implant dentistry. Clin Oral Implants Res 2009; 20 Suppl 4: 73–86.
Hultin M, Svensson K G, Trulsson M . Clinical advantages of computer-guided implant placement: A systematic review. Clin Oral Implants Res 2012; 23 Suppl. 6: 124–135.
Sennerby L, Rocci A, Becker W, Jonsson L, Johansson L A, Albrektsson T . Short-term clinical results of Nobel Direct implants: A retrospective multicentre analysis. Clin Oral Implants Res 2008; 19: 219–226.
Malo P, Nobre M D . Flap vs. flapless surgical techniques at immediate implant function in predominantly soft bone for rehabilitation of partial edentulism: a prospective cohort study with follow-up of 1 year. Eur J Oral Implantol 2008; 1: 293–304.
Berdougo M, Fortin T, Blanchet E, Isidori M, Bosson J L . Flapless implant surgery using an image-guided system. A 1-to 4-year retrospective multicentre comparative clinical study. Clin Implant Dent Relat Res 2010; 12: 142–152.
van Steenberghe D, Glauser R, Blombäck U et al. A computed tomographic scan-derived customized surgical template and fixed prosthesis for flapless surgery and immediate loading of implants in fully edentulous maxillae: a prospective multicentre study. Clin Implant Dent Relat Res 2005; 7 Suppl 1: S111–S120.
Cannizzaro G, Leone M, Consolo U, Ferri V, Esposito M . Immediate functional loading of implants placed with flapless surgery versus conventional implants in partially edentulous patients: a 3-year randomized controlled clinical trial. Int J Oral Maxillofac Implants 2008; 23: 867–875.
Sanna AM, Molly L, van Steenberghe D . Immediately loaded CAD-CAM manufactured fixed complete dentures using flapless implant placement procedures: a cohort study of consecutive patients. J Prosthet Dent 2007; 97: 331–339.
Wittwer G, Adeyemo WL, Wagner A, Enislidis G . Computer-guided flapless placement and immediate loading of four conical screw-type implants in the edentulous mandible. Clin Oral Implants Res 2007; 18: 534–539.
Becker W, Goldstein M, Becker B E, Sennerby L, Kois D, Hujoel P . Minimally invasive flapless implant placement: follow-up results from a multicentre study. J Periodontol 2009; 80: 347–352.
Rousseau P . Flapless and traditional dental implant surgery: an open, retrospective comparative study. J Oral Maxillofac Surg 2010; 68: 2299–2230.
Moraschini V, Velloso G, Luz D, Porto Barboza E . Implant survival rates, marginal bone level changes, and complications in full-mouth rehabilitation with flapless computer-guided surgery: a systematic review and meta-analysis. Int J Oral Maxillofac Surg 2015; 44: 892–901.
Lin G H, Chan H L, Bashutski J D, Oh T J, Wang H L . The effect of flapless surgery on implant survival and marginal bone level: a systematic review and meta-analysis. J Periodontol 2014; 85: e91–e103.
Wilderman M N, Wentz F M . Repair of a dentogingival defect with a paedicle flap. J Periodontol 1965; 36: 218–231.
Pennel B M, King K O, Wilderman M N, Barron J M . Repair of the alveolar process following osseous surgery. J Periodontol 1967; 38: 426–431.
Wilderman M N, Pennel B M, King K, Barron J M . Histogenesis of repair following osseous surgery. J Periodontol 1970; 41: 551–565.
Wood D L, Hoag P M, Donnenfeld O W, Rosenfeld L D . Alveolar crest reduction following full and partial thickness flaps. J Periodontol 1972; 42: 141–144.
Pisoni L, Ordesi P, Siervo P et al. Flapless Versus Traditional Dental Implant Surgery: Long-Term Evaluation of Crestal Bone Resorption. J Oral Maxillofac Surg 2016; 74: 1354–1359.
Kan J Y, Rungcharassaeng K, Ojano M, Goodacre C J . Flapless anterior implant surgery: a surgical and prosthodontic rationale. Pract Periodontics Aesthet Dent 2000; 12: 467–474.
Cosyn J, Hooghe N, De Bruyn H . A systematic review on the frequency of advanced recession following single immediate implant treatment. J Clin Periodontol 2012; 39: 582–589.
De Bruyn H, Atashkadeh M, Cosyn J, van de Velde T . Clinical outcome and bone preservation of single TiUnit implants installed with flapless or flap surgery. Clin Implant Dent Relat Res 2011; 13: 175–183.
Covani U, Cornelini R, Barone A . Buccal bone augmentation around immediate implants with and without flap elevation: a modified approach. Int J Oral Maxillofac Implants 2008; 23: 841–846.
Van de Velde T, Sennerby L, De Bruyn H . The clinical and radiographic outcome of implants placed in the posterior maxilla with a guided flapless approach and immediately restored with a provisional rehabilitation: a randomized clinical trial. Clin Oral Implants Res 2010; 21: 1223–1233.
Rousseau P . Flapless and traditional dental implant surgery: an open, retrospective comparative study. J Oral Maxillofac Surg 2010; 68: 2299–2306.
