Key Points
-
IOM is a primitive traditional practice involving the 'gouging out' of an infant's healthy primary tooth germs
-
IOM can lead to systemic complications and irreversible damage to the permanent dentition
-
IOM identified in the UK should be considered a child safeguarding issue
Abstract
Infant oral mutilation (IOM) is a primitive traditional practice involving the 'gouging out' of an infant's healthy primary tooth germs. This can lead to transmission of blood-borne diseases such as HIV/ AIDS, septicaemia and death. Other complications include eradication and/ or malformation of the child's permanent dentition. IOM is usually performed by village healers in low income countries as an accepted remedy for common childhood illness. The gingival swelling of the unerupted teeth is mistakenly thought to indicate the presence of 'tooth worms'. Crude methods to remove these are employed using unsterile tools. IOM has been reported in many African countries. More recently, some immigrants living in high income countries, such as the UK, have shown signs of IOM. Our aim is to raise awareness among clinicians about the existence of IOM practice being carried out among respective African immigrant groups. We encourage clinicians, particularly those working with paediatric patients to inform parents and carers of children with a history of IOM about the risks and consequences. As part of child safeguarding policies, dental practitioners and health care professionals should intervene if they are aware of any perceived plan that IOM is to be carried out in the future.
Similar content being viewed by others
Background
There has been increased media coverage and published literature about female genital mutilation (FGM) in the UK and worldwide,1,2,3 but very little is known about infant oral mutilation (IOM).
We aim to highlight the practice of this traditional healing practice involving the mouth. This is particularly prudent in light of recent increased mobilisation and immigration from Africa to developed countries over the last 20 years.4,5 These young children may present to general dental practitioners with complex dentitions as a result of IOM. This traditional practice is mainly performed in children in Eastern Africa which involves the 'gouging out' of tooth germs, and is carried out by village healers for what they deem as medical intervention. We wish to raise awareness of this condition and the recognition of the dentoalveolar complications which may present later in life.
The term
IOM is known by alternative terms by both the international dental community (Table 1), and by the indigenous populations, depending on the country in which it is practised (Table 2). Traditionally, among tribes, there are many terms for IOM (Table 3).
More recently, Mogensen coined the term 'germectomy' in Uganda, for a more radical form of practice involving removal of primary canines and / or permanent tooth germs6,7 which led to missing, impacted or malformed permanent canines.
History
The historical origins of IOM is unknown, although canine enucleation has been well described in many regions of Africa.8
It is speculated that the practice was introduced to East Africa by colonial dentists and subsequently adopted by traditional healers.9 Incising the gingiva over an erupting tooth as a means of decreasing pain was promoted in Europe by Joseph Hurlock in 1742 and then continued into the twentieth century.9
It was first reported in the 1930s in the Neur pagan tribes of Nilotic in Sudan, Africa4,6,10 where primary canines of infants were enucleated with a piece of iron. In the 1960s, it was reported among the Maasai, in Kenya and subsequently spread to Uganda and Tanzania.4 It was later introduced in vvsouthern Sudan by refugees from Uganda and neighbouring countries.4,6,9
Avetiology
IOM is essentially based on a cultural belief that the swelling in the area of the gums associated with un-erupted primary teeth causes illnesses such as diarrhoea, prolonged fever, vomiting, loss of appetite, dehydration, infectious diseases,11,12,13,14,15,16 gastroenteritis,4 aspiration bronchopneumonia,17 and growth retardation.18 Other reported reasons for such practice include general malaise or ill health, itching gums, crying with an unknown cause and failure to suckle.9,19
The perceived medical benefits of IOM range from preventing and treating bodily symptoms to prevention of the death of the baby.6,20 This tends to be more common in rural areas, with a less educated population and lower socio-economic status.13,16,21,22,23
The practice of IOM is deeply rooted in people's beliefs and is therefore challenging to modify or change.21 A study by Nuwaha et al. of 215 heads of households concluded that more than 80% of respondents used traditional medicine alone or in combination with modern medicine to treat 'false teeth'21 in the Bushenyi district of Uganda. In Tanzania, Kikwilu et al. report that more than 50% of parents took their children to a traditional healer after receiving advice from esteemed members of their communities.20
Kenyan focus groups with mothers of Maasi infants older than two years revealed that canine tooth buds are thought to be associated with bad spirits that cause diarrhoea and vomiting, and IOM would provide a cure.18
The underlying causes for such superstitious beliefs is lack of education, poverty, lack of belief in medical practice and a lack of basic medical infrastructure.19
In various regions of Africa there have been several interventions condemning IOM. In Tanzania, since 1983 there have been public addresses by political leaders and the use of mass media for health education messages. In Kenya, non-government organisations (NGO), such as Kinga Africa, provide free health education and awareness of IOM.
