Key Points
-
Suggests the referral pathways to specialist dental services for patients with disabilities are commonly unclear.
-
Many factors may contribute to a referral decision for patients with disabilities, including the need for supportive measures such as sedation and GA.
-
Demonstrates the BDA Case Mix Model is a useful tool to identify the complexity of patients requiring dental care.
Abstract
Background Access to health services is a right for every individual. However, there is evidence that people with disabilities face barriers in accessing dental health. One of the reasons associated with this is the unclear referral pathway existing in the Irish dental health service. The appropriate assignment of patients to relevant services is an important issue to ensure better access to healthcare. This is all the more pertinent because there are only a few trained dental practitioners to provide dental treatment for people with disabilities, as well as even fewer qualified specialists in special care dentistry.
Aims The aim of this part of the study was to assess the use of the BDA Case Mix Model to determine the need for referral of patients to specialist dental services, and to determine any association between patient complexity and the need for adjunct measures, such as sedation and general anaesthesia for the management of people with disabilities and complex needs.
Methodology A retrospective analysis of dental records using the BDA Case Mix Model.
Results The results showed that patients with different levels of complexities were being referred to the special care dentistry clinic at the Dublin Dental University Hospital. The results also showed that the need for supportive adjunct measures such as sedation and general anaesthesia was not necessarily the main reason for referring patients to specialist services. The assessment with the BDA Case Mix Model was comprehensive as it looked at many factors contributing to the cases' complexity. Not all categories in the Case Mix Model had significant association with the need for an adjunct.
Conclusion The BDA Case Mix Model can be used to measure the need for supportive adjunct measures, such as sedation and general anaesthesia.
Similar content being viewed by others
Introduction
People with disabilities require access to quality oral health care services in order to overcome difficulties in maintaining good oral health and preventing oral diseases. Studies have confirmed that although people with disabilities have similar levels of oral disease as the general population, they experience poorer oral health.1 This is mainly, but not exclusively, a consequence of difficult access to oral healthcare services.2
Barriers to dental health services
Barriers to accessible dental services exist and these barriers can be associated with the individual, the dental profession, the society, or the policy makers. Accessible services are not only concerned about the availability of physically accessible dental service centres, but also the availability of appropriate referral systems that provide seamless care, allocating suitable management approaches for each individual according to their needs, and the availability of the essential resources. The appropriate assignment of patients to relevant services is an important issue to ensure better access to health care, particularly as there are few clinicians either experienced or even qualified to provide dental treatment for people with disabilities. In addition, people with disabilities may require dental treatment under general anaesthesia or sedation, and these very restricted services should be used appropriately. General anaesthesia is a useful and effective modality used to facilitate dental treatment for individuals with disabilities who cannot accept dental care by other means, especially with those suffering from challenging behaviours. On the other hand, general anaesthesia is a complex and expensive option that is not without risk. This method of patient management has to be hospital-based due to its side effects, and the waiting list in most circumstances is very long. The more favourable option now is the use of sedation due to its perceived safety, effectiveness and relative ease of access. All treatment options need to be carefully planned for every individual to facilitate appropriate care.
Guidelines are available to assist oral healthcare providers on the decision-making processes for choosing the appropriate methods of treatment suitable for each individual. Nevertheless, there are only a few referral tools developed for designating patients with disabilities and complex medical conditions, whether they require specialist level of care or not.2,3,4
The BDA Case Mix Model
The British Dental Association (BDA) Case Mix Model is one example of an assessment tool designed to measure patients' complexity. It was introduced as a commissioning tool to describe the mix of patients served by the community dental services in the UK so as to enable service managers to ensure adequate and appropriate service provision for people with disabilities.5
The BDA Case Mix Model identifies the various challenges patient complexity can present to dental services. Every episode of care is measured separately to reflect the different complexities for the individual patient at different episodes of care, depending on the nature of each episode. Six independent criteria are included in this model to measure the level of patient complexity. Each of the criteria is independently measured on a 4 point scale where 0 represents an average fit and well child or adult, and A, B and C represent increasing levels of complexity. The criteria included in the Case Mix Model are: ability to communicate, ability to cooperate, medical status, oral risk factors, access to oral care, and legal and ethical barriers to care.