Becker W, Wikesjo¨ UM, Sennerby L et al. Histologic evaluation of implants following flapless and flapped surgery: A study in canines. J Periodontol 2006; 77: 1717–1722.
Eriksson R A, Albrektsson T : The effect of heat on bone regeneration: an experimental study in the rabbit using the bone growth chamber. J Oral Maxillofac Surg 1984; 42: 705–711.
Eriksson R A, Adell R : Temperatures during drilling for the placement of implants using the osseointegration technique. J Oral Maxillifac Surg 1986; 44: 4–7.
Matthews J, Hirsch C . Temperatures measured in human cortical bone when drilling. J Bone Joint Surg. 1972; 45: 297–308.
Ercoli C, Funkenbusch P D, Lee H J . The influence of drill wear on cutting efficiency and heat production during osteotomy preparation for dental implants: a study of drill durability. Int J Oral Maxillofac Implant 2004; 19: 335–349.
Brisman D L . The effect of speed, pressure, and time on bone temperature during the drilling of implant sites. Int J Oral Maxillofac Implant 1996; 11: 35–37.
Hobkirk J, Rusiniak K : Investigation of variable factors in drilling bone. J Oral Surg 1977; 35: 968–973.
Jeong S M, Yoo J H, Fang Y, Choi B H, Son J S, Oh J H . The effect of guided flapless implant procedure on heat generation from implant drilling. J Craniomaxillofac Surg 2014; 42: 725–729.
Voulgarakis A, Strub J R, Att W . Outcomes of implants placed with three different flapless surgical procedures: A systematic review. Int J Oral Maxillofac Surg 2014; 43: 476–486.
Chiapasco M, Zaniboni M . Clinical outcomes of GBR procedures to correct peri-implant dehiscences and fenestrations: a systematic review. Clin Oral Implants Res 2009; 20 Suppl 4: 113–123.
Annibali S, Ripari M, La Monaca G, Tonoli F, Cristalli M P . Local accidents in dental implant surgery: Prevention and treatment. Int J Periodontics Restorative Dent 2009; 29: 325–331.
Wittwer G, Adeyemo W L, Schicho K, Gigovic N, Turhani D, Enislidis G . Computer-guided flapless transmucosal implant placement in the mandible: A new combination of two innovative techniques. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2006; 101: 718–723.
Cannizzaro G, Leone M, Esposito M . Immediate functional loading of implants placed with flapless surgery in the edentulous maxilla: 1-year follow-up of a single cohort study. Int J Oral Maxillofac Implants 2007; 22: 87–95.
Campelo L D, Camara J R . Flapless implant surgery: a 10-year clinical retrospective analysis. Int J Oral Maxillofac Implants 2002; 17: 271–276.
Puig C P . A retrospective study of edentulous patients rehabilitated according to the 'all-on-four' or the 'all-on-six' immediate function concept using flapless computer-guided implant surgery. Eur J Oral Implantol 2010; 3: 155–163.
Jain D, Gaur G . Flapless implant placement: a case report. J Oral Implantol 2014; 40: 321–324.
Höckl K, Stoll P, Stoll V, Bähr W, Bach G . Flapless implant surgery and its effect on periimplant soft tissue. Int J Oral Maxillofac Surg 2011; 40: e24.
Romero-Ruiz M M, Mosquera-Perez R, Gutierrez-Perez J L, Torres-Lagares D . Flapless implant surgery: A review of the literature and 3 case reports. J Clin Exp Dent 2015; 7: e146–e152.
Pommer B, Mailath-Pokorny G, Haas R, Busenlechner D, Fürhauser R, Watzek G . Patients' preferences towards minimally invasive treatment alternatives for implant rehabilitation of edentulous jaws. Eur J Oral Implantol 2014; 7 Suppl 2: 91–109.
Youk S Y, Lee J H, Park J M et al. A survey of the satisfaction of patients who have undergone implant surgery with and without employing a computer-guided implant surgical template. J Adv Prosthodont 2014; 6: 395–405.
Nkenke E, Eitner S, Radespiel-Tröger M, Vairaktaris E, Neukam FW, Fenner M . Patient-centred outcomes comparing transmucosal implant placement with an open approach in the maxilla: a prospective, non-randomized pilot study. Clin Oral Implants Res 2007; 18: 197–203.
Esposito M, Maghaireh H, Grusovin M G, Ziounas I, Worthington H V . Interventions for replacing missing teeth: management of soft tissues for dental implants. Cochrane Database Syst Rev 2012; 18: CD004970.
Doan N V, Du Z, Reher P, Xiao Y . Flapless dental implant surgery: a retrospective study of 1,241 consecutive implants. Int J Oral Maxillofac Implants 2014; 29: 650–658.
Oh T J, Shotwell J L, Billy E J, Wang H L . Effect of flapless implant surgery on soft tissue profile: a randomized controlled clinical trial. J Periodontol 2006; 77: 874–882.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Laverty, D., Buglass, J. & Patel, A. Flapless dental implant surgery and use of cone beam computer tomography guided surgery. Br Dent J 224, 591–602 (2018). https://doi.org/10.1038/sj.bdj.2018.268
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.2018.268