In the UK, the oral health charity Dentaid has been committed to the eradication of IOM since 1999 and in 2008 an action group against IOM was set up to examine this common malpractice and evaluate ways of preventing it.24
However, sociological and environmental factors are on-going and need to be addressed.20 In the west, cultural and deep-rooted beliefs are challenging to address, particularly in migrant communities. IOM will continue outside of the native settlements if the healthcare professionals in high income countries are not aware of its existence.
Prevalence
The practice of IOM has been reported in many African countries including Republic of the Sudan, South Sudan, Tanzania, Kenya, Ethiopia, Uganda, Somalia, DR Congo, Burundi, Chad, Rwanda and Burkina Faso.25
IOM is not confined to communities in Sub-Saharan Africa, but is now recognised and reported in many western countries.26 There are reports of prevalence of traditional extraction of primary canines in Ethiopian Jewish children living in Israel (1994), Ethiopians living in Sweden (1999), and Somali children living in the United States (2000).6 Other cases of IOM have also been reported in Norway, France, Australia, and New Zeland.13,27,28
In the UK, IOM was more common among UK-born children with immigrant Somali mothers who did not speak English and were from rural and less educated communities.8
Offspring of parents who had emigrated from Ethiopia 15–20 years earlier have been reported to have greater prevalence of missing primary canines and dental defects, when compared with the native Israeli parents living in the same low socio-economic neighbourhoods.27
The lack of accessibly to healthcare for these communities may be explained by the stress of migration which can lead to depression, reduced self-confidence, personal and family crises, low utilisation of health services, and unfavourable health behaviour.27
The practice
IOM is usually carried out by a village healer30 with no formal medical training, but is recognised by the local community as competent to provide health care by using vegetable, animal and mineral substances and methods in treating disease and disability.31 They are a well-established institution and are often esteemed members of their villages.19
A village healer is a highly recognised, respected older woman, family member, priest, teacher, religious healer or the tribal head,20 who makes a living from ritualistic practices like IOM.4,9
IOM is performed in non-sterile conditions using basic sharp instruments such as regular knives, razor blades, bicycle spokes, finger nails and hot nails without anaesthesia (Fig. 1).4,11,19,26,32,33,34
Teeth affected
The most commonly affected teeth are mandibular canines9,10,13,32,33,34 followed by lateral incisors.32 This is due to the fact that mandibular primary canine tooth germs are easily noticed as the whitish buldges.30
Village healers note the pale mandibular canine swelling to be abnormal and a cause of the child's illness.30 The tooth follicles resemble worms to some village healers as they are soft mineralised masses of tissue (Fig. 2).20
In all cases tooth buds are extracted bilaterally9,10,27,30 and affected children would have either two or four missing primary teeth; more than four in rare cases.30
It is usually performed on children under one year of age and affects both boys and girls equally.18,30
In Uganda, procedures are carried out from six months to three years of age6 with the peak ages between 4–18 months.4
Complications of IOM
Complications of IOM can be systemic and local (dentoalveolar).
The systemic complications of IOM include anaemia, pneumonia, meningitis, tetanus, as well as risk of transmission of blood born infections such as hepatitis B, and HIV. In severe cases septicaemia can lead to death.8,13,20,21,26,30,32
A Ugandan study reported 21% of paediatric admissions were caused by the effects of treatment for 'nylon teeth' resulting in death.34 Other complications are listed in Table 4.