This tool is being used in some locations in the UK to develop referral criteria, or to demonstrate compliance with patient acceptance, or as a discharge criteria.5 A study was performed to test the internal validity of the case mix model and the reliability of the dentists using it, and the results showed significant variation in the assessment of patient complexity using the tool.6 It was suggested that the reason for the variation may be from a general misunderstanding of the scoring system in the tool and/or the scenarios, and the authors recommended that further investigations are needed before the tool can be said to be reliable and valid. A more recent study was conducted in an attempt to assess the use of the weighted case mix model and to assess the possibility of simplifying it to improve its efficient use.7
Oral health services for people with disabilities in Ireland
In Ireland, there are two main referral centres for providing dental services for people with disabilities; the Dublin Dental University Hospital and the University Dental School and Hospital, Cork. These two hospitals provide both secondary and tertiary dental care, as well as a substantial amount of primary care delivered by students in training. The main provider of primary dental care services for people with disabilities in most areas of the country is the Health Services Executive (HSE). The range of dental services available within these centres varies widely around the country; some areas report having relatively good services, while others report minimal care.8 The scope of services provided include screening in special schools and sheltered workshops, services to psychiatric and homeless centres, residential units, addiction services, travellers and older persons. Following screening, patients who require routine dental treatment are called to the HSE or referred to the Dental Treatment Services Scheme; under this service scheme all adult medical card holders can access a range of free dental treatments from private dentists who hold contracts with the HSE. For patients requiring specialist services, referrals are sent to the two main hospitals depending on the geographic area. The main challenges reported by most health board centres were 'lack of manpower, resources and no or limited access to secondary care facilities such as general anaesthesia.'8 In addition, the report on the Strategic Review of the Delivery and Management of Health Service Executive Dental Services stated that the referral pathways between services were unclear, in particular between primary and secondary/tertiary services, and this could lead to uncertainty and cause inappropriate referrals by some.9
In order to help overcome some of the challenges in providing oral and dental healthcare services for people with disabilities, developing a comprehensive referral pathway in Ireland was considered necessary.
This study was part of a larger study that aimed at assessing the appropriate oral and dental health service settings for people with disabilities in Ireland, and the factors that influence their referral, utilising a combination of the BDA Case Mix Model and another model.2
Aim
The aim of this part of the study was to assess the use of the BDA Case Mix Model to determine the need for referring patients to specialist dental services, and to determine any association between patient complexity and the need for adjunct measures, such as sedation and general anaesthesia for the management of people with disabilities and complex needs.
Methodology
In the study, a retrospective analysis of dental records was undertaken in order to look at the level of complexity of the patients referred to the special care dentistry clinic at Dublin Dental University Hospital, using the BDA Case Mix Model. In addition, the need for supportive adjuncts such as sedation and general anaesthesia was also assessed. Ethical approval was sought from the Faculty Research Ethics Committee at Trinity College Dublin and was granted in October 2010. Approval from the Clinical Director of the Dublin Dental University Hospital to access dental records to begin the retrospective study was also granted.
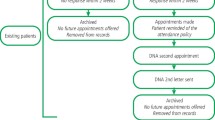
A convenience sample was targeted from the hospital's waiting list. All patients on the special care dentistry clinic clinic waiting list from 2001 were initially included; there were 919 on the original list. From the waiting list, 649 were selected for the study as the remaining 270 people did not attend for their assessment appointments. From the selected list, a total number of 305 dental records were randomly included in the study (Fig. 1). The exclusion criteria were patients who only attended the assessment clinic but did not return for further treatment, patients who did not have a disability or medical condition but were placed on the waiting list, and deceased patients. All included patients received an invitation letter by post with an information leaflet in a frequently asked questions format and a consent form, in order to allow the researcher to access their dental records. Participants were asked to return the signed forms by post, using the provided self-addressed and pre-stamped envelopes. An independent 'gatekeeper' (a role required by the Ethics Committee to prevent coercion of subjects) was assigned to look at the records before sending out the invitation letters in order to identify the level of capacity to give informed consent. There were three types of consent forms and information leaflets used: a basic informed consent form, a simplified consent form using illustrations, and an assent form.
Following receipt of the signed informed consent/assent forms, each dental record was assessed using the weighted scoring system of the BDA Case Mix Model, and a total score was assigned for each participant. When an item was not recorded in the dental records, it was assumed it was not a concern or issue for the individual and so a score of 0 was given for that criterion.
Another component assessed from the dental records was the use of adjunct measures. Where more than one type of adjunct was needed, the first option was noted.
Results
From the total list of dental records, 305 records were randomly included in the retrospective analysis; out of this, 140 individuals responded to the postal invitation, giving a response rate of 45.9%.
Demographics
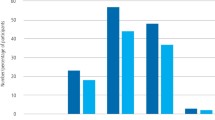
There were more individuals from the non-respondents group who required an assent form for approval to gain access to their dental records than in the respondents group. By contrast, more individuals responded to the invitation to participate in the study when the simple form was used, in comparison to the non-respondents of the same group. There was a minor difference between respondents and non-respondents in the group requiring the basic informed consent. Overall, the response rate for those requiring the basic and simple informed consent group combined, in both the respondent and non-respondent groups, was higher in comparison to those requiring assent forms (Figs 2 and 3).
The age distribution of the participating individuals is shown in Table 1. There was an equal gender distribution with seventy males and seventy females.
The use of adjuncts
Table 2 shows the distribution of the adjuncts used in the studied group. A large number of this group did not require any adjunct measures to manage their dental treatment (44.3%); treatment under sedation and general anaesthesia were performed at about the same frequency, where inhalation sedation was more frequently used than IV sedation.
The BDA Case Mix Model
Using the BDA Case Mix Model, the level of complexity of each case was assessed and recorded for all categories and the total complexity was calculated using the weighted banded score. Many items could not be identified from the referral letters or dental records as these were not documented either in the letter or on assessment or subsequent visits. For these items, it was anticipated that they were not present and a value of 0 was given for the category.
For the purposes of analysis, the two types of sedation, inhalation sedation and IV sedation were both recorded initially, but were combined later giving only one total value of the number of times sedation was used in every category. When local anaesthesia or behavioural management was used for the provision of dental treatment, it was recorded as none.
Categories of the BDA Case Mix Tool (Table 3)
1. Ability to communicate
In this category, more than half of the participants did not have issues with communication, given score 0 (62.9%). When the scores for communication were cross-tabulated with the adjunct used for each score, there was a significant association between them using Pearson chi-square test (P value set at 0.05). This significance however should be interpreted carefully as the expected values in some cells were less than five.
2. Ability to cooperate:
The most frequently scored level in this category was C (29.3%), where the cases had serious difficulties in cooperation and general anaesthesia was required to provide the dental treatment needed. There were equal number of scores 0 and A. There was a highly significant association between the ability to cooperate and the adjunct measure used clinically (P = 0.000).
The higher the complexity score individuals were given, the more advanced the adjunct measure used.
3. Medical status:
More than half of the group (59.3%) had no significant medical condition. The complexity of the medical status of the studied group was significantly associated with the adjunct used (P = 0.008).
4. Oral risk factors
For this category, there was no significant association between oral risk factors and the adjunct chosen for the management of each case (P = 0.120).
5. Access to oral care
Access issues were also not highly significantly associated with the adjuncts used (P = 0.213). There were no cases that required domiciliary dental care. Most cases referred either scored 0 or A, and 17.9% of the cases scored level B where access was severely restricted and the patients needed to be treated in their wheelchair or a hoist was used to transfer the patient to the dental chair.
6. Legal and ethical barriers
The majority of the cases in the studied group had no ethical or legal issues (79.3%). There were no cases with highly complex ethical barriers. There were an almost equal number of cases that scored A and B (15 and 14 respectively), where A describes cases with some legal or ethical barriers, such as when the clinician is required to make a best interest decision not requiring a second opinion, and B describes moderate legal or ethical barriers, such as when the patient had fluctuating capacity to consent or the clinician was required to make a best interest decision requiring obtaining a second opinion.
Interestingly, there was a significant association between the complexity of the ethical barriers and the adjuncts used to provide dental treatment (P = 0.004). Nevertheless, due to the small number of the sample size there were four cells (44.4%) with an expected count of less than five in the cross-tabulation table. This will have a considerable effect on the validity of the significance of the Pearson chi-square test results.
Total banded scores
The total score of the complexity of each case was calculated by adding the given scores in each category. The provided weighted scores in the BDA Case Mix Model were used to determine the level of complexity. Table 4 shows the distribution of the different levels of complexity in the studied group.