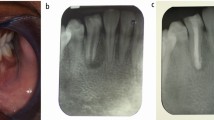
Although IOM is carried out in the early primary dentition, detrimental and irreversible impact on the permanent dentition can occur later in life (Fig. 2,3).
Enamel hypoplasia with circular hypoplastic defects of the labial surface of the mandibular crown,8 and malformation of canines and adjacent teeth have been reported.27 Other dentoalveolar complications include retention of primary lateral incisors, midline and occlusal discrepancies, displacement and impaction of permanent teeth, ectopic eruption, development of peg-shaped and invaginated teeth, transpositions, and early eruption of permanent teeth where primary buds were removed.27
In a study by Hanssanli et al. 87% of children had undergone extraction of mandibular primary and permanent central incisors in a dental cast study of 6–8 and 12-year-old Kenyan children. When compared with other comparable groups, there was a marked decrease in inter-canine distance, mandibular anterior arc circumferences and mandibular length.35 Other complications are listed in Table 5.4,5,6,8,20,26,27,33,35
Child protection against IOM – globally and in the UK
It is well established that the practice of Female Genital Mutilation (FGM) has been a criminal offence in the UK since 1985 (Prohibition of Female Circumcision Act). This has now been superseded by a 2003 act where it is now an offence for any person in England, Wales and Northern Ireland to perform FGM; or assist a girl to carry out FGM on herself. This includes non-UK nationals or residents performing FGM outside the UK on a UK national or permanent UK resident. This is, in fact, punishable by a prison sentence between 4–14 years.36
No such law exist in the UK for IOM. Healthcare professionals may not be aware of IOM due to the limited literature and publicity.
In the United National Convention on the Right of the Children in 1989, world leaders agreed the rights and protections of children (under 18 years of age) globally.37
In the UK, NHS England published a framework intended to support NHS organisations to fulfil their statutory child safeguarding duties.38
As a dental profession, we share the responsibility of upholding the welfare of children and we are governed by the General Dental Council's standards guidance. This clearly states that the dental team has an ethical obligation to take appropriate action if concerned about the possible abuse of a child:
'Find out about local procedures for the protection of children and vulnerable adults. You must follow these procedures if you suspect that a child or vulnerable adult may be at risk because of abuse or neglect.'39
The Care Quality Commission also outlines safety standards and regulations required to be met by dental service providers:
'Ensure that government and local guidance about safeguarding people from abuse is accessible to all staff and put into practice.'40,41
IOM is a harmful practice with negative consequences including death. It requires a long-term and sensitive approach by clinicians, and discussion among African parents and carers who often have deeply rooted cultural beliefs. Simplistic health education approaches that are available in the west may not be sufficient to change their traditional ritualistic beliefs. Trained and skilled counsellors with an in-depth understanding of African cultures are needed to tackle these negative cultural beliefs and practices, often mistaken as a medical intervention. Like FGM, IOM should be made a child protection issue not just in the UK, but also in African countries in order to raise the awareness of this harmful practice.
Conclusion
Healthcare professionals practising dentistry in the UK often provide a service in richly diverse and multi-ethnic communities. IOM should be considered when patients present with dental anomalies, particularly affecting the canines, without an obvious cause. We should recognise the odontogenic sequelae and complications of IOM, particularly among those who are African refugees or migrants.
A sensitive approach and communication from clinicians is essential in educating the parents and carers, as they often hold deep seated core values and cultural traditions. Should a dental practitioner or healthcare professional perceive possible planned IOM to be carried out in the parents' native country, it should be managed in accordance with the child's safeguarding policies.
Disclosures
This paper is part of a presentation at the XXII conference of the International Oral and Maxillofacial Surgery, Melbourne, Australia, 2015.
More information and resources about IOM A comprehensive overview of the subject is available at www.dentaid.org/infant-oral-mutilation . For more information, please contact Dentaid, Giles Lane, Landford, Salisbury, SP5 2BG, UK Tel: +44 (0) 1794 324,249
References
NHS Choices. Female genital mutilation. Available online at http://www.nhs.uk/conditions/female-genital-mutilation/Pages/Introduction.aspx (accessed March 2016).
World Health Organization (WHO). Female genital mutilation. Updated 2016. Available online at http://www.who.int/mediacentre/factsheets/fs241/en/.