In the studied group, 40.7% scored a moderate level of complexity. Only 2.1% were standard cases and 9.3% were considered extremely complex using the BDA Case Mix Model.
When measuring the association between the total level of complexity with the adjunct used (Table 5), using Pearson chi-square test, there was a significant association (P = 0.000) between the two. Individuals with lower total complexity levels did not require any adjunct measures, while those scoring on the extreme levels of complexity required general anaesthesia.
Discussion
This retrospective study looked at dental records of patients attending the special care dentistry clinic (SCD) clinic at Dublin Dental University Hospital. This was part of a larger study. The aim of this particular phase of the study was to assess the type and complexity of the patients seen at this clinic using the BDA Case Mix Model. This part also aimed at assessing any association between the level of complexity and the need for adjunct measures, such as general anaesthesia and sedation for the provision of dental care. With the retrospective analysis, it was intended to collect the factors that would affect or drive the decision for referring patients to specialist level of care, in order to develop a robust and predictive model to aid in decision-making.
In the context of disability research ethics, in ensuring the involvement of the people with disabilities in the decision-making process and allowing accessible information, a capacity-specific format was used in this research to gain informed consent.10 Simplified information and consent forms were provided to adult individuals with mild intellectual disabilities. For children and adults who are not legally able to give consent to participate, assent forms were used; this allowed a responsible parent or legal guardian to agree on the participation in the research. In Ireland, the Assisted-Decision Making (Capacity) Act11 was approved in 2015. This legislation allows adults above the age of 18 years to either appoint an assistant, choose a co-decision maker, or a decision-making representative is appointed, to assist, advise or make decisions depending on the assessed level of capacity.
In general, the response rate for this part of the study was low. Follow up phone-calls were deemed impractical due to the large number of dental records initially included in the study. Further participants were not recruited subsequently owing to time constraints. The reduced number of participants may have affected the results obtained in the statistical analysis.
Research participants were not selected in any particular order or form; lists of the individuals on the special care dentistry database, fulfilling the inclusion criteria were randomly submitted to the central medical records personnel, in order to gain access to the paper charts.
Bias may have been introduced, as the response rate from those who required assent, as opposed to consent, to participate was lower in comparison to the remaining participants. However, this was also true for the non-respondents; the percentage of non-respondents in the assent group was also lower than respondent.
The assessment with the BDA Case Mix Model was comprehensive as it looked at many factors contributing to the cases' complexity. The model looks at the person's level of communication and cooperation, their medical risk and dental risk, ethical factors and issues around accessing services. The total level of complexity measured with the BDA Case Mix Model of the cases seen at the SCD clinic varied from standard to extreme complexity. This demonstrates that even though only a small number of low complexity cases were assessed in this part of the study, simple cases are still being referred for specialist care. In addition, the majority of the cases with some level of complexity did not require any adjunct measures, such as sedation or general anaesthesia, for their dental management. The reasons for these referrals were for a second opinion or they required complex dental procedures and interdisciplinary dental care not requiring support with general anaesthesia or sedation.
The highest level of complexity, as measured by the BDA Case Mix Model scoring system, in the studied group, was in the moderate category; even in this category many of the cases did not require any adjunctive measures.
In the severe and extreme complexity categories, there were 40 individuals in total. Only four of the cases did not require an adjunct measure and the remaining cases had sedation or general anaesthesia to manage their dental needs.
These results suggest the possibility of the BDA Case Mix Model being used as a tool to determine the patients' need for adjunct measures and thus referral to a specialist level of care if such services are not available in the community.
However, from the results of the retrospective study, it was shown that not all of the domains in the BDA Case Mix Model had a significant association with the need for an adjunct; an example of this was with the domain on oral risk. This finding is supported in the study by Duane et al., where they found that the omission of the assessment on oral risk had a minor effect on the internal consistency of the case mix tool and its presence did not add to its reliability.7
The limitations of the BDA Case Mix tool, including the inconsistency of the results obtained from the model in a recently published study,6 implies that the results of this study have to be analysed carefully. Also, many of the items in the tool could not be identified retrospectively from the dental records, some of which may have been due to poor entry in the records by the clinicians. These effects limited the accuracy of the findings obtained. Another factor affecting the results of this part of the study is that the researcher did not have any training or calibration in the use of the BDA Case Mix tool.
It is worth noting that, in its development, the BDA Case Mix tool was intended to be used retrospectively by the providing dentists based on their experience on providing care. It is also important to note that the tool is treatment specific and for each individual the complexity can vary from one visit to another, depending on the type of treatment provided.5
Nevertheless, this part of the study helped the larger study that was conducted following this retrospective study in collecting the items to develop a tool for assessing suitable dental service settings for people with disabilities.
Conclusion
Specialist services are required for providing care to individuals who are unable to cope with dental treatments provided in a primary care setting. Using the BDA Case Mix Model, it was possible to measure the complexity of the dental patients seen at the special care dentistry clinic in Dublin Dental University Hospital. It was evident that a mix of patients with different levels of complexity were being referred to this specialist service.
The BDA Case Mix Model demonstrated the need for adjunct measures in those individuals with higher levels of complexity, as measured by this model. The results suggest the possibility of using the model to measure the need for supportive adjunct measures such as sedation and general anaesthesia. Factors such as anxiety and fear will necessitate the use of these services which are mainly available in specialist centres in Ireland. However, it is apparent from the results that a large number of those referred to the dental hospital did not require any adjuncts for their dental treatment. Some of the referrals to specialist services were for a second opinion, where the dental needs were complex or required interdisciplinary care, not readily available at a primary care level, for whatever reasons. Medical risk is another common reason for referring patients to specialist centres. However, some medical conditions can be safely managed at a primary care setting with proper training and knowledge; dental professionals need to gain the skills necessary to enable them to provide dental care safely in a primary care setting.
The application of the available tools in the literature was useful in focusing on the main factors driving the decision for referring cases for specialist service settings.
References
Anders P L, Davis E L . Oral health of patients with intellectual disabilities: a systematic review. Spec Care Dent 2010; 30: 110–117.
Prabhu N T, Nunn J H, Evans D J, Girdler N M . 2008. Development of a screening tool to assess the suitability of people with a disability for oral care under sedation or general anesthesia. Spec Care Dent 28: 145–158.
Faulks D, Norderyd J, Molina G, Phadraig C M, Scagnet G, Eschevins C, Hennequin M . (2013). Using the International Classification of Functioning, Disability and Health (ICF) to describe children referred to special care or paediatric dental services. PloS One 8: e61993.
Carey H, Ackerie A, Houtzaerr L, Purnomo J, Jeganathan S . Oral health referral trigger tools for people living with HIV. Spec Care Dent 2014; 34: 41–45.
Bateman P, Arnold C, Brown R . BDA special care case mix model. Br Dent J 2010; 208: 291–296.
Burgess M, Monaghan N, Morgan M Z, Playle, R ., Thompson, S . Reliability of the BDA case mix tool for the use in special care dentistry. J Dis Oral Health 2011; 12: 107–113.
Duane B G, Humphris G, Richards D, Okeefe, E J, Gordon K, Freeman R . Weighing up the Weighted Case Mix Tool (WCMT): a psycho-metric investigation using confirmatory factor analysis. Comm Dent Health 2014; 31: 200–206.
Crowley E, Whelton H, Murphy A . Oral health of adults with an intellectual disability in residential care in Ireland 2003. Department of Health and Children: Dublin, 2005.
Health Service Executive. Strategic review of the delivery and management of HSE dental services. 2010. Information available online at. http://www.hse.ie/eng/services/publications/ (accessed April 2016).
National Disability Authority-Ireland 2009. Ethical guidance for research with people with disabilities. 2009. Information available online at http://nda.ie/Policy-and-research/Research/Research-Ethics/Ethical-Guidance-for-Research-with-People-with-Disabilities.html (accessed April 2016).
Assisted-Decision Making (Capacity) Act in Ireland (2015). http://www.oireachtas.ie/viewdoc.asp?DocID=30677 (accessed April 2016).
Author information
Authors and Affiliations
Corresponding author
Additional information
Refereed Paper
Rights and permissions
About this article
Cite this article
AlKindi, N., Nunn, J. The use of the BDA Case Mix Model to assess the need for referral of patients to specialist dental services. Br Dent J 220, 401–406 (2016). https://doi.org/10.1038/sj.bdj.2016.296
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.2016.296