Garba I D, Muhammed Z, Abubakar I S, Yakasai I A . Prevalence of female genital mutilation among female infants in Kano, Norhtern Nigeria. Arch Gynecol Obstet 2012; 286: 423–428.
Graham E A, Domoto P K, Lynch H, Egbert M A . Dental injuries due to African traditional therapies for diarrhoea. West J Med 2000; 173: 135–137.
Amailuk P, Grubor D . Erupted compound odontoma: case report of a 15-year-old Sudanese boy with a history of traditional dental mutilation. Br Dent J 2008; 204: 11–14.
Barzangi J, Unell L, Söderfeldt B, Bond J, Musse I F, Arnrup K . Infant dental enucleation in an East African population in Sweden: a cross-sectional study on dental records. Intern J Paed Dent 2014; 24: 209–214.
Mogensen H O . False teeth and real suffering: The social course of 'Germectomy' in Eastern Uganda. Cult Med Psychiatry 2000; 24: 331–351.
Rodd H D, Davidson LE . 'Ilko dacowo: ' canine enucleation and dental sequelae in Somali children. Inter J Paed Dent 2000; 10: 290–297.
Johnston N L, Riordan P J . Tooth follicle extirpation and uvulectomy. Aust Dent J 2005; 50: 267–272.
Pindborg J J . Dental mutilation and associated abnormalities in Uganda. Am J Phys Anthropol 1969; 31: 383–389.
Edwards P C, Levering N . Wetzel E, Saini T . Extirpation of the primary canine tooth follicles: a form of infant oral mutilation. J Am Den Assoc 2008; 139: 442–450.
da Fonseca M A, Hoge C . Extraction of “killer” teeth: the case of two Somali siblings. J Dent Child (Chic) 2007; 74: 143–146.
Bataringaya A, Ferguson M, Lalloo R . The impact of ebinyo, a form of dental mutilation, on the malocclusion status in Uganda. Community Dental Health 2005; 22: 146–150.
Edwards P C, Levering N, Wetzel E, Saini T . Extirpation of the primary canine tooth follicles. J Am Dent Assoc 2008; 139: 442–450.
Baba S P, Kay E J . The mythology of the killer deciduous canine tooth in southern Sudan. J Paedod 1989; 14: 48–49.
A/Wahab M M . Traditional practice as a cause of infant morbidity and mortality in Juba area (Sudan). Ann Trop Paediatr 1987; 7: 18–21.
Woodruff A W, Suni A E, Kaku M, Adamson E A, Maughan T S, Bundru. Infants in Juba, Southern Sudan: the first six months of life. Lancet 1983; 322: 262–264.
Mutai J, Muniu E, Sawe J, Hassanali J, Kibet P, Wanzala P . Socio-cultural practices of deciduous canine tooth bud removal among Maasai children. Int Dent J 2010; 60: 94–98.
Noman A V, Wong F, Pawar R R . Canine gouging: A taboo resurfacing in migrant urban population. Case Rep Dent 2015.
Kikwilu E N, Hiza J F R . Tooth bud extraction and rubbing of herbs y traditional healers in Tanzania: prevalence, and sociological and environmental factor influencing the practices. Int J Paed Dent 1997; 7: 19–24.
Nuwaha F, Okware J, Janningtone T, Charles M . False teeth 'ebiino' and millet disease 'oburo' in Bushenyi district in Uganda. Afr Health Sci 2007; 7: 25–32.
Rasmussen P, Elhassan E, Raadal M . Enamel defects in primary canines related to traditional treatment of teething problems in Sudan. Int J Paed Dent 1992 2: 151–155.
Kahabuka F K, Mugonzibwa E A, Mwalutambi S, Kikwilu E N . Diseases and conditions falsely linked with 'nylon teeth' myth: a cross sectional study of Tanzanian adults. Tana J Health Res 2015; 17: 1–10.
Longhurst R . Tooth gouging: an African tradition. Dent Nurs 2015; 11: 379–382.
Gollings J, Longhurst R H . Infant oral mutilation 2013. Dentaid 2013. Available online at http://dentaid.org/wp-content/uploads/IOM-September-2013.pdf (accessed March 2016).
Beavis F, Foster A, Fuge K, Whyman R . Infant oral mutilation: a New Zealand case series. New Zealand Dent J 2011; 107: 57–59.
Davidovich E, Kooby E, Shapira J, Ram D . The traditional practice of canine bud removal in the offspring of Ethiopian immigrants. BMC Oral Health 2013; 13: 34.
Barbieri P, Focardi M, Pradella F, Garatii S . Infant Oral Mutilation (IOM). J Forse Odontostomatology 2013; 31(Suppl 1): 156.
Zini A, Vered Y, Sgan-Cohen H D . Are immigrant populations aware about their oral health status? A study among immigrants from Ethopia. BMC Public Health 2009; 26: 205.
Hiza J F R, Kikwilu E N . Missing primary teeth due to tooth bud extraction in a remote village in Tanzania. Int J Paediatr Dent 1992; 2: 31–34.
Ngilisho L A F, Mosha H J, Poulsen S . The role of traditional healers in the treatment of toothache in Tanga Region, Tanzania. Community Dent Health 1994; 11: 240–242.
Matee M I N, van Palenstein Helderman W H . Extraction of 'Nylon' tooth and associated abnormalities in Tanzanian children. African Dent J 1991; 5: 21–25.
Khonsari R H, Corre P, Perrin J-P . Piot B . Orthodontic consequences of ritual dental mutilations in Northern Tchad. J Oral Maxillofac Surg 2009; 67: 902–905.
Iriso R, Accorsi S, Akena S et al. 'Killer' canines: the morbidity and mortality of ebino in northern Uganda. Trop Med Int Health 2000; 5: 706–710.
Hassanali J, Odhiambo J W . Analysis of dental casts of 6–8 and 12 year old Kenyan children. Europ J Ortho 2000; 22: 135–142.
The National Archives. Female Genital Mutilation Act 2003. Available online at http://www.legislation.gov.uk/ukpga/2003/31 (accessed March 2016).
British Dental Association. Child protection and safeguarding. 2015. Online information available at https://www.bda.org/dentists/policy-campaigns/research/patient-care/childprotection (accessed March 2016).
NHS Commissioning Board. Safeguarding vulnerable people in the reformed NHS accountability and assurance framework. 2013. Available online at https://www.england.nhs.uk/wp-content/uploads/2013/03/safeguarding-vulnerable-people.pdf (accessed March 2016).
General Dental Council. Standards for the dental team. 2013. Online information at http://www.gdc-uk.org/dentalprofessionals/standards/pages/standards.aspx (accessed March 2016).
Royal College of Paediatrics and Child Health. Safeguarding children and young people: roles and competences for healthcare staff. Intercollegiate document. 3rd ed. RCPCH, 2014. Available online at http://www.rcpch.ac.uk/sites/default/files/page/Safeguarding%20Children%20-%20Roles%20and%20Competences%20for%20Healthcare%20Staff%20%2002%200%20%20%20%20(3)_0.pdf (accessed March 2016).
Care Quality Commission. Guidance about compliance. Essential standards of quality and safety. pp 92–101. Care Quality Commission, 2010.
Acknowledgements
The authors would like to thank Dentaid for kind permission for use of the photographs included in this article.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Girgis, S., Gollings, J., Longhurst, R. et al. Infant oral mutilation – a child protection issue?. Br Dent J 220, 357–360 (2016). https://doi.org/10.1038/sj.bdj.2016.264
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.2016.264
This article is cited by
-
Infant oral mutilation: data collection, clinical management and public health guidelines
British Dental Journal (2022)
-
Child refugees and asylum seekers: oral health and its place in the UK system
British Dental Journal (2020)
-
Child refugees and asylum seekers: oral health and its place in the UK system
BDJ Team (2020)
-
The dental complications of canine tooth bud removal in 2–12 years old children in Northwest Ethiopia
BMC Research Notes (2019)
-
Prevalence and dental effects of infant oral mutilation or Ebiino among 3–5 year–old children from a rural district in Uganda
BMC Oral Health (2